Submitted:
07 March 2025
Posted:
10 March 2025
You are already at the latest version
Abstract
Dental hygienists play a crucial role in patient communication, making communication competency an essential skill. This study aimed to develop and validate the Patient-Centered Communication Competency Scale (PCCS) for dental hygienists. Initial items were generated through a literature review, expert content validity assessment, and preliminary survey. An online survey was conducted with 400 dental hygienists working in dental clinics and hospitals. Construct validity was examined using exploratory factor analysis (EFA) and confirmatory factor analysis (CFA), and reliability was assessed with Cronbach’s alpha. The preliminary 38-item scale was refined through five rounds of EFA, resulting in an 11-item scale with three subscales: Assertiveness, Empathy, and Respect. The CFA results indicated a good model fit (χ²/df = 1.749, RMR = 0.027, RMSEA = 0.061, GFI = 0.941, NFI = 0.911, IFI = 0.960, CFI = 0.959, TLI = 0.949), with strong convergent and discriminant validity. The PCCS demonstrated strong internal consistency (Cronbach’s alpha = 0.862) and criterion validity, confirmed by its positive correlation with self-efficacy and job satisfaction. The proposed PCCS is a valid and reliable tool for assessing and improving dental hygienists’ communication skills, with potential applications in training programs and communication competency research in dental settings.
Keywords:
1. Introduction
2. Materials and Methods
2.1. Design and Ethical Considerations
2.2. Scale Development
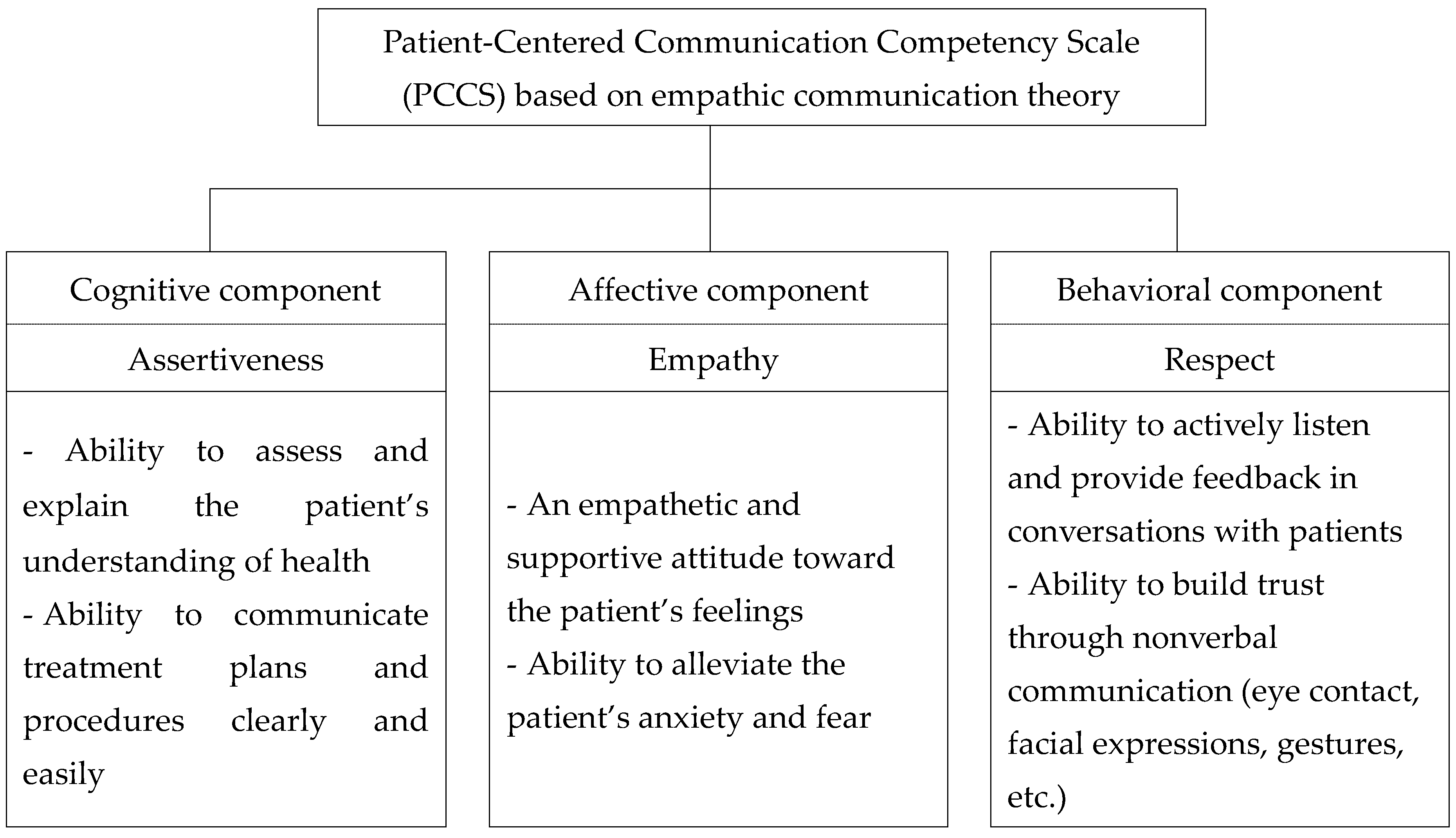
2.2.1. Conceptual Framework and Initial Item Generation
2.2.2. Content Validity
2.2.3. Preliminary survey
2.3. Validity and Reliability
2.3.1. Participants
2.3.2. Measurement
2.3.3. Data Collection
2.3.4. Validity and Reliability Tests
2.4. Optimization of the PCCS
3. Results
3.1. Characteristics of the Study Participants
3.2. Item Analysis
3.3. Construct Validity
3.3.1. Exploratory Factor Analysis (EFA)
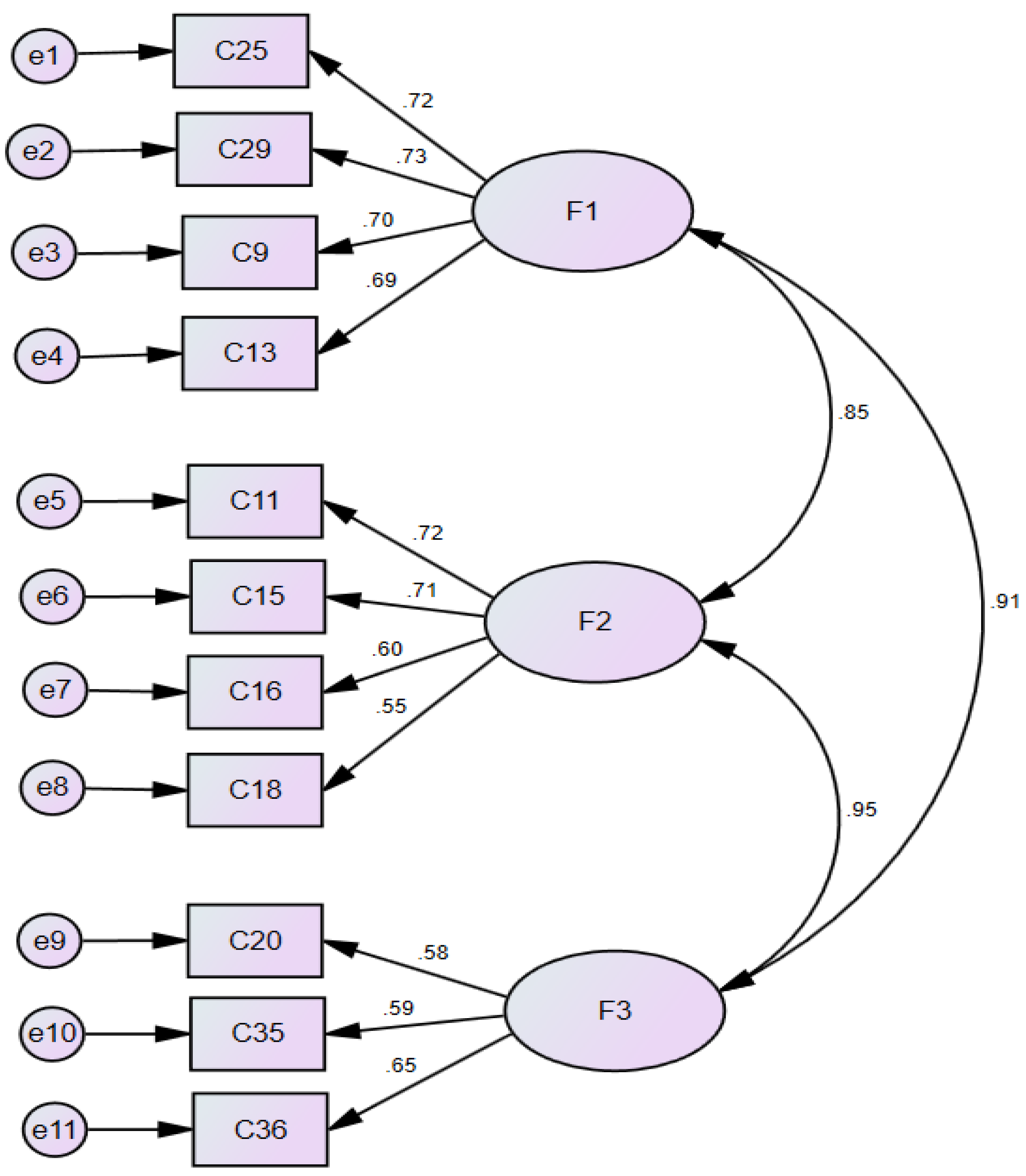
3.3.2. Confirmatory Factor Analysis for Validity (CFA)
3.4. Criteria Validity and Reliability of PCCS
4. Discussion
4.1. Strengths and Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| AVE | average variance extracted |
| CFA | confirmatory factor analysis |
| CFI | comparative fit index |
| CR | construct reliability |
| EFA | exploratory factor analysis |
| GFI | goodness-of-fit index |
| IFI | incremental fit index |
| NFI | normed fit index |
| PCCS | Patient-Centered Communication Competency Scale |
| RMR | root mean residual |
| RMSEA | root mean square error of approximation |
| TLI | Tucker-Lewis index |
References
- Arrindell, W. A., & Van der Ende, J. (1985). An empirical test of the utility of the observations-to-variables ratio in factor and components analysis. Applied Psychological Measurement, 9(2),165-178.
- Chen, G., Gully, S. M., & Eden, D. (2001). Validation of a new general self-efficacy scale. Organizational Research Methods, 4(1), 62-83. [CrossRef]
- Cho, H. J. (2016). A study of the effects of resilience factor on flight attendants' job performance and organizational effectiveness, Focused on the mediating effects of self-efficacy [Doctoral dissertation, Kyonggi University, Seoul, South Korea].
- Choi, C. H., & Yoo, Y.Y. (2017). The study on the comparative analysis of EFA and CFA. Journal of Digital Convergence, 15(10), 103-111. [CrossRef]
- Choi, D. S., Kim, S. H.,& Kim, J. S. (2015). A comparative analysis of competencies in American dental education association and American dental hygiene schools. Journal of Korean Society of Dental Hygiene, 15(3), 547-53. [CrossRef]
- Cohen J. A power primer. (1992). Psychological Bulletin. 112(1), 155-159. [CrossRef]
- DeVellis, R. F. (2017). Scale development: Theory and applications (4th ed.). Thousand Oaks, CA: Sage.
- Field A. (2013). Discovering statistics using IBM SPSS statistics: And sex and drugs and rock 'n' roll. 4th ed. London, UK: Sage publications.
- Gwon, A. R., & Han, S. J. (2015). Effect of communication competence on the organizational effectiveness in dental hygienists, Journal of Korean society of Dental Hygiene, 15(6), 1009-1017. [CrossRef]
- Hair JR, J. F., Anderson, R. E., Babin, B. J., & Black, W. C. (2010). Multivariate data analysis: A global perspective. 7th ed. Edinburgh Gate, Harlow: Pearson Education.
- Haribhai-Thompson, J., McBride-Henry, K., Hales, C., & Rook, H. (2022). Understanding of empathetic communication in acute hospital settings: A scoping review. BMJ Open, 12: e063375. [CrossRef]
- Heo, M. L. (2018). Development of the patient caring communication scale [Doctoral dissertation, Eulji University, Daejeon, South Korea].
- Heo, M. L., & Im, S. B. (2019). Development of the patient caring communication scale. Journal of Korean Academy of Nursing, 49(1), 80-90. [CrossRef]
- Heo, Y. J. (2014). Doctor’s competency and empowerment measures desired by the state and society. Journal of the Korean Medical Association, 57(2), 121-7. [CrossRef]
- Ho, J. C. Y., Chai, H. H., Luo, B. W., Lo, E. C. M., Huang, M. Z., & Chu, C. H. (2025). An Overview of Dentist–Patient Communication in Quality Dental Care. Dentistry Journal, 13(1), 31. [CrossRef]
- Howick, J., Moscrop, A., Mebius, A., Fanshawe, T. R, Lewith, G., Bishop, F.L., Mistiaen, P., Roberts, N.W., Dieninytė, E., Hu, X.Y., Aveyard, P., & Onakpoya, I. J. (2018). Effects of empathic and positive communication in healthcare consultations: A systematic review and meta-analysis. Journal of the Royal Society of Medicine, 111(7), 240–252. [CrossRef]
- Hur, G. H. (2003). Construction and validation of a global interpersonal communication competence scale. Korean Society for Journalism and Communication Studies, 47(6), 380-408.
- Hymes, D. (1974). Foundation in sociolinguistics. Philadelphia: University of Pennsylvania Press.
- Jang, J. Y. (2023). The effect of nurses’ communication skills and self-efficacy on job satisfaction [Master’s Thesis, Changwon University, Gyeongsangnam-do, South Korea].
- Jeong, M. A. (2022). The study on effect of communication ability of dental hygienist on job satisfaction and turnover intention. The Journal of the Korea Contents Association, 22(8), 579-586. [CrossRef]
- Kang, J. O., Kim, J. H., Hwang, J. M, Kwon, H. J., Seong, J. M., Lee, S. K., Kim, C. H., Kim, H.Y., Cho, Y. S., & Park, Y. D. (2010). Recognition about communication of dental personnels in dental clinics and hospitals in the capital. Journal of the Korean Academy of Oral Health, 34(3), 318-326.
- Kang, S. K., Bae, K. H., & Lim., S. R. (2014). Analysis of communication of dental hygienist in oral hygiene instruction during scaling. Journal of Dental Hygiene Science, 14(4), 546-553. [CrossRef]
- Kim, B. J., Lee, S. Y., An, G. J., Lee, G. A., & Yun, H. J. (2019). Influence of communication competency and nursing work environment on job satisfaction in hospital nurses. Journal of Health Informatics and Statistics, 44(2):189-197. [CrossRef]
- Kim, H. J. (2021). Development and validation of a self-assessment tool for communication skills needed in nursing assessment [Doctoral dissertation, Eulji University, Daejeon, South Korea].
- Kim, H. J., Ha, J. H., & Jue, J. (2020). Compassion satisfaction and fatigue, emotional dissonance, and burnout in therapists in rehabilitation hospitals. Psychology, 11, 190-203. [CrossRef]
- Kim, H. J., & Oh, H. Y. (2023). The Validity and Reliability of Nursing Assessment Communication-Competence Scale for Clinical Nurses. Journal of Korean Academy of Fundamentals of Nursing, 30(1), 78-89. [CrossRef]
- Kim, D. E., Jang, J. H. (2024). Communication competency for dental hygienists in Korea: A scoping review. Journal of Korean society of Dental Hygiene, 12(5), 361-372. [CrossRef]
- Ko, Y. J., & Hong, G. R. (2022). Development and evaluation of nursing work environment scale of clinical nurses. Journal of Korean Academy of Nursing Administration, 28(5), 576-585. [CrossRef]
- Lee, A. K., Yeo, J. Y., Jung, S. W., & Byun, S. S. (2013). Relations on Communication Competence, Job-stress and Job-satisfaction of Clinical Nurse. The Journal of the Korea Contents Association, 13(12):299-308. [CrossRef]
- Lee, B. S., Eo, Y. S., & Lee, M. A. (2018), Development of job satisfaction scale for clinical nurses. Journal of Korean Academy of Nursing, 48(1), 12-25. [CrossRef]
- Lee, I. H. (2019). The sub-elements of communication competency as core competence reflected in the 2015 revised curriculum. Journal of Curriculum and Evaluation, 22(3):1-29. [CrossRef]
- Lee, J. H., & Choi, J. M. (2012). A study on the relationship between patient's medical communication, reliance and satisfaction to dental hygienist. Journal of Korean society of Dental Hygiene, 12(5), 1017-1027. [CrossRef]
- Lee, J. Y., & Kang, Y. J. (2019). A study on factors affecting job satisfaction of dental hygienists. The Journal of the Korea Contents Association, 19(7), 478-488. [CrossRef]
- Lee, S. K., Hwang, K. S., Park, Y. D., & Beom, K. C. (2011). The relationship between factors influencing smooth communication among dental workers. Journal of the Korean Academy of Oral Health, 35(1), 85-92.
- Lee, Y. H., Lee, Y. M., & Park. Y, G. (2011). Patients’ expectations of a good dentist: The views of communication. Korean Journal of Health Communication, 6(2), 89-104. [CrossRef]
- Mishra, P., Pandey, C. M., Singh, U., Gupta, A., Sahu, C., & Keshri, A. (2019). Descriptive statistics and normality tests for statistical data. Annals of Cardiac Anaesthesia, 22(1): 67-72. [CrossRef]
- McCabe C. (2004). Nurse-patient communication: An exploration of patients’ experiences. Journal of Clinical Nursing, 13(1), 41-49. [CrossRef]
- Moon H. J., & Lim S.R. (2017). Development of a job competency model of a dental intermediary-manager using the Delphi method. Journal of Dental Hygiene Science, 17(2), 150-159. [CrossRef]
- Moon, H. J., Lee, S. Y., & Lim, S. R. (2014). Validity and reliability of the assessment tool for measuring communication skills of dental hygienist. Journal of dental hygiene science, 14(2):198-206.
- Namkung, J., & Kim, J. H. (2010). The developing and validation of communication ability scale. Korean Society for Creativity Education, 10(1), 85-109.
- Nunnally, J., & Bernstein, I. H. (1994). Psychometric theory (3rd ed). New York: McGraw Hill.
- Park, J. H. (2020). Development of dental hygienists job satisfaction scale and path analysis of psychological ownership, job engagement, job performance [Doctoral dissertation, Namseoul University, Chungcheongnam-do, South Korea].
- Park, J. H., Sung, Y. H., Song, M. S., Cho, J. S., & Sim, W. H. (2000). The classification of standard nursing activities in Korea. Journal of Korean Academy of Nursing, 30(6), 1411-1426. [CrossRef]
- Rogers, Carl R. (1951). Client-centered therapy. Boston: Houghton-Mifflin, pp. 560. [CrossRef]
- Song, T. M., & Kim, G. S. (2012). Structural equation modeling for health & welfare research: From beginner to advanced. Seoul: Hannarae academy.
- Son, Y. H. (2016). An exploratory study for development of tools to measure university students’ communication competence. Journal of Speech, Media & Communication Association, 15(1), 83-107.
| Variables | Categories | Total (n = 400) | EFA (n = 200) | CFA (n = 200) |
|---|---|---|---|---|
| n (%) | n (%) | n (%) | ||
| Sex | Male | 38 (9.5) | 18 (9.0) | 20 (10.0) |
| Female | 362 (90.5) | 182 (91.0) | 180 (90.0) | |
| Age (in years) | ≤ 29 | 147 (36.8) | 75 (37.5) | 72 (36.0) |
| 30–39 | 212 (53.0) | 103 (51.5) | 109 (54.5) | |
| ≥ 40 | 41 (10.3) | 22 (11.0) | 19 (9.5) | |
| Education | College | 222 (55.5) | 112 (56.0) | 110 (55.0) |
| University | 132 (33.0) | 67 (33.5) | 65 (32.5) | |
| ≥ Master | 46 (11.5) | 21 (10.5) | 25 (12.5) | |
| Workplace | Dental clinic | 300 (75.0) | 143 (71.5) | 157 (78.5) |
| Dental hospital | 84 (21.0) | 48 (24.0) | 36 (18.0) | |
| Tertiary hospital | 13 (3.3) | 8 (4.0) | 5 (2.5) | |
| Others | 3 (0.8) | 1 (0.5) | 2 (1.0) | |
| Work experience (in years) | ≤ 3 | 70 (17.5) | 32 (16.0) | 38 (9.0) |
| ≥ 3–≤ 7 | 140 (35.0) | 69 (34.5) | 71 (35.5) | |
| ≥ 7 | 178 (44.5) | 94 (47.0) | 84 (42.0) | |
| Current position | Clinical dental hygienist | 257 (64.3) | 129 (64.5) | 128 (64.0) |
| Team leader | 53 (13.3) | 29 (14.5) | 24 (12.0) | |
| Counseling manager | 68 (17.0) | 31 (15.5) | 37 (18.5) | |
| Others | 22 (5.5) | 11 (5.5) | 11 (5.5) |
| No | Items | Item-total correlation |
Factor loading | ||
|---|---|---|---|---|---|
| 1 | 2 | 3 | |||
| 25 | Encourage patients to express their emotions freely | 0.612 | 0.743 | 0.093 | 0.226 |
| 29 | Present information by topic at a pace the patient can follow | 0.600 | 0.763 | 0.107 | 0.080 |
| 9 | Mirror the patient’s words or actions to demonstrate empathy | 0.587 | 0.692 | 0.272 | 0.185 |
| 13 | Repeat questions to clarify implied content and emotions | 0.502 | 0.661 | 0.198 | 0.157 |
| 11 | Communicate in a structured and proficient manner | 0.462 | 0.361 | 0.526 | 0.235 |
| 15 | Summarize key points throughout the conversation | 0.683 | 0.161 | 0.791 | 0.176 |
| 16 | Clearly signal transitions between topics or situations. | 0.628 | 0.103 | 0.695 | 0.367 |
| 18 | Redirect off-topic discussions back to the main topic | 0.553 | 0.164 | 0.725 | -0.011 |
| 20 | Clarify expectations regarding diagnosis, treatment, prognosis | 0.682 | 0.165 | 0.302 | 0.751 |
| 35 | Conclude communication with gratitude for cooperation | 0.675 | 0.151 | 0.104 | 0.801 |
| 36 | Ask if the patient has any additional questions or concerns | 0.672 | 0.256 | 0.118 | 0.770 |
| Eigenvalues | 2.360 | 2.160 | 21.453 | ||
| % of variance | 21.453 | 19.640 | 41.093 | ||
| % of cumulated variance | 21.453 | 19.413 | 60.508 | ||
| Kaiser-Meyer-Olkin (KMO) value: 0.84, Bartlett’s sphericity test value: 674.772 (p < 0.001) | |||||
| Concept | Factors | Item number |
Standardized estimate (β) |
SE | AVE | CR |
|---|---|---|---|---|---|---|
| Behavioral | Respect | 25 | 0.715 | 0.308 | 0.614 | 0.864 |
| 29 | 0.729 | 0.273 | ||||
| 9 | 0.703 | 0.339 | ||||
| 13 | 0.691 | 0.348 | ||||
| Cognitive | Assertiveness | 11 | 0.715 | 0.342 | 0.533 | 0.818 |
| 15 | 0.705 | 0.327 | ||||
| 16 | 0.598 | 0.318 | ||||
| 18 | 0.547 | 0.473 | ||||
| Affective | Empathy | 20 | 0.583 | 0.441 | 0.472 | 0.728 |
| 35 | 0.594 | 0.440 | ||||
| 36 | 0.646 | 0.362 | ||||
| Model fitness: χ2/df = 1.749, RMR = 0.027, RMSEA = 0.061, GFI = 0.941, NFI = 0.911, IFI = 0.960, CFI = 0.959, TLI = 0.949 | ||||||
| Factors | Respect | Assertiveness | Empathy |
|---|---|---|---|
| Respect | 0.783 | ||
| Assertiveness | 0.584* | 0.730 | |
| Empathy | 0.551* | 0.566* | 0.687 |
| *p < 0.001; The shaded section = discriminant validity; The non-shaded section = correlation | |||
| PCCS | Self-efficacy | Job satisfaction | Mean ± SD | Cronbach’s α |
|---|---|---|---|---|
| r | r | |||
| Total | 0.603* | 0.624* | 3.94 ± 0.52 | 0.862 |
| Respect | 0.441* | 0.592* | 3.94 ± 0.63 | 0.777 |
| Assertiveness | 0.526* | 0.520* | 3.95 ± 0.57 | 0.731 |
| Empathy | 0.548* | 0.452* | 3.93 ± 0.66 | 0.701 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




