Submitted:
06 August 2025
Posted:
07 August 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Objective
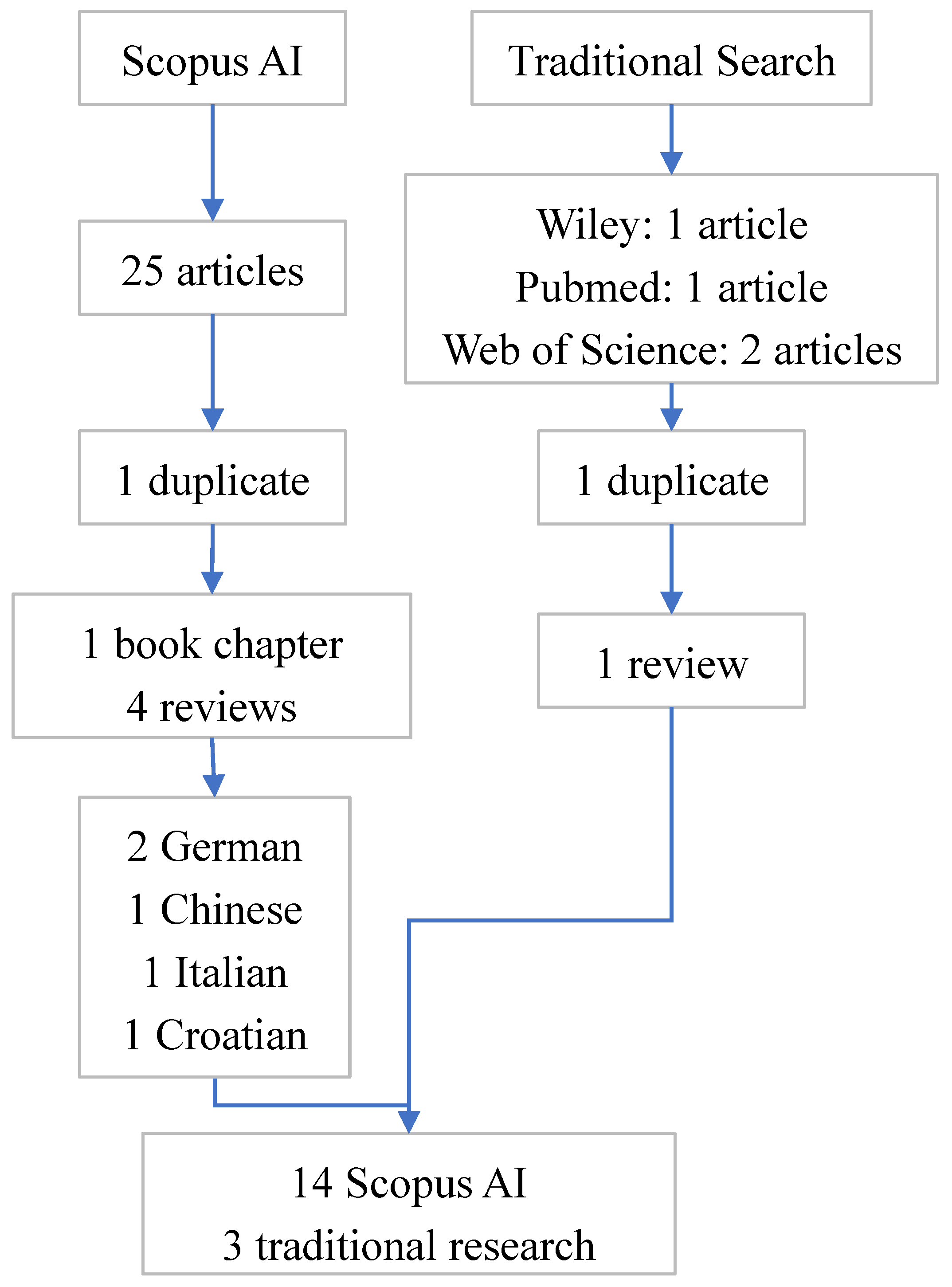
2.2. Search Strategy
2.2.1. Scopus AI Methodology
2.2.2. Traditional Keyword Search
2.3. Comparison of Methodologies
2.3.1. Efficiency
2.3.2. Quality of Results
2.3.3. Analysis of Results
3. Results
| Title 1 | Title 2 | ||
|---|---|---|---|
| Primary Prepectoral Breast Reconstruction After Radical Mastectomy | Prepectoral breast reconstruction (PPBR) has gained popularity as a technique for breast reconstruction following mastectomy due to its numerous advantages over traditional subpectoral methods. This summary provides an overview of the benefits, complications, and outcomes associated with PPBR based on recent studies. | ||
| Advantages of Prepectoral Breast Reconstruction: | |||
| Complications and Considerations: | |||
| Clinical Outcomes: |
|
||
| Comparison of Prepectoral and Subpectoral Techniques: | Aspect | Prepectoral | Subpectoral |
| Postoperative Pain | Lower[1,2,3] | Higher[1,2,3] | |
| Aesthetic Outcomes | Improved [4,5] | Comparable[4,5] | |
| Complication Rates | Lower capsular contracture [6,7] | Similar overall [2,6,8] | |
| Patient Satisfaction | High [4,10,11] | High[4,10,11] | |
| Functional Recovery | Faster[3] | Slower[3] | |
| In conclusion, primary prepectoral breast reconstruction after radical mastectomy offers several benefits, including reduced postoperative pain, improved aesthetic outcomes, and high patient satisfaction. However, careful patient selection and management of potential complications are essential for optimal results. | |||
| Based on the query, I will provide a summary that covers the surgical techniques, advantages and disadvantages, patient selection considerations, and long-term outcomes and complications associated with primary prepectoral breast reconstruction after radical mastectomy. | |
| Surgical Techniques: |
|
| Advantages and Disadvantages: |
|
| Patient Selection Considerations: |
|
| Long-term Outcomes and Complications: |
|
| In conclusion, primary prepectoral breast reconstruction after radical mastectomy involves various surgical techniques, each with its own set of advantages and disadvantages. By placing the implant above the pectoral muscle, this method reduces postoperative pain, shortens recovery time, and eliminates animation deformity, improving both functional and aesthetic outcomes. Unlike submuscular placement, it avoids disruption of muscle function and allows for a more natural contour, particularly in direct-to-implant procedures. Patient selection considerations and long-term outcomes and complications are important factors to consider when opting for this reconstruction method. However, it's important to note that the evidence is limited, and further research is needed to fully understand the implications of prepectoral breast reconstruction. | |
| Theme name (with references) | Definition | Potential hypothesis (with hyperlinks) |
|---|---|---|
| Patient Satisfaction and Quality of Life in Prepectoral Breast Reconstruction | The consistent interest in patient satisfaction and quality of life following prepectoral breast reconstruction highlights the importance of understanding patient-centered outcomes. This theme is crucial for improving surgical techniques and postoperative care to enhance patient experiences and satisfaction. |
|
| Advancements in Acellular Dermal Matrix (ADM) Utilization | The ongoing research into the use of acellular dermal matrices (ADM) in prepectoral breast reconstruction indicates a sustained interest in optimizing surgical outcomes and reducing complications. This theme is vital for developing new materials and techniques to improve the safety and efficacy of breast reconstruction procedures. |
|
| Innovations in Imaging and Measurement Techniques for Breast Reconstruction | The rising interest in advanced imaging and measurement techniques for prepectoral breast reconstruction reflects the need for precise preoperative planning and postoperative assessment. These innovations are crucial for improving surgical accuracy and patient outcomes. |
|
| Nipple-Sparing Mastectomy and Prepectoral Reconstruction | The increasing focus on nipple-sparing mastectomy combined with prepectoral reconstruction highlights the trend towards more conservative and aesthetically favorable surgical options. This approach aims to preserve the nipple-areolar complex while providing effective reconstruction, which is significant for patient satisfaction and cosmetic outcomes. |
|
| Prepectoral Tissue Expander Techniques | The novel focus on prepectoral tissue expander techniques without the use of acellular dermal matrix (ADM) represents a new direction in breast reconstruction research. This theme explores the feasibility, safety, and outcomes of using tissue expanders in a prepectoral plane, which could offer alternative options for patients and surgeons. |
|
| What are the key considerations for patient selection in primary prepectoral breast reconstruction? How does primary prepectoral breast reconstruction compare to subpectoral reconstruction in terms of outcomes and complications? What are the potential challenges and limitations of primary prepectoral breast reconstruction after radical mastectomy? |
4. Discussion
4.1. Implications for Future Research
4.2. Enhanced Comprehensiveness
4.3. Improved Accessibility for Novices
4.4. Focused and Manageable Results
4.5. Impact on Breast Reconstruction Research
4.6. Encouraging Interdisciplinary Research
5. Conclusions
5.1. Efficiency and Comprehensiveness of Scopus AI
5.2. Impact on Researchers with Limited Expertise
5.3. Quality and Relevance of Results
5.4. Manual Assessment in Traditional Searches
5.5. Implications for Future Research
5.6. Encouraging Interdisciplinary Research
References
- Roberts, K., Mills, N., Metcalfe, C., Lane, A., Clement, C., Hollingworth, W., Taylor, J., Holcombe, C., Skillman, J., Fairhurst, K., Whisker, L., Cutress, R., Thrush, S., Fairbrother, P., & Potter, S. (2021). Best-BRA (Is subpectoral or prepectoral implant placement best in immediate breast reconstruction?): a protocol for a pilot randomised controlled trial of subpectoral versus prepectoral immediate implant-based breast reconstruction in women following mastectomy. BMJ Open, 11(11), e050886. [CrossRef]
- Sbitany, H., Piper, M., & Lentz, R. (2017). Prepectoral Breast Reconstruction: A Safe Alternative to Submuscular Prosthetic Reconstruction following Nipple-Sparing Mastectomy. Plastic & Reconstructive Surgery, 140(3), 432–443. [CrossRef]
- Lee, J. S., Park, E., Lee, J. H., Lee, J., Park, H. Y., Yang, J. D., & Jung, T.-D. (2021). A prospective comparison study of early functional outcomes after implant-based breast reconstruction: subpectoral versus prepectoral technique. Annals of Palliative Medicine, 10(3), 2520–2529. [CrossRef]
- Taj, S., Chandavarkar, R., & Vidya, R. (2024). Current Global Trends in Prepectoral Breast Reconstruction. Medicina, 60(3), 431. [CrossRef]
- Rebowe, R. E., Allred, L. J., & Nahabedian, M. Y. (2018). The Evolution from Subcutaneous to Prepectoral Prosthetic Breast Reconstruction. Plastic and Reconstructive Surgery - Global Open, 6(6), e1797. [CrossRef]
- Graziano, F. D., Shay, P. L., Sanati-Mehrizy, P., & Sbitany, H. (2021b). Prepectoral implant reconstruction in the setting of post-mastectomy radiation. Gland Surgery, 10(1), 411–416. [CrossRef]
- Sigalove, S. (2019). Prepectoral breast reconstruction and radiotherapy—a closer look. Gland Surgery, 8(1), 67–74. [CrossRef]
- Mégevand, V., Scampa, M., McEvoy, H., Kalbermatten, D. F., & Oranges, C. M. (2022). Comparison of Outcomes Following Prepectoral and Subpectoral Implants for Breast Reconstruction: Systematic Review and Meta-Analysis. Cancers, 14(17), 4223. [CrossRef]
- Kumbla, P. A., Ananthasekar, S., & Denney, B. D. (2021). Two-Stage, Prepectoral Breast Reconstruction. Annals of Plastic Surgery, 86(6S), S482–S486. [CrossRef]
- Abd El Maksoud, W. M., Ahmed, Y. S., Hamza, A., Alghamdi, M. A., Alhashash, M., Rizk, P. A., al Amri, F. S., Abbas, K. S., Dalboh, A., Alzahrani, H. A., Alshandeer, M. H., Bawahab, A. M., & Sultan, M. H. (2024). Management of Breast Cancer by Skin-Reducing Mastectomy and Immediate Breast Reconstruction by Prepectoral Implant Approach with Polypropylene Mesh for Patients with Large Breasts. Aesthetic Plastic Surgery. [CrossRef]
- Abbas, A., Rizki, H., Tanska, A., Concepcion, M., Tasoulis, M. K., & Gui, G. (2022). A comparative study of secondary procedures after sub-pectoral and pre-pectoral single-stage implant-based breast reconstruction. Plastic & Reconstructive Surgery. [CrossRef]
- Onesti, M. G., di Taranto, G., Ribuffo, D., & Scuderi, N. (2020). ADM-assisted prepectoral breast reconstruction and skin reduction mastectomy: Expanding the indications for subcutaneous reconstruction. Journal of Plastic, Reconstructive & Aesthetic Surgery, 73(4), 673–680. [CrossRef]
- Visnjic, M., Kovacevic, P., Paunkovic, L., Djordjevic, G., Budjevac, D., & Visnjic, A. (2009). Breast reconstruction following amputation for cancer. Vojnosanitetski Pregled, 66(6), 427–433. [CrossRef]
- Ma, J. X., Xia, Y. C., Li, B., Zhao, H. M., Lei, Y. T., & Bu, X. (2023). [Choice of immediate breast reconstructive methods after modified radical mastectomy]. Beijing Da Xue Xue Bao. Yi Xue Ban = Journal of Peking University. Health Sciences, 55(4), 612–618. [CrossRef]
- Rezai, M., Darsow, M., Kümmel, S., & Krämer, S. (2008). Autologous and Alloplastic Breast Reconstruction – Overview of Techniques, Indications and Results. Gynäkologisch-Geburtshilfliche Rundschau, 48(2), 68–75. [CrossRef]
- Talwar, A. A., Lanni, M. A., Ryan, I. A., Kodali, P., Bernstein, E., McAuliffe, P. B., Broach, R. B., Serletti, J. M., Butler, P. D., & Fosnot, J. (2023). Prepectoral vs. Submuscular Implant-based Breast Reconstruction: A Matched-Pair Comparison of Outcomes. Plastic & Reconstructive Surgery. [CrossRef]
- Kronowitz, S. J., & Kuerer, H. M. (2006). Advances and surgical decision-making for breast reconstruction. Cancer, 107(5), 893–907. [CrossRef]
- Lee JS, Park E, Lee JH, Lee J, Park HY, Yang JD, Jung TD. A prospective comparison study of early functional outcomes after implant-based breast reconstruction: subpectoral versus prepectoral technique. Ann Palliat Med 2021;10(3):2520-2529. [CrossRef]
- Fredman R, Wu C, Rapolti M, Luckett D, Fine J, McGuire K, Gallagher K, Roughton M. Prepectoral Direct-to-Implant Breast Reconstruction: Early Outcomes and Analysis of Postoperative Pain. Aesthet Surg J Open Forum. 2019 Feb 27;1(1):ojz006. PMID: 33791602; PMCID: PMC7984832. [CrossRef]
- Rugină, A.I.; Ungureanu, A.; Giuglea, C.; Marinescu, S.A. Artificial Intelligence in Breast Reconstruction: A Narrative Review. Medicina 2025, 61, 440. [CrossRef]
- Shi YC, Li J, Li SJ, Li ZP, Zhang HJ, Wu ZY, Wu ZY. Flap failure prediction in microvascular tissue reconstruction using machine learning algorithms. World J Clin Cases. 2022 Apr 26;10(12):3729-3738. PMID: 35647170; PMCID: PMC9100718. [CrossRef]
- Mansoor, M.; Ibrahim, A.F. The Transformative Role of Artificial Intelligence in Plastic and Reconstructive Surgery: Challenges and Opportunities. J. Clin. Med. 2025, 14, 2698. [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




