Submitted:
05 August 2025
Posted:
05 August 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Epidemiological Landscape
3. Surgical Technique and Geographic Variation
4. Strengths and Limitations of the Literature
5. Neuropathic vs. Nociceptive CPIP: Diagnostic Challenges and Clinical Implications
6. Neuropathic and Nociceptive Pain Profiles
7. Limitations and Methodological Considerations
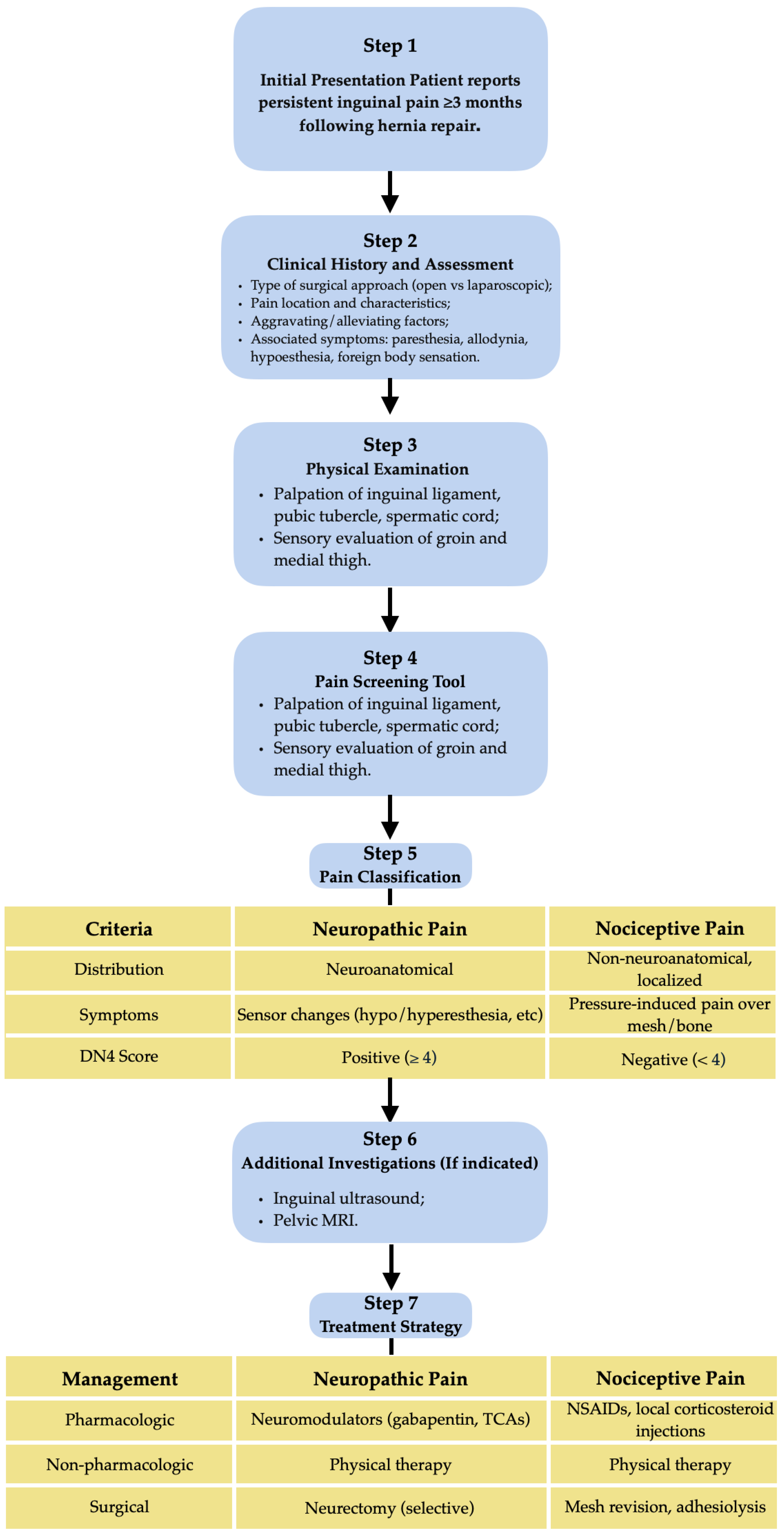
8. Toward a Structured Diagnostic Approach
9. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| CPIP | Chronic postoperative inguinal pain |
| IASP | International Association for the Study of Pain |
| NR | Not Reported |
| DN4 | Douleur Neuropathique 4 |
| TAPP | Transabdominal Preperitoneal |
| TEP | Totally Extraperitoneal |
| CI | Confidence Interval |
| PMID | PubMed Identifier |
References
- Scott NW, McCormack K, Graham P, Go PM, Ross SJ, Grant AM. Open mesh versus non-mesh for repair of femoral and inguinal hernia. Cochrane Database Syst Rev. 2002;(4):CD002197.
- Bay-Nielsen M, Perkins FM, Kehlet H, Danish Hernia Database. Pain and functional impairment 1 year after inguinal herniorrhaphy: a nationwide questionnaire study. Ann Surg. 2001 Jan;233(1):1–7. [CrossRef]
- Poobalan AS, Bruce J, Smith WCS, King PM, Krukowski ZH, Chambers WA. A review of chronic pain after inguinal herniorrhaphy. Clin J Pain. 2003;19(1):48–54. [CrossRef]
- Chapman CR, Vierck CJ. The Transition of Acute Postoperative Pain to Chronic Pain: An Integrative Overview of Research on Mechanisms. J Pain. 2017 Apr;18(4):359.e1-359.e38.
- Classification of chronic pain. Descriptions of chronic pain syndromes and definitions of pain terms. Prepared by the International Association for the Study of Pain, Subcommittee on Taxonomy. Pain Suppl. 1986;3:S1-226.
- Stabilini C, van Veenendaal N, Aasvang E, Agresta F, Aufenacker T, Berrevoet F, et al. Update of the international HerniaSurge guidelines for groin hernia management. BJS Open. 2023 Oct 20;7(5):zrad080. [CrossRef]
- HerniaSurge Group. International guidelines for groin hernia management. Hernia. 2018 Feb;22(1):1–165.
- Faessen JL, Stoot JHMB, van Vugt R. Safety and efficacy in inguinal hernia repair: a retrospective study comparing TREPP, TEP and Lichtenstein (SETTLE). Hernia. 2021 Oct;25(5):1309–15. [CrossRef]
- Lo CW, Chen YT, Jaw FS, Yu CC, Tsai YC. Predictive factors of post-laparoscopic inguinal hernia acute and chronic pain: prospective follow-up of 807 patients from a single experienced surgeon. Surg Endosc. 2021 Jan;35(1):148–58. [CrossRef]
- Forester B, Attaar M, Chirayil S, Kuchta K, Denham W, Linn JG, et al. Predictors of chronic pain after laparoscopic inguinal hernia repair. Surgery. 2021 Mar;169(3):586–94.
- Min L, Yong P, Yun L, Balde AI, Chang Z, Qian G, et al. Propensity score analysis of outcomes between the transabdominal preperitoneal and open Lichtenstein repair techniques for inguinal hernia repair: a single-center experience. Surg Endosc. 2020 Dec;34(12):5338–45.
- Bande D, Moltó L, Pereira JA, Montes A. Chronic pain after groin hernia repair: pain characteristics and impact on quality of life. BMC Surg. 2020 Jul 6;20(1):147. [CrossRef]
- Köckerling F, Lorenz R, Hukauf M, Grau H, Jacob D, Fortelny R, et al. Influencing Factors on the Outcome in Female Groin Hernia Repair: A Registry-based Multivariable Analysis of 15,601 Patients. Ann Surg. 2019 Jul;270(1):1–9.
- Chinchilla-Hermida PA, Baquero-Zamarra DR, Guerrero-Nope C, Bayter-Mendoza EF. Incidence of chronic post-surgical pain and its associated factors in patients taken to inguinal hernia repair. Colombian Journal of Anesthesiology. 2017 Oct 1;45(4):291–9.
- Andercou O, Olteanu G, Stancu B, Mihaileanu F, Chiorescu S, Dorin M. Risk factors for and prevention of chronic pain and sensory disorders following inguinal hernia repair. Ann Ital Chir. 2019;90:442–6.
- Lundström KJ, Holmberg H, Montgomery A, Nordin P. Patient-reported rates of chronic pain and recurrence after groin hernia repair. Br J Surg. 2018 Jan;105(1):106–12. [CrossRef]
- Matikainen M, Aro E, Vironen J, Kössi J, Hulmi T, Silvasti S, et al. Factors predicting chronic pain after open inguinal hernia repair: a regression analysis of randomized trial comparing three different meshes with three fixation methods (FinnMesh Study). Hernia. 2018 Oct;22(5):813–8.
- Niebuhr H, Wegner F, Hukauf M, Lechner M, Fortelny R, Bittner R, et al. What are the influencing factors for chronic pain following TAPP inguinal hernia repair: an analysis of 20,004 patients from the Herniamed Registry. Surg Endosc. 2018 Apr;32(4):1971–83.
- Ergönenç T, Beyaz SG, Özocak H, Palabıyık O, Altıntoprak F. Persistent postherniorrhaphy pain following inguinal hernia repair: A cross-sectional study of prevalence, pain characteristics, and effects on quality of life. Int J Surg. 2017 Oct;46:126–32. [CrossRef]
- Olsson A, Sandblom G, Fränneby U, Sondén A, Gunnarsson U, Dahlstrand U. Impact of postoperative complications on the risk for chronic groin pain after open inguinal hernia repair. Surgery. 2017 Feb;161(2):509–16.
- Schioldann J, Berrios GE. “My insanity in the year 1783”, by C.S. Andresen (1801). Hist Psychiatry. 2020 Dec;31(4):495–510.
- Pierides GA, Paajanen HE, Vironen JH. Factors predicting chronic pain after open mesh based inguinal hernia repair: A prospective cohort study. Int J Surg. 2016 May;29:165–70.
- Gutlic N, Rogmark P, Nordin P, Petersson U, Montgomery A. Impact of Mesh Fixation on Chronic Pain in Total Extraperitoneal Inguinal Hernia Repair (TEP): A Nationwide Register-based Study. Ann Surg. 2016 Jun;263(6):1199–206.
- Langeveld HR, Klitsie P, Smedinga H, Eker H, Van’t Riet M, Weidema W, et al. Prognostic value of age for chronic postoperative inguinal pain. Hernia. 2015 Aug;19(4):549–55. [CrossRef]
- Jeroukhimov I, Wiser I, Karasic E, Nesterenko V, Poluksht N, Lavy R, et al. Reduced postoperative chronic pain after tension-free inguinal hernia repair using absorbable sutures: a single-blind randomized clinical trial. J Am Coll Surg. 2014 Jan;218(1):102–7.
- Nikkolo C, Murruste M, Vaasna T, Seepter H, Tikk T, Lepner U. Three-year results of randomised clinical trial comparing lightweight mesh with heavyweight mesh for inguinal hernioplasty. Hernia. 2012 Oct;16(5):555–9. [CrossRef]
- Reinpold W. Risk factors of chronic pain after inguinal hernia repair: a systematic review. Innovative Surgical Sciences. 2017 Jun 1;2(2):61–8.
- Hompes R, Vansteenkiste F, Pottel H, Devriendt D, Van Rooy F. Chronic pain after Kugel inguinal hernia repair. Hernia. 2008 Apr;12(2):127–32. [CrossRef]
- Liu J, Shen J, Liu N, Liu Z, Zhu X, Zhong M, et al. Comparison of open and laparoscopic preperitoneal tension-free repair of groin hernia: a prospective nonrandomized controlled study. Surg Endosc. 2025 Jul 29;
- Nienhuijs SW, Boelens OBA, Strobbe LJA. Pain after anterior mesh hernia repair. J Am Coll Surg. 2005 Jun;200(6):885–9. [CrossRef]
- Fränneby U, Sandblom G, Nordin P, Nyrén O, Gunnarsson U. Risk factors for long-term pain after hernia surgery. Ann Surg. 2006 Aug;244(2):212–9.
- de la Croix H, Montgomery A, Holmberg H, Melkemichel M, Nordin P. Surgical expertise and risk of long-term complications following groin hernia mesh repair in sweden: a prospective, patient-reported, nationwide register study. Int J Surg. 2025 Jul 9; [CrossRef]
- Kwee E, Langeveld M, Duraku LS, Hundepool CA, Zuidam M. Surgical Treatment of Neuropathic Chronic Postherniorrhaphy Inguinal Pain: A Systematic Review and Meta-Analysis. Journal of Clinical Medicine. 2024 Jan;13(10):2812. [CrossRef]
- Taha-Mehlitz S, Taha A, Janzen A, Saad B, Hendie D, Ochs V, et al. Is pain control for chronic neuropathic pain after inguinal hernia repair using endoscopic retroperitoneal neurectomy effective? A meta-analysis of 142 patients from 1995 to 2022. Langenbecks Arch Surg. 2023 Jan 18;408(1):39.
- Loos MJA, Roumen RMH, Scheltinga MRM. Classifying post-herniorrhaphy pain syndromes following elective inguinal hernia repair. World J Surg. 2007 Sep;31(9):1760–5.
- Herrmann E, Schindehütte M, Kindl G, Reinhold AK, Aulbach F, Rose N, et al. Chronic postsurgical inguinal pain: incidence and diagnostic biomarkers from a large German national claims database. Br J Anaesth. 2025 Jun;134(6):1746–55. [CrossRef]
- Reistrup H, Fonnes S, Rosenberg J. Chronic pain and sexual dysfunction after groin hernia repair in adolescents: a nationwide survey. ANN SURG [Internet]. 2025 [cited 2025 Aug 1]; Available from: https://research.regionh.dk/en/publications/chronic-pain-and-sexual-dysfunction-after-groin-hernia-repair-in-.
| Author and year of publication | Nation | Time of evaluation | Surgical approach | Number of patients enrolled | Number of patients with CPIP | Rate of patients with CPIP |
| Lo et al 2021[9] | Taiwan | 3 months | Laparoscopy | 664 | 53 | 8.7% |
| Forester et al 2021(10) | UK | 6 months | Laparoscopy | 960 | 58 | 6% |
| Min et al 2020 [11] | China | 3 months | Open/ Laparoscopy |
800 | 215 | 26.8% |
| Bande et al 2020 [12] | Spain | 4 months | Open | 1.761 | 239 | 13.6% |
| Köckerling et al 2019 [13] | Germany | 1 year | Open/ Laparoscopy |
15.601 | 1.189 | 7.6% |
| Chinchilla Hermida et al 2018 [14] | Colombia | 6 months | Open/ Laparoscopy |
108 | 30 | 27.8% |
| Andercou et al 2018 [15] | Romania | 3 months | Open/ Laparoscopy |
365 | 38 | 10.4% |
| Lundström et al 2018 [16] | Sweden | 1 year | Open/ Laparoscopy |
22.917 | 3.492 | 15.2% |
| Matikainen et al 2018 [17] |
Finland | 1 year | Open | 625 | 52 | 8.32% |
| Niebuhr et al 2018 [18] | Germany | 1 year | Laparoscopy | 20.004 | 12.866 | 64.3% |
| Ergönenç et al 2017 [19] | Turkey | 3 months | Open | 264 | 61 | 23.4% |
| Olsson et al 2017 [20] | Sweden | NR | Open | 952 | 170 | 17.8% |
| Andresen et al 2017 [21] | Denmark | NR | Laparoscopy | 1.421 | 278 | 19.5% |
| Pierides et al 2016 [22] | Finland | 1 year | Open | 932 | 99 | 11.5% |
| Gutlic et al 2016 [23] | Sweden | NR | Laparoscopy | 1.098 | 85 | 7.7% |
| Langeveld et al 2015 [24] | The Netherlands | 1 year | Open/ Laparoscopy |
489 | 130 | 27% |
| Jeroukhimov et al 2014 [25] | Israel | 1 year | Open | 192 | 63 | 32.8% |
| Nikkolo et al 2012 [26] | Estonia | 3 years | Open | 116 | 27 | 23.3% |
| Reinpold et al 2011 [27] | Germany | 6 months | Open | 704 | 116 | 16.6% |
| Hompes et al 2008 [28] | Belgium | 1 year | Open | 377 | 57 | 15.1% |
| Poobalan et al 2008 [3] | UK | 3 months | Open | 226 | 67 | 30% |
| Loos et al 2007 |
The Netherlands | NR | Open/ Laparoscopy |
1.776 | 211 | 11.9% |
| Fränneby et al 2006 | Sweden | NR | Open | 2.456 | 758 | 31% |
| Nienhuijs et al 2005 | The Netherlands | NR | Open | 319 | 139 | 43.3% |
| Author and year of publication | Number of patients with CPIP | Surgical approach | Patients with neuropathic CPIP | Rate of neuropathic CPIP | Patients with no neuropathic CPIP | Rate of no neuropathic CPIP |
| Bande 2020 [12] | 239 | Open | 92 | 38.5% | 147 | 61.5% |
| Ergönenç 2017 [19] | 61 | Open | 45 | 73.7% | 16 | 26.3% |
| Loos 2007 [35] | 148 | Open/Lapa-roscopy | 72 | 46.5% | 76 | 53.5% |
| Nienhuijs 2005 [30] | 139 | Open | 56 | 40.3% | 82 | 59.7% |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




