Submitted:
28 August 2025
Posted:
29 August 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design and Participants
2.2. Radiographic Analysis
2.3. Disc Status
2.4. Statistical Analysis
3. Results
3.1. Demographic Data
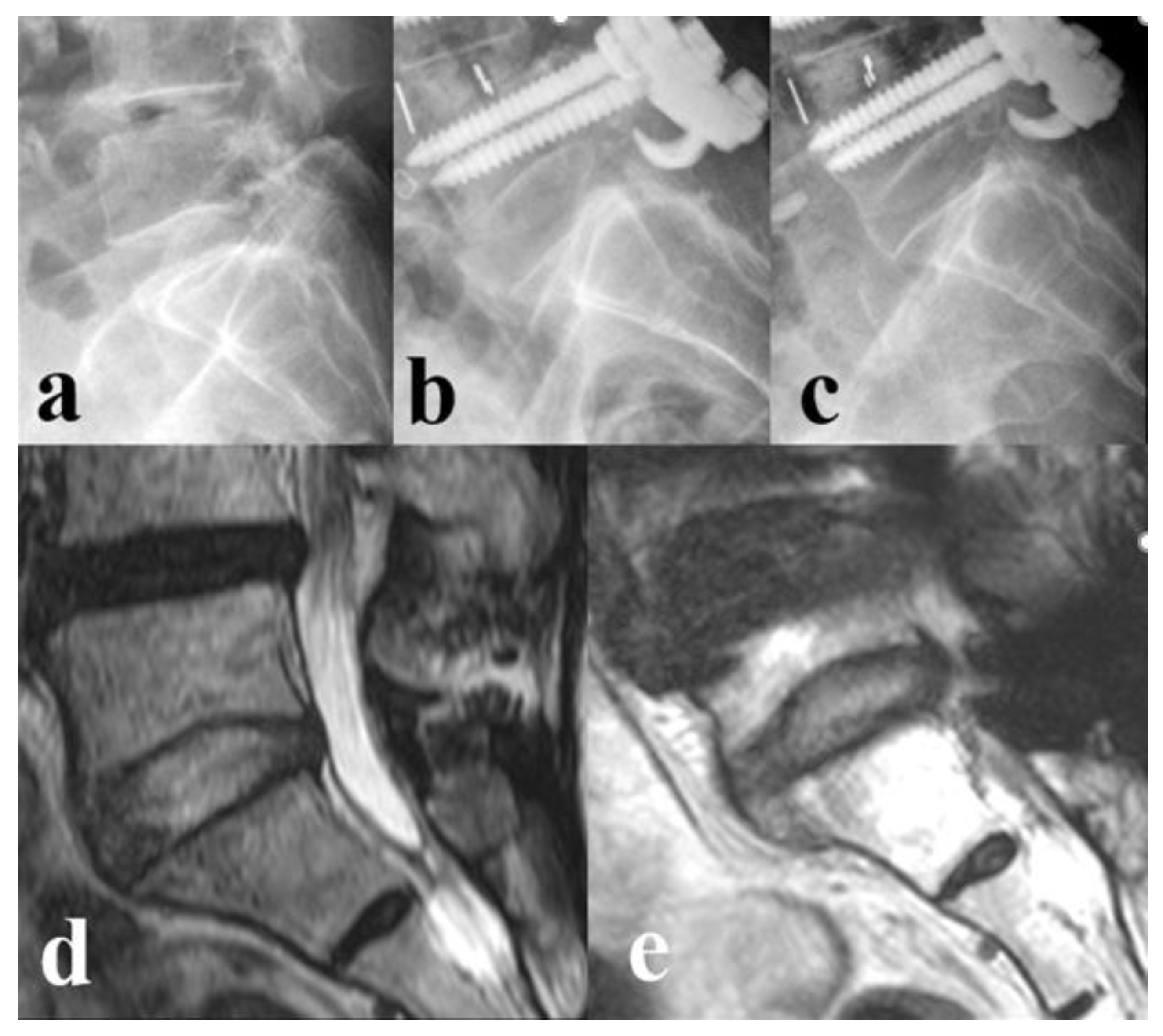
3.2. Disc Status
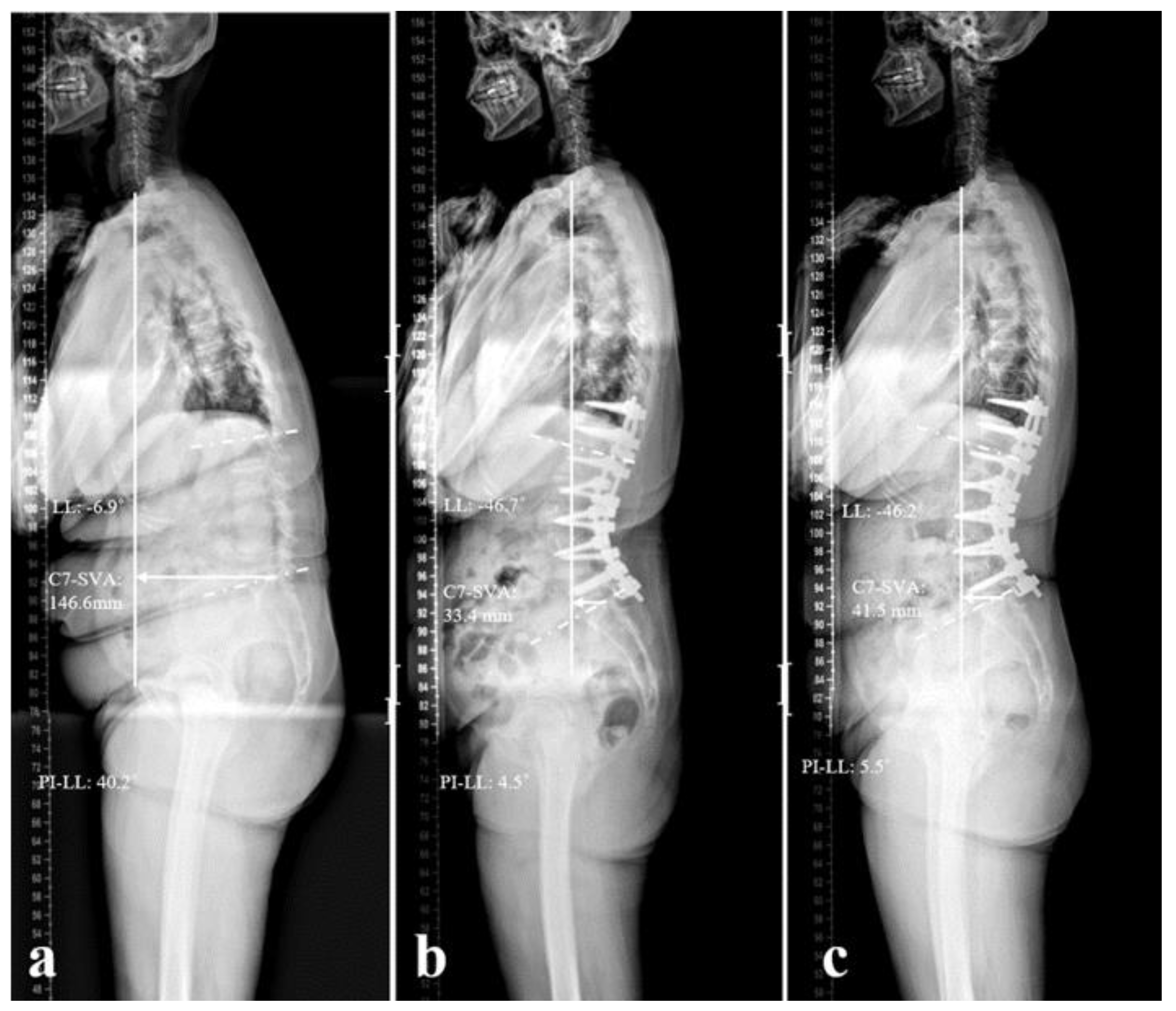
3.3. Sagittal Spinopelvic Parameters
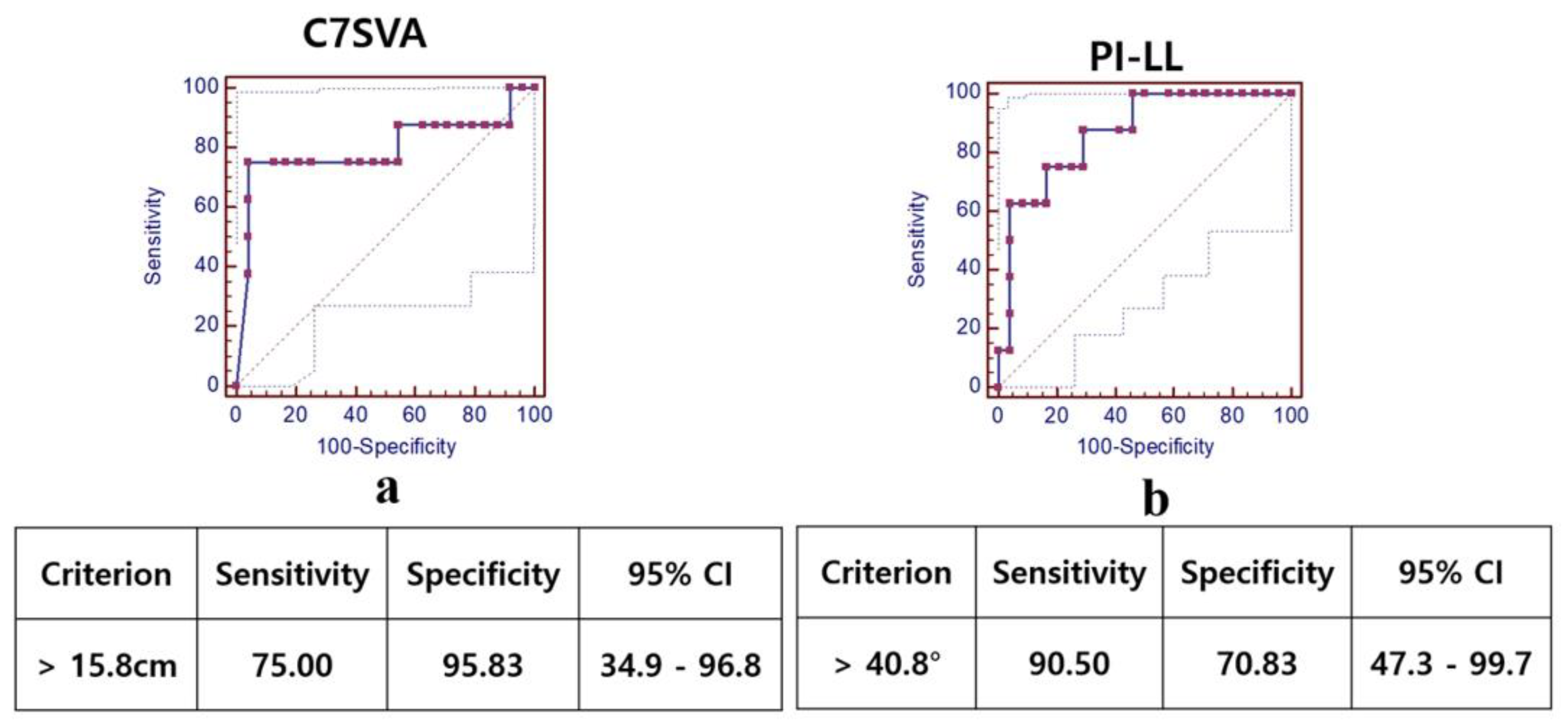
3.4. Subgroup Analysis
4. Discussion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
| DSI | Degenerative sagittal imbalance |
| C7SVA | C7 sagittal vertical axis |
| LL | Lumbar lordosis |
| PI | Pelvic incidence |
| BMI | Body mass index |
| TK | Thoracic kyphosis |
| TLK | Thoracolumbar kyphosis |
| PT | Pelvic tilt |
| SS | Sacral slope |
| ROC | Receiver operating characteristic |
References
- Edwards CC, 2nd, Bridwell KH, Patel A, Rinella AS, Berra A, Lenke LG: Long adult deformity fusions to L5 and the sacrum. A matched cohort analysis. Spine (Phila Pa 1976) 2004, 29(18):1996-2005.
- Taneichi H, Inami S, Moridaira H, Takeuchi D, Sorimachi T, Ueda H, Aoki H, Iimura T: Can we stop the long fusion at L5 for selected adult spinal deformity patients with less severe disability and less complex deformity? Clinical neurology and neurosurgery 2020, 194:105917.
- Margulies JY, Casar RS, Caruso SA, Neuwirth MG, Haher TR: The mechanical role of laminar hook protection of pedicle screws at the caudal end vertebra. Eur Spine J 1997, 6(4):245-248.
- Wilke HJ, Kaiser D, Volkheimer D, Hackenbroch C, Püschel K, Rauschmann M: A pedicle screw system and a lamina hook system provide similar primary and long-term stability: a biomechanical in vitro study with quasi-static and dynamic loading conditions. European spine journal : official publication of the European Spine Society, the European Spinal Deformity Society, and the European Section of the Cervical Spine Research Society 2016, 25(9):2919-2928.
- Hasegawa K, Takahashi HE, Uchiyama S, Hirano T, Hara T, Washio T, Sugiura T, Youkaichiya M, Ikeda M: An experimental study of a combination method using a pedicle screw and laminar hook for the osteoporotic spine. Spine 1997, 22(9):958-962; discussion 963.
- Pfirrmann CW, Metzdorf A, Zanetti M, Hodler J, Boos N: Magnetic resonance classification of lumbar intervertebral disc degeneration. Spine (Phila Pa 1976) 2001, 26(17):1873-1878.
- Cannizzaro D, Anania CD, De Robertis M, Pizzi A, Gionso M, Ballabio C, Ubezio MC, Frigerio GM, Battaglia M, Morenghi E et al: The lumbar adjacent-level syndrome: analysis of clinical, radiological, and surgical parameters in a large single-center series. J Neurosurg Spine 2023, 39(4):479-489.
- Leduc S, Mac-Thiong JM, Maurais G, Jodoin A: Posterior pedicle screw fixation with supplemental laminar hook fixation for the treatment of thoracolumbar burst fractures. Can J Surg 2008, 51(1):35-40.
- Lentz J, Mun F, Suresh K, Groves M, Sponseller PJJ: How and When to Use Hooks to Improve Deformity Correction. 2021, 3(4).
- Sun E, Alkalay R, Vader D, Snyder BD: Preventing distal pullout of posterior spine instrumentation in thoracic hyperkyphosis: a biomechanical analysis. Journal of spinal disorders & techniques 2009, 22(4):270-277.
- Salo S, Hurri H, Rikkonen T, Sund R, Kröger H, Sirola J: Association between severe lumbar disc degeneration and self-reported occupational physical loading. J Occup Health 2022, 64(1):e12316.
- de Jonge T, Dubousset JF, Illés T: Sagittal plane correction in idiopathic scoliosis. Spine 2002, 27(7):754-760.
- Okuda S, Nagamoto Y, Matsumoto T, Sugiura T, Takahashi Y, Iwasaki M: Adjacent Segment Disease After Single Segment Posterior Lumbar Interbody Fusion for Degenerative Spondylolisthesis: Minimum 10 Years Follow-up. Spine (Phila Pa 1976) 2018, 43(23):E1384-E1388.
- Yugue I, Okada S, Masuda M, Ueta T, Maeda T, Shiba K: Risk factors for adjacent segment pathology requiring additional surgery after single-level spinal fusion: impact of pre-existing spinal stenosis demonstrated by preoperative myelography. Eur Spine J 2016, 25(5):1542-1549.
- Cho KJ, Suk SI, Park SR, Kim JH, Choi SW, Yoon YH, Won MH: Arthrodesis to L5 versus S1 in long instrumentation and fusion for degenerative lumbar scoliosis. European spine journal : official publication of the European Spine Society, the European Spinal Deformity Society, and the European Section of the Cervical Spine Research Society 2009, 18(4):531-537.
- Kuhns CA, Bridwell KH, Lenke LG, Amor C, Lehman RA, Buchowski JM, Edwards C, 2nd, Christine B: Thoracolumbar deformity arthrodesis stopping at L5: fate of the L5-S1 disc, minimum 5-year follow-up. Spine (Phila Pa 1976) 2007, 32(24):2771-2776.
- Wang T, Ding W: Risk factors for adjacent segment degeneration after posterior lumbar fusion surgery in treatment for degenerative lumbar disorders: a meta-analysis. J Orthop Surg Res 2020, 15(1):582.
- Steinmetz B, and Benzel. In: Benzel’s Spine Surgery Elsevier Health Sciences. edn.; 2021.
- Jia F, Wang G, Liu X, Li T, Sun J: Comparison of long fusion terminating at L5 versus the sacrum in treating adult spinal deformity: a meta-analysis. Eur Spine J 2020, 29(1):24-35.
| Group I (hook+, n=64) |
Group II (hook-, n=48) |
p-value | |
|---|---|---|---|
| Age at surgery (years) | 73.5 ± 7.19 | 72.86 ± 6.20 | 0.128 |
| Sex (Female/Male) | 28: 4 | 20: 4 | 0.269 |
| BMI (kg/m²) | 25.05 ± 3.98 | 26.86 ± 4.67 | 0.114 |
| BMD (T-score) | -1.24 ± 1.14 | -1.03 ± 2.15 | 0.625 |
| UIV level (n, %) | 0.125 | ||
| T9 | 2 (3.1%) | 2 (4.2%) | |
| T10 | 12 (18.7%) | 6 (12.5%) | |
| T11 | 28 (43.8%) | 16 (33.3%) | |
| T12 | 22 (34.4%) | 24 (50%) | |
| Preoperative diagnosis (n, %) | 0.546 | ||
| Multi-seg. Spinal stenosis with sagittal imbalance |
50 (78.1%) | 36 (75%) | |
| Multiple-level fractures | 8 (12.5%) | 6 (12.5%) | |
| Iatrogenic flatback | 4 (6.3%) | 4 (8.3%) | |
| Post-traumatic kyphosis | 2 (3.1%) | 2 (4.2%) | |
| Pelvic incidence (n, %) | 0.411 | ||
| ≤ 45° | 10 (15.6%) | 8 (16.6%) | |
| > 45° but ≤ 60° | 30 (46.9%) | 20 (41.7%) | |
| > 60° | 24 (37.5%) | 20 (41.7%) |
| Group I (hook+, n=64) |
Group II (hook-, n=48) |
p-value | |
|---|---|---|---|
| Degeneration Grade of L5-S1 (n, %) | |||
| Preoperative | 1.000 | ||
| Pfirrmann grade 1, 2 or 3 (healthy) | 64 (100%) | 48 (100%) | |
| Pfirrmann grade 4 or 5 (degenerated) | 0 | 0 | |
| Follow-up at 2 years | <0.001* | ||
| Pfirrmann grade 1, 2 or 3 (healthy) | 50 (78.1%) | 12 (25.0%) | |
| Pfirrmann grade 4 or 5 (degenerated) | 14 (21.9%) | 36 (75.0%) |
| Parameter | Group I (hook+, n=64) |
Group II (hook-, n=48) |
p-value | |
|---|---|---|---|---|
| C7 SVA (mm) |
Preop. Immed. postop. 2 years postop. |
174.6 ± 45.5 38.1 ± 45.3 49.4 ± 33.8 |
52.9 ± 65.1 23.8 ± 35.4 54.5 ± 64.3 |
0.011* 0.412 0.584 |
| Change | -136.2 ± 68.6 | -29.3 ± 75.8 | 0.018* | |
| TK (°) | Preop. Immed. postop. 2 years postop. |
13.8 ± 14.5 24.8 ± 11.7 26.7 ± 10.8 |
8.2 ± 18.5 23.3 ± 14.6 27.9 ± 16.3 |
0.333 0.611 0.584 |
| Change | 10.9 ± 9.5 | 15.1 ± 14.4 | 0.219 | |
| TLK (°) | Preop. Immed. postop. 2 years postop. |
16.9 ± 16.2 2.6 ± 10.4 7.4 ± 12.1 |
12.5. ± 14.2 0.7 ± 5.7 5.3 ± 6.6 |
0.398 0.454 0.433 |
| Change | -14.3 ± 14.9 | -16.2 ± 15.5 | 0.414 | |
| LL (°) | Preop. Immed. postop. 2 years postop. |
-11.6 ± 19.3 -52.1 ± 10.3 -46.9 ± 11.2 |
-22.8 ± 23.6 -48.2 ± 17.7 -43.3 ± 20.9 |
0.029* 0.299 0.322 |
| Change | -40.5 ± 15.4 | -25.4 ± 21.3 | 0.021* | |
| PT (°) | Preop. Immed. postop. 2 years postop. |
26.8 ± 8.6 18.6 ± 7.9 22.6 ± 8.1 |
24.4 ± 9.7 18.1 ± 9.9 21.4 ± 9.2 |
0.428 0.644 0.521 |
| Change | -8.2 ± 7.8 | -6.3 ± 4.8 | 0.447 | |
| SS (°) | Preop. Immed. postop. 2 years postop. |
26.5 ± 10.2 38.2 ± 9.3 34.1 ± 8.1 |
29.1 ± 7.9 34.7 ± 7.6 31.2 ± 7.2 |
0.341 0.331 0.421 |
| Change | 7.6 ± 7.9 | 5.6 ± 5.7 | 0.457 | |
| PI-LL (°) | Preop. Immed. postop. 2 years postop. |
44.4 ± 17.5 3.9 ± 9.3 -10.51 ± 5.5 |
29.1 ± 21.2 4.3 ± 6.6 -15.42 ± 9.72 |
0.041* 0.551 0.551 |
| Change | -40.5 ± 15.3 | -24.8 ± 21.4 | 0.034* |
| Group A (preserved, n=50) |
Group B (exacerbated, n=14) |
p-value | |
|---|---|---|---|
| Age at surgery (years) | 72.86 ± 6.43 | 74.13 ± 8.28 | 0.187 |
| Gender (Female/Male) | 22: 3 | 6: 1 | 0.245 |
| BMI (kg/m²) | 24.11 ± 3.52 | 27.94 ± 4.39 | 0.038* |
| BMD (T-score) | -1.25 ± 3.52 | -1.26 ± 1.20 | 0.523 |
| Preoperative diagnosis (n, %) | 0.312 | ||
| Multi-seg. Spinal stenosis with sagittal imbalance |
40(80.0%) | 12(85.7%) | |
| Multiple-level fractures | 6(12.0%) | 2(14.3%) | |
| Iatrogenic flatback | 2(4.0%) | 0 | |
| Post-traumatic kyphosis | 2(4.0%) | 0 | |
| Preop. L5-S1 Deg. grade (n, %) | 0.891 | ||
| Pfirrmann grade 1, 2, or 3 | 50(100%) | 14(100%) | |
| Pfirrmann grade 4 or 5 | 0 | 0 |
| Parameter | Group A (preserved disc) |
Group B (exacerbated disc) |
p-value | |
|---|---|---|---|---|
| C7 SVA (mm) | Preop. Immed. postop. |
158.9 ± 94.1 34.7 ± 36.1 |
205.8 ± 109.4 45.8 ± 60.1 |
0.026* 0.312 |
| Change | -124.2 ± 85.7 | -160.0 ± 77.8 | 0.037* | |
| TK (°) | Preop. Immed. postop. |
12.1 ± 9.9 19.6 ± 8.2 |
14.7 ± 16.5 27.4 ± 12.5 |
0.511 0.227 |
| Change | 7.5 ± 8.1 | 12.7 ± 10.8 | 0.331 | |
| TLK (°) | Preop. Immed. postop. |
14.5 ± 22.4 1.4 ± 10.3 |
18.7 ± 15.3 4.1 ± 10.9 |
0.317 0.385 |
| Change | -13.1 ± 10.8 | -14.6 ± 9.8 | 0.554 | |
| LL (°) | Preop. Immed. postop. |
-15.1 ± 16.9 -53.9 ± 10.8 |
-8.8 ± 23.1 -48.5 ± 8.8 |
0.167 0.221 |
| Change | -38.8 ± 22.7 | -39.7 ± 22.7 | 0.548 | |
| PT (°) | Preop. Immed. postop. |
28.1 ± 8.5 18.3 ± 8.4 |
26.9 ± 9.1 19.3 ± 7.5 |
0.531 0.544 |
| Change | -10.8 ± 11.4 | -7.6 ± 7.4 | 0.362 | |
| SS (°) | Preop. Immed. postop. |
25.4 ± 10.9 37.6 ± 8.1 |
27.4 ± 9.1 36.4 ± 11.9 |
0.487 0.514 |
| Change | 12.2 ± 7.9 | 9.1 ± 10.8 | 0.365 | |
| PI-LL (°) | Preop. Immed. postop. |
40.7 ± 18.1 2.2 ± 10.5 |
51.9 ± 14.4 7.5 ± 8.1 |
0.039* 0.287 |
| Change | -38.5 ± 12.8 | -44.4 ± 10.8 | 0.044* |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




