Submitted:
28 March 2025
Posted:
31 March 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| CI | Confidence interval |
| COVID-19 | Coronavirus disease 2019 |
| GAS | Group A Streptococcus |
| NPIa | Non-pharmaceutical interventions |
| PCR | Polymerase chain reaction |
| RSV | Respiratory syncytial virus |
| SARS-CoV-2 | Severe acute respiratory syndrome coronavirus 2 |
| SD | Standard deviation |
References
- Ashurst, J.V.; Edgerley-Gibb, L. Streptococcal pharyngitis.
- Kakimoto, S. Impact of the early phase of COVID-19 on the trends of isolated bacteria in the national database of Japan: an interrupted time-series analysis. J Infect 2023, 86, 147–153. [Google Scholar] [PubMed]
- McBride, J.A.; Eickhoff, J.; Wald, E.R. Impact of COVID-19 quarantine and school cancelation on other common infectious diseases. Pediatr Infect Dis J 2020, 39, e449–e452. [Google Scholar]
- Li, A, Zhang, L. Reduced incidence of acute pharyngitis and increased incidence of chornic pharyngitis under COVID-19 control strategy in Beijing. J Infect 2022, 85, 174–211.
- Boyanton, B.L. Jr.; Snowden, J.N.; Frenner, R.A.; Rosenbaum, E.R.; Young, H.L.; Kennedy, J.L. SARS-CoV-2 infection mitigation strategies concomitantly reduce group a streptococcus pharyngitis. Clin Pediatr (Phila) 2022, 99228221141534. [Google Scholar]
- Tokyo Metropolitan Infectious Disease Surveilance Center. Available online: https://idsc.tmiph.metro.tokyo.lg.jp/diseases/group-a/group-a/ (accessed on 22 May 2023).
- Massese M, Sorda ML, Maio FD, Gatto A, Rosato R, Pansini V, Caroselli A, Fiori B, Sanguinetti M, Chiaretti A, Posteraro B. Epidemiology of group A streptococcal infection: are we ready for a new scenario? Lancet Microbe 2024, 5, 620–621.
- Lassoued, Y. Unexpected Increase in Invasive Group A Streptococcal Infections in Children After Respiratory Viruses Outbreak in France: A 15-Year Time-Series Analysis. Open Forum Infect Dis 2023, 10, ofad188. [Google Scholar]
- Chan, K.H.; Veeraballi, S.; Ahmed, E. Ramy Yakobi, Jihad Slim. A case of co-occurrence of COVID-19 and group A streptococcal pharyngitis. Cureus 2021, 13, e14729. [Google Scholar]
- Khaddour, K.; Sikora, A.; Tahir, N.; Nepomuceno, D.; Huang, T. Case report: the importance of novel coronavirus disease (COVID-19) and coinfection with other respiratory pathogens in the current pandemic. Am J Trop Med Hyg 2020, 102, 1208–1209. [Google Scholar]
- Capilia™ Strep, A. Available online: https://www.tauns.co.jp/en/wp-content/uploads/2021/08/capilia_strep_a_Brochure_2007A.pdf (accessed on 22 May 2023).
- Ministry of Health, Labor and welfare. Clinical management of patients with COVID-19. Available online: https://www.niph.go.jp/h-crisis/wp-content/uploads/2020/07/20200706103735_content_000646531.pdf (accessed on 17 November 2023).
- Nakamoto, D.; Nojiri, S.; Taguchi, C.; Kawakami, Y.; Miyazawa, S.; Kuroki, M.; Nishizaki, Y. The impact of declaring the state of emergency on human mobility during COVID-19 pandemic in Japan. Clin Epidemiol Glob Health 2022, 17, 101149. [Google Scholar]
- Mettias, B.; Jenkins, D.; Rea, P. Ten-year prevalence of acute hospital ENT infections and the impact of COVID: a large population study. Clin Otolaryngol 2023, 48, 10–16. [Google Scholar]
- Kennis, M.; Kung, V.M.; Montalbano, G.; Narvaez, I.; Franco-Paredes, C.; Vargas Barahona, L.; Madinger, N.; Shapiro, L.; Chastain, D.B.; Henao-Martínez, A.F. Seasonal variations and risk factors of Streptococcus pyogenes infection: a multicenter research network stidy. Ther Adv Infect Dis 2022, 9, 20499361221132101. [Google Scholar] [PubMed]
- Frenck RW Jr, Laudat F, Liang J, Giordano-Schmidt F, Jansen KU, Gruber W, Anderson AS, Scully IL. A Longitudinal Study of Group A Streptococcal Colonization and Pharyngitis in US Children. Pediatr Infect Dis J 2023, 42, 1045–1050.
- Brechje de Gier. Increase in invasive group A streptococcal (Streptococcus pyogenes) infections (iGAS) in young children in the Netherlands, 2022. Euro Surveill 2023, 28, 2200941.
- Elvira Cobo-Vázquez. Increasing incidence and severity of invasive Group A streptococcal disease in Spanish children in 2019–2022. Lancet Reg Health Eur 2023, 27, 100597.
- Nityanand Jain. Group A streptococcal (GAS) infections amongst children in Europe: Taming the rising tide. New Microbes New Infect 2023, 51, 101071. [Google Scholar]
- Herrera, A.L. The association between invasive group a streptococcal diseases and viral respiratory tract infections. Front Microbiol 2016, 7, 342. [Google Scholar]
- Okamoto, S. Pathogenic mechanisms of invasive group A Streptococcus infections by influenza virus–group A Streptococcus superinfection. Microbiol Immunol 2018, 62, 141–149. [Google Scholar]
- Ujiie, M. Resurgence of Respiratory Syncytial Virus Infections during COVID-19 Pandemic, Tokyo, Japan. Emerg Infect Dis 2021, 27, 2969–2970. [Google Scholar]
- Ohnishi, T. An atypical surge in RSV infections among children in Saitama, Japan in 2021. IJID 2022, 7, 124–126. [Google Scholar]
- Takahashi H, Nagamatsu H, Yamada Y, Toba N, Toyama-Kousaka M, Ota S, Morikawa M, Shinoda M, Takano S, Fukasawa S, Park K, Yano T, Mineshita M, Shinkai M. Surveillance of seasonal influenza viruses during the COVID-19 pandemic in Tokyo, Japan, 2018-2023, a single-center study. Influenza Other Respir Viruses 2024, 18, e13248.
- Flu case numbers in Japan surge, signal epidemic beginning. Available online: https://themeghalayan.com/flu-case-numbers-in-japan-surge-signal-epidemic-beginning/ (accessed on 3 June 2023).
- Japan relaxes mask guidelines in COVID milestone. Available online: https://asia.nikkei.com/Spotlight/Coronavirus/Japan-relaxes-mask-guidelines-in-COVID-milestone (accessed on 22 May 2023).
- Akaishi, T.; Kushimoto, S.; Katori, Y.; Sugawara, N.; Egusa, H.; Igarashi, K.; Fujita, M.; Kure, S.; Takayama, S.; Abe, M.; et al. COVID-19-related symptoms during the SARS-CoV-2 Omicron (B.1.1.529) variant surge in Japan. Tohoku J Exp Med 2022, 258, 103–110.
- Ashurst JV, Edgerley-Gibb L. Streptococcal pharyngitis. StatPearls. 2023.
- Pichichero, ME. Group A streptococcal infections. Pediatr Rev. 2016;37(10):403–415.
- Tan, L; et al. Lymphopenia predicts disease severity of COVID-19: a descriptive and predictive study. Signal Transduct Target Ther. 2020;5:33. 28-30.
- Fan, Y. SARS-CoV-2 Omicron variant: recent progress and future perspectives. Signal Transduct Target Ther 2022, 7, 141. [Google Scholar]
- Piersiala, K.; Bruckova, A.; Starkhammar, M.; Cardell, L.O. Acute odynophagia: a new symptom of COVID-19 during the SARS-CoV-2 Omicron variant wave in Sweden. Case Reports J Intern Med 2022, 292, 154–161. [Google Scholar]
- Sreenath K, Batra P, Vinayaraj EV, Bhatia R, SaiKiran K, Singh V, Singh S, Verma N, Singh UB, Mohan A, Bhatnagar S, Trikha A, Guleria R, Chaudhry R. Coinfections with Other Respiratory Pathogens among Patients with COVID-19. Microbiol Spectr 2021, 9, e0016321.
- Kawaguchi A, Nagaoka K, Kawasuji H, Kawagishi T, Fuchigami T, Ikeda K, Kanatani J, Doi T, Oishi K, Yamamoto Y. COVID-19 complicated with severe M1UK-lineage Streptococcus pyogenes infection in elderly patients: A report of two cases. Int J Infect Dis 2024, 148, 107246.
- Takahashi H, Morikawa M, Satake Y, Nagamatsu H, Hirose R, Yamada Y, Toba N, Toyama-Kousaka M, Ota S, Shinoda M, Mineshita M, Shinkai M. Int J Infect Dis 2024, 149, 107244.
- Boia ER, Huț AR, Roi A, Luca RE, Munteanu IR, Roi CI, Riviș M, Boia S, Duse AO, Vulcănescu DD, Horhat FG. Associated Bacterial Coinfections in COVID-19-Positive Patients. Medicina (Kaunas) 2023, 59, 1858.
| Variable | Overall | ① Pre-COVID Social Period (Jan 2019–Apr 2020) |
② Restricted Social Period (May 2020–Apr 2023) |
③ Post-Restriction Period (May 2023–Dec 2024) |
p-value Overall, (① vs. ②, ② vs. ③, ① vs. ③) |
|---|---|---|---|---|---|
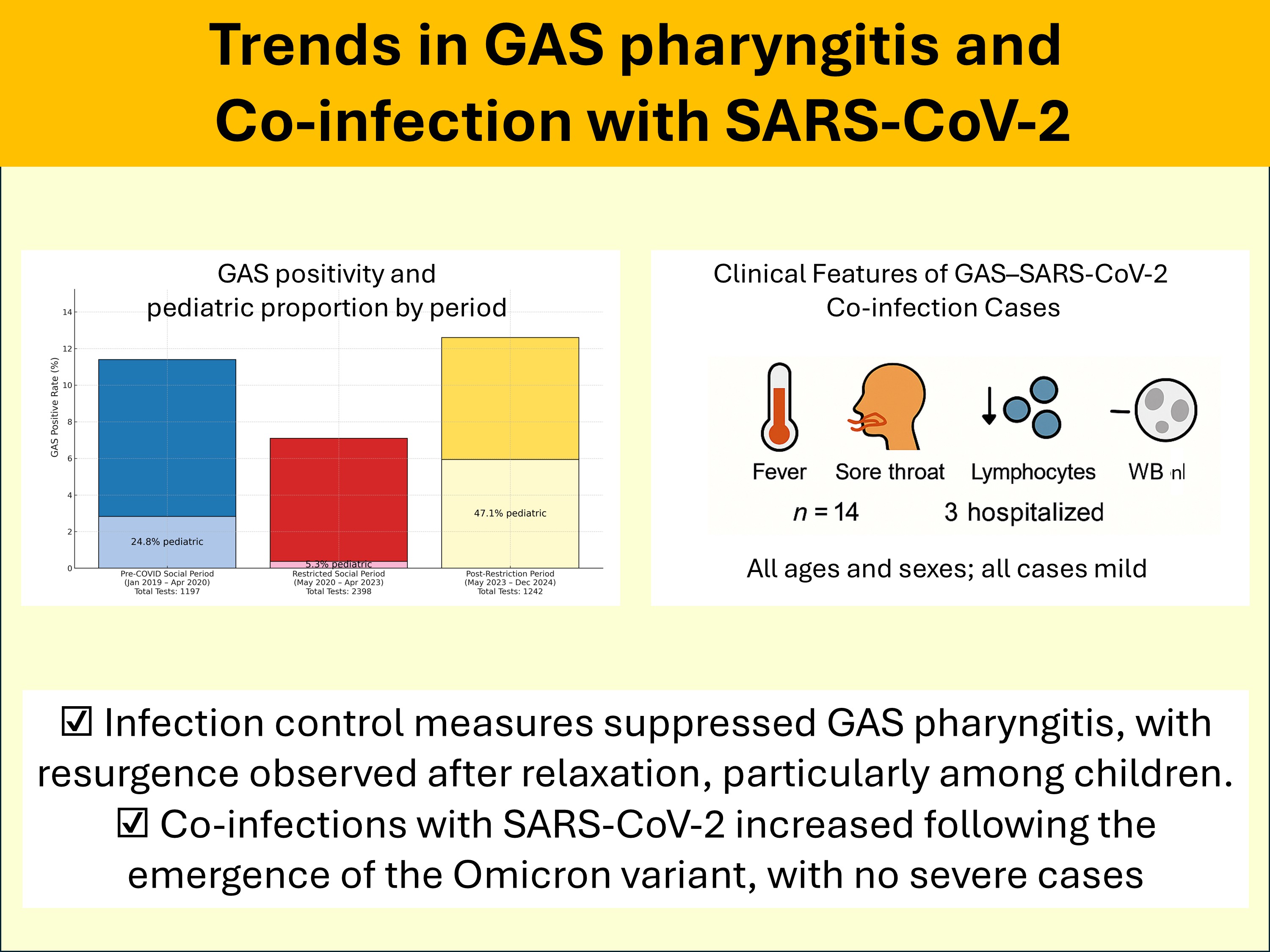
| Positivity rate (%) | 463/4,837 (9.6) | 137/1197 (11.4) | 169/2398 (7.0) | 157/1242 (12.6) | <0.001 (0.000015, <0.001, 0.459) |
| Age (mean ± SD, years) | 28.0 ± 17.2 | 27.8 ± 16.5 | 33.1 ± 14.3 | 22.6 ± 18.9 | <0.001 (0.0029, <0.001, 0.013) |
| Male (%) | 278 (60.0) | 81 (59.1) | 107 (63.3) | 90 (57.3) | 0.52 (0.48, 0.31, 0.81) |
| Children <14 years (%) | 117 (25.3) | 34 (24.8) | 9 (5.3) | 74 (47.1) | <0.001 (<0.001, <0.001, 0.00010) |
| Basic characteristics | |
|---|---|
| Total patients | 14 |
| Age (mean±SD) | 34.4 ± 17.7 |
| Sex (male/female) | 7/7 |
| Past history of COVID-19 | 2 |
| Immunodeficiency | 0 |
| Vaccine doses | |
| ≥2 doses | 10 |
| Never | 4 |
| Days from onset (mean±SD, [range]) | 1.5 ± 1.2 [0–4] |
| Complaints | |
| Fever | 14 (100%) |
| Sore throat | 12 (85.7%) |
| Cough | 7 (50%) |
| Headache | 6 (42.9%) |
| Malaise | 6 (42.9%) |
| Arthralgia | 4 (28.6%) |
| Sputum | 4 (28.6%) |
| Nasal discharge | 3 (21.4%) |
| Muscle pain | 2 (14.3%) |
| Nasal congestion | 2 (14.3%) |
| Chills | 2 (14.3%) |
| Nausea | 2 (14.3%) |
| Vital signs | |
| Body temperature (mean±SD, [range]) | 38.4 ± 1.2℃ [37.1–40.0] |
| SpO2 under room air (mean±SD, [range]) | 98.0 ± 1.0% [97–99] |
| Systolic blood pressure (mean±SD, [range]) | 122.5 ± 16.9 [90–149] |
| Heart rate (mean±SD, [range]) | 97.1 ± 15.5 [72–120] |
| Laboratory and imaging data | |
| WBC (/μL) | 5812.5 ± 660.0 [4400–6600] |
| Neutrophil count (/μL) | 4342 ± 911 [3089–5316] |
| Lymphocyte count (/μL) | 954 ± 542 [180–1401] |
| CRP (mg/dL) | 2.0 ± 1.5 [0.6–4.0] |
| Ct value of SARS-CoV-2 PCR | 20.2 ± 4.3 [15.2–29.4] |
| Pneumonia findings on chest imaging/total examined (%) | 1/5 (20%) |
| Clinical course and treatment | |
| Hospitalized/outpatient cases | 3/11 |
| Treatment | Antibiotics: 9 patients, antibiotics + antiviral: 5 patients |
| Treatment details | |
| AMPC/CVA | 5 |
| CAM | 2 |
| ABPC/SBT | 1 |
| CFPN-PI | 1 |
| CCL+ensitrelvir | 2 |
| AMPC/CVA+molnupiravir | 1 |
| ABPC/SBT+CAM+remdesivir | 1 |
| ABPC/SBT+nirmatrelvir | 1 |
| Outcomes | Recovery: 14/14 (100%) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).




