Submitted:
09 June 2025
Posted:
10 June 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Participants
2.2. Study Design
2.3. Study Measurements
2.3.1. Demographic and Clinical Variables
2.3.2. Olfactory Functions
2.3.3. Evaluation of Cognitive Function
2.3.4. Nutritional Assessment
2.3.5. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| BMI | Body mass index |
| CC | Calf circumference |
| MAC | Middle arm circumference |
| MMSE | Mini mental state examination |
| MNA | Mini nutritional assessment |
| PCS | Post-COVD syndrome |
References
- OMS. Información basica sobre la COVID-19 Organización Mundial de la Salud 2023. Available from: https://www.who.int/es/news-room/questions-and-answers/item/coronavirus-disease-covid-19.
- Ángeles Correa MG, Villarreal Ríos E, Galicia Rodríguez L, et al. Enfermedades crónicas degenerativas como factor de riesgo de letalidad por COVID-19 en México. Revista panamericana de salud publica, Pan American journal of public health. 2022;46.
- Arikawa E, Kaneko N, Nohara K, et al. Influence of Olfactory Function on Appetite and Nutritional Status in the Elderly Requiring Nursing Care. J Nutr Health Aging. 2020;24(4):398-403.
- Reyes de Beaman S, Beaman PE, García-Peña C, et al. “Validation of a modified version of the Mini-Mental State Examination (MMSE) in spanish”. Aging, Neuropsychology and Cognition 2004;11:1-11.
- Borsetto D, Hopkins C, Philips V, et al. Self-reported alteration of sense of smell or taste in patients with COVID-19: a systematic review and meta-analysis on 3563 patients. Rhinology. 2020;58(5):430-436.
- Wanga V, Chevinsky JR, Dimitrov LV, et al. Long-Term Symptoms Among Adults Tested for SARS-CoV-2 - United States, January 2020-April 2021. MMWR Morb Mortal Wkly Rep. 2021;70(36):1235-1241.
- Prevention CfDCa. Long COVID Basics Centers for Disease Control and Prevention: U.S. Department of Health and Human Services.; 2024 [updated 204; cited 2024 July 26]. Available from: https://www.cdc.gov/covid/long-term-effects/.
- Carrillo-Esper R. Post-COVID-19 syndrome. Gac Med Mex. 2022;158(3):115-117.
- Carfi A, Bernabei R, Landi F, et al. Persistent Symptoms in Patients After Acute COVID-19. JAMA. 2020;324(6):603-605.
- Cabrera Martimbianco AL, Pacheco RL, Bagattini ÂM, et al. Frequency, signs and symptoms, and criteria adopted for long COVID-19: A systematic review. International journal of clinical practice. 2021;75(10).
- Ceban F, Ling S, Lui LMW, et al. Fatigue and cognitive impairment in Post-COVID-19 Syndrome: A systematic review and meta-analysis. Brain Behav Immun. 2022;101:93-135.
- Cereda E, Pedrolli C, Klersy C, et al. Nutritional status in older persons according to healthcare setting: A systematic review and meta-analysis of prevalence data using MNA((R)). Clin Nutr. 2016;35(6):1282-1290.
- Cho JH, Jeong YS, Lee YJ, et al. The Korean version of the Sniffin’ stick (KVSS) test and its validity in comparison with the cross-cultural smell identification test (CC-SIT). Auris Nasus Larynx. 2009;36(3):280-6.
- Dong Y, Li Y, Liu K, et al. Anosmia, mild cognitive impairment, and biomarkers of brain aging in older adults. Alzheimers Dement. 2023;19(2):589-601.
- Doty RL. Olfactory dysfunction in COVID-19: pathology and long-term implications for brain health. Trends Mol Med. 2022;28(9):781-794.
- Benchimol EI, Smeeth L, Guttmann A, et al. The REporting of studies Conducted using Observational Routinely-collected health Data (RECORD) statement. PLoS Med. 2015;12(10):e1001885.
- He D, Yuan M, Dang W, et al. Long term neuropsychiatric consequences in COVID-19 survivors: Cognitive impairment and inflammatory underpinnings fifteen months after discharge. Asian J Psychiatr. 2023;80:103409.
- Mansell V, Hall Dykgraaf S, Kidd M, et al. Long COVID and older people. Lancet Healthy Longev. 2022;3(12):e849-e854.
- Chen Y, Yang W, Chen F, et al. COVID-19 and cognitive impairment: neuroinvasive and blood‒brain barrier dysfunction. J Neuroinflammation. 2022;19(1):222.
- Tavares-Junior JWL, de Souza ACC, Borges JWP, et al. COVID-19 associated cognitive impairment: A systematic review. Cortex. 2022;152:77-97.
- Rothenberg E. Coronavirus Disease 19 from the Perspective of Ageing with Focus on Nutritional Status and Nutrition Management-A Narrative Review. Nutrients. 2021;13(4).
- Fatuzzo I, Niccolini GF, Zoccali F, et al. Neurons, Nose, and Neurodegenerative Diseases: Olfactory Function and Cognitive Impairment. Int J Mol Sci. 2023;24(3).
- al Se. Declaración de la Iniciativa STROBE (Strengthening the Reporting of Observational studies in Epidemiology): directrices para la comunicación de estudios observacionales. Nefrología. 2009;29(1):11-16.
- Resneck JS, Jr. Revisions to the Declaration of Helsinki on Its 60th Anniversary: A Modernized Set of Ethical Principles to Promote and Ensure Respect for Participants in a Rapidly Innovating Medical Research Ecosystem. JAMA. 2024.
- Kroc L, Fife E, Piechocka-Wochniak E, et al. Comparison of Nutrition Risk Screening 2002 and Subjective Global Assessment Form as Short Nutrition Assessment Tools in Older Hospitalized Adults. Nutrients. 2021;13(1).
- Silva DFO, Lima S, Sena-Evangelista KCM, et al. Nutritional Risk Screening Tools for Older Adults with COVID-19: A Systematic Review. Nutrients. 2020;12(10).
- López-Sampalo A, Bernal-López MR, Gómez-Huelgas R. Síndrome de COVID-19 persistente. Una revisión narrativaPersistent COVID-19 syndrome. A narrative review. Revista Clínica Española. 2022;222(4):241-250.
- Xiong J, Lipsitz O, Nasri F, et al. Impact of COVID-19 pandemic on mental health in the general population: A systematic review. J Affect Disord. 2020;277:55-64.
- Muccioli L, Sighinolfi G, Mitolo M, et al. Cognitive and functional connectivity impairment in post-COVID-19 olfactory dysfunction. Neuroimage Clin. 2023;38:103410.
- Winter AL, Henecke S, Lundstrom JN, et al. Impairment of quality of life due to COVID-19-induced long-term olfactory dysfunction. Front Psychol. 2023;14:1165911.
- Hopkins C, Surda P, Whitehead E, et al. Early recovery following new onset anosmia during the COVID-19 pandemic - an observational cohort study. J Otolaryngol Head Neck Surg. 2020;49(1):26.
- Gunzer W. Changes of Olfactory Performance during the Process of Aging - Psychophysical Testing and Its Relevance in the Fight against Malnutrition. J Nutr Health Aging. 2017;21(9):1010-1015.
- Lechien JR, Chiesa-Estomba CM, De Siati DR, et al. Olfactory and gustatory dysfunctions as a clinical presentation of mild-to-moderate forms of the coronavirus disease (COVID-19): a multicenter European study. Eur Arch Otorhinolaryngol. 2020;277(8):2251-2261.
- Butowt R, von Bartheld CS. Anosmia in COVID-19: Underlying Mechanisms and Assessment of an Olfactory Route to Brain Infection. Neuroscientist. 2021;27(6):582-603.
- Williams FMK, Freidin MB, Mangino M, et al. Self-Reported Symptoms of COVID-19, Including Symptoms Most Predictive of SARS-CoV-2 Infection, Are Heritable. Twin Res Hum Genet. 2020;23(6):316-321.
- von Bartheld CS, Hagen MM, Butowt R. Prevalence of Chemosensory Dysfunction in COVID-19 Patients: A Systematic Review and Meta-analysis Reveals Significant Ethnic Differences. ACS Chem Neurosci. 2020;11(19):2944-2961.
- Meinhardt J, Radke J, Dittmayer C, et al. Olfactory transmucosal SARS-CoV-2 invasion as a port of central nervous system entry in individuals with COVID-19. Nat Neurosci. 2021;24(2):168-175.
- Grund S, Bauer JM. Malnutrition and Sarcopenia in COVID-19 Survivors. Clin Geriatr Med. 2022;38(3):559-564.
- Hummel T, Nordin S. Olfactory disorders and their consequences for quality of life. Acta Otolaryngol. 2005;125(2):116-21.
- Toller SV. Assessing the impact of anosmia: review of a questionnaire’s findings. Chem Senses. 1999;24(6):705-12.
- Raff AC, Lieu S, Melamed ML, et al. Relationship of impaired olfactory function in ESRD to malnutrition and retained uremic molecules. Am J Kidney Dis. 2008;52(1):102-10.
- Mattes RD. The chemical senses and nutrition in aging: challenging old assumptions. J Am Diet Assoc. 2002;102(2):192-6.
- Schubert CR, Cruickshanks KJ, Fischer ME, et al. Olfactory impairment in an adult population: the Beaver Dam Offspring Study. Chem Senses. 2012;37(4):325-34.
- Toussaint N, de Roon M, van Campen JP, et al. Loss of olfactory function and nutritional status in vital older adults and geriatric patients. Chem Senses. 2015;40(3):197-203.
- Jin SY, Jeong HS, Lee JW, et al. Effects of nutritional status and cognitive ability on olfactory function in geriatric patients. Auris Nasus Larynx. 2016;43(1):56-61.

| Parameter | Mean (SD) | P value | |
| No risk for CI (n=15) |
Risk for CI or CI (n=30) |
||
| Age, y | 75.6 (5.9) | 75.9 (6.7) | 0.862 |
| Males, No. (%) | 9 (60) | 13 (43.3) | 0.292 |
| Weight, Kg | 60.8 (18.4) | 67.6 (13.7) | 0.169 |
| Height, mt | 1.6 (0.09) | 1.6 (0.9) | 0.212 |
| BMI | 23.2 (18.1-26.07) | 26.82 (21.8-31.2) | 0.057 |
| CC | 29.09 (25.7-32.5) | 31.45 (28.4-35.0) | 0.109 |
| MAC | 26.72 (21.3-34) | 28.21 (24-30.7) | 0.295 |
| Obesity, No. (%) | 5 (33.3) | 17 (56.7) | 0.140 |
| Risk Factors,No. (%) | |||
| Basic education, | 13 (86.6) | 20 (66.6) | 0.312 |
| Diabetes | 5 (33.3) | 13 (43.3) | 0.519 |
| Hypertension | 8 (53.3) | 17 (56.7) | 0.832 |
| Kidney Disease | 3 (20) | 7 (23.3) | 0.800 |
| COPD | 5 (33.3) | 11 (36.7) | 0.826 |
| >3 comorbilities | 8 (53.3) | 18 (60) | 0.670 |
| Smoker | 2 (13.3) | 4 (13.3) | 1.000 |
| Ex Smoker | 4 (26.7) | 7 (23.3) | 0.806 |
| COVID Symptoms, No. (%) | |||
| Anosmia | 13 (86) | 26 (86) | 1.000 |
| Ageusia | 9 (60) | 16 (53.3) | 0.671 |
| Fatigue | 15 (100) | 26 (86.7) | 0.138 |
| Memory Problems | 6 (40) | 27 (90) | <0.001* |
| Insomnia | 12 (80) | 23 (76.7) | 0.800 |
| COVID Severity, No. (%) | |||
| Hospitalization | 9 (60) | 15 (50) | 0.526 |
| Suplementary 02 | 12 (80) | 22 (76.6) | 0.920 |
| Intubation | 1 (6.7) | 1 (3.3) | 0.920 |
| Hospital stays days median (ICR) | 8 (0-60) | 4 (0-15) | 0.252 |
| Reinfection COVID | 1 (6.7) | 2 (6.7) | 1.000 |
| Post-COVID Syndrome | 6 (40) | 15 (50) | 0.526 |
| Tests, Median (ICR) | |||
| MNA | 15.7 (12-17) | 20.0 (16.5-24) | 0.004* |
| MMSE | 26 (25-29) | 19 (15-22) | <0.001* |
| SNIFFIN TEST | 9 (7-10) | 8 (5-10) | 0.5124 |
| Variable | Coefficient | R2 | P | (95% CI) |
| Sniffing Test MNA BMI |
0.701 | 0.137 | 0.012* | 0.161 – 1.242 |
| -0.194 | 0.030 | 0.254 | -0.531 - 0.144 | |
| -0.061 | 0.006 | 0.606 | -0.299 – 0.176 | |
| Obesity | -0.830 | 0.007 | 0.600 | -3.994 – 2.334 |
| Age, yr | -0.150 | 0.033 | 0.229 | -0.397 - 0.098 |
| Male | 1.660 | 0.0259 | 0.291 | -1.473 – 4.793 |
| Days with PCS | -0.005 | 0.043 | 0.171 | -0.014 - 0.002 |
| COVID reinfection | -0.714 | 0.0012 | 0.822 | -7.072 – 5.643 |
| Multivariate model | ||||
| Sniffing Test | 0.738 | 0.212 | 0.028* | 0.081-1.39 |
| MNA Age, yr |
-0.293 | data | 0.077 | -0.620 - 0.032 |
| -0.04 | data | 0.784 | -0.293 - 0.222 | |
| Days with PCS | -0.002 | data | 0.680 | -0.010 - 0.007 |
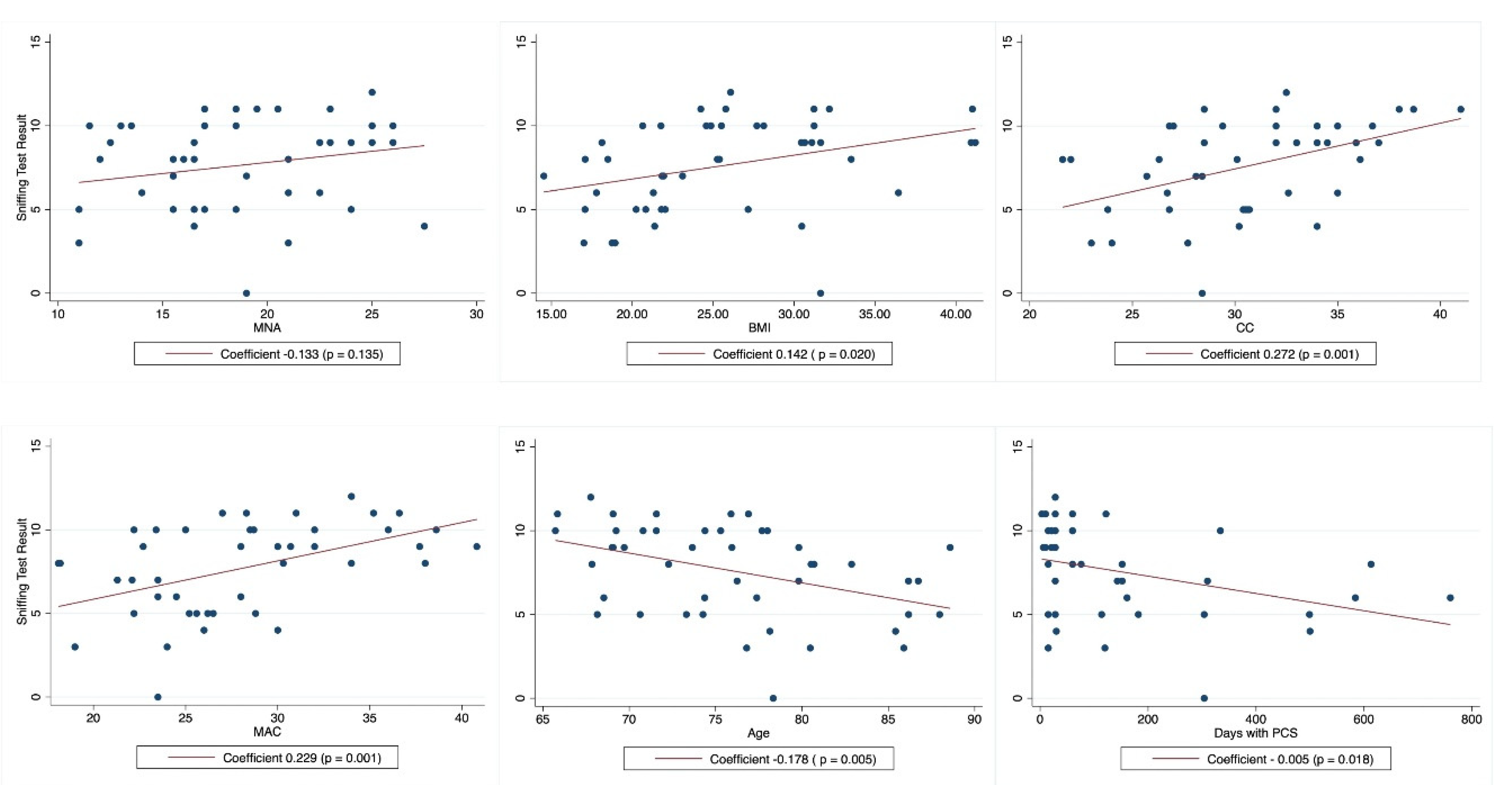
| Variable | Coefficient | R2 | P | (95% CI) |
| MNA | 0.133 | 0.051 | 0.135 | -0.043 - 0.309 |
| BMI | 0.142 | 0.120 | 0.020* | 0.024 – 0.261 |
| Obesity | 1.895 | 0.121 | 0.019* | 0.322 – 3.468 |
| CC | 0.272 | 0.212 | 0.001* | 0.111 – 0.435 |
| MAC | 0.229 | 0.238 | 0.001* | 0.103 – 0.356 |
| Age, yr | -0.178 | 0.168 | 0.005* | -0.299 – 0.056- |
| Male | -0.773 | 0.020 | 0.353 | -2.433 – 0.888 |
| Days with PCS | -0.005 | 0.123 | 0.018* | -0.009 – -0.001 |
| COVID reinfection | -1.381 | 0.016 | 0.408 | -4.716 – 1.954 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




