Submitted:
27 August 2025
Posted:
29 August 2025
You are already at the latest version
Abstract
Objectives: To investigate the clinical effect and safety of large-channel endoscopic unilateral laminotomy decompression for the treatment of multilevel cervical canal stenosis. Methods: A retrospective study was conducted on 36 Cervical spinal stenosis patients who underwent surgical treatment between January 2020–December 2023.Patients were divided into two groups according to the surgical method: endoscopic group(n=16) and open group(n=20).Perioperative Basic parameters were record and Clinical efficacy were systematically assessed using validated metrics: Visual Analog Scale , Japanese Orthopaedic Association score and Neck Disability Index. Radiographical parameters(C2–C7 Cobb angle, T1 slope, pavlov ratio) are used to assess the decompression effect and stability of cervical spine. Results: The endoscopic group demonstrated significant advantages over the open group in operative time , incision length , blood loss, and hospitalization duration . Both groups showed significant postoperative improvements in VAS, JOA, and NDI scores compared to preoperative baselines (P<0.05). At 1 month postoperatively, the endoscopic group exhibited superior VAS scores to the open group (2.69 ± 0.79 vs. 4.4 ± 0.88, P<0.05). Radiographic outcomes at final follow-up revealed significantly better cervical Cobb angle (13.57 ± 2.29° vs. 16.34 ± 2.95°, P<0.05) and T1 slope (22.62 ± 1.51° vs. 25.24 ± 2.41°, P<0.05) in the endoscopic group. Conversely, the open group demonstrated greater postoperative spinal canal area and Pavlov ratio (P<0.05). Conclusions: The large-channel endoscopic unilateral laminotomy decompression demonstrates satisfactory short-term efficacy in treating multilevel Cervical Spinal Stenosis. This technique offers significant advantages including reduced surgical trauma, accelerated recovery, enhanced postoperative cervical stability and higher patient satisfaction.
Keywords:
1. Introduction
2. Materials and Methods
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
| VAS | Visual Analog Scale |
| JOA | Japanese Orthopaedic Association score |
| NDI | Neck Disability Index |
| BMI | Body mass index |
References
- Theodore, N. Degenerative Cervical Spondylosis. N Engl J Med 2020, 383, 159–168. [Google Scholar] [CrossRef] [PubMed]
- Matsumoto, M.; Okada, E.; et al. Modic changes in the cervical spine: prospective 10-year follow-up study in asymptomatic subjects. J Bone Joint Surg Br 2012, 94, 678–683. [Google Scholar] [CrossRef] [PubMed]
- Hansson, T.; Suzuki, N.; et al. The narrowing of the lumbar spinal canal during loaded MRI: the effects of the disc and ligamentum flavum. European spine journal 2009, 18, 679–686. [Google Scholar] [CrossRef] [PubMed]
- Hoti, Y.U.D.; Aziz, A.; et al. Clinical Outcome of Laminoplasty in Cervical Myelopathy. Journal of the College of Physicians and Surgeons--Pakistan : JCPSP 2018, 28, 466–469. [Google Scholar] [CrossRef] [PubMed]
- Lv Y, Tian W, et al. The prevalence and associated factors of symptomatic cervical Spondylosis in Chinese adults: a community-based cross-sectional study. BMC musculoskeletal disorders 2018,19(1),325.
- Wang, L.; Liu, S.Y.; et al. Comparative study of Kurokawa's double door laminoplasty and modified Kurokawa's double door laminoplasty for the treatment of cervical disorders. Zhonghua Wai Ke Za Zhi 2013, 51, 508–512. [Google Scholar] [PubMed]
- Hirabayashi, K.; Watanabe, K.; et al. Expansive open-door laminoplasty for cervical spinal stenotic myelopathy. Spine (Phila Pa 1976) 1983, 8, 693–699. [Google Scholar] [CrossRef] [PubMed]
- Miyazaki, K.; Kirita, Y. Extensive simultaneous multisegment laminectomy for myelopathy due to the ossification of the posterior longitudinal ligament in the cervical region. Spine (Phila Pa 1976) 1986, 11, 531–542. [Google Scholar] [CrossRef] [PubMed]
- Lin CR, Tsai SHL, et al. What is the best strategy for C3 in open-door laminoplasty: laminectomy versus laminoplasty-a systematic review and meta-analysis. Spine J 2025,25(7),1440-54.
- Wu PF, Li YW, et al. Posterior Cervical Foraminotomy Via Full-Endoscopic Versus Microendoscopic Approach for Radiculopathy: A Systematic Review and Meta-analysis. Pain Physician 2019,22(1),41-52.
- Song, C.; Wei, Z.; et al. Clinical study of posterior percutaneous large channel full-endoscopic cervical laminectomy and decompression in the treatment of single-segment cervical spondylotic myelopathy. Chinese Journal of Anatomy and Clinics 2021, 26, 61–67. [Google Scholar]
- Han, S.; Zeng, X.; et al. Clinical Application of Large Channel Endoscopic Systems with Full Endoscopic Visualization Technique in Lumbar Central Spinal Stenosis: A Retrospective Cohort Study. Pain Ther 2022, 11, 1309–1326. [Google Scholar] [CrossRef] [PubMed]
- Siepe CJ, Bridts AL, et al. Full-endoscopic bilateral over-the-top decompression in lumbar central stenosis: surgical technique and outcomes. European spine journal : official publication of the European Spine Society, the European Spinal Deformity Society, and the European Section of the Cervical Spine Research Society 2023,32(8),2918-23.
- Huang, Y.H.; Lien, F.C.; et al. Full Endoscopic Uniportal Unilateral Laminotomy for Bilateral Decompression in Degenerative Lumbar Spinal Stenosis: Highlight of Ligamentum Flavum Detachment and Survey of Efficacy and Safety in 2 Years of Follow-up. World neurosurgery 2020, 134, e672–e681. [Google Scholar] [CrossRef] [PubMed]
- Hirabayashi, K.; Watanabe, K. A Review of My Invention of Expansive Laminoplasty. Neurospine 2019, 16, 379–382. [Google Scholar] [CrossRef] [PubMed]
- Vedantam A, Harinathan B, et al. Differences in spinal cord biomechanics after laminectomy, laminoplasty, and laminectomy with fusion for degenerative cervical myelopathy. J Neurosurg Spine 2023,39(1),28-39.
- Lin, Y.; Rao, S.; et al. Posterior Percutaneous Full-Endoscopic Cervical Laminectomy and Decompression for Cervical Stenosis with Myelopathy: A Technical Note. World neurosurgery 2019, 124, 350–357. [Google Scholar] [CrossRef] [PubMed]
- Carr DA, Abecassis IJ, et al. Full endoscopic unilateral laminotomy for bilateral decompression of the cervical spine: surgical technique and early experience. Journal of spine surgery (Hong Kong) 2020,6(2),447-56.
- xin FJ, Yi J, et al. Relationship between T1 slope angle and cervical curvature change after posterior cervical single open-door lamin-oplasty. Orthopedic Journal of China 2015,23(15),1360-4.
- Cho SK, Kim JS, et al. Cervical Laminoplasty: Indications, Surgical Considerations, and Clinical Outcomes. J Am Acad Orthop Surg 2018,26(7),e142-e52.
- Usami, Y.; Yokota, A.; et al. Morphology of cervical periradicular fibrous sheath and nerve roots in relation to postoperative C5 palsy. Spine J 2022, 22, 690–696. [Google Scholar] [CrossRef] [PubMed]
- Currier, B.L. Neurological complications of cervical spine surgery: C5 palsy and intraoperative monitoring. Spine (Phila Pa 1976) 2012, 37, E328–E334. [Google Scholar] [CrossRef] [PubMed]
- Thompson SE, Smith ZA, et al. C5 Palsy After Cervical Spine Surgery: A Multicenter Retrospective Review of 59 Cases. Global Spine J 2017,7(1 Suppl),64s-70s.
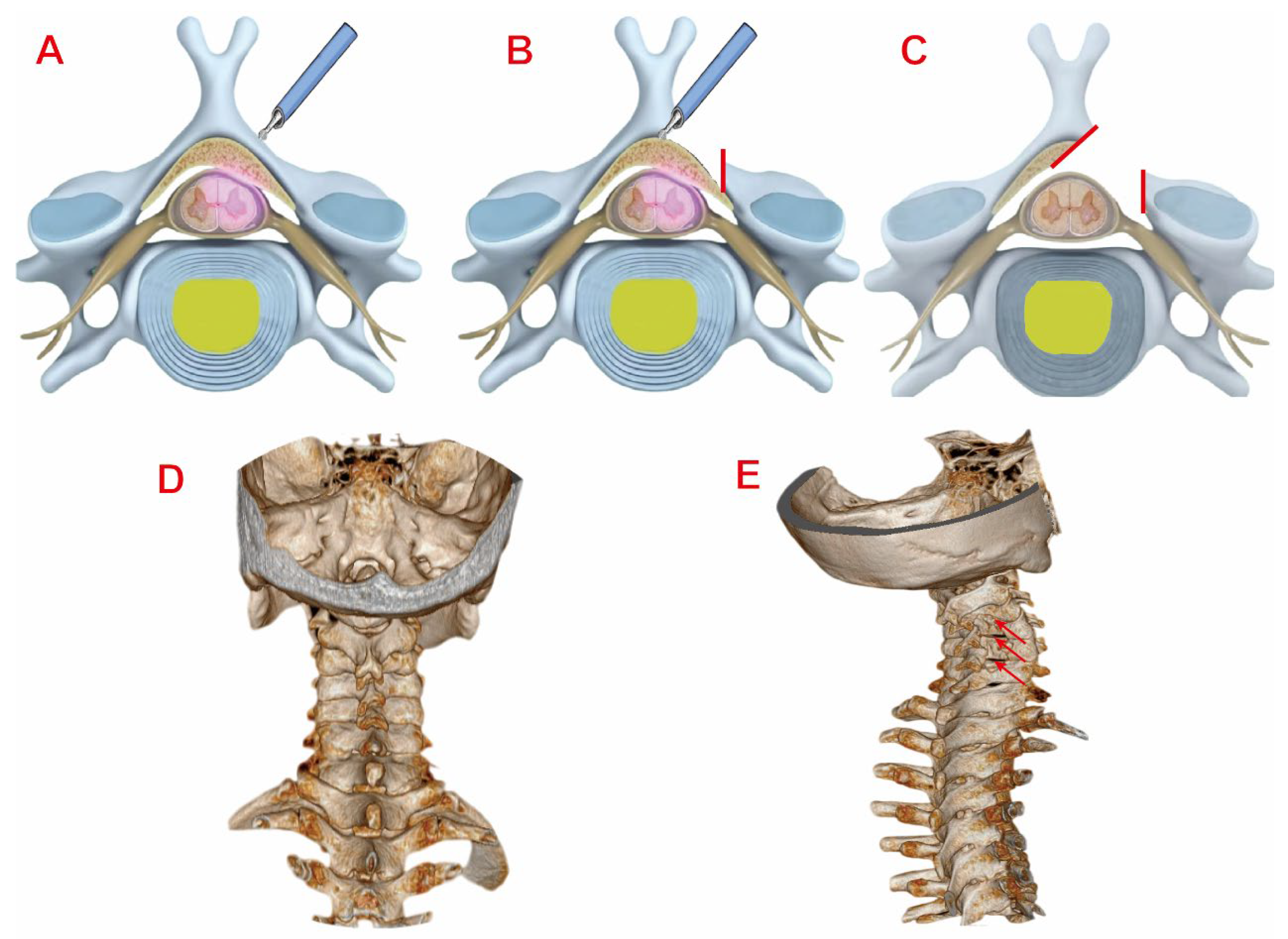
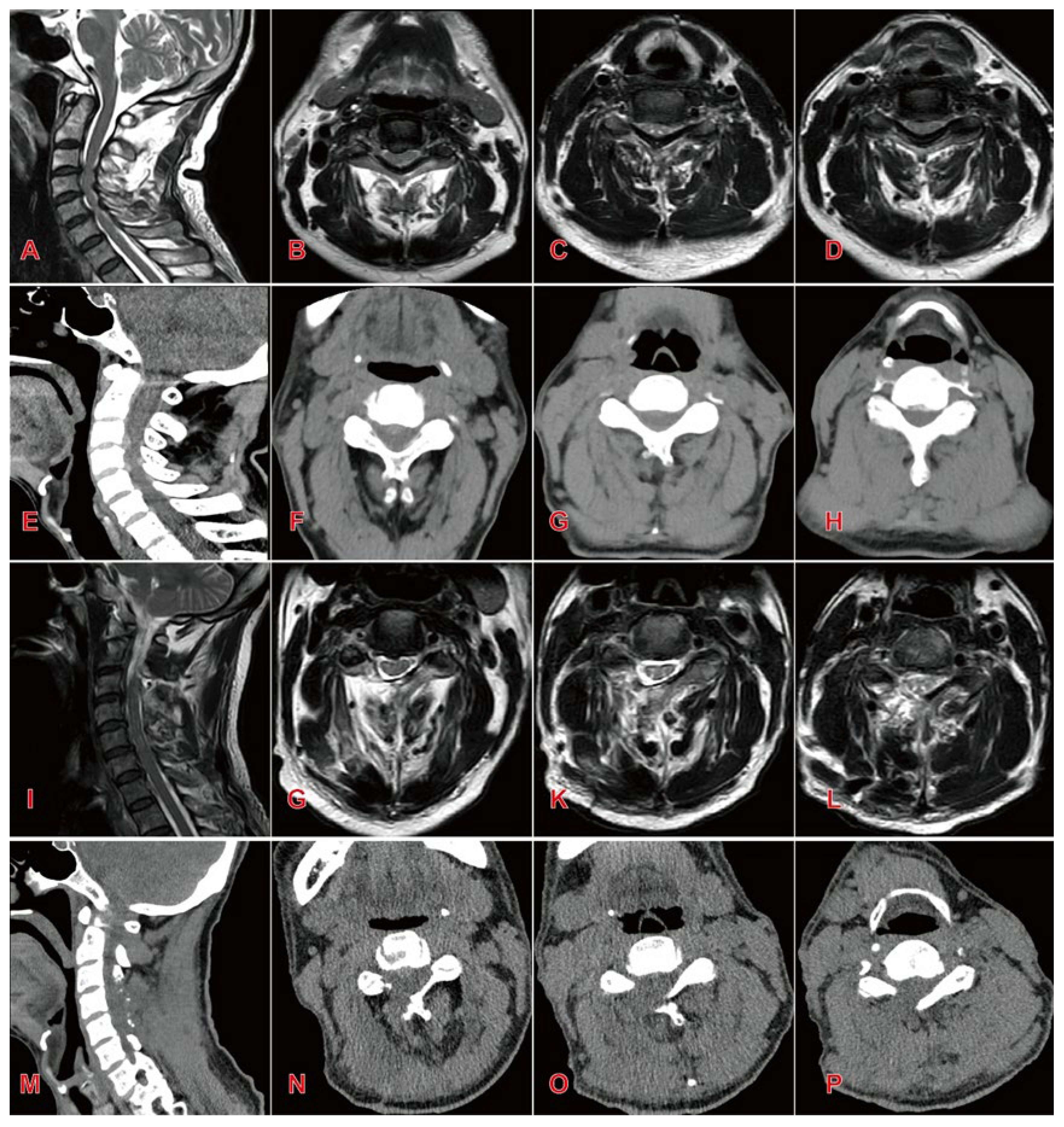
| Index | Endoscopic Group (n=16) | Open Group(n=20) | Statistic(t/χ²) | P value |
| Gender (Male/Female) |
10/6 | 11/9 | 0.206 | 0.650 |
| Age(years) | 57.7±9.2 | 60.5±10.2 | 0.859 | 0.397 |
| BMI (kg/m²) |
23.4±1.7 | 24.1±1.3 | 0.791 | 0.435 |
| Duration of illness(months) | 14.1±3.7 | 13.9±4.6 | 0.114 | 0.910 |
| Smoking (Yes/No) | 6/10 | 7/13 | 0.024 | 0.877 |
| Hypertension (Yes/No) | 7/9 | 11/9 | 0.450 | 0.502 |
| Diabetes (Yes/No) | 4/12 | 8/12 | 0.900 | 0.343 |
| Follow-up time (months) | 15.3±1.9 | 13.6±1.6 | 2.956 | 0.006 |
| Surgical times (h) |
1.6±0.6 | 2.1±0.2 | 3.333 | 0.002 |
| Incision length (cm) |
1.3±0.1 | 9.5±0.7 | 45.018 | 0.000 |
| Blood loss (ml) |
12.4±7.4 | 64.3±19.5 | 10.065 | 0.000 |
| Hospital stay (days) |
6.6±1.1 | 8.6±1.4 | 4.512 | 0.000 |
| Index | Endoscopic Group(n=16) | Open Group(n=20) | t value | P value |
| VAS score | ||||
| Preoperative | 7.25±0.86 | 7.05±1.15 | 0.58 | 0.57 |
| Postoperative 1 month |
2.69±0.79① | 4.4±0.88① | 6.05 | 0.00 |
| Postoperative 3 months |
1.75±0.45① | 2.3±0.80① | 1.21 | 0.27 |
| Postoperative 6 months |
1.38±0.50① | 1.75±0.64① | 1.92 | 0.06 |
| Postoperative 12months |
1.06±0.68① | 1.20±0.52① | 0.69 | 0.49 |
| Final follow-up | 0.56±0.63① | 0.80±0.52① | 1.24 | 0.22 |
| F value | 217.35 | 185.08 | ||
| P value | 0.00 | 0.00 | ||
| JOA score | ||||
| Preoperative | 6.69±1.35 | 6.9±1.55 | 0.43 | 0.67 |
| Postoperative 1 month |
13.31±1.14① | 13.15±1.60① | 0.34 | 0.73 |
| Postoperative 3 months |
15.00±0.82① | 14.80±1.74① | 0.42 | 0.67 |
| Postoperative 6 months |
15.19±0.66① | 15.45±1.05① | 0.87 | 0.39 |
| Postoperative 12 months |
15.56±0.89① | 15.95±0.69① | 1.47 | 0.15 |
| Final follow-up | 15.94±0.68① | 16.20±0.77① | 1.07 | 0.29 |
| F value | 216.07 | 147.03 | ||
| P value | 0.00 | 0.00 | ||
| JOA improvement rate at final follow-up (%) | 0.89±0.06 | 0.91±0.07 | 0.94 | 0.354 |
| NDI (%) | ||||
| Preoperative | 40.13±5.24 | 38.7±3.51 | 0.98 | 0.34 |
| Postoperative 1 month |
18.06±3.71① | 18.7±4.55① | 0.452 | 0.654 |
| Postoperative 3 months |
9.63±2.36① | 7.95±3.27① | 1.72 | 0.95 |
| Postoperative 6 months |
7.69±1.85① | 6.10±1.48① | 2.86 | 0.01 |
| Postoperative 12 months |
4.56±1.86① | 3.65±1.46① | 1.65 | 0.11 |
| Final follow-up | 2.56±1.41① | 2.55±1.19① | 0.03 | 0.97 |
| F value | 336.87 | 466.69 | ||
| P value | 0.00 | 0.00 |
| Index | Endoscopic Group (n=16) | Open Group (n=20) | t value | P value |
| Cervical C2–C7 Cobb angle (°) |
||||
| Preoperative | 16.78±3.32 | 16.64±3.07 | 0.14 | 0.89 |
| Postoperative | 16.71±3.43 | 16.16±2.9 | 0.52 | 0.61 |
| Final follow-up | 13.57±2.29① | 16.34±2.95 | 3.08 | 0.01 |
| F value | 5.73 | 0.13 | ||
| P value | 0.06 | 0.87 | ||
| T1 slope (°) | ||||
| Preoperative | 23.37±1.95 | 23.11±1.98 | 0.79 | 0.69 |
| Postoperative | 23.25±1.90 | 24.02±2.3 | 1.08 | 0.28 |
| Final follow-up | 22.62±1.51 | 25.24±2.41① | 5.95 | 0.00 |
| F value | 0.79 | 4.56 | ||
| P value | 0.45 | 0.01 | ||
| Note: ① P < 0.05, compared with pre-operation | ||||
| Index | Time Point | Endoscopic Group (n=16) | Open Group (n=20) | t value | P value |
| C3 Pavlov ratio | Preoperative | 0.62±0.08 | 0.69±0.08 | 1.83 | 0.08 |
| Postoperative | 0.85±0.10① | 0.95±0.06① | 2.97 | 0.007 | |
| Final follow-up | 0.84±0.05① | 0.93±0.07① | 3.27 | 0.003 | |
| F value | 14.91 | 89.61 | |||
| P value | 0.00 | 0.00 | |||
| C4 Pavlov ratio | Preoperative | 0.63±0.08 | 0.60±0.06 | 1.47 | 0.15 |
| Postoperative | 0.84±0.06① | 1.01±0.07① | 6.58 | 0.00 | |
| Final follow-up | 0.83±0.06① | 1.00±0.06① | 7.64 | 0.00 | |
| F value | 38.09 | 280.27 | |||
| P value | 0.00 | 0.00 | |||
| C5 Pavlov ratio | Preoperative | 0.65±0.08 | 0.68±0.11 | 1.09 | 0.28 |
| Postoperative | 0.85±0.06① | 1.01±0.09① | 6.50 | 0.00 | |
| Final follow-up | 0.86±0.05① | 0.99±0.09① | 4.99 | 0.00 | |
| F value | 62.27 | 69.84 | |||
| P value | 0.00 | 0.00 | |||
| C6 Pavlov ratio | Preoperative | 0.65±0.07 | 0.66±0.11 | 0.22 | 0.83 |
| Postoperative | 0.88±0.04① | 0.99±0.09① | 4.13 | 0.00 | |
| Final follow-up | 0.86±0.05① | 0.98±0.08① | 4.49 | 0.00 | |
| F value | 61.05 | 76.52 | |||
| P value | 0.00 | 0.00 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




