Submitted:
05 June 2025
Posted:
09 June 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Patients and Methods
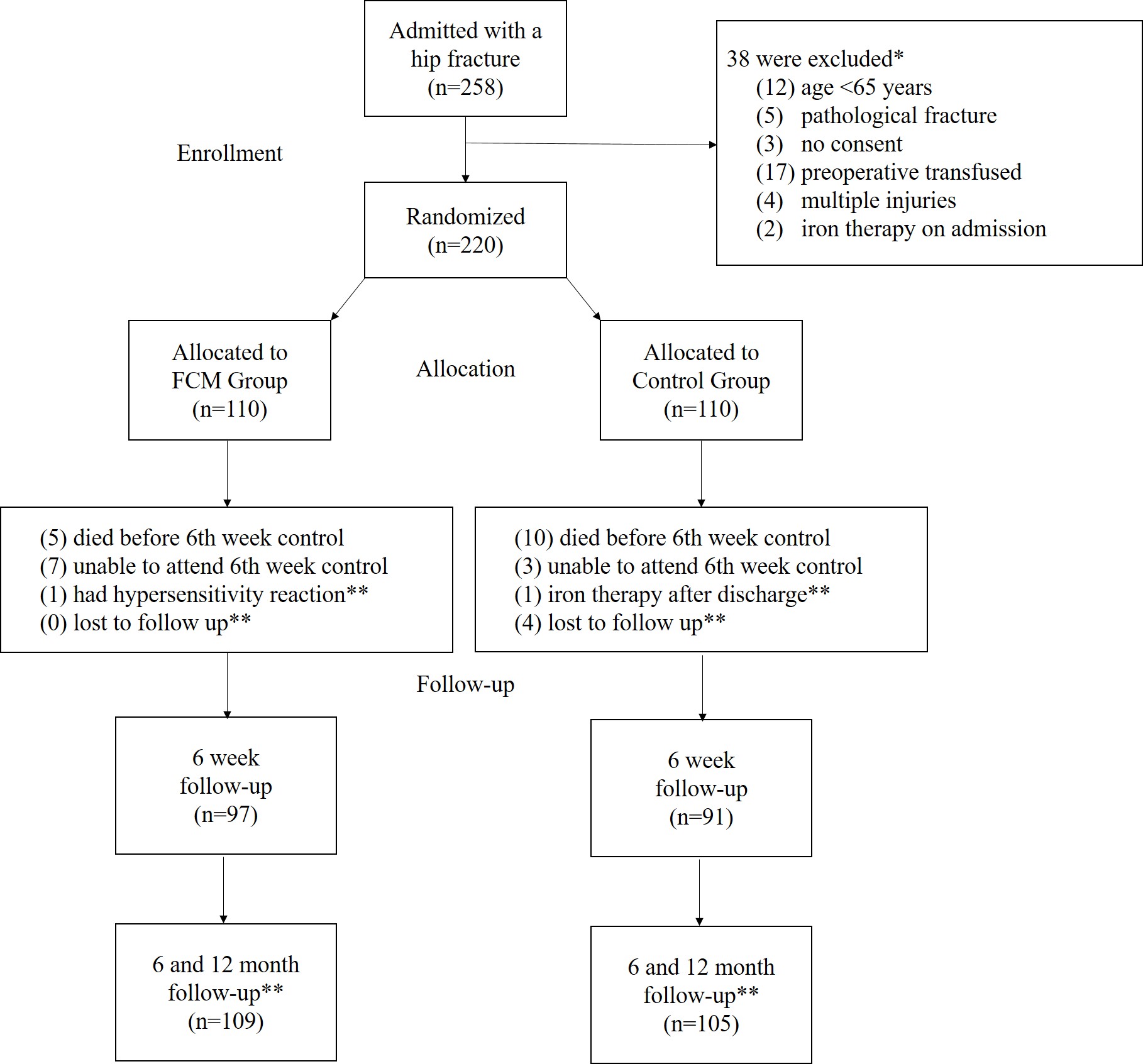
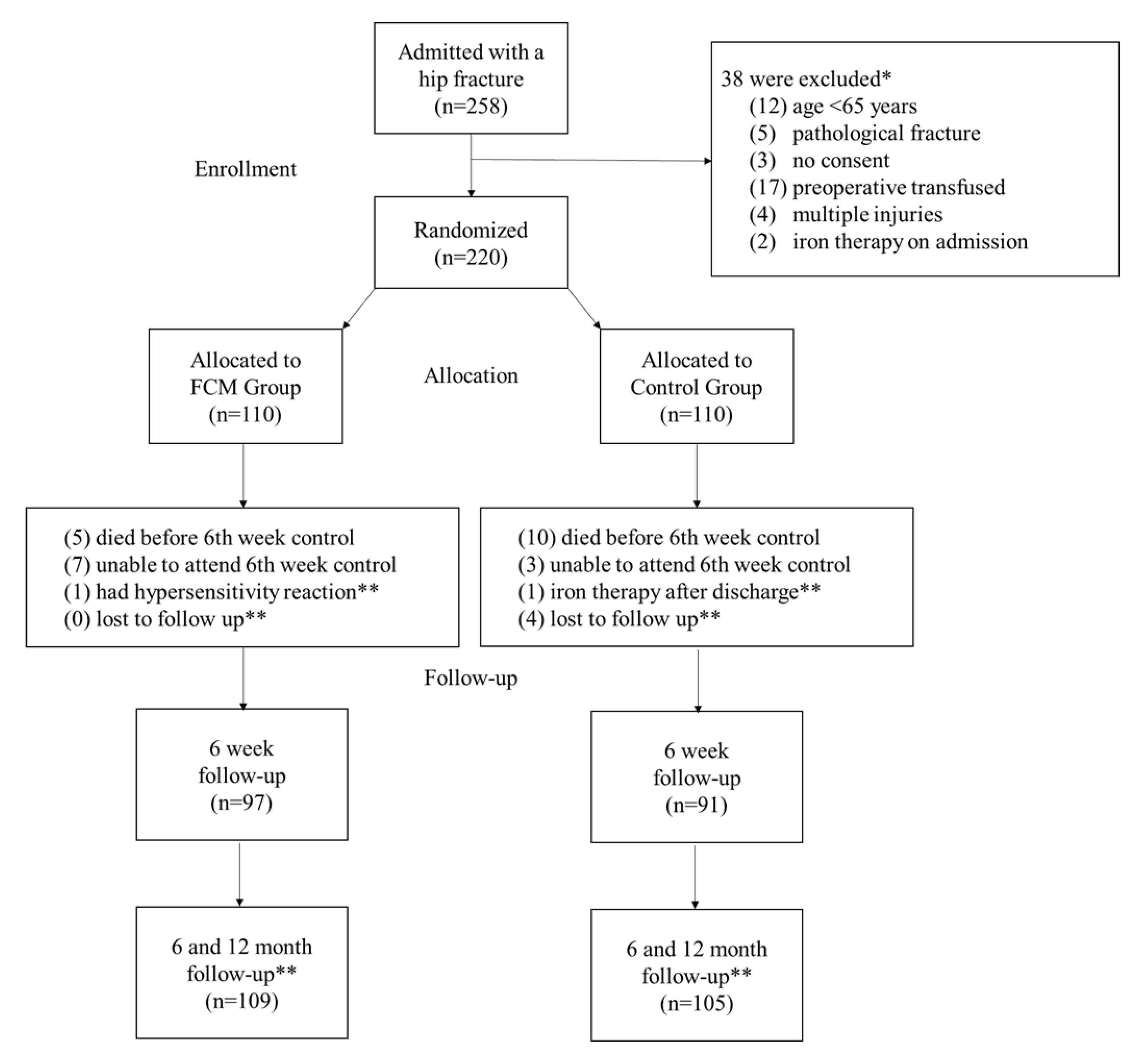
2.1. Study Design and Eligibility Criteria
2.2. Randomisation and Intervention
2.3. Perioperative Transfusion Protocol
2.4. Outcome Measures and Follow-Up Protocol
2.5. Statistical Analysis
3. Results
3.1. Baseline Characteristics and Comorbidity Profile
3.2. Primary Outcomes: Mortality rates
3.3. Secondary Outcomes
3.3.1. Anemia Status
3.3.2. Hemoglobin Trends Over Time
3.3.3. Perioperative Transfusion Characteristic
3.3.4. Length of Hospitalization
3.3.5. Adverse Events Related to FCM Administration
3.4. Multivariate Analysis of Mortality Outcomes
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
References
- Gullberg, B.; Johnell, O.; Kanis, J. World-wide projections for hip fracture. Osteoporosis international, 1997, 7, 407–413. [Google Scholar] [CrossRef] [PubMed]
- Parker, M.J. Iron supplementation for anemia after hip fracture surgery: a randomized trial of 300 patients. JBJS, 2010, 92, 265–269. [Google Scholar] [CrossRef]
- Gruson, K.I.; Aharonoff, G.B.; Egol, K.A.; Zuckerman, J.D.; Koval, K.J. The relationship between admission hemoglobin level and outcome after hip fracture. Journal of orthopaedic trauma 2002, 16, 39–44. [Google Scholar] [CrossRef] [PubMed]
- Koval, K.J.; Rosenberg, A.D.; Zuckerman, J.D.; Aharonoff, G.B.; Skovron, M.L.; Bernstein, R.L.; Chakka, M. Does blood transfusion increase the risk of infection after hip fracture? Journal of orthopaedic trauma 1997, 11, 260–265. [Google Scholar] [CrossRef]
- Smeets, S.; Verbruggen, J.; Poeze, M. Effect of blood transfusion on survival after hip fracture surgery. European Journal of Orthopaedic Surgery & Traumatology 2018, 28, 1297–1303. [Google Scholar]
- Shin, H.J.; Kim, J.H.; Han, S.-B.; Park, J.H.; Jang, W.Y. Allogeneic red blood cell transfusion is an independent risk factor for 1-year mortality in elderly patients undergoing femoral neck fracture surgery: retrospective study. Medicine 2020, 99, e21897. [Google Scholar] [CrossRef] [PubMed]
- Engoren, M.; Mitchell, E.; Perring, P.; Sferra, J. The effect of erythrocyte blood transfusions on survival after surgery for hip fracture. Journal of Trauma and Acute Care Surgery 2008, 65, 1411–1415. [Google Scholar] [CrossRef]
- Arshi, A.; Lai, W.C.; Iglesias, B.C.; McPherson, E.J.; Zeegen, E.N.; Stavrakis, A.I.; Sassoon, A.A. Blood transfusion rates and predictors following geriatric hip fracture surgery. Hip international 2021, 31, 272–279. [Google Scholar] [CrossRef]
- Khatib, Y.; Bal, G.; Liu, R.; Ashaia, W.; Sorial, R. A randomised controlled trial assessing the effect of tranexamic acid on post-operative blood transfusions in patient with intra-capsular hip fractures treated with hemi-or total hip arthroplasty. Archives of Orthopaedic and Trauma Surgery 2024, 144, 3095–3102. [Google Scholar] [CrossRef]
- Gregersen, M.; Borris, L.C.; Damsgaard, E.M. Postoperative blood transfusion strategy in frail, anemic elderly patients with hip fracture: the TRIFE randomized controlled trial. Acta orthopaedica 2015, 86, 363–372. [Google Scholar] [CrossRef]
- Hung, K.-C.; Chang, L.-C.; Ho, C.-N.; Hsu, C.-W.; Yu, C.-H.; Wu, J.-Y.; Lin, C.-M.; Chen, I.-W. Efficacy of intravenous iron supplementation in reducing transfusion risk following cardiac surgery: an updated meta-analysis of randomised controlled trials. British Journal of Anaesthesia 2024. [CrossRef] [PubMed]
- Froessler, B.; Palm, P.; Weber, I.; Hodyl, N.A.; Singh, R.; Murphy, E.M. The important role for intravenous iron in perioperative patient blood management in major abdominal surgery: a randomized controlled trial. in Editor (Ed.)^(Eds.) Book The important role for intravenous iron in perioperative patient blood management in major abdominal surgery: a randomized controlled trial’ (LWW, 2016, edn.), pp.
- Kulnigg, S.; Stoinov, S.; Simanenkov, V.; Dudar, L.V.; Karnafel, W.; Garcia, L.C.; Sambuelli, A.M.; D'haens, G.; Gasche, C. A novel intravenous iron formulation for treatment of anemia in inflammatory bowel disease: the ferric carboxymaltose (FERINJECT®) randomized controlled trial. Official journal of the American College of Gastroenterology| ACG 2008, 103, 1182–1192. [Google Scholar] [CrossRef] [PubMed]
- Van Wyck, D.B.; Martens, M.G.; Seid, M.H.; Baker, J.B.; Mangione, A. Intravenous ferric carboxymaltose compared with oral iron in the treatment of postpartum anemia: a randomized controlled trial. Obstetrics & Gynecology 2007, 110, (2 Part 1), 267–278. [Google Scholar]
- Camaschella, C. Iron-deficiency anemia. New England journal of medicine 2015, 372, 1832–1843. [Google Scholar] [CrossRef] [PubMed]
- Yoon, B.-H.; Lee, B.S.; Won, H.; Kim, H.-K.; Lee, Y.-K.; Koo, K.-H. Preoperative iron supplementation and restrictive transfusion strategy in hip fracture surgery. Clinics in orthopedic surgery 2019, 11, 265. [Google Scholar] [CrossRef]
- Cuenca, J.; García-Erce, J.A.; Martínez, A.A.; Solano, V.M.; Molina, J.; Munoz, M. Role of parenteral iron in the management of anaemia in the elderly patient undergoing displaced subcapital hip fracture repair: preliminary data. Archives of Orthopaedic and Trauma Surgery 2005, 125, 342–347. [Google Scholar] [CrossRef]
- Bernabeu-Wittel, M.; Romero, M.; Ollero-Baturone, M.; Aparicio, R.; Murcia-Zaragoza, J.; Rincón-Gómez, M.; Monte-Secades, R.; Melero-Bascones, M.; Rosso, C.M.; Ruiz-Cantero, A. Ferric carboxymaltose with or without erythropoietin in anemic patients with hip fracture: a randomized clinical trial. Transfusion 2016, 56, 2199–2211. [Google Scholar] [CrossRef]
- Carson, J.L.; Stanworth, S.J.; Guyatt, G.; Valentine, S.; Dennis, J.; Bakhtary, S.; Cohn, C.S.; Dubon, A.; Grossman, B.J.; Gupta, G.K. Red blood cell transfusion: 2023 AABB international guidelines. Jama 2023, 330, 1892–1902. [Google Scholar] [CrossRef]
- Horvath, B.; Kloesel, B.; Todd, M.M.; Cole, D.J.; Prielipp, R.C. The evolution, current value, and future of the American Society of Anesthesiologists Physical Status Classification System. Anesthesiology 2021, 135, 904–919. [Google Scholar] [CrossRef]
- Charlson, M.E.; Pompei, P.; Ales, K.L.; MacKenzie, C.R. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. Journal of chronic diseases 1987, 40, 373–383. [Google Scholar] [CrossRef]
- Miralles-Muñoz, F.A.; Perez-Aznar, A.; Gonzalez-Parreño, S.; Sebastia-Forcada, E.; Mahiques-Segura, G.; Lizaur-Utrilla, A.; Vizcaya-Moreno, M.F. Change in 1-year mortality after hip fracture surgery over the last decade in a European population. Archives of Orthopaedic and Trauma Surgery 2023, 143, 4173–4179. [Google Scholar] [CrossRef] [PubMed]
- Yoo, S.; Jang, E.J.; Jo, J.; Jo, J.G.; Nam, S.; Kim, H.; Lee, H.; Ryu, H.G. The association between hospital case volume and in-hospital and one-year mortality after hip fracture surgery: a population-based retrospective cohort study. The Bone & Joint Journal 2020, 102, 1384–1391. [Google Scholar]
- Huette, P.; Abou-Arab, O.; Djebara, A.-E.; Terrasi, B.; Beyls, C.; Guinot, P.-G.; Havet, E.; Dupont, H.; Lorne, E.; Ntouba, A. Risk factors and mortality of patients undergoing hip fracture surgery: a one-year follow-up study. Scientific reports 2020, 10, 9607. [Google Scholar] [CrossRef] [PubMed]
- Muñoz, M.; Gómez-Ramírez, S.; Cuenca, J.; García-Erce, J.A.; Iglesias-Aparicio, D.; Haman-Alcober, S.; Ariza, D.; Naveira, E. Very-short-term perioperative intravenous iron administration and postoperative outcome in major orthopedic surgery: a pooled analysis of observational data from 2547 patients. Transfusion 2014, 54, 289–299. [Google Scholar] [CrossRef]
- Spahn, D.R. Anemia and patient blood management in hip and knee surgery: a systematic review of the literature. Anesthesiology 2010, 113, 482–495. [Google Scholar] [CrossRef]
- Qunibi, W.Y.; Martinez, C.; Smith, M.; Benjamin, J.; Mangione, A.; Roger, S.D. A randomized controlled trial comparing intravenous ferric carboxymaltose with oral iron for treatment of iron deficiency anaemia of non-dialysis-dependent chronic kidney disease patients. Nephrology Dialysis Transplantation 2011, 26, 1599–1607. [Google Scholar] [CrossRef]
- Avni, T.; Bieber, A.; Grossman, A.; Green, H.; Leibovici, L.; Gafter-Gvili, A. The safety of intravenous iron preparations: systematic review and meta-analysis. in Editor (Ed.)^(Eds.) Book The safety of intravenous iron preparations: systematic review and meta-analysis’ (Elsevier, 2015, edn.), 12-23.
| Variables | FCM Group | Control Group | P values | |
|---|---|---|---|---|
| Number of patients | n | 109 | 105 | |
| Age (years) |
Mean ± SD Median (IQR) |
78.19 ± 10.79 80.0 (71.0–87.0) |
78.91 ± 9.20 79.0 (74.0–88.0) |
0.98 |
| Gender | (n, %) | |||
| Female | 65 (60%) | 68 (65%) | 0.44 | |
| Male | 44 (40%) | 37 (35%) | ||
| BMI (kg/m²) | 29.5 (±2.3) 29 (28.0–31.0) |
28.8 (±3.1) 28.5 (26.5–31.0) |
0.19 | |
| ASA grade | (n, %) | |||
| I | 8 | 6 | 0.290 | |
| II | 45 | 43 | ||
| III | 50 | 51 | ||
| IV | 6 | 5 | ||
| Fracture location | (n, %) | |||
| Femoral neck fracture | 39 (36%) | 38 (36%) | 0.53 | |
| Intertrochanteric fracture | 70 (64%) | 67 (64%) | ||
| Surgery | (n, %) | |||
| Hemiarthroplasty | 35 (32.1%) | 31 (29.5%) | 0.658 | |
| Total hip arthroplasty | 6 (5.5%) | 9 (8.6%) | ||
| Intramedullary nail | 68 (62.4%) | 65 (61.9%) | ||
| Preoperative haemoglobin level (g/dL) |
Mean ± SD Median (IQR) |
10.78 ± 1.74 10.85 (9.6–12.0) |
10.47 ± 1.96 10.55 (9.2–11.7) |
0.955 |
| Preoperative anemia | (n, %) | 88 (81%) | 86 (82%) | 0.826 |
| Comorbidities | FCM Group (n=109) |
Control Group (n=105) | P values |
|---|---|---|---|
| Number of comorbidities | |||
| 0-1 | 32 (29%) | 31 (30%) | 0.979 |
| ≥2 | 77 (71%) | 74 (70%) | |
| Renal dysfunction | 11 (10%) | 12 (11%) | 0.752 |
| Hypertension | 78 (72%) | 71 (68%) | 0.531 |
| Cardiac disease a | 36 (33%) | 32 (31%) | 0.689 |
| Diabetes Mellitus | 33 (30%) | 35 (33%) | 0.631 |
| Thyroid dysfunction | 12 (11%) | 13 (12%) | 0.910 |
| COPD | 20 (19%) | 13 (12%) | 0.149 |
| Neurological disorders b | 17 (16%) | 13 (12%) | 0.498 |
| Dementia | 7 (7%) | 19 (17%) | 0.016 |
| Malignancy | 10 (9%) | 6 (6%) | 0.336 |
|
CCI,Mean ± SD Median (IQR) |
4.81 ± 1.68 5 (2–4) |
4.58 ± 1.52 4 (1–2) |
0.326 |
| Variables | FCM Group (n=109) | Control Group (n=105) | P values | |
|---|---|---|---|---|
| Primary Outcomes | ||||
| 6-month mortality rate | n (%) | 25 (23%) | 41 (39%) | 0.011 |
| 1-year mortality rate | 31 (28%) | 45 (43%) | 0.028 | |
| Secondary Outcomes | ||||
| Anemia rates | ||||
| Preoperative | n (%) | 88 (81%) | 86 (82%) | 0.826 |
| Postoperative | 107 (98%) | 101 (96%) | 0.382 | |
| At discharge | 106 (97%) | 99 (94%) | 0.281 | |
| At 6th week | 97 (89%) | 103 (98%) | 0.007 | |
| Hemoglobin levels (g/dL) | ||||
| Preoperative |
Mean ± SD Median (IQR) |
10.76 ± 1.74 10.8 [9.7–12.3] |
10.46 ± 1.96 10.5 [9.2–11.7] |
0.427 |
| Postoperative | 9.70 ± 1.35 9.6 [9.0–10.8] |
9.91 ± 1.20 9.9 [9.0–10.6] |
0.159 | |
| At discharge | 10.61 ± 8.89 9.7 [8.8–11.1] |
10.29 ± 1.01 10.2 [9.6–11.4] |
0.001 | |
| At 6th week | 11.57 ± 11.6 10.4 [9.4–11.0] |
10.30 ± 0.91 10.3 [9.9–10.9] |
0.242 | |
| Perioperative transfusion characteristic | ||||
|
Transfused patients (ES replacement) |
n (%) | 34 (30%) | 48 (46%) | 0.013 |
| 1–2 units | 33 (97%) | 45 (94%) | ||
| ≥3 units | 1 (3%) | 3 (6%) | ||
| Length of hospitalization (days) |
Mean ± SD Median (IQR) |
12.19 ± 9.58 10 [6,7,8,9,10] |
15.14 ± 12.7 11 [7,8,9,10,11,12,13,14] |
0.250 |
| Variable included in step 12 | OR (Exp(B)) | 95% CI | P values |
|---|---|---|---|
|
Preoperative IV FCM administration (Received vs. Not received) |
0.330 | 0.158 – 0.690 | 0.003 |
| Age (per year increase) | 1.062 | 1.017 – 1.109 | 0.006 |
| Gender (female vs male) | 0.424 | 0.188 – 0.956 | 0.038 |
|
Fracture type (femoral neck vs intertrochanteric) |
0.388 | 0.179 – 0.843 | 0.017 |
| CCI score (per point) | 1.398 | 1.070 – 1.827 | 0.014 |
| ASA class (high vs low) | 2.309 | 1.063 – 5.016 | 0.035 |
| Hypertension(Present vs. Absent) | 6.446 | 2.004 – 20.735 | 0.002 |
|
Neurologic disorders (Present vs. Absent) |
1.292 | 1.092 – 1.926 | 0.037 |
| Surgery: THA vs Hemiarthroplasty | 0.203 | 0.023 – 1.785 | 0.150 |
| Surgery: IMN vs Hemiarthroplasty | 1.257 | 0.448 – 3.526 | 0.659 |
|
ES transfusion (Received vs. Not received) |
2.074 | 0.988 – 4.355 | 0.054 |
| Variable included in step 13 | OR (Exp(B)) | 95% CI | P values |
|---|---|---|---|
|
Preoperative IV FCM administration (Received vs. Not received) |
0.449 | 0.227 – 0.887 | 0.021 |
| Age (per year increase) | 1.059 | 1.020 – 1.100 | 0.003 |
| Gender (female vs male) | 0.445 | 0.233 – 0.849 | 0.015 |
| CCI score (per point) | 1.248 | 1.036 – 1.504 | 0.019 |
| ASA class (high vs low) | 2.309 | 1.063 – 5.016 | 0.035 |
| Hypertension(Present vs. Absent) | 3.583 | 1.676 – 7.656 | 0.001 |
|
Neurologic disorders (Present vs. Absent) |
3.266 | 1.230 – 8.673 | 0.018 |
|
ES transfusion (Received vs. Not received) |
1.995 | 0.938 – 4.243 | 0.070 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




