Submitted:
19 February 2025
Posted:
21 February 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
1.1. What Is the Gut Microbiota?
1.2. Intestinal Dysbiosis and Its Effects on Canine Health
1.3. Modulation of Intestinal Microbiota Composition
2. Materials and Methods
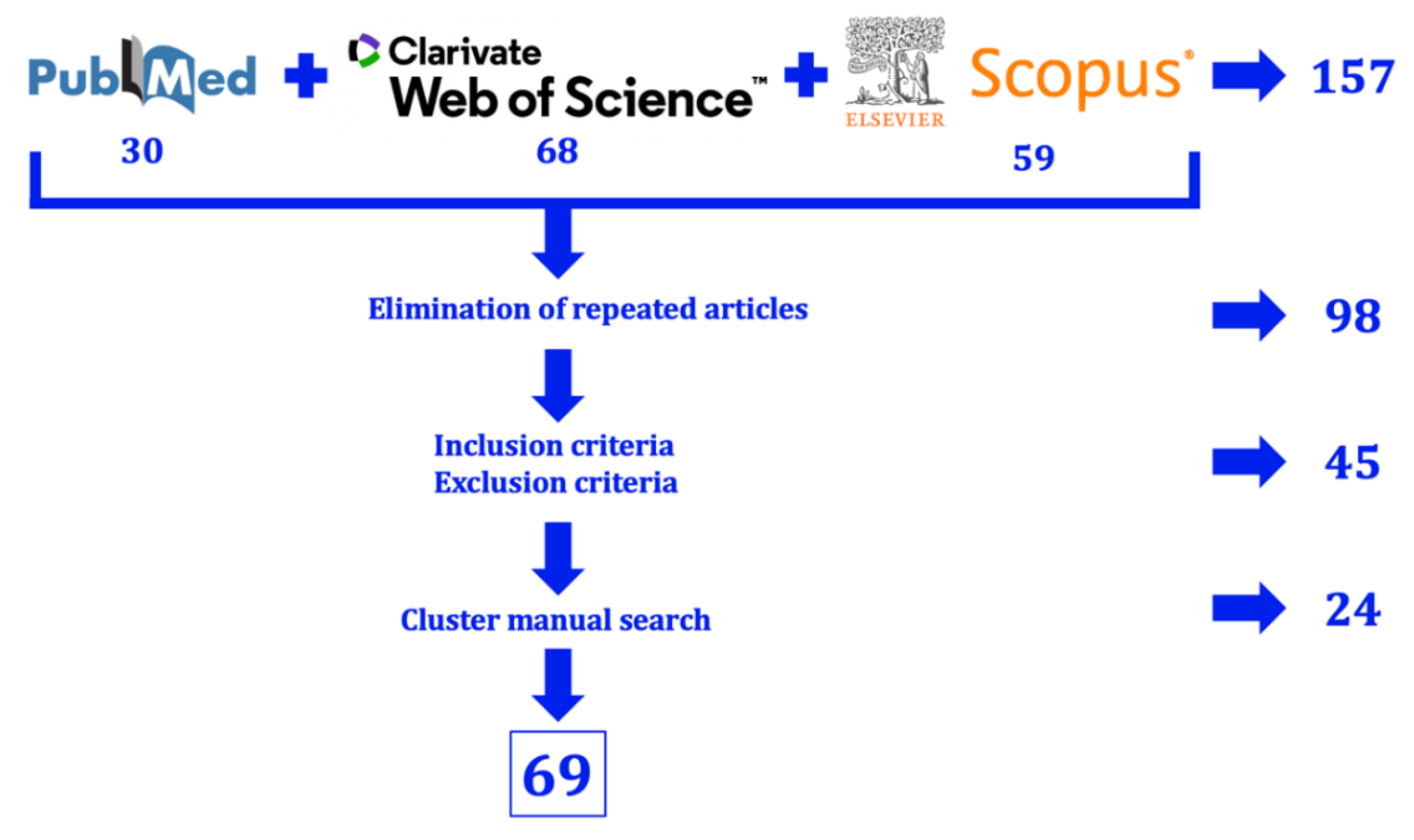
2.1. Systematic Literature Review
2.2. Meta-Analysis
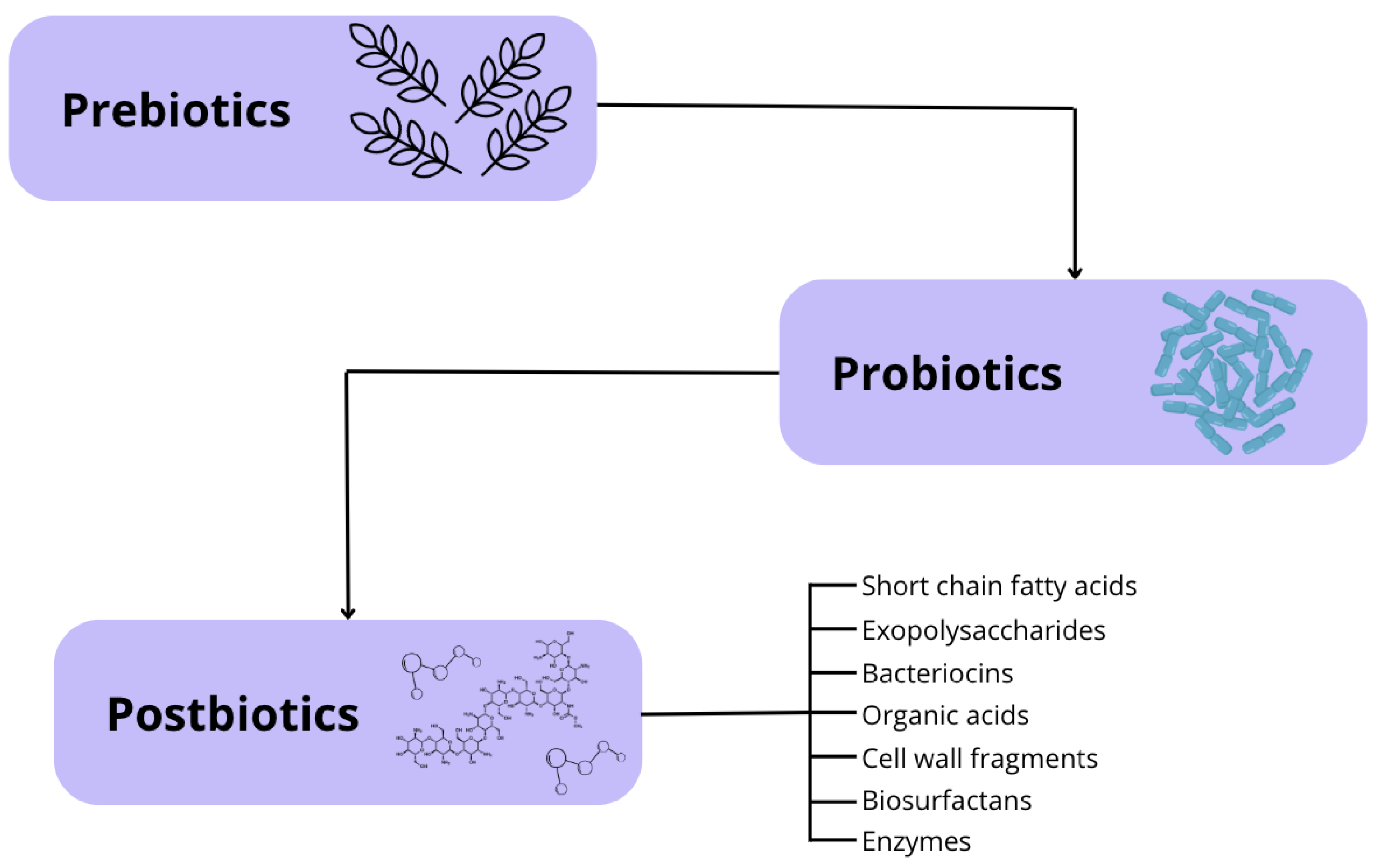
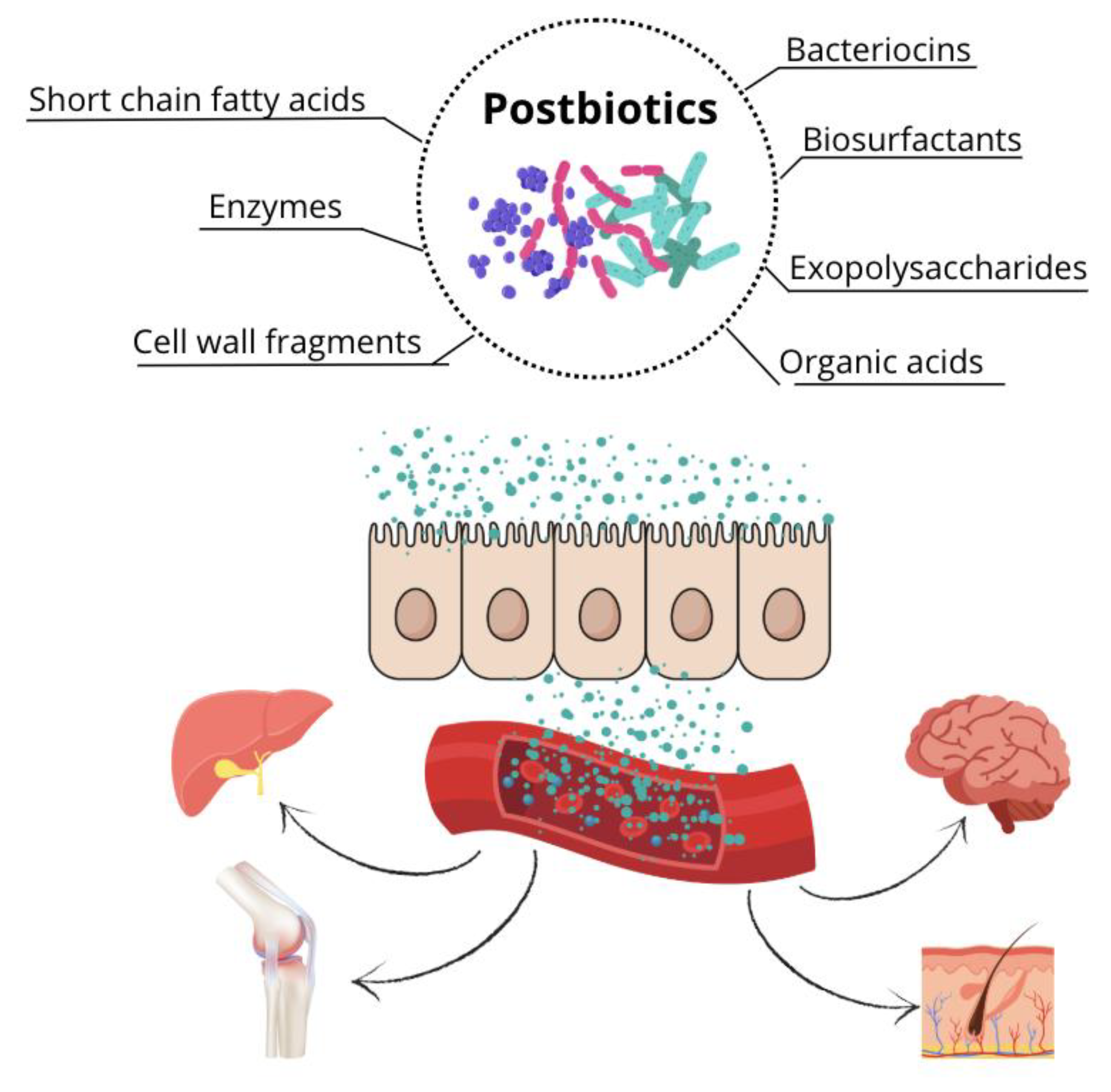
3. Type of Postbiotics
3.1. Short-Chain Fatty Acids
3.2. Cell Wall Fragments
3.3. Exopolysaccharides
3.4. Bacteriocins
3.5. Organic Acids
3.6. Biosurfactants
3.7. Enzymes
3.8. Other Metabolites
4. Mechanisms of Action and Health Effects in Dogs
4.1. Immunomodulatory Action
4.2. Anti-Inflammatory Action
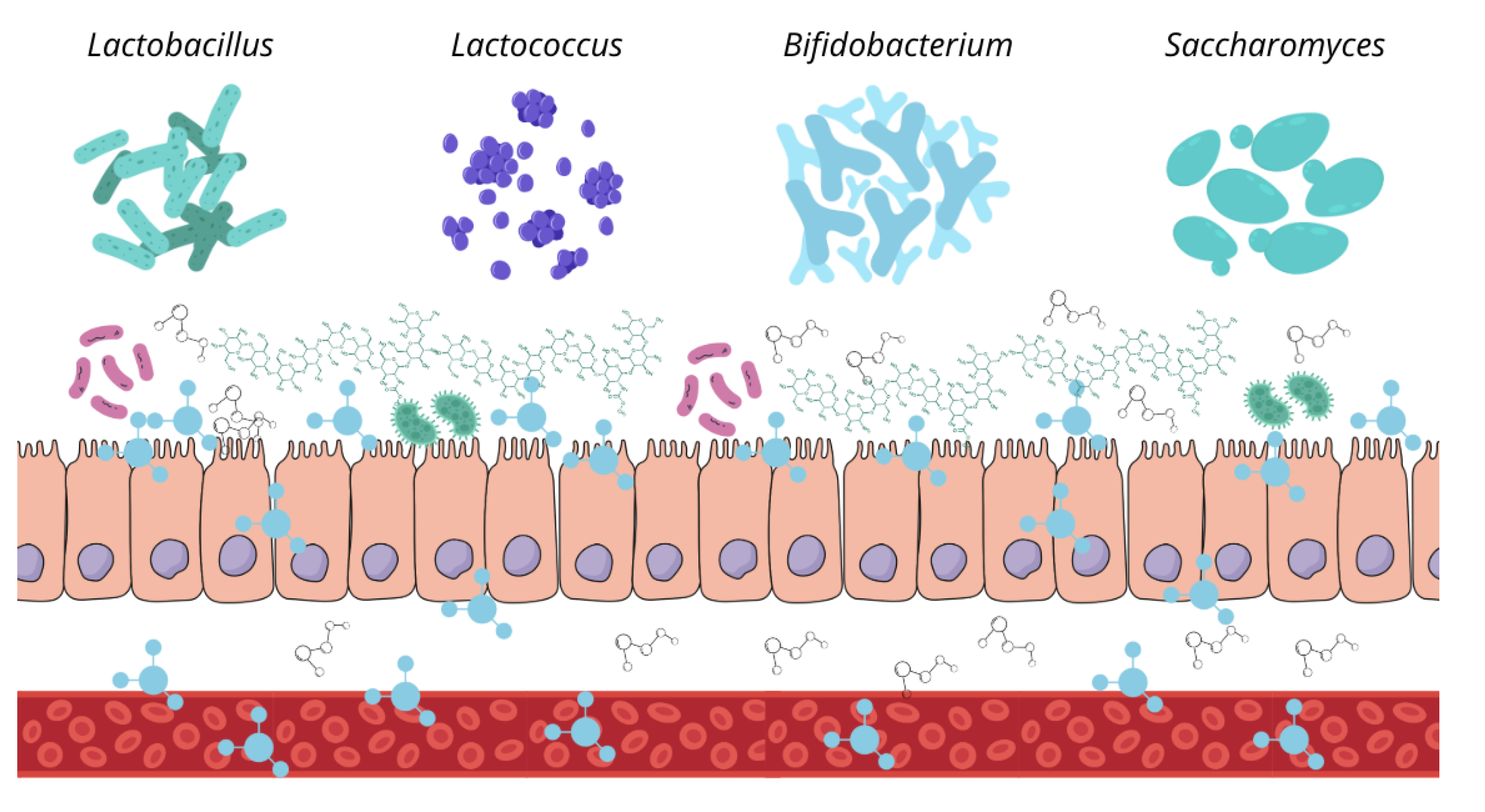
4.3. Modulatory Effects on the Gut Microbiota
4.4. Antimicrobial Action
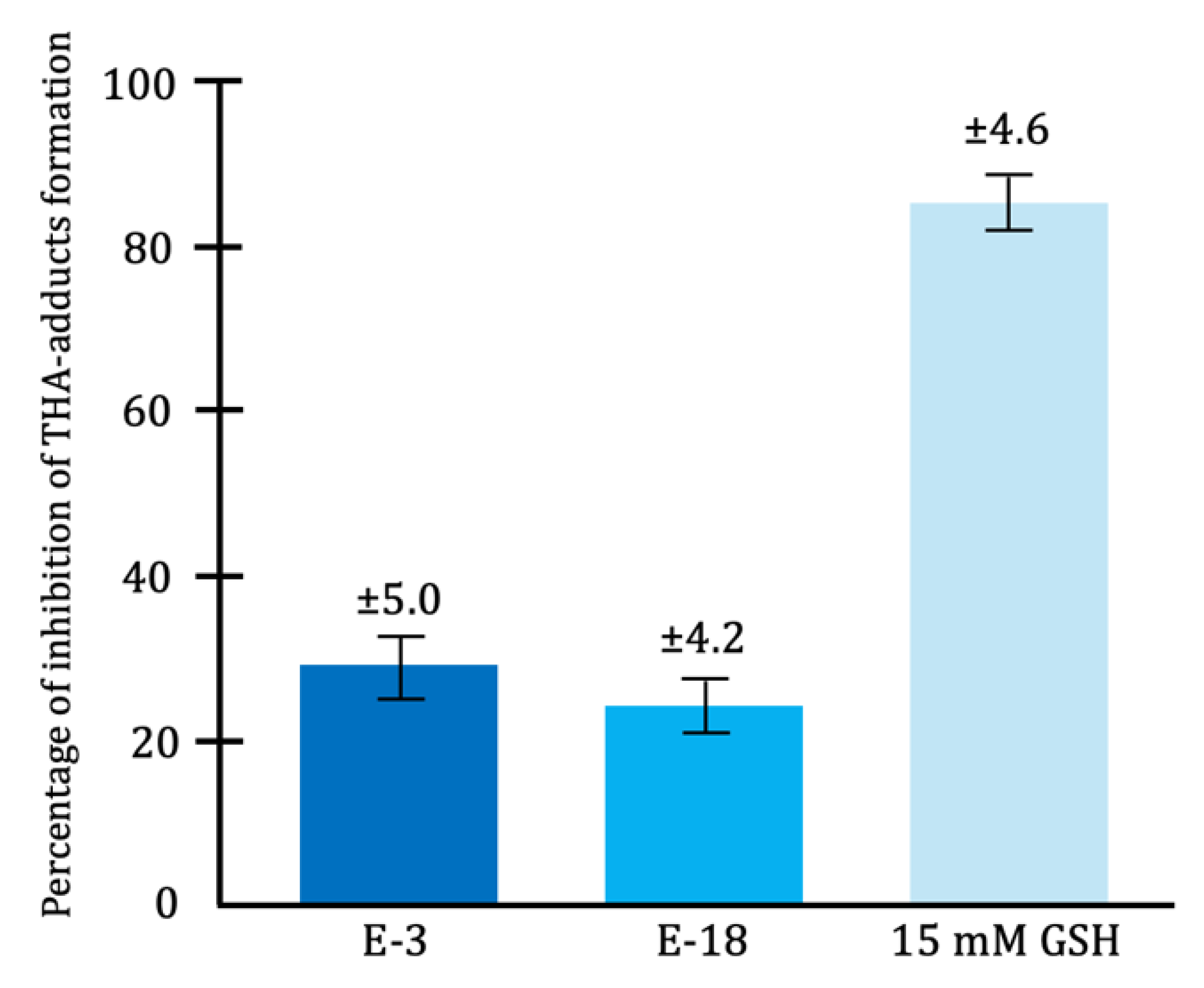
4.5. Antioxidant Action
4.6. Other Effects of Postbiotics
5. Meta-Analysis
5.1. Fecal Parameters
5.2. Gut Microbiota
6. Production and Presentation Forms of Postbiotics
7. Future Perspectives
8. Conclusions
Supplementary Materials
Author Contributions
Funding
Review and Meta-analysis Statement
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| SCFA | Short-Chain Fatty Acids |
| BCFA | Branched-Chain Fatty Acids |
| TLR | Toll-like receptor |
| IBD | Inflammatory bowel disease |
| LPS | Lipopolysaccharide |
| AMR | Antimicrobial resistance |
| ENS | Enteric nervous system |
| CNS | Central nervous system |
| MOS | Mannan-oligosaccharides |
| FOS | Fructooligosaccharides |
| ISAPP | International Scientific Association of Probiotics and Prebiotics |
| IL | Interleukin |
| TNF-α | Tumor necrosis factor-alpha |
| GPx | Glutathione peroxidase |
| SOD | Superoxide dismutase |
| THA | Terephtalic acid |
| GSH | Reduced glutathione |
References
- Yang, Q.; Wu, Z. Gut Probiotics and Health of Dogs and Cats: Benefits, Applications, and Underlying Mechanisms. Microorganisms 2023, 11(10), 2452. [Google Scholar] [CrossRef]
- Rowland, I.; Gibson, G.; Heinken, A.; Scott, K.; Swann, J.; Thiele, I.; Tuohy, K. Gut microbiota functions: metabolism of nutrients and other food components. Eur. J. Nutr. 2017, 57(1), 1–24. [Google Scholar] [CrossRef] [PubMed]
- Pilla, R.; Suchodolski, J.S. The Role of the Canine Gut Microbiome and Metabolome in Health and Gastrointestinal Disease. Front. Vet. Sci. 2020, 6. [Google Scholar] [CrossRef] [PubMed]
- Gomaa, E.Z. Human gut microbiota/microbiome in health and diseases: a review. Antonie Van Leeuwenhoek 2020, 113(12), 2019–2040. [Google Scholar] [CrossRef] [PubMed]
- Manor, O.; Dai, C.L.; Kornilov, S.A.; Smith, B.; Price, N.D.; Lovejoy, J.C.; Gibbons, S.M.; Magis, A.T. Health and disease markers correlate with gut microbiome composition across thousands of people. Nat. Commun. 2020, 11(1). [Google Scholar] [CrossRef]
- Kinross, J.M.; Darzi, A.W.; Nicholson, J.K. Gut microbiome-host interactions in health and disease. Genome Med. 2011, 3(3), 14. [Google Scholar] [CrossRef]
- Kers, J.G.; Saccenti, E. The Power of Microbiome Studies: Some Considerations on Which Alpha and Beta Metrics to Use and How to Report Results. Front. Microbiol. 2022, 12. [Google Scholar] [CrossRef]
- Clemente, J.C.; Manasson, J.; Scher, J.U. The role of the gut microbiome in systemic inflammatory disease. BMJ 2018, j5145. [Google Scholar] [CrossRef]
- Duvallet, C.; Gibbons, S.M.; Gurry, T.; Irizarry, R.A.; Alm, E.J. Meta-analysis of gut microbiome studies identifies disease-specific and shared responses. Nat. Commun. 2017, 8(1). [Google Scholar] [CrossRef]
- Ma, L.; Zhao, H.; Wu, L.B.; Cheng, Z.; Liu, C. Impact of the microbiome on human, animal, and environmental health from a One Health perspective. Sci. One Health 2023, 2, 100037. [Google Scholar] [CrossRef]
- Gómez, J.M.R. La microbiota, un pilar esencial del enfoque One Health (“Una Salud”). Microbiota, Probióticos & Prebióticos, 2022. [Google Scholar]
- Gortázar, C.; Ferroglio, E.; Höfle, U.; Frölich, K.; Vicente, J. Diseases shared between wildlife and livestock: a European perspective. Eur. J. Wildl. Res. 2007, 53(4). [Google Scholar] [CrossRef]
- Deng, P.; Swanson, K.S. Gut microbiota of humans, dogs and cats: current knowledge and future opportunities and challenges. Br. J. Nutr. 2014, 113(S1), S6–S17. [Google Scholar] [CrossRef] [PubMed]
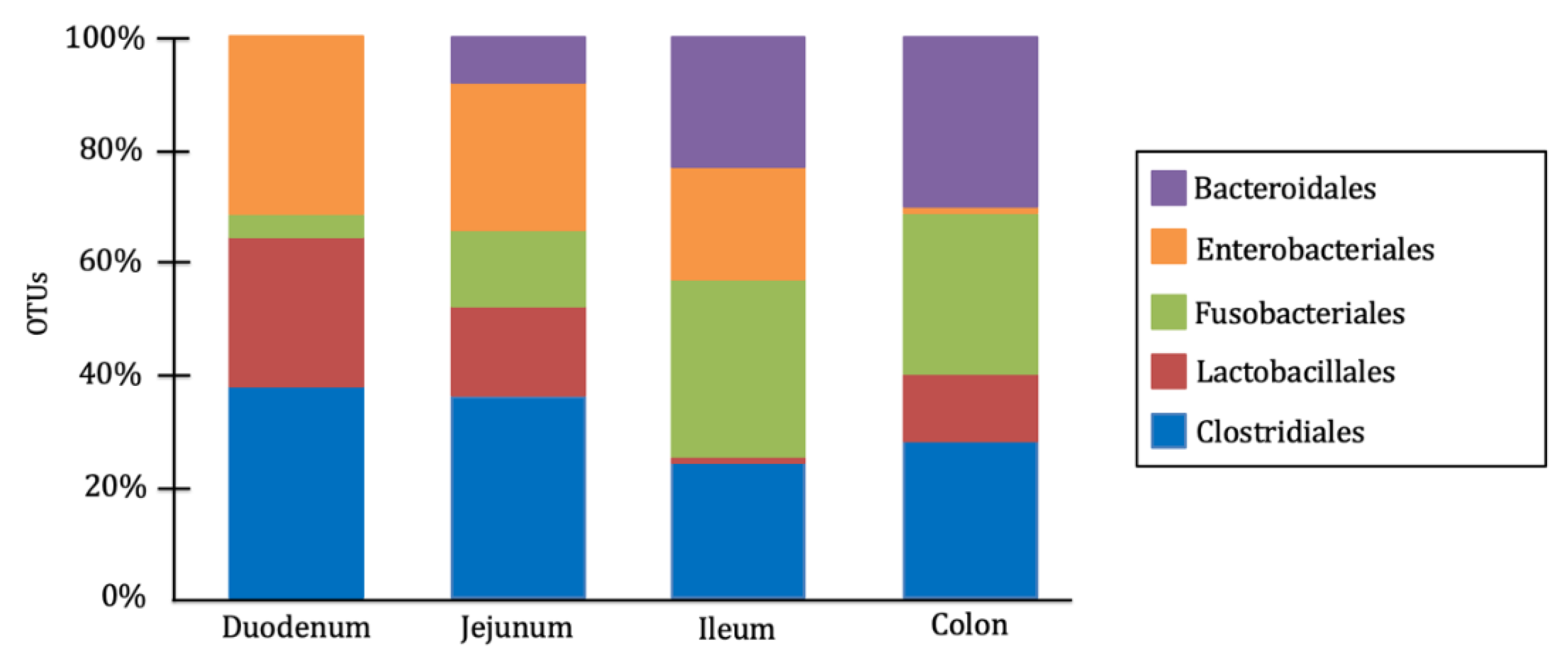
- Suchodolski, J.S.; Camacho, J.; Steiner, J.M. Analysis of bacterial diversity in the canine duodenum, jejunum, ileum, and colon by comparative 16S rRNA gene analysis. FEMS Microbiol. Ecol. 2008, 66(3), 567–578. [Google Scholar] [CrossRef] [PubMed]
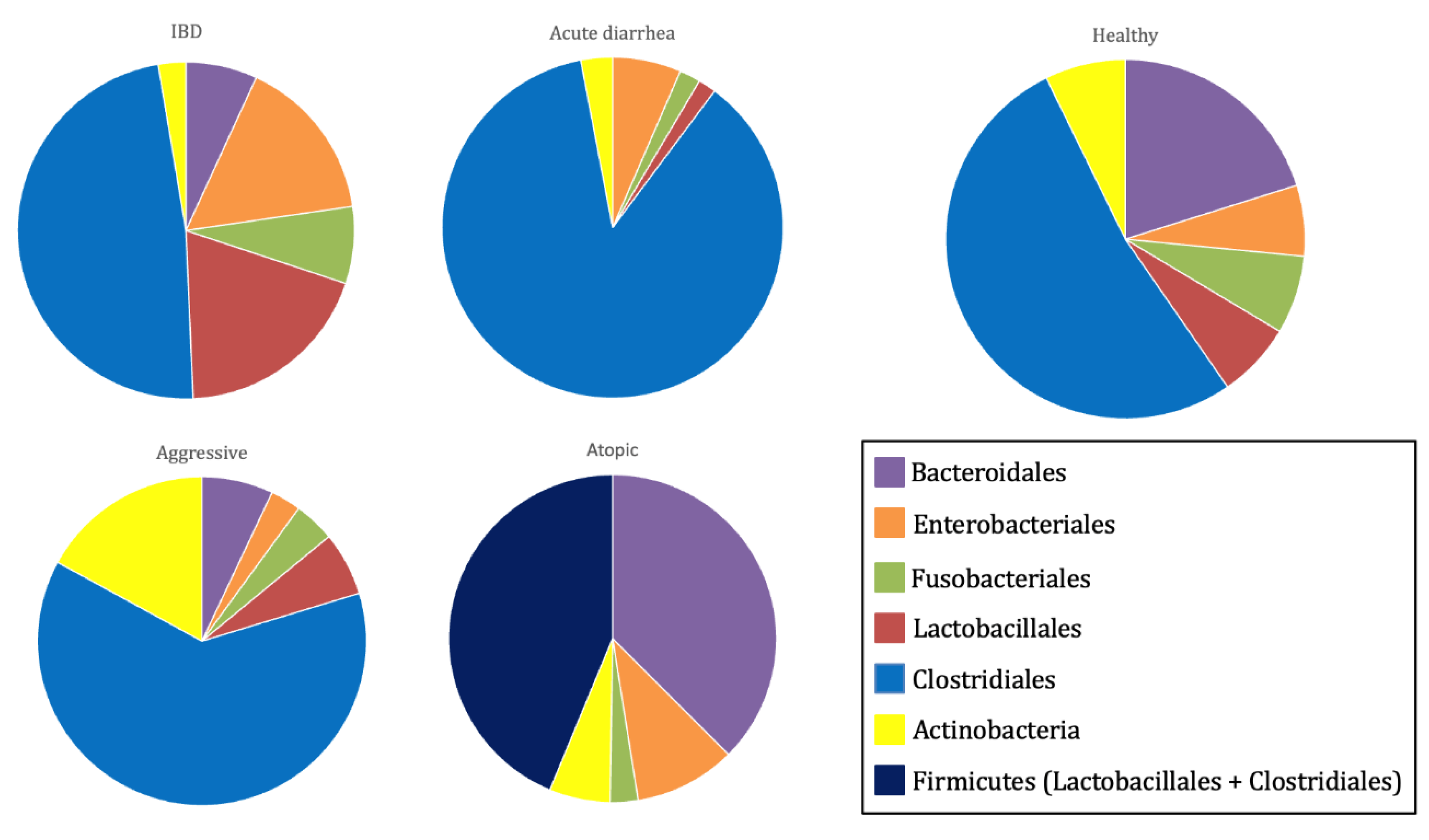
- Suchodolski, J.S.; Markel, M.E.; Garcia-Mazcorro, J.F.; Unterer, S.; Heilmann, R.M.; Dowd, S.E.; Kachroo, P.; Ivanov, I.; Minamoto, Y.; Dillman, E.M.; Steiner, J.M.; Cook, A.K.; Toresson, L. The Fecal Microbiome in Dogs with Acute Diarrhea and Idiopathic Inflammatory Bowel Disease. PLoS ONE 2012, 7(12), e51907. [Google Scholar] [CrossRef]
- Tilg, H.; Zmora, N.; Adolph, T.E.; Elinav, E. The intestinal microbiota fuelling metabolic inflammation. Nat. Rev. Immunol. 2019, 20(1), 40–54. [Google Scholar] [CrossRef]
- Rostaher, A.; Morsy, Y.; Favrot, C.; Unterer, S.; Schnyder, M.; Scharl, M.; Fischer, N.M. Comparison of the Gut Microbiome between Atopic and Healthy Dogs—Preliminary Data. Animals 2022, 12(18), 2377. [Google Scholar] [CrossRef]
- Cintio, M.; Scarsella, E.; Sgorlon, S.; Sandri, M.; Stefanon, B. Gut Microbiome of Healthy and Arthritic Dogs. Vet. Sci. 2020, 7(3), 92. [Google Scholar] [CrossRef]
- Kiełbik, P.; Witkowska-Piłaszewicz, O. The Relationship between Canine Behavioral Disorders and Gut Microbiome and Future Therapeutic Perspectives. Animals 2024, 14(14), 2048. [Google Scholar] [CrossRef]
- Summers, S.; Quimby, J. Insights into the gut-kidney axis and implications for chronic kidney disease management in cats and dogs. Vet. J. 2024, 306, 106181. [Google Scholar] [CrossRef]
- Samuelson, D.R.; Welsh, D.A.; Shellito, J.E. Regulation of lung immunity and host defense by the intestinal microbiota. Front. Microbiol. 2015, 6. [Google Scholar] [CrossRef]
- Chai, J.; Deng, F.; Li, Y.; Wei, X.; Zhao, J. Editorial: The gut-skin axis: interaction of gut microbiome and skin diseases. Front. Microbiol. 2024, 15. [Google Scholar] [CrossRef]
- Bresciani, F.; Minamoto, Y.; Suchodolski, J.S.; Galiazzo, G.; Vecchiato, C.G.; Pinna, C.; Biagi, G.; Pietra, M. Effect of an extruded animal protein-free diet on fecal microbiota of dogs with food-responsive enteropathy. J. Vet. Intern. Med. 2018, 32(6), 1903–1910. [Google Scholar] [CrossRef] [PubMed]
- Bermingham, E.N.; Maclean, P.; Thomas, D.G.; Cave, N.J.; Young, W. Key bacterial families (Clostridiaceae, Erysipelotrichaceae and Bacteroidaceae) are related to the digestion of protein and energy in dogs. PeerJ 2017, 5, e3019. [Google Scholar] [CrossRef] [PubMed]
- Schmidt, M.; Unterer, S.; Suchodolski, J.S.; Honneffer, J.B.; Guard, B.C.; Lidbury, J.A.; Steiner, J.M.; Fritz, J.; Kölle, P. The fecal microbiome and metabolome differs between dogs fed Bones and Raw Food (BARF) diets and dogs fed commercial diets. PLoS ONE 2018, 13(8), e0201279. [Google Scholar] [CrossRef]
- Whittemore, J.C.; Price, J.M.; Moyers, T.; Suchodolski, J.S. Effects of Synbiotics on the Fecal Microbiome and Metabolomic Profiles of Healthy Research Dogs Administered Antibiotics: A Randomized, Controlled Trial. Front. Vet. Sci. 2021, 8. [Google Scholar] [CrossRef]
- Pilla, R.; Gaschen, F.P.; Barr, J.W.; Olson, E.; Honneffer, J.; Guard, B.C.; Blake, A.B.; Villanueva, D.; Khattab, M.R.; AlShawaqfeh, M.K.; Lidbury, J.A.; Steiner, J.M.; Suchodolski, J.S. Effects of metronidazole on the fecal microbiome and metabolome in healthy dogs. J. Vet. Intern. Med. 2020, 34(5), 1853–1866. [Google Scholar] [CrossRef]
- Ziese, A.; Suchodolski, J.S. Impact of Changes in Gastrointestinal Microbiota in Canine and Feline Digestive Diseases. Vet. Clin. North Am. Small Anim. Pract. 2021, 51(1), 155–169. [Google Scholar] [CrossRef]
- Tizard, I.R.; Jones, S.W. The Microbiota Regulates Immunity and Immunologic Diseases in Dogs and Cats. Vet. Clin. North Am. Small Anim. Pract. 2018, 48(2), 307–322. [Google Scholar] [CrossRef]
- Di Cerbo, A.; Morales-Medina, J.C.; Palmieri, B.; Pezzuto, F.; Cocco, R.; Flores, G.; Iannitti, T. Functional foods in pet nutrition: Focus on dogs and cats. Res. Vet. Sci. 2017, 112, 161–166. [Google Scholar] [CrossRef]
- Perini, M.P.; Pedrinelli, V.; Marchi, P.H.; Henríquez, L.B.F.; Zafalon, R.V.A.; Vendramini, T.H.A.; De Carvalho Balieiro, J.C.; Brunetto, M.A. Potential Effects of Prebiotics on Gastrointestinal and Immunological Modulation in the Feeding of Healthy Dogs: A Review. Fermentation 2023, 9(7), 693. [Google Scholar] [CrossRef]
- Moreno, F.J.; Corzo, N.; Montilla, A.; Villamiel, M.; Olano, A. Current state and latest advances in the concept, production and functionality of prebiotic oligosaccharides. Curr. Opin. Food Sci. 2017, 13, 50–55. [Google Scholar] [CrossRef]
- Pinna, C.; Biagi, G. The Utilisation of Prebiotics and Synbiotics in Dogs. Ital. J. Anim. Sci. 2014, 13(1), 3107. [Google Scholar] [CrossRef]
- Sivamaruthi, B.S.; Kesika, P.; Chaiyasut, C. Influence of Probiotic Supplementation on Health Status of the Dogs: A Review. Appl. Sci. 2021, 11(23), 11384. [Google Scholar] [CrossRef]
- Aggeletopoulou, I.; Konstantakis, C.; Assimakopoulos, S.F.; Triantos, C. The role of the gut microbiota in the treatment of inflammatory bowel diseases. Microb. Pathog. 2019, 137, 103774. [Google Scholar] [CrossRef]
- Aguilar-Toalá, J.; Garcia-Varela, R.; Garcia, H.; Mata-Haro, V.; González-Córdova, A.; Vallejo-Cordoba, B.; Hernández-Mendoza, A. Postbiotics: An evolving term within the functional foods field. Trends Food Sci. Technol. 2018, 75, 105–114. [Google Scholar] [CrossRef]
- Salminen, S.; Collado, M.C.; Endo, A.; Hill, C.; Lebeer, S.; Quigley, E.M.M.; Sanders, M.E.; Shamir, R.; Swann, J.R.; Szajewska, H.; Vinderola, G. The International Scientific Association of Probiotics and Prebiotics (ISAPP) consensus statement on the definition and scope of postbiotics. Nat. Rev. Gastroenterol. Hepatol. 2021, 18(9), 649–667. [Google Scholar] [CrossRef]
- Kim, M.; Friesen, L.; Park, J.; Kim, H.M.; Kim, C.H. Microbial metabolites, short-chain fatty acids, restrain tissue bacterial load, chronic inflammation, and associated cancer in the colon of mice. Eur. J. Immunol. 2018, 48(7), 1235–1247. [Google Scholar] [CrossRef]
- Sittipo, P.; Shim, J.; Lee, Y. Microbial Metabolites Determine Host Health and the Status of Some Diseases. Int. J. Mol. Sci. 2019, 20(21), 5296. [Google Scholar] [CrossRef]
- Takagi, R.; Sasaki, K.; Sasaki, D.; Fukuda, I.; Tanaka, K.; Yoshida, K.; Kondo, A.; Osawa, R. A Single-Batch Fermentation System to Simulate Human Colonic Microbiota for High-Throughput Evaluation of Prebiotics. PLoS ONE 2016, 11(8), e0160533. [Google Scholar] [CrossRef]
- Żółkiewicz, J.; Marzec, A.; Ruszczyński, M.; Feleszko, W. Postbiotics—A Step Beyond Pre- and Probiotics. Nutrients 2020, 12(8), 2189. [Google Scholar] [CrossRef]
- Higashi, B.; Mariano, T. B.; De Abreu Filho, B. A.; Gonçalves, R. A. C.; De Oliveira, A. J. B. Effects of fructans and probiotics on the inhibition of Klebsiella oxytoca and the production of short-chain fatty acids assessed by NMR spectroscopy. Carbohydrate Polymers 2020, 248, 116832. [Google Scholar] [CrossRef] [PubMed]
- Lee, C.; Kim, B. G.; Kim, J. H.; Chun, J.; Im, J. P.; Kim, J. S. Sodium butyrate inhibits the NF-kappa B signaling pathway and histone deacetylation, and attenuates experimental colitis in an IL-10 independent manner. International Immunopharmacology 2017, 51, 47–56. [Google Scholar] [CrossRef]
- Gill, P. A.; Van Zelm, M. C.; Muir, J. G.; Gibson, P. R. Review article: short chain fatty acids as potential therapeutic agents in human gastrointestinal and inflammatory disorders. Alimentary Pharmacology & Therapeutics 2018, 48(1), 15-34. [Google Scholar] [CrossRef]
- Zakrzewska, Z.; Zawartka, A.; Schab, M.; Martyniak, A.; Skoczeń, S.; Tomasik, P. J.; Wędrychowicz, A. Prebiotics, Probiotics, and Postbiotics in the Prevention and Treatment of Anemia. Microorganisms 2022, 10(7), 1330. [Google Scholar] [CrossRef]
- Das, N. K.; Schwartz, A. J.; Barthel, G.; Inohara, N.; Liu, Q.; Sankar, A.; Hill, D. R.; Ma, X.; Lamberg, O.; Schnizlein, M. K.; Arqués, J. L.; Spence, J. R.; Nunez, G.; Patterson, A. D.; Sun, D.; Young, V. B.; Shah, Y. M. Microbial Metabolite Signaling Is Required for Systemic Iron Homeostasis. Cell Metabolism 2019, 31(1), 115-130.e6. [CrossRef]
- Aoki, R.; Kamikado, K.; Suda, W.; Takii, H.; Mikami, Y.; Suganuma, N.; Hattori, M.; Koga, Y. A proliferative probiotic Bifidobacterium strain in the gut ameliorates progression of metabolic disorders via microbiota modulation and acetate elevation. Scientific Reports 2017, 7(1). [CrossRef]
- Fukuda, S.; Toh, H.; Taylor, T. D.; Ohno, H.; Hattori, M. Acetate-producing Bifidobacteria protect the host from enteropathogenic infection via carbohydrate transporters. Gut Microbes 2012, 3(5), 449–454. [Google Scholar] [CrossRef] [PubMed]
- Fisher, J. F.; Mobashery, S. Constructing and deconstructing the bacterial cell wall. Protein Science 2019, 29(3), 629–646. [Google Scholar] [CrossRef]
- Saeui, C. T.; Urias, E.; Liu, L.; Mathew, M. P.; Yarema, K. J. Metabolic glycoengineering bacteria for therapeutic, recombinant protein, and metabolite production applications. Glycoconjugate Journal 2015, 32(7), 425–441. [Google Scholar] [CrossRef] [PubMed]
- Kaji, R.; Kiyoshima-Shibata, J.; Nagaoka, M.; Nanno, M.; Shida, K. Bacterial teichoic acids reverse predominant IL-12 production induced by certain Lactobacillus strains into predominant IL-10 production via TLR2-dependent ERK activation in macrophages. The Journal of Immunology 2010, 184(7), 3505–3513. [Google Scholar] [CrossRef]
- Piqué, N.; Berlanga, M.; Miñana-Galbis, D. Health Benefits of Heat-Killed (Tyndallized) Probiotics: An Overview. International Journal of Molecular Sciences 2019, 20(10), 2534. [Google Scholar] [CrossRef]
- Nataraj, B. H.; Ali, S. A.; Behare, P. V.; Yadav, H. Postbiotics-parabiotics: the new horizons in microbial biotherapy and functional foods. Microbial Cell Factories 2020, 19(1). [Google Scholar] [CrossRef]
- Chaisuwan, W.; Jantanasakulwong, K.; Wangtueai, S.; Phimolsiripol, Y.; Chaiyaso, T.; Techapun, C.; Phongthai, S.; You, S.; Regenstein, J. M.; Seesuriyachan, P. Microbial exopolysaccharides for immune enhancement: Fermentation, modifications and bioactivities. Food Bioscience 2020, 35, 100564. [Google Scholar] [CrossRef]
- Gezgi̇Nç, Y.; Karabekmez-Erdem, T.; Tatar, H. D.; Ayman, S.; Gani̇Yusufoğlu, E.; Dayisoylu, K. S. Health promoting benefits of postbiotics produced by lactic acid bacteria: Exopolysaccharide. Biotech Studies 2022, 31(2), 61–70. [Google Scholar] [CrossRef]
- Moradi, M.; Kousheh, S. A.; Almasi, H.; Alizadeh, A.; Guimarães, J. T.; Yılmaz, N.; Lotfi, A. Postbiotics produced by lactic acid bacteria: The next frontier in food safety. Comprehensive Reviews in Food Science and Food Safety 2020, 19(6), 3390–3415. [Google Scholar] [CrossRef]
- Roca, C.; Alves, V. D.; Freitas, F.; Reis, M. A. M. Exopolysaccharides enriched in rare sugars: bacterial sources, production, and applications. Frontiers in Microbiology 2015, 6. [Google Scholar] [CrossRef] [PubMed]
- Singh, P.; Saini, P. Food and Health Potentials of Exopolysaccharides Derived from Lactobacilli. Microbiology Research Journal International 2017, 22(2), 1–14. [Google Scholar] [CrossRef]
- Makino, S.; Sato, A.; Goto, A.; Nakamura, M.; Ogawa, M.; Chiba, Y.; Hemmi, J.; Kano, H.; Takeda, K.; Okumura, K.; Asami, Y. Enhanced natural killer cell activation by exopolysaccharides derived from yogurt fermented with Lactobacillus delbrueckii ssp. bulgaricus OLL1073R-1. Journal of Dairy Science 2016, 99(2), 915–923. [Google Scholar] [CrossRef]
- Wang, J.; Wu, T.; Fang, X.; Min, W.; Yang, Z. Characterization and immunomodulatory activity of an exopolysaccharide produced by Lactobacillus plantarum JLK0142 isolated from fermented dairy tofu. International Journal of Biological Macromolecules 2018, 115, 985–993. [Google Scholar] [CrossRef] [PubMed]
- Li, S.; Shah, N. P. Characterization, Anti-Inflammatory and Antiproliferative Activities of Natural and Sulfonated Exo-Polysaccharides from Streptococcus thermophilus ASCC 1275. Journal of Food Science 2016, 81(5). [Google Scholar] [CrossRef]
- Scarpellini, E.; Rinninella, E.; Basilico, M.; Colomier, E.; Rasetti, C.; Larussa, T.; Santori, P.; Abenavoli, L. From Pre- and Probiotics to Post-Biotics: A Narrative Review. International Journal of Environmental Research and Public Health 2021, 19(1), 37. [Google Scholar] [CrossRef]
- Adebayo-Tayo, B.; Fashogbon, R. In vitro antioxidant, antibacterial, in vivo immunomodulatory, antitumor and hematological potential of exopolysaccharide produced by wild type and mutant Lactobacillus delbrueckii subsp. bulgaricus. Heliyon 2020, 6(2), e03268. [Google Scholar] [CrossRef]
- Yu, Y.; Chen, Z.; Chen, P. T.; Ng, I. Production, characterization and antibacterial activity of exopolysaccharide from a newly isolated Weissella cibaria under sucrose effect. Journal of Bioscience and Bioengineering 2018, 126(6), 769–777. [Google Scholar] [CrossRef]
- Alsaadi, L. G.; Baker, B. A. A.; Kadhem, B. M.; Mahdi, L. H.; Mater, H. N. Exopolysaccharide as antiviral, antimicrobial and as immunostimulants: A review. Plant Archives 2020, 20(2), 5859-5875. eISSN: 2581-6063.
- Khalil, M. A.; Sonbol, F. I.; Al-Madboly, L. A.; Aboshady, T. A.; Alqurashi, A. S.; Ali, S. S. Exploring the Therapeutic Potentials of Exopolysaccharides Derived From Lactic Acid Bacteria and Bifidobacteria: Antioxidant, Antitumor, and Periodontal Regeneration. Frontiers In Microbiology 2022, 13. [Google Scholar] [CrossRef]
- Haase, S.; Haghikia, A.; Wilck, N.; Müller, D. N.; Linker, R. A. Impacts of microbiome metabolites on immune regulation and autoimmunity. Immunology 2018, 154(2), 230–238. [Google Scholar] [CrossRef]
- Montalban-Lopez, M.; Sanchez-Hidalgo, M.; Valdivia, E.; Martinez-Bueno, M.; Maqueda, M. Are Bacteriocins Underexploited? NOVEL Applications for OLD Antimicrobials. Current Pharmaceutical Biotechnology 2011, 12(8), 1205–1220. [Google Scholar] [CrossRef]
- Yang, S.; Lin, C.; Sung, C. T.; Fang, J. Antibacterial activities of bacteriocins: application in foods and pharmaceuticals. Frontiers in Microbiology 2014, 5. [Google Scholar] [CrossRef]
- Mokoena, M. P. Lactic Acid Bacteria and Their Bacteriocins: Classification, Biosynthesis and Applications against Uropathogens: A Mini-Review. Molecules 2017, 22(8), 1255. [Google Scholar] [CrossRef]
- Parada, J.L.; Caron, C.R.; Medeiros, A.B.P.; Soccol, C.R. Bacteriocins from lactic acid bacteria: purification, properties and use as biopreservatives. Braz. Arch. Biol. Technol. 2007, 50, 512–542. [Google Scholar] [CrossRef]
- Darbandi, A.; Asadi, A.; Ari, M.M.; Ohadi, E.; Talebi, M.; Zadeh, M.H.; Emamie, A.D.; Ghanavati, R.; Kakanj, M. Bacteriocins: Properties and potential use as antimicrobials. J. Clin. Lab. Anal. 2021, 36. [Google Scholar] [CrossRef]
- Roces, C.; Rodríguez, A.; Martínez, B. Cell Wall-active Bacteriocins and Their Applications Beyond Antibiotic Activity. Probiotics Antimicrob. Proteins 2012, 4, 259–272. [Google Scholar] [CrossRef] [PubMed]
- Lee, D.; Kim, B.S.; Kang, S. Bacteriocin of Pediococcus acidilactici HW01 Inhibits Biofilm Formation and Virulence Factor Production by Pseudomonas aeruginosa. Probiotics Antimicrob. Proteins 2019, 12, 73–81. [Google Scholar] [CrossRef]
- Ilayajara, R.; Radhamadhavan, P.A.; Nirmala, C.B. Assessment for potential use of bacteriocin producing Lactobacillus fermentum isolated from human milk for preventing urinary tract infections. J. Pharm. Res. 2011, 4, 3445–3447. [Google Scholar]
- Soltani, S.; Hammami, R.; Cotter, P.D.; Rebuffat, S.; Said, L.B.; Gaudreau, H.; Bédard, F.; Biron, E.; Drider, D.; Fliss, I. Bacteriocins as a new generation of antimicrobials: toxicity aspects and regulations. FEMS Microbiol. Rev. 2020, 45. [Google Scholar] [CrossRef]
- Blanco-Blanco, J.; Bravo, M.; Simón, I.; Fernández-Llario, P.; Fajardo-Olivares, M.; Fernández-Calderón, M.C.; Cerrato, R. Synergistic Activity of Ingulados Bacteria with Antibiotics against Multidrug-Resistant Pathogens. Antibiotics 2024, 13, 200. [Google Scholar] [CrossRef]
- Bravo, M.; Combes, T.; Martinez, F.O.; Cerrato, R.; Rey, J.; Garcia-Jimenez, W.; Fernandez-Llario, P.; Risco, D.; Gutierrez-Merino, J. Lactobacilli Isolated From Wild Boar (Sus scrofa) Antagonize Mycobacterium bovis Bacille Calmette-Guerin (BCG) in a Species-Dependent Manner. Front. Microbiol. 2019, 10. [Google Scholar] [CrossRef]
- Hols, P.; Ledesma-García, L.; Gabant, P.; Mignolet, J. Mobilization of Microbiota Commensals and Their Bacteriocins for Therapeutics. Trends Microbiol. 2019, 27, 690–702. [Google Scholar] [CrossRef] [PubMed]
- Mani-López, E.; García, H.; López-Malo, A. Organic acids as antimicrobials to control Salmonella in meat and poultry products. Food Res. Int. 2011, 45, 713–721. [Google Scholar] [CrossRef]
- Homayouni, A.; Aghebati-Maleki, L.; Kafil, H.; Gilani, N.; Abbasi, A.; Khani, N. Postbiotics, as Dynamic Biomolecules, and Their Promising Role in Promoting Food Safety. Biointerface Res. Appl. Chem. 2021, 11, 14529–14544. [Google Scholar] [CrossRef]
- Kareem, K.Y.; Ling, F.H.; Chwen, L.T.; Foong, O.M.; Asmara, S.A. Inhibitory activity of postbiotic produced by strains of Lactobacillus plantarum using reconstituted media supplemented with inulin. Gut Pathog. 2014, 6. [Google Scholar] [CrossRef] [PubMed]
- Hu, C.; Ren, L.; Zhou, Y.; Ye, B. Characterization of antimicrobial activity of three Lactobacillus plantarum strains isolated from Chinese traditional dairy food. Food Sci. Nutr. 2019, 7, 1997–2005. [Google Scholar] [CrossRef]
- Cameotra, S.S.; Makkar, R.S. Biosurfactant-enhanced bioremediation of hydrophobic pollutants. Pure Appl. Chem. 2010, 82, 97–116. [Google Scholar] [CrossRef]
- Rahman, P.K.; Gakpe, E. Production, Characterisation and Applications of Biosurfactants-Review. Biotechnology (Faisalabad) 2008, 7, 360–370. [Google Scholar] [CrossRef]
- Satpute, S.K.; Kulkarni, G.R.; Banpurkar, A.G.; Banat, I.M.; Mone, N.S.; Patil, R.H.; Cameotra, S.S. Biosurfactant/s from Lactobacilli species: Properties, challenges and potential biomedical applications. J. Basic Microbiol. 2016, 56, 1140–1158. [Google Scholar] [CrossRef]
- Aggarwal, S.; Sabharwal, V.; Kaushik, P.; Joshi, A.; Aayushi, A.; Suri, M. Postbiotics: From emerging concept to application. Front. Sustain. Food Syst. 2022, 6. [Google Scholar] [CrossRef]
- Melegy, T.; Khaled, N.F.; El-Bana, R.; Abdellatif, H. Dietary fortification of a natural biosurfactant, lysolecithin in broiler. Afr. J. Agric. Res. 2010, 5, 2886–2892. [Google Scholar] [CrossRef]
- Kullisaar, T.; Zilmer, M.; Mikelsaar, M.; Vihalemm, T.; Annuk, H.; Kairane, C.; Kilk, A. Two antioxidative lactobacilli strains as promising probiotics. Int. J. Food Microbiol. 2002, 72, 215–224. [Google Scholar] [CrossRef]
- Izuddin, W.I.; Humam, A.M.; Loh, T.C.; Foo, H.L.; Samsudin, A.A. Dietary Postbiotic Lactobacillus plantarum Improves Serum and Ruminal Antioxidant Activity and Upregulates Hepatic Antioxidant Enzymes and Ruminal Barrier Function in Post-Weaning Lambs. Antioxidants 2020, 9, 250. [Google Scholar] [CrossRef] [PubMed]
- LeBlanc, J.G.; Del Carmen, S.; Miyoshi, A.; Azevedo, V.; Sesma, F.; Langella, P.; Bermúdez-Humarán, L.G.; Watterlot, L.; Perdigon, G.; De Moreno de LeBlanc, A. Use of superoxide dismutase and catalase producing lactic acid bacteria in TNBS induced Crohn’s disease in mice. J. Biotechnol. 2010, 151, 287–293. [Google Scholar] [CrossRef]
- Tomusiak-Plebanek, A.; Heczko, P.; Skowron, B.; Baranowska, A.; Okoń, K.; Thor, P.J.; Strus, M. Lactobacilli with superoxide dismutase-like or catalase activity are more effective in alleviating inflammation in an inflammatory bowel disease mouse model. Drug Des. Dev. Ther. 2018, 12, 3221–3233. [Google Scholar] [CrossRef]
- Prajapati, N.; Patel, J.; Singh, S.; Yadav, V.K.; Joshi, C.; Patani, A.; Prajapati, D.; Sahoo, D.K.; Patel, A. Postbiotic production: harnessing the power of microbial metabolites for health applications. Front. Microbiol. 2023, 14. [Google Scholar] [CrossRef] [PubMed]
- Thorakkattu, P.; Khanashyam, A.C.; Shah, K.; Babu, K.S.; Mundanat, A.S.; Deliephan, A.; Deokar, G.S.; Santivarangkna, C.; Nirmal, N.P. Postbiotics: Current Trends in Food and Pharmaceutical Industry. Foods 2022, 11, 3094. [Google Scholar] [CrossRef] [PubMed]
- Mohammad, M.A.; Molloy, A.; Scott, J.; Hussein, L. Plasma cobalamin and folate and their metabolic markers methylmalonic acid and total homocysteine among Egyptian children before and after nutritional supplementation with the probiotic bacteria Lactobacillus acidophilus in yoghurt matrix. Int. J. Food Sci. Nutr. 2006, 57, 470–480. [Google Scholar] [CrossRef]
- Liu, Y.; Hou, Y.; Wang, G.; Zheng, X.; Hao, H. Gut Microbial Metabolites of Aromatic Amino Acids as Signals in Host–Microbe Interplay. Trends Endocrinol. Metab. 2020, 31, 818–834. [Google Scholar] [CrossRef]
- Devlin, A.S.; Marcobal, A.; Dodd, D.; Nayfach, S.; Plummer, N.; Meyer, T.; Pollard, K.S.; Sonnenburg, J.L.; Fischbach, M.A. Modulation of a Circulating Uremic Solute via Rational Genetic Manipulation of the Gut Microbiota. Cell Host Microbe 2016, 20, 709–715. [Google Scholar] [CrossRef]
- Xia, B.; Shi, X.C.; Xie, B.C.; Zhu, M.Q.; Chen, Y.; Chu, X.Y.; Cai, G.H.; Liu, M.; Yang, S.Z.; Mitchell, G.A.; Pang, W.J.; Wu, J.W. Urolithin A exerts antiobesity effects through enhancing adipose tissue thermogenesis in mice. PLoS Biol. 2020, 18, e3000688. [Google Scholar] [CrossRef]
- Andreux, P.A.; Blanco-Bose, W.; Ryu, D.; Burdet, F.; Ibberson, M.; Aebischer, P.; Auwerx, J.; Singh, A.; Rinsch, C. The mitophagy activator urolithin A is safe and induces a molecular signature of improved mitochondrial and cellular health in humans. Nat. Metab. 2019, 1, 595–603. [Google Scholar] [CrossRef] [PubMed]
- Tousen, Y.; Ezaki, J.; Fujii, Y.; Ueno, T.; Nishimuta, M.; Ishimi, Y. Natural S-equol decreases bone resorption in postmenopausal, non-equol-producing Japanese women. Menopause 2011, 18, 563–574. [Google Scholar] [CrossRef]
- Patterson, E.; Cryan, J. F.; Fitzgerald, G. F.; Ross, R. P.; Dinan, T. G.; Stanton, C. Gut microbiota, the pharmabiotics they produce and host health. Proceedings Of The Nutrition Society 2014, 73, 477–489. [Google Scholar] [CrossRef]
- Wenninger, J.; Meinitzer, A.; Holasek, S.; Schnedl, W. J.; Zelzer, S.; Mangge, H.; Herrmann, M.; Enko, D. Associations between tryptophan and iron metabolism observed in individuals with and without iron deficiency. Scientific Reports 2019, 9(1). [Google Scholar] [CrossRef]
- Day, M. Ageing, Immunosenescence and Inflammageing in the Dog and Cat. Journal Of Comparative Pathology 2010, 142, S60–S69. [Google Scholar] [CrossRef] [PubMed]
- Wambacq, W. A.; Apper, E.; Le Bourgot, C.; Barbe, F.; Lyu, Y.; Pelst, M. P.; Broeckx, B.; Devriendt, B.; Cox, E.; Hesta, M. A new combination of a pre-and postbiotic mitigates immunosenescence in vaccinated healthy senior dogs. Frontiers In Veterinary Sciences 2024, 11. [Google Scholar] [CrossRef]
- Lin, C.; Alexander, C.; Steelman, A. J.; Warzecha, C. M.; De Godoy, M. R. C.; Swanson, K. S. Effects of a Saccharomyces cerevisiae fermentation product on fecal characteristics, nutrient digestibility, fecal fermentative end-products, fecal microbial populations, immune function, and diet palatability in adult dogs. Journal Of Animal Science 2019, 97(4), 1586–1599. [Google Scholar] [CrossRef]
- Timlin, C. L.; Mccracken, F. B.; Dickerson, S. M.; Skaggs, P. M.; Fowler, J. W.; Jalukar, S.; Coon, C. N. Effects of a Saccharomyces cerevisiae-Derived Postbiotic in Adult Labrador Retrievers Undergoing Exercise and Transport Stress. Pets 2024, 1(3), 350–371. [Google Scholar] [CrossRef]
- Tate, D. E.; Tanprasertsuk, J.; Jones, R. B.; Maughan, H.; Chakrabarti, A.; Khafipour, E.; Norton, S. A.; Shmalberg, J.; Honaker, R. W. A Randomized Controlled Trial to Evaluate the Impact of a Novel Probiotic and Nutraceutical Supplement on Pruritic Dermatitis and the Gut Microbiota in Privately Owned Dogs. Animals 2024, 14(3), 453. [Google Scholar] [CrossRef]
- Wilson, S. M.; Oba, P. M.; Koziol, S. A.; Applegate, C. C.; Soto-Diaz, K.; Steelman, A. J.; Panasevich, M. R.; Norton, S. A.; Swanson, K. S. Effects of a Saccharomyces cerevisiae fermentation product-supplemented diet on circulating immune cells and oxidative stress markers of dogs. Journal Of Animal Science 2022, 100(9). [Google Scholar] [CrossRef]
- Xuan, C.; Shan, L.; Ying, W.; Ming-Ke, F.; Ya-Zhen, Y. Effect of postbiotic supplementation on fecal characteristics, serum biochemical indexes, and fecal flora of dogs. Feed Research 2024, 47(1), 131. [Google Scholar] [CrossRef]
- Belà, B.; Coman, M. M.; Verdenelli, M. C.; Gramenzi, A.; Pignataro, G.; Fiorini, D.; Silvi, S. In Vitro Assessment of Postbiotic and Probiotic Commercial Dietary Supplements Recommended for Counteracting Intestinal Dysbiosis in Dogs. Veterinary Sciences 2024, 11(1), 19. [Google Scholar] [CrossRef]
- Belà, B.; Crisi, P. E.; Pignataro, G.; Fusaro, I.; Gramenzi, A. Effects of a Nutraceutical Treatment on the Intestinal Microbiota of Sled Dogs. Animals 2024, 14(15), 2226. [Google Scholar] [CrossRef] [PubMed]
- Oba, P. M.; Carroll, M. Q.; Sieja, K. M.; De Souza Nogueira, J. P.; Yang, X.; Epp, T. Y.; Warzecha, C. M.; Varney, J. L.; Fowler, J. W.; Coon, C. N.; Swanson, K. S. Effects of a Saccharomyces cerevisiae fermentation product on fecal characteristics, metabolite concentrations, and microbiota populations of dogs subjected to exercise challenge. Journal Of Animal Science 2022, 101. [Google Scholar] [CrossRef] [PubMed]
- Koziol, S. A.; Oba, P. M.; Soto-Diaz, K.; Steelman, A. J.; Suchodolski, J. S.; Eckhardt, E. R. M.; Swanson, K. S. Effects of a Lactobacillus fermentation product on the fecal characteristics, fecal microbial populations, immune function, and stress markers of adult dogs. Journal Of Animal Science 2023, 101. [Google Scholar] [CrossRef]
- Kayser, E.; He, F.; Davenport, G. M.; De Godoy, M. R. Functional Properties of Bifidobacterium Animalis Subsp. Lactis Cect 8145 in Canine Nutrition. Journal Of Animal Science 2022, 100(Supplement_3), 55–56. [Google Scholar] [CrossRef]
- Kayser, E.; He, F.; Nixon, S.; Howard-Varona, A.; Lamelas, A.; Martinez-Blanch, J.; Chenoll, E.; Davenport, G. M.; De Godoy, M. R. C. Effects of Supplementation of Live and Heat-treated Bifidobacterium animalis subspecies lactis CECT 8145 on Glycemic and Insulinemic Response, Fecal Microbiota, Systemic Biomarkers of Inflammation, and White Blood Cell Gene Expression of Adult Dogs. Journal Of Animal Science 2024. [CrossRef] [PubMed]
- Panasevich, M. R.; Daristotle, L.; Quesnell, R.; Reinhart, G. A.; Frantz, N. Z. Altered fecal microbiota, IgA, and fermentative end-products in adult dogs fed prebiotics and a nonviable Lactobacillus acidophilus. Journal Of Animal Science 2021, 99(12). [Google Scholar] [CrossRef]
- Kilburn, L. R.; Allenspach, K.; Jergens, A. E.; Bourgois-Mochel, A.; Mochel, J. P.; Serao, M. C. R. Apparent total tract digestibility, fecal characteristics, and blood parameters of healthy adult dogs fed high-fat diets. Journal Of Animal Science 2020, 98(3). [Google Scholar] [CrossRef]
- Chaitman, J.; Ziese, A.; Pilla, R.; Minamoto, Y.; Blake, A. B.; Guard, B. C.; Isaiah, A.; Lidbury, J. A.; Steiner, J. M.; Unterer, S.; Suchodolski, J. S. Fecal Microbial and Metabolic Profiles in Dogs With Acute Diarrhea Receiving Either Fecal Microbiota Transplantation or Oral Metronidazole. Frontiers In Veterinary Science 2020, 7. [Google Scholar] [CrossRef]
- Rolfe, V. E.; Adams, C. A.; Butterwick, R. E.; Batt, R. M. Relationships between fecal consistency and colonic microstructure and absorptive function in dogs with and without nonspecific dietary sensitivity. American Journal Of Veterinary Research 2002, 63(4), 617–622. [Google Scholar] [CrossRef]
- Von Engelhardt, W.; Rönnau, K.; Rechkemmer, G.; Sakata, T. Absorption of short-chain fatty acids and their role in the hindgut of monogastric animals. Animal Feed Science And Technology 1989, 23(1-3), 43–53. [Google Scholar] [CrossRef]
- Rafique, N.; Jan, S. Y.; Dar, A. H.; Dash, K. K.; Sarkar, A.; Shams, R.; Pandey, V. K.; Khan, S. A.; Amin, Q. A.; Hussain, S. Z. Promising bioactivities of postbiotics: A comprehensive review. Journal Of Agriculture And Food Research 2023, 14, 100708. [Google Scholar] [CrossRef]
- Wegh, N.; Geerlings, N.; Knol, N.; Roeselers, N.; Belzer, N. Postbiotics and Their Potential Applications in Early Life Nutrition and Beyond. International Journal Of Molecular Sciences 2019, 20(19), 4673. [Google Scholar] [CrossRef]
- Lee, J. Y.; Kim, Y.; Kim, J.; Lee, H.; Moon, G.; Kang, C. Improvements in Human Keratinocytes and Antimicrobial Effect Mediated by Cell-Free Supernatants Derived from Probiotics. Fermentation 2022, 8(7), 332. [Google Scholar] [CrossRef]
- Moradi, M.; Molaei, R.; Guimarães, J. T. A review on preparation and chemical analysis of postbiotics from lactic acid bacteria. Enzyme And Microbial Technology 2020, 143, 109722. [Google Scholar] [CrossRef]
- Cuevas-González, P.; Liceaga, A.; Aguilar-Toalá, J. Postbiotics and paraprobiotics: From concepts to applications. Food Research International 2020, 136, 109502. [Google Scholar] [CrossRef] [PubMed]
- Foo, H. L.; Loh, T. C.; Mutalib, N. E. A.; Rahim, R. A. The Myth and Therapeutic Potentials of Postbiotics. Elsevier eBooks 2019, 201–211. [Google Scholar] [CrossRef]
- Blazheva, D.; Mihaylova, D.; Averina, O. V.; Slavchev, A.; Brazkova, M.; Poluektova, E. U.; Danilenko, V. N.; Krastanov, A. Antioxidant Potential of Probiotics and Postbiotics: A Biotechnological Approach to Improving Their Stability. Russian Journal Of Genetics 2022, 58(9), 1036–1050. [Google Scholar] [CrossRef]
- Neut, C.; Mahieux, S.; Dubreuil, L. Antibiotic susceptibility of probiotic strains: Is it reasonable to combine probiotics with antibiotics? Médecine Et Maladies Infectieuses 2017, 47(7), 477–483. [Google Scholar] [CrossRef]
- Tóth, A. G.; Csabai, I.; Judge, M. F.; Maróti, G.; Becsei, Á.; Spisák, S.; Solymosi, N. Mobile Antimicrobial Resistance Genes in Probiotics. Antibiotics 2021, 10(11), 1287. [Google Scholar] [CrossRef]
- Kim, H.; Rather, I. A.; Kim, H.; Kim, S.; Kim, T.; Jang, J.; Seo, J.; Lim, J.; Park, Y. A Double-Blind, Placebo Controlled-Trial of a Probiotic Strain Lactobacillus sakei Probio-65 for the Prevention of Canine Atopic Dermatitis. Journal Of Microbiology And Biotechnology 2015, 25(11), 1966–1969. [Google Scholar] [CrossRef]
| Postbiotic-producing microorganism | Type of postbiotics | Effect | References |
|---|---|---|---|
| Limosilactobacillus reuteri NBF 1 | Fermentation ptoducts | Modulate the composition of the intestinal microbiota. | Belà et al., 2024 [110] |
| Modulate and reduce changes in the intestinal microbiota of dogs under stress. | Belà et al., 2024 [111] | ||
| Limosilactobacillus fermentum and Lactobacillus delbrueckii | Fermentation ptoducts | Modulate and reduce changes in the intestinal microbiota of dogs under stress. Antioxidant action by increasing serum superoxide dismutase levels in stressed dogs. Fewer changes in serum levels of corticoid isoenzymes of alkaline phosphatase and alanine aminotransferase in stressed dogs. |
Koziol et al., 2023 [113] |
| Bifidobacterium animalis subsp. lactis CECT 8145 | Fermentation ptoducts | Reduction of intestinal pH in healthy dogs. Reduction in plasma levels of pancreatic polypeptide. |
Kayser et al., 2022 [114] |
| Inactivated bacteria | Reduction of pH and increase in propionate concentration in the feces of healthy dogs. | Kayser et al., 2024 [115] | |
| Lactobacillus acidophilus | Inactivated bacteria | Increase in fecal IgA concentration in healthy dogs. | Panasevich et al., 2021 [116] |
| - | - | Reduction in the production of pro-inflammatory cytokines. Reduction of serum triglyceride, cholesterol, and uric acid levels. |
Xuan et al., 2024 [109] |
| Saccharomyces cerevisiae | Short-chain fructooligosaccharides | Modulate the immune system and prevent immunosenescence in geriatric dogs. | Wambacq et al., 2024 [104] |
| Saccharomyces cerevisiae | Fermentation ptoducts | Increase leukocyte count and modulate the immune system. Modulate and reduce changes in the intestinal microbiota of dogs under stress. |
Lin et al., 2019 [105] |
| Modulate and prevent immune system changes under stress. Increase production of anti-inflammatory cytokines and decrease pro-inflammatory cytokines in stressed dogs. Modulate and reduce changes in the intestinal microbiota of dogs under stress. |
Timlin et al., 2024 [106] | ||
| Decrease the severity of lesions produced by atopic dermatitis (PVAS10 and OA-SASI indices). Modulate and reduce changes in the intestinal microbiota of dogs with atopic dermatitis. |
Tate et al., 2024 [107] | ||
| Control immune response, transepidermal water loss, and sebum concentration in dogs with atopic dermatitis. Antioxidant action by increasing serum superoxide dismutase and catalase levels. |
Wilson et al., 2022 [108] | ||
| Modulate and reduce changes in the intestinal microbiota of dogs under stress. | Oba et al., 2022 [112] |
| Meta-analysis parameter | Analyzed studies |
|---|---|
| Fecal score | Lin et al., 2019 [105] Oba et al., 2022 [112] Panasevich et al., 2021 [116] |
| Fecal pH | Lin et al., 2019 [105] Oba et al., 2022 [112] Kayser et al., 2024 [115] Panasevich et al., 2021 [116] |
| Fecal acetate concentration | |
| Fecal propionate concentration | |
| Fecal butyrate concentration | |
| Fecal isobutyrate concentration | |
| Fecal isovalerate concentration | |
| Fecal valerate concentration | |
| Fecal phenol concentration | |
| Fecal indole concentration | |
| Shannon index | Tate et al., 2024 [107] Oba et al., 2022 [112] Koziol et al., 2023 [113] |
| Richness | Lin et al., 2019 [105] Tate et al., 2024 [107] Koziol et al., 2023 [113] Oba et al., 2022 [112] Panasevich et al., 2021 [116] |
| Abundance of major bacterial phyla (Fusobacteria, Firmicutes, Actinobacteria, Bacteroidetes, and Proteobacteria) | Lin et al., 2019 [105] Tate et al., 2024 [107] Oba et al., 2022 [112] Panasevich et al., 2021 [116] |
| Parameter | Group | Mean value | Q-test | p | Fail-Safe N | p | Begg and Mazumdar Rank Correlation | p | Egger's Regression | p |
|---|---|---|---|---|---|---|---|---|---|---|
| Fecal score | Control | 3.13 | 0.0004 | 0.9998 | 0.000 | 0.419 | -1.000 | 0.333 | -0.019 | 0.985 |
| Supplemented | 3.17 | 0.0003 | 0.9999 | 0.000 | 0.418 | -1.000 | 0.333 | -0.015 | 0.988 | |
| pH | Control | 6.29 | 0.0007 | 1.000 | 0.000 | 0.324 | 0.183 | 0.718 | 0.013 | 0.990 |
| Supplemented | 6.32 | 0.0008 | 1.000 | 0.000 | 0.324 | -0.183 | 0.718 | 0.001 | 0.999 | |
| Acetate1 | Control | 311 | 1.0220 | 0.7959 | 4.000 | 0.013 | 0.183 | 0.718 | -0.082 | 0.935 |
| Supplemented | 313 | 0.9112 | 0.8227 | 4.000 | 0.012 | -0.183 | 0.718 | -0.073 | 0.942 | |
| Propionate1 | Control | 160 | 0.2018 | 0.9773 | 0.000 | 0.128 | -0.183 | 0.718 | -0.125 | 0.901 |
| Supplemented | 167 | 0.1839 | 0.9801 | 0.000 | 0.117 | -0.183 | 0.718 | -0.114 | 0.910 | |
| Butyrate1 | Control | 61.05 | 3.1650 | 0.3669 | 25.000 | < 0.001 | 0.183 | 0.718 | -0.204 | 0.839 |
| Supplemented | 70.65 | 5.1391 | 0.1619 | 35.000 | < 0.001 | 0.183 | 0.718 | 0.378 | 0.705 | |
| Isobutyrate1 | Control | 5.75 | 0.0082 | 0.9998 | 0.000 | 0.333 | 0.913 | 0.071 | 0.085 | 0.932 |
| Supplemented | 5.80 | 0.0079 | 0.9998 | 0.000 | 0.333 | 0.548 | 0.279 | 0.076 | 0.940 | |
| Isovalerate1 | Control | 8.67 | 0.0169 | 0.9994 | 0.000 | 0.258 | 0.913 | 0.071 | 0.122 | 0.903 |
| Supplemented | 8.93 | 0.0189 | 0.9993 | 0.000 | 0.253 | 0.548 | 0.279 | 0.103 | 0.918 | |
| Valerate1 | Control | 3.14 | 0.0593 | 0.9962 | 0.000 | 0.401 | 0.548 | 0.279 | 0.133 | 0.895 |
| Supplemented | 4.51 | 0.1052 | 0.9912 | 0.000 | 0.362 | 0.548 | 0.279 | 0.159 | 0.874 | |
| Phenol1 | Control | 1.58 | 0.0226 | 0.9991 | 0.000 | 0.448 | 0.913 | 0.071 | 0.094 | 0.925 |
| Supplemented | 1.41 | 0.0182 | 0.9994 | 0.000 | 0.454 | 0.913 | 0.071 | 0.075 | 0.941 | |
| Indole1 | Control | 1.49 | 0.0009 | 1.0000 | 0.000 | 0.455 | 0.913 | 0.071 | 0.030 | 0.976 |
| Supplemented | 1.42 | 0.0006 | 1.000 | 0.000 | 0.458 | 0.913 | 0.071 | 0.024 | 0.981 |
| Parameter | Estimated effect | p | Q-test | p | Fail-Safe N | p | Begg and Mazumdar Rank Correlation | p | Egger's Regression | p |
|---|---|---|---|---|---|---|---|---|---|---|
| Fecal score | 0.0946 | 0.624 | 1.064 | 0.587 | 0.000 | 0.268 | 1.000 | 0.333 | 0.954 | 0.340 |
| pH | -0.1052 | 0.621 | 4.647 | 0.200 | 0.000 | 0.242 | -1.000 | 0.083 | -1.606 | 0.108 |
| Acetate | 0.1287 | 0.463 | 3.178 | 0.365 | 0.000 | 0.213 | 0.333 | 0.750 | 0.434 | 0.664 |
| Propionate | 0.2802 | 0.276 | 6.086 | 0.107 | 0.000 | 0.058 | 0.333 | 0.750 | 1.005 | 0.315 |
| Butyrate | 0.8601 | 0.361 | 32.035 | < 0.001 | 6.000 | 0.007 | 0.667 | 0.333 | 5.089 | < 0.001 |
| Isobutyrate | 0.0302 | 0.862 | 0.221 | 0.974 | 0.000 | 0.445 | -0.667 | 0.333 | -0.235 | 0.814 |
| Isovalerate | 0.1017 | 0.560 | 0.684 | 0.877 | 0.000 | 0.296 | 0.000 | 1.000 | -0.276 | 0.782 |
| Valerate | 0.3887 | 0.124 | 5.863 | 0.118 | 3.000 | 0.015 | 0.667 | 0.333 | 1.357 | 0.175 |
| Phenol | -0.1400 | 0.424 | 2.326 | 0.508 | 0.000 | 0.158 | -1.000 | 0.083 | -1.377 | 0.168 |
| Indole | -0.1381 | 0.429 | 1.414 | 0.702 | 0.000 | 0.182 | -0.667 | 0.333 | -0.822 | 0.411 |
| Parameter | Group | Mean value | Q-test | p | Fail-Safe N | p | Begg and Mazumdar Rank Correlation | p | Egger's Regression | p |
|---|---|---|---|---|---|---|---|---|---|---|
| Richness | Control | 142 | 0.1282 | 0.9980 | 0.000 | 0.110 | -0.200 | 0.817 | 0.003 | 0.998 |
| Supplemented | 139 | 0.0861 | 0.9991 | 0.000 | 0.107 | 0.000 | 1.000 | 0.058 | 0.954 | |
| Shannon index | Control | 4.06 | 0.0030 | 0.9985 | 0.000 | 0.389 | 0.333 | 1.000 | 0.039 | 0.969 |
| Supplemented | 4.11 | 0.0047 | 0.9977 | 0.000 | 0.382 | 0.333 | 1.000 | 0.062 | 0.951 | |
| Fusobacteria2 | Control | 23.10 | 0.3484 | 0.9507 | 2.000 | 0.028 | 0.000 | 1.000 | 0.446 | 0.656 |
| Supplemented | 20.52 | 0.1548 | 0.9845 | 1.000 | 0.042 | 0.333 | 0.750 | 0.309 | 0.758 | |
| Firmicutes2 | Control | 61.31 | 1.3877 | 0.7084 | 29.000 | < 0.001 | -1.000 | 0.083 | -1.149 | 0.251 |
| Supplemented | 63.21 | 1.0321 | 0.7935 | 34.000 | < 0.001 | -0.667 | 0.333 | -0.941 | 0.346 | |
| Actinobacteria2 | Control | 1.59 | 0.0019 | 1.0000 | 0.000 | 0.451 | -0.333 | 0.750 | -0.016 | 0.987 |
| Supplemented | 3.35 | 0.0302 | 0.9986 | 0.000 | 0.387 | 0.667 | 0.333 | 0.072 | 0.943 | |
| Bacteroidetes2 | Control | 16.75 | 0.2647 | 0.9665 | 0.000 | 0.080 | 1.000 | 0.083 | 0.446 | 0.656 |
| Supplemented | 17.14 | 0.2467 | 0.9697 | 0.000 | 0.072 | 0.333 | 0.750 | 0.358 | 0.720 | |
| Proteobacteria2 | Control | 5.43 | 0.0092 | 0.9998 | 0.000 | 0.328 | 1.000 | 0.083 | 0.093 | 0.926 |
| Supplemented | 5.50 | 0.0082 | 0.9998 | 0.000 | 0.322 | 0.333 | 0.750 | 0.074 | 0.941 |
| Parameter | Estimated effect | p | Q-test | p | Fail-Safe N | p | Begg and Mazumdar Rank Correlation | p | Egger's Regression | p |
|---|---|---|---|---|---|---|---|---|---|---|
| Richness | -0.0900 | 0.539 | 2.631 | 0.621 | 0.000 | 0.313 | 0.400 | 0.483 | 0.909 | 0.363 |
| Shannon index | 0.0254 | 0.892 | 1.242 | 0.537 | 0.000 | 0.400 | 1.000 | 0.333 | 1.114 | 0.265 |
| Fusobacteria | -0.1476 | 0.355 | 0.413 | 0.938 | 0.000 | 0.178 | 0.000 | 1.000 | -0.062 | 0.951 |
| Firmicutes | 0.0571 | 0.720 | 0.274 | 0.965 | 0.000 | 0.347 | 0.333 | 0.750 | 0.285 | 0.775 |
| Actinobacteria | 0.1150 | 0.471 | 0.513 | 0.916 | 0.000 | 0.251 | -0.333 | 0.750 | -0.313 | 0.755 |
| Bacteroidetes | 0.0574 | 0.719 | 0.146 | 0.986 | 0.000 | 0.377 | -0.333 | 0.750 | -0.314 | 0.754 |
| Proteobacteria | 0.0360 | 0.821 | 0.653 | 0.884 | 0.000 | 0.431 | -0.333 | 0.750 | -0.359 | 0.720 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




