Submitted:
13 June 2025
Posted:
16 June 2025
You are already at the latest version
Abstract
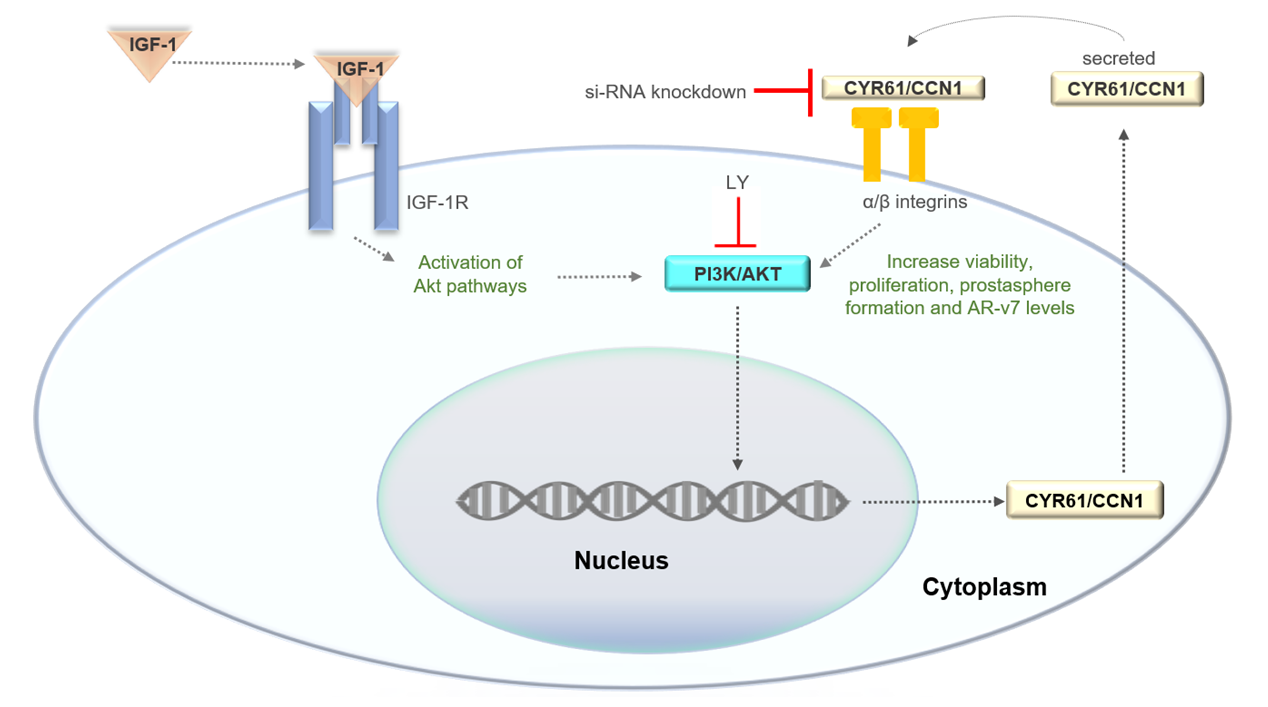
Keywords:
1. Introduction
2. Results
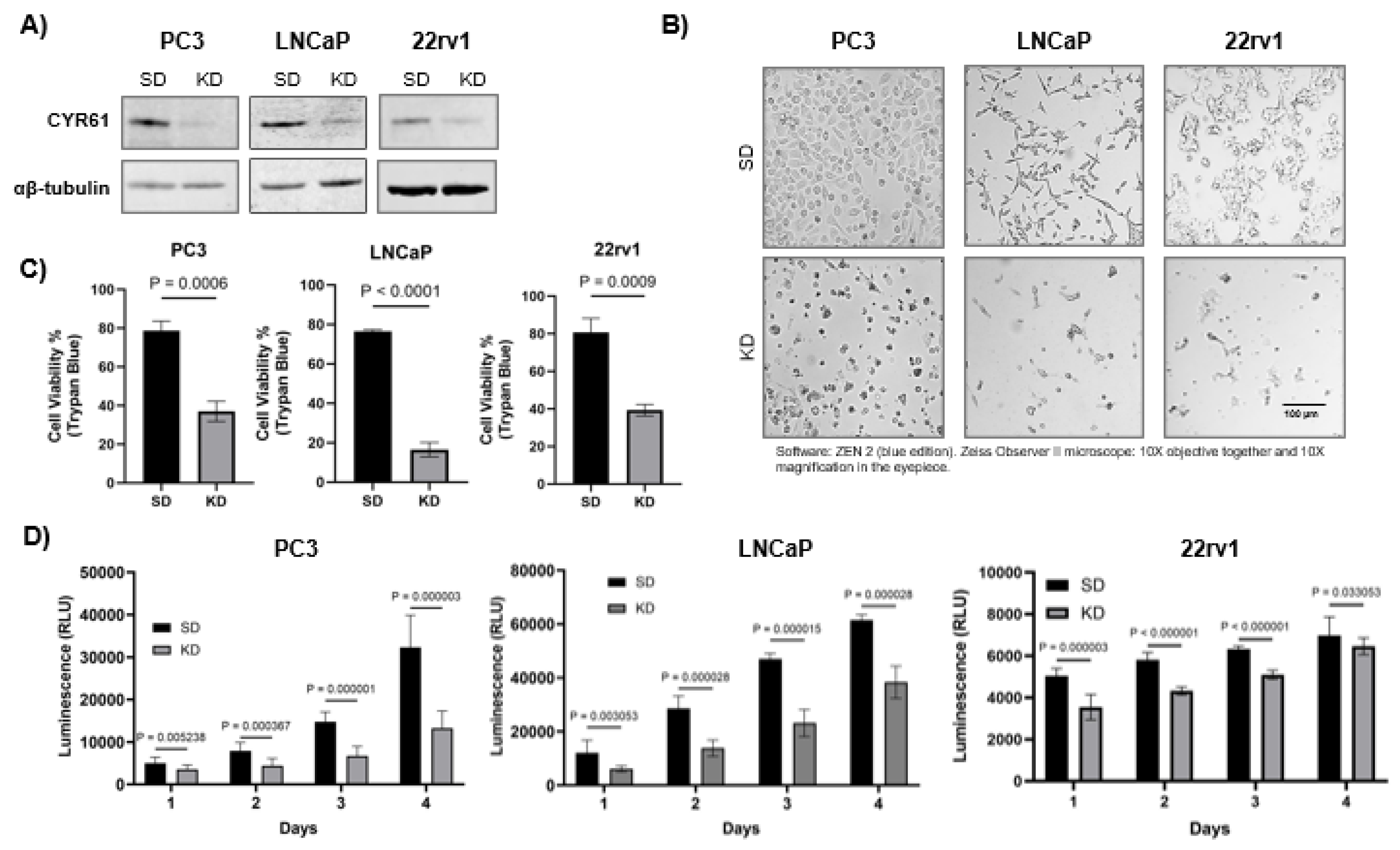
2.1. CYR61 Promoted PCa Cell Lines Viability and Proliferation
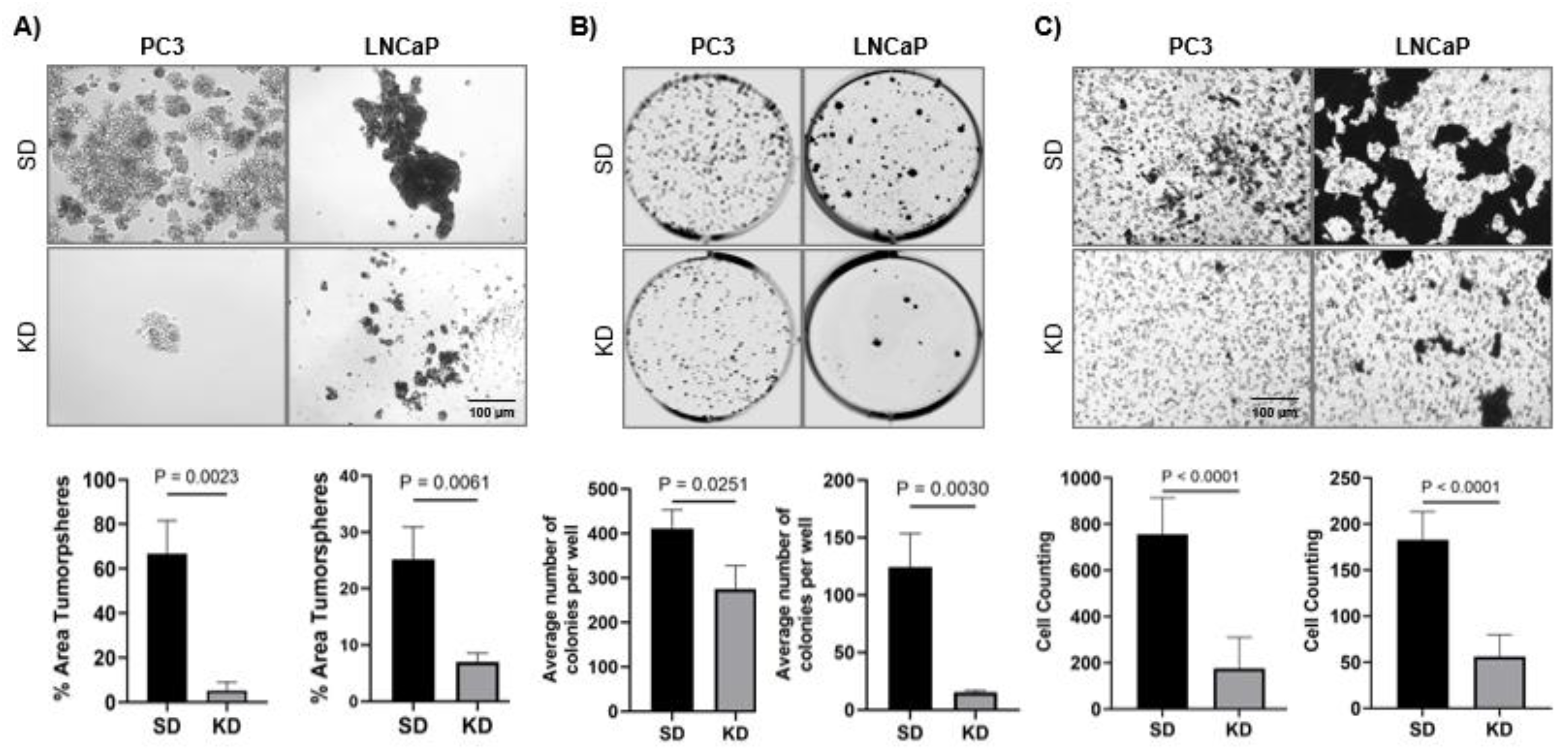
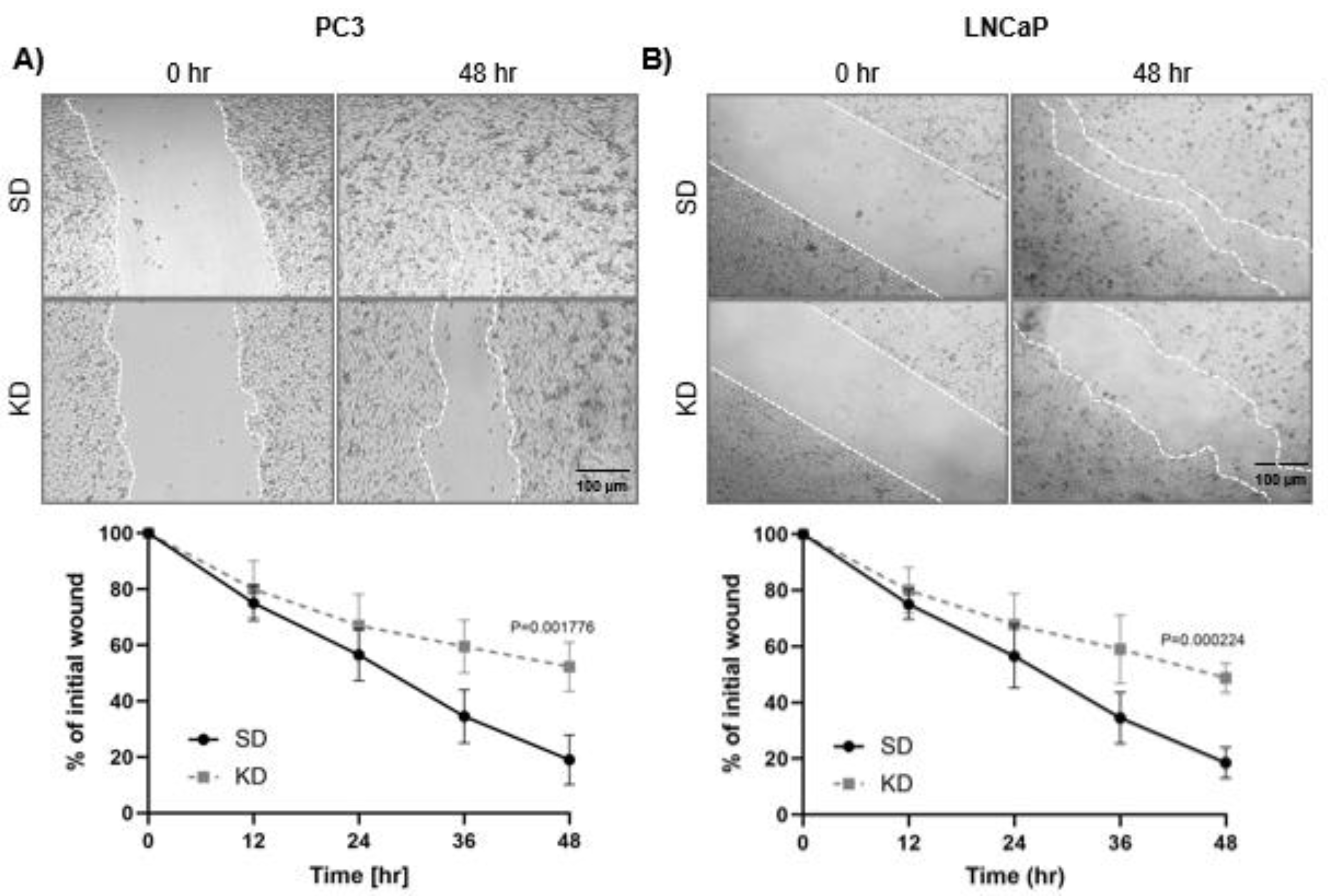
2.2. Silencing of CYR61 Inhibited Prostasphere Formation, Clonogenicity, Wound Healing, and Migration of PCa Cell Lines
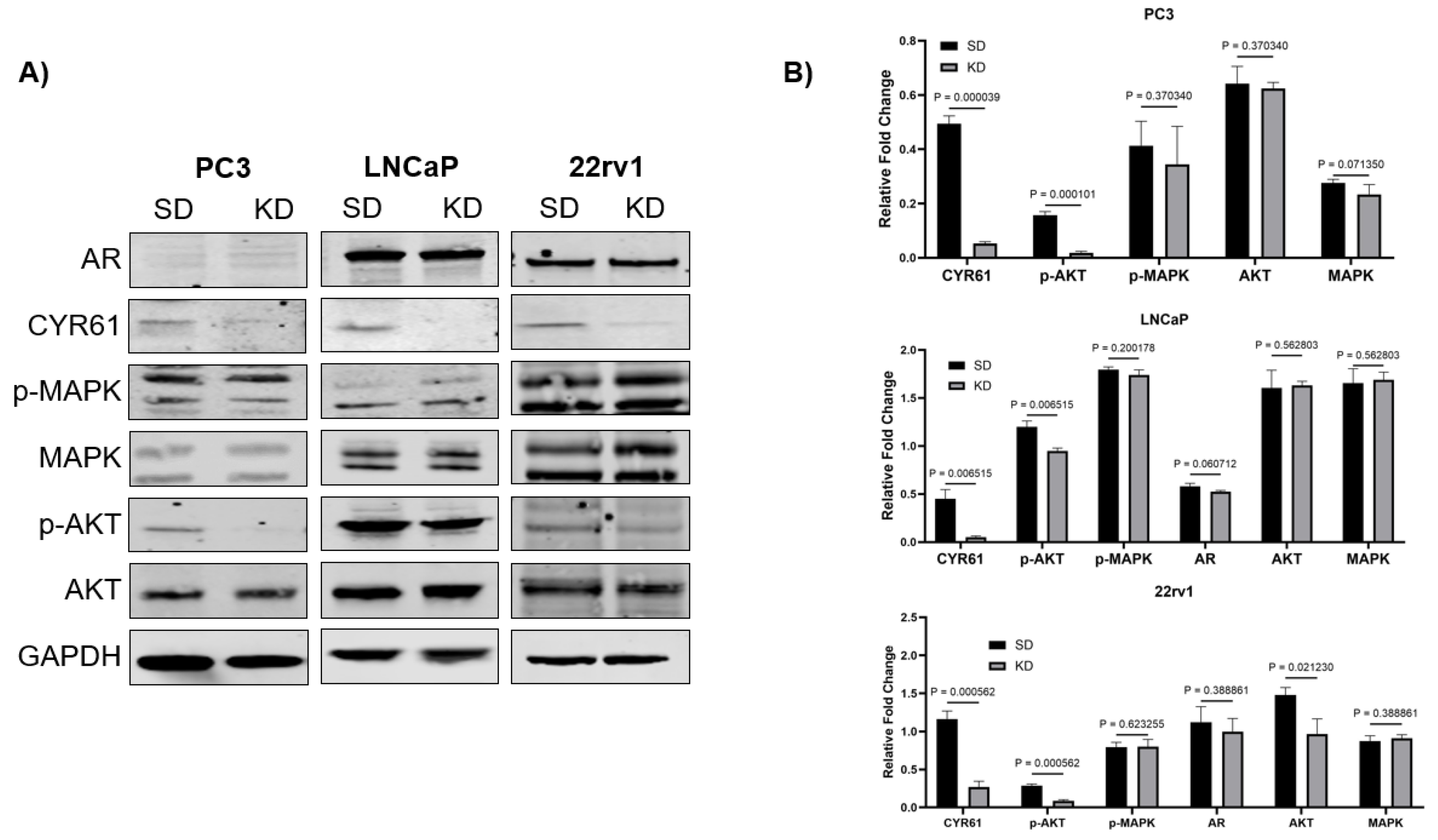
2.3. Effect of CYR61 Silencing on the AKT, MAPK, and AR Signaling Pathways in PCa Cells
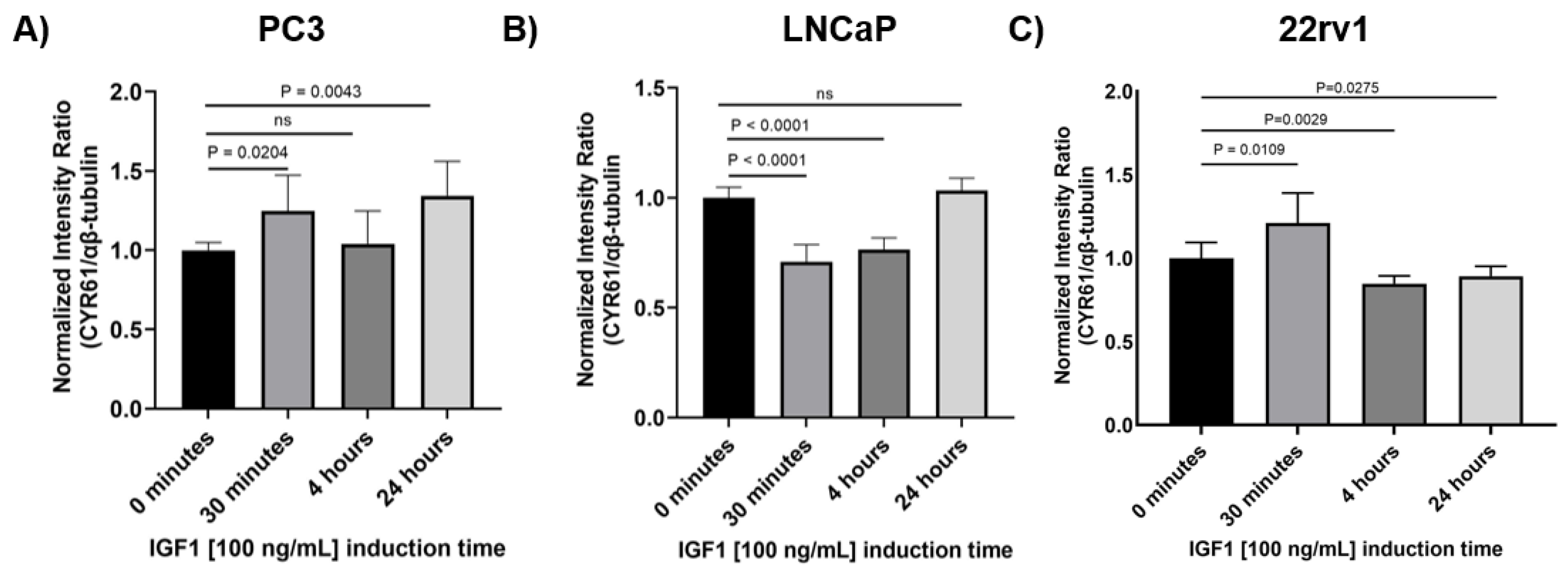
2.4. IGF1 Regulated CYR61 Expression Differently in PC3, LNCaP and 22rv1 Cells
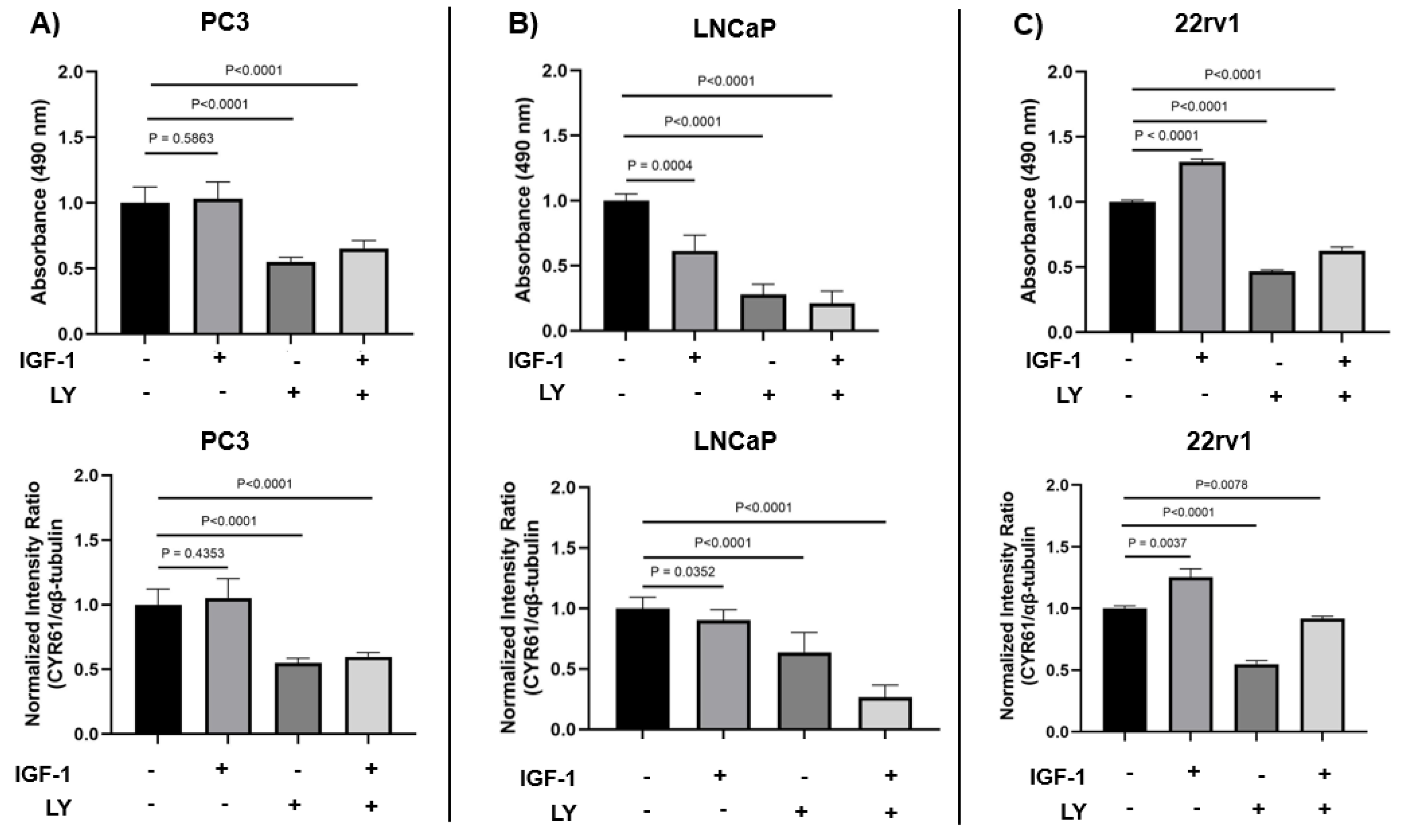
2.5. IGF1 Induced Cell Proliferation via CYR61 Expression and the PI3K/AKT Signaling Pathway
3. Discussion
4. Materials and Methods
4.1. Cell Lines
4.2. Antibodies
4.3. Immunoblotting
4.4. Cell Viability Assay
4.5. RNA Interference
4.6. Clonogenic Assay
4.7. Prostasphere Formation Assay
4.8. Wound Healing Assay
4.9. IGF1 Induction Treatment
4.10. In-Cell Western (ICW) Assay
4.11. Transwell Migration Assay
4.12. PI3K/AKT Inhibitor Induction Treatments
4.13. Statistical Analysis
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| AR | Androgen Receptor |
| CCN | Connective tissue growth factor, Cysteine-rich protein and Nephroblastoma overexpressed gene |
| CRPC | Castration Resistant Prostate Cancer |
| CSC | Cancer Stem-Like Cell |
| CYR61 | Cysteine-Rich Angiogenic Inducer 61 |
| H/L | Hispanic/Latino |
| ICW | In-Cell Western |
| IGF1 | Insulin-Like Growth Factor-I |
| IGF1-R | Insulin-Like Growth Factor-Receptor |
| KD | Knockdown |
| LNCaP | Lymph Node Carcinoma of the Prostate |
| MAPK | Mitogen-Activated Protein Kinases |
| p-AKT | Phosphorylated Protein Kinase B |
| p-MAPK | Phosphorylated Mitogen-Activated Protein Kinases |
| PBS | Phosphate-Buffered Saline |
| PC3 | Prostate Carcinoma 3 |
| PCa | Prostate Cancer |
| PFA | Paraformaldehyde |
| PI3/AKT | Phosphatidylinositol 3-Kinase/Protein kinase B |
| PSA | Prostate-Specific Antigen |
| SD | Scramble siRNA Duplex |
| siRNA | Small Interference RNA |
| TBS | Tris Buffer Saline |
References
- Siegel RL, Giaquinto AN, Jemal A. Cancer statistics, 2024. CA Cancer J Clin. 2024, 74, 12–49. [Google Scholar] [CrossRef] [PubMed]
- Morgan TM, Lange PH, Porter MP, Lin DW, Ellis WJ, Gallaher IS, et al. Disseminated tumor cells in prostate cancer patients after radical prostatectomy and without evidence of disease predicts biochemical recurrence. Clin Cancer Res. 2009, 15, 677–683. [Google Scholar] [CrossRef] [PubMed]
- Schenker AJ, Ortiz-Hernandez GL. CYR61 as a Potential Biomarker and Target in Cancer Prognosis and Therapies. Cells.
- Lau, LF. CCN1/CYR61: the very model of a modern matricellular protein. Cell Mol Life Sci. 2011, 68, 3149–3163. [Google Scholar] [CrossRef] [PubMed]
- Terada N, Kulkarni P, Getzenberg RH. Cyr61 is a potential prognostic marker for prostate cancer. Asian J Androl. 2012, 14, 405–408. [Google Scholar] [CrossRef]
- Lau, LF. Cell surface receptors for CCN proteins. J Cell Commun Signal. 2016, 10, 121–127. [Google Scholar] [CrossRef]
- Lin CM, Liang CZ. Cyr61: a potential therapeutic target for prostate cancer. Asian J Androl. 2014, 16, 788–789. [Google Scholar] [CrossRef]
- Sun ZJ, Wang Y, Cai Z, Chen PP, Tong XJ, Xie D. Involvement of Cyr61 in growth, migration, and metastasis of prostate cancer cells. Br J Cancer. 2008, 99, 1656–1667. [Google Scholar] [CrossRef]
- D'Antonio KB, Toubaji A, Albadine R, Mondul AM, Platz EA, Netto GJ, et al. Extracellular matrix associated protein CYR61 is linked to prostate cancer development. J Urol. 2010, 183, 1604–1610. [Google Scholar] [CrossRef]
- LeRoith D, Roberts CT, Jr. The insulin-like growth factor system and cancer. Cancer Lett. 2003, 195, 127–137. [Google Scholar] [CrossRef]
- Watts EL, Perez-Cornago A, Appleby PN, Albanes D, Ardanaz E, Black A, et al. The associations of anthropometric, behavioural and sociodemographic factors with circulating concentrations of IGF-I, IGF-II, IGFBP-1, IGFBP-2 and IGFBP-3 in a pooled analysis of 16,024 men from 22 studies. Int J Cancer. 2019, 145, 3244–3256. [Google Scholar] [CrossRef]
- Bellmunt J, Oh WK. Castration-resistant prostate cancer: new science and therapeutic prospects. Ther Adv Med Oncol. 2010, 2, 189–207. [Google Scholar] [CrossRef] [PubMed]
- Habel N, Stefanovska B, Carene D, Patino-Garcia A, Lecanda F, Fromigue O. CYR61 triggers osteosarcoma metastatic spreading via an IGF1Rbeta-dependent EMT-like process. BMC Cancer. 2019, 19, 62. [Google Scholar]
- Espinoza I, Kurapaty C, Park CH, Vander Steen T, Kleer CG, Wiley E, et al. Depletion of CCN1/CYR61 reduces triple-negative/basal-like breast cancer aggressiveness. Am J Cancer Res. 2022, 12, 839–851. [Google Scholar]
- Shimo T, Okui T, Horie N, Yokozeki K, Takigawa M, Sasaki A. Mouse Models of Tumor Bone Metastasis and Invasion for Studying CCN Proteins. Methods Mol Biol. 2023, 2582, 343–353. [Google Scholar]
- Barreto SC, Ray A, Ag Edgar P. Biological characteristics of CCN proteins in tumor development. J BUON. 2016, 21, 1359–1367. [Google Scholar]
- Ascencao K, Lheimeur B, Szabo C. Regulation of CyR61 expression and release by 3-mercaptopyruvate sulfurtransferase in colon cancer cells. Redox Biol. 2022, 56, 102466. [Google Scholar]
- Jia Q, Xu B, Zhang Y, Ali A, Liao X. CCN Family Proteins in Cancer: Insight Into Their Structures and Coordination Role in Tumor Microenvironment. Front Genet. 2021, 12, 649387. [Google Scholar] [CrossRef]
- Li J, Ye L, Owen S, Weeks HP, Zhang Z, Jiang WG. Emerging role of CCN family proteins in tumorigenesis and cancer metastasis (Review). Int J Mol Med. 2015, 36, 1451–1463. [Google Scholar] [CrossRef]
- Kim H, Son S, Shin I. Role of the CCN protein family in cancer. BMB Rep. 2018, 51, 486–492. [Google Scholar] [CrossRef]
- Lee YJ, Lee DM, Lee SH. Production of Cyr61 protein is modulated by extracellular acidification and PI3K/Akt signaling in prostate carcinoma PC-3 cells. Food Chem Toxicol. 2013, 58, 169–176. [Google Scholar] [CrossRef]
- Horoszewicz JS, Leong SS, Kawinski E, Karr JP, Rosenthal H, Chu TM, et al. LNCaP model of human prostatic carcinoma. Cancer Res. 1983, 43, 1809–1818. [Google Scholar]
- van Bokhoven A, Varella-Garcia M, Korch C, Johannes WU, Smith EE, Miller HL, et al. Molecular characterization of human prostate carcinoma cell lines. Prostate 2003, 57, 205–225. [Google Scholar] [CrossRef] [PubMed]
- Kaighn ME, Narayan KS, Ohnuki Y, Lechner JF, Jones LW. Establishment and characterization of a human prostatic carcinoma cell line (PC-3). Invest Urol. 1979, 17, 16–23. [Google Scholar]
- Sarkissyan S, Sarkissyan M, Wu Y, Cardenas J, Koeffler HP, Vadgama JV. IGF-1 regulates Cyr61 induced breast cancer cell proliferation and invasion. PLoS One 2014, 9, e103534. [Google Scholar]
- Leu SJ, Liu Y, Chen N, Chen CC, Lam SC, Lau LF. Identification of a novel integrin alpha 6 beta 1 binding site in the angiogenic inducer CCN1 (CYR61). J Biol Chem. 2003, 278, 33801–33808. [Google Scholar] [CrossRef]
- Siech C, Rutz J, Maxeiner S, Grein T, Sonnenburg M, Tsaur I, et al. Insulin-like Growth Factor-1 Influences Prostate Cancer Cell Growth and Invasion through an Integrin alpha3, alpha5, alphaV, and beta1 Dependent Mechanism. Cancers.
- Jandova J, Beyer TE, Meuillet EJ, Watts GS. The matrix protein CCN1/CYR61 is required for alpha(V)beta5-mediated cancer cell migration. Cell Biochem Funct. 2012, 30, 687–695. [Google Scholar] [CrossRef]
- Ma J, Li H, Giovannucci E, Mucci L, Qiu W, Nguyen PL, et al. Prediagnostic body-mass index, plasma C-peptide concentration, and prostate cancer-specific mortality in men with prostate cancer: a long-term survival analysis. Lancet Oncol. 2008, 9, 1039–1047. [Google Scholar] [CrossRef]
- Schayek H, Seti H, Greenberg NM, Sun S, Werner H, Plymate SR. Differential regulation of insulin-like growth factor-I receptor gene expression by wild type and mutant androgen receptor in prostate cancer cells. Mol Cell Endocrinol. 2010, 323, 239–245. [Google Scholar] [CrossRef]
- Watson A, Eilers A, Lallemand D, Kyriakis J, Rubin LL, Ham J. Phosphorylation of c-Jun is necessary for apoptosis induced by survival signal withdrawal in cerebellar granule neurons. J Neurosci. 1998, 18, 751–762. [Google Scholar] [CrossRef]
- Chen CC, Mo FE, Lau LF. The angiogenic factor Cyr61 activates a genetic program for wound healing in human skin fibroblasts. J Biol Chem. 2001, 276, 47329–47337. [Google Scholar] [CrossRef]
- Leu SJ, Lam SC, Lau LF. Pro-angiogenic activities of CYR61 (CCN1) mediated through integrins alphavbeta3 and alpha6beta1 in human umbilical vein endothelial cells. J Biol Chem. 2002, 277, 46248–46255. [Google Scholar] [CrossRef] [PubMed]
- Burgering BM, Kops GJ. Cell cycle and death control: long live Forkheads. Trends Biochem Sci. 2002, 27, 352–360. [Google Scholar] [CrossRef] [PubMed]
- Bisson I, Prowse DM. WNT signaling regulates self-renewal and differentiation of prostate cancer cells with stem cell characteristics. Cell Res. 2009, 19, 683–697. [Google Scholar] [CrossRef] [PubMed]
- Grundker C, Bauerschmitz G, Schubert A, Emons G. Invasion and increased expression of S100A4 and CYR61 in mesenchymal transformed breast cancer cells is downregulated by GnRH. Int J Oncol. 2016, 48, 2713–2721. [Google Scholar] [CrossRef]
- Haque I, Mehta S, Majumder M, Dhar K, De A, McGregor D, et al. Cyr61/CCN1 signaling is critical for epithelial-mesenchymal transition and stemness and promotes pancreatic carcinogenesis. Mol Cancer 2011, 10, 8. [Google Scholar] [CrossRef]
- Schmitz M, Grignard G, Margue C, Dippel W, Capesius C, Mossong J, et al. Complete loss of PTEN expression as a possible early prognostic marker for prostate cancer metastasis. Int J Cancer 2007, 120, 1284–1292. [Google Scholar] [CrossRef]
- Matsushita M, Fujita K, Hayashi T, Kayama H, Motooka D, Hase H, et al. Gut Microbiota-Derived Short-Chain Fatty Acids Promote Prostate Cancer Growth via IGF1 Signaling. Cancer Res. 2021, 81, 4014–4026. [Google Scholar] [CrossRef]
- Isaacs JT, Isaacs WB. Androgen receptor outwits prostate cancer drugs. Nat Med. 2004, 10, 26–27. [Google Scholar] [CrossRef]
- Han D, Labaf M, Zhao Y, Owiredu J, Zhang S, Patel K, et al. Androgen receptor splice variants drive castration-resistant prostate cancer metastasis by activating distinct transcriptional programs. J Clin Invest.
- Suzuki H, Ueda T, Ichikawa T, Ito H. Androgen receptor involvement in the progression of prostate cancer. Endocr Relat Cancer 2003, 10, 209–216. [Google Scholar]
- Shi XB, Ma AH, Tepper CG, Xia L, Gregg JP, Gandour-Edwards R, et al. Molecular alterations associated with LNCaP cell progression to androgen independence. Prostate 2004, 60, 257–271. [Google Scholar] [CrossRef]
- Watson PA, Arora VK, Sawyers CL. Emerging mechanisms of resistance to androgen receptor inhibitors in prostate cancer. Nat Rev Cancer. 2015, 15, 701–711. [Google Scholar] [CrossRef] [PubMed]
- Marcias G, Erdmann E, Lapouge G, Siebert C, Barthelemy P, Duclos B, et al. Identification of novel truncated androgen receptor (AR) mutants including unreported pre-mRNA splicing variants in the 22Rv1 hormone-refractory prostate cancer (PCa) cell line. Hum Mutat. 2010, 31, 74–80. [Google Scholar] [CrossRef] [PubMed]
- Roberts CT, Jr. IGF-1 and prostate cancer. Novartis Found Symp. 2004, 262, 193–199. [Google Scholar]
- Hernandez W, Grenade C, Santos ER, Bonilla C, Ahaghotu C, Kittles RA. IGF-1 and IGFBP-3 gene variants influence on serum levels and prostate cancer risk in African-Americans. Carcinogenesis 2007, 28, 2154–2159. [Google Scholar] [CrossRef] [PubMed]
- Liu L, Li X. A Review of IGF1 Signaling and IGF1-related Long Noncoding RNAs in Chemoresistance of Cancer. Curr Cancer Drug Targets. 2020, 20, 325–334. [Google Scholar] [CrossRef]
- Ameri P, Giusti A, Boschetti M, Bovio M, Teti C, Leoncini G, et al. Vitamin D increases circulating IGF1 in adults: potential implication for the treatment of GH deficiency. Eur J Endocrinol. 2013, 169, 767–772. [Google Scholar] [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).



