Submitted:
14 October 2025
Posted:
15 October 2025
Read the latest preprint version here
Abstract
Keywords:
1. Introduction
2. Methods
3. Case Reports
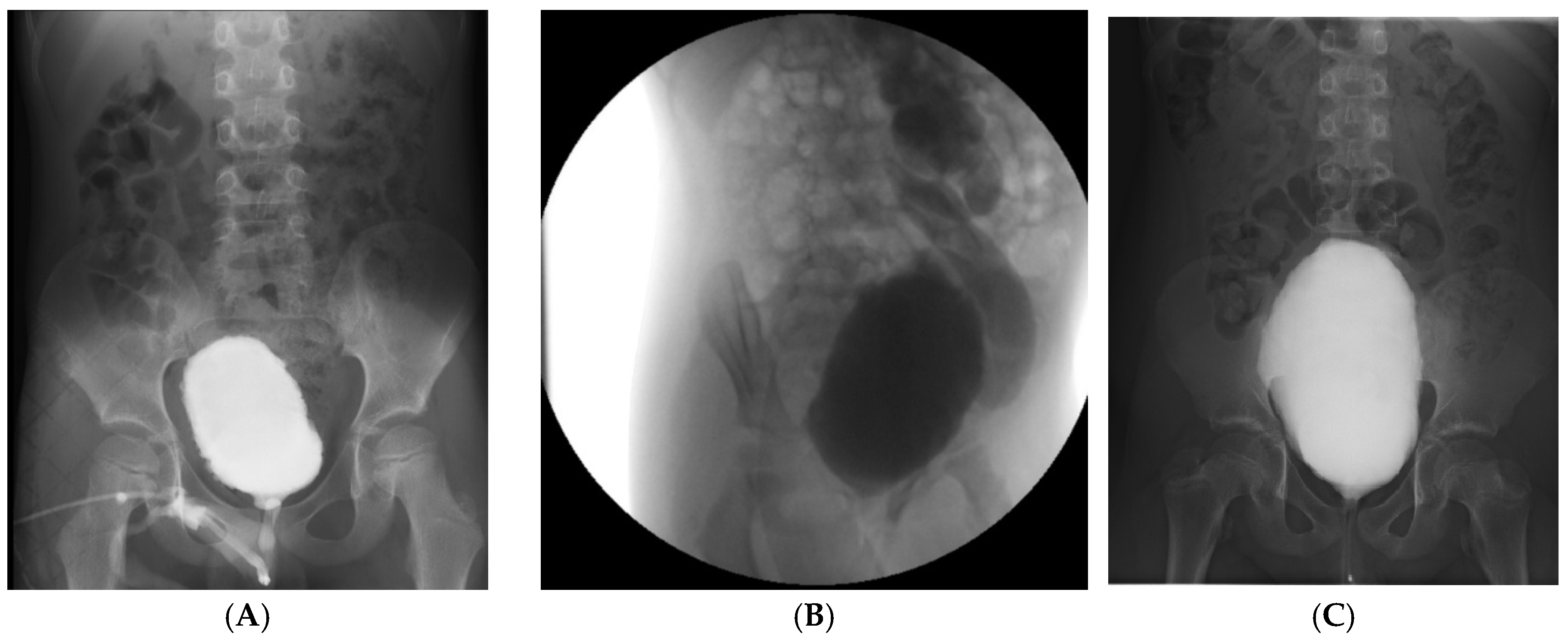
- (A) Case 1: Voiding cystourethrography showing a crenulated, asymmetric bladder contour without reflux;
- (B) Case 2: Voiding cystourethrography demonstrating grade V left vesicoureteral reflux with a tortuous, dilated ureter and dilated pelvis and calyces;
- (C) Case 3: Voiding cystourethrography depicting a large-capacity bladder with mild crenulation and grade I reflux, associated with incomplete voiding and high post-void residual;
4. Discussion
- 1.
- Pathophysiologic considerations
- 2.
- Clinical and Diagnostic Correlation
- 3.
- Hinman Syndrome and Its Relevance to Severe Functional LUTD
- 4.
- Management implications
- 5.
- Literature Review Methods
- 6.
- Outcomes and comparison with literature
- 7.
- Combination Therapy with Trospium Chloride and Biofeedback
- 8.
- Misdiagnosis and Iatrogenic Management Pitfalls
- 9.
- Prognosis and Long-Term Outcomes
- 10.
- Limitations
- 11.
- Clinical takeaways
5. Conclusions
Author Contributions
Funding
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| LUTD | Lower Urinary Tract Dysfunction |
| UTI | Urinary Tract Infection |
| VCUG | Voiding Cystourethrography |
| ED | Emergency Department |
References
- Austin PF, Bauer SB, Bower W, Chase J, Franco I, Hoebeke P. The standardization of terminology of lower urinary tract function in children and adolescents. Neurourol Urodyn 2016;35:471–81. [CrossRef]
- Chase J, Austin PF, Hoebeke P, McKenna P. The management of dysfunctional voiding in children: A report from the International Children’s Continence Society. Journal of Urology 2010;183:1296–302. [CrossRef]
- Nevéus T, von Gontard A, Hoebeke P, Hjälmås K, Bauer S, Bower W, et al. The standardization of terminology of lower urinary tract function in children and adolescents: report from the Standardisation Committee of the International Children’s Continence Society. J Urol 2006;176:314–24. [CrossRef]
- Kopač M, Lusuardi L, Sillen U. Pediatric lower urinary tract dysfunction. Biomedicines 2024;12:547. [CrossRef]
- Wang J, Cheng Z, Liu H. Underactive bladder and detrusor underactivity: From symptoms to pathophysiology. Int J Mol Sci 2023;24:8106. [CrossRef]
- Fuentes M, Figueroa V, Burbano J. Diagnosis and management of bladder dysfunction in children. Front Pediatr 2019;7:298. [CrossRef]
- Franco I. Functional bladder problems in children: Pathophysiology, diagnosis, and treatment. Pediatr Clin North Am 2012;59:783–817. [CrossRef]
- Keren R, Shaikh N, Pohl HG. Risk factors for recurrent urinary tract infection and renal scarring in children. JAMA Pediatr 2015;169:913–21. [CrossRef]
- Shaikh N, Morone NE, Lopez J. Recurrent urinary tract infections in children with bladder and bowel dysfunction. Pediatrics 2016;137:e20152982. [CrossRef]
- Veauthier B, Cabrera J. Urinary tract infections in young children and infants: Common questions and answers. Am Fam Physician 2020;102:278–85.
- Hinman F, Bauman FW. Functional disorders of the lower urinary tract in children: Nonneurogenic neurogenic bladder. Journal of Urology 1973;109:727–32.
- Hinman F. Nonneurogenic neurogenic bladder (the Hinman syndrome)—15-year follow-up of 14 cases. Journal of Urology 1986;136:769–77.
- Hinman F, Baskin LS. Hinman’s Atlas of Pediatric Urologic Surgery. Elsevier Health Sciences; 2009.
- Nevéus T, von Gontard A, Hoebeke P. The standardization of terminology of lower urinary tract function in children and adolescents. Neurourol Urodyn 2016;35:471–81. [CrossRef]
- Hoebeke P, Van Laecke E, Van Camp C. Non-neurogenic neurogenic bladder dysfunction in children: Pathophysiology and management. Eur Urol 2010;58:655–61. [CrossRef]
- Kocvara R, Sedláček J, Dvoráček J. Long-term follow-up of non-neurogenic neurogenic bladder in children. Eur Urol 2007;51:1720–8. [CrossRef]
- de Jong TPVM, Klijn AJ, Vijverberg MAW. Biofeedback treatment for non-neurogenic voiding dysfunction in children: Long-term results. Journal of Urology 2008;179:197–202. [CrossRef]
- Pereira JR. Trospium Chloride for the Treatment of Detrusor Instability in Children. Journal of Urology 2003;170:151–5. [CrossRef]
- Board UE. Efficacy and Safety of Trospium Chloride Use in Children With Idiopathic and Neurogenic Detrusor Overactivity: An Overview of Available Data. Urotoday 2011;4:34–8.
- Schultz-Lampel D, Steuber C, al. et. Urinary Incontinence in Children. Dtsch Arztebl Int 2011;108:418–25.
- Danilov V, Kuznetsov I, al. et. Dynamic Changes of the Residual Urine Symptom During Trospium Chloride Treatment in Children. Russian Journal of Pediatric Urology 2018;14:23–8.
- Lee DH, Kim YS, Lee HY, Han SW. Hinman Syndrome: Long-Term Follow-up of 14 Cases. Korean J Urol 2007;48:1058–64. [CrossRef]
- Jayanthi VR, Khoury AE, McLorie GA, Agarwal SK. The Nonneurogenic Neurogenic Bladder of Early Infancy. Journal of Urology 1997;158:1282–6. [CrossRef]
- Chaichanamongkol V, Ikeda M, Ishikura K. An Infantile Case of Hinman Syndrome with Severe Acute Renal Failure. Clin Exp Nephrol 2008;12:145–9. [CrossRef]
- Gampala S, Alkukhun L, Khan Z, al. et. Hinman Syndrome: A Rare Entity with Neurogenic Bladder-Like Symptoms. Cureus 2024;16:e55684. [CrossRef]
- Hoebeke P, Van Laecke E, al. et. Non-neurogenic Neurogenic Bladder: Clinical Spectrum and Treatment. Pediatric Nephrology 2010;25:813–24. [CrossRef]
- Wan KS, Yang CC. Psychogenic Urinary Retention in Children: A Case Report. Pediatr Neonatol 2010;51:375–8. [CrossRef]
- Nerli R, Pujar S, Ghagane S, Hiremath M, Dixit N. Persistence and appearance of vesicoureteral reflux/obstruction following open reimplantation for vesicoureteral reflux. Journal of the Scientific Society 2019;46:90. [CrossRef]
- Capozza N, Lais A, Matarazzo E, Nappo S, Patricolo M, Caione P. Influence of Voiding Dysfunction on the Outcome of Endoscopic Treatment for Vesicoureteral Reflux. J Urol 2002;168:1695–8. [CrossRef]
- Sillén U. Bladder Dysfunction and Vesicoureteral Reflux. Adv Urol 2008;2008:1–8. [CrossRef]
- Chase J, Austin PF, Hoebeke P, McKenna P. The management of dysfunctional voiding in children: A report from the International Children’s Continence Society. Journal of Urology 2010;183:1296–302. [CrossRef]
- Hoberman A, Keren R, of Philadel-phia H, Mathews R, Kropp BP, Nelson CP, et al. Antimicrobial Prophylaxis for Children with Vesicoureteral Reflux. New England Journal of Medicine 2014;370:2367–76. [CrossRef]
| Category | Criteria | Rationale / Notes |
| Inclusion Criteria | - Severe lower urinary tract dysfunction (LUTD) manifested by recurrent urinary retention, post-void residual (PVR) > 20 % of age-expected bladder capacity, or persistent daytime incontinence refractory to initial urotherapy. | Defines clinically significant LUTD requiring tertiary-level evaluation. |
| - Recurrent urinary tract infections (rUTIs): ≥ 2 febrile or ≥ 3 culture-proven infections within 12 months. | Ensures selection of children with significant morbidity related to LUTD. | |
| - No detectable neurological or structural abnormalities on comprehensive evaluation (clinical exam, imaging, and cystoscopy). | Confirms non-neurogenic, functional etiology. | |
| Exclusion Criteria | - Neurological disorders affecting bladder control (spinal dysraphism, myelomeningocele, tethered cord, cerebral palsy, peripheral neuropathies). | Eliminates neurogenic bladder causes. |
| - Structural urinary tract abnormalities (posterior urethral valves, urethral stricture, ectopic ureter, ureterocele, bladder diverticulum, high-grade VUR ≥ III). | Excludes anatomical obstruction or reflux-related dysfunction. | |
| - Prior lower urinary tract or reconstructive surgery (e.g., ureteral reimplantation, bladder augmentation, endoscopic bulking). | Avoids postoperative or iatrogenic LUTD confounders. | |
| - Systemic diseases influencing micturition (diabetes mellitus, chronic kidney disease, endocrine or metabolic disorders). | Removes systemic confounders. | |
| - Current or recent ( < 3 months ) use of medications affecting detrusor or sphincter function (anticholinergics, α-blockers, diuretics). | Prevents pharmacologic bias in urodynamic interpretation. |
| Characteristic | Case 1 | Case 2 | Case 3 |
| Age / Sex | 7 years / Male | 3 years / Female | 10 years / Male |
| Presenting Symptoms | Recurrent febrile UTIs, daytime incontinence, urgency, enuresis | Fever, pollakiuria, dysuria, incontinence | Acute urinary retention (recurrent episodes) |
| Prior History | Multiple UTIs over the preceding year | Persistent LUTS after treated UTI | Three prior ED visits for retention |
| Ultrasound Findings | Moderate bladder wall thickening; no residual urine | Left ureterohydronephrosis; crenulated bladder wall | Bladder wall thickened (7–8 mm), irregular contour, heterogeneous content |
| VCUG Findings | Crenulated bladder, no reflux, normal emptying | Grade V left VUR, dilated tortuous ureter, no voiding achieved | Large-capacity bladder, mild crenulation, grade I VUR, incomplete emptying |
| Renal Scintigraphy (DMSA) | – | Left kidney: small, irregular, cortical scarring; function 18.7% | – |
| Cystoscopy Findings | Deep trabeculations, pseudopolypoid mucosa, diverticula, dilated vessels | Marked trabeculation, cell-like and columnar mucosa, difficult ureteric visualization | Trabeculated, pseudodiverticular bladder mucosa, normal urethra |
| Urodynamic Pattern | Detrusor overactivity, reduced capacity, uninhibited contractions | Poor compliance, detrusor–sphincter dyssynergia, high PVR | Hypocontractile detrusor, weak flow (Qmax 4 mL/s), high PVR |
| Diagnosis | Severe functional LUTD | Hinman syndrome (non-neurogenic neurogenic bladder) | Functional LUTD with hypocontractile bladder |
| Treatment | Urotherapy, trospium chloride, CAP, biofeedback | CAP, trospium chloride, CIC, biofeedback | Tamsulosin (Omnic-Tocas), biofeedback |
| Outcome | Initial remission; recurrence after withdrawal, improved with retreatment | Gradual improvement; resolution of UTIs, stable bladder function | Gradual recovery; resolution of acute retention episodes |
| Study / Source | Age / Sex | Neurological Findings | Key Imaging / Cystoscopic Findings | Urodynamic Pattern | Management | Outcome / Remarks |
| Present Report – Case 1 | 7 y / M | Normal | Crenulated bladder, trabeculated mucosa, pseudopolypoid changes | Detrusor overactivity, small capacity, uninhibited contractions | Trospium chloride, CAP, biofeedback | Resolution of incontinence and UTIs; relapse after withdrawal, improved with retreatment |
| Present Report – Case 2 | 3 y / F | Normal | Grade V VUR, trabeculated pseudopolypoid mucosa, difficult ureteric visualization | Poor compliance, detrusor–sphincter dyssynergia, high PVR | CAP, trospium chloride, CIC, biofeedback | Gradual functional improvement; resolution of UTIs; diagnosed as Hinman syndrome |
| Present Report – Case 3 | 10 y / M | Normal | Large-capacity bladder, mild crenulation, trabeculated trigone | Hypocontractile detrusor, low Qmax (4 mL/s), high PVR | Tamsulosin (Omnic-Tocas), biofeedback | Slow but complete resolution of acute retention |
| Hinman & Bauman, 1973 (J Urol 109:727–732) | 6–15 y / Mixed | Normal | Trabeculated, thick-walled bladder; VUR common | Detrusor–sphincter dyssynergia; high pressures | Behavioral retraining, catheterization | Variable; some progressed to renal failure |
| Lee et al., 2007 (Korean J Urol 48:1058) | 5–17 y / 14 pts | Normal | Trabeculation, diverticula, VUR in 50% | Poor compliance; DSD | CIC ± anticholinergics | Improved bladder compliance; preserved renal function in most |
| Chaichanamongkol et al., 2008 (Clin Exp Nephrol 12:145) | 1.5 y / M | Normal | VUR, hydronephrosis | DSD; poor compliance | CIC, CAP | Recovery from renal failure; long-term follow-up stable |
| Gampala et al., 2024 (Cureus 16:e55684) | 14 y / M | Normal | Bilateral VUR, trabeculated bladder | DSD; incomplete voiding | Anticholinergic, CIC | Improved voiding and infection control |
| Jayanthi et al., 1997 (J Urol 158:1282) | <2 y / Mixed | Normal | Thickened bladder wall; reflux | DSD, poor compliance | CIC, behavioral therapy | Early infancy presentation; good outcome with early management |
| Psychogenic Urinary Retention (Wan et al., 2010) | 9 y / F | Normal | Normal bladder and urethra | Normal detrusor; voluntary retention | Psychological counseling | Complete recovery; illustrates differential |
| Common Misstep | Underlying Issue / Reason | Typical Consequence | Evidence-Based Alternative (ICCS & Current Guidelines) |
| Performing cystoscopic bulking injections for presumed VUR without functional assessment | Misinterpretation of rUTIs or hydronephrosis as anatomical reflux | Persistence or recurrence of UTIs and incontinence; unresolved high bladder pressures; possible upper tract deterioration | Comprehensive LUTD work-up first: uroflowmetry, post-void residual (PVR), and urodynamics; initiate urotherapy ± pharmacotherapy before considering anti-reflux surgery |
| Ureteral reimplantation in children with unrecognized dysfunctional voiding | Reflux secondary to bladder outlet dysfunction misdiagnosed as primary anatomical VUR | Postoperative persistence of reflux/incontinence; recurrent infections despite technically successful surgery | Treat functional outlet dysfunction (biofeedback, timed voiding, bowel management, antimuscarinics/α-blockers); reassess reflux after functional correction |
| Labeling incontinence or retention as behavioral without urodynamic confirmation | Lack of objective testing; underestimation of detrusor overactivity or underactivity | Delayed diagnosis; progression to hydronephrosis or renal scarring | Early non-invasive uroflow/PVR; cystometry when indicated; phenotype-guided therapy |
| Neglecting constipation or bowel dysfunction in LUTD management | Overlooking bladder–bowel interaction | Treatment failure; recurrent UTIs and incontinence | Integrated bowel regimen as part of standard urotherapy; dietary fiber, laxatives, timed toileting |
| Prolonged antibiotic prophylaxis without addressing voiding dysfunction | Treating infection consequence rather than the cause | Persistent bacteriuria and antimicrobial resistance | Functional evaluation and correction; prophylaxis only as temporary adjunct during therapy initiation |
| Proceeding to invasive or surgical intervention before multidisciplinary review | Fragmented care, absence of urodynamic input | Iatrogenic morbidity, continued symptoms | Multidisciplinary team evaluation (urology, nephrology, physiotherapy, psychology); individualized stepwise management |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




