Submitted:
10 August 2025
Posted:
12 August 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Case Presentation
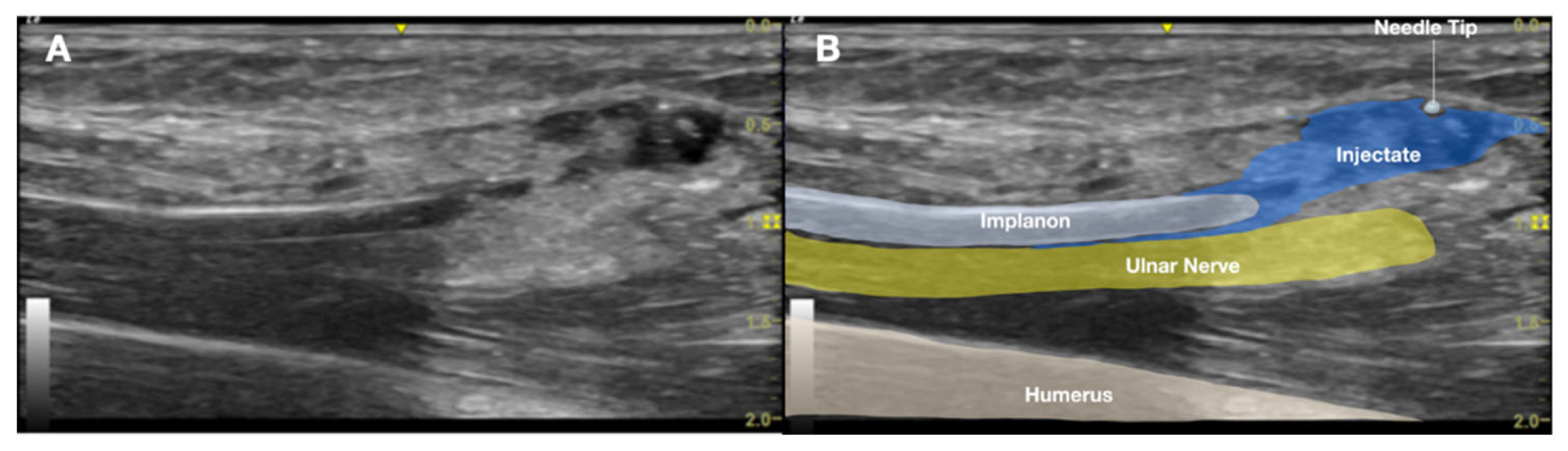
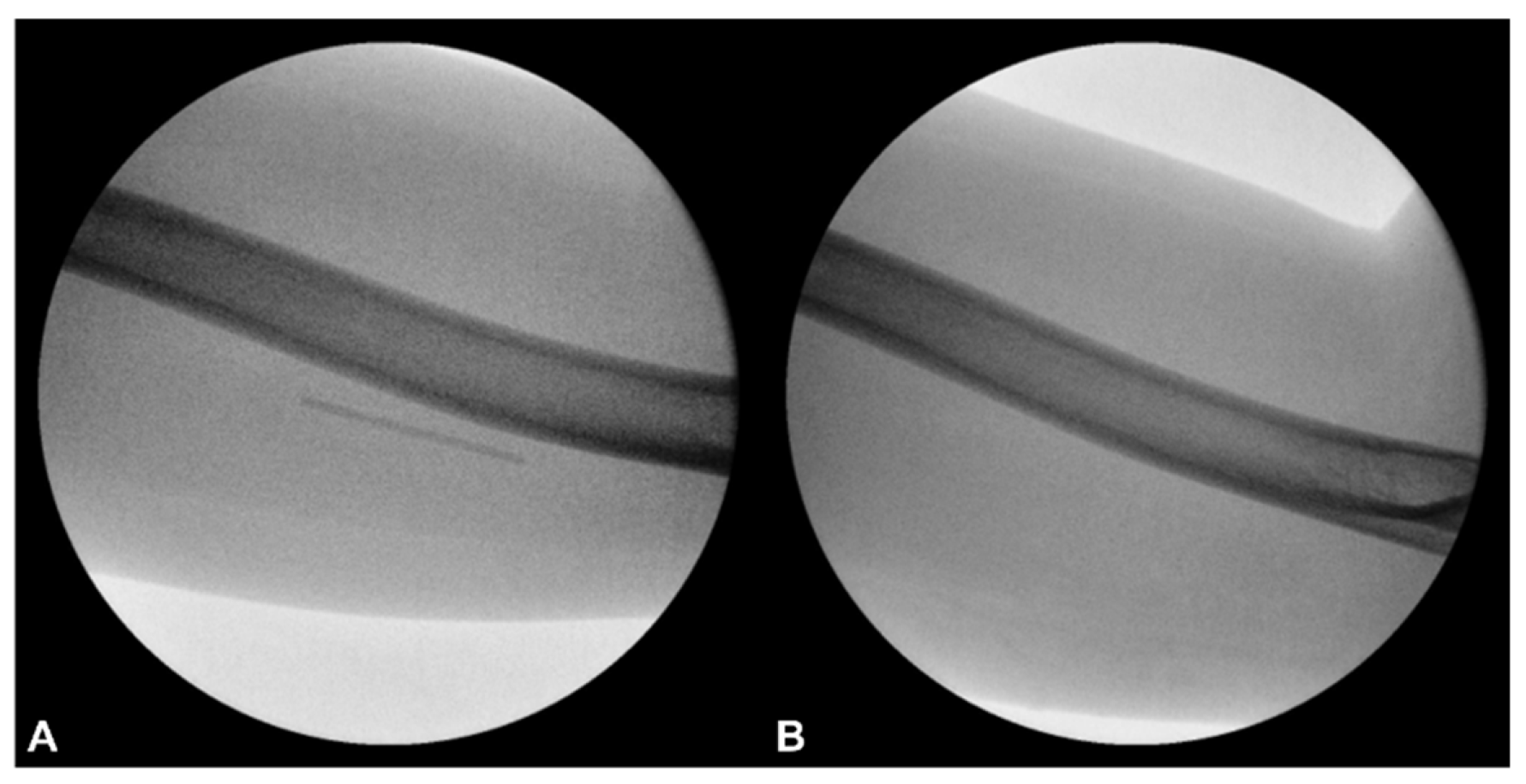
2.1. Prior Imaging Included Radiography (Figure 3) Confirming Implant Location, and Ultrasound (Figure 4) Demonstrating Its Adjacency to the Ulnar Nerve
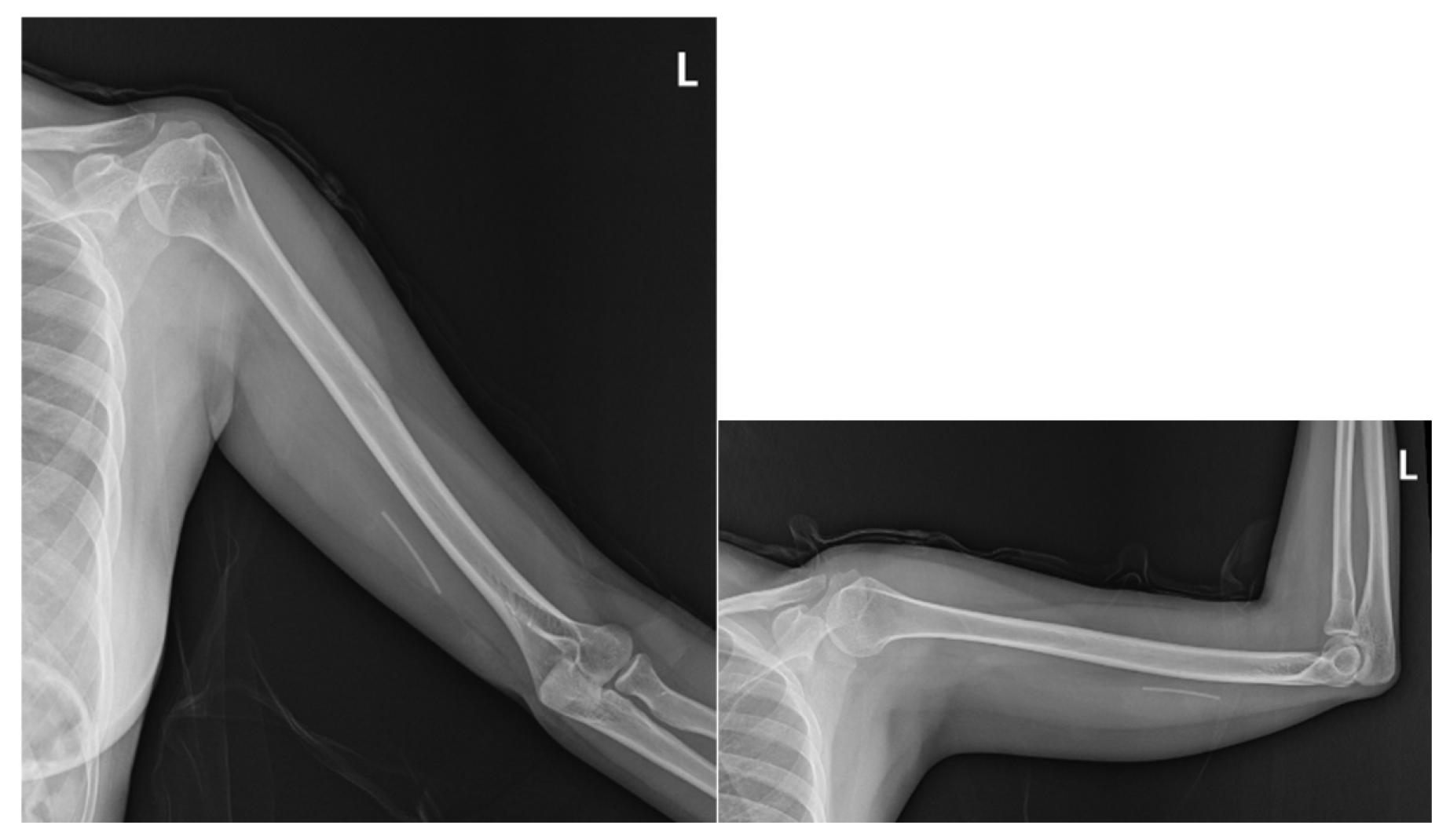
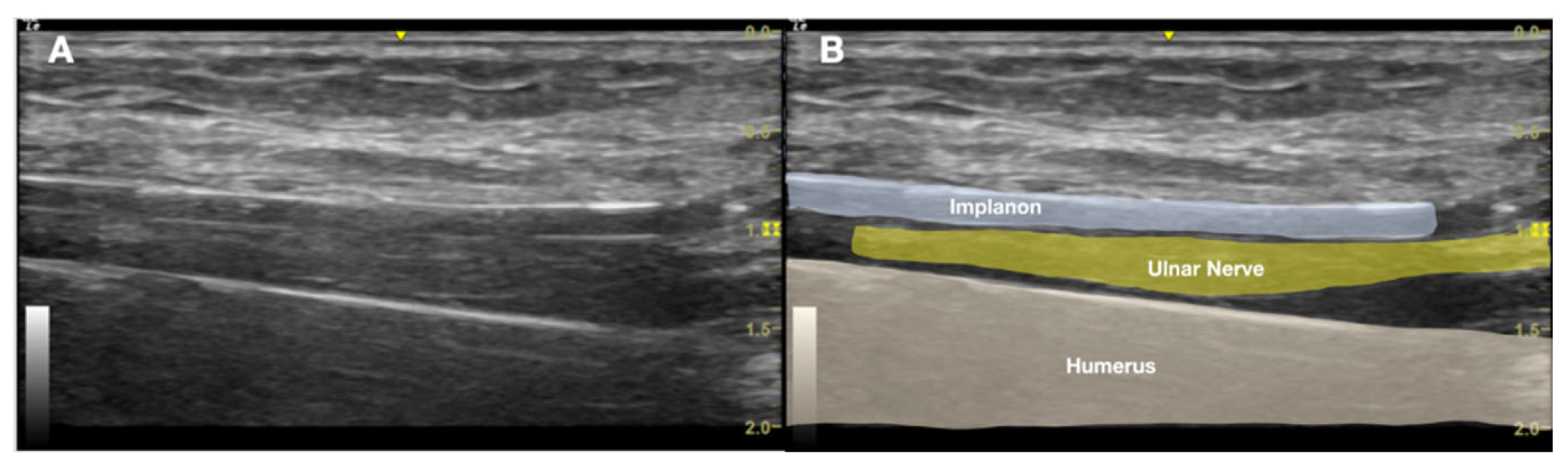
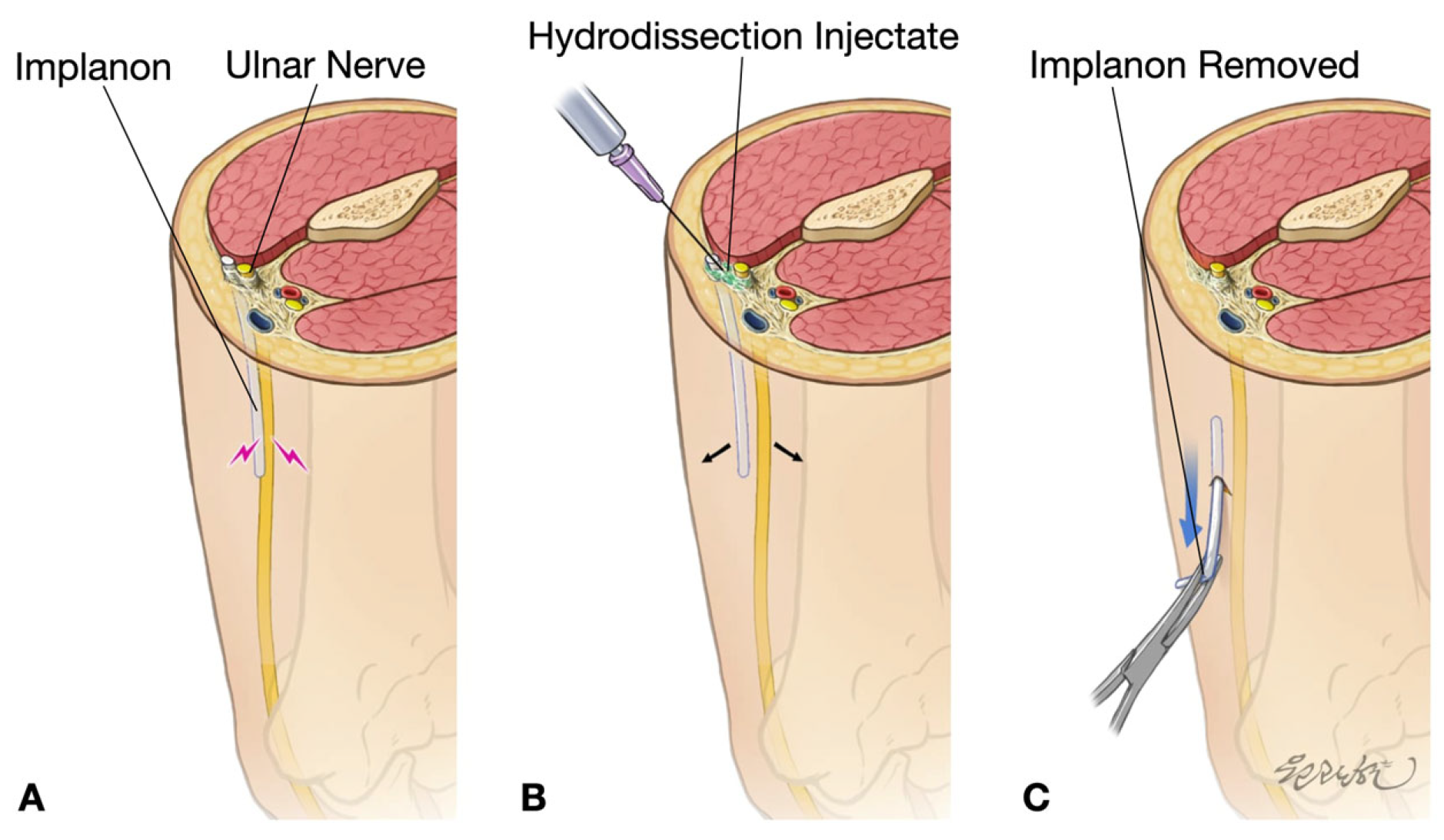
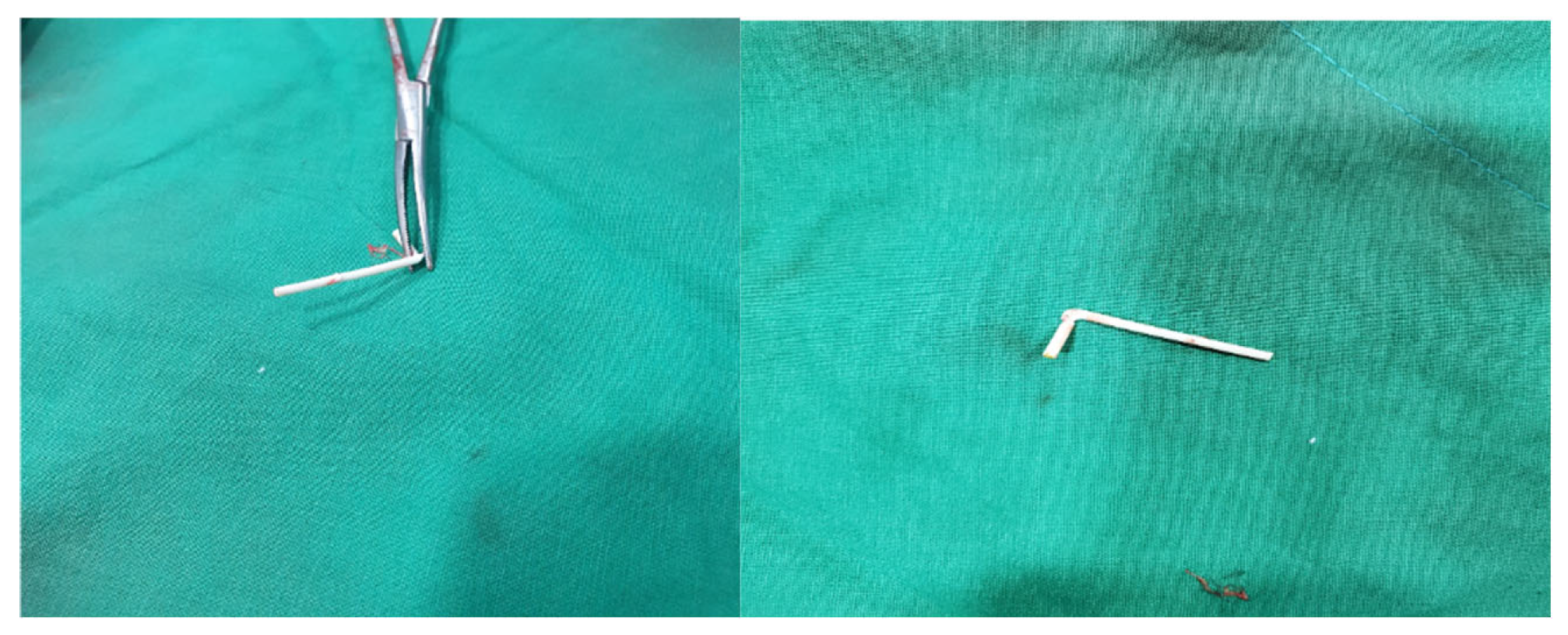
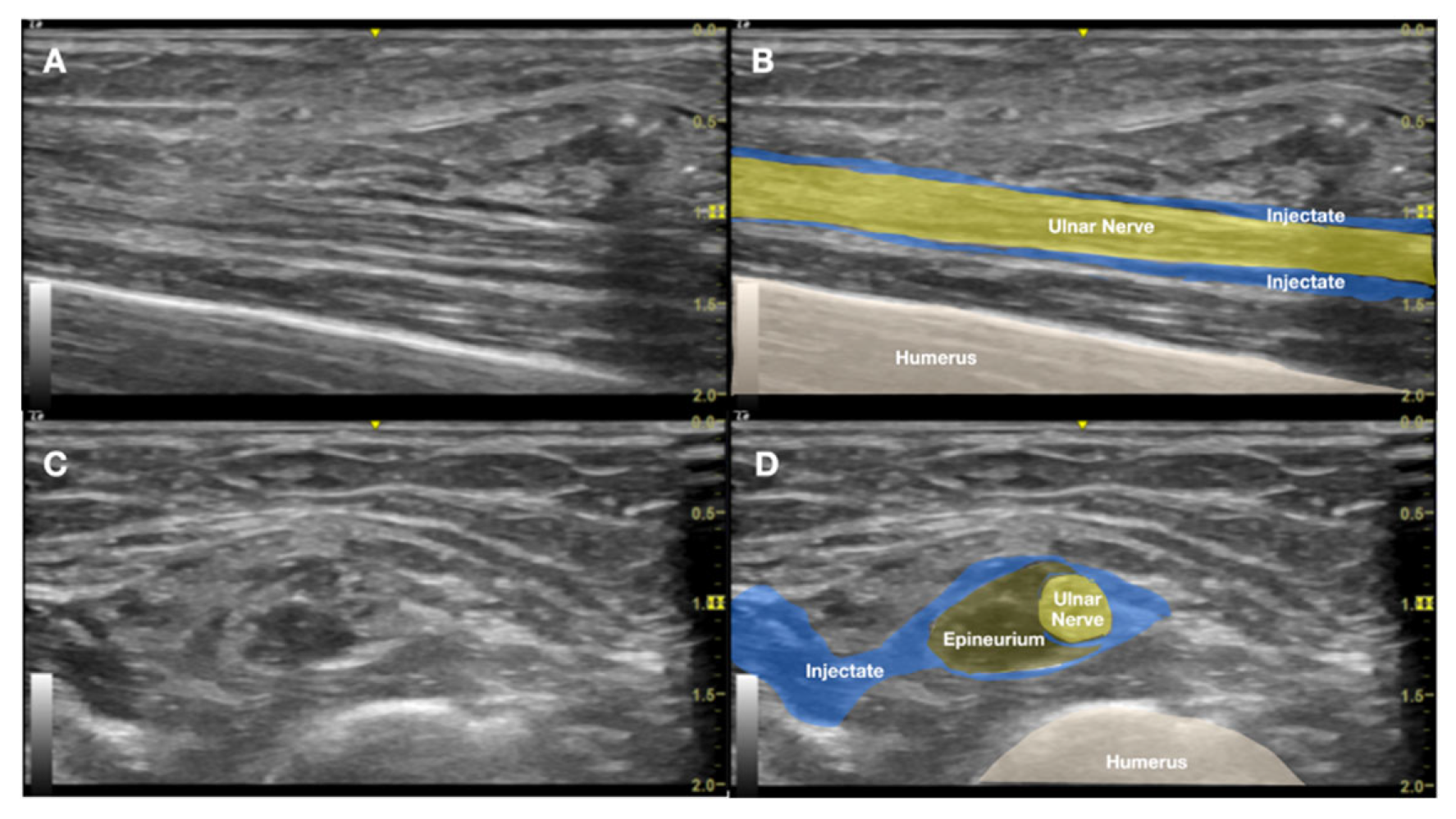
2.2. The Procedures:
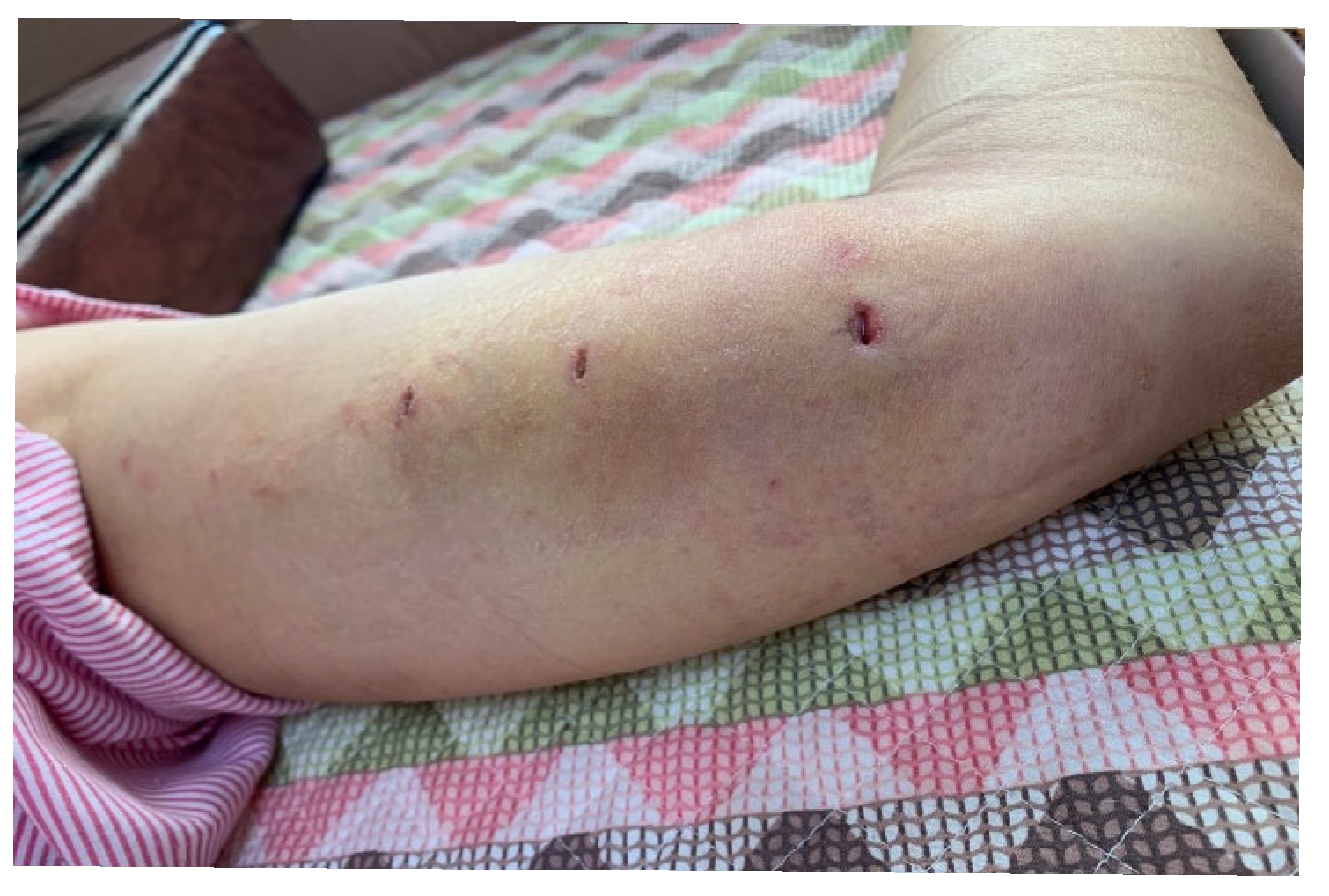
2.3. Follow-Up and Long-Term Outcomes
3. Discussion
Management Strategies for Non-Palpable or Deeply Placed Implants
4. Conclusions
- Early Imaging Evaluation: Essential for non-palpable implants presenting with neurological symptoms.
- Specialized Technical Skills: Needle stabilization and HD techniques are crucial for optimal outcomes.
- Centralized Referral Pathways: Should be established for complex cases.
Key Lessons
- Prevention Potential: Proper insertion technique and post-placement palpation can help prevent most migration complications [21].
- Technique Triad: The combination of (a) 5% dextrose HD, (b) 25G needle stabilization, and (c) real-time US visualization enables successful percutaneous removal of nerve-adherent implants.
- Research Priorities: Multicenter registries should track (a) optimal HD volumes, (b) long-term nerve outcomes, and (c) cost-benefit analyses compared to surgery [6].
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| HD | Hydrodissection |
| LA | Local anesthetic |
| NPRS | Numeric pain rating scale |
| QuickDASH | Quick Disabilities of the Arm, Shoulder, and Hand |
| US | Ultrasound |
References
- Adler, R.S.; Sofka, C.M. Percutaneous ultrasound-guided injections in the musculoskeletal system. Ultrasound Q 2003, 19, 3–12. [Google Scholar] [CrossRef] [PubMed]
- Gatt, D.L.; Charalambous, C.P. Ultrasound-guided barbotage for calcific tendonitis of the shoulder: a systematic review including 908 patients. Arthroscopy 2014, 30, 1166–1172. [Google Scholar] [CrossRef] [PubMed]
- Singh, M.; Mansour, D.; Richardson, D. Location and removal of non-palpable Implanon implants with the aid of ultrasound guidance. J Fam Plann Reprod Health Care 2006, 32, 153–156. [Google Scholar] [CrossRef]
- Rivera, F.; Bianciotto, A. Contraceptive subcutaneous device migration: what does an orthopaedic surgeon need to know? A case report and literature review. Acta Biomed 2020, 91, 232–237. [Google Scholar] [PubMed]
- United Nations Department of Economic and Social Affairs (UNDESA). *Contraceptive Use by Method, D.B.A.a.; Available from: https://www.un.org/en/development/desa/population/publications/pdf/family/ContraceptiveUseByMethodDataBooklet2019.pdf.
- Soler-Perromat, J.C.; et al. Ultrasound-guided minimally invasive removal of deep contraceptive implants: outcomes and challenges. Quant Imaging Med Surg 2024, 14, 7791–7802. [Google Scholar] [CrossRef]
- Matulich, M.C.; et al. Referral Center Experience With Nonpalpable Contraceptive Implant Removals. Obstet Gynecol 2019, 134, 801–806. [Google Scholar] [CrossRef]
- Jacques, T.; et al. Minimally invasive removal of deep contraceptive implants under continuous ultrasound guidance is effective, quick, and safe. Eur Radiol 2022, 32, 1718–1725. [Google Scholar] [CrossRef]
- Asaad, S.K.; et al. Contraceptive implant migration to the ulnar nerve: A case report with literature review. Clin Case Rep 2024, 12, e9420. [Google Scholar] [CrossRef]
- Lam, K.H.S.; et al. Ultrasound-Guided Nerve Hydrodissection for Pain Management: Rationale, Methods, Current Literature, and Theoretical Mechanisms. Journal of Pain Research 2020, 13, 1957–1968. [Google Scholar] [CrossRef]
- Nugroho, N.; et al. Novel Sonoguided Digital Palpation and Ultrasound-Guided Hydrodissection of the Long Thoracic Nerve for Managing Serratus Anterior Muscle Pain Syndrome: A Case Report with Technical Details. Diagnostics 2025, 15. [Google Scholar] [CrossRef]
- Lee, H.W. Confirming the Presence of Neurapraxia and Its Potential for Immediate Reversal by Novel Diagnostic and Therapeutic Ultrasound-Guided Hydrodissection Using 5% Dextrose in Water Without Local Anesthetics: Application in a Case of Acute Radial Nerve Palsy. Diagnostics 2025, 15. [Google Scholar] [CrossRef]
- Su, D.C.; Chang, K.V.; Lam, S.K.H. Shear Wave Elastography to Guide Perineural Hydrodissection: Two Case Reports. Diagnostics (Basel) 2020, 10. [Google Scholar] [CrossRef]
- Bertrand, H.; et al. Topical mannitol reduces capsaicin-induced pain: Results of a pilot-level, double-blind, randomized controlled trial. PM R 2015, 7, 1111–1117. [Google Scholar] [CrossRef] [PubMed]
- Liu, C. Discovery of first-in-class highly selective TRPV1 antagonists with dual analgesic and hypoglycemic effects. Bioorganic & Medicinal Chemistry 2024, 107, 117750. [Google Scholar]
- Cherng, J.H.; et al. The Potential of Glucose Treatment to Reduce Reactive Oxygen Species Production and Apoptosis of Inflamed Neural Cells In Vitro. Biomedicines 2023, 11. [Google Scholar] [CrossRef]
- Wu, Y.T.; et al. Mechanism of Glucose Water as a Neural Injection: A Perspective on Neuroinflammation. Life (Basel) 2022, 12. [Google Scholar] [CrossRef]
- Babaei-Ghazani, A.; et al. Ultrasound-guided 5% dextrose prolotherapy versus corticosteroid injection in carpal tunnel syndrome: a randomized, controlled clinical trial. Pain management 2022, 12, 687–697. [Google Scholar] [CrossRef]
- Topol, G.A.; et al. Dextrose Prolotherapy for Symptomatic Grade IV Knee Osteoarthritis: A Pilot Study of Early and Longer-Term Analgesia and Pain-Specific Cytokine Concentrations. Clin Pract 2022, 12, 926–938. [Google Scholar] [CrossRef]
- Saeed, A.; Narayan, N.; Pandya, A. Contraceptive Implant-Related Acute Ulnar Neuropathy: Prompt Diagnosis, Early Referral, and Management Are Key. Eplasty 2018, 18, e28. [Google Scholar] [PubMed]
- Mansour, D.; et al. Methods of accurate localisation of non-palpable subdermal contraceptive implants. J Fam Plann Reprod Health Care 2008, 34, 9–12. [Google Scholar] [CrossRef]
- Lam, K.H.S.; et al. Ultrasound-Guided Nerve Hydrodissection for Pain Management: Rationale, Methods, Current Literature, and Theoretical Mechanisms. J Pain Res 2020, 13, 1957–1968. [Google Scholar] [CrossRef]
- Tsui, B.C.; Kropelin, B. The electrophysiological effect of dextrose 5% in water on single-shot peripheral nerve stimulation. Anesth Analg 2005, 100, 1837–1839. [Google Scholar] [CrossRef]
- Hashimoto, K.; et al. Comparative toxicity of glucose and lidocaine administered intrathecally in the rat. Reg Anesth Pain Med 1998, 23, 444–450. [Google Scholar] [PubMed]
- Dufour, E.; et al. Ultrasound-guided perineural circumferential median nerve block with and without prior dextrose 5% hydrodissection: a prospective randomized double-blinded noninferiority trial. Anesth Analg 2012, 115, 728–733. [Google Scholar] [CrossRef]
- Buntragulpoontawee, M.; et al. The Effectiveness and Safety of Commonly Used Injectates for Ultrasound-Guided Hydrodissection Treatment of Peripheral Nerve Entrapment Syndromes: A Systematic Review. Front Pharmacol 2020, 11, 621150. [Google Scholar] [CrossRef] [PubMed]
- Wu, Y.T.; et al. Efficacy of 5% Dextrose Water Injection for Peripheral Entrapment Neuropathy: A Narrative Review. Int J Mol Sci 2021, 22. [Google Scholar] [CrossRef]
- Lam, K.H.S.; et al. Ultrasound-Guided Interventions for Carpal Tunnel Syndrome: A Systematic Review and Meta-Analyses. Diagnostics (Basel) 2023, 13. [Google Scholar] [CrossRef] [PubMed]
- Wu, Y.T.; et al. Novel Motor-Sparing Ultrasound-Guided Neural Injection in Severe Carpal Tunnel Syndrome: A Comparison of Four Injectates. Biomed Res Int 2022, 2022, 2022, 9745322. [Google Scholar] [CrossRef]
- Lin, C.P.; et al. Utility of ultrasound elastography in evaluation of carpal tunnel syndrome: A systematic review and meta-analysis. Ultrasound Med Biol 2019, 45, 2855–2865. [Google Scholar] [CrossRef]
- Wu, Y.T.; et al. Randomized double-blinded clinical trial of 5% dextrose versus triamcinolone injection for carpal tunnel syndrome patients. Ann Neurol 2018, 84, 601–610. [Google Scholar] [CrossRef]
- Chen, L.C.; et al. Perineural Dextrose and Corticosteroid Injections for Ulnar Neuropathy at the Elbow: a Randomized Double-blind Trial. Archives of physical medicine and rehabilitation 2020, 101, 1296–1303. [Google Scholar] [CrossRef] [PubMed]
- Patel, P.R.; et al. The Feasibility of In-Clinic Ultrasound-Guided Removal of Contraceptive Implants: A Case Series. 2014, 2014.
- Persaud, T.; et al. Ultrasound-guided removal of Implanon devices. Eur Radiol 2008, 18, 2582–2585. [Google Scholar] [CrossRef] [PubMed]
- Jacques, T.; et al. Minimally-invasive fully ultrasound-guided removal of nonpalpable single-rod contraceptive implant: Case report and technical description. Contraception 2020, 101, 338–341. [Google Scholar] [CrossRef] [PubMed]
| Characteristic | Open Removal | US-Guided Removal | US-Guided HD + Stabilization + Removal |
| Target Indications | Excessively difficult implants | Deep implants (not mentioning distance from nearby nerves in literature) | Nerve-adjacent or impinging implants |
| Operation Time | Long (>2 hours) | Short (<30 minutes) | Moderate (30 to 60 minutes) |
| Scar Size | Large incision | Small incision | Small incision |
| Nerve Injury Risk | Possible | Possible | Minimal |
| Soft Tissue Damage | Extensive | Moderate | Minimal |
| Migration Risk | Negligible | Possible | Reduced |
| Conversion to Open | N/A | Possible | Rare |
| Learning Curve | Low | Moderate | High |
| Complication Rate | Higher | Lower | Minimal |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




