Submitted:
07 October 2025
Posted:
08 October 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Data Sourcing
2.2. Procurement and Storage of Blood and Urine Samples
2.3. Quantification of Metals and Biomarkers of Kidney Effects
2.4. Normalization of ECd, Eβ2M and ENAG
2.5. Computation of eGFR, Fβ2M, TDβ2M and FrTDβ2M
2.6. Analysis for Cause-Effect Relationship
2.7. Statistical Analysis
3. Results
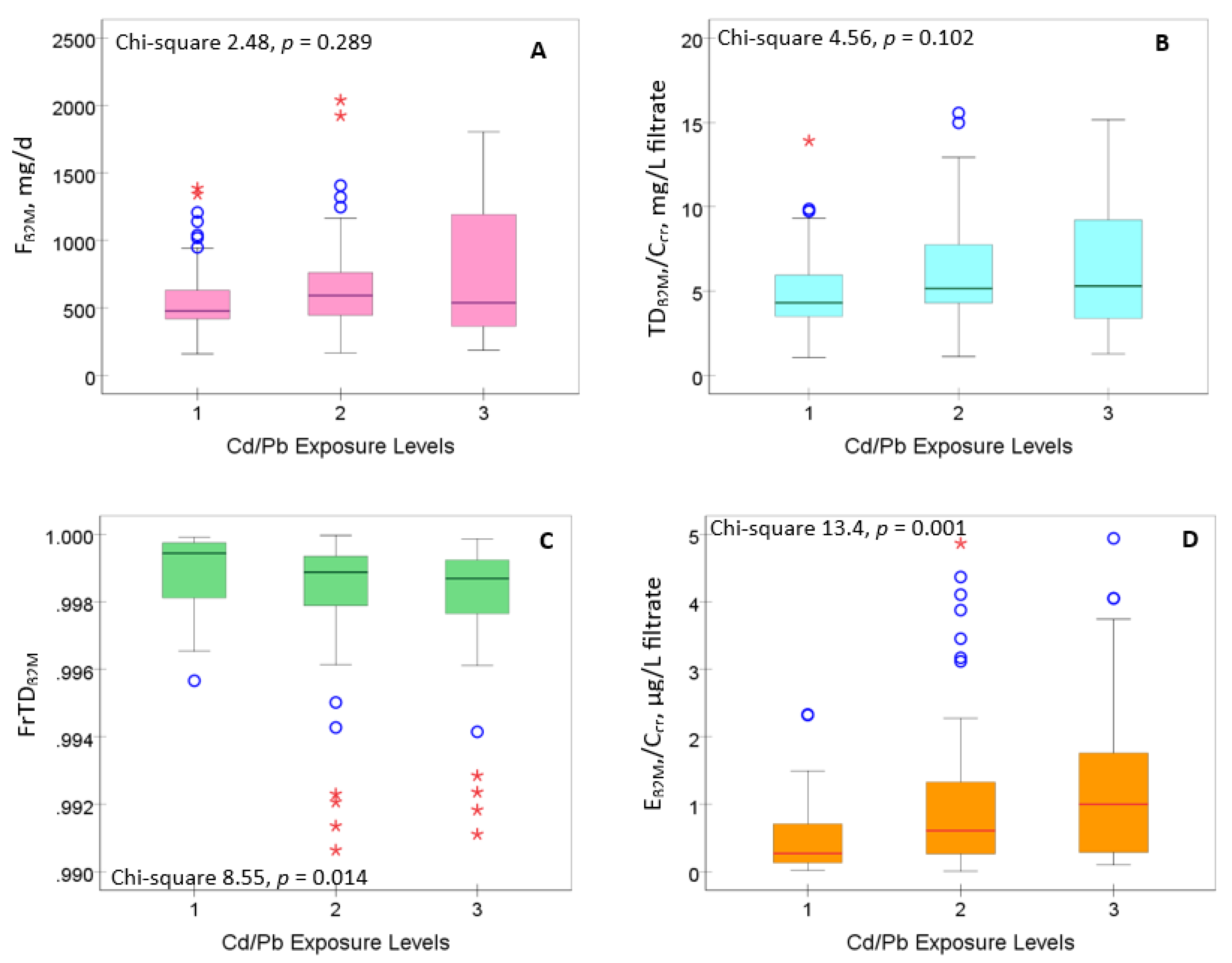
3.1. Cd/Pb Exposure Categorization
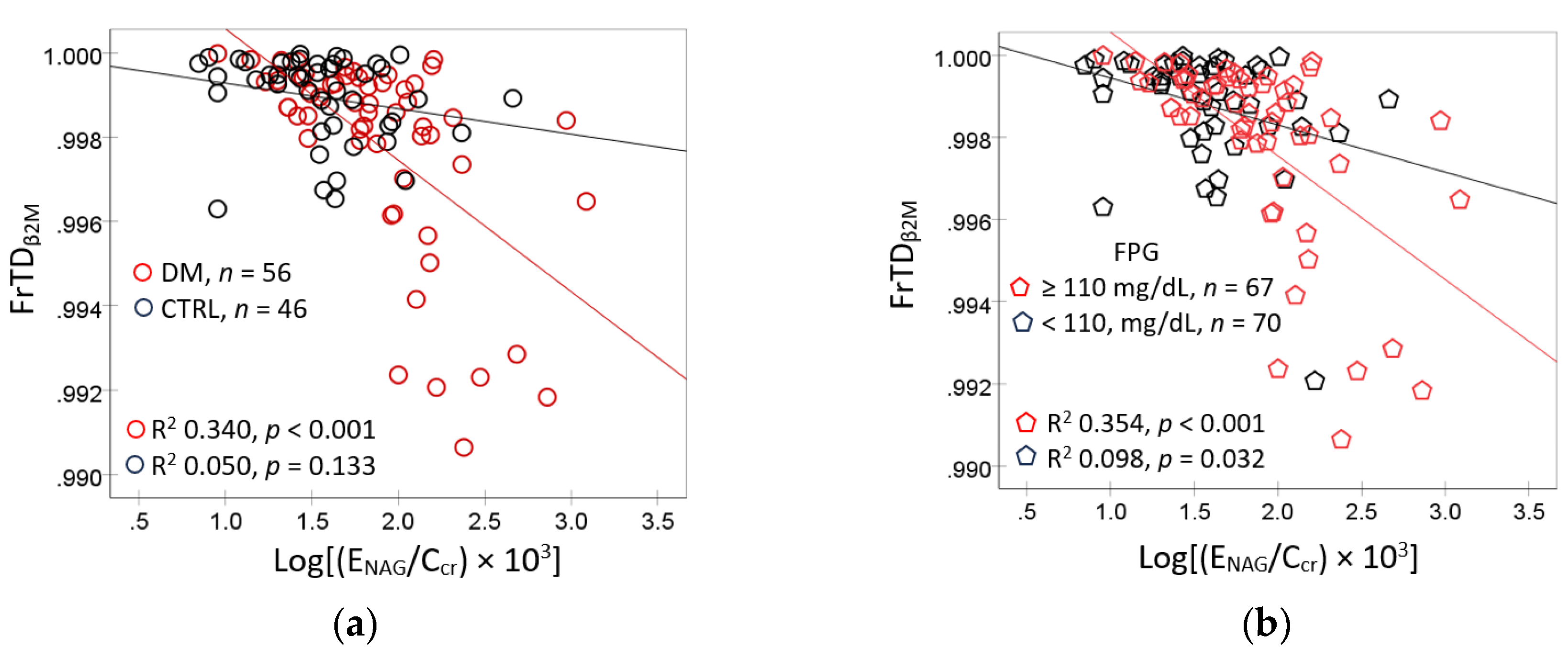
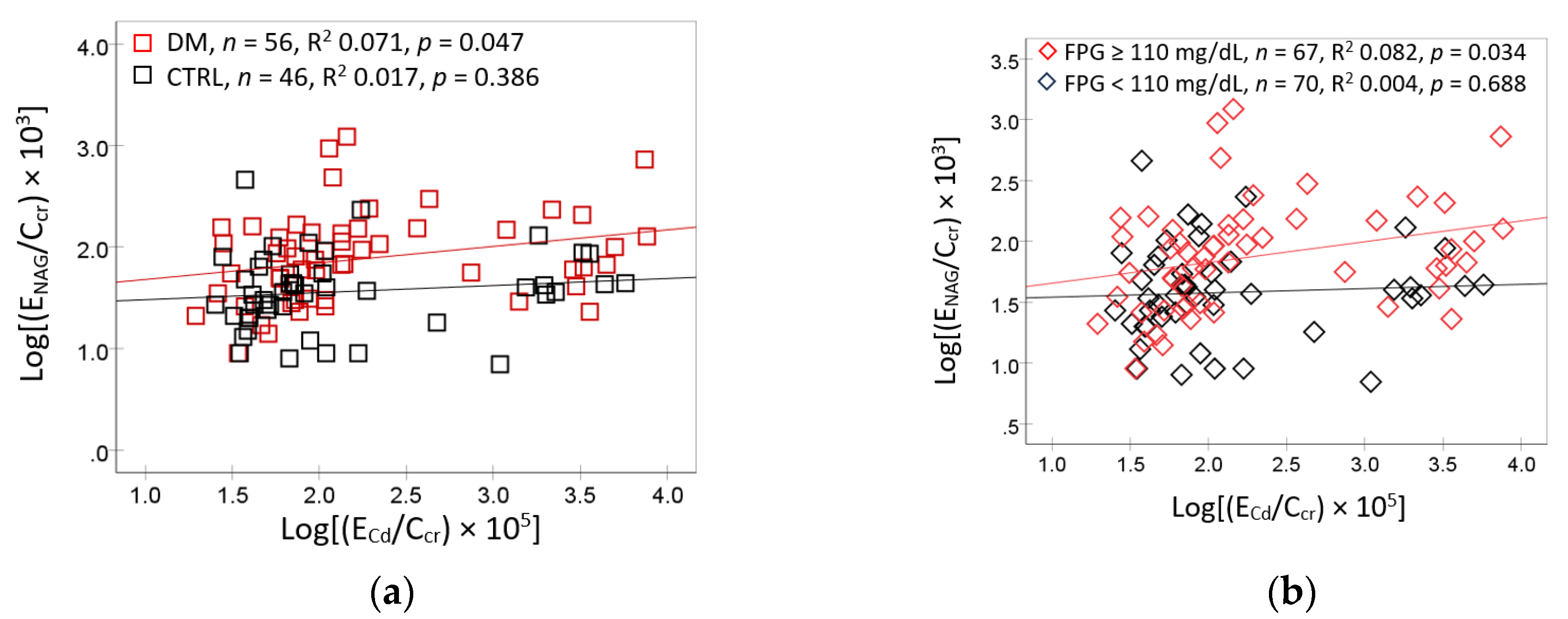
3.2. Cd/Pb Exposure and Kidney Handling of β2M
3.3. Multiple Linear Regression Models for FrTDβ2M in Diabetes vs. Controls
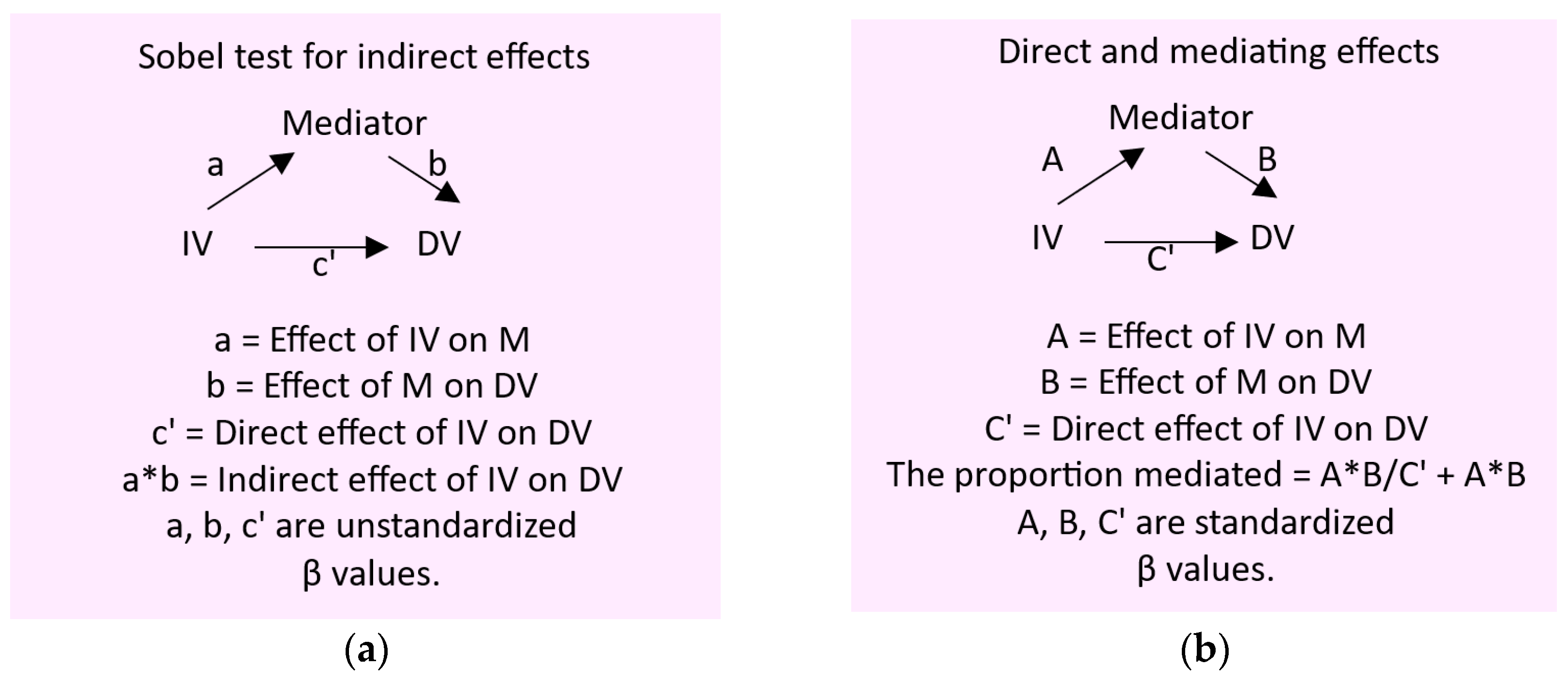
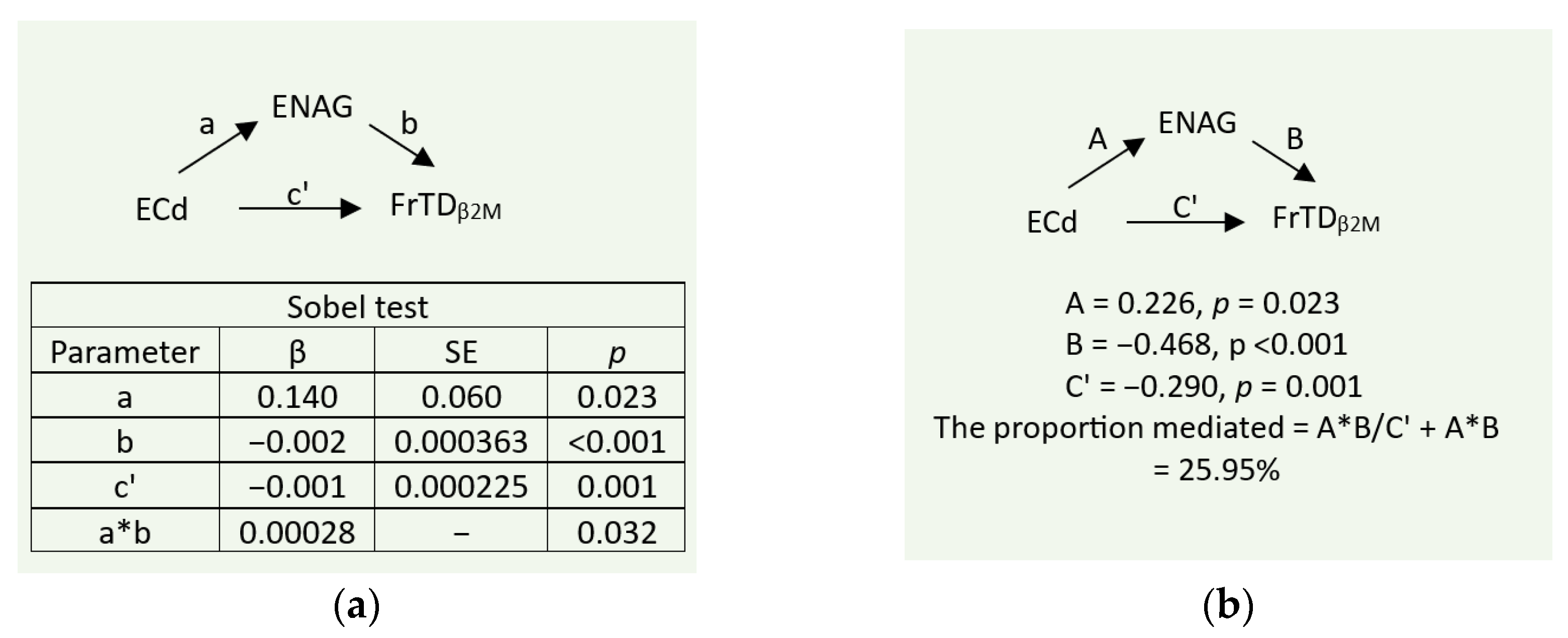
3.4. Mediation Analysis of Effects of Cd/Pb Exposure on FrTDβ2M
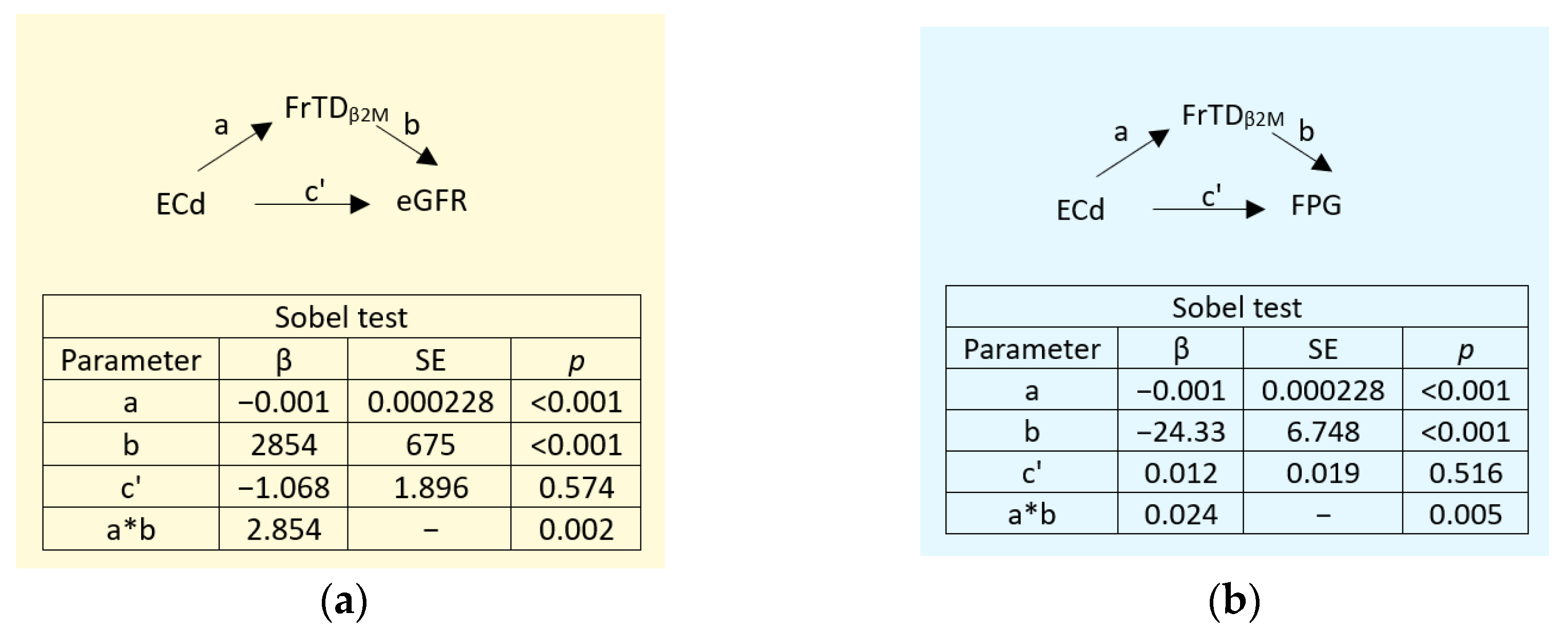
3.5. Mediation Analysis of Effects of Cd/Pb Exposure on eGFR and FPG
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| GFR | glomerular filtration rate |
| eGFR | estimated GFR |
| Cd | cadmium |
| ECd | urinary excretion rate of Cd |
| Pb | Lead |
| cr | creatinine |
| Ccr | Creatinine clearance |
| β2M | β2-microglobulin |
| Fβ2M | rate of glomerular filtration of β2M |
| Eβ2M | urinary excretion rate of β2M |
| TDβ2M | rate of tubular degradation of β2M |
| FrTDβ2M | fractional tubular degradation of filtered β2M |
References
- Guariguata, L.; Whiting, D.R.; Hambleton, I.; Beagley, J.; Linnenkamp, U.; Shaw, J.E. Global estimates of diabetes prevalence for 2013 and projections for 2035. Diabetes Res. Clin. Pract. 2014, 103, 137–149. [Google Scholar] [CrossRef]
- Zac-Varghese, S. Diabetes and the kidney. Clin. Med. (Lond) 2025, 100512. [Google Scholar] [CrossRef] [PubMed]
- Santulli, G. The 2025 AHA/ACC hypertension guidelines: implications for cardiovascular and renal risk in patients with diabetes. Cardiovasc. Diabetol. Endocrinol. Rep. 2025, 11, 21. [Google Scholar] [CrossRef] [PubMed]
- Semenikhina, M.; Mathew, R.O.; Barakat, M.; Van Beusecum, J.P.; Ilatovskaya, D.V.; Palygin, O. Blood Pressure Management Strategies and Podocyte Health. Am. J. Hypertens. 2025, 38, 85–96. [Google Scholar] [CrossRef] [PubMed]
- Haruhara, K.; Kanzaki, G.; Tsuboi, N. Nephrons, podocytes and chronic kidney disease: Strategic antihypertensive therapy for renoprotection. Hypertens. Res. 2023, 46, 299–310. [Google Scholar] [CrossRef]
- Ilatovskaya, D.V.; Behr, A.; Staruschenko, A.; Hall, G.; Palygin, O. Mechanistic Insights Into Redox Damage of the Podocyte in Hypertension. Hypertension 2025, 82, 14–25. [Google Scholar] [CrossRef]
- Murton, M.; Goff-Leggett, D.; Bobrowska, A.; Garcia Sanchez, J.J.; James, G.; Wittbrodt, E.; Nolan, S.; Sörstadius, E.; Pecoits-Filho, R.; Tuttle, K. Burden of Chronic Kidney Disease by KDIGO Categories of Glomerular Filtration Rate and Albuminuria: A Systematic Review. Adv. Ther. 2021, 38, 180–200. [Google Scholar] [CrossRef]
- Kalantar-Zadeh, K.; Jafar, T.H.; Nitsch, D.; Neuen, B.L.; Perkovic, V. Chronic kidney disease. Lancet 2021, 398, 786–802. [Google Scholar] [CrossRef] [PubMed]
- Farrell, D.R.; Vassalotti, J.A. Screening, identifying, and treating chronic kidney disease: Why, who, when, how, and what? BMC Nephrol. 2024, 25, 34. [Google Scholar] [CrossRef]
- Liu, D.; Lv, L.L. New Understanding on the Role of Proteinuria in Progression of Chronic Kidney Disease. Adv. Exp. Med. Biol. 2019, 1165, 487–500. [Google Scholar]
- Sharma, S.; Smyth, B. From Proteinuria to Fibrosis: An Update on Pathophysiology and Treatment Options. Kidney Blood Press. Res. 2021, 46, 411–420. [Google Scholar] [CrossRef]
- Makhammajanov, Z.; Gaipov, A.; Myngbay, A.; Bukasov, R.; Aljofan, M.; Kanbay, M. Tubular toxicity of proteinuria and the progression of chronic kidney disease. Nephrol. Dial. Transplant. 2024, 39, 589–599. [Google Scholar] [CrossRef] [PubMed]
- Faivre, A.; Verissimo, T.; de Seigneux, S. Proteinuria and tubular cells: Plasticity and toxicity. Acta Physiol. 2025, 241, e14263. [Google Scholar] [CrossRef] [PubMed]
- Hall, A.M. Protein handling in kidney tubules. Nat. Rev. Nephrol. 2025, 21, 241–252. [Google Scholar] [CrossRef] [PubMed]
- Hou, D.; Jia, X.; Wang, L.; McGrath, S.P.; Zhu, Y.G.; Hu, Q.; Zhao, F.J.; Bank, M.S.; O’Connor, D.; Nriagu, J. Global soil pollution by toxic metals threatens agriculture and human health. Science 2025, 388, 316–321. [Google Scholar] [CrossRef]
- Zhou, B.; Liao, Y.; Zheng, X.; Wang, Z.; Li, Q.; Chen, M. The effects of amendments on Cd and Pb under different fertilizer application conditions. Sci. Rep. 2025, 15, 5385. [Google Scholar] [CrossRef]
- Zhao, R.; Lin, S.; Han, M.; Lin, Z.; Yu, M.; Zhang, B.; Ma, L.; Li, D.; Peng, L. Association between machine learning-assisted heavy metal exposures and diabetic kidney disease: a cross-sectional survey and Mendelian randomization analysis. Front. Public Health 2024, 12, 1367061. [Google Scholar] [CrossRef]
- Wang, R.; Long, T.; He, J.; Xu. Y.; Wei, Y.; Zhang, Y.; He, X.; He, M. Associations of multiple plasma metals with chronic kidney disease in patients with diabetes. Ecotoxicol. Environ. Saf. 2022, 244, 14048.
- Hagedoorn, I.J.M.; Gant, C.M.; Huizen, S.V.; Maatman, R.G.H.J.; Navis, G.; Bakker, S.J.L.; Laverman, G.D. Lifestyle-Related Exposure to Cadmium and Lead is Associated with Diabetic Kidney Disease. J. Clin. Med. 2020, 9, 2432. [Google Scholar] [CrossRef]
- Choudhury, T.R.; Zaman, S.Z.; Chowdhury, T.I.; Begum, B.A.; Islam, M.A.; Rahman, M.M. Status of metals in serum and urine samples of chronic kidney disease patients in a rural area of Bangladesh: An observational study. Heliyon 2021, 7, e08382. [Google Scholar] [CrossRef]
- Cai, L.; Yan, J.; Sun, L.; Dan, W. The independent and combined effects of blood heavy metal concentrations on all-cause mortality and cardiovascular mortality in adult patients with diabetes mellitus. Front. Public Health 2025, 13, 1588078. [Google Scholar] [CrossRef]
- Zhao, H.; Yin, R.; Wang, Y.; Wang, Z.; Zhang, L.; Xu, Y.; Wang, D.; Wu, J.; Wei, L.; Yang, L.; et al. Association between blood heavy metals and diabetic kidney disease among type 2 diabetic patients: A cross-sectional study. Sci. Rep. 2024, 14, 26823. [Google Scholar] [CrossRef] [PubMed]
- Barregard, L.; Bergström, G.; Fagerberg, B. Cadmium, type 2 diabetes, and kidney damage in a cohort of middle-aged women. Environ. Res. 2014, 135, 311–316. [Google Scholar] [CrossRef] [PubMed]
- Oosterwijk, M.M.; Hagedoorn, I.J.M.; Maatman, R.G.H.J.; Bakker, S.J.L.; Navis, G.; Laverman, G.D. Cadmium, active smoking and renal function deterioration in patients with type 2 diabetes. Nephrol. Dial. Transplant. 2023, 38, 876–883. [Google Scholar] [CrossRef]
- Phelps, K. R.; Yimthiang, S.; Pouyfung, P.; Khamphaya, T.; Vesey, D. A.; Satarug, S. Homeostasis of β2-microglobulin in diabetics and non-diabetics with modest cadmium intoxication. J. Environ. Expo. Assess. 2025, 4, 23. [Google Scholar] [CrossRef]
- Yimthiang, S.; Pouyfung, P.; Khamphaya, T.; Kuraeiad, S.; Wongrith, P.; Vesey, D.A.; Gobe, G.C.; Satarug, S. Effects of Environmental Exposure to Cadmium and Lead on the Risks of Diabetes and Kidney Dysfunction. Int. J. Environ. Res. Public Health 2022, 19, 2259. [Google Scholar] [CrossRef]
- Zhang, Y.; Peng, G.; Leng, W.; Li, Y.; Li, H.; Zhou, L.; Ge, L.; Shao, J.; Li, X.; Long, M. Association between serum β2-microglobulin and left ventricular hypertrophy in patients with type 2 diabetes mellitus: A cross-sectional study. J. Diabetes 2024, 16, e13599. [Google Scholar] [CrossRef]
- Cheung, C.L.; Lam, K.S.; Cheung, B.M. Serum beta-2 microglobulin predicts mortality in people with diabetes. Eur. J. Endocrinol. 2013, 169, 1–7. [Google Scholar] [CrossRef]
- Kim, M.K.; Yun, K.J.; Chun, H.J.; Jang, E.H.; Han, K.D.; Park, Y.M.; Baek, K.H.; Song, K.H.; Cha, B.Y.; Park, C.S.; et al. Clinical utility of serum beta-2-microglobulin as a predictor of diabetic complications in patients with type 2 diabetes without renal impairment. Diabetes Metab. 2014, 40, 459–465. [Google Scholar] [CrossRef]
- Huan, T.; Meng, Q.; Saleh, M.A.; Norlander, A.E.; Joehanes, R.; Zhu, J.; Chen, B.H.; Zhang, B.; Johnson, A.D.; Ying, S.; et al. Integrative network analysis reveals molecular mechanisms of blood pressure regulation. Mol. Syst. Biol. 2015, 11, 799. [Google Scholar] [CrossRef]
- Keefe, J.A.; Hwang, S.J.; Huan, T.; Mendelson, M.; Yao, C.; Courchesne, P.; Saleh, M.A.; Madhur, M.S.; Levy, D. Evidence for a causal role of the SH2B3-β2M axis in blood pressure regulation. Hypertension 2019, 73, 497–503. [Google Scholar] [CrossRef] [PubMed]
- Pandey, K.N. Genetic and Epigenetic Mechanisms Regulating Blood Pressure and Kidney Dysfunction. Hypertension 2024, 81, 1424–1437. [Google Scholar] [CrossRef] [PubMed]
- Xu, R.; Tan, X.; Li, T.; Liu, S.; Li, Y.; Li, H. Norepinephrine-induced AuPd aerogels with peroxidase- and glucose oxidase-like activity for colorimetric determination of glucose. Mikrochim. Acta 2021, 188, 362. [Google Scholar] [CrossRef]
- Apple, F.; Bandt, C.; Prosch, A.; Erlandson, G.; Holmstrom, V.; Scholen, J.; Googins, M. Creatinine clearance: Enzymatic vs Jaffé determinations of creatinine in plasma and urine. Clin. Chem. 1986, 32, 388–390. [Google Scholar] [CrossRef] [PubMed]
- Trzcinka-Ochocka, M.; Brodzka, R.; Janasik, B. Useful and Fast Method for Blood Lead and Cadmium Determination Using ICP-MS and GF-AAS; Validation Parameters. J. Clin. Lab. Anal. 2016, 30, 130–139. [Google Scholar] [CrossRef]
- Hornung, R.W.; Reed, L.D. Estimation of average concentration in the presence of nondetectable values. Appl. Occup. Environ. Hyg. 1990, 5, 46–51. [Google Scholar] [CrossRef]
- Phelps, K.R.; Gosmanova, E.O. A generic method for analysis of plasma concentrations. Clin. Nephrol. 2020, 94, 43–49. [Google Scholar] [CrossRef] [PubMed]
- Grandjean, P.; Budtz-Jørgensen, E. Total imprecision of exposure biomarkers: Implications for calculating exposure limits. Am. J. Ind. Med. 2007, 50, 712–719. [Google Scholar] [CrossRef]
- Satarug, S.; Vesey, D. A.; Buha Đorđević, A. Use of Urinary β2-Microglobulin in the Assessment of the Health Risk from Environmental Cadmium Exposure. Preprints 2025, 2025092442. [Google Scholar] [CrossRef]
- Levey, A.S.; Becker, C.; Inker, L.A. Glomerular filtration rate and albuminuria for detection and staging of acute and chronic kidney disease in adults: A systematic review. JAMA 2015, 313, 837–846. [Google Scholar] [CrossRef]
- Preacher, K.J. Advances in mediation analysis: A survey and synthesis of new developments. Annu. Rev. Psychol. 2015, 66, 825–852. [Google Scholar] [CrossRef]
- MacKinnon, D.P.; Warsi, G.; Dwyer, J.H. A simulation study of mediated effect measures. Multiv. Behav. Res. 1995, 30, 41–62. [Google Scholar] [CrossRef]
- Preacher, K.J.; Hayes, A.F. SPSS and SAS procedures for estimating indirect effects in simple mediation models. Behav. Res. Meth. Instrum. Comput. 2004, 36, 717–731. [Google Scholar] [CrossRef] [PubMed]
- Little, B.B.; Reilly, R.; Walsh, B.; Vu, G.T. Cadmium is associated with type 2 diabetes in a Superfund Site Lead Smelter community in Dallas, Texas. Int. J. Environ. Res. Public Health 2020, 17, 4558. [Google Scholar] [CrossRef] [PubMed]
- Reilly, R.; Spalding, S.; Walsh, B.; Wainer, J.; Pickens, S.; Royster, M.; Villanacci, J.; Little, B.B. Chronic environmental and occupational lead exposure and kidney function among African Americans: Dallas Lead Project II. Int. J. Environ. Res. Public Health 2018, 15, 2875. [Google Scholar] [CrossRef]
- Son, H.S.; Kim, S.G.; Suh, B.S.; Park, D.U.; Kim, D.S.; Yu, S.D.; Hong, Y.S.; Park, J.D.; Lee, B.K.; Moon, J.D.; et al. Association of cadmium with diabetes in middle-aged residents of abandoned metal mines: The first health effect surveillance for residents in abandoned metal mines. Ann. Occup. Environ. Med. 2015, 27, 20. [Google Scholar] [CrossRef]
- Argyropoulos, C.P.; Chen, S.S.; Ng, Y.-H.; Roumelioti, M.-E.; Shaffi, K.; Singh, P.P.; Tzamaloukas, A.H. Rediscovering Beta-2 Microglobulin As a Biomarker across the Spectrum of Kidney Diseases. Front. Med. 2017, 4, 73. [Google Scholar] [CrossRef] [PubMed]
- Buchet, J.P.; Lauwerys, R.; Roels, H.; Bernard, A.; Bruaux, P.; Claeys, F.; Ducoffre, G.; de Plaen, P.; Staessen, J.; Amery, A.; et al. Renal effects of cadmium body burden of the general population. Lancet 1990, 336, 699–702. [Google Scholar] [CrossRef]
- Satarug, S.; Vesey, D. A.; Đorđević A., B. The NOAEL equivalent for the cumulative body burden of cadmium: focus on proteinuria as an endpoint. J. Environ. Expo. Assess. 2024, 3, 26. [Google Scholar] [CrossRef]
| Variables | All Subjects n = 137 |
Cd/Pb Exposure Levels | p | ||
|---|---|---|---|---|---|
| Level 1 n = 44 |
Level 2 n = 54 |
Level 3 n = 39 |
|||
| Women, % | 78.1 | 90.9 | 72.2 | 71.8 | 0.045 |
| Smoking, % | 10.2 | 0 | 9.3 | 23.1 | 0.002 |
| Diagnosed diabetes, % | 47.4 | 34.1 | 46.3 | 64.1 | 0.023 |
| Hypertension, % | 54.5 | 51.2 | 44.4 | 71.8 | 0.029 |
| Age (range), years | 59.7 (41−80) | 59.6 (42−80) | 59.8 (45−78) | 59.5 (41−78) | 0.994 |
| BMI, kg/m2 | 25.6 (4.8) | 25.6 (4.2) | 25.4 (4.0) | 25.9 (6.2) | 0.805 |
| FPG, mg/dL | 129 (61) | 115 (40) | 131 (73) | 143 (59) | 0.099 |
| FPG ≥ 110 mg/dL, % | 48.9 | 38.6 | 48.1 | 61.5 | 0.115 |
| FPG ≥ 126 mg/dL, % | 39.4 | 29.5 | 35.2 | 56.4 | 0.031 |
| eGFR, mL/min/1.73 m2 | 79 (16) | 81 (15) | 77 (16) | 80 (18) | 0.461 |
| a Low eGFR, % | 12.4 | 9.1 | 16.7 | 10.3 | 0.469 |
| [β2M]s, mg/L | 5.98 (3.29) | 5.01 (2.47) | 6.16 (3.12) | 6.83 (4.06) | 0.099 |
| [Pb]b, mg/dL | 4.49 (4.78) | 2.12 (0.00) | 4.65 (5.63) | 6.95 (5.00) | <0.001 |
| [Cd]b, µg/L | 0.57 (0.70) | 0.05 (0.05) | 0.60 (0.68) | 1.10 (0.73) | <0.001 |
| [Cd]u, µg/L | 0.65 (1.11) | 0.27 (0.69) | 0.59 (1.09) | 1.17 (1.33) | <0.001 |
| Ecr-normalized data | |||||
| ECd/Ecr, µg/g creatinine | 0.98 (1.86) | 0.33 (0.72) | 0.99 (2.06) | 1.70 (2.20) | 0.006 |
| Eβ2M/Ecr, µg/g creatinine | 108 (118) | 60 (58) | 116 (128) | 151 (136) | 0.002 |
| ENAG/Ecr, U/g creatinine | 10.6 (14.5) | 6.67 (4.93) | 11.6 (16.7) | 13.4 (17.6) | 0.288 |
| Ccr-normalized data | |||||
| ECd/Ccr, (µg/L filtrate) × 100 | 0.86 (1.68) | 0.28 (0.62) | 0.86 (1.78) | 1.50 (2.11) | 0.001 |
| Eβ2M/Ccr, (μg/L filtrate) × 100 | 99 (115) | 52 (56) | 108 (123) | 139 (134) | 0.001 |
| ENAG/Ccr, (U/L filtrate) × 100 | 10.2 (17.4) | 5.31 (4.03) | 10.6 (16.0) | 14.6 (24.5) | 0.154 |
| Variables | Spearman’s rank correlation coefficient | ||||||
|---|---|---|---|---|---|---|---|
| FrTDβ2M | Age | BMI | eGFR | FPG | ECd/Ccr | ENAG/Ccr | |
| Age | −0.096 | ||||||
| BMI | 0.048 | −0.262** | |||||
| eGFR | 0.434** | −0.356** | 0.161 | ||||
| FPG | −0.215* | −0.222** | 0.184* | 0.089 | |||
| ECd/Ccr | −0.527** | 0.078 | −0.083 | −0.227** | 0.166 | ||
| ENAG/Ccr | −0.536** | −0.115 | 0.002 | −0.467** | 0.278** | 0.328** | |
| Cd/Pb exposure a | −0.249** | 0.009 | −0.012 | −0.013 | 0.181* | 0.301** | 0.165 |
| Independent Variables |
FrTDβ2M | |||||
|---|---|---|---|---|---|---|
| All, n = 137 | Diabetes, n = 72 | Controls, n = 65 | ||||
| β | p | β | p | β | p | |
| Age, years | −0.009 | 0.913 | 0.095 | 0.483 | −0.079 | 0.513 |
| BMI, kg/m2 | 0.082 | 0.300 | 0.123 | 0.300 | 0.082 | 0.471 |
| eGFR, mL/min/1.73 m2 | 0.372 | <0.001 | 0.476 | <0.001 | 0.360 | 0.003 |
| (ECd/Ccr) ×100, µg/L filtrate | −0.189 | 0.013 | −0.295 | 0.009 | −0.102 | 0.383 |
| Diagnosed diabetes | −0.222 | 0.021 | − | − | − | − |
| Gender | 0.057 | 0.544 | 0.036 | 0.790 | 0.140 | 0.337 |
| Smoking | −0.016 | 0.866 | 0.021 | 0.877 | −0.085 | 0.559 |
| Hypertension | 0.052 | 0.492 | 0.172 | 0.113 | −0.239 | 0.053 |
| FPG, mg/dL | −0.258 | 0.007 | −0.220 | 0.055 | 0.247 | 0.033 |
| Adjusted R2 | 0.311 | <0.001 | 0.301 | <0.001 | 0.215 | 0.003 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




