Submitted:
12 April 2025
Posted:
14 April 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Immortalized Murine Myoblast Cell Line (C2C12)
2.2. C2C12 BMPRIa Knockout Cell Line
2.3. Mice Subjects
2.4. Euthanasia and Isolation of Bone Marrow Stem Cells from B6 Mice
2.5. C2C12 Cell Culture
2.6. Primary Cell Culture
2.7. Immunostaining of primary cells
2.8. Immunofluorescence Quantification
2.9. Lysate Collection for Western Blotting
2.10. Western Blotting
2.11. Oil Red O Staining Protocol
2.12. Statistical Analysis
3. Results
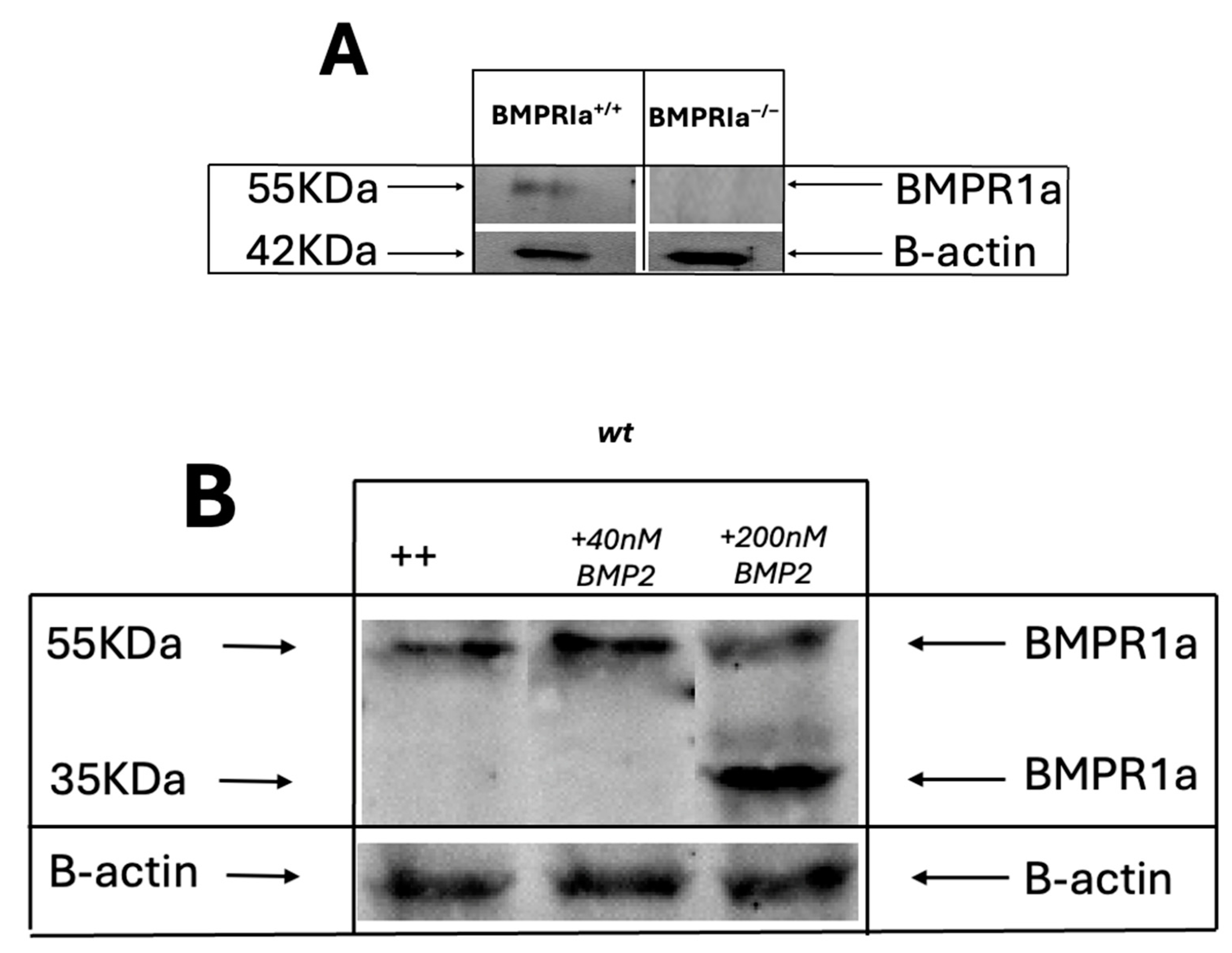
3.1. Confirmation of Antibody Specificity and BMP2-Induced BMPRIa Cleavage in C2C12 Cells
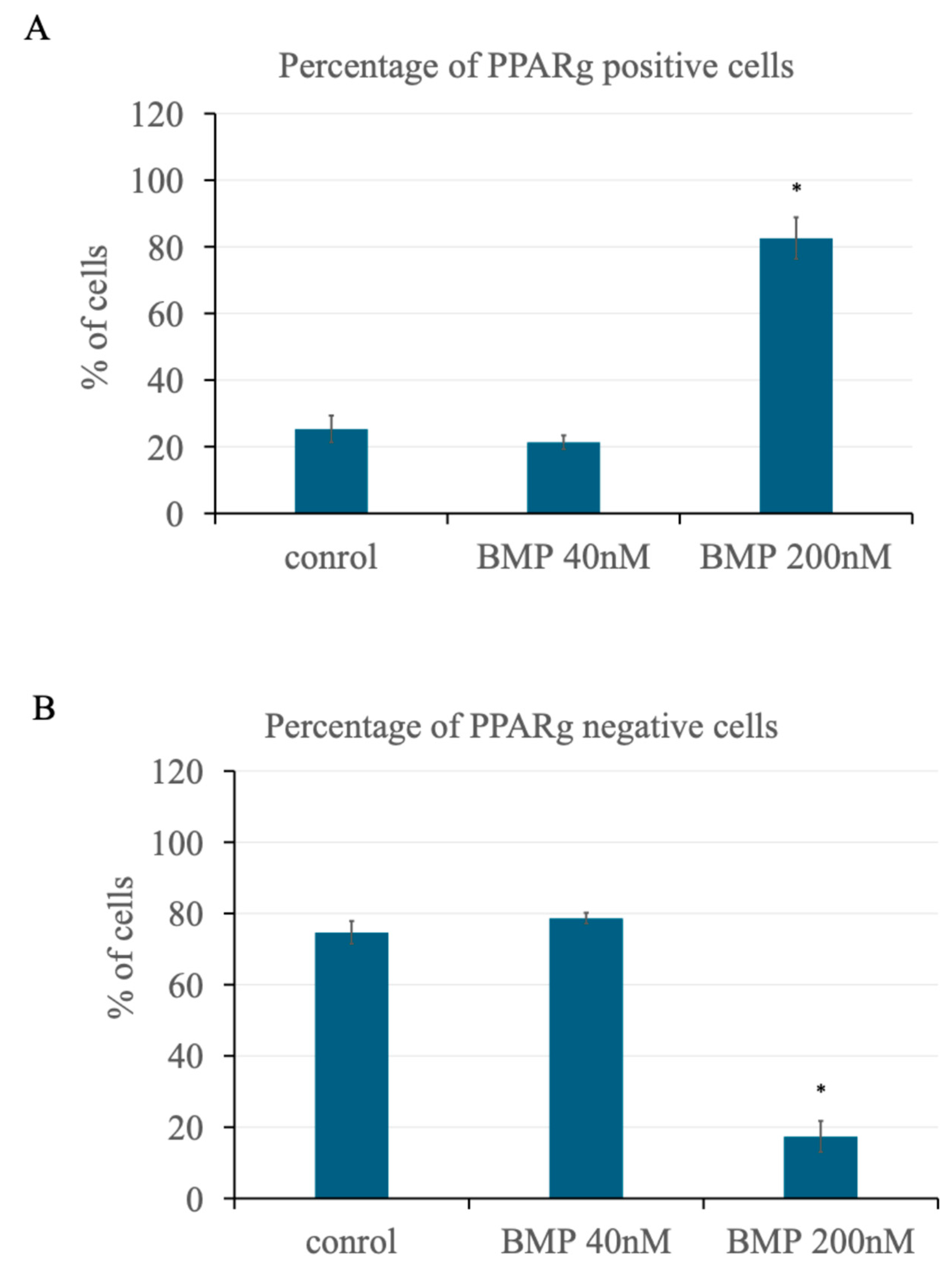
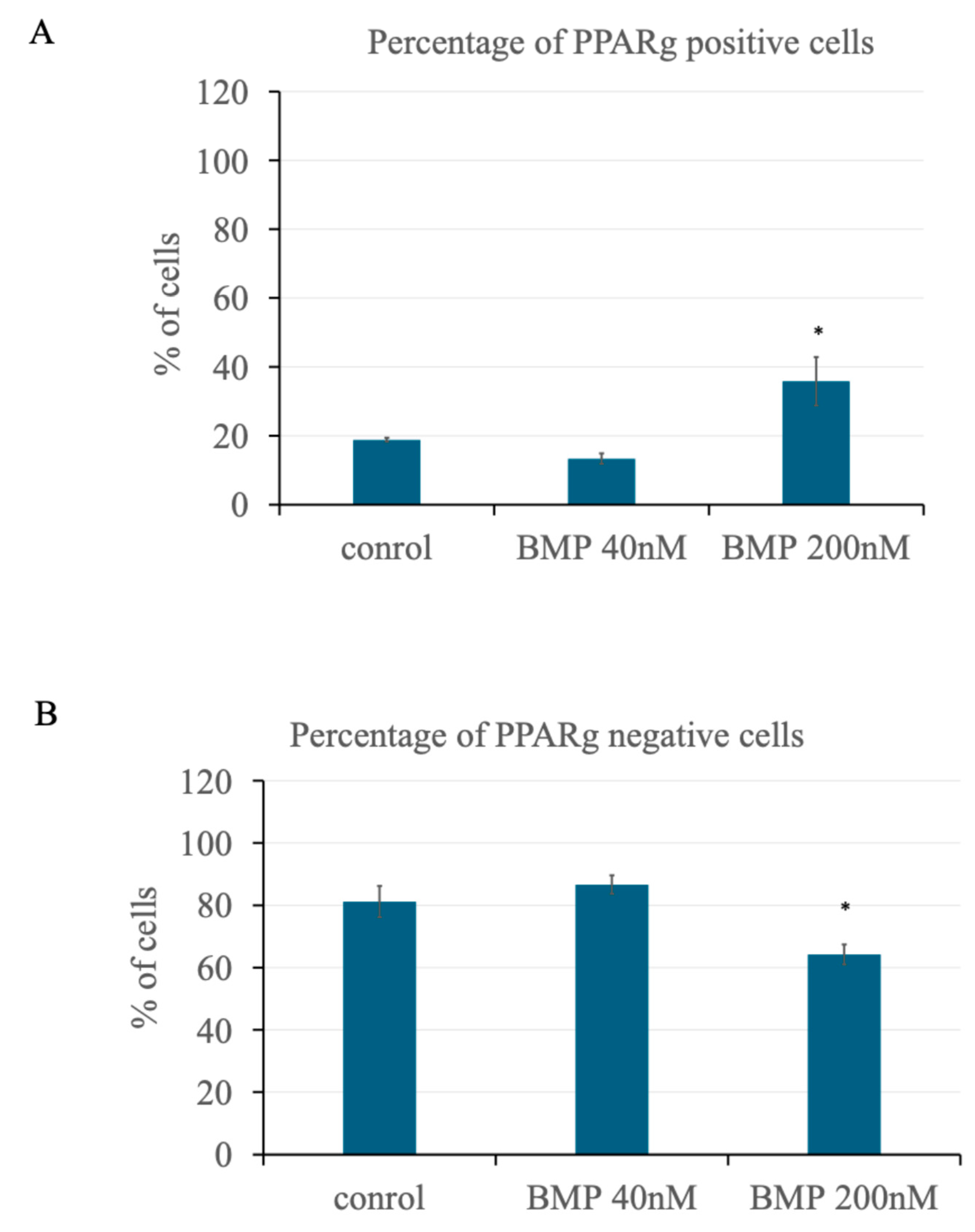
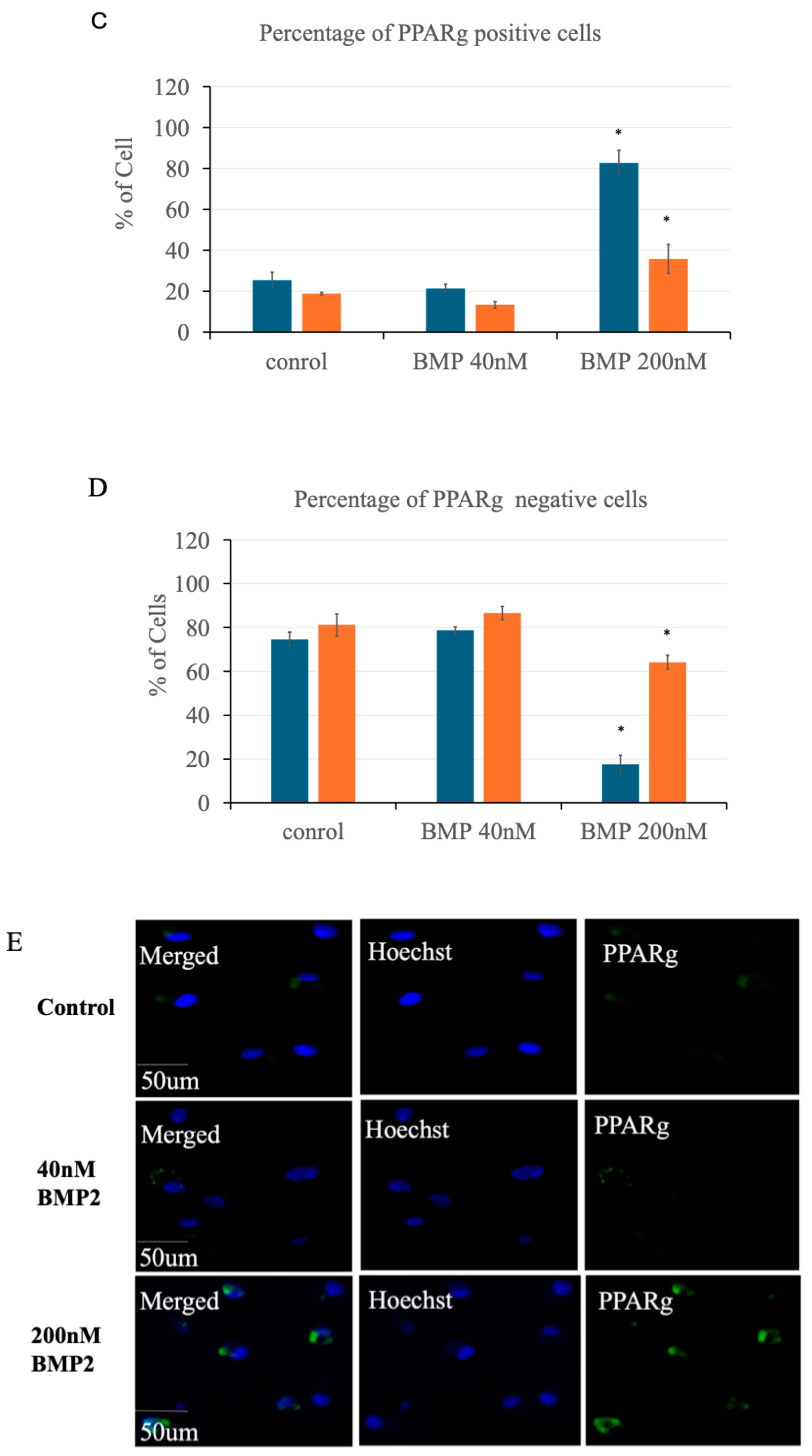
3.2. BMP2 Stimulation at 200 nM Leads to an Increase in PPARγ Expression in Primary BMSCs
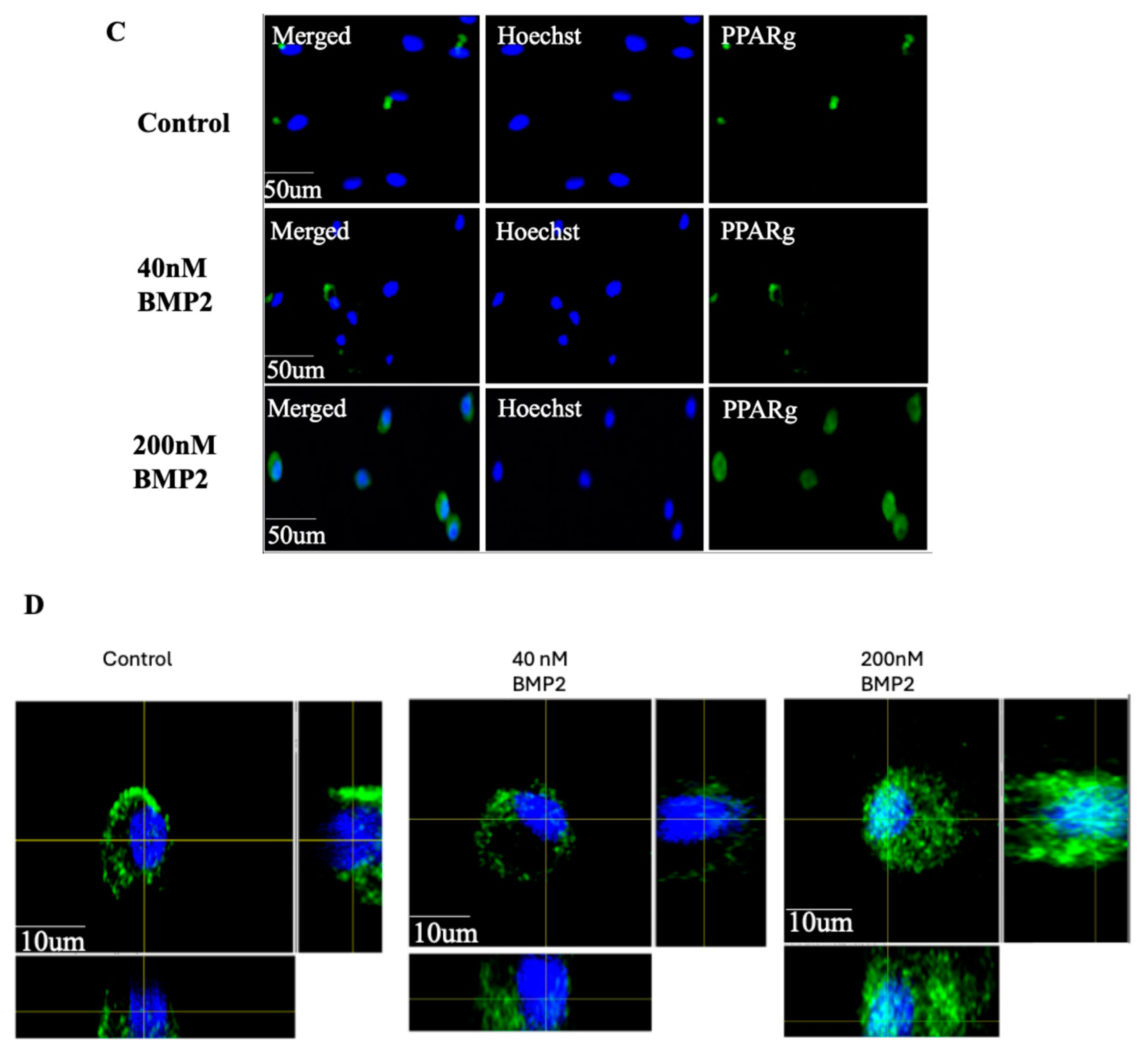
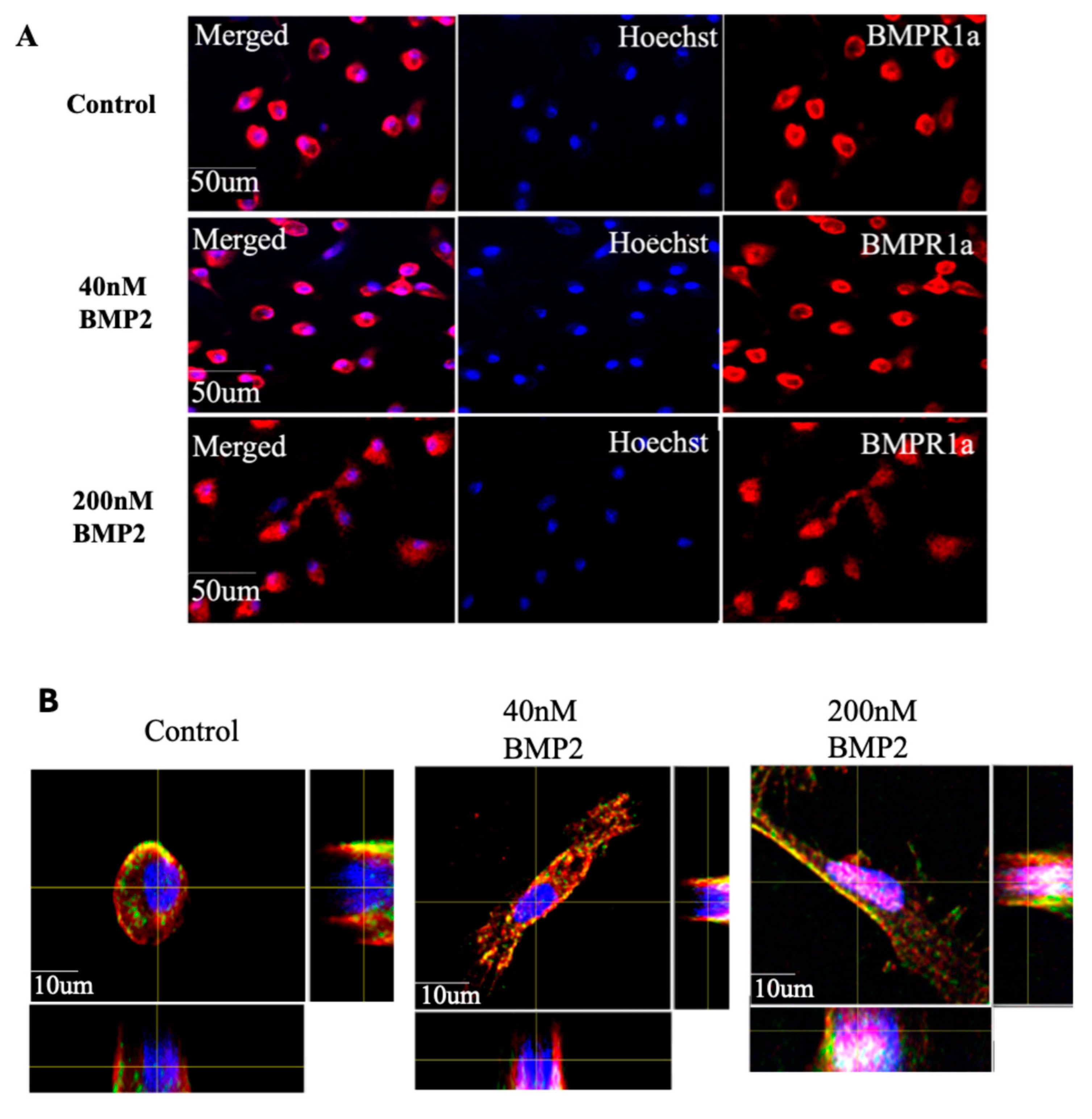
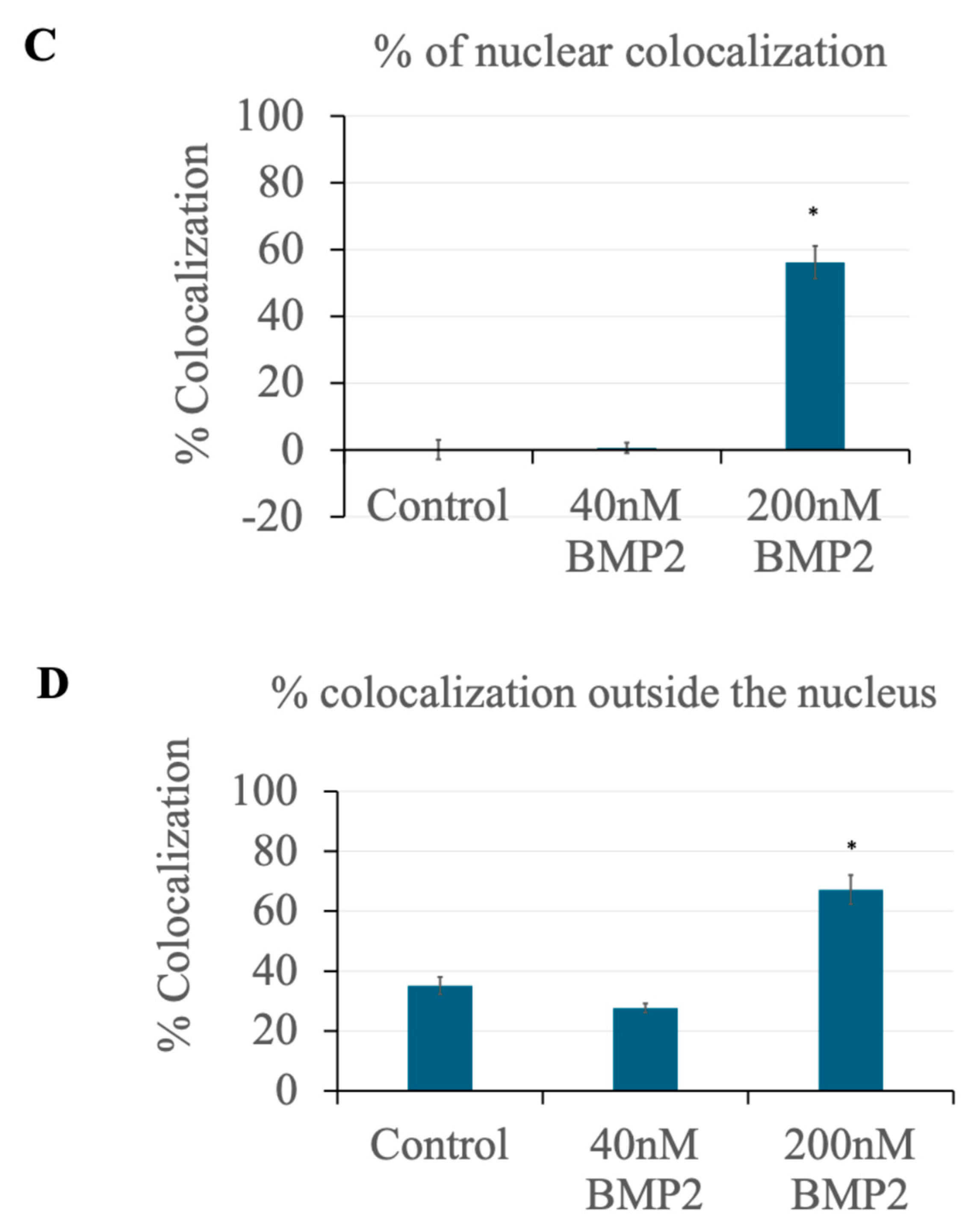
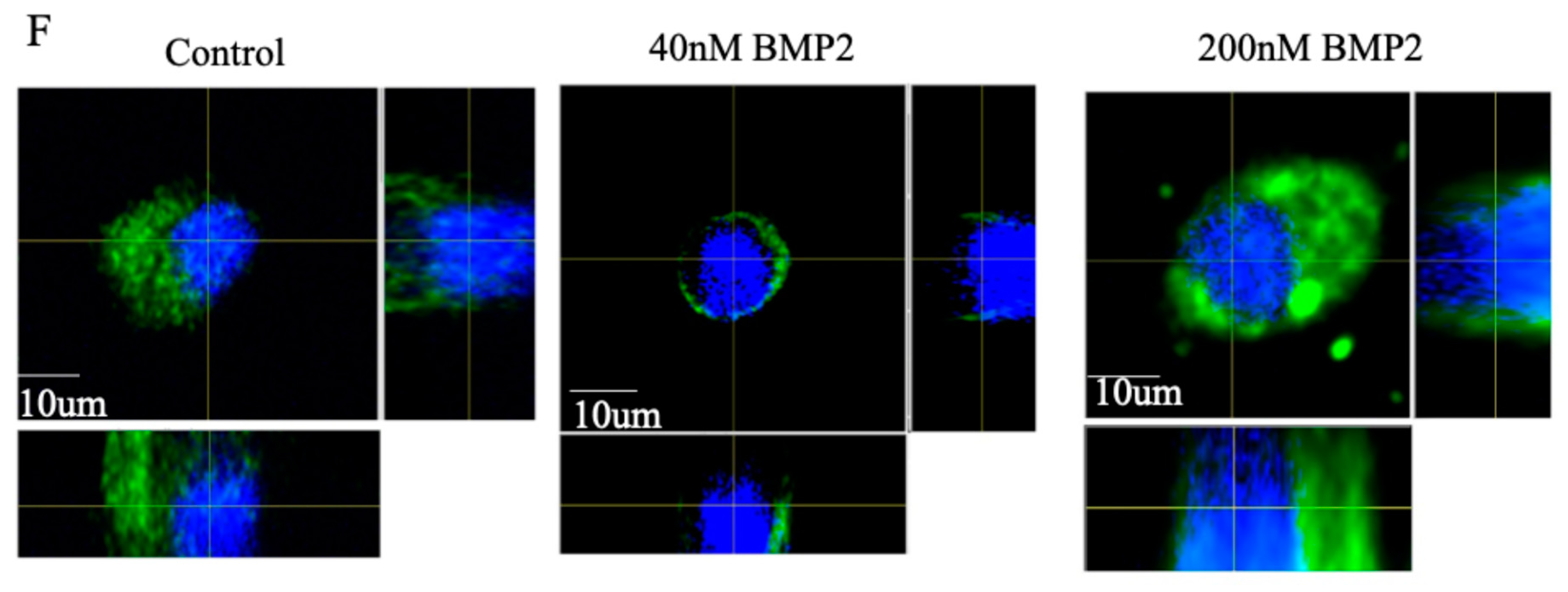
3.3. BMP2 Stimulation at 200 nM Concentration Leads to the Nuclear Accumulation of BMPRIa in BMSCs
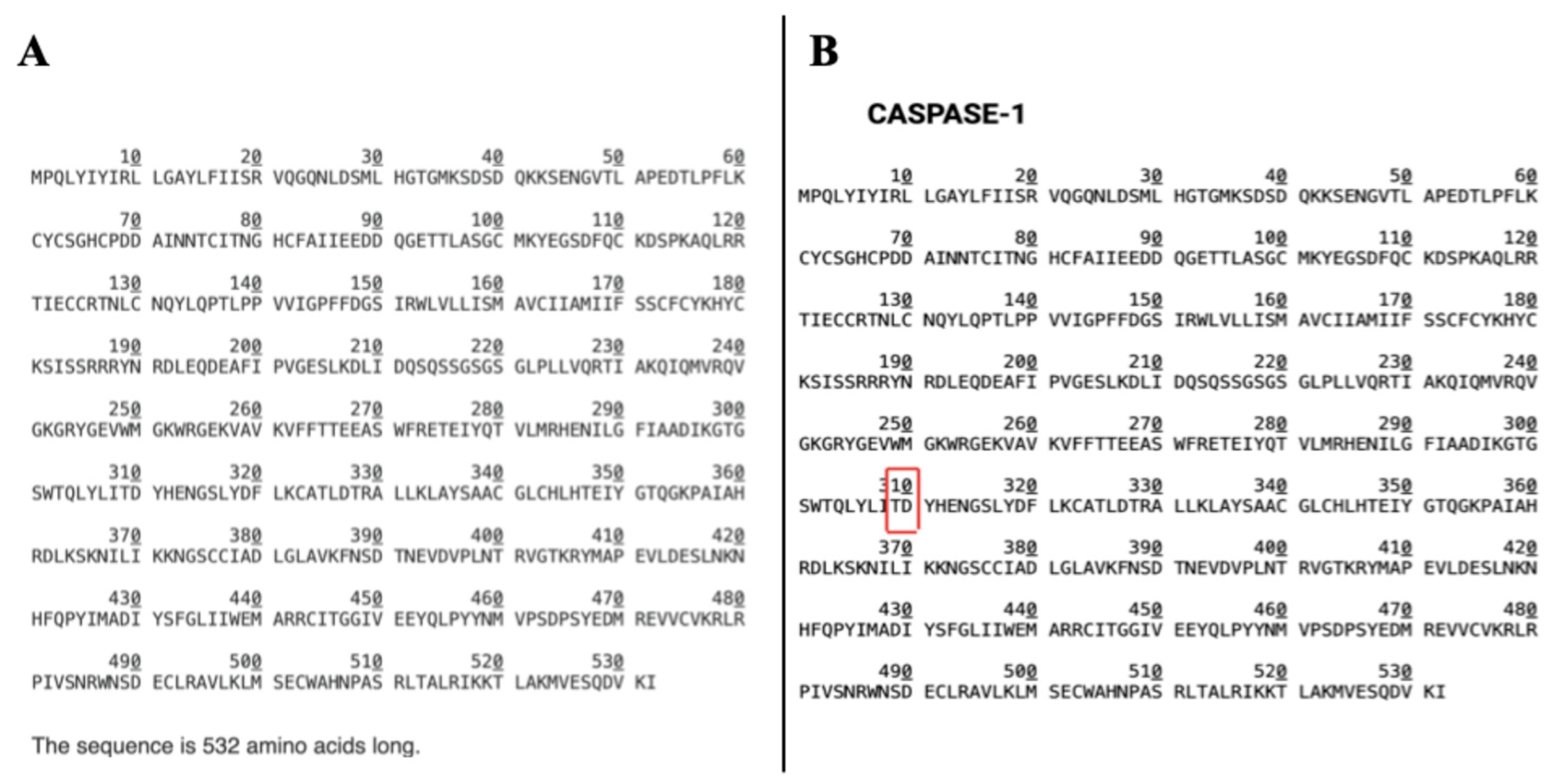
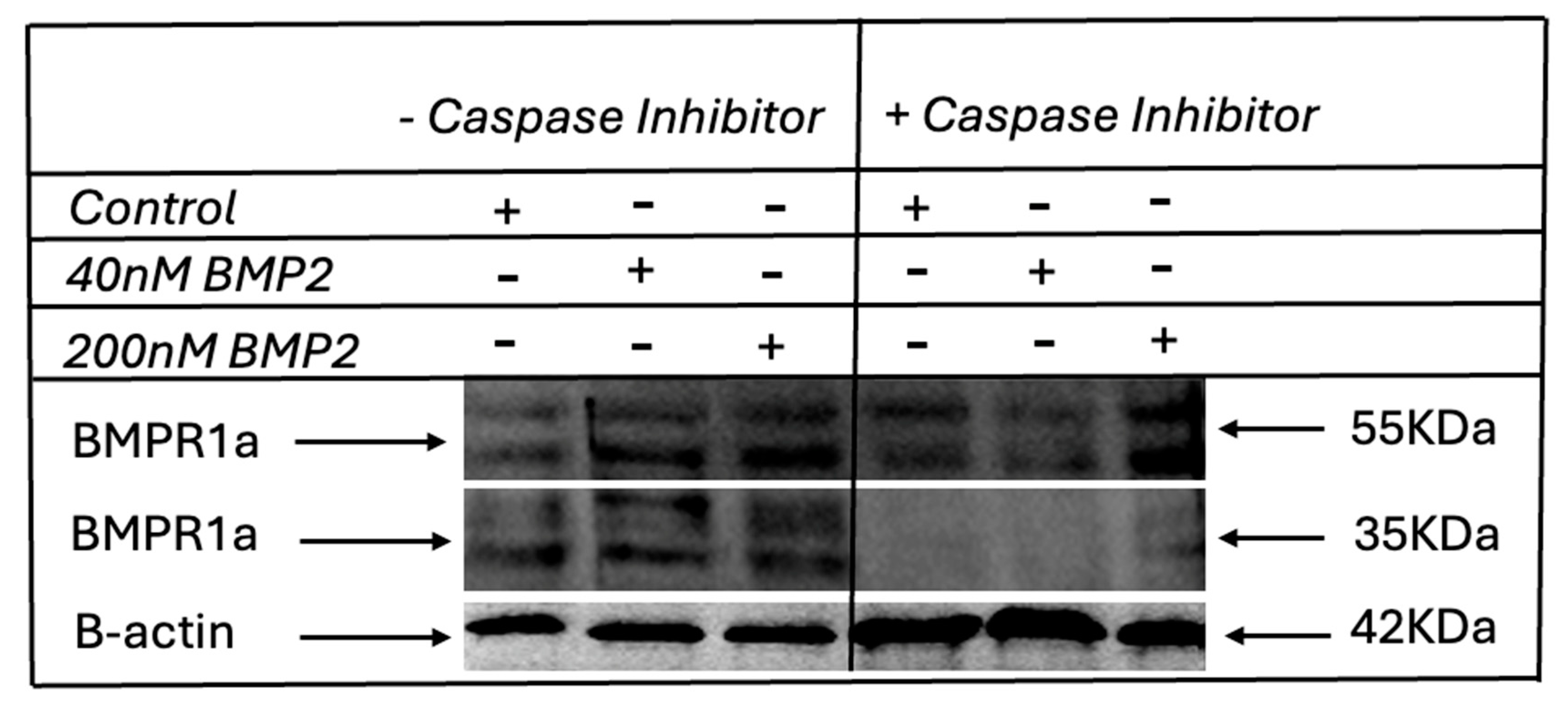
3.4. Identification of Caspase-1 as a BMPRIa Protease
3.5. BMP2 induces BMPRIa Cleavage, and Inhibition of Caspase-1 Abolished the Cleavage in Primary BMSCs
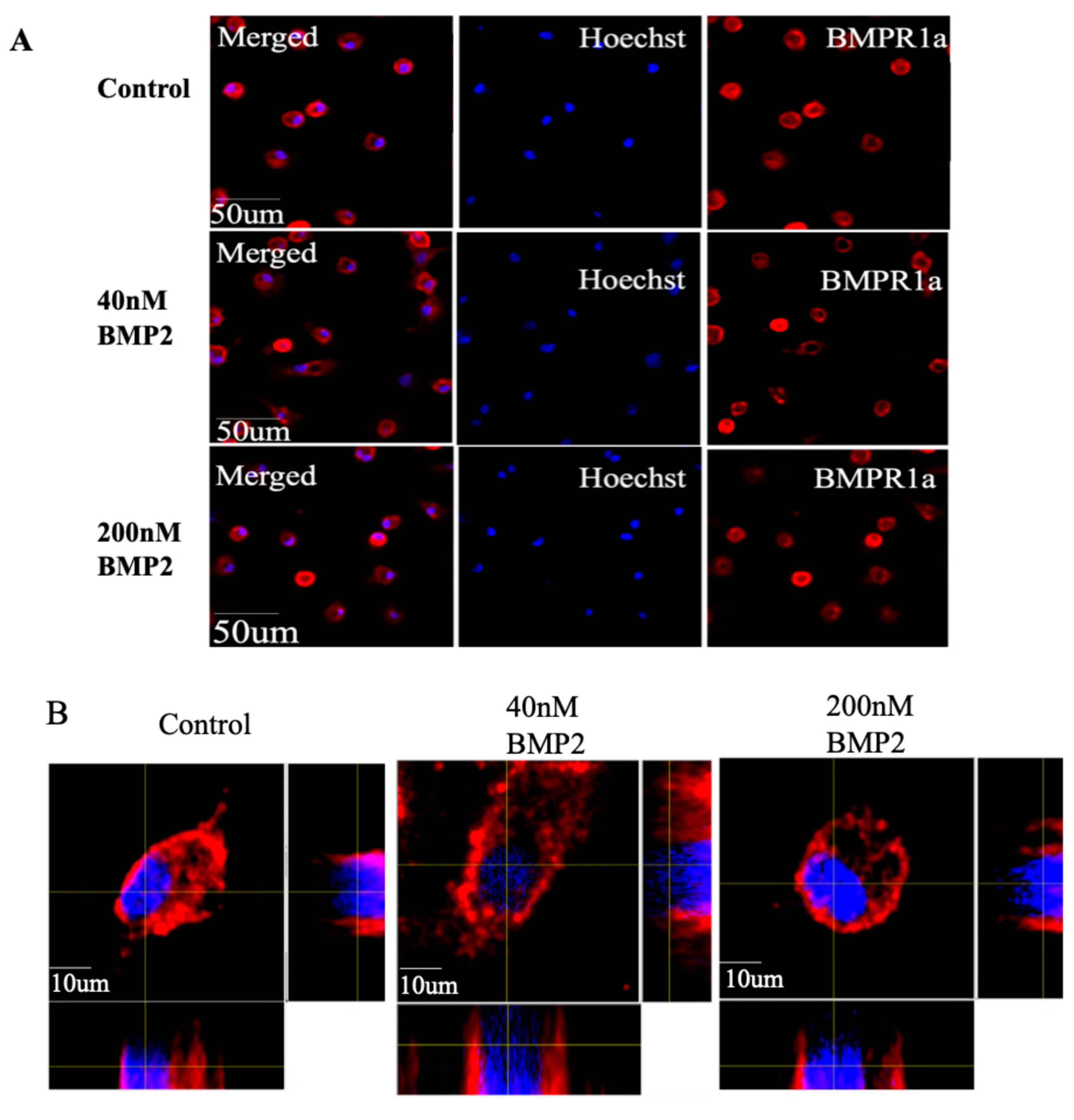
3.6. Caspase-1 Inhibition Prevents the Nuclear Accumulation of BMPRIa in 6-Months-Old Primary BMSCs
3.7. Caspase-1 Inhibition Leads to a Reduction in PPARγ Expression in BMSC
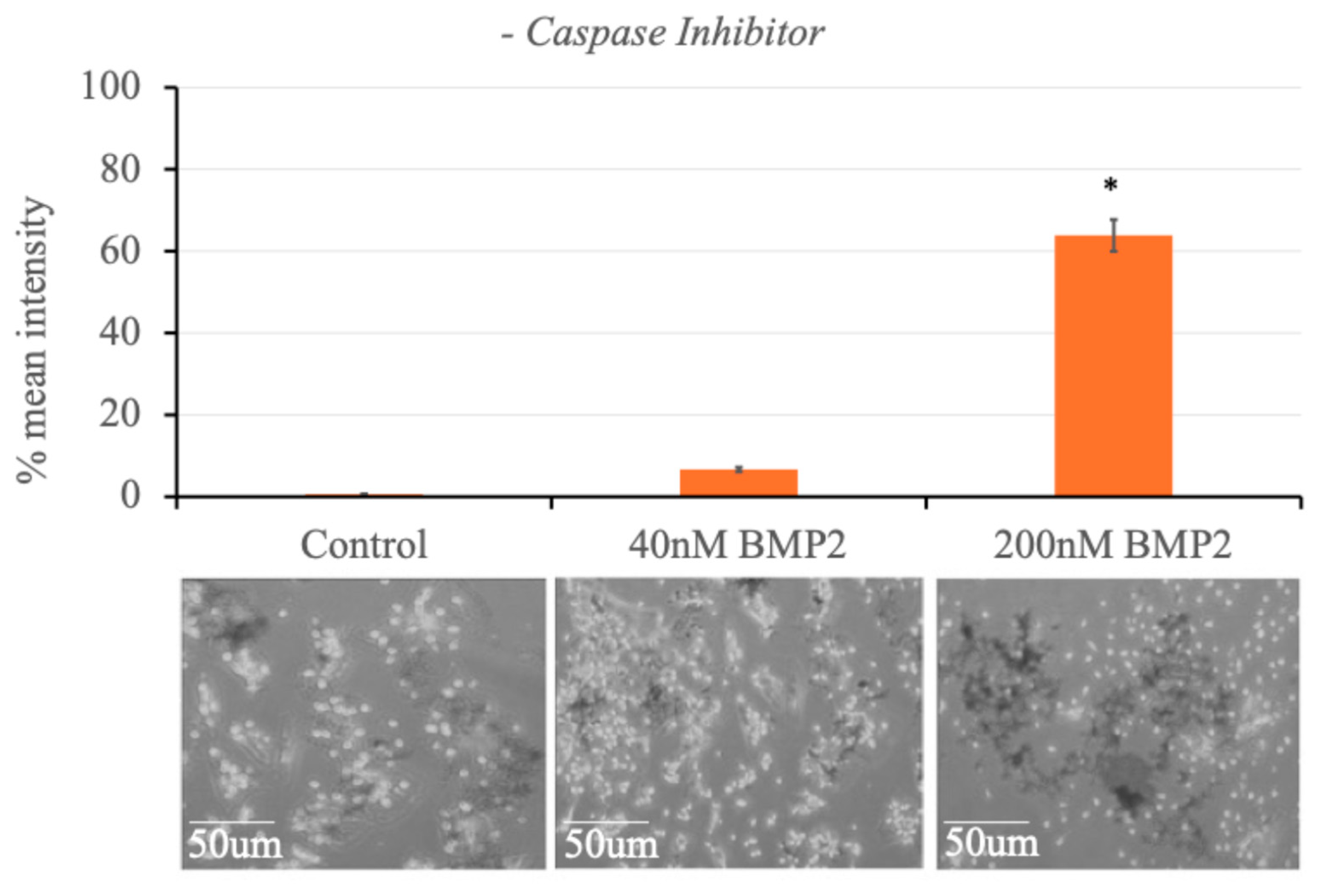
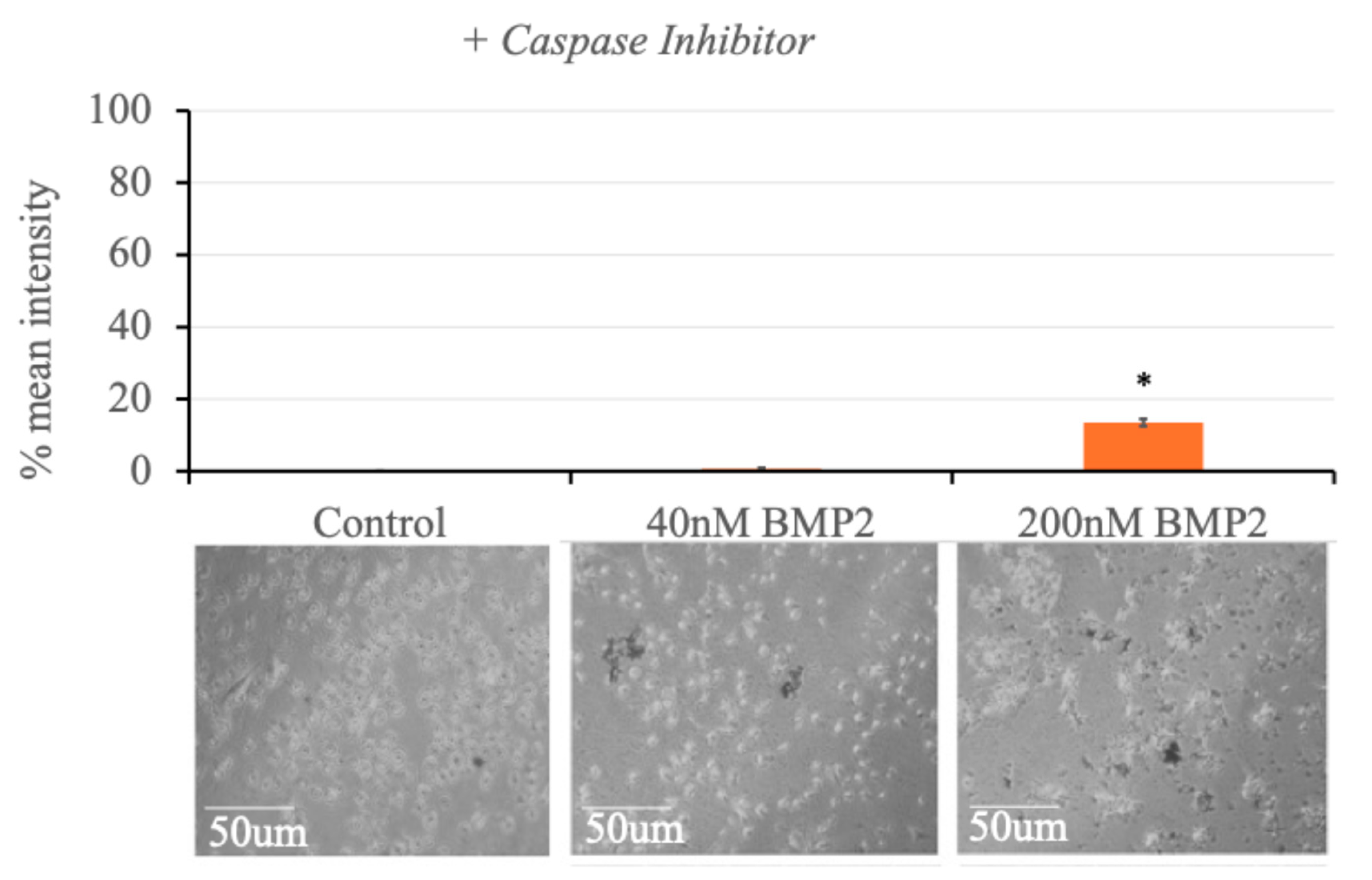
3.8. High BMP2 Concentration Induces Adipogenesis and Caspase-1 Inhibition Leads to the Reduction
4. Discussion
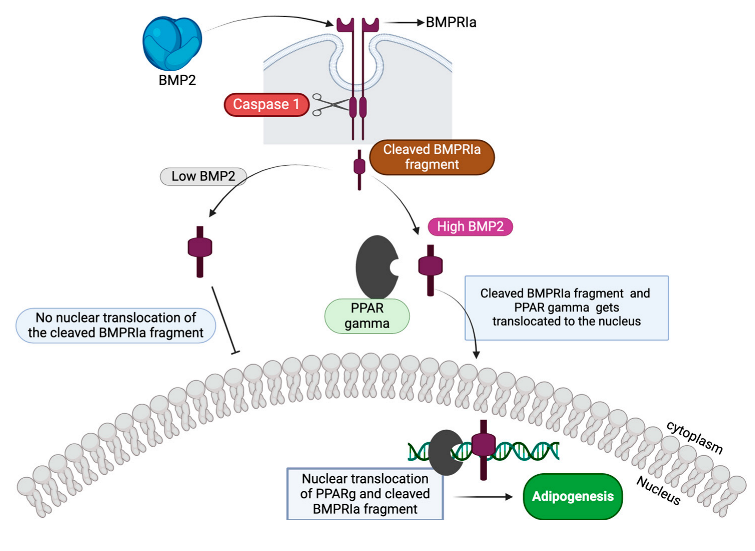
- Limitations and Future Directions.
Author Contributions
Funding
Institutional Review Board Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Ding D-C, Shyu W-C, Lin S-Z, Dah-Ching Ding W-CS, Shinn-Zong Lin. Mesenchymal Stem Cells. Cell Transplantation. 2011-02-01;20(1). [CrossRef]
- Fu X, Liu G, Halim A, Ju Y, Luo Q, Song G, et al. Mesenchymal Stem Cell Migration and Tissue Repair. Cells 2019, Vol 8, Page 784. 2019-07-28;8(8). [CrossRef]
- Naji A, Eitoku M, Favier B, Deschaseaux F, Rouas-Freiss N, Suganuma N, et al. Biological functions of mesenchymal stem cells and clinical implications. Cellular and Molecular Life Sciences 2019 76:17. 2019-05-04;76(17). [CrossRef]
- Arthur A, Gronthos S, Arthur A, Gronthos S. Clinical Application of Bone Marrow Mesenchymal Stem/Stromal Cells to Repair Skeletal Tissue. International Journal of Molecular Sciences 2020, Vol 21, Page 9759. 2020-12-21;21(24). [CrossRef]
- Shi Y, Wang Y, Li Q, Liu K, Hou J, Shao C, et al. Immunoregulatory mechanisms of mesenchymal stem and stromal cells in inflammatory diseases. Nature Reviews Nephrology 2018 14:8. 2018-06-12;14(8). [CrossRef]
- Cai Z, Wu B, Ye G, Liu W, Chen K, Wang P, et al. Enhanced Osteogenic Differentiation of Human Bone Marrow Mesenchymal Stem Cells in Ossification of the Posterior Longitudinal Ligament Through Activation of the BMP2-Smad1/5/8 Pathway. Stem Cells and Development. 2020-12-09;29(24). [CrossRef]
- Komori T, Komori T. Regulation of Proliferation, Differentiation and Functions of Osteoblasts by Runx2. International Journal of Molecular Sciences 2019, Vol 20, Page 1694. 2019-04-04;20(7). [CrossRef]
- Tanaka Y, Nakayamada S, Okada Y. Osteoblasts and Osteoclasts in Bone Remodeling and Inflammation. Current Drug Target -Inflammation & Allergy. 2005;4(3). [CrossRef]
- Okamoto M, Murai J, Yoshikawa H, Tsumaki N. Bone Morphogenetic Proteins in Bone Stimulate Osteoclasts and Osteoblasts During Bone Development*. Journal of Bone and Mineral Research. 2006/07/01;21(7). [CrossRef]
- Adipocyte differentiation of bone marrow-derived mesenchymal stem cells: cross talk with the osteoblastogenic program—PubMed. Cellular and molecular life sciences : CMLS. 2009 Jan;66(2). [CrossRef]
- Li Y, Jin D, Xie W, Wen L, Chen W, Xu J, et al. PPAR-γ and Wnt Regulate the Differentiation of MSCs into Adipocytes and Osteoblasts Respectively. Current Stem Cell Research & Therapy. 2018;13(3). [CrossRef]
- Zhuang H, Zhang X, Zhu C, Tang X, Yu F, Shang Gw, et al. Molecular Mechanisms of PPAR-g Governing MSC Osteogenic and Adipogenic Differentiation. Current Stem Cell Research & Therapy. 2016;11(3). [CrossRef]
- Pokrovskaya LA, Nadezhdin SV, Zubareva EV, Burda YE, Gnezdyukova ES, Pokrovskaya LA, et al. Expression of RUNX2 and Osterix in Rat Mesenchymal Stem Cells during Culturing in Osteogenic-Conditioned Medium. Bulletin of Experimental Biology and Medicine 2020 169:4. 2020-09-10;169(4). [CrossRef]
- Suppression of PPAR transactivation switches cell fate of bone marrow stem cells from adipocytes into osteoblasts—PubMed. Annals of the New York Academy of Sciences. 2007 Nov;1116(1). [CrossRef]
- Cristancho AG, Lazar MA. Forming functional fat: a growing understanding of adipocyte differentiation. Nature reviews Molecular cell biology. 2011/09/09;12(11). [CrossRef]
- Cornish J, Wang T, Lin J-m, Cornish J, Wang T, Lin J-m. Role of Marrow Adipocytes in Regulation of Energy Metabolism and Bone Homeostasis. Current Osteoporosis Reports 2018 16:2. 2018-03-16;16(2). [CrossRef]
- The relationship between bone marrow adipose tissue and bone metabolism in postmenopausal osteoporosis—PubMed. Cytokine & growth factor reviews. 2020 Apr;52. [CrossRef]
- Donoso O, Pino AM, Seitz G, Osses N, Rodríguez JP. Osteoporosis-associated alteration in the signalling status of BMP-2 in human MSCs under adipogenic conditions. Journal of Cellular Biochemistry. 2015/07/01;116(7). [CrossRef]
- Jiao Li XC, Lingyun Lu , Xijie Yu. The relationship between bone marrow adipose tissue and bone metabolism in postmenopausal osteoporosis. Cytokine & Growth Factor Reviews. 2020/04/01;52. [CrossRef]
- Durbano HW, Halloran D, Nguyen J, Stone V, Mctague S, Eskander M, et al. Aberrant BMP2 Signaling in Patients Diagnosed with Osteoporosis. International Journal of Molecular Sciences. 2020;21(18):6909. [CrossRef]
- Wright NC, Looker AC, Saag KG, Curtis JR, Delzell ES, Randall S, et al. The Recent Prevalence of Osteoporosis and Low Bone Mass in the United States Based on Bone Mineral Density at the Femoral Neck or Lumbar Spine. Journal of bone and mineral research : the official journal of the American Society for Bone and Mineral Research. 2014/11;29(11). [CrossRef]
- Ji M-X, Yu Q. Primary osteoporosis in postmenopausal women. Chronic Diseases and Translational Medicine. 2015/03;1(1). [CrossRef]
- Westhovens R, Dequeker J, Westhovens R, Dequeker J. Rheumatoid arthritis and osteoporosis. Zeitschrift für Rheumatologie 2000 59:1. 2014-04-10;59(1). [CrossRef]
- Li J, Hu Y, You H, Li R, Ran Q, Ouyang T, et al. Trabecular Bone Microarchitecture Evaluation in an Osteoporosis Mouse Model. Journal of Visualized Experiments. 2023(199). [CrossRef]
- Moerman EJ, Teng K, Lipschitz DA, Lecka-Czernik B. Aging activates adipogenic and suppresses osteogenic programs in mesenchymal marrow stroma/stem cells: the role of PPAR-γ2 transcription factor and TGF-β/BMP signaling pathways. Aging cell. 2004/12;3(6). [CrossRef]
- Camacho PM, Petak SM, Binkley N, Diab DL, Eldeiry LS, Farooki A, et al. American Association of Clinical Endocrinologists/American College of Endocrinology Clinical Practice Guidelines for the Diagnosis and Treatment of Postmenopausal Osteoporosis—2020 Update. Endocrine Practice. 2020/05/01;26. [CrossRef]
- Halloran D, Pandit V, Macmurray C, Stone V, Degeorge K, Eskander M, et al. Age-Related Low Bone Mineral Density in C57BL/6 Mice Is Reflective of Aberrant Bone Morphogenetic Protein-2 Signaling Observed in Human Patients Diagnosed with Osteoporosis. International Journal of Molecular Sciences. 2022;23(19):11205. [CrossRef]
- Reeve J, Meunier PJ, Parsons JA, Bernat M, Bijvoet OL, Courpron P, et al. Anabolic effect of human parathyroid hormone fragment on trabecular bone in involutional osteoporosis: a multicentre trial. British Medical Journal. 1980/06/06;280(6228). [CrossRef]
- A review of anabolic therapies for osteoporosis—PubMed. Arthritis research & therapy. 2003;5(5). [CrossRef]
- MUÑOZ M, ROBINSON K, SHIBLI-RAHHAL A. Bone Health and Osteoporosis Prevention and Treatment. Clinical Obstetrics and Gynecology. December 2020;63(4). [CrossRef]
- Blahoš J, Blahoš J. Treatment and prevention of osteoporosis. Wiener Medizinische Wochenschrift 2007 157:23. 2007-12-01;157(23). [CrossRef]
- Delaney MF. Strategies for the prevention and treatment of osteoporosis during early postmenopause. American Journal of Obstetrics & Gynecology. 2006/02/01;194(2). [CrossRef]
- Kemmak AR, Rezapour A, Jahangiri R, Nikjoo S, Farabi H, Soleimanpour S. Economic burden of osteoporosis in the world: A systematic review. Medical Journal of the Islamic Republic of Iran. 2020;34. [CrossRef]
- Wang RN, Green J, Wang Z, Deng Y, Qiao M, Peabody M, et al. Bone Morphogenetic Protein (BMP) signaling in development and human diseases. Genes & Diseases. 2014/09;1(1). [CrossRef]
- Amitabha Bandyopadhyay PSY, Paritosh Prashar. BMP signaling in development and diseases: A pharmacological perspective. Biochemical Pharmacology. 2013/04/01;85(7). [CrossRef]
- Weiss A, Attisano L. The TGFbeta Superfamily Signaling Pathway. Wiley Interdisciplinary Reviews: Developmental Biology. 2013/01/01;2(1). [CrossRef]
- Chen G, Deng C, Li Y-P. TGF-β and BMP Signaling in Osteoblast Differentiation and Bone Formation. International Journal of Biological Sciences. 2012;8(2). [CrossRef]
- Poniatowski ŁA, Wojdasiewicz P, Gasik R, Szukiewicz D. Transforming Growth Factor Beta Family: Insight into the Role of Growth Factors in Regulation of Fracture Healing Biology and Potential Clinical Applications. Mediators of Inflammation. 2015;2015. [CrossRef]
- Carlisle E, Fischgrund JS. Bone morphogenetic proteins for spinal fusion. The Spine Journal. 2005/11/01;5(6). [CrossRef]
- Urist MR. Bone: Formation by Autoinduction. Science. 1965-11-12;150(3698). [CrossRef]
- Halloran D, Durbano HW, Nohe A. Bone Morphogenetic Protein-2 in Development and Bone Homeostasis. Journal of Developmental Biology. 2020/09;8(3). [CrossRef]
- Haid RW, Branch CL, Alexander JT, Burkus JK. Posterior lumbar interbody fusion using recombinant human bone morphogenetic protein type 2 with cylindrical interbody cages. The Spine Journal. 2004/09/01;4(5). [CrossRef]
- J Kenneth Burkus MFG, Curtis A Dickman , Thomas A Zdeblick. Anterior lumbar interbody fusion using rhBMP-2 with tapered interbody cages—PubMed. Journal of spinal disorders & techniques. 2002 Oct;15(5). [CrossRef]
- Biswas S, Li P, Wu H, Shafiquzzaman M, Murakami S, Schneider MD, et al. BMPRIA is required for osteogenic differentiation and RANKL expression in adult bone marrow mesenchymal stromal cells. Scientific Reports. 2018;8(1). [CrossRef]
- Gu S, Wu W, Liu C, Yang L, Sun C, Ye W, et al. BMPRIA Mediated Signaling Is Essential for Temporomandibular Joint Development in Mice. PLoS ONE. 2014;9(8):e101000. [CrossRef]
- Rogers MB, Shah TA, Shaikh NN. Turning Bone Morphogenetic Protein 2 (BMP2) On and Off in Mesenchymal Cells. Journal of cellular biochemistry. 2015/10;116(10). [CrossRef]
- Agnew C, Ayaz P, Kashima R, Loving HS, Ghatpande P, Kung JE, et al. Structural basis for ALK2/BMPR2 receptor complex signaling through kinase domain oligomerization. Nature Communications. 2021;12(1). [CrossRef]
- Marcelo Ehrlich DH, Barak Marom , Petra Knaus , Yoav I Henis. Homomeric and heteromeric complexes among TGF-β and BMP receptors and their roles in signaling. Cellular Signalling. 2011/09/01;23(9). [CrossRef]
- Gilboa L, Nohe A, Geissendörfer T, Sebald W, Henis YI, Knaus P. Bone Morphogenetic Protein Receptor Complexes on the Surface of Live Cells: A New Oligomerization Mode for Serine/Threonine Kinase Receptors. Molecular Biology of the Cell. 2000/03;11(3). [CrossRef]
- Hartung A, Bitton-Worms K, Rechtman MM, Wenzel V, Boergermann JH, Hassel S, et al. Different Routes of Bone Morphogenic Protein (BMP) Receptor Endocytosis Influence BMP Signaling. Molecular and Cellular Biology. 2006/10;26(20). [CrossRef]
- Chu K-Y, Malik A, Thamilselvan V, Martinez-Hackert E. Type II BMP and activin receptors BMPR2 and ACVR2A share a conserved mode of growth factor recognition. The Journal of Biological Chemistry. 2022/07;298(7). [CrossRef]
- Derynck R, Zhang YE, Derynck R, Zhang YE. Smad-dependent and Smad-independent pathways in TGF-β family signalling. Nature 2003 425:6958. 2003/10;425(6958). [CrossRef]
- Pervan CL. Smad-independent TGF-β2 signaling pathways in human trabecular meshwork cells. Experimental Eye Research. 2017/05/01;158. [CrossRef]
- Graham TR, Odero-Marah VA, Chung LW, Agrawal KC, Davis R, Abdel-Mageed AB. PI3K/Akt-Dependent Transcriptional Regulation and Activation of BMP-2-Smad Signaling by NF-κB in Metastatic Prostate Cancer Cells. The Prostate. 2009/02/02;69(2). [CrossRef]
- Mu Y, Gudey SK, Landström M, Mu Y, Gudey SK, Landström M. Non-Smad signaling pathways. Cell and Tissue Research 2011 347:1. 2011-06-24;347(1). [CrossRef]
- U P, H I, S S, S I, S G, U E, et al. The L45 loop in type I receptors for TGF-beta family members is a critical determinant in specifying Smad isoform activation. FEBS Letters. 1998;434(1-2). [CrossRef]
- Jeffrey W. Wertz PMB. Caveolin-1 regulates BMPRII localization and signaling in vascular smooth muscle cells. Biochemical and Biophysical Research Communications. 2008/10/31;375(4). [CrossRef]
- Bragdon B, Bonor J, Schultz KL, Beamer WG, Rosen CJ, Nohe A. Bone Morphogenetic Protein Receptor Type Ia Localization Causes Increased BMP2 Signaling in Mice Exhibiting Increased Peak Bone Mass Phenotype. Journal of Cellular Physiology. 2012/07;227(7). [CrossRef]
- Bonor J, Adams EL, Bragdon B, Moseychuk O, Czymmek KJ, Nohe A. Initiation of BMP2 Signaling in Domains on the Plasma Membrane. Journal of Cellular Physiology. 2012/07;227(7). [CrossRef]
- Saldanha S, Bragdon B, Moseychuk O, Bonor J, Dhurjati P, Nohe A. Caveolae regulate smad signaling as verified by novel imaging and system biology approaches. Journal of Cellular Physiology. 2013/05/01;228(5). [CrossRef]
- Wang S, Hu S, Wang J, Liu Y, Zhao R, Tong M, et al. Conditioned medium from bone marrow-derived mesenchymal stem cells inhibits vascular calcification through blockade of the BMP2–Smad1/5/8 signaling pathway. Stem Cell Research & Therapy. 2018;9(1). [CrossRef]
- Beth Bragdon ST, Oleksandra Moseychuk , Lauren Gurski , Jeremy Bonor , Christopher Price , Liyun Wang , Wesley G Beamer , Anja Nohe. Casein kinase 2 regulates in vivo bone formation through its interaction with bone morphogenetic protein receptor type Ia. Bone. 2011/11/01;49(5). [CrossRef]
- Bragdon B, Thinakaran S, Moseychuk O, King D, Young K, Litchfield W, David, et al. Casein Kinase 2 β-Subunit Is a Regulator of Bone Morphogenetic Protein 2 Signaling. Biophysical Journal. 2010;99(3):897-904. [CrossRef]
- Beth Bragdon OM, Sven Saldanha , Daniel King , Joanne Julian , Anja Nohe. Bone Morphogenetic Proteins: A critical review. Cellular Signalling. 2011/04/01;23(4). [CrossRef]
- Villavicencio AT, Burneikiene S. RhBMP-2-induced radiculitis in patients undergoing transforaminal lumbar interbody fusion: relationship to dose. The Spine Journal. 2016/10/01;16(10). [CrossRef]
- Alkhathami AG, Abdullah MR, Ahmed M, Hassan Ahmed H, Alwash SW, Muhammed Mahdi Z, et al. Bone morphogenetic protein (BMP)9 in cancer development: mechanistic, diagnostic, and therapeutic approaches? Journal of Drug Targeting. 2023;31(7):714-24. [CrossRef]
- Lewandrowski K-U, Nanson C, Calderon R. Vertebral osteolysis after posterior interbody lumbar fusion with recombinant human bone morphogenetic protein 2: A report of five cases. The Spine Journal. 2007/09/01;7(5). [CrossRef]
- James AW, LaChaud G, Shen J, Asatrian G, Nguyen V, Zhang X, et al. A Review of the Clinical Side Effects of Bone Morphogenetic Protein-2. Tissue Engineering Part B, Reviews. 2016/08/08;22(4). [CrossRef]
- Moseychuk O, Akkiraju H, Dutta J, D’Angelo A, Bragdon B, Duncan RL, et al. Inhibition of CK2 binding to BMPRIa induces C2C12 differentiation into osteoblasts and adipocytes. Journal of Cell Communication and Signaling. 2013/12;7(4). [CrossRef]
- Stienstra R, Joosten LAB, Koenen T, Tits Bv, Diepen JAv, Berg SAAvd, et al. The Inflammasome-Mediated Caspase-1 Activation Controls Adipocyte Differentiation and Insulin Sensitivity. Cell metabolism. 2010/12/12;12(6). [CrossRef]
- Molla MD, Ayelign B, Dessie G, Geto Z, Admasu TD, Molla MD, et al. Caspase-1 as a regulatory molecule of lipid metabolism. Lipids in Health and Disease 2020 19:1. 2020-03-06;19(1). [CrossRef]
- Wang Y, Chen G, Xu M, Cui Y, He W, Zeng H, et al. Caspase-1 Deficiency Modulates Adipogenesis through Atg7-Mediated Autophagy: An Inflammatory-Independent Mechanism. Biomolecules 2024, Vol 14, Page 501. 2024-04-20;14(4). [CrossRef]
- Gasteiger E, Hoogland C, Gattiker A, Duvaud Se, Wilkins MR, Appel RD, et al. Protein Identification and Analysis Tools on the ExPASy Server. The Proteomics Protocols Handbook. 2005. [CrossRef]
- Srivastava M, Deal C. Osteoporosis in elderly: prevention and treatment. Clinics in Geriatric Medicine. 2002/08/01;18(3). [CrossRef]
- AL B, R. C. Aging and bone. Journal of Dental Research. 2010;89(12). [CrossRef]
- Shoji H, Miyakawa T. Age-related behavioral changes from young to old age in male mice of a C57BL/6J strain maintained under a genetic stability program. Neuropsychopharmacology Reports. 2019/06;39(2). [CrossRef]
- Ambrosi TH, Scialdone A, Graja A, Gohlke S, Jank A-M, Bocian C, et al. Adipocyte Accumulation in the Bone Marrow during Obesity and Aging Impairs Stem Cell-Based Hematopoietic and Bone Regeneration. Cell Stem Cell. 2017/06/06;20(6). [CrossRef]
- Chen Q, Shou P, Zheng C, Jiang M, Cao G, Yang Q, et al. Fate decision of mesenchymal stem cells: adipocytes or osteoblasts? Cell Death & Differentiation 2016 23:7. 2016-02-12;23(7). [CrossRef]

Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).



