Submitted:
01 August 2025
Posted:
04 August 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Androgen Receptor in Melanoma Metastasis
3. Androgen Receptor-Mediated Immune Evasion and Tumor Microenvironment Reprogramming
4. Androgen Receptor and Therapy Resistance
5. Clinical Translation and Future Directions
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
| AR | Androgen receptor |
| ICIs | Immune Checkpoint Inhibitors |
| UV | Ultraviolet |
| EMT | Epithelial-to-mesenchymal transition |
| TWIST1 | Twist-related protein |
| SNAI1 | Zinc finger protein SNAI1 |
| MMPs | Matrix Metalloproteinases |
| ICAM1 | Intracellular adhesion molecule 1 |
| IL-6 | Interleukin 6 |
| FUT4 | Fucosyltransferase 4 |
| AJs | Adherence junctions |
| TCGA SKCM | The Cancer Genome Atlas human skin cutaneous melanoma |
| TME | Tumor Microenvironment |
| MICA | Major histocompatibility complex class I chain-related protein A |
| MICB | Major histocompatibility complex class I chain-related protein B |
| MHC | Major histocompatibility complex |
| TAP | Transporter associated with antigen processing protein |
| Tregs | T regulatory cells |
| MDSCs | Myeloid-derived suppressor cells |
| ADT | Androgen deprivation therapy |
| SARDs | Selective AR degraders |
| PROTACs | Proteolysis-targeting chimeras |
| RNAi | RNA interface |
| SARMs | Selective Androgen Receptor Modulators |
References
- Bellenghi M, Puglisi R, Pontecorvi G, De Feo A, Carè A, Mattia G: Sex and Gender Disparities in Melanoma. Cancers 2020, 12, 1819. [CrossRef] [PubMed]
- Sung, H.; Ferlay, J.; Siegel, R.L.; Laversanne, M.; Soerjomataram, I.; Jemal, A.; Bray, F. Global Cancer Statistics 2020: GLOBOCAN Estimates of Incidence and Mortality Worldwide for 36 Cancers in 185 Countries. CA: A Cancer J. Clin. 2021, 71, 209–249. [Google Scholar] [CrossRef] [PubMed]
- Sood S, Jayachandiran R, Pandey S: Current Advancements and Novel Strategies in the Treatment of Metastatic Melanoma. Integrative Cancer Therapies 2021, 20, 1534735421990078. [CrossRef] [PubMed]
- Mancianti ML, Herlyn M: Tumor progression in melanoma: the biology of epidermal melanocytes in vitro. Carcinog Compr Surv 1989, 11, 369–386.
- Xu J, Mu S, Wang Y, Yu S, Wang Z: Recent advances in immunotherapy and its combination therapies for advanced melanoma: a review. Frontiers in Oncology 2024, 14.
- Davey, R.A.; Grossmann, M. Androgen Receptor Structure, Function and Biology: From Bench to Bedside. Clin. Biochem. Rev. 2016, 37, 3–15. [Google Scholar]
- Samarkina, A.; Youssef, M.K.; Ostano, P.; Ghosh, S.; Ma, M.; Tassone, B.; Proust, T.; Chiorino, G.; Levesque, M.P.; Goruppi, S.; et al. Androgen receptor is a determinant of melanoma targeted drug resistance. Nat. Commun. 2023, 14, 1–19. [Google Scholar] [CrossRef]
- Ben-Batalla I, Vargas-Delgado ME, von Amsberg G, Janning M, Loges S: Influence of Androgens on Immunity to Self and Foreign: Effects on Immunity and Cancer. Front Immunol 2020, 11, 1184. [CrossRef]
- Jamroze A, Chatta G, Tang DG: Androgen receptor (AR) heterogeneity in prostate cancer and therapy resistance. Cancer Letters 2021, 518, 1–9. [CrossRef]
- Zarif, J.C.; Miranti, C.K. The importance of non-nuclear AR signaling in prostate cancer progression and therapeutic resistance. Cell. Signal. 2016, 28, 348–356. [Google Scholar] [CrossRef]
- Brawer MK: Androgen deprivation therapy: a cornerstone in the treatment of advanced prostate cancer. Rev Urol 2004, 6 (Suppl 8), S3–9.
- Liu, Q.; Adhikari, E.; Lester, D.K.; Fang, B.; Johnson, J.O.; Tian, Y.; Mockabee-Macias, A.T.; Izumi, V.; Guzman, K.M.; White, M.G.; et al. Androgen drives melanoma invasiveness and metastatic spread by inducing tumorigenic fucosylation. Nat. Commun. 2024, 15, 1–20. [Google Scholar] [CrossRef]
- Vellano CP, White MG, Andrews MC, Chelvanambi M, Witt RG, Daniele JR, Titus M, McQuade JL, Conforti F, Burton EM et al. : Androgen receptor blockade promotes response to BRAF/MEK-targeted therapy. Nature 2022, 606, 797–803. [Google Scholar] [CrossRef] [PubMed]
- Wang Y, Ou Z, Sun Y, Yeh S, Wang X, Long J, Chang C: Androgen receptor promotes melanoma metastasis via altering the miRNA-539-3p/USP13/MITF/AXL signals. Oncogene 2017, 36, 1644–1654. [CrossRef] [PubMed]
- Stidham KR, Johnson JL, Seigler HF: Survival superiority of females with melanoma. A multivariate analysis of 6383 patients exploring the significance of gender in prognostic outcome. Arch Surg 1994, 129, 316–324. [Google Scholar] [CrossRef]
- de Vries, E.; Nijsten, T.E.C.; Visser, O.; Bastiaannet, E.; van Hattem, S.; Janssen-Heijnen, M.L.; Coebergh, J.-. .-W.W. Superior survival of females among 10 538 Dutch melanoma patients is independent of Breslow thickness, histologic type and tumor site. Ann. Oncol. 2007, 19, 583–589. [Google Scholar] [CrossRef]
- Joosse A, Collette S, Suciu S, Nijsten T, Patel PM, Keilholz U, Eggermont AM, Coebergh JW, de Vries E: Sex is an independent prognostic indicator for survival and relapse/progression-free survival in metastasized stage III to IV melanoma: a pooled analysis of five European organisation for research and treatment of cancer randomized controlled trials. J Clin Oncol 2013, 31, 2337–2346.
- Balch, C.M.; Soong, S.-J.; Gershenwald, J.E.; Reintgen, D.S.; Cascinelli, N.; Urist, M.; McMasters, K.M.; Ross, M.I.; Kirkwood, J.M.; Atkins, M.B.; et al. Prognostic Factors Analysis of 17,600 Melanoma Patients: Validation of the American Joint Committee on Cancer Melanoma Staging System. J. Clin. Oncol. 2001, 19, 3622–3634. [Google Scholar] [CrossRef]
- Olsen, C.M.; Pandeya, N.; Miranda-Filho, A.; Rosenberg, P.S.; Whiteman, D.C. Does Sex Matter? Temporal Analyses of Melanoma Trends among Men and Women Suggest Etiologic Heterogeneity. J. Investig. Dermatol. 2024, 145, 135–143. [Google Scholar] [CrossRef]
- Switzer B, Puzanov I, Skitzki JJ, Hamad L, Ernstoff MS: Managing Metastatic Melanoma in 2022: A Clinical Review. JCO Oncology Practice 2022, 18, 335–351. [CrossRef]
- Castellani G, Buccarelli M, Arasi MB, Rossi S, Pisanu ME, Bellenghi M, Lintas C, Tabolacci C: BRAF Mutations in Melanoma: Biological Aspects, Therapeutic Implications, and Circulating Biomarkers. Cancers (Basel) 2023, 15(16).
- Anna B, Blazej Z, Jacqueline G, Andrew CJ, Jeffrey R, Andrzej S: Mechanism of UV-related carcinogenesis and its contribution to nevi/melanoma. Expert Rev Dermatol 2007, 2, 451–469. [CrossRef] [PubMed]
- Ma, M.; Ghosh, S.; Tavernari, D.; Katarkar, A.; Clocchiatti, A.; Mazzeo, L.; Samarkina, A.; Epiney, J.; Yu, Y.-R.; Ho, P.-C.; et al. Sustained androgen receptor signaling is a determinant of melanoma cell growth potential and tumorigenesis. J. Exp. Med. 2020, 218. [Google Scholar] [CrossRef] [PubMed]
- Chuang, K.-T.; Chiou, S.-S.; Hsu, S.-H. Recent Advances in Transcription Factors Biomarkers and Targeted Therapies Focusing on Epithelial–Mesenchymal Transition. Cancers 2023, 15, 3338. [Google Scholar] [CrossRef] [PubMed]
- Khatiwada P, Kannan A, Malla M, Dreier M, Shemshedini L: Androgen up-regulation of Twist1 gene expression is mediated by ETV1. PeerJ 2020, 8, e8921. [CrossRef]
- Sorrentino C, D’Angiolo R, Gentile G, Giovannelli P, Perillo B, Migliaccio A, Castoria G, Di Donato M: The Androgen Regulation of Matrix Metalloproteases in Prostate Cancer and Its Related Tumor Microenvironment. Endocrines 2023, 4, 350–365. [CrossRef]
- Larsson P, Syed Khaja AS, Semenas J, Wang T, Sarwar M, Dizeyi N, Simoulis A, Hedblom A, Wai SN, Ødum N et al. : The functional interlink between AR and MMP9/VEGF signaling axis is mediated through PIP5K1α/pAKT in prostate cancer. International Journal of Cancer 2020, 146, 1686–1699. [Google Scholar] [CrossRef]
- Liao X, Thrasher JB, Pelling J, Holzbeierlein J, Sang QX, Li B: Androgen stimulates matrix metalloproteinase-2 expression in human prostate cancer. Endocrinology 2003, 144, 1656–1663. [CrossRef]
- Singh N, Khatib J, Chiu C-Y, Lin J, Patel TS, Liu-Smith F: Tumor Androgen Receptor Protein Level Is Positively Associated with a Better Overall Survival in Melanoma Patients. Genes 2023, 14, 345. [CrossRef]
- Morgese, F.; Sampaolesi, C.; Torniai, M.; Conti, A.; Ranallo, N.; Giacchetti, A.; Serresi, S.; Onofri, A.; Burattini, M.; Ricotti, G.; et al. Gender Differences and Outcomes in Melanoma Patients. Oncol. Ther. 2020, 8, 103–114. [Google Scholar] [CrossRef]
- Lai J-J, Lai K-P, Zeng W, Chuang K-H, Altuwaijri S, Chang C: Androgen Receptor Influences on Body Defense System via Modulation of Innate and Adaptive Immune Systems: Lessons from Conditional AR Knockout Mice. The American Journal of Pathology 2012, 181, 1504–1512. [CrossRef]
- Ashcroft GS, Mills SJ: Androgen receptor-mediated inhibition of cutaneous wound healing. J Clin Invest 2002, 110, 615–624. [CrossRef]
- Becerra-Díaz, M.; Strickland, A.B.; Keselman, A.; Heller, N.M. Androgen and Androgen Receptor as Enhancers of M2 Macrophage Polarization in Allergic Lung Inflammation. J. Immunol. 2018, 201, 2923–2933. [Google Scholar] [CrossRef]
- Kissick, H. T.; Sanda, M. G.; Dunn, L. K.; Pellegrini, K. L.; On, S. T.; Noel, J. K.; Arredouani, M. S. Androgens alter T-cell immunity by inhibiting T-helper 1 differentiation. Proc. Natl. Acad. Sci. USA Am. 2014, 111, 9887–9892. [Google Scholar] [CrossRef]
- Guan, X.; Polesso, F.; Wang, C.; Sehrawat, A.; Hawkins, R.M.; Murray, S.E.; Thomas, G.V.; Caruso, B.; Thompson, R.F.; Wood, M.A.; et al. Androgen receptor activity in T cells limits checkpoint blockade efficacy. Nature 2022, 606, 791–796. [Google Scholar] [CrossRef] [PubMed]
- Villanueva J, Herlyn M: Melanoma and the tumor microenvironment. Curr Oncol Rep 2008, 10, 439–446. [CrossRef] [PubMed]
- Somasundaram R, Herlyn M, Wagner SN: The role of tumor microenvironment in melanoma therapy resistance. Melanoma Manag 2016, 3, 23–32. [CrossRef] [PubMed]
- Yang C, Jin J, Yang Y, Sun H, Wu L, Shen M, Hong X, Li W, Lu L, Cao D et al. : Androgen receptor-mediated CD8(+) T cell stemness programs drive sex differences in antitumor immunity. Immunity 2022, 55, 1268–1283. [Google Scholar] [CrossRef]
- Hu YM, Zhao F, Graff JN, Chen C, Zhao X, Thomas GV, Wu H, Kardosh A, Mills GB, Alumkal JJ et al.: Androgen receptor activity inversely correlates with immune cell infiltration and immunotherapy response across multiple cancer lineages. bioRxiv 2024.
- Shen, B.; Mei, J.; Xu, R.; Cai, Y.; Wan, M.; Zhou, J.; Ding, J.; Zhu, Y. B7-H3 is associated with the armored-cold phenotype and predicts poor immune checkpoint blockade response in melanoma. Pathol. - Res. Pr. 2024, 256, 155267. [Google Scholar] [CrossRef]
- Flem-Karlsen K, Tekle C, Andersson Y, Flatmark K, Fodstad Ø, Nunes-Xavier CE: Immunoregulatory protein B7-H3 promotes growth and decreases sensitivity to therapy in metastatic melanoma cells. Pigment Cell Melanoma Res 2017, 30, 467–476. [CrossRef]
- Nunes-Xavier, C.E.; Kildal, W.; Kleppe, A.; Danielsen, H.E.; Wæhre, H.; Llarena, R.; Mælandsmo, G.M.; Fodstad, Ø.; Pulido, R.; López, J.I. Immune checkpoint B7-H3 protein expression is associated with poor outcome and androgen receptor status in prostate cancer. Prostate 2021, 81, 838–848. [Google Scholar] [CrossRef]
- Petroff, M.G.; Kharatyan, E.; Torry, D.S.; Holets, L. The Immunomodulatory Proteins B7-DC, B7-H2, and B7-H3 Are Differentially Expressed across Gestation in the Human Placenta. Am. J. Pathol. 2005, 167, 465–473. [Google Scholar] [CrossRef] [PubMed]
- Hofmeyer KA, Ray A, Zang X: The contrasting role of B7-H3. Proc Natl Acad Sci U S A 2008, 105, 10277–10278. [CrossRef] [PubMed]
- Passarelli A, Mannavola F, Stucci LS, Tucci M, Silvestris F: Immune system and melanoma biology: a balance between immunosurveillance and immune escape. Oncotarget 2017, 8, 106132–106142. [CrossRef] [PubMed]
- Xing S, Ferrari de Andrade L: NKG2D and MICA/B shedding: a ‘tag game’ between NK cells and malignant cells. Clin Transl Immunology 2020, 9, e1230. [CrossRef]
- Zingoni A, Molfetta R, Fionda C, Soriani A, Paolini R, Cippitelli M, Cerboni C, Santoni A: NKG2D and Its Ligands: “One for All, All for One”. Frontiers in Immunology, 2018.
- Dhatchinamoorthy K, Colbert JD, Rock KL: Cancer Immune Evasion Through Loss of MHC Class I Antigen Presentation. Frontiers in Immunology 2021, Volume 12 - 2021.
- Chesner, L.N.; Polesso, F.; Graff, J.N.; Hawley, J.E.; Smith, A.K.; Lundberg, A.; Das, R.; Shenoy, T.; Sjöström, M.; Zhao, F.; et al. Androgen Receptor Inhibition Increases MHC Class I Expression and Improves Immune Response in Prostate Cancer. Cancer Discov. 2024, 15, 481–494. [Google Scholar] [CrossRef]
- Tao, J.; Li, Y.; Liu, Y.-Q.; Wang, L.; Yang, J.; Dong, J.; Wu, Y.; Shen, G.-X.; Tu, Y.-T. Restoration of the Expression of Transports Associated with Antigen Processing in Human Malignant Melanoma Increases Tumor-Specific Immunity. J. Investig. Dermatol. 2008, 128, 1991–1996. [Google Scholar] [CrossRef]
- Consiglio CR, Udartseva O, Ramsey KD, Bush C, Gollnick SO: Enzalutamide, an Androgen Receptor Antagonist, Enhances Myeloid Cell-Mediated Immune Suppression and Tumor Progression. Cancer Immunol Res 2020, 8, 1215–1227. [CrossRef]
- van Rooijen JM, Qiu S-Q, Timmer-Bosscha H, van der Vegt B, Boers JE, Schröder CP, de Vries EGE: Androgen receptor expression inversely correlates with immune cell infiltration in human epidermal growth factor receptor 2–positive breast cancer. European Journal of Cancer 2018, 103, 52–60. [CrossRef]
- Klein RM, Bernstein D, Higgins SP, Higgins CE, Higgins PJ: SERPINE1 expression discriminates site-specific metastasis in human melanoma. Exp Dermatol 2012, 21, 551–554. [CrossRef]
- Efficacy of Immune Checkpoint Inhibitors Is Modulated by Androgen Receptor. Cancer Discov 2022, 12, 1405. [CrossRef]
- Gamat M, McNeel DG: Androgen deprivation and immunotherapy for the treatment of prostate cancer. Endocr Relat Cancer 2017, 24, T297–t310. [CrossRef] [PubMed]
- Dallos, M.C.; Obradovic, A.Z.; McCann, P.; Chowdhury, N.; Pratapa, A.; Aggen, D.H.; Gaffney, C.; Autio, K.A.; Virk, R.K.; De Marzo, A.M.; et al. Androgen Deprivation Therapy Drives a Distinct Immune Phenotype in Localized Prostate Cancer. Clin. Cancer Res. 2024, 30, 5218–5230. [Google Scholar] [CrossRef] [PubMed]
- Lin PY, Sun L, Thibodeaux SR, Ludwig SM, Vadlamudi RK, Hurez VJ, Bahar R, Kious MJ, Livi CB, Wall SR et al. : B7-H1-dependent sex-related differences in tumor immunity and immunotherapy responses. J Immunol 2010, 185, 2747–2753. [Google Scholar] [CrossRef] [PubMed]
- Gubbels Bupp MR, Jorgensen TN: Androgen-Induced Immunosuppression. Front Immunol 2018, 9, 794. [CrossRef]
- Conforti, F.; Pala, L.; Bagnardi, V.; De Pas, T.; Martinetti, M.; Viale, G.; Gelber, R.D.; Goldhirsch, A. Cancer immunotherapy efficacy and patients' sex: a systematic review and meta-analysis. Lancet Oncol. 2018, 19, 737–746. [Google Scholar] [CrossRef]
- Bienz, M.; Saad, F. Androgen-deprivation therapy and bone loss in prostate cancer patients: a clinical review. BoneKEy Rep. 2015, 4, 716. [Google Scholar] [CrossRef]
- Hussain, A.; Tripathi, A.; Pieczonka, C.; Cope, D.; McNatty, A.; Logothetis, C.; Guise, T. Bone health effects of androgen-deprivation therapy and androgen receptor inhibitors in patients with nonmetastatic castration-resistant prostate cancer. Prostate Cancer Prostatic Dis. 2020, 24, 290–300. [Google Scholar] [CrossRef]
- Levine GN, D’Amico AV, Berger P, Clark PE, Eckel RH, Keating NL, Milani RV, Sagalowsky AI, Smith MR, Zakai N: Androgen-deprivation therapy in prostate cancer and cardiovascular risk: a science advisory from the American Heart Association, American Cancer Society, and American Urological Association: endorsed by the American Society for Radiation Oncology. CA Cancer J Clin 2010, 60, 194–201.
- Kim, J.; Freeman, K.; Ayala, A.; Mullen, M.; Sun, Z.; Rhee, J.-W. Cardiovascular Impact of Androgen Deprivation Therapy: from Basic Biology to Clinical Practice. Curr. Oncol. Rep. 2023, 25, 965–977. [Google Scholar] [CrossRef]
- Cattrini, C.; Caffo, O.; De Giorgi, U.; Mennitto, A.; Gennari, A.; Olmos, D.; Castro, E. Apalutamide, Darolutamide and Enzalutamide for Nonmetastatic Castration-Resistant Prostate Cancer (nmCRPC): A Critical Review. Cancers 2022, 14, 1792. [Google Scholar] [CrossRef]
- Robert C, Lebbé C, Lesimple T, Lundström E, Nicolas V, Gavillet B, Crompton P, Baroudjian B, Routier E, Lejeune FJ: Phase I Study of Androgen Deprivation Therapy in Combination with Anti–PD-1 in Melanoma Patients Pretreated with Anti–PD-1. Clinical Cancer Research 2023, 29, 858–865. [CrossRef]
- Ager CR, Obradovic A, McCann P, Chaimowitz M, Wang ALE, Shaikh N, Shah P, Pan S, Laplaca CJ, Virk RK et al.: Neoadjuvant androgen deprivation therapy with or without Fc-enhanced non-fucosylated anti-CTLA-4 (BMS-986218) in high risk localized prostate cancer: a randomized phase 1 trial. medRxiv 2024.
- Fang, Q.; Cole, R.N.; Wang, Z. Mechanisms and targeting of proteosome-dependent androgen receptor degradation in prostate cancer. 2022, 10, 366–376.
- Mannion, J.; Gifford, V.; Bellenie, B.; Fernando, W.; Garcia, L.R.; Wilson, R.; John, S.W.; Udainiya, S.; Patin, E.C.; Tiu, C.; et al. A RIPK1-specific PROTAC degrader achieves potent antitumor activity by enhancing immunogenic cell death. Immunity 2024, 57, 1514–1532.e15. [Google Scholar] [CrossRef]
- Tiemann K, Rossi JJ: RNAi-based therapeutics-current status, challenges and prospects. EMBO Mol Med 2009, 1, 142–151. [CrossRef]
- Solomon ZJ, Mirabal JR, Mazur DJ, Kohn TP, Lipshultz LI, Pastuszak AW: Selective Androgen Receptor Modulators: Current Knowledge and Clinical Applications. Sex Med Rev 2019, 7, 84–94. [CrossRef]
- Narayanan R, Coss CC, Dalton JT: Development of selective androgen receptor modulators (SARMs). Mol Cell Endocrinol 2018, 465, 134–142. [CrossRef] [PubMed]
- Gao W, Kearbey JD, Nair VA, Chung K, Parlow AF, Miller DD, Dalton JT: Comparison of the Pharmacological Effects of a Novel Selective Androgen Receptor Modulator, the 5α-Reductase Inhibitor Finasteride, and the Antiandrogen Hydroxyflutamide in Intact Rats: New Approach for Benign Prostate Hyperplasia. Endocrinology 2004, 145, 5420–5428.
- Dalton JT, Barnette KG, Bohl CE, Hancock ML, Rodriguez D, Dodson ST, Morton RA, Steiner MS: The selective androgen receptor modulator GTx-024 (enobosarm) improves lean body mass and physical function in healthy elderly men and postmenopausal women: results of a double-blind, placebo-controlled phase II trial. J Cachexia Sarcopenia Muscle 2011, 2, 153–161.
- Basaria S, Collins L, Dillon EL, Orwoll K, Storer TW, Miciek R, Ulloor J, Zhang A, Eder R, Zientek H et al. : The safety, pharmacokinetics, and effects of LGD-4033, a novel nonsteroidal oral, selective androgen receptor modulator, in healthy young men. J Gerontol A Biol Sci Med Sci 2013, 68, 87–95. [Google Scholar] [CrossRef]
- Narayanan R, Mohler ML, Bohl CE, Miller DD, Dalton JT: Selective androgen receptor modulators in preclinical and clinical development. Nucl Recept Signal 2008, 6, e010.
- El Sharouni MA, Witkamp AJ, Sigurdsson V, van Diest PJ, Louwman MWJ, Kukutsch NA: Sex matters: men with melanoma have a worse prognosis than women. J Eur Acad Dermatol Venereol 2019, 33, 2062–2067. [CrossRef]
| Mechanism | Implication |
|---|---|
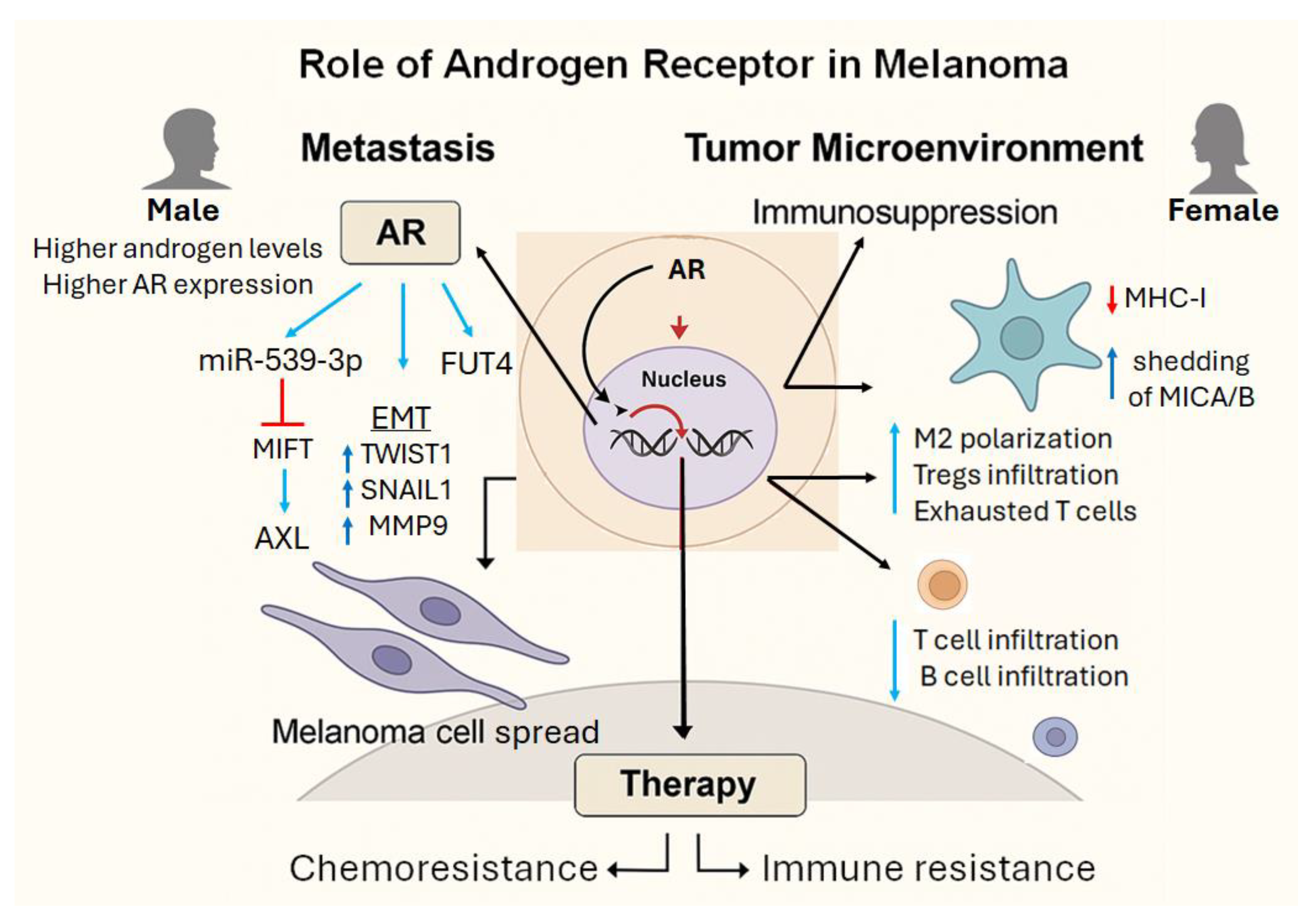
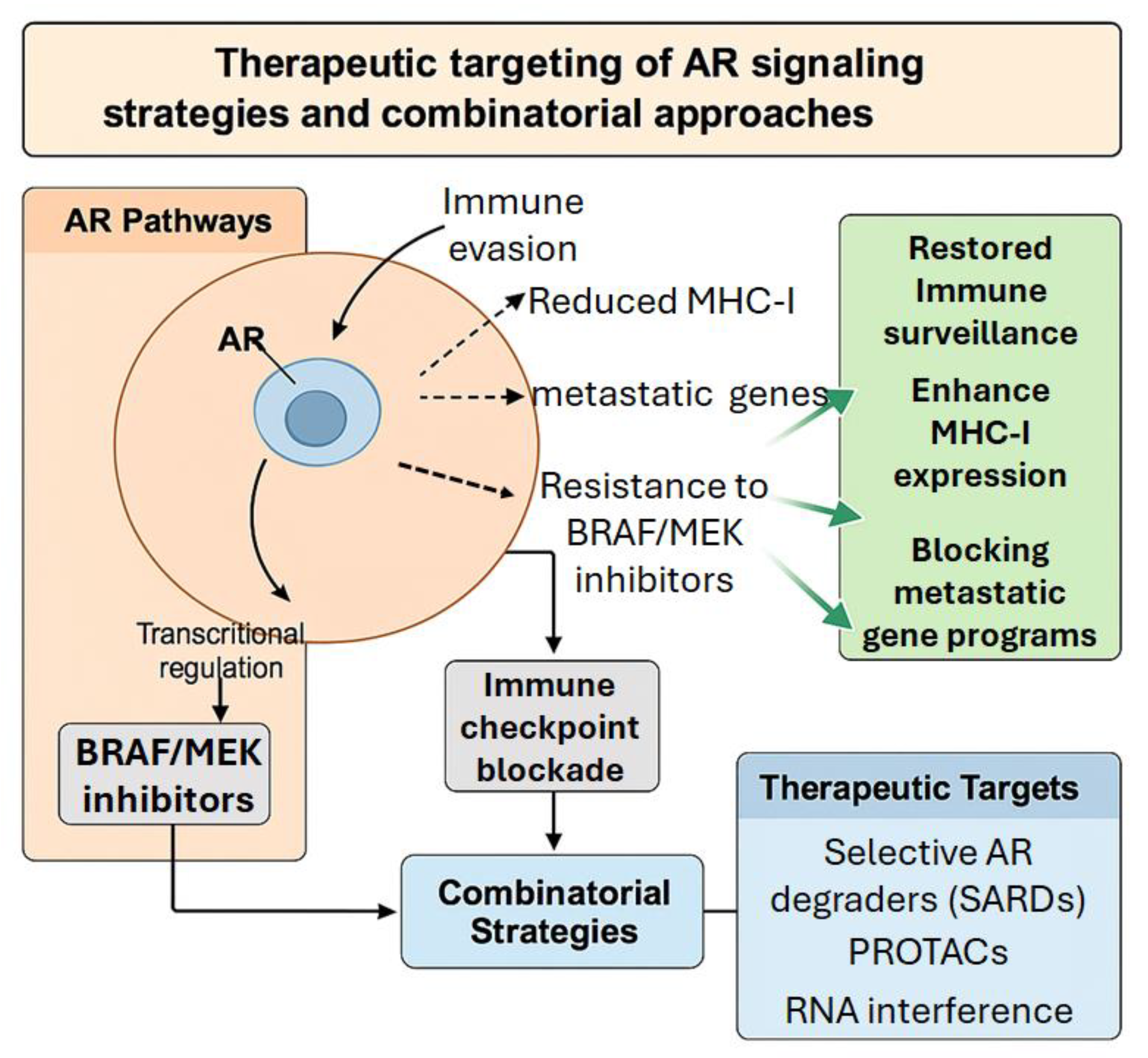
| Metastasis Promotion | AR enhances melanoma cell invasiveness by disrupting cell adhesion (e.g., FUT4-mediated junctions) and degrading MITF, a key factor in the melanoma lineage [12]. |
| Immunosuppression | AR signaling promotes immune evasion by facilitating MICA shedding and upregulating immune checkpoint molecules [42,46,49]. |
| Therapy Resistance | AR activity contributes to resistance against chemotherapy, targeted therapies, and immunotherapy [7,58]. AR blockade has been shown to restore sensitivity to treatment [12]. |
| TME Reprogramming | AR modulates the tumor microenvironment (TME) by recruiting immunosuppressive cells such as MDSCs and Tregs and altering the expression of key cytokines and chemokines [39]. |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




