Submitted:
10 November 2025
Posted:
11 November 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
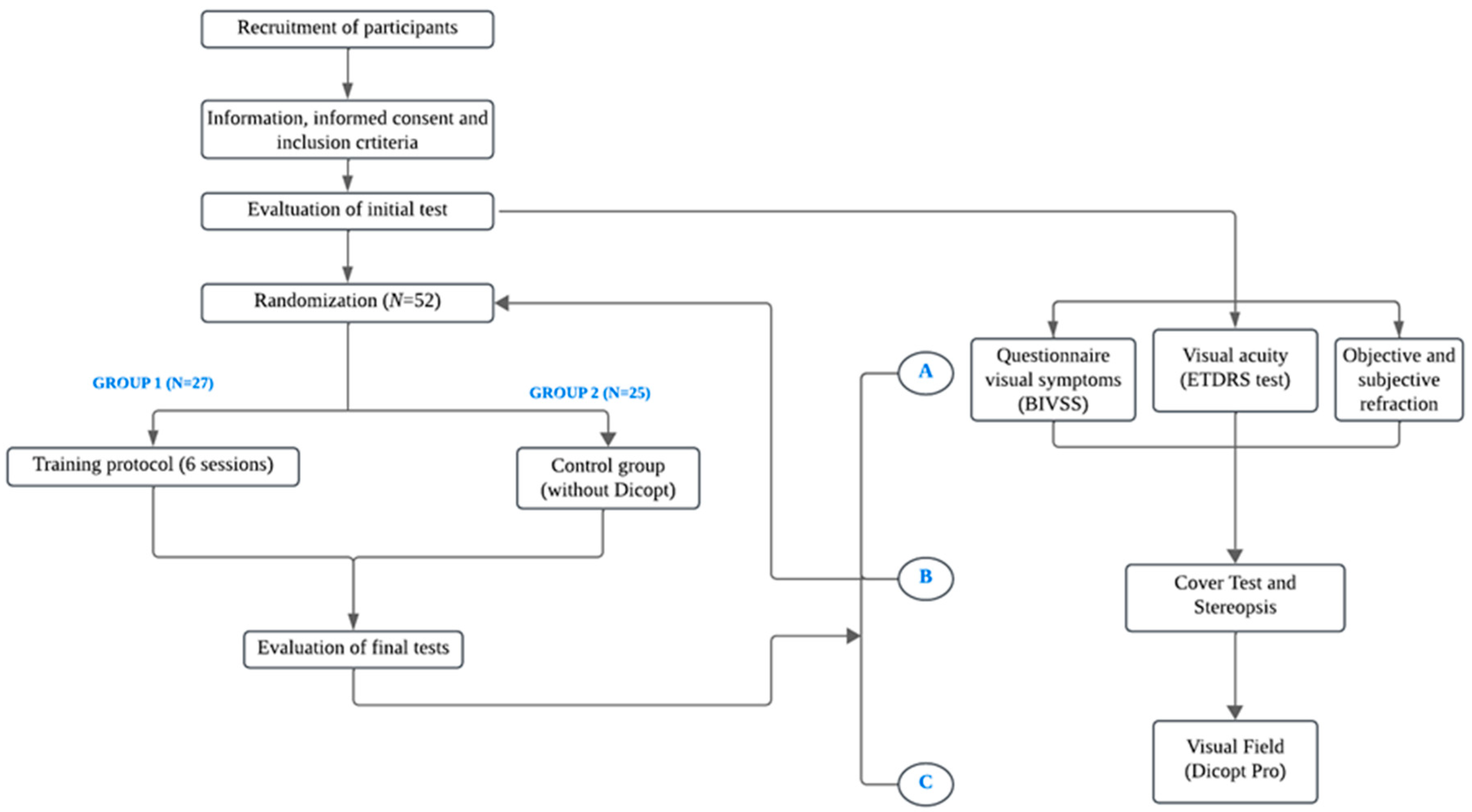
2. Materials and Methods
2.1. Sample
2.2. Experimental Protocol
- Percentage of detected stimuli (“seen/not seen”) per quadrant (%),
- Reaction time per quadrant (ms).
- Module 1: “Monster Game”- oculomotor training (2 sessions),
- Module 2: “Runner”- binocular vision training (2 sessions),
- Module 3: “Double Space”- vergence training (2 sessions).
2.3. Materials
- Brain Injury Vision Symptom Survey (BIVSS): Visual symptoms were assessed using the validated Brain Injury Vision Symptom Survey (BIVSS) questionnaire (Laukkanen et al., 2017(15)), composed of 28 items addressing blur, double vision, glare, photophobia, eye discomfort, dryness, depth perception, peripheral awareness, and reading difficulties. Each item was rated according to symptom frequency, providing an overall score that reflects the perceived visual impact in patients with acquired brain injury.
- Visual Acuity (VA): Best-corrected VA was measured monocularly and binocularly using a standard ETDRS logMAR chart (Early Treatment Diabetic Retinopathy Study) at 4 m for distance and 40 cm for near vision. The smallest line correctly identified by the participant was recorded as the final VA score.
- Cover Test (CT): The CT was performed for both distance and near fixation to identify and quantify ocular misalignments using prism bars. Base-in (BI) prisms were applied for exodeviations and base-out (BO) prisms for esodeviations. The fixation target corresponded to two lines below the VA of the worse eye.
- Stereopsis: Depth perception was evaluated at 40 cm using the Titmus stereo test with polarized glasses. The smallest measurable disparity in seconds of arc was recorded as the stereopsis threshold.
- Visual Field (VF): Binocular VF (120°) was evaluated using the Dicopt Pro virtual reality (VR) device, which integrates an eye-tracking system. After calibration, participants fixated on a central red cross and pressed a trigger each time they detected a peripheral stimulus. The test automatically paused if fixation was lost. A “seen/not seen” strategy was applied to assess the functional VF across quadrants, and results were automatically generated and exported for analysis (Figure 2).

- Dicopt Home Vision Therapy: The intervention was carried out using the Dicopt Home mobile application, a VR-based tool that allows patients to perform vision therapy (VT) either in a clinical or home-based setting. The system is designed to enhance binocular vision, accommodation, and oculomotor control by presenting distinct stimuli to each eye, thus promoting binocular integration.
- Monster Game: oculomotor training; participants aim and shoot only at the monster matching the central reference image (Figure 4a).
- Runner: binocular coordination training; the goal is to avoid obstacles and collect coins by pressing the “X” button to jump (Figure 4b).
- Double Space: vergence training; participants control two spaceships—blue (left joystick) and red (right joystick)—to avoid asteroids and collect stars of the corresponding color (Figure 4c).
2.4. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
| ABI | Acquired Brain Injury |
| BI | Base-In (prism) |
| BIVSS | Brain Injury Vision Symptom Survey |
| BO | Base-Out (prism) |
| BT | Brain Tumor |
| CT | Cover Test |
| CVA | Cerebrovascular Accident |
| DEM | Developmental Eye Movement Test |
| EEG | Electroencephalography |
| fMRI | Functional Magnetic Resonance Imaging |
| IPD | Interpupillary Distance |
| IQR | Interquartile Range |
| PPS | Percentage of Points Seen |
| RT | Reaction Time |
| TBI | Traumatic Brain Injury |
| VA | Visual Acuity |
| VF | Visual Field |
| VR | Virtual Reality |
| VT | Vision Therapy |
References
- De Dios Perez, B.; Morris, R.P.G.; Craven, K.; Radford, K.A. Peer mentoring for people with acquired brain injury—A systematic review. Brain Inj. 2024, 38, 316–329. [Google Scholar] [CrossRef]
- Wang, Z.; He, K.; Sui, X.; Yi, J.; Yang, Z.; Wang, K.; et al. The effect of web-based telerehabilitation programs on children and adolescents with brain injury: Systematic review and meta-analysis. J. Med. Internet Res. 2023, 25, e46957. [Google Scholar] [CrossRef]
- Berthold Lindstedt, M.; Johansson, J.; Ygge, J.; Borg, K. Vision-related symptoms after acquired brain injury and the association with mental fatigue, anxiety and depression. J. Rehabil. Med. 2019, 51, 499–505. [Google Scholar] [CrossRef] [PubMed]
- Rowe, F.J.; Hanna, K.; Evans, J.R.; Noonan, C.P.; Garcia-Finana, M.; Dodridge, C.S.; et al. Interventions for eye movement disorders due to acquired brain injury. Cochrane Database Syst. Rev. 2018, 3, CD011290. [Google Scholar] [CrossRef] [PubMed]
- Yoo, P.Y.; Scott, K.; Myszak, F.; Mamann, S.; Labelle, A.; Holmes, M.; et al. Interventions addressing vision and visual-perceptual impairments following acquired brain injury: A cross-sectional survey. Can. J. Occup. Ther. 2020, 87, 117–126. [Google Scholar] [CrossRef]
- Ciuffreda, K.J.; Rutner, D.; Kapoor, N.; Suchoff, I.B.; Craig, S.; Han, M.E. Vision therapy for oculomotor dysfunctions in acquired brain injury: A retrospective analysis. Optometry 2008, 79, 18–22. [Google Scholar] [CrossRef]
- Ciuffreda, K.J.; Kapoor, N.; Rutner, D.; Suchoff, I.B.; Han, M.E.; Craig, S. Occurrence of oculomotor dysfunctions in acquired brain injury: A retrospective analysis. Optometry 2007, 78, 155–161. [Google Scholar] [CrossRef]
- Bridge, H. Effects of cortical damage on binocular depth perception. Philos. Trans. R. Soc. Lond. B Biol. Sci. 2016, 371, 1697. [Google Scholar] [CrossRef] [PubMed]
- Mueller, I.; Gall, C.; Kasten, E.; Sabel, B.A. Long-term learning of visual functions in patients after brain damage. Behav. Brain Res. 2008, 191, 32–42. [Google Scholar] [CrossRef]
- Pouget, M.C.; Lévy-Bencheton, D.; Prost, M.; Tilikete, C.; Husain, M.; Jacquin-Courtois, S. Acquired visual field defects rehabilitation: Critical review and perspectives. Ann. Phys. Rehabil. Med. 2012, 55, 53–74. [Google Scholar] [CrossRef]
- McDonald, M.A.; Tayebi, M.; McGeown, J.P.; Kwon, E.E.; Holdsworth, S.J.; Danesh-Meyer, H.V. A window into eye movement dysfunction following mTBI: A scoping review of magnetic resonance imaging and eye-tracking findings. Brain Behav. 2022, 12, e2714. [Google Scholar] [CrossRef] [PubMed]
- Johansson, J.; Berthold Lindstedt, M.; Borg, K. Vision therapy as part of neurorehabilitation after acquired brain injury—A clinical study in an outpatient setting. Brain Inj. 2021, 35, 82–89. [Google Scholar] [CrossRef]
- Vilageliu-Jordà, E.; Enseñat-Cantallops, A.; García-Molina, A. Use of immersive virtual reality for cognitive rehabilitation of patients with brain injury. Rev. Neurol. 2022, 74, 331–339. [Google Scholar] [CrossRef]
- Martino Cinnera, A.; Verna, V.; Marucci, M.; Tavernese, A.; Magnotti, L.; Matano, A.; et al. Immersive virtual reality for treatment of unilateral spatial neglect via eye-tracking biofeedback: RCT protocol and usability testing. Brain Sci. 2024, 14, 283. [Google Scholar] [CrossRef]
- Laukkanen, H.; Scheiman, M.; Hayes, J.R. Brain Injury Vision Symptom Survey (BIVSS) questionnaire. Optom. Vis. Sci. 2017, 94, 43–50. [Google Scholar] [CrossRef]
- Rowe, F.J.; WRightt, D.; Brand, D.; Jackson, C.; Harrison, S.; Maan, T.; et al. A prospective profile of visual field loss following stroke: Prevalence, type, rehabilitation, and outcome. Biomed. Res. Int. 2013, 2013, 719096. [Google Scholar] [CrossRef]
- Lee, Y.J.; Lee, S.C.; Wy, S.Y.; Lee, H.Y.; Lee, H.L.; Lee, W.H.; et al. Ocular manifestations, visual field pattern, and visual field test performance in traumatic brain injury and stroke. J. Ophthalmol. 2022, 2022, 1703806. [Google Scholar] [CrossRef] [PubMed]
- Matteo, B.M.; Viganò, B.; Cerri, C.G.; Perin, C. Visual field restorative rehabilitation after brain injury. J. Vis. 2016, 16, 11. [Google Scholar] [CrossRef] [PubMed]
- Aimola, L.; Lane, A.R.; Smith, D.T.; Kerkhoff, G.; Ford, G.A.; Schenk, T. Efficacy and feasibility of home-based training for individuals with homonymous visual field defects. Neurorehabil. Neural Repair 2014, 28, 207–218. [Google Scholar] [CrossRef]
- Hazelton, C.; Todhunter-Brown, A.; Dixon, D.; Taylor, A.; Davis, B.; Walsh, G.; et al. The feasibility and effects of eye movement training for visual field loss after stroke: A mixed methods study. Br. J. Occup. Ther. 2020, 84, 030802262093605. [Google Scholar] [CrossRef]
- Smaakjær, P.; Wachner, L.G.; Rasmussen, R.S. Vision therapy improves binocular visual dysfunction in patients with mild traumatic brain injury. Neurol. Res. 2022, 44, 439–445. [Google Scholar] [CrossRef] [PubMed]
- Mena-Garcia, L.; Pastor-Jimeno, J.C.; Maldonado, M.J.; Coco-Martin, M.B.; Fernandez, I.; Arenillas, J.F. Multitasking compensatory saccadic training program for hemianopia patients: A new approach with 3-dimensional real-world objects. Transl. Vis. Sci. Technol. 2021, 10, 3. [Google Scholar] [CrossRef] [PubMed]
- Nelles, G.; Pscherer, A.; de Greiff, A.; Gerhard, H.; Forsting, M.; Esser, J.; et al. Eye-movement training-induced changes of visual field representation in patients with post-stroke hemianopia. J. Neurol. 2010, 257, 1832–1840. [Google Scholar] [CrossRef]
- Kerkhoff, G.; Münssinger, U.; Meier, E.K. Neurovisual rehabilitation in cerebral blindness. Arch. Neurol. 1994, 51, 474–481. [Google Scholar] [CrossRef] [PubMed]


| Total (n = 52) |
TBI (n = 9) |
CVA (n = 29) |
BT (n = 14) |
|||
|---|---|---|---|---|---|---|
| Age (years) | 51.00 (38.25, 60.75) |
50.00 (34.00-55.00) |
51.00 (40.50-61.00) |
54.50 (24.00-65.00) |
||
| VA (logMAR) | 0.00 (-0.10, 0.10) |
0.00 (-0.15, 0.08) |
0.00 (-0.10, 0.01) |
0.05 (0.00, 0.24) |
||
| Cover Test Far (Δ) | 0.00 (-2.00, 0.00) |
-2.00 (-9.00, 0.00) |
0.00 (-1.50, 0.00) |
0.00 (-2.25, 0.00) |
||
| Cover Test Near (Δ) | -3.00 (-8.00, 0.00) |
-14.00 (-17.00, -3.00) |
0.00 (-6.00, 0.00) |
-4.00 (-6.00, 0.00) |
||
| Stereopsis (arc sec) | 120.00 (60.0, 3552.0) |
100.00 (40.00, 1976.0) |
80.00 (45.00, 300.0) |
1976.00 (100.00, 3552.0) |
||
| PPS - VF (%) | Top Right | 79.00 (50.25, 94.00) |
86.00 (47.50, 94.00) |
77.00 (50.00, 89.50) |
81.00 (47.75, 96.00) |
|
| Bottom Righ | 88.00 (64.25, 98.00) |
83.00 (48.50, 98.00) |
90.00 (72.00, 98.00) |
87.00 (48.75, 98.00) |
||
| Top Left | 75.50 (46.00, 92.00) |
88.00 (53.50, 94.50) |
71.00 (45.00, 91.00) |
79.50 (40.75, 95.00) |
||
| Bottom Left | 91.50 (26.25, 100.00) |
98.00 (61.50, 99.00) |
88.00 (17.50, 100.00) |
79.50 (44.75, 100.00) |
||
| RT – VF (ms) | Top Right | 562.50 (511.50, 625.75) |
548.00 (451.00, 575.00) |
564.00 (506.50, 624.00) |
582.50 (540.50, 636.50) |
|
| Bottom Right | 554.00 (487.50, 599.50) |
523.00 (448.50, 575.50) |
563.00 (493.00, 618.00) |
556.00 (511.75, 594.25) |
||
| Top Left | 551.00 (494.75, 613.00) |
523.00 (448.50, 575.50) |
564.00 (503.50, 681.50) |
561.00 (479.25, 625.00) |
||
| Bottom Left | 543.50 (491.25, 608.25) |
503.00 (441.50, 587.50) |
541.00 (491.50, 686.00) |
557.50 (527.50, 612.75) |
||
| BIVSS (points) | 35.50 (25.50, 54.75) |
27.00 (16.50, 46.00) |
32.00 (27.00, 57.00) |
48.50 (34.50, 58.00) |
||
| Variable (unit) | Control Group (n = 25) | Therapy Group (n = 27) | Mann–Whitney U test |
|---|---|---|---|
| Age (years) | 50.0 (32.50, 62.50) | 52.00 (42.00, 59.00) | 0.63 |
| Visual Acuity (logMAR) | 0.00 (-0.10, 0.08) | 0.00 (-0.14, 0.10) | 0.14 |
| Ocular deviation – Distance (Δ) | 0.00 (-3.00, 0.00) | 0.00 (-2.00, 0.00) | 0.05 |
| Ocular deviation – Near (Δ) | -4.00 (-6.00, 0.00) | 0.00 (-8.00, 0.00) | 0.59 |
| Stereopsis (arc sec) | 200.0 (100.00, 3552.00) |
60.0 (40.00, 400.00) |
0.003 |
| Δ% Top Right VF | 1.00 (-1.00, 3.00) | 2.00 (-2.00, 8.00) | 0.25 |
| Δ% Lower Right VF | 0.00 (-2.00, 1.00) | 0.00 (-6.00, 8.00) | 0.77 |
| Δ% Top Left VF | 2.00 (-1.50, 2.00) | 2.00 (-4.00, 9.00) | 0.31 |
| Δ% Lower Left VF | 0.00 (-2.00, 1.00) | 0.00 (-6.00, 7.00) | 0.99 |
| ΔRT Top Right VF (ms) | 1.00 (-2.00, 9.50) | -6.00 (-34.00, 32.00) | 0.41 |
| ΔRT Lower Right VF (ms) | 0.00 (-6.00, 3.00) | -2.00 (-61.00, 15.00) | 0.40 |
| ΔRT Top Left VF (ms) | 1.00 (-3.50, 5.50) | -3.00 (-58.00, 19.00) | 0.43 |
| ΔRT Lower Left VF (ms) | 2.00 (-2.00, 21.00) | -8.00 (-50.00, 22.00) | 0.10 |
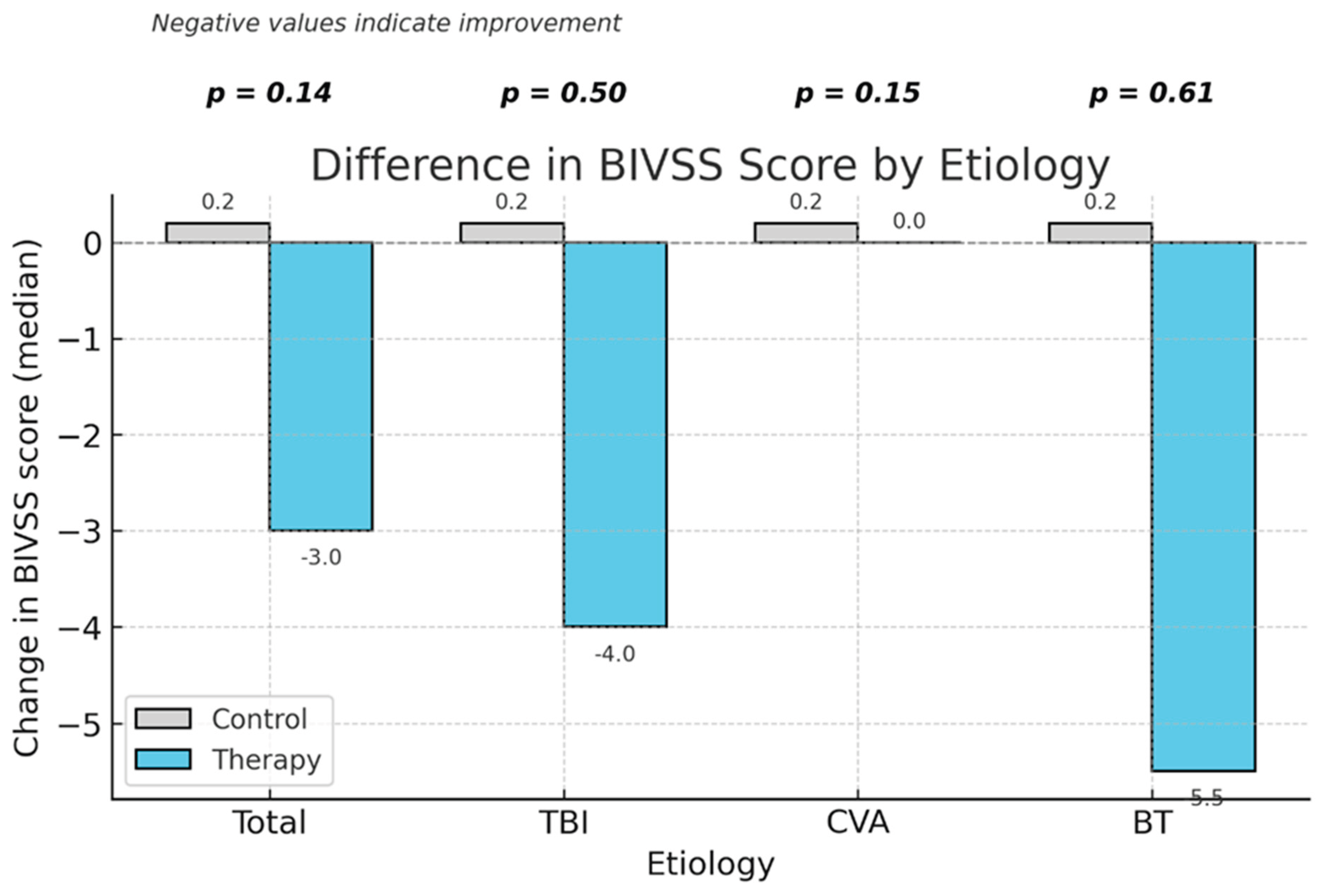
| ΔBIVSS (score) | 0.00 (-2.00, 0.00) | -3.00 (-8.00, 0.00) | 0.14 |
| Cause | Quadrant of the VF | Control group | Therapy group | Mann–Whitney U test |
|---|---|---|---|---|
| TBI | Top Right | 3.0 (3.0, 4.0) | 5.0 (2.0, 22.0) | 0.32 |
| Bottom Right | 0.0 (-2.0, 0) | 5.0 (-2.0, 29.5) | 0.32 | |
| Top Left | 2.0 (-2.0, 2.0) | 5.0 (3.0, 7.09) | 0.04 | |
| Bottom Left | 0.0 (-1.0, 1.0) | 2.0 (0.0, 8.5) | 0.32 | |
| CVA | Top Right | 1.5 (0.0, 5.0) | 2.0 (-2.0, 8.0) | 0.70 |
| Bottom Right | 0.0 (-2.0, 2.0) | 0.0 (-6.0, 8.0) | 0.73 | |
| Top Left | 1.5 (-1.0, 2.0) | 2.0 (-7.0, 9.0) | 0.58 | |
| Bottom Left | -0.5 (-1.0, 2.0) | -1.0 (-8.0, 7.0) | 0.66 | |
| BT | Top Right | 0.5 (-1.0, 2.0) | 1.5 (-1.5, 8.0) | 0.62 |
| Bottom Right | 0.0 (-1.0, 1.0) | -3.0 (-5.0, 11.5) | 0.22 | |
| Top Left | 1.5 (0.0, 2.0) | -2.5 (-5.0, 5.0) | 0.35 | |
| Bottom Left | -0.5 (-3.0, 1.0) | -1.0 (-4.0, 17.5) | 1.00 |
| Cause | Quadrant of the VF | Control group | Therapy group | Mann–Whitney U test |
|---|---|---|---|---|
| TBI | Top Right | 9.0 (5.0, 10.0) | -27.0 (-52.0, -5.5) | 0.18 |
| Bottom Right | 3.0 (-1.0, 18.0) | -31.5 (-75.0, -2.0) | 0.07 | |
| Top Left | 2.0 (2.0, 7.0) | -22.0 (-68.5,27.5) | 0.71 | |
| Bottom Left | 7.0 (2.0, 20.0) | -35.5 (-84.0,18.5) | 0.39 | |
| CVA | Top Right | 3.0 (-1.0, 15.0) | 15.0 (-41.0, 51.0) | 0.93 |
| Bottom Right | -1.0 (-7.0, 2.0) | 1.0 (-53.0, 22.0) | 0.82 | |
| Top Left | 1.5 (-3.0, 5.0) | -3.0 (-23.0, 19.0) | 0.89 | |
| Bottom Left | 2.5 (-4.0, 22.0) | -19.0 (-50.0,22.0) | 0.16 | |
| BT | Top Right | -0.75 (-7.0, 1.0) | -25.5 (-31.0, 9.0) | 0.18 |
| Bottom Right | -0.5 (-5.0, 6.0) | -26.5 (-63.5, 5.0) | 0.52 | |
| Top Left | 0.0 (-4.0, 3.0) | -15.5 (-78.0, 3.5) | 0.40 | |
| Bottom Left | -0.5 (-1.0, 8.0) | 2.5 (-24.5, 39.0) | 0.94 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




