1. Introduction
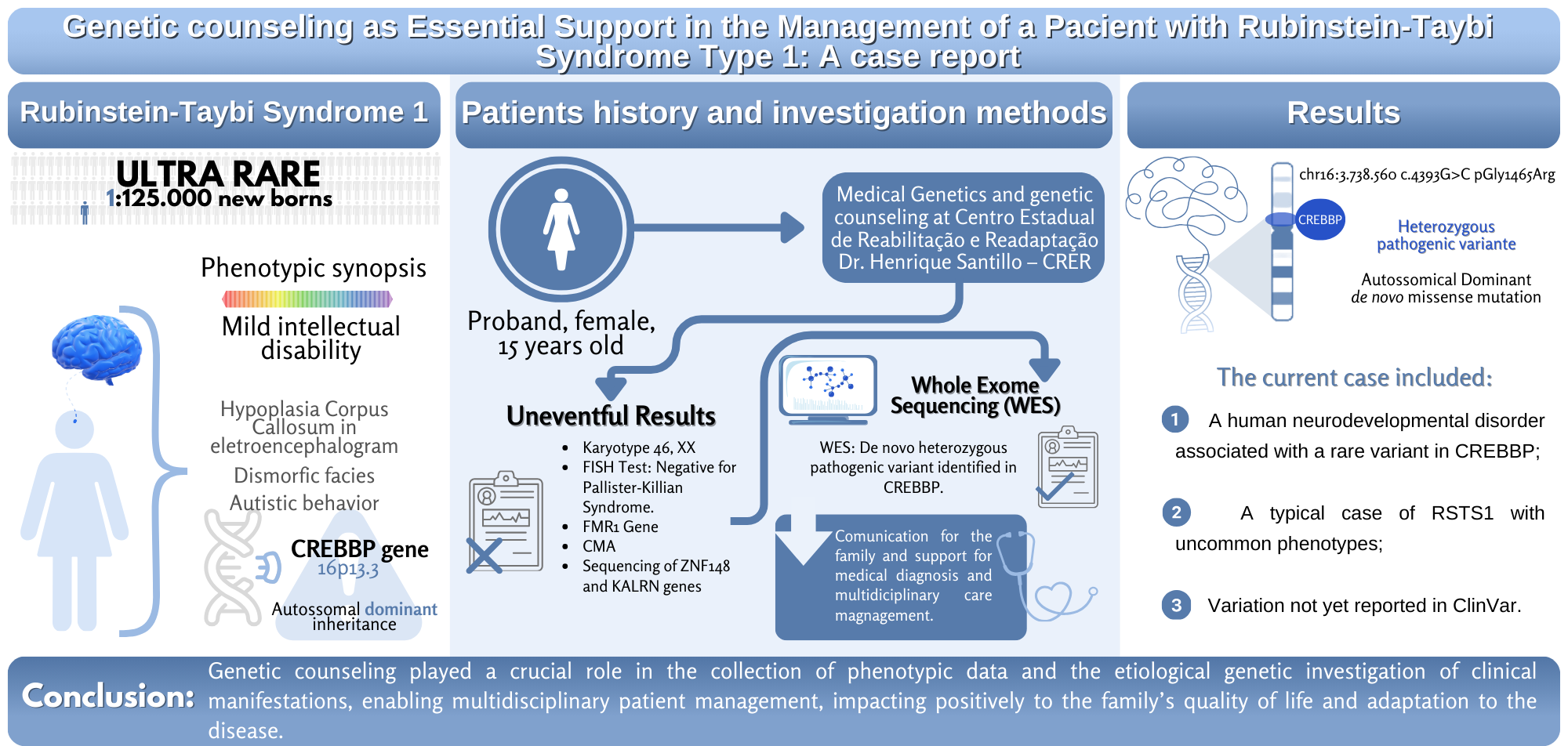
Rubinstein-Taybi Syndrome (RSTS; OMIM #180849; OMIM #613684) is an ultrarare genetic disorder associated with multiple congenital anomalies and neurodevelopmental disorders, with an incidence of 1:100,000–125,000 live births. The main clinical phenotypes of RSTS include short stature, facial dysmorphisms, broad thumbs and halluces, polydactyly, palpebral fissures, low columella, high-arched palate, mask-like face, talon cusps, ptosis, and epicanthus [
1]. Individuals with RSTS may present phenotypic variability, particularly regarding the degree of multisystemic involvement, which can affect the respiratory, cardiac, genitourinary, ocular, auditory, orthopedic, endocrine, neurological, dental, and cutaneous systems. Additionally, individuals affected by RSTS exhibit a predisposition to the proliferation of benign tumors [
1,
2,
3,
4]. Neurological involvement in RSTS is evident, with highly variable phenotypic features among patients. These include global developmental delay (GDD), moderate to severe intellectual disability (ID), with an intelligence quotient (IQ) ranging from 35–50, autistic behavior, hypotonia, hyperreflexia, electroencephalogram abnormalities, and agenesis of the corpus callosum. Moreover, psychiatric disorders are frequently observed in RSTS patients, including attention deficit hyperactivity disorder (ADHD), good social interaction, and emotional lability [
4]. The inheritance pattern of RSTS is autosomal dominant, with 99% of reported cases involving de novo mutations in two genes: CREBBP (RSTS1; OMIM 600140) and EP300 (RSTS2; OMIM 602700). The CREBBP gene is located on cytoband 16p13.3 and encodes the CREB Binding Protein (CBP) (NM_600140). The EP300 gene is located in region 22q13 and encodes the EA1 Binding Protein p300 or p300 (NM_602700). These two genes are similar in function and biological importance. Both are ubiquitously expressed and regulate gene expression through their acetyltransferase activity. Functionally, CBP and p300 transfer acetyl groups (CH
3CO) to lysine residues on histones and other proteins. Histone acetylation opens chromatin, making it more accessible to the transcription machinery, while acetylation of transcription factors and regulatory proteins modulates their expression [
5,
6].
Interestingly, missense mutations involving the terminal portion of exon 30 and the beginning of exon 31 in both the CREBBP and EP300 genes are associated with a distinct phenotype, Menke-Hennekam syndrome. Individuals with Menke-Hennekam syndrome do not exhibit the characteristic facial features of RSTS or broad/angled thumbs and halluces. RSTS phenotypes show facial features including ptosis, telecanthus, short and upward-slanting palpebral fissures, depressed nasal bridge, short nose, anteverted nostrils, short columella, and a long philtrum. Other features include short stature, intellectual disability, microcephaly, feeding difficulties, seizures, autistic behavior, and variable additional manifestations [
7,
8,
9]. A search conducted in March 2024 in the DECIPHER database identified 165 reported cases of mutations involving CREBBP and 122 involving EP300, without specifying the phenotypes (RSTS1, RSTS2, or Menke-Hennekam) associated with these mutations [
10].
In 2010, RSTS1 represented approximately 50–70% of RSTS cases, while RSTS2 accounted for only 3%, often associated with de novo variants. However, to date, approximately 600 individuals with pathogenic variants in the CREBBP and EP300 genes have been reported [
11,
12,
13,
14]. Generally, mutations involving CREBBP, related to the RSTS1 subtype, are not only more frequent but also have a more critical impact on development, resulting in a more severe phenotype compared to the RSTS2 subtype. Exclusive manifestations of RSTS1 include congenital heart disease, genitourinary abnormalities, recurrent respiratory infections, ophthalmological complications, and skeletal malformations [
1,
10].
Genetic counseling for families of RSTS patients is essential, as it assists with genetic diagnosis, identifies phenotypic variability, assesses and discusses the risk of transmission to offspring, and provides valuable and necessary guidance regarding surveillance and multidisciplinary care required for managing RSTS complications [
15]. In this context, the present study aims to report a case of RSTS1 addressed in the genetic counseling process, describing its genotypic-phenotypic correlations and the patient’s clinical peculiarities. The description of rare cases is crucial for a better understanding of patient prognosis, inheritance patterns—which enable tailored genetic counseling for each family—treatment, follow-up, and case management, ultimately improving the quality of life for patients and their families.
2. Case Report
Female proband, 15 years old, from Goiânia, Central Brazil, was referred to the Genetic Counseling (GC) service at the State Center Rehabilitation and Readaptation (CRER) due to an undiagnosed rare disease presenting with multiple neurological abnormalities and some congenital malformations. The proband is the second child of non-consanguineous, healthy parents, aged 30 (mother) and 41 (father) at conception. In the preconception period, the parents experienced reproductive difficulties, leading them to seek assistance at a human reproduction clinic, although initially without success. Later, they managed to conceive naturally. During pregnancy, regular prenatal care was performed. All ultrasounds scheduled in the prenatal period were completed, with no clinically relevant findings. The mother took all the recommended prenatal vitamins. A single episode of maternal bleeding was recorded, which received appropriate medical treatment. There were no reports of infections, amniotic fluid loss, skin rashes, fever, maternal hypertension, or edema. The mother denied exposure to teratogenic agents during pregnancy. Fetal movements were noted around the 18th week; the fetus was not as active as in a previous pregnancy but continued to move until the end of the pregnancy. Maternal weight gain was 15 kg during gestation.
The proband was born at term at 39 weeks of gestation by cesarean delivery due to medical decision. At birth, her length was 47 cm (p.4%; -1.72 SD), weight 3,100 g (p.25%; -0.67 SD), and head circumference 35 cm (p.64%; +0.37 SD), with an Apgar score of 9/10. She delayed the newborn reflexive cry. The proband remained in the maternity ward for 3 days before discharged, and by the 5th day of life, she presented with myotonic reflexes that persisted for approximately 15 days. At that time, the parents sought pediatric neurology services. Subsequently, she exhibited significant delays in all developmental milestones, according to pediatric developmental standards. She experienced recurrent infantile ear and throat infections, as well as pneumonia, treated with antibiotics. Over time, the infections became less frequent. Pubertal development began, and menarche occurred at age 10. Currently, based on medical recommendations, menstrual suppression is currently achieved using a contraceptive implant to inhibit the menstrual cycle.
The child has good social interaction, good dietary acceptance, and relative independence for her daily life activities. She has cognitive challenges, particularly in reading, mathematics, and written expression. She demonstrated attachment to certain toys and objects, using them as elements of emotional security and comfort. During early adolescence, at the time of COVID-19 pandemics, she engaged in remote schooling but experienced regression in previously acquired skills, including delays in gross motor development and language acquisition. Additionally, she exhibited impaired social reciprocity, which contributed to the infantilization of her behavior.
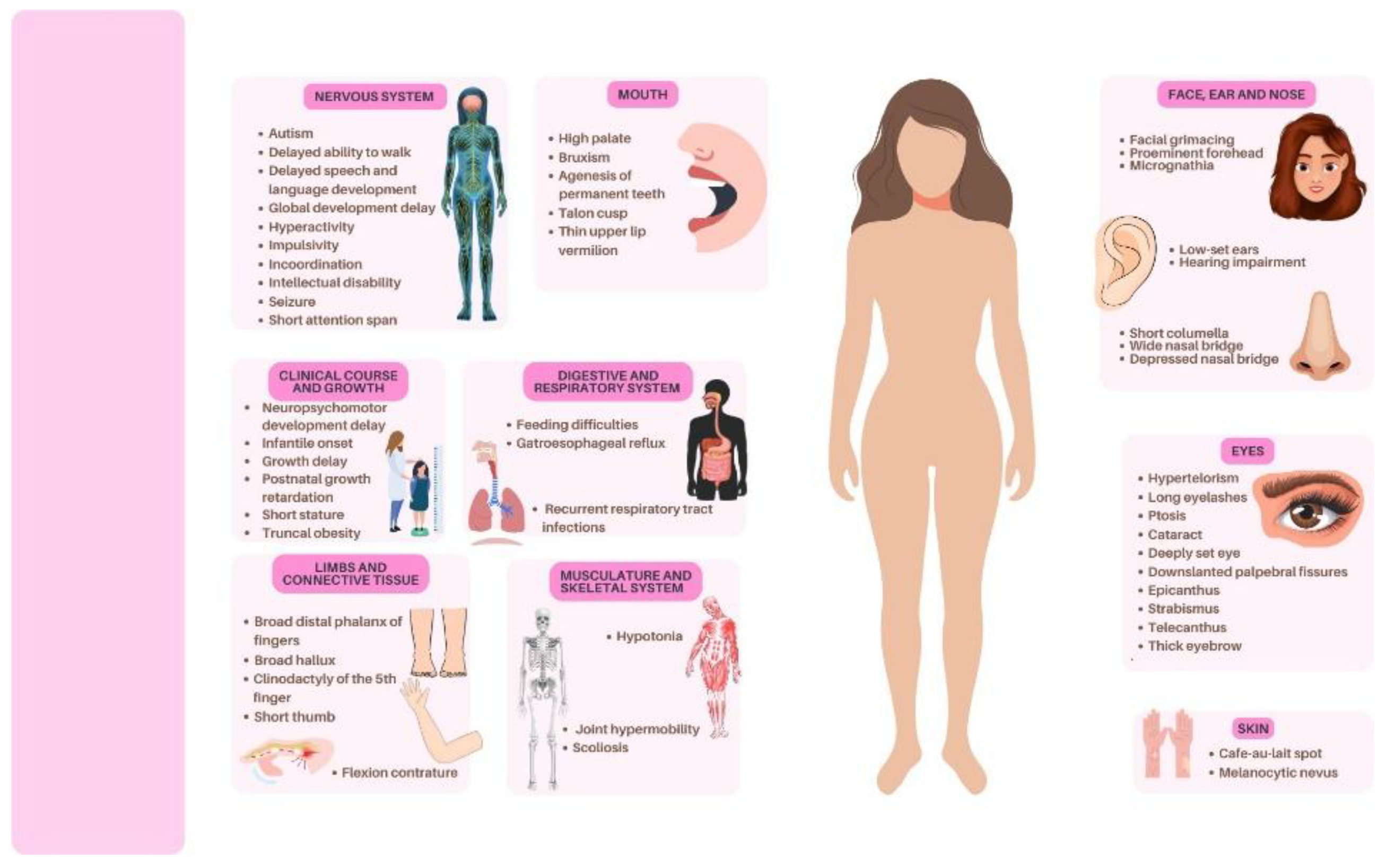
During case management and observation of complementary exams requested by the attending multidisciplinary team, several phenotypes were identified in the patient (
Figure 1). Facial features included ocular hypertelorism, strabismus, broad nasal base with depressed nasal bridge, high-arched palate, low-set ears, small mouth, prominent eyebrows, and mask-like face. Skin findings included melanocytic nevi, café-au-lait spots, atypical scarring, and keloid formation. Additionally, neurological abnormalities were identified, including bruxism, neuropsychomotor developmental delay, irritability, anxiety, attention deficit, hyperactivity, impulsivity, sibling-restricted aggressiveness, irrational fears, mood instability, repetitive questioning, agoraphobia, obsessive-compulsive disorder, onychophagia of hands and feet, and soliloquies.
A cranial MRI revealed a millimetric gap at the anterior extremity of the right caudate nucleus, along with a reduced hypotrophic encephalic volume. There was diffuse cortical hypotrophy atypical for her age, widening of the subarachnoid spaces in the middle cranial fossae and frontal convexities, and mild delays in cerebral myelination, including hypomyelination of the anterior limbs of the internal capsules. Moreover, there was a hypotrophic corpus callosum.
The patient’s autistic behavior was evident. In 2022, a behavioral assessment classified the patient with mild-to-moderate autism using the Childhood Autism Rating Scale 2 (CARS2, score = 30.5) and an age-compatible diagnosis of ≥10 years on the Autism Diagnostic Interview-Revised (ADI-R). Both tools highlighted qualitative impairments in social interaction and communication, along with restricted, repetitive, and stereotyped behavior patterns.
Skeletal abnormalities included pectus carinatum, joint hyperflexibility, short arms, broad fingers, micrognathia, bilateral clinodactyly of digitus minimus, along with short, broad toes. Radiography revealed humeral hypotrophy and cranial deformity with a hammered copper appearance. During childhood, the patient exhibited short stature for her age and underwent endocrinological treatment to delay the onset of puberty and promote growth, showing slow growth compared to children of the same age. At her last GC consultation, at age 16, the proband’s anthropometric measurements were: weight of 71 kg (p.94%; +1.60 SD), height of 160 cm (p.29%; -0.53 SD), and head circumference of 55 cm (p.40%; -0.2 SD).
The patient receives regular multidisciplinary follow-up, with weekly psychology and psychopedagogy sessions. This approach has maintained good behavior and peer interaction, although occasional agitation crises still occur. She continues with daily prescriptions of fluoxetine (20 mg) and sertraline (50 mg).
Based on the family history and phenotypic synopsis, several diagnostic hypotheses were proposed and subsequently evaluated through genetic testing, requested by the medical geneticist and the genetic counselor following parental consent (
Table 1).
WES preparation and enrichment were performed using the Illumina DNA Prep with Enrichment kit, and target region capture was carried out with the Twist Biosciences Custom V3 kit, including probes for all exonic and adjacent regions. WES was performed using the NovaSeq 6000 platform. DNA alignment was referenced against version GRCh38 of the human genome using the BWA-MEM program. A de novo heterozygous variant was identified at chr16:3,738,560 (NM_004380.3; c.4393G>C; p.Gly1465Arg) in the CREBBP gene. This resulted in the substitution of the amino acid glycine for arginine. The variant was classified as likely pathogenic (LP) according to the laboratory; however, the same variant has once been reported previously as pathogenic in the ClinVar database. Thus, phenotype and genotype contribute to close the proband’s diagnosis as Rubinstein-Taybi Syndrome 1 (OMIM #600140), ending a 15-year diagnostic odyssey for the family.
According to the family history, the proband represented a simplex case of an autosomal dominant inheritance, with unknown variant penetrance. To date, reported cases of RSTS1 have indicated high penetrance with variable expressivity, even in instances caused by sequence variants [
16]. The de novo variant observed in our patient had previously been reported only once in ClinVar as pathogenic. Although the variant observed in the proband and the one reported in ClinVar are located at the same position (c.4393), the nucleotide substitutions differ. The variant previously reported in ClinVar had a G>A substitution, while in the proband, a G>C substitution occurred. Despite this difference, both result in the same protein consequence (p.Gly1465Arg) due to the redundancy of the genetic code, thus sharing the same pathogenicity. Additionally, another variant has been reported in ClinVar in a nearby position (c.4394), which also results in the p.Gly1465Arg substitution. Therefore, this case represents the third worldwide report of an alteration involving position 1465 [
17]. Thus, we claim that sequence variants at the amino acid residue 1465 in CBP are deleterious to the protein’s functions and are associated with RSTS1. Therefore, laboratories should report it accordingly.
RSTS1 carriers rarely inherit the condition, as most affected individuals are simplex cases. However, this does not eliminate the possibility of parental germline mosaicism, which carries an empirical risk of <1% for siblings. It is recommended that this information be discussed during the genetic counseling process, particularly in situations where the parents express reproductive interest. For the case reported here, her parents denied reproductive interest for themselves and for their daughter. However, they expressed a desire to know the recurrence risk for their daughter’s offspring in the event of an unexpected future pregnancy. In this context, they were informed of a 50% transmission risk for the variant, corresponding to the Mendelian risk for autosomal dominant inheritance in heterozygosity [
15]. Due to the lack of reliable information regarding the penetrance of this variant, the family was informed that, if transmitted, the variant would manifest the RSTS1 phenotype in the carrier.
Surveillance and Care
Individuals with RSTS1 can present a wide range of associated comorbidities, such as cardiac problems, respiratory disorders, seizures, and a predisposition to infections. Therefore, medical surveillance must be comprehensive and multidisciplinary, with the goal of monitoring and managing the medical and progression aspects of the condition. Regular annual follow-up should include the following specialties: a). Pediatrics, with annual visits for complete physical examinations, growth monitoring, and evaluation of motor and cognitive development, including the management of the autistic behaviour; b). Dermatology, with annual consultations to monitor skin conditions; c). Cardiology, with yearly evaluations to detect and manage cardiac issues; d). Ophthalmology, due to the increased risk of glaucoma; e). Otolaryngology, to monitor potential hearing impairments; f). Nephrology, given the risk of renal abnormalities, including cysts development; g). Oral health should be monitored with a dentist consultations every 6 months to address orthodontic problems and manage conditions, such as bruxism.
Due to the vulnerability resulting from the gap between mental and chronological ages in these patients, a multidisciplinary approach is crucial. This includes regular follow-up with psychology, music therapy, occupational therapy, and speech therapy to support the patient’s overall development and address specific needs. Finally, genetic counseling plays a fundamental role in assisting with diagnosis, guiding medical and reproductive decisions, providing information on recurrence risks, and offering appropriate support to families.
With proper monitoring and multidisciplinary interventions, individuals with RSTS1 can achieve a life expectancy comparable to that of the general population. Furthermore, to ensure that patients and their families receive the necessary support, dedicated support groups can provide therapeutic guidance, specialized educational services, and family assistance. These initiatives significantly improve the quality of life and reduce the sense of isolation, often experienced due to the low prevalence of RSTS1 in the population.
3. Discussion
The proband exhibited multisystem impairments typical of the RSTS1, which can be explained by the multifaceted functions of the CBP protein. CBP acts as a transcriptional co-activator for various transcription factors, regulates gene expression through chromatin remodeling, and is essential for proper embryonic development by controlling cellular processes such as growth, differentiation, and homeostasis. CBP haploinsufficiency can result in significant phenotypic variability among carriers, as observed in our proband [
15,
18]. She presented four clinical phenotypes not included in the HPO syndromic spectrum for RSTS1, namely: melanocytic nevi, pectus carinatum, bruxism, and encephalic hypotrophy.
Regarding the spectrum of mutations in the CREBBP gene associated with RSTS1, among the 165 reported cases of the syndrome in the DECIPHER database, 68 out of 165 (41.2%) corresponded to single nucleotide variants (SNVs), and 95 out of 165 (58.8%) were copy number variants (CNVs). Additionally, SNVs and CNVs are of de novo origin in 63% and 36% of cases, respectively. Large CNVs are often inherited (27%) from parents carrying balanced rearrangements [
10]. The present case is characterized by a de novo SNV, which corresponds to the smaller portion of the mutation profile in individuals with RSTS1.
Genetic evaluation for individuals with suspected RSTS1 is essential since the phenotypes associated with this syndrome are not exclusive and may overlap with other syndromes. This phenotypic overlap often occurs among Mendelian disorders affecting genes involved in chromatin structure and remodeling, known as chromatinopathies. These disorders include Floating-Harbor syndrome (FHS) (OMIM #136140), Cornelia de Lange syndrome (CDLS) (OMIM #122470, #300590, #610759, #614701, #300882, #608749), Wiedemann-Steiner syndrome (WDSTS) (OMIM #605130), Kabuki syndrome (OMIM #147920, #300867), Genitopatellar syndrome (OMIM #606170), Biesecker-Young-Simpson syndrome (OMIM #603736), and Gabriele-de Vries syndrome (OMIM #617557) [
18].
A literature review analyzed the main clinical phenotypes in 308 reported cases of RSTS1 [
18]. Among the 30 highlighted phenotypes, the proband exhibited 25 of them and did not exhibit 5, namely microcephaly, hypertrichosis, keloids, cardiac anomalies, constipation, and urinary tract anomalies (
Table 2). The 83% overlap with the main phenotypes of RSTS1 reinforces the proband as a typical case of the RSTS1. On the other hand, some phenotypes presented by the proband were not identified as the most common among the 308 reviewed cases, specifically: pectus carinatum, café-au-lait spots, bruxism, feeding difficulties, gastroesophageal reflux, respiratory tract infections, prominent forehead, joint hypermobility, hypotonia, and ptosis.
Genetic counseling for individuals with suspected RSTS1 is critical as it allows for detailed phenotyping, addressing the syndrome’s phenotypic variability. Furthermore, it discusses and provides guidance on the most appropriate genetic tests, which are essential for a differential genetic diagnosis, and identifies at-risk family members. The process also includes genetic education on the inheritance pattern and the medical, psychological, and familial implications of the disease, providing key information for medical surveillance and therapies that can enhance the quality of life of affected individuals [
15]. The family assisted at our Institution received a comprehensive report, which systematically documented and consolidated all pieces of information discussed during the genetic counseling to ensure that current and future professionals assisting the proband could have a clear understanding of her genetic condition and its clinical implications.