Submitted:
20 July 2025
Posted:
21 July 2025
Read the latest preprint version here
Abstract
Keywords:
1. Introduction
2. Materials and Methods
3. Results
Etiology and Pathogenesis
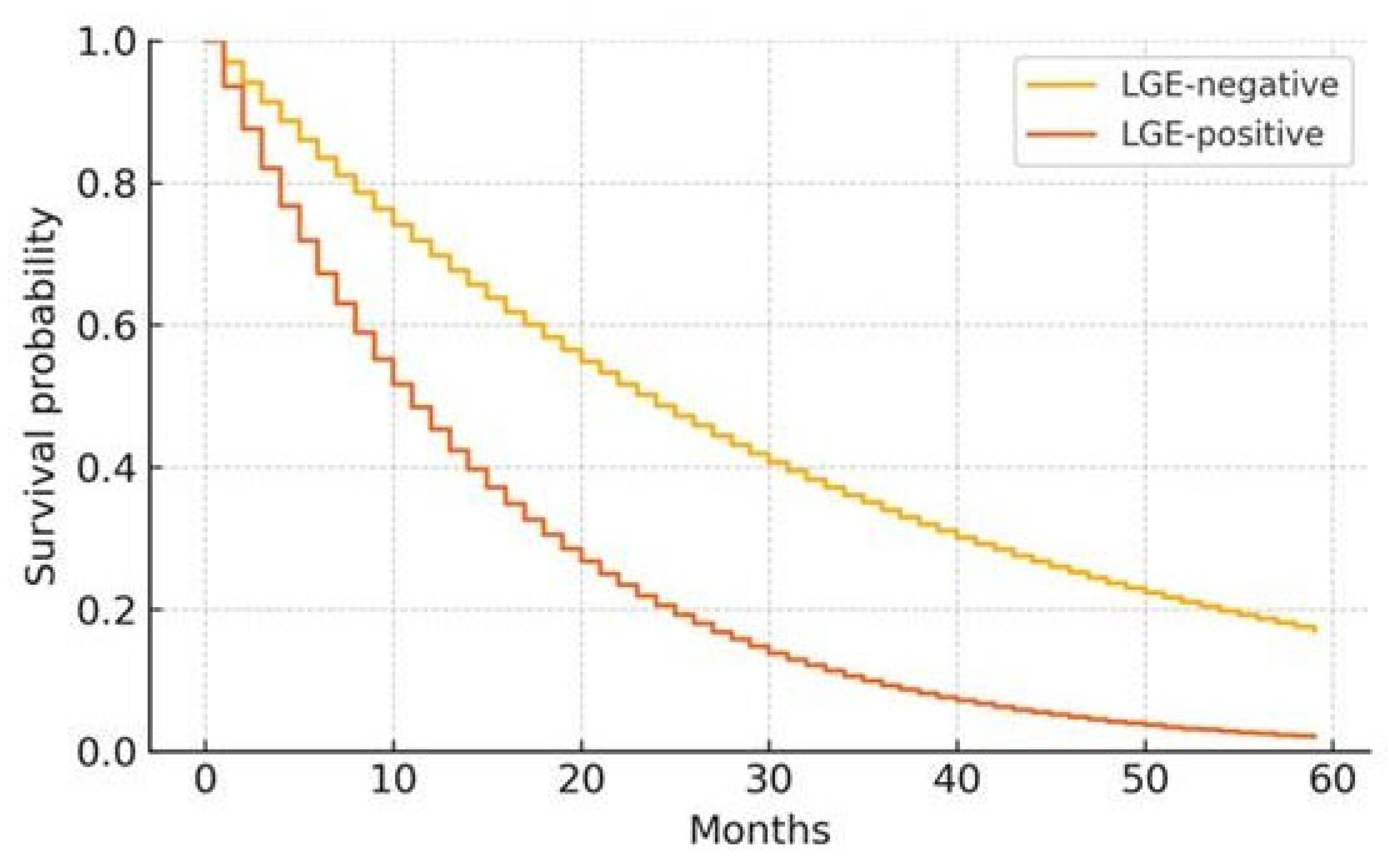
Clinical Presentation and Prognosis
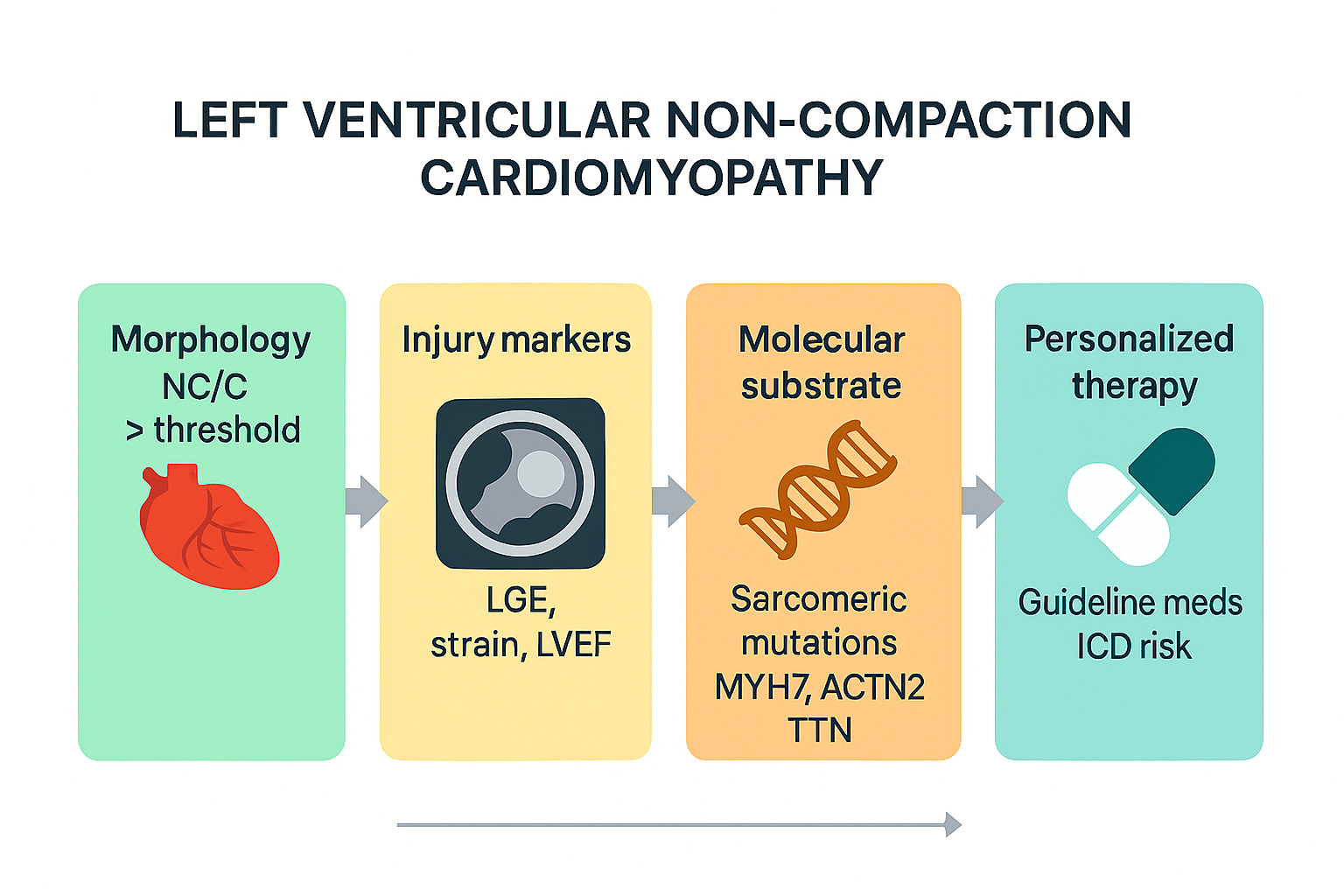
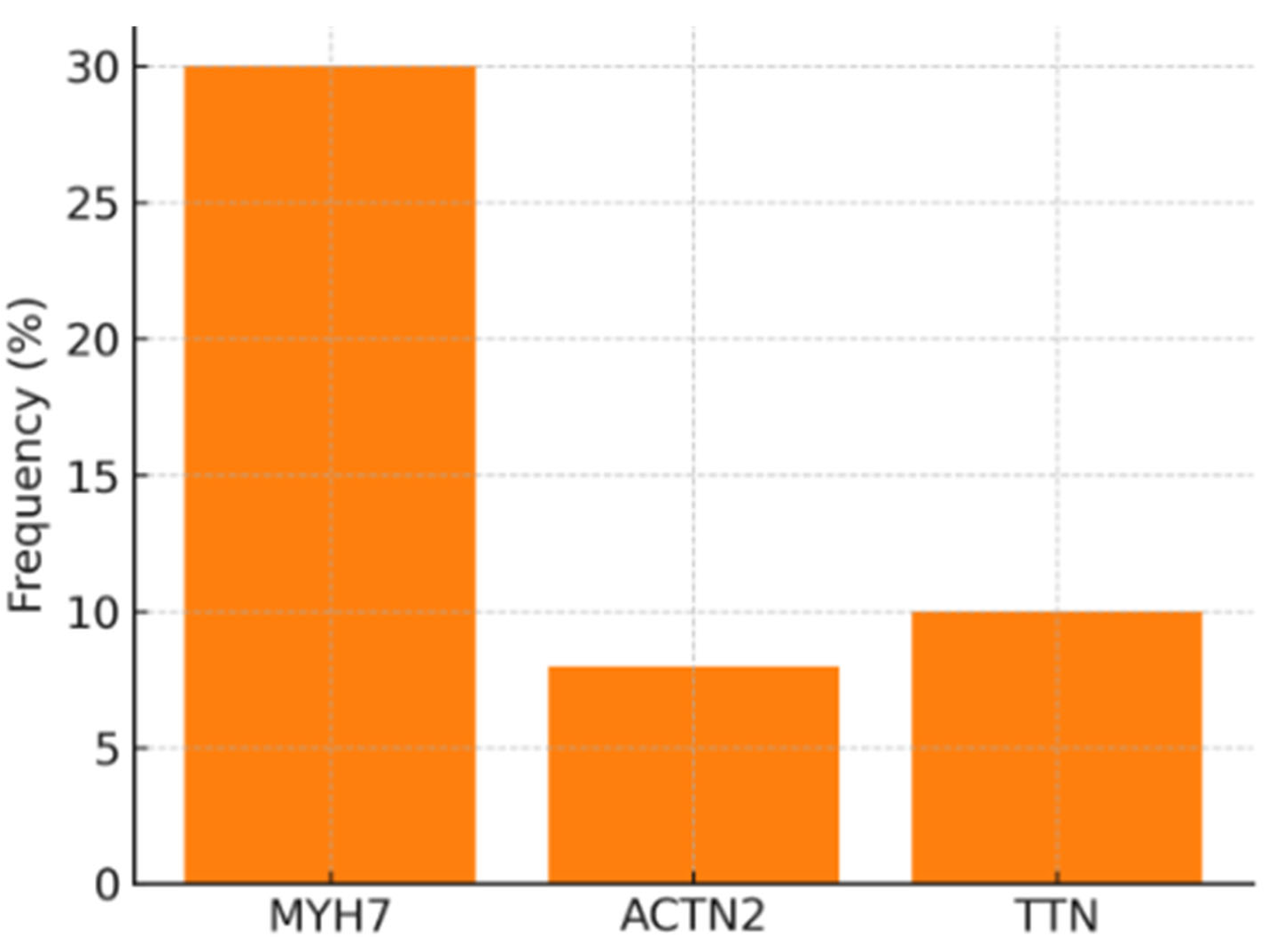
Personalized-Risk Stratification and Genotype–Phenotype Correlations
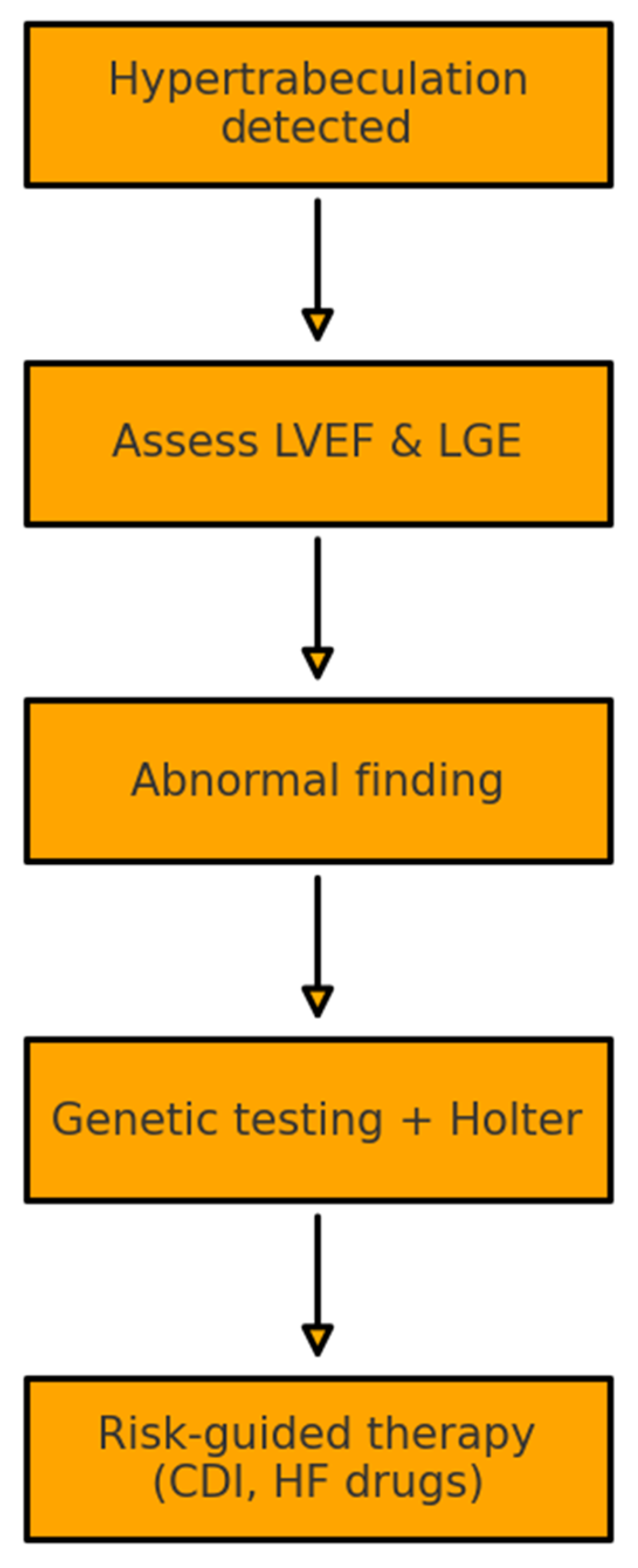
Diagnostic Methodology
- Chin criterion, based on an X/Y ratio ≤ 0.5 in diastole [1];
- Jenni criterion, pathological when a non-compacted/compacted (NC/C) ratio > 2 in systole [2];
- Stöllberger criterion, which diagnoses the disease when three or more prominent trabeculae with inter-trabecular perfusion are seen and an NC/C ratio > 2 [14].
Differential Diagnosis
Treatment
- Only annual follow-up with high-resolution imaging and Holter monitoring is advised. Retrospective cohorts show a low event rate with this strategy.
-
Introduce the “quadruple therapy”:.
- −
- ACEi or ARB or sacubitril–valsartan.
- −
- Beta-blocker.
- −
- Mineralocorticoid-receptor antagonist.
- −
- SGLT2 inhibitor.
- These recommendations are extrapolated from dilated-cardiomyopathy trials and supported by prospective NCC series.
- Prophylactic ICD implantation, as endorsed by the ESC heart-failure guidelines.
- Add CRT, which observational studies show improves reverse remodelling and functional capacity.
-
Long-term anticoagulation is mandatory:.
- −
- Prefer DOACs.
- −
- Reserve warfarin (VKA) for documented apical thrombus.
Device and Interventional Indications:
- LVEF ≤ 35 % or sustained VT justifies prophylactic ICD implantation.
- A wide QRS complex (≥ 130 ms) may benefit from CRT.
- Atrial fibrillation or a prior embolic event requires lifelong anticoagulation, preferably with direct oral anticoagulants.
Advanced Options:
- Surgery: Apical trabecular resection, with ≈10-point LVEF improvement at one year.
- Ablation: Reduces sustained-VT recurrence to 18 % at 3 years.
- Left-ventricular assist device: Bridge to transplant with 82 % one-year survival, without complications attributable to hyper-trabeculation.
- Gene therapies: Adeno-associated vectors (e.g., targeting MYBPC3 or TTN) normalized cardiac morphology in murine models; RNA-interference silencing is at pre-clinical stage.
Follow-Up and Lifestyle:
- Control: Every six months in the first year, then annually, with echocardiography/CMR, Holter, and NT-proBNP (if LVEF > 50 %).
-
Exercise:
- o
- Recreational—moderate intensity; contraindicated if fibrosis or arrhythmias are present.
- o
- Competitive—only with normal LVEF and exercise test free of VT.
- o
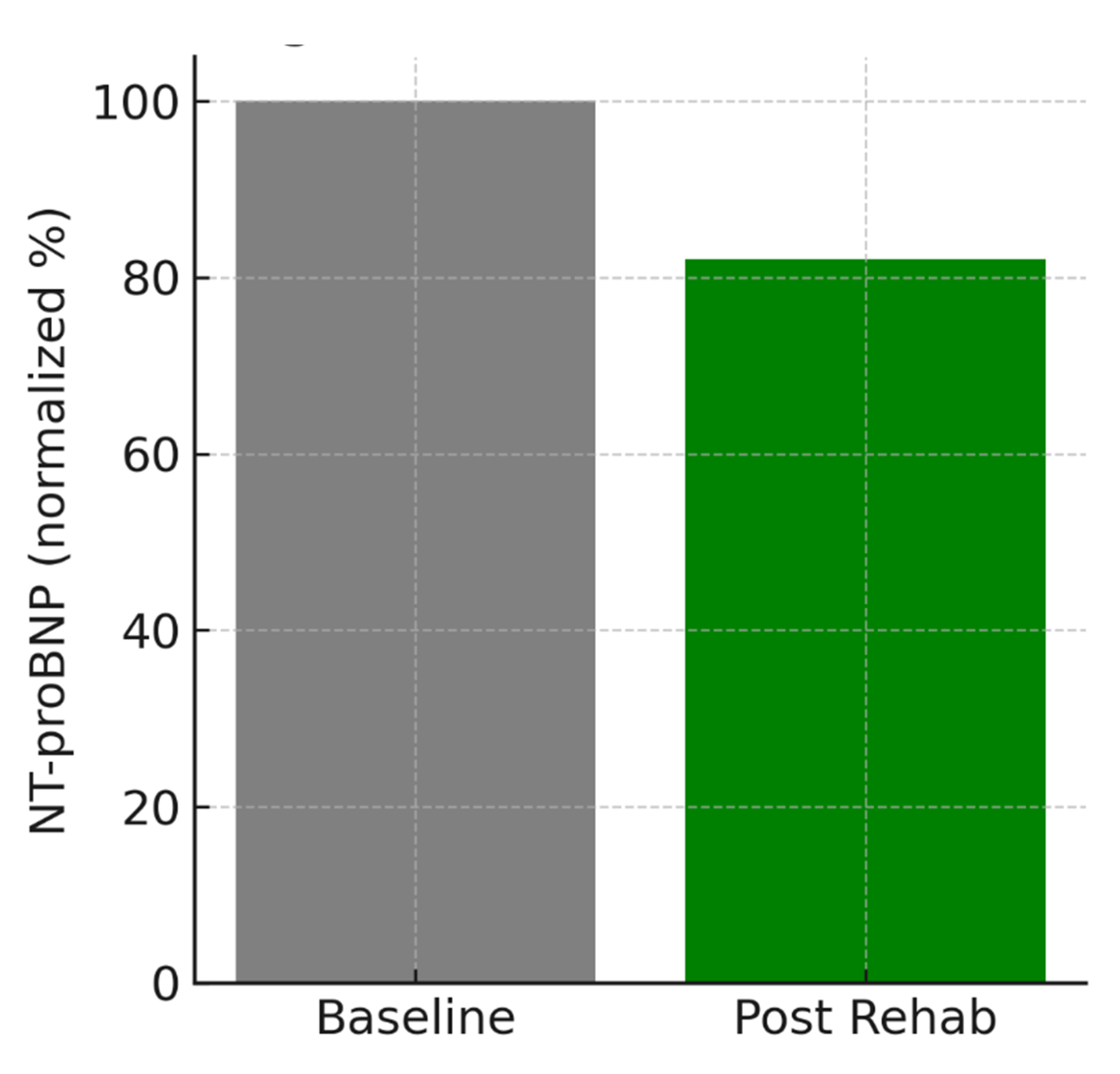
- Cardiac rehabilitation—12-week programs (60–70 % of maximal HR) improve VO2-peak by 2.1 mL/kg/min and reduce NT-proBNP by 18 %.
- Tele-monitoring improves clinical follow-up: wearable photoplethysmography detects AF with 93 % sensitivity, and remote weight and blood-pressure monitoring reduces heart-failure admissions by 22 %. In the near future, integrated algorithms combining AI, CMR T1/T2 maps, and omics profiles will predict early decompensation.
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Informed Consent Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| LVNC | Left-ventricular non-compaction cardiomyopathy |
| CMR | Cardiac magnetic resonance |
| LGE | Late gadolinium enhancement |
| LVEF | Left-ventricular ejection fraction |
| ICD | Implantable cardioverter-defibrillator |
| CRT | Cardiac resynchronisation therapy |
| SGLT2i | Sodium–glucose co-transporter-2 inhibitor |
| DCM | Dilated cardiomyopathy |
| HCM | Hypertrophic cardiomyopathy |
| NC/C | Non-compacted/compacted ratio |
| NT-proBNP | N-terminal pro-B-type natriuretic peptide |
References
- Chin, T.K.; Perloff, J.K.; Williams, R.G.; Jue, K.; Mohrmann, R. Isolated noncompaction of left ventricular myocardium: A study of eight cases. Circulation 1990, 82, 507–513. [Google Scholar] [CrossRef] [PubMed]
- Jenni, R.; Oechslin, E.; Schneider, J.; Attenhofer Jost, C.; Kaufmann, P.A. Echocardiographic and pathoanatomical characteristics of isolated left ventricular non-compaction: A step towards classification as a distinct cardiomyopathy. Heart 2001, 86, 666–671. [Google Scholar] [CrossRef] [PubMed]
- Petersen, S.E.; Selvanayagam, J.B.; Wiesmann, F.; Robson, M.D.; Francis, J.M.; Anderson, R.H.; et al. Left ventricular non-compaction: Insights from cardiovascular magnetic resonance imaging. J. Am. Coll. Cardiol. 2005, 46, 101–105. [Google Scholar] [CrossRef] [PubMed]
- Jacquier, A.; Thuny, F.; Jop, B.; Giorgi, R.; Cohen, F.; Gaubert, J.Y.; et al. Measurement of trabeculated left ventricular mass using cardiac MRI in the diagnosis of left ventricular non-compaction. Eur. Heart J. 2010, 31, 1098–1104. [Google Scholar] [CrossRef] [PubMed]
- Oechslin, E.N.; Attenhofer Jost, C.H.; Rojas, J.R.; Kaufmann, P.A.; Jenni, R. Long-term follow-up of adults with isolated left ventricular non-compaction. J. Am. Coll. Cardiol. 2000, 36, 493–500. [Google Scholar] [CrossRef] [PubMed]
- Habib, G.; Charron, P.; Eicher, J.C.; Giorgi, R.; Baron, O.; Jondeau, G.; et al. Isolated left ventricular non-compaction in adults: Clinical and echocardiographic features in 105 patients. Eur. J. Heart Fail. 2011, 13, 177–185. [Google Scholar] [CrossRef] [PubMed]
- Lofiego, C.; Biagini, E.; Pasquale, F.; Ferlito, M.; Rocchi, G.; Perugini, E.; et al. Wide spectrum of presentation and variable outcomes of isolated left ventricular non-compaction. Heart 2007, 93, 65–71. [Google Scholar] [CrossRef] [PubMed]
- Grigoratos, C.; Barison, A.; Ivanov, A.; Andreini, D.; Amzulescu, M.S.; Mazurkiewicz, L.; et al. Prognostic role of late gadolinium enhancement and global systolic impairment in left ventricular non-compaction: A meta-analysis. JACC Cardiovasc. Imaging 2019, 12, 2141–2151. [Google Scholar] [CrossRef] [PubMed]
- Vaidya, V.R.; Kowlgi, G.N.; Greason, K.L.; Lyle, M.P.; Dearani, J.A.; Nishimura, R.A.; et al. Long-term survival of patients with left ventricular non-compaction. J. Am. Heart Assoc. 2021, 10, e020349. [Google Scholar] [CrossRef] [PubMed]
- Casas G, Limeres J, Oristrell G, Gutierrez-Garcia L, Andreini D, Borregan M, et al. Clinical risk prediction in patients with left-ventricular myocardial non-compaction. Journal of the American College of Cardiology. 2021;78(7):643-662.
- Towbin, J.A.; Lorts, A.; Jefferies, J.L. Left ventricular non-compaction cardiomyopathy. Lancet 2015, 386, 813–825. [Google Scholar] [CrossRef] [PubMed]
- Ross, S.B.; Jones, K.; Blanch, B.; Barratt, A.; Semsarian, C.; Ingles, J. Prevalence of left ventricular non-compaction in adults: A systematic review and meta-analysis. Eur. Heart J. 2020, 41, 1428–1436. [Google Scholar] [CrossRef] [PubMed]
- Mazzarotto F, Hawley MH, Beltrami M, Beekman L, de Marvao A, McGurk KA, et al. Systematic large-scale assessment of the genetic architecture of left ventricular noncompaction reveals diverse etiologies. Genet Med. 2021;23(5):856–864.
- Aras, D.; Tufekcioglu, O.; Ergun, K.; Ozeke, O.; Yildiz, A.; Topaloglu, S.; et al. Clinical features of isolated ventricular non-compaction in adults: Long-term clinical course and predictors of left ventricular failure. J. Card. Fail. 2006, 12, 726–733. [Google Scholar] [CrossRef] [PubMed]
- Kohli, S.K.; Pantazis, A.A.; Shah, J.S.; Adeyemi, B.; Robinson, S.; McKenna, W.J.; et al. Diagnosis of left-ventricular non-compaction in patients with left-ventricular systolic dysfunction: Time for a reappraisal of diagnostic criteria? Eur. Heart J. 2008, 29, 89–95. [Google Scholar] [CrossRef] [PubMed]
- Casas G, Rodríguez-Palomares JF, Ferreira-González I. Left ventricular noncompaction: a disease or a phenotypic trait? Revista Española de Cardiología. 2022;75(12):1059-1069. [CrossRef]
- Gerecke, G.; Engberding, R. Left ventricular non-compaction: Genesis, diagnosis, prognosis, therapy. J. Clin. Med. 2021, 10, 2457.
- Ogah OS, Iyawe EP, Okwunze KF, Nwamadiegesi CA, Obiekwe FE, Fabowale MO, et al. Left ventricular noncompaction cardiomyopathy: a scoping review. Ann Ib Postgrad Med. 2023;21(2):8–16.
- Huang W, Sun R, Liu W, Xu R, Zhou Z, Bai W, et al. Prognostic Value of Late Gadolinium Enhancement in Left Ventricular Noncompaction: A Multicenter Study. Diagnostics. 2022;12(10):2457.
- Zhou Z-Q, He W-C, Li X, Bai W, Huang W, Hou R-L, Wang Y-N, Guo Y-K. Comparison of cardiovascular magnetic resonance characteristics and clinical prognosis in left ventricular non-compaction patients with and without arrhythmia. BMC Cardiovascular Disorders. 2022;22(1):25.
- Vershinina T, Fomicheva Y, Muravyev A, Jorholt J, Kozyreva A, Kiselev A, et al. Genetic Spectrum of Left Ventricular Non-Compaction in Paediatric Patients. Cardiology. 2020;145(11):746-756.
- Izquierdo C, Casas G, Martin-Isla C, Campello VM, Guala A, Gkontra P, Rodríguez-Palomares JF, Lekadir K. Radiomics-Based Classification of Left Ventricular Non-Compaction, Hypertrophic Cardiomyopathy, and Dilated Cardiomyopathy in Cardiovascular Magnetic Resonance. Front Cardiovasc Med. 2021;8:764312.
- Akhan O, Demir E, Dogdus M, Ozerkan Cakan F, Nalbantgil S. Speckle Tracking Echocardiography and Left Ventricular Twist Mechanics: Predictive Capabilities for Non-Compaction Cardiomyopathy in First-Degree Relatives. Int J Cardiovasc Imaging. 2021;37(2):429-438.
- Rojanasopondist P, Nesheiwat L, Piombo S, Porter GA Jr, Ren M, Phoon CKL. Genetic basis of left ventricular noncompaction. Circ Genom Precis Med. 2022;15(3):e003517.
- Huttin O, Venner C, Frikha Z, Voilliot D, Marie P-Y, Aliot E, et al. Myocardial deformation pattern in left-ventricular non-compaction: comparison with dilated cardiomyopathy. IJC Heart & Vessels. 2014;5:9-14.
- Shi WY, Moreno-Betancur M, Nugent AW, Cheung M, Colan SD, Turner C, et al. Long-Term Outcomes of Childhood Left Ventricular Non-Compaction Cardiomyopathy: Results From a National Population-Based Study. Circulation. 2018;138(4):367-376.
- Jacquier A, Thuny F, Jop B, Giorgi R, Cohen F, Gaubert J-Y, et al. Measurement of trabeculated left-ventricular mass using cardiac MRI in the diagnosis of left-ventricular non-compaction. European Heart Journal. 2010;31(9):1098-1104.
- Wilde AAM, Semsarian C, Márquez MF, Shamloo AS, Ackerman MJ, Ashley EA, et al. European Heart Rhythm Association (EHRA)/Heart Rhythm Society (HRS)/Asia Pacific Heart Rhythm Society (APHRS)/Latin American Heart Rhythm Society (LAHRS) Expert Consensus Statement on the State of Genetic Testing for Cardiac Diseases. Heart Rhythm. 2022;19(7):e1-e60.
- de la Chica JA, Gómez-Talavera S, García-Ruiz JM, et al. Association Between Left Ventricular Non-compaction and Vigorous Physical Activity. Journal of the American College of Cardiology. 2020;76(15):1723-1733.
- Hirono K, Takarada S, Miyao N, Nakaoka H, Ibuki K, Ozawa S, Origasa H, Ichida F. Thromboembolic events in left-ventricular non-compaction: comparison between children and adults — a systematic review and meta-analysis. Open Heart. 2022;9(1):e001908.
- McDonagh, T.A.; Metra, M.; Adamo, M.; et al. 2021 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure. Eur. Heart J. 2021, 42, 3599–3726. [Google Scholar] [CrossRef] [PubMed]
- Inglis, S.C.; Conway, A.; Cleland, J.G.F.; et al. Remote monitoring to reduce hospitalizations in heart failure: An updated meta-analysis. Eur. Heart J. 2016, 37, 3144–3151. [Google Scholar]
- Perez MV, Mahaffey KW, Hedlin H, Rumsfeld JS, Garcia A, et al. Large-scale assessment of a smartwatch to identify atrial fibrillation. New England Journal of Medicine. 2019;381(20):1909-1917.
- Varasteh Z, Mohanta S, Robu S, Braeuer M, Li Y, Omidvari N, et al. Molecular imaging of fibroblast activity after myocardial infarction using a ^68Ga-labeled fibroblast-activation protein inhibitor (FAPI-04). Journal of Nuclear Medicine. 2019;60(12):1743-1749.
- Fatkin D, Calkins H, Elliott P, et al. Contemporary and future approaches to precision medicine in inherited cardiomyopathies. J Am Coll Cardiol. 2021;77(20):2551-2572.
- Mayourian J, Asztalos IB, El-Bokl A, Lukyanenko P, Kobayashi RL, La Cava WG, et al. Electrocardiogram-based deep learning to predict left-ventricular systolic dysfunction in paediatric and adult congenital heart disease: a multicentre modelling study. Lancet Digital Health. 2025;7(4):e264-e274.
- Grebur K, Mester B, Fekete BA, et al. Genetic, clinical and imaging implications of a non-compaction phenotype population with preserved ejection fraction. Front Cardiovasc Med. 2024;11:1337378.
- Sethi Y, Patel N, Kaka N, et al. Precision medicine and the future of cardiovascular diseases: a clinically oriented comprehensive review. J Clin Med. 2023;12(5):1799.
- Pittorru R, Corrado D. Left ventricular non-compaction: evolving concepts. J Clin Med. 2024;13(19):5674.
| Situation | Strategy | Evidence |
|---|---|---|
|
LVEF > 50 % and asymptomatic |
Annual review with echocardiography or CMR and Holter monitoring | Retrospective cohorts |
| Heart failure | Quadruple therapy (ACE-I or ARB or sacubitril-valsartan + β-blocker + mineralocorticoid-receptor antagonist + SGLT2 inhibitor) | Prospective series |
| LVEF ≤ 35 % or sustained VT | Prophylactic implantable cardioverter-defibrillator (ICD) | ESC Guidelines |
| QRS ≥ 130 ms | Cardiac resynchronisation therapy (CRT) | Observational studies |
| Atrial fibrillation or prior embolism | Direct oral anticoagulant (vitamin-K antagonist if apical thrombus) | Systematic reviews |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).




