1. Introduction
The whole-genome oral microbiome research is an emerging field [
1,
2,
3,
4,
5,
6,
7]. However, limited research has been published on the oral microbiome of patients with Epidermolysis bullosa (EB). EB is a group of rare genetic skin disorders characterized by fragile skin and mucous membranes, leading to blisters and wounds [
8]. Oral health complications, including chronic wounds, erosions, and microbial infections, are common in EB patients due to impaired barrier functions [
9,
10]. Studying the oral microbiome in EB patients using whole-genome sequencing (WGS) can provide insights into microbial diversity, pathogenic species, and functional pathways involved in oral health and disease. The influence of the oral microbiome in patients with EB arises from oral dysbiosis, or a disrupted balance of microbial communities. Chronic wounds and altered oral environments can allow opportunistic pathogens to flourish [
11].
WGS provides high-resolution profiling of bacteria, archaea, fungi, and viruses [
12]. Functional analysis of microbial genes can reveal potential impacts on wound healing and inflammation. Repeated trauma and wound care interventions may shift dermal and oral microbial populations [
13,
14,
15]. Moreover, limited dietary options due to oral pain or dysfunction can alter the oral microbiome [
16]. Therefore, identifying specific pathogens can guide antimicrobial treatments. Additionally, exploring beneficial microbes could lead to probiotic therapies that promote healing and prevent infections. For this study, a probiotic is defined as a microorganism that provides a health advantage to its host [
17]. Numerous research studies have been published on the effects of probiotics on inflammation and immune modulation [
18,
19].
The interaction between the oral microbiome and the host immune system could contribute to systemic inflammation, a common complication in EB [
17] [
20]. Research indicates that dental caries are more prevalent in dystrophic and junctional EB compared to unaffected individuals or other EB types [
21,
22]. While rampant caries seems to be related to soft tissue and enamel involvement in these two EB types, other, yet unclear cofactors must also play a role [
23]. An examination of 216 affected individuals revealed significant differences in oral soft tissue involvement among the various types of EB. The frequency of oral involvement was greater in the dominant dystrophic (81.1%) and simplex (generalized, 58.6%; localized, 34.7%) types than previously reported [
24].
Restrictions in the mobility of the mouth, tongue, and lips are frequently present in EB patients, with the most severe cases occurring in the RDEB group, highlighting the clinical relevance of optimizing symptomatic treatment [
25]. Due to blister formation and oral restrictions, the EB diet is almost always soft and often high in carbohydrates. Diet is one of the factors influencing the diversity and interactions of the oral microbiota [
26]. It has been established that diet affects the progression of tooth decay, tooth erosion, and periodontal disease [
27]. Indeed, a high-sugar diet adversely influences the balance of the oral microbiota and increases the risk of tooth decay [
28]. Unfortunately, many patients with EB adhere to a soft, high-carbohydrate diet that contributes to dental disease and oral inflammation. The abundance and diversity of oral microorganisms are significantly lower in individuals with higher sugar intake [
16,
29]. This lack of diversity may also contribute to oral diseases and painful inflammation. Increased Streptococcus species and decreased numbers of Proteobacteria, Pasteurellaceae, Bacteroidia, and Porphyromonas species have been observed in individuals on a high-sugar diet [
30].
The whole-genome deep sequencing analysis of the oral microbiome plays a crucial role in research applications and therapeutic development. Harnessing oral microbial gene products for wound care is vital for EB patients [
31]. Personalized medicine could tailor antimicrobial or probiotic interventions based on individual microbiome profiles. Disease monitoring using microbial markers to assess disease progression or treatment responses will be crucial for long-term treatment success [
32].
2. Materials and Methods
Salivary samples were collected from three patients diagnosed with epidermolysis bullosa and treated for it. The patients had consulted a private practitioner for dental care and consultation. The patients obtained a salivary sample at home and mailed it to the laboratory for processing. The samples were de-identified, and whole genome sequencing was carried out using a proprietary Bristle system. Total genomic DNA was extracted from the samples using a Zymobiomics DNA isolation kit. DNA underwent quality control to ensure high-quality isolation. Purified DNA was subjected to in-house library preparation methods to create Illumina sequencing libraries, which were quality-controlled through fragment analysis and pooled equimolar for sequencing. The pooled libraries were sequenced on an Illumina NovaSeq to generate at least 5 million paired-end reads per sample at a length of 150 bp. Bioinformatics The bioinformatics pipeline utilizes well-established algorithms that are widely used in academic and commercial labs. Fastqs were downsampled using seqtk to 5M reads and aligned to a human genome reference sequence (hg38) to eliminate human reads. The remaining reads were processed through Bristle's proprietary bioinformatics workflow to identify and quantify the relative abundance of bacterial species. In summary, raw sequencing data were mapped to over 30,000 bacterial reference genomes to assess the relative abundance of various bacterial strains, including those identified as periodontal and dental caries pathogens. An algorithm that considers the relative abundance of each bacterial strain was implemented to compute a risk score for both caries and gum disease. The Bristle algorithm calculates the abundance of disease- and health-associated bacterial strains supported by internal studies and peer-reviewed research articles. The Bristle Comprehensive Oral Microbiome Test achieves an AUC of 0.88, with 74% sensitivity and 85% specificity for periodontal disease (
Figure 1A), and an AUC of 0.81, with 69% sensitivity and 75% specificity for dental caries.
3. Results
3.1. Relative Abundance of Dominant Species
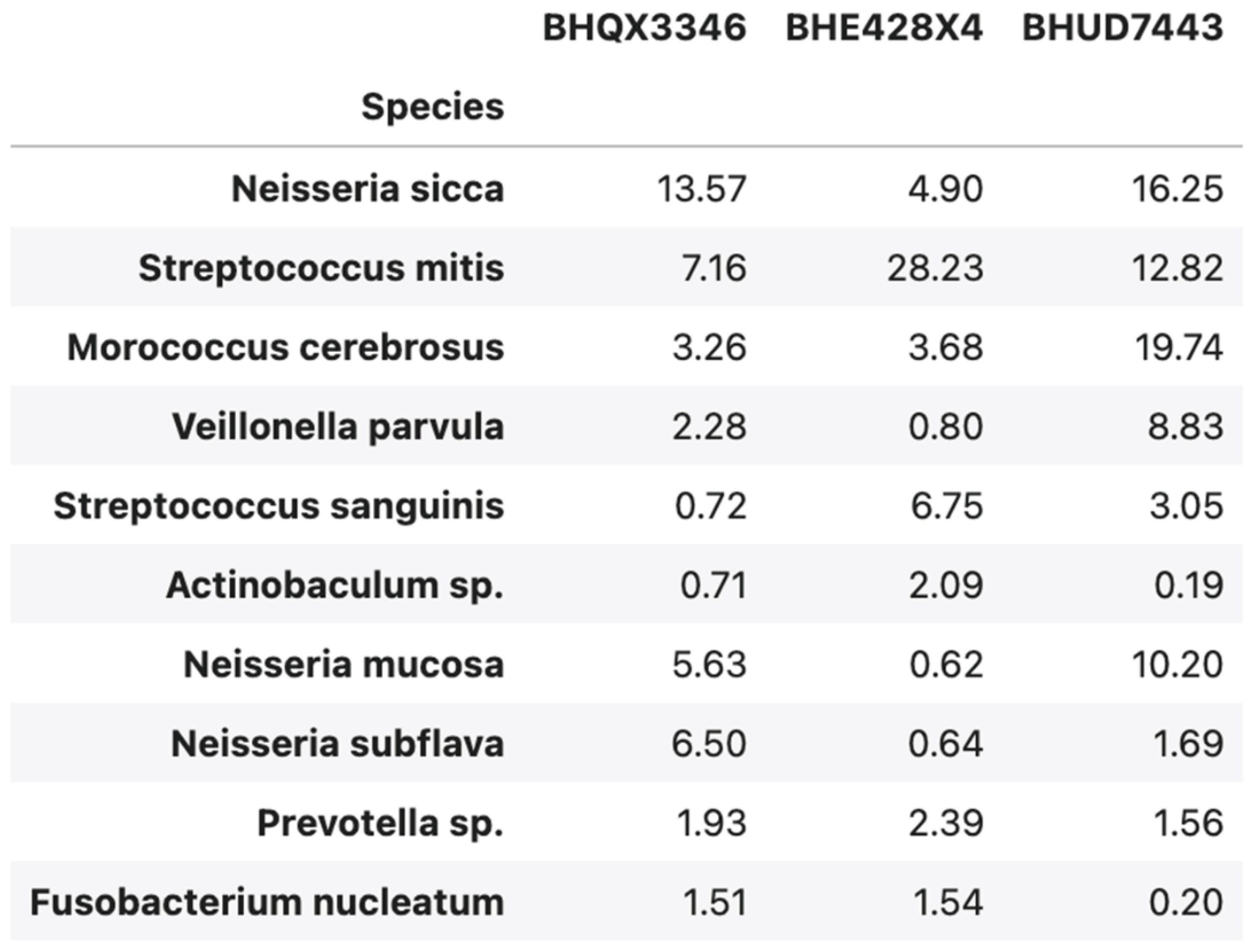
The whole genome of the oral microbiome of patients with epidermolysis bullosa revealed a commonality in microbial species. However, relative abundance differences were significant and possibly attributable to the extent of preventive dentistry provided (see
Table 1). Neisseria sicca was the most abundant in BHQ but not in BHE nor BHU (abbreviations of sample codes).
Heatmap of Species Relative Abundance
Significant inter-patient differences in microbiome composition exist, and a few prevalent species are common to all three (the horizontal bands that are consistently darker across all columns, see
Figure 2). Such differences can be linked to each patient’s unique condition and may deviate from typical population trends (e.g., the unusually high
M. cerebrosus in BHU).
3.2. Alpha Diversity
Alpha diversity measures the number of different species in a community and how evenly distributed they are. Here, we use the Shannon Diversity Index to compare the three samples. Higher values indicate greater diversity (a more significant number of species with more even abundances). A higher H' indicates more diversity. BHQ’s microbiome is the most diverse, whereas BHE’s is the least diverse.
3.3. Differential Abundance
Differential Abundance of Key Species
Particular bacterial species show marked differences in abundance between the patients, standing out as either dominant in one sample or rare/absent in others.
Table 2 below highlights a selection of such species and how their relative abundances vary across the three individuals:
This table highlights the unique features of each patient’s microbiome: for example, S. mitis comprises 28.2% in BHE (making it dominant there) but remains much lower in BHQ and BHU. Similarly, M. cerebrosus reaches 19.7% in BHU (an unusually high value) but is only about 3% in the others. N. sicca is found in all patients, yet BHE has relatively little compared to BHQ and BHU. We also observe species one patient has that others essentially do not (e.g., A. viscosus found only in BHQ). These differences are statistically significant given the small cohort and emphasize the personalized microbial signatures associated with each patient. While a single pathogen does not dominate BHQ, it features the exclusive presence of certain bacteria (e.g., A. viscosus) and moderate levels of others, enhancing its diversity. These variations may be clinically significant, as certain bacteria (such as Streptococcus and Actinomyces) are linked to oral health or disease states. The table illustrates that the dominant species in one patient can be minor or undetectable in another, underscoring the personalized nature of the oral microbiome in these EB patients.
Figure 3.
Principal Coordinates Analysis (PCoA) plot of beta diversity, comparing overall microbiome composition between the three patients. Each point represents one patient’s oral microbiome profile in a reduced dimensional space; the distance between points reflects how different the communities are. In this PCoA plot, the three samples do not cluster together, indicating clear compositional differences among them. Notably, the point for BHU (Patient 3) is separated far from BHQ and BHE, consistent with BHU’s distinct microbiome dominated by M. cerebrosus and other unique taxa. BHQ and BHE’s points sit somewhat closer, suggesting they share more similarities with each other than either does with BHU (for example, BHQ and BHE both contain Actinobaculum sp. and certain Actinomyces species that BHU lacks). Overall, the beta diversity analysis confirms that each patient harbors a markedly different community of oral microbes. These differences are also substantial compared to general population norms – all three EB patients’ profiles are significantly distinct from normotypical oral samples, underlining how the disease context (EB) might shift the microbiome composition. The PCoA visualization thus helps to identify which samples are more alike or divergent; in our case, it highlights BHU as an outlier community and suggests a moderate similarity between BHQ and BHE.
Figure 3.
Principal Coordinates Analysis (PCoA) plot of beta diversity, comparing overall microbiome composition between the three patients. Each point represents one patient’s oral microbiome profile in a reduced dimensional space; the distance between points reflects how different the communities are. In this PCoA plot, the three samples do not cluster together, indicating clear compositional differences among them. Notably, the point for BHU (Patient 3) is separated far from BHQ and BHE, consistent with BHU’s distinct microbiome dominated by M. cerebrosus and other unique taxa. BHQ and BHE’s points sit somewhat closer, suggesting they share more similarities with each other than either does with BHU (for example, BHQ and BHE both contain Actinobaculum sp. and certain Actinomyces species that BHU lacks). Overall, the beta diversity analysis confirms that each patient harbors a markedly different community of oral microbes. These differences are also substantial compared to general population norms – all three EB patients’ profiles are significantly distinct from normotypical oral samples, underlining how the disease context (EB) might shift the microbiome composition. The PCoA visualization thus helps to identify which samples are more alike or divergent; in our case, it highlights BHU as an outlier community and suggests a moderate similarity between BHQ and BHE.
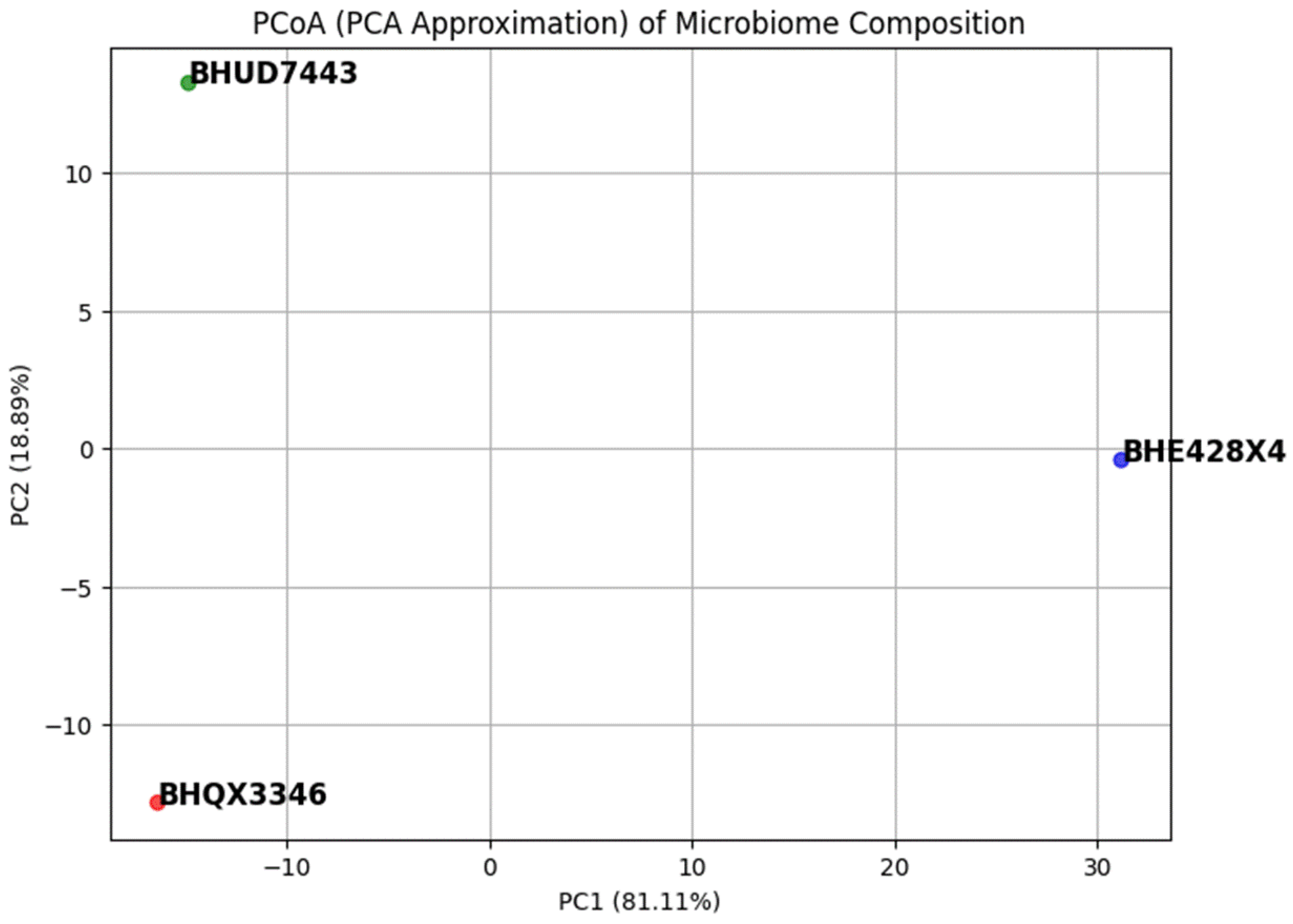
3.4. Beta Diversity
Beta Diversity (PCoA Plot)
High-Percentile Species Comparison
One way to understand how these patients’ microbiomes differ from general population trends is to look at which bacteria are unusually abundant
relative to a large reference population. We identified species at >90th percentile for each patient compared to a reference database (i.e., their abundance is higher than 90% of typical individuals).
Table 3 lists each sample's high-percentile species and their relative abundances. These high-percentile microbes can be considered unusual “signature” organisms for the patient since they flourish far more in these EB patients than in most people.
BHQ’s sample is remarkable for several high-percentile species like Actinobaculum sp. and
Veillonella parvula, reflecting its diverse but uniquely shifted community. BHE has S. mitis and a large fraction of unclassified Streptococcus at >90th percentile, consistent with its Streptococcus-dominated profile. BHU stands out with
M. cerebrosus at the 100th percentile (higher than any value in the reference data) and other high-percentile taxa (
S. sanguinis, S. sinensis) uncommon at such levels in typical populations. These findings underscore how the EB patients’ oral microbiomes contain certain bacteria in extreme abundance compared to expected trends, potentially contributing to disease-related oral health issues.
Table 4 shows that
BHQ and BHU have a broader array of high-percentile species (each has five or more species above the 90th percentile). In contrast, BHE
has a narrower set (only
N. sicca,
S. mitis, and one
Streptococcus sp. are above the 90th percentile for BHE). This suggests that BHQ and BHU harbor more unusual overgrowths of certain bacteria than typical individuals, reflecting a more significant deviation from the norm. For instance, BHQ’s high
Actinobaculum sp. (≈99th percentile) and BHU’s extremely high
M. cerebrosus (100th percentile) are apparent deviations from population averages. In contrast, aside from
S. mitis, BHE’s microbiome, while imbalanced, doesn’t feature as many extreme outlier species. Identifying these high-percentile organisms is essential because it highlights potential pathogens or keystone species that are unusually prolific in EB patients. These species could contribute to oral health issues (e.g., gum inflammation or caries risk) and represent targets for tailored treatment or further investigation.
Overall, the combined tables and figures illustrate that the oral microbiome in these three EB patients is markedly different from general population trends, with each patient showing unique dominant bacteria and a set of high-percentile “outlier” species. BHQ’s sample is highly diverse with several moderately high-abundance taxa, a typically common bacterium dominates BHE’s turned extreme, and BHU’s shows an unprecedented bloom of a usually minor species. These patterns underscore the need to consider personalized microbiome profiles in managing oral health for EB patients, as their microbial communities do not align with the norm and may require specialized interventions. The apparent differences in alpha diversity, specific species abundances, and beta diversity clustering all point to the distinctive ecological shifts in the oral microbiome associated with Epidermolysis Bullosa.
3.5. Deep Sequencing Data Summary
Neisseria sicca appears across all samples with relatively high percentiles (>95th percentile in all 3). Streptococcus mitis is present in all samples, with its percentile and abundance differing significantly between them. This is to be expected, though, given how common it is. Actinobaculum sp. It is present in two samples with a mean percentile of 97.77 and a maximum of 99.42) - These two samples had more similar Gum Inflammation and other scores than sample 3 - which was distinct from the other two. Dominant Species were present in the samples, with BHQ—Neisseria sicca dominating with a relative abundance of 13.57%. BHE—Streptococcus mitis was overwhelmingly dominant, accounting for 28.23% of the total community. BHU Morococcus cerebrosus was the top species with 19.74% relative abundance (100th percentile), an outlier compared to the other samples. This species is in ~60% of Bristle samples, but this is the highest they have noted.
All three samples (BHQ, BHE, and BHU) had at least one Actinomyces species ranked above the 70th percentile. Actinomyces species with >70 Percentile per Sample: BHQ three species above the 70th percentile, BHE one species above the 70th percentile, and BHU with one species above the 70th percentile. Two samples had Actinomyces species >85 Percentile, Actinomyces viscosus in BHQ (88.62 percentile, 1.24% relative abundance), Actinomyces naeslundii in BHQ (95.10 percentile, 0.51% relative abundance), and Actinomyces naeslundii in BHE (89.33 percentile, 0.31% relative abundance). BHQ exhibited Actinomyces species' highest diversity and dominance, particularly with multiple species exceeding the 85th percentile. Actinomyces naeslundii appears prominently in both BHQ and BHE, suggesting it may be a common, high-ranking species associated with these microbiomes.
4. Discussion
While fluoride has been considered the ‘gold standard’ for conservative caries management for over five decades, its ability to arrest dentin caries has proven insufficient [
33,
34]. Marinho et al. [
35] reported that fluoride varnish applications arrested only 37% of early childhood caries lesions. Systematic reviews indicate that SDF can stabilize approximately 50% of caries lesions in primary dentition [
33,
36]. Therefore, current preventive therapy for EB patients still seems inadequate, with dental treatment often urgently needed. Treatment is occasionally performed under general anesthesia in major medical centers. Haworth et al. found that therapy under general anesthesia is associated with compromised oral health and an increased likelihood of dental fear and anxiety in the future [
37]. Additionally, children whose primary teeth were treated under general anesthesia exhibited a higher severity of caries in their permanent dentition [
37].
Dental caries, a complex condition influenced by multiple factors, remains a prevalent chronic disease among children [
38]. Despite ongoing efforts to implement preventive measures and modify behavioral factors, epidemiological studies report alarmingly high rates of dental caries [
39,
40]. Between 1990 and 2019, there was an average 3% reduction in the prevalence of dental caries, but the number of new cases increased by 6%, resulting in a staggering 1.15 billion untreated dental caries cases [
41,
42]. Improved management of this common chronic disease is required, especially in individuals with concomitant systemic disease. The bacterial species detected in the EB patients’ samples must be explicitly studied to determine their potential health complications.
Actinomyces naeslundii is a Gram-positive, rod-shaped bacterium found in humans' mouths. The species has been implicated in periodontal disease and dental caries [
43]. In other cases,
A. naeslundii has been associated with good oral health. It is one of the first bacteria to occupy the oral cavity and colonize the tooth's surface.
A. naeslundii may behave as a pathobiont in certain host situations.
Neisseria sicca is a commensal organism belonging to the genus Neisseria. It is Gram-negative and oxidase-positive. Multiple strains of this species exist, some of which have been reported to have caused septicemia in immunocompromised patients [
44].
Streptococcus mitis is a species of Gram-positive, mesophilic, alpha-hemolytic bacteria in the genus Streptococcus. These facultative anaerobes consist of non-motile and non-sporing cocci that are catalase-negative.
Streptococcus mitis is a commensal and commonly inhabits the human mouth, throat, and upper respiratory tract as part of the oral microbiota and the gastrointestinal tract [
45].
Morrocus cerebrosus is a gram-negative, oxidase-positive, aggregate-forming coccus found in healthy controls and periodontal patients during pregnancy [
46,
47]. It may be more prevalent in adolescents with fluorosis [
48].
The whole genome deep sequencing of the three patients with Epidermolysis bullosa was just a pilot study done as part of their oral health care. The surprisingly significant differences between the oral microbiome of EB patients and the vast normotypical oral microbiome in an extensive database should encourage far larger prospective studies and the implementation of large randomized clinical trials with multiple therapeutic interventions to determine the best possible therapy to reduce oral disease. Patients suffering from Epidermolysis bullosa should receive the best oral care possible, and recognizing the significant difference in their oral microbiota is just the first step. Recent WGS studies of specific human microbiomes have provided data necessary for understanding the differences between healthy and dysbiotic microbiota that strongly influence human health [
49,
50,
51,
52]. While xylitol and probiotics have proven effective in preventing dental disease, their efficacy in Epidermolysis bullosa patients remains unstudied, and this pilot study has provided the first information on their oral microbiome.
5. Conclusions
Epidermolysis bullosa is a very severe, although rare, disease. Patients with EB have a lifetime of painful blisters, scarring, and other complications that the general population is often unaware of. Understanding the EB oral microbiome and the adverse effects of their specific pathogens can help healthcare professionals provide some relief and comfort through appropriate treatment. Specifically, probiotics targeted to address the dysbiosis in EB patients’ oral microbiomes could improve the incidence of dental caries and gingival inflammation. Further analysis with a greater representation of the various subtypes of EB will allow for a better understanding of which pathogens to target.
Author Contributions
Conceptualization, M.C. and B.M.; methodology, B.M.; software, B.M.; validation, A.V., L.G. and S.B.; formal analysis, B.M.; investigation, M.C.; resources, A.V.; data curation, M.B.; writing—original draft preparation, M.C.; writing—review and editing, L.G. and S. B.; visualization, C.X.; supervision, M.C.; project administration, A.V.; funding acquisition, M.C. All authors have read and agreed to the published version of the manuscript
Funding
This research was funded by a non-restricted grant from The Swanson Fund
Institutional Review Board Statement
Ethical review and approval were waived for this study due to the retrospective nature of the research.
Informed Consent Statement
Informed consent was obtained by Bristle Health as part of their established protocol.
Data Availability Statement
Data is available at Bristle Health, requiring written permission from subjects.
Acknowledgments
Dr. Amy Paller, thank you for the many years of dedication to the health of patients with epidermolysis bullosa.
Conflicts of Interest
The authors declare no conflicts of interest in the results. Brina Maurer is a co-founder of Bristle Health
Abbreviations
The following abbreviations are used in this manuscript:
| MDPI |
Multidisciplinary Digital Publishing Institute |
| DOAJ |
Directory of open access journals |
| TLA |
Three letter acronym |
| LD |
Linear dichroism |
References
- Baker, J.L. Illuminating the oral microbiome and its host interactions: recent advancements in omics and bioinformatics technologies in the context of oral microbiome research. FEMS microbiology reviews 2023, 47, fuad051. [Google Scholar] [CrossRef] [PubMed]
- Manghi, P.; Filosi, M.; Zolfo, M.; et al. Large-scale metagenomic analysis of oral microbiomes reveals markers for autism spectrum disorders. Nat Commun 2024, 15, 9743. [Google Scholar] [CrossRef] [PubMed]
- Gao, L.; Xu, T.; Huang, G.; Jiang, S.; Gu, Y.; Chen, F. Oral microbiomes: more and more importance in oral cavity and whole body. Protein & cell 2018, 9, 488–500. [Google Scholar] [CrossRef]
- Caselli, E.; Fabbri, C.; D'Accolti, M.; Soffritti, I.; Bassi, C.; Mazzacane, S.; Franchi, M. Defining the oral microbiome by whole-genome sequencing and resistome analysis: the complexity of the healthy picture. BMC microbiology 2020, 20, 120. [Google Scholar] [CrossRef]
- Bhandary, R.; Venugopalan, G.; Ramesh, A.; Tartaglia, G.M.; Singhal, I.; Khijmatgar, S. Microbial Symphony: Navigating the Intricacies of the Human Oral Microbiome and Its Impact on Health. Microorganisms 2024, 12, 571. [Google Scholar] [CrossRef]
- Liu, X.; Tong, X.; Zhu, J.; et al. Metagenome-genome-wide association studies reveal human genetic impact on the oral microbiome. Cell Discov 2021, 7, 117. [Google Scholar] [CrossRef]
- Brzychczy-Sroka, B.; Talaga-Ćwiertnia, K.; Sroka-Oleksiak, A.; Gurgul, A.; Zarzecka-Francica, E.; Ostrowski, W.; Kąkol, J.; Drożdż, K.; Brzychczy-Włoch, M.; Zarzecka, J. Standardization of the protocol for oral cavity examination and collecting of the biological samples for microbiome research using the next-generation sequencing (NGS): own experience with the COVID-19 patients. Scientific reports 2024, 14, 3717. [Google Scholar] [CrossRef]
- Bardhan, A.; Bruckner-Tuderman, L.; Chapple, I.L.C.; et al. Epidermolysis bullosa. Nat Rev Dis Primers 2020, 6, 78. [Google Scholar] [CrossRef]
- Mariath, L.M.; Santin, J.T.; Schuler-Faccini, L.; Kiszewski, A.E. Inherited epidermolysis bullosa: update on the clinical and genetic aspects. Anais brasileiros de dermatologia 2020, 95, 551–569. [Google Scholar] [CrossRef]
- Pope, Elena MD, MSc, FRCPC; Lara-Corrales, Irene MD, FRCPC (Derm); Mellerio, Jemima E. BSc, MD, FRCP; Martinez, Anna E. MBBS,MRCP,MRCPCH; Sibbald, Cathryn RPh, BScPhm, ACPR; Sibbald, R. Gary BSc, MD, MEd, FRCPC (Med) (Derm), FACP, FAAD, MAPWCA, for the EB International Consensus Panel. Epidermolysis Bullosa and Chronic Wounds: A Model for Wound Bed Preparation of Fragile Skin. Advances in Skin & Wound Care 2013, 26, 177–188. [Google Scholar] [CrossRef]
- Uberoi, A.; McCready-Vangi, A.; Grice, E.A. The wound microbiota: microbial mechanisms of impaired wound healing and infection. Nat Rev Microbiol 2024, 22, 507–521. [Google Scholar] [CrossRef] [PubMed]
- Purushothaman, S.; Meola, M.; Egli, A. Combination of Whole Genome Sequencing and Metagenomics for Microbiological Diagnostics. International Journal of Molecular Sciences 2022, 23, 9834. [Google Scholar] [CrossRef] [PubMed]
- Krämer, S.M.; Serrano, M.C.; Zillmann, G.; Gálvez, P.; Araya, I.; Yanine, N.; Carrasco-Labra, A.; Oliva, P.; Brignardello-Petersen, R.; Villanueva, J. DEBRA International Oral health care for patients with epidermolysis bullosa--best clinical practice guidelines. International journal of paediatric dentistry 2012, 22, 1–35. [Google Scholar] [CrossRef]
- Eriksson, E.; Liu, P.Y.; Schultz, G.S.; Martins-Green, M.M.; Tanaka, R.; Weir, D.; Gould, L.J.; Armstrong, D.G.; Gibbons, G.W.; Wolcott, R.; Olutoye, O.O.; Kirsner, R.S.; Gurtner, G.C. Chronic wounds: Treatment consensus. Wound repair and regeneration : official publication of the Wound Healing Society [and] the European Tissue Repair Society 2022, 30, 156–171. [Google Scholar] [CrossRef]
- Schultz, G.; Bjarnsholt, T.; James, G.A.; Leaper, D.J.; McBain, A.J.; Malone, M.; Stoodley, P.; Swanson, T.; Tachi, M.; Wolcott, R.D. Global Wound Biofilm Expert Panel Consensus guidelines for the identification and treatment of biofilms in chronic nonhealing wounds. Wound repair and regeneration : official publication of the Wound Healing Society [and] the European Tissue Repair Society 2017, 25, 744–757. [Google Scholar] [CrossRef]
- Esberg, A.; Haworth, S.; Hasslöf, P.; Lif Holgerson, P.; Johansson, I. Oral microbiota profile associates with sugar intake and taste preference genes. Nutrients. 2020, 12, 681. [Google Scholar] [CrossRef]
- Yan, F.; Polk, D.B. Probiotics and immune health. Current opinion in gastroenterology 2011, 27, 496–501. [Google Scholar] [CrossRef]
- Gilad, O.; Svensson, B.; Viborg, A.H.; Stuer-Lauridsen, B.; Jacobsen, S. The extracellular proteome of Bifidobacterium animalis subsp. lactis BB-12 reveals proteins with putative roles in probiotic effects. Proteomics 2011, 11, 2503–2514. [Google Scholar] [CrossRef]
- Cristofori, F.; Dargenio, V.N.; Dargenio, C.; Miniello, V.L.; Barone, M.; Francavilla, R. Anti-Inflammatory and Immunomodulatory Effects of Probiotics in Gut Inflammation: A Door to the Body. Frontiers in immunology 2021, 12, 578386. [Google Scholar] [CrossRef]
- Kleinstein, S.E.; Nelson, K.E.; Freire, M. Inflammatory Networks Linking Oral Microbiome with Systemic Health and Disease. Journal of dental research 2020, 99, 1131–1139. [Google Scholar] [CrossRef]
- Louloudiadis, A.K.; Louloudiadis, K.A. Case report: Dystrophic Epidermolysis Bullosa: dental management and oral health promotion. European archives of paediatric dentistry : official journal of the European Academy of Paediatric Dentistry 2009, 10, 42–45. [Google Scholar] [CrossRef] [PubMed]
- Wright, J.T. Oral manifestations in the epidermolysis bullosa spectrum. Dermatologic clinics 2010, 28, 159–164. [Google Scholar] [CrossRef]
- Wright, J.T.; Fine, J.D.; Johnson, L. Dental caries risk in hereditary epidermolysis bullosa. Pediatric dentistry 1994, 16, 427–432. [Google Scholar] [PubMed]
- Wright, J.T.; Fine, J.D.; Johnson, L.B. Oral soft tissues in hereditary epidermolysis bullosa. Oral surgery, oral medicine, and oral pathology, 1991, 71, 440–446. [Google Scholar] [CrossRef] [PubMed]
- Stellingsma, C.; Dijkstra, P.U.; Dijkstra, J.; Duipmans, J.C.; Jonkman, M.F.; Dekker, R. Restrictions in oral functions caused by oral manifestations of epidermolysis bullosa. European journal of dermatology : EJD 2011, 21, 405–409. [Google Scholar] [CrossRef]
- Angarita-Díaz, M.D.P.; Fong, C.; Bedoya-Correa, C.M.; Cabrera-Arango, C.L. Does high sugar intake really alter the oral microbiota? : A systematic review. Clin. Exp. Dent. Res. 2022, 8, 1376–1390. [Google Scholar] [CrossRef]
- Kantorowicz, M.; Olszewska-Czyż, I.; Kolarzyk, E.; Chomyszyn-Gajewska, M. Influence of diet on oral health in young adults–pilot study. Przegl. Lek. 2014, 71, 505–511. [Google Scholar]
- Anderson, C.A.; Curzon, M.E.; Van Loveren, C.; Tatsi, C.; Duggal, M.S. Sucrose and dental caries: A review of the evidence. Obes. Rev. 2009, 10, 41–54. [Google Scholar] [CrossRef]
- Esberg, A.; Eriksson, L.; Hasslöf, P.; Haworth, S.; Holgerson, P.L.; Johansson, I. Using oral microbiota data to design a short sucrose intake index. Nutrients. 2021, 13, 1400. [Google Scholar] [CrossRef]
- Anderson, A.C.; Rothballer, M.; Altenburger, M.J. , et al. In-vivo shift of the microbiota in oral biofilm in response to frequent sucrose consumption. Sci. Rep. 2018, 8, 14202. [Google Scholar] [CrossRef]
- Misic, A.M.; Gardner, S.E.; Grice, E.A. The Wound Microbiome: Modern Approaches to Examining the Role of Microorganisms in Impaired Chronic Wound Healing. Advances in wound care 2014, 3, 502–510. [Google Scholar] [CrossRef] [PubMed]
- Gao, W.; Lin, W.; Li, Q.; et al. Identification and validation of microbial biomarkers from cross-cohort datasets using xMarkerFinder. Nat Protoc 2024, 19, 2803–2830. [Google Scholar] [CrossRef] [PubMed]
- Duangthip, M.C.M.; Wong, C.H.; Chu, E.C.M.L. Caries arrest by topical fluorides in preschool children: 30-month results. Journal of Dentistry 2018, 70, 74–79. [Google Scholar] [CrossRef] [PubMed]
- Horst, J.A.; Tanzer, J.M.; Milgrom, P.M. Fluorides and Other Preventive Strategies for Tooth Decay. Dental clinics of North America 2018, 62, 207–234. [Google Scholar] [CrossRef]
- Marinho, V.C.; Worthington, H.V.; Walsh, T.; Clarkson, J.E. Fluoride varnishes for preventing dental caries in children and adolescents. The Cochrane database of systematic reviews 2013, 2013, CD002279. [Google Scholar] [CrossRef]
- Zaffarano, L.; Salerno, C.; Campus, G.; Cirio, S.; Balian, A.; Karanxha, L.; Cagetti, M.G. Silver Diamine Fluoride (SDF) Efficacy in Arresting Cavitated Caries Lesions in Primary Molars: A Systematic Review and Metanalysis. International journal of environmental research and public health 2022, 19, 12917. [Google Scholar] [CrossRef]
- Haworth, S.; Dudding, T.; Waylen, A.; Thomas, S.J.; Timpson, N.J. Ten years on: Is dental general anaesthesia in childhood a risk factor for caries and anxiety? . British dental journal 2017, 222, 299–304. [Google Scholar] [CrossRef]
- Mathur, V.P.; Dhillon, J.K. Dental Caries: A Disease Which Needs Attention. Indian journal of pediatrics 2018, 85, 202–206. [Google Scholar] [CrossRef]
- Kazeminia, M.; Abdi, A.; Shohaimi, S.; Jalali, R.; Vaisi-Raygani, A.; Salari, N.; Mohammadi, M. Dental caries in primary and permanent teeth in children's worldwide, 1995 to 2019: a systematic review and meta-analysis. Head & face medicine 2020, 16, 22. [Google Scholar] [CrossRef]
- Wen PY, F.; Chen, M.X.; Zhong, Y.J.; Dong, Q.Q.; Wong, H.M. Global Burden and Inequality of Dental Caries, 1990 to 2019. Journal of dental research 2022, 101, 392–399. [Google Scholar] [CrossRef]
- Zhao, G.N.; Wong, H.M.; Wen PY, F.; Wu, Y.; Zhong, Y.J.; Jiang, Y. Burden, Trends, and Inequality of Dental Caries in the U. S., 1990-2019. American journal of preventive medicine 2023, 64, 788–796. [Google Scholar] [CrossRef] [PubMed]
- Sun, R.; Xu, X.; Dong, Y.; Li, J.; Guan, W.; Huang, Y.; Li, S.; Wang, Y.; Li, J. Global and regional trends in prevalence of untreated caries in permanent teeth: Age-period-cohort analysis from 1990 to 2019 and projections until 2049. Journal of dentistry 2024, 147, 105122. [Google Scholar] [CrossRef] [PubMed]
- Palmer, R.J., Jr. Composition and development of oral bacterial communities. Periodontology 2000 2014, 64, 20–39. [Google Scholar] [CrossRef]
- Russo, K.A.; Louie, T. A case of Neisseria sicca bacteremia due to eculizumab therapy. AIM Clinical Cases 2023, 2, e220934. [Google Scholar] [CrossRef]
- Sharma, A.; Masood, U.; Kahlon, A.; Pattar, S.; Iqbal, S.; Lehmann, D. Streptococcus mitis bacteremia and endocarditis: An early sign in pre-cancerous colon polyps. American Journal of Gastroenterology 2016, 111, S616. [Google Scholar] [CrossRef]
- Zhao, M.; Yang, C.; Zhu, L.; Guo, X.; Ma, H.; Luo, Y.; Wang, Q.; Chen, J. Multiomics Analysis Reveals Significant Disparities in the Oral Microbiota and Metabolites Between Pregnant Women with and without Periodontitis. Infection and drug resistance 2024, 17, 4665–4683. [Google Scholar] [CrossRef]
- Baris, O.; Demir, T.; Gulluce, M. Investigation of In vitro Mineral forming bacterial isolates from supragingival calculus. Nigerian journal of clinical practice 2017, 20, 1571–1575. [Google Scholar] [CrossRef]
- Wang, Q.; Chen, X.; Hu, H. , et al. Structural changes in the oral microbiome of the adolescent patients with moderate or severe dental fluorosis. Sci Rep. 2021, 11, 2897. [Google Scholar] [CrossRef]
- Brlek, P.; Bulić, L.; Bračić, M.; Projić, P.; Škaro, V.; Shah, N.; Shah, P.; Primorac, D. Implementing whole genome sequencing (WGS) in clinical practice: Advantages, challenges, and future perspectives. Cells 2024, 13, 504. [Google Scholar] [CrossRef]
- Cannon, M.; Ferrer, G.; Tesch, M.; Schipma, M. Whole-genome deep sequencing of the healthy adult nasal microbiome. Microorganisms 2024, 12, 1407. [Google Scholar] [CrossRef]
- Caselli, E.; Fabbri, C.; D'Accolti, M.; Soffritti, I.; Bassi, C.; Mazzacane, S.; Franchi, M. Defining the oral microbiome by whole-genome sequencing and resistome analysis: The complexity of the healthy picture. BMC Microbiology, 2014, 20, 120. [Google Scholar] [CrossRef] [PubMed]
- Ye, J.; Lv, Y.; Xie, H.; Lian, K.; Xu, X. Whole-genome metagenomic analysis of the oral microbiota in patients with obstructive sleep apnea comorbid with major depressive disorder. Nature and Science of Sleep 2024, 16, 1091–1108. [Google Scholar] [CrossRef]
Figure 1.
Stacked bar chart comparing the relative abundance of dominant oral bacteria across the three patient samples. Each bar represents one patient’s microbiome, with segments colored by bacterial species. The chart highlights that each patient has a different dominant species: one sample (BHE) is overwhelmingly dominated by Streptococcus mitis (~28% of the community), another (BHU) by Morococcus cerebrosus (~19.7%), while the third (BHQ) shows a more balanced profile with Neisseria sicca (~13.6%) as the top species. In BHE, S. mitis far exceeds its levels in the other patients, whereas BHU’s M. cerebrosus is an outlier – present at the highest concentration yet observed in any sample. BHQ’s community is more evenly distributed among several species, reflecting higher diversity. This visual emphasizes the distinct microbial profiles: for example, N. sicca is present in all three but at varying levels, and some major taxa in one patient are only minor in others (as seen by the different segment sizes for each bar).
Figure 1.
Stacked bar chart comparing the relative abundance of dominant oral bacteria across the three patient samples. Each bar represents one patient’s microbiome, with segments colored by bacterial species. The chart highlights that each patient has a different dominant species: one sample (BHE) is overwhelmingly dominated by Streptococcus mitis (~28% of the community), another (BHU) by Morococcus cerebrosus (~19.7%), while the third (BHQ) shows a more balanced profile with Neisseria sicca (~13.6%) as the top species. In BHE, S. mitis far exceeds its levels in the other patients, whereas BHU’s M. cerebrosus is an outlier – present at the highest concentration yet observed in any sample. BHQ’s community is more evenly distributed among several species, reflecting higher diversity. This visual emphasizes the distinct microbial profiles: for example, N. sicca is present in all three but at varying levels, and some major taxa in one patient are only minor in others (as seen by the different segment sizes for each bar).
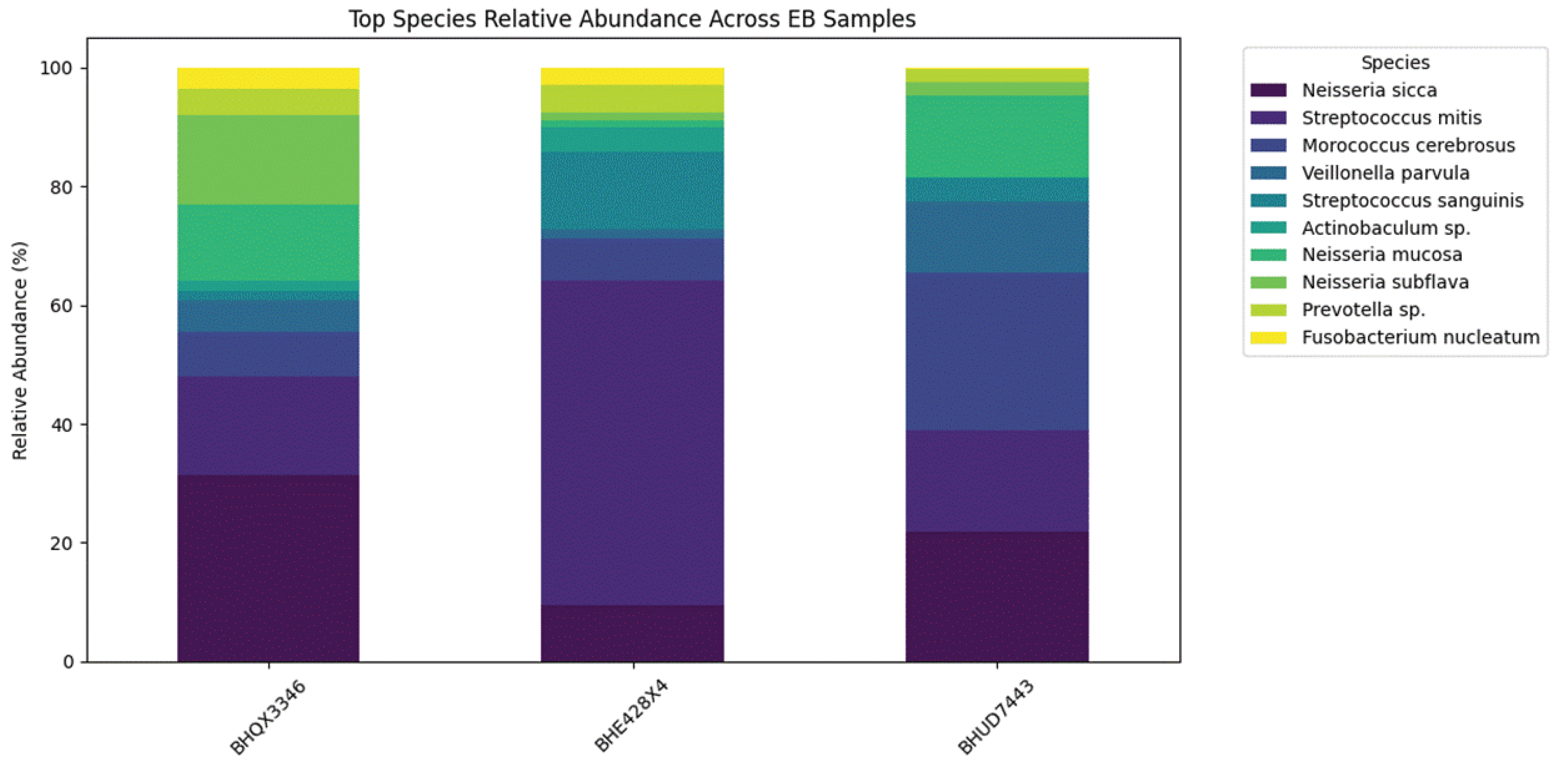
Figure 2.
Heatmap of oral microbiome species’ relative abundances in the three patients. Rows correspond to bacterial species; columns are the patient samples (BHQ, BHE, BHU). Color intensity represents the relative abundance (darker = more abundant). This heatmap underscores both shared and unique microbial patterns across the patients. For instance, certain species (e.g., Neisseria sicca) show high abundance (dark cells) across all individuals, indicating typical core microbiota. In contrast, other species are highly abundant in only one patient but nearly absent in the others (dark cell in one column, light in the others). For example, S. mitis is strongly enriched in BHE, and M. cerebrosus in BHU, consistent with the bar chart. Many lighter-colored cells in BHE’s column (aside from S. mitis) suggest that most other taxa are comparatively low due to the dominance of S. mitis. Meanwhile, BHQ’s column has moderately intense signals for a wider range of species, reflecting a more even community. Overall, the heatmap visually highlights the significant inter-patient differences in microbiome composition while also showing a few prevalent species common to all three (the horizontal bands are consistently darker across all columns.
Figure 2.
Heatmap of oral microbiome species’ relative abundances in the three patients. Rows correspond to bacterial species; columns are the patient samples (BHQ, BHE, BHU). Color intensity represents the relative abundance (darker = more abundant). This heatmap underscores both shared and unique microbial patterns across the patients. For instance, certain species (e.g., Neisseria sicca) show high abundance (dark cells) across all individuals, indicating typical core microbiota. In contrast, other species are highly abundant in only one patient but nearly absent in the others (dark cell in one column, light in the others). For example, S. mitis is strongly enriched in BHE, and M. cerebrosus in BHU, consistent with the bar chart. Many lighter-colored cells in BHE’s column (aside from S. mitis) suggest that most other taxa are comparatively low due to the dominance of S. mitis. Meanwhile, BHQ’s column has moderately intense signals for a wider range of species, reflecting a more even community. Overall, the heatmap visually highlights the significant inter-patient differences in microbiome composition while also showing a few prevalent species common to all three (the horizontal bands are consistently darker across all columns.
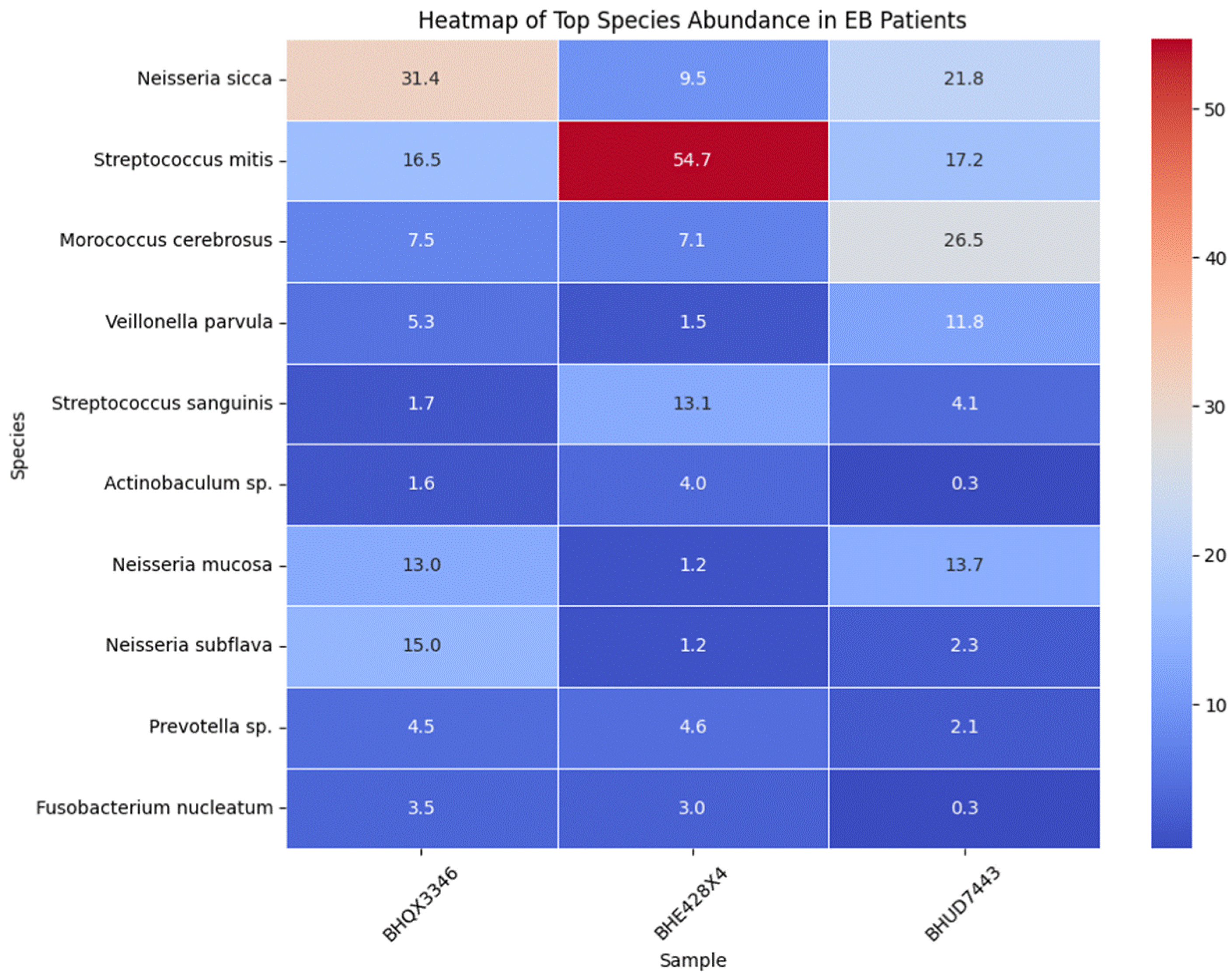
Table 1.
Relative Abundance of Dominant Species (Stacked Bar Chart).
Table 1.
Relative Abundance of Dominant Species (Stacked Bar Chart).
Table 2.
Shannon Diversity Index for Each Patient’s Sample – This table shows that BHQ’s sample has the highest diversity, while BHE’s is the lowest. BHQ’s oral microbiome is the most diverse (Shannon ≈ 3.3), reflecting a community with many species at relatively balanced abundances. BHU’s diversity is intermediate (Shannon ≈ 2.8), and BHE’s sample has the lowest diversity (Shannon ≈ 2.4), consistent with the dominance of a single species in BHE. These findings align with observations that BHQ harbors a broad range of microbes (including several moderately abundant species), whereas BHE is skewed towards one predominant bacterium
Table 2.
Shannon Diversity Index for Each Patient’s Sample – This table shows that BHQ’s sample has the highest diversity, while BHE’s is the lowest. BHQ’s oral microbiome is the most diverse (Shannon ≈ 3.3), reflecting a community with many species at relatively balanced abundances. BHU’s diversity is intermediate (Shannon ≈ 2.8), and BHE’s sample has the lowest diversity (Shannon ≈ 2.4), consistent with the dominance of a single species in BHE. These findings align with observations that BHQ harbors a broad range of microbes (including several moderately abundant species), whereas BHE is skewed towards one predominant bacterium
| Sample ID |
Shannon Diversity Index (H') |
|
BHQ (Patient 1) |
3.3 (highest diversity) |
|
BHE (Patient 2) |
2.4 (lowest diversity) |
|
BHU (Patient 3) |
2.8 (intermediate) |
Table 3.
Differentially Abundant Species Across the Three Samples – Each row lists a species that differs significantly between patients, with its relative abundance (%) in each sample. Bolded values indicate notably high abundance in that sample.
Table 3.
Differentially Abundant Species Across the Three Samples – Each row lists a species that differs significantly between patients, with its relative abundance (%) in each sample. Bolded values indicate notably high abundance in that sample.
| Species |
BHQ (% RA) |
BHE (% RA) |
BHU (% RA) |
Notable Differences |
| Streptococcus mitis |
~12.0% |
28.2% |
~7.1% |
Dominant in BHE; much lower in BHQ/BHU. |
| Neisseria sicca |
13.6% |
4.9% |
16.3% |
Present in all, but lowest in BHE (common core species). |
| Morococcus cerebrosus |
3.7% |
3.3% |
19.7% |
Dramatically higher in BHU (top species). |
| Streptococcus sanguinis |
3.1% |
0.1% |
6.8% |
High in BHU, nearly absent in BHE. |
| Actinomyces viscosus |
1.24% |
0% |
0% |
Detected only in BHQ (unique to BHQ). |
Table 4.
Species with Abundance Above the 90th Percentile in Each Patient (and their relative abundance). This comparison shows that BHQ and BHU each have multiple species at exceptionally high percentiles, whereas BHE has fewer such outliers. For example, Neisseria sicca is >95th percentile in all three patients (a common high-abundance organism in EB patients).
Table 4.
Species with Abundance Above the 90th Percentile in Each Patient (and their relative abundance). This comparison shows that BHQ and BHU each have multiple species at exceptionally high percentiles, whereas BHE has fewer such outliers. For example, Neisseria sicca is >95th percentile in all three patients (a common high-abundance organism in EB patients).
|
Species (>90th percentile)
|
BHQ (Patient 1) |
BHE (Patient 2) |
BHU (Patient 3) |
| Neisseria sicca |
13.6% ✔ |
4.9% ✔ |
16.3% ✔ |
| Streptococcus mitis |
– |
28.2% ✔ |
– |
| Streptococcus (unclassified) |
– |
11.0% ✔ |
– |
| Morococcus cerebrosus |
3.7% ✔ |
3.3% ✔ |
19.7%✔
|
| Streptococcus sanguinis |
– |
– |
6.8% ✔ |
| Streptococcus sinensis |
– |
– |
0.7% ✔ |
| Actinobaculum sp. |
2.1%✔
|
0.7% ✔ |
– |
| Actinomyces naeslundii |
0.5% ✔ |
– |
– |
| Veillonella parvula |
8.8% ✔ |
– |
– |
|
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).