Submitted:
17 February 2025
Posted:
18 February 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Patient inclusion and exclusion criteria
2.2. Comprehensive clinical evaluation
- Physical activity level: to avoid classification as sedentary, participants were required to engage in a minimum of 150 minutes of moderate to vigorous physical activity per week, or at least 30 minutes of such activity daily, in addition to basal activity levels.
- Sleep duration: a nightly sleep duration of fewer than 7 hours was categorized as sleep deprivation, consistent with established guidelines [85].
- Alcohol consumption: participants self-reported their alcohol intake, specifying the number of alcohol units consumed. One unit was defined as equivalent to 10 mL of pure ethanol, with two units corresponding to a pint or can of beer, one unit representing a 25 mL shot of distilled spirits, and one unit equating to a standard 175 mL glass of wine. Participants who consumed more than two units of alcohol per day were classified as "alcoholic," whereas those who abstained completely from alcohol were categorized as "non-alcoholic" [86].
- Smoking status: to ensure comprehensive categorization within the evaluation of the QRISK3 score, participants were classified into the following groups: non-smoker, ex-smoker, light smoker (fewer than 10 cigarettes per day), moderate smoker (10-19 cigarettes per day), and heavy smoker (20 or more cigarettes per day).
- Height measurement: Participant height was measured using a calibrated, wall-mounted stadiometer. Each individual was instructed to stand upright, barefoot, with their heels together and back straight, ensuring accurate vertical alignment for precise measurement.
- Body weight measurement: Body weight at the time of presentation was recorded using a certified mechanical scale with a maximum capacity of 180 kg. Each participant was instructed on the procedure, which involved standing upright on the scale with minimal clothing and no footwear to ensure consistent and accurate results.
- Circumference measurements: Waist circumference was measured at the midpoint between the lower edge of the last palpable rib and the uppermost point of the iliac crest, while hip circumference was measured at the widest portion of the buttocks. These measurements were performed using a non-elastic, calibrated measuring tape positioned parallel to the floor, adhering to standardized anthropometric protocols.
- Waist-to-hip ratio measurement: After determining the waist circumference, the hip circumference was subsequently measured. It was measured at the widest part of the buttocks, ensuring the tape remained parallel to the floor. WHR was then calculated as waist circumference (cm) divided by hip circumference (cm). This standardized method ensured consistency and minimized measurement error across participants.
2.3. QRISK3 Score calculation and cardiovascular risk assessment
- Age (years)
- Sex (male/female)
- Ethnicity
- Body mass index (BMI) (kg/m²)
- Systolic blood pressure (mmHg)
- Total cholesterol to high-density lipoprotein cholesterol (TC/HDL) ratio
- Smoking status (non-smoker, ex-smoker, light smoker <10 cigarettes/day, moderate smoker 10-19 cigarettes/day, heavy smoker ≥20 cigarettes/day)
- Diagnosis of hypertension
- Diagnosis of type 2 diabetes mellitus
- Diagnosis of chronic kidney disease (stages 3, 4, or 5)
- Diagnosis of rheumatoid arthritis
- Diagnosis of systemic lupus erythematosus
- History of atrial fibrillation
- History of migraine
- Diagnosis of severe mental illness (e.g., schizophrenia, bipolar disorder, major depression)
- Use of atypical antipsychotic medication
- Regular corticosteroid therapy
- Presence of erectile dysfunction (in male participants)
- Family history of premature cardiovascular disease (angina or myocardial infarction before the age of 60 in a first-degree relative) [89].
2.4. Segmental body composition assessment using bioelectrical impedance analysis
2.5. Clinical weight management intervention
2.6. Statistical analysis
3. Results
3.1. Baseline characteristics of participants across dietary groups
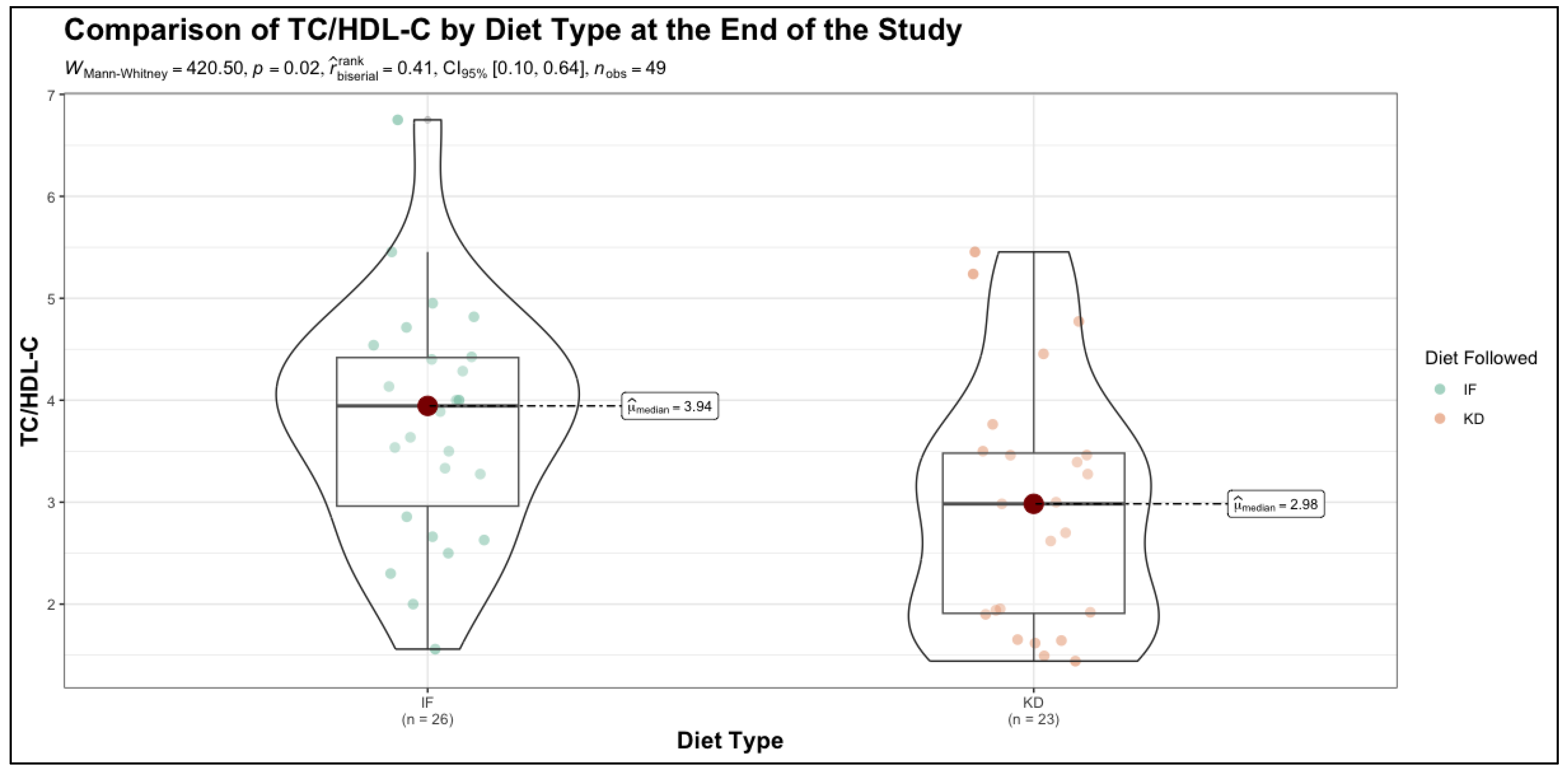
3.2. Post-Intervention Outcomes and Comparative Analysis Between Diets
3.3. Longitudinal Analysis of Health Markers Within Dietary Groups
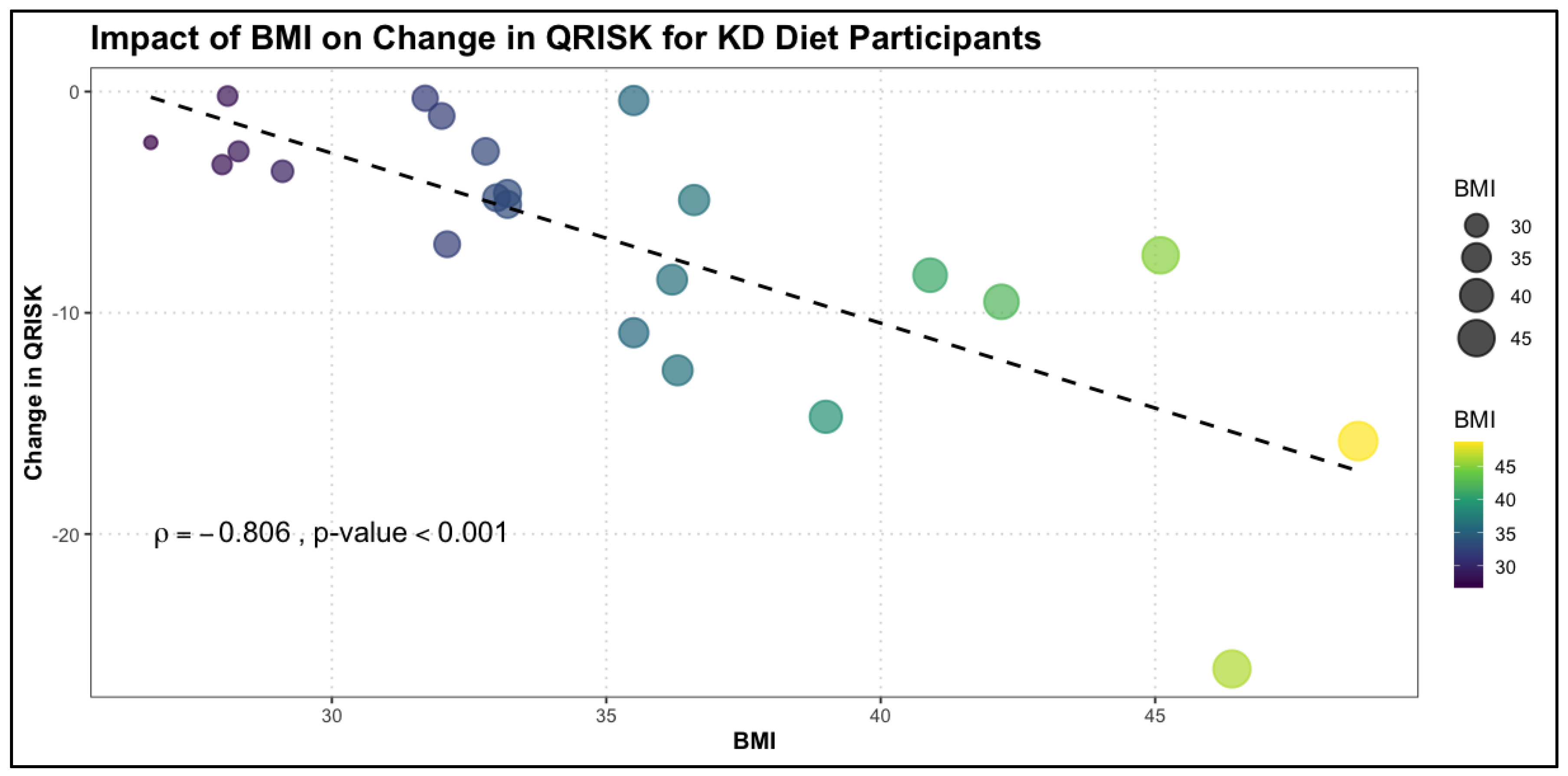
3.4. Correlations between change in QRISK and health markers stratified by diet type
3.5. Predictors of final cardiovascular risk
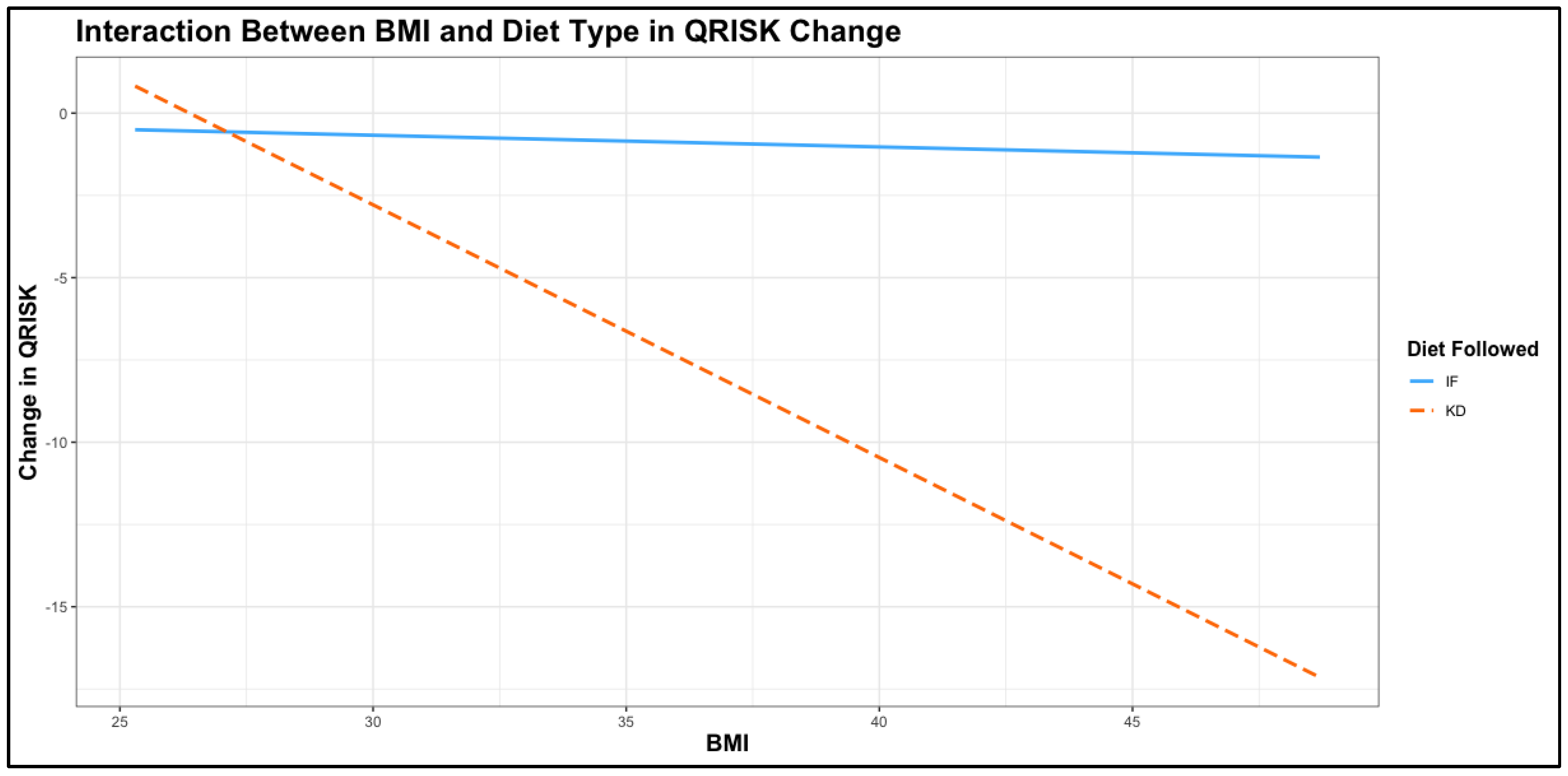
3.6. Exploring interaction effects between predictors and diet type on cardiovascular Risk reduction
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Acknowledgments
Conflicts of Interest
Abbreviations
References
- Wang Y, Lim H. The global childhood obesity epidemic and the association between socio-economic status and childhood obesity. Int Rev Psychiatry. 2022;34(5):502-516. [CrossRef]
- Baumeister SE, Leitzmann MF. Sedentary behavior and the risk of obesity and type 2 diabetes. Diabetol Metab Syndr. 2020;12:13. [CrossRef]
- NCD Risk Factor Collaboration (NCD-RisC). Rising trends in obesity across the globe: analysis and strategies. Lancet. 2022;400(10356):1345-1355. [CrossRef]
- Swinburn BA, Kraak VI, Allender S, et al. The Global Syndemic of Obesity, Undernutrition, and Climate Change: The Lancet Commission report. Lancet. 2019;393(10173):791-846. [CrossRef]
- World Obesity Federation. World Obesity Atlas 2022. London: World Obesity Federation; 2022. Available at: https://www.worldobesity.org/resources/resource-library/world-obesity-atlas-2022. Accessed January 27, 2025.
- Stewart, C. Obesity in Europe [Internet]. Statista; Available from: https://www.statista.com/topics/9419/obesity-in-europe/.
- Hubert HB, Feinleib M, McNamara PM, Castelli WP. Obesity as an independent risk factor for cardiovascular disease: a 26-year follow-up of participants in the Framingham Heart Study. Circulation. 1983;67:968-77.
- Kusminski CM, Perez-Tilve D, Müller TD, DiMarchi RD, Tschöp MH, Scherer PE. Transforming obesity: The advancement of multi-receptor drugs. Cell. 2024;187(15):3829-3853. [CrossRef] [PubMed] [PubMed Central]
- Bruning JC, Fenselau H. Integrative neurocircuits that control metabolism and food intake. Science. 2023;381:eabl7398. [CrossRef]
- Müller TD, Blüher M, Tschöp MH, DiMarchi RD. Anti-obesity drug discovery: advances and challenges. Nat Rev Drug Discov. 2022;21(3):201-223. [CrossRef] [PubMed] [PubMed Central]
- Woolf EK, Cabre HE, Niclou AN, et al. Body Weight Regulation. [Updated 2024 Jun 13]. In: Feingold KR, Anawalt B, Blackman MR, et al., editors. Endotext [Internet]. South Dartmouth (MA): MDText.com, Inc.; 2000-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK278932/.
- Busetto L, Dicker D, Frühbeck G, et al. A new framework for the diagnosis, staging, and management of obesity in adults. Nat Med. 2024. [CrossRef]
- Wadden TA, Tronieri JS, Butryn ML. Lifestyle modification approaches for the treatment of obesity in adults. Am Psychol. 2020;75(2):235-251.
- Aragon AA, Schoenfeld BJ, Wildman R, Kleiner S, VanDusseldorp T, Taylor L, et al. International society of sports nutrition position stand: diets and body composition. J Int Soc Sports Nutr. 2017;14:16. [CrossRef] [PubMed] [PubMed Central]
- Brehm BJ, Seeley RJ, Daniels SR, D’Alessio DA. A randomized trial comparing a very low carbohydrate diet and a calorie-restricted low fat diet on body weight and cardiovascular risk factors in healthy women. J Clin Endocrinol Metab. 2003;88(4):1617-1623.
- Muscogiuri G, El Ghoch M, Colao A, Hassapidou M, Yumuk V, Busetto L; Obesity Management Task Force (OMTF) of the European Association for the Study of Obesity (EASO). European guidelines for obesity management in adults with a very low-calorie ketogenic diet: a systematic review and meta-analysis. Obes Facts. 2021;14(2):222-245. [CrossRef] [PubMed] [PubMed Central]
- Estruch R, Ros E, Salas-Salvadó J, et al. Primary prevention of cardiovascular disease with a Mediterranean diet. N Engl J Med. 2018;378(25):e34. [CrossRef]
- Lichtenstein AH, Appel LJ, Vadiveloo M, et al. 2021 Dietary Guidance to Improve Cardiovascular Health: A Scientific Statement From the American Heart Association. Circulation. 2021;144(23):e472-e487. [CrossRef]
- Sofi F, Abbate R, Gensini GF, Casini A. Accruing evidence on benefits of adherence to the Mediterranean diet on health: an updated systematic review and meta-analysis. Am J Clin Nutr. 2018;92(5):1189-1196. [CrossRef]
- Tosti V, Bertozzi B, Fontana L. Health benefits of the Mediterranean diet: metabolic and molecular mechanisms. J Gerontol A Biol Sci Med Sci. 2018;73(3):318-326. [CrossRef]
- Sacks FM, Svetkey LP, Vollmer WM, et al. Effects on blood pressure of reduced dietary sodium and the Dietary Approaches to Stop Hypertension (DASH) diet. N Engl J Med. 2018;344(1):3-10. [CrossRef]
- Appel LJ, Moore TJ, Obarzanek E, et al. A clinical trial of the effects of dietary patterns on blood pressure. N Engl J Med. 1997;336(16):1117-1124. [CrossRef]
- Hu T, Mills KT, Yao L, et al. Effects of low-carbohydrate diets versus low-fat diets on metabolic risk factors: a meta-analysis of randomized controlled trials. PLOS ONE. 2019;7(12):e1003117. [CrossRef]
- Bueno NB, de Melo IS, de Oliveira SL, da Rocha Ataide T. Very-low-carbohydrate ketogenic diet v. low-fat diet for long-term weight loss: a meta-analysis of randomised controlled trials. Br J Nutr. 2021;110(7):1178-1187. [CrossRef]
- Satija A, Hu FB. Plant-based diets and cardiovascular health. Trends Cardiovasc Med. 2018;28(7):437-441. [CrossRef]
- Kahleova H, Levin S, Barnard ND. Vegetarian dietary patterns and cardiovascular disease. Prog Cardiovasc Dis. 2021;64:1-8. [CrossRef]
- Willett W, Rockström J, Loken B, et al. Food in the Anthropocene: the EAT–Lancet Commission on healthy diets from sustainable food systems. Lancet. 2019;393(10170):447-492. [CrossRef]
- Antonio J, Peacock CA, Ellerbroek A, Fromhoff B, Silver T. The effects of consuming a high protein diet (4.4 g/kg/d) on body composition in resistance-trained individuals. J Int Soc Sports Nutr. 2014;11:19. [CrossRef]
- Luong TV, Abild CB, Bangshaab M, Gormsen LC, Søndergaard E. Ketogenic Diet and Cardiac Substrate Metabolism. Nutrients. 2022;14(7).
- Kim, JM. Ketogenic diet: Old treatment, new beginning. Clin Neurophysiol Pract. 2017;2:161-2.
- Antonio J, Peacock CA, Ellerbroek A, Fromhoff B, Silver T. The effects of consuming a high protein diet (4.4 g/kg/d) on body composition in resistance-trained individuals. J Int Soc Sports Nutr. 2014;11:19. [CrossRef]
- Lemon, PW. Do athletes need more dietary protein and amino acids?. Int J Sport Nutr. 1995;5(Suppl):S39-S61.
- Lemon PW, Tarnopolsky MA, MacDougall JD, Atkinson SA. Protein requirements and muscle mass/strength changes during intensive training in novice bodybuilders. J Appl Physiol. 1992;73:767-75.
- Lemon PW, Proctor DN. Protein intake and athletic performance. Sports Med. 1991;12:313-25.
- Lemon, PW. Protein and amino acid needs of the strength athlete. Int J Sport Nutr. 1991;1:127-45.
- Lemon, PW. Protein and exercise: update 1987. Med Sci Sports Exerc. 1987;19:S179-S190.
- Wilson J, Wilson GJ. Contemporary issues in protein requirements and consumption for resistance trained athletes. J Int Soc Sports Nutr. 2006;3:7-27.
- Campbell B, Kreider RB, Ziegenfuss T, La Bounty P, Roberts M, Burke D, et al. International Society of Sports Nutrition position stand: protein and exercise. J Int Soc Sports Nutr. 2007;4:8.
- Institute of Medicine. Dietary Reference Intakes for Energy, Carbohydrate, Fiber, Fat, Fatty Acids, Cholesterol, Protein and Amino Acids. Washington, DC: National Academies Press; 2005.
- Westerterp-Plantenga, MS. How are normal, high- or low-protein diets defined?. Br J Nutr. 2007;97:217-8.
- Johnston CS, Tjonn SL, Swan PD. High-protein, low-fat diets are effective for weight loss and favorably alter biomarkers in healthy adults. J Nutr. 2004;134:586-91.
- Westerterp-Plantenga MS, Rolland V, Wilson SA, Westerterp KR. Satiety related to 24 h diet-induced thermogenesis during high protein/carbohydrate vs high fat diets measured in a respiration chamber. Eur J Clin Nutr. 1999;53:495-502.
- Westerterp-Plantenga MS, Lejeune MP, Nijs I, van Ooijen M, Kovacs EM. High protein intake sustains weight maintenance after body weight loss in humans. Int J Obes Relat Metab Disord. 2004;28:57-64.
- Leidy HJ, Carnell NS, Mattes RD, Campbell WW. Higher protein intake preserves lean mass and satiety with weight loss in pre-obese and obese women. Obesity (Silver Spring). 2007;15:421-9.
- Tang M, Armstrong CL, Leidy HJ, Campbell WW. Normal vs high-protein weight loss diets in men: Effects on body composition and indices of metabolic syndrome. Obesity. 2013;21:E204-10.
- Tang M, Leidy HJ, Campbell WW. Regional, but not total, body composition changes in overweight and obese adults consuming a higher protein, energy-restricted diet are sex specific. Nutr Res. 2013;33(8):629-35.
- Paoli, A. Ketogenic diet for obesity: friend or foe? Int J Environ Res Public Health. 2014;11(2):2092-107. [CrossRef]
- Westerterp-Plantenga MS, Nieuwenhuizen A, Tome D, Soenen S, Westerterp KR. Dietary protein, weight loss, and weight maintenance. Annu Rev Nutr. 2009;29:21-41.
- Veldhorst M, Smeets A, Soenen S, Hochstenbach-Waelen A, Hursel R, Diepvens K, et al. Protein-induced satiety: Effects and mechanisms of different proteins. Physiol Behav. 2008;94(2):300-7.
- Gardner CD, Kiazand A, Alhassan S, Kim S, Stafford RS, Balise RR, et al. Comparison of the Atkins, Zone, Ornish, and LEARN diets for change in weight and related risk factors among overweight premenopausal women: the A TO Z Weight Loss Study: a randomized trial. JAMA. 2007;297(9):969-77.
- Oh R, Gilani B, Uppaluri KR. Low-Carbohydrate Diet. [Updated 2023 Aug 17]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK537084/.
- Westman E, Feinman R, Mavropoulos J, Vernon M, Volek J, Wortman J, et al. Low-carbohydrate nutrition and metabolism. Am J Clin Nutr. 2007;86(2):276-84.
- Masood W, Annamaraju P, Khan Suheb MZ, et al. Ketogenic Diet. [Updated 2023 Jun 16]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK499830/.
- O'Neill B, Raggi P. The ketogenic diet: Pros and cons. Atherosclerosis. 2020;292:119-126.
- Ma S, Suzuki K. Keto-Adaptation and Endurance Exercise Capacity, Fatigue Recovery, and Exercise-Induced Muscle and Organ Damage Prevention: A Narrative Review. Sports (Basel). 2019;7(2).
- Oh R, Gilani B, Uppaluri KR. Low-Carbohydrate Diet. [Updated 2023 Aug 17]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-.
- Broom GM, Shaw IC, Rucklidge JJ. The ketogenic diet as a potential treatment and prevention strategy for Alzheimer's disease. Nutrition. 2019;60:118-21.
- Ezpeleta M, Cienfuegos S, Lin S, Pavlou V, Gabel K, Tussing-Humphreys L, et al. Time-restricted eating: Watching the clock to treat obesity. Cell Metab. 2024;36(2):301-14. [CrossRef]
- Chaix A, Manoogian ENC, Melkani GC, Panda S. Time-restricted eating to prevent and manage chronic metabolic diseases. Annu Rev Nutr. 2019;39:291-315.
- Patikorn C, Roubal K, Veettil SK, Chandran V, Pham T, Lee YY, et al. Intermittent Fasting and Obesity-Related Health Outcomes: An Umbrella Review of Meta-analyses of Randomized Clinical Trials. JAMA Netw Open. 2021;4(12):e2139558. [CrossRef]
- Anton SD, Moehl K, Donahoo WT, Lee SA, Mainous AG, Leeuwenburgh C, et al. Flipping the metabolic switch: understanding and applying the health benefits of fasting. Obesity (Silver Spring). 2018;26(2):254-68.
- Trepanowski JF, Bloomer RJ. The impact of religious fasting on human health. Nutr J. 2010;9(1):57.
- Varady KA, Cienfuegos S, Ezpeleta M, Gabel K. Clinical application of intermittent fasting for weight loss: progress and future directions. Nat Rev Endocrinol. 2022;18:309-21.
- Cienfuegos S, Gabel K, Kalam F, Ezpeleta M, Wiseman E, Pavlou V, et al. Effects of 4- and 6-h time-restricted feeding on weight and cardiometabolic health: a randomized controlled trial in adults with obesity. Cell Metab. 2020;32(3):366-78.
- Gabel K, Hoddy KK, Haggerty N, Song J, Kroeger CM, Trepanowski JF, et al. Effects of 8-hour time restricted feeding on body weight and metabolic disease risk factors in obese adults: a pilot study. Nutr Healthy Aging. 2018;4:345-53.
- Lin S, Cienfuegos S, Ezpeleta M, Gabel K, Pavlou V, Mulas A, et al. Time-restricted eating without calorie counting for weight loss in a racially diverse population: a randomized controlled trial. Ann Intern Med. 2023;176(6):885-95.
- Haganes KL, Silva CP, Eyjólfsdóttir SK, Steen S, Grindberg M, Lydersen S, et al. Time-restricted eating and exercise training improve HbA1c and body composition in women with overweight/obesity: a randomized controlled trial. Cell Metab. 2022;34(10):1457-71.
- Zhang LM, Liu Z, Wang JQ, Li RQ, Ren JY, Gao X, et al. Randomized controlled trial for time-restricted eating in overweight and obese young adults. iScience. 2022;25(8):104870.
- Chow LS, Manoogian ENC, Alvear A, Fleischer JG, Thor H, Dietsche K, et al. Time-restricted eating effects on body composition and metabolic measures in humans who are overweight: a feasibility study. Obesity (Silver Spring). 2020;28(5):860-9.
- Hippisley-Cox J, Coupland C, Brindle P. Development and validation of QRISK3 risk prediction algorithms to estimate future risk of cardiovascular disease: prospective cohort study. BMJ. 2017;357:j2099. [CrossRef]
- National Institute for Health and Care Excellence (NICE). Cardiovascular disease: risk assessment and reduction, including lipid modification. NICE guideline [CG181]. Published July 2014. Updated September 2016. Available from: https://www.nice.org.uk/guidance/cg181. Accessed January 27, 2025.
- Collins GS, Altman DG. An independent external validation and evaluation of QRISK cardiovascular risk prediction: a prospective open cohort study. BMJ. 2009;339:b2584. [CrossRef]
- D’Agostino RB, Vasan RS, Pencina MJ, et al. General cardiovascular risk profile for use in primary care: the Framingham Heart Study. Circulation. 2008;117(6):743-753. [CrossRef]
- Estruch R, Ros E, Salas-Salvadó J, et al. Primary prevention of cardiovascular disease with a Mediterranean diet. N Engl J Med. 2018;378(25):e34. [CrossRef]
- Tosti V, Bertozzi B, Fontana L. Health benefits of the Mediterranean diet: metabolic and molecular mechanisms. J Gerontol A Biol Sci Med Sci. 2018;73(3):318-326. [CrossRef]
- Sofi F, Cesari F, Abbate R, Gensini GF, Casini A. Adherence to Mediterranean diet and health status: meta-analysis. *BMJ*. 2008;337:a1344. [CrossRef]
- Sacks FM, Svetkey LP, Vollmer WM, et al. Effects on blood pressure of reduced dietary sodium and the Dietary Approaches to Stop Hypertension (DASH) diet. N Engl J Med. 2001;344(1):3-10. [CrossRef]
- Satija A, Bhupathiraju SN, Spiegelman D, et al. Healthful and unhealthful plant-based diets and the risk of coronary heart disease in U.S. adults. J Am Coll Cardiol. 2017;70(4):411-422. [CrossRef]
- Kahleova H, Levin S, Barnard ND. Cardio-metabolic benefits of plant-based diets. Nutrients. 2017;9(8):848. [CrossRef]
- Willett W, Rockström J, Loken B, et al. Food in the Anthropocene: the EAT-Lancet Commission on healthy diets from sustainable food systems. Lancet. 2019;393(10170):447-492. [CrossRef]
- Holt RI, Bushe C, Citrome L. Diabetes and schizophrenia 2005: are we any closer to understanding the link?. J Psychopharmacol. 2005;19(Suppl 6):56-65.
- Mitchell SL, Leon DAC, Chaugai S, Kawai VK, Levinson RT, Wei WQ, et al. Pharmacogenetics of hypoglycemia associated with sulfonylurea therapy in usual clinical care. Pharmacogenomics J. 2020;20(6):831-9.
- Magiakou MA, Mastorakos G, Oldfield EH, Chrousos GP. Cushing’s syndrome in children and adolescents. Presentation, diagnosis and therapy. N Engl J Med. 1994;331(10):629-36.
- Consensus development conference on antipsychotic drugs and obesity and diabetes. Diabetes Care. 2004;27:596-601.
- Watson NF, Badr MS, Belenky G, Bliwise DL, Buxton OM, Buysse D, et al. Recommended amount of sleep for a healthy adult: A joint consensus statement of the American Academy of Sleep Medicine and Sleep Research Society. Sleep. 2015;38(6):843-4.
- Daviet R, Aydogan G, Jagannathan K, Karlsson Linnér R, Perry DI, Wiers CE, et al. Associations between alcohol consumption and gray and white matter volumes in the UK Biobank. Nat Commun. 2022;13:1175.
- Kuriyan, R. Body composition techniques. Indian J Med Res. 2018;148(5):648-58. [CrossRef] [PubMed] [PubMed Central]
- Weir CB, Jan A. BMI Classification Percentile And Cut Off Points. [Updated 2022 Jun 27]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-.
- Hippisley-Cox J, Coupland C, Brindle P. Development and validation of QRISK3 risk prediction algorithms to estimate future risk of cardiovascular disease: prospective cohort study. BMJ. 2017;357:j2099.
- QRISK3 Calculator. University of Nottingham. Available at: https://qrisk.org/. Accessed January 29, 2025.
- Ling CHY, de Craen AJM, Slagboom PE, et al. Accuracy of direct segmental multi-frequency bioimpedance analysis in the assessment of total body and segmental body composition in middle-aged adult population. Clin Nutr. 2011;30(5):610-615. [CrossRef]
- Miller RM, Chambers TL, Burns SP. Validating InBody® 570 Multi-frequency Bioelectrical Impedance Analyzer versus DXA for Body Fat Percentage Analysis. J Exerc Physiol Online. 2016;19(5):71-78.
- Fosbøl MØ, Zerahn B. Contemporary methods of body composition measurement. Clin Physiol Funct Imaging. 2015;35(2):81-97. [CrossRef]
- Tanita Corporation. Accuracy and reliability of Tanita Body Composition Analyzers. Available at: https://www.tanita.com/en/research. Accessed January 29, 2025.
- Kyle UG, Bosaeus I, De Lorenzo AD, et al. Bioelectrical impedance analysis—part I: review of principles and methods. Clin Nutr. 2004;23(5):1226-1243. [CrossRef]
- Wang JG, Zhang Y, Chen HE, et al. Validation of body composition analysis using bioelectrical impedance analysis in different populations. J Clin Med. 2021;10(4):856. [CrossRef]
- Sardinha LB, Júdice PB, Silva AM, et al. Accuracy of bioelectrical impedance analysis in estimating body composition changes in overweight and obese women during weight loss. Obesity. 2018;26(3):507-513. [CrossRef]
- Bosy-Westphal A, Danielzik S, Dörhöfer RP, et al. Patterns of bioelectrical impedance vector analysis and association with body composition in obese women. Obesity. 2005;13(8):1466-1473. [CrossRef]
- Khalil SF, Mohktar MS, Ibrahim F. The theory and fundamentals of bioimpedance analysis in clinical status monitoring and diagnosis of diseases. Sensors. 2014;14(6):10895-10928. [CrossRef]
- Dehghan M, Merchant AT. Is bioelectrical impedance accurate for use in large epidemiological studies? Nutr J. 2008;7:26. [CrossRef]
- Malavolti M, Mussi C, Poli M, et al. Cross-calibration of eight-polar bioelectrical impedance analysis versus dual-energy X-ray absorptiometry for the assessment of total and regional body composition in healthy subjects. Nutr Metab Cardiovasc Dis. 2003;13(6):245-251.
- Kora. “Microsoft Word - 9.Ene.doc” 29 Apr. 2014, upg-bulletin-se.ro/old_site/archive/2014-1/upg-bulletin-se.ro/old_site/archive/2014-1/9.Ene.pdf. Accessed 24 Aug. 2024.
- Gerrior S, Juan W, Basiotis P. An easy approach to calculating estimated energy requirements. Prev Chronic Dis. 2006;3(4):A129. [PubMed] [PubMed Central]
- Human energy requirements: report of a joint FAO/WHO/UNU Expert Consultation. Food Nutr Bull. 2005;26(1):166. [PubMed]
- Freeman JM, Kossoff EH, Hartman AL. The ketogenic diet: one decade later. Pediatrics. 2007;119(3):535-43. [CrossRef] [PubMed]
- Patikorn C, Saidoung P, Pham T, Phisalprapa P, Lee YY, Varady KA, et al. Effects of ketogenic diet on health outcomes: an umbrella review of meta-analyses of randomized clinical trials. BMC Med. 2023;21(1):196. [CrossRef] [PubMed] [PubMed Central]
- Kim, JY. Optimal Diet Strategies for Weight Loss and Weight Loss Maintenance. J Obes Metab Syndr. 2021;30(1):20-31. [CrossRef] [PubMed] [PubMed Central]
- World Health Organization. Obesity and overweight. Fact sheet No. 311. Geneva: World Health Organization; 2020. Available from: https://www.who.int/news-room/fact-sheets/detail/obesity-and-overweight.
- Powell-Wiley TM, Poirier P, Burke LE, Després JP, Gordon-Larsen P, Lavie CJ, et al. Obesity and Cardiovascular Disease: A Scientific Statement From the American Heart Association. Circulation. 2021;143(21):e984-e1010. [CrossRef]
- Ouchi N, Parker JL, Lugus JJ, Walsh K. Adipokines in inflammation and metabolic disease. Nat Rev Immunol. 2018;18(2):95-106. [CrossRef]
- Piché ME, Tchernof A, Després JP. Obesity Phenotypes, Diabetes, and Cardiovascular Diseases. Circ Res. 2020;126(11):1477-1500. [CrossRef]
- Catapano AL, Graham I, De Backer G, Wiklund O, Chapman MJ, Drexel H, et al. 2019 ESC/EAS Guidelines for the management of dyslipidaemias: lipid modification to reduce cardiovascular risk. Eur Heart J. 2020;41(1):111-188. [CrossRef]
- Hall JE, do Carmo JM, da Silva AA, Wang Z, Hall ME. Obesity-induced hypertension: interaction of neurohumoral and renal mechanisms. Circ Res. 2019;124(6): 865-887. [CrossRef]
- Kenchaiah S, Evans JC, Levy D, Wilson PW, Benjamin EJ, Larson MG, et al. Obesity and the risk of heart failure. N Engl J Med. 2019;347(5):305-313. [CrossRef]
- Iacobellis, G. Epicardial adipose tissue in endocrine and metabolic diseases. Endocr Rev. 2019;40(2):432-460. [CrossRef]
- Pathak RK, Middeldorp ME, Meredith M, Mehta AB, Mahajan R, Wong CX, et al. Long-term effect of goal-directed weight management in an atrial fibrillation cohort: a randomized controlled study. J Am Coll Cardiol. 2019;64(21):2159-2169. [CrossRef]
- Javaheri S, Barbe F, Campos-Rodriguez F, Dempsey JA, Khayat R, Malhotra A, et al. Sleep apnea: types, mechanisms, and clinical cardiovascular consequences. J Am Coll Cardiol. 2020;69(7):841-858. [CrossRef]
- De Marco C, Perna S, Bramanti E, Guerriero F, Luzzi S, Biondi-Zoccai G, et al. Insulin resistance and endothelial dysfunction: molecular basis and therapeutic perspectives. Life Sci. 2022;308:120964. [CrossRef]
- Hippisley-Cox J, Coupland C, Brindle P. Development and validation of QRISK3 risk prediction algorithms to estimate future risk of cardiovascular disease: prospective cohort study. BMJ. 2017;357:j2099. [CrossRef]
- Collins GS, Altman DG. Predicting cardiovascular risk in the UK: QRISK3 and other risk prediction models. Heart. 2017;103(10):683-689. [CrossRef]
- Yates T, Zaccardi F, Razieh C, et al. Obesity, risk stratification and cardiovascular disease: QRISK3 utility in clinical practice. J Clin Med. 2021;10(7):1487. [CrossRef]
- Ramos R, Ballo E, Marrugat J, et al. Validation of QRISK3 for cardiovascular risk prediction in a Mediterranean cohort. Int J Cardiol. 2020;315:122-128. [CrossRef]
- Stefan N, Häring HU, Schulze MB. Metabolically healthy obesity: epidemiology, mechanisms, and clinical implications. Lancet Diabetes Endocrinol. 2023;11(1):34-47. [CrossRef]
- van der Ende MY, Hartman MHT, Hagemeijer Y, et al. The association between atrial fibrillation, obesity and cardiovascular risk scores in QRISK3: a cohort study. Eur Heart J. 2022;43(5):456-466. [CrossRef]
- Banach M, Penson PE, Fras Z, et al. The role of QRISK3 in lipid management: implications for statin therapy in primary prevention. Atherosclerosis. 2021;320:112-122. [CrossRef]
- Zinman B, Wanner C, Lachin JM, et al. Empagliflozin, cardiovascular outcomes, and mortality in type 2 diabetes. N Engl J Med. 2018;373(22):2117-2128. [CrossRef]
- O’Donovan G, Lee IM, Hamer M, Stamatakis E. Association of “weekend warrior” and other leisure-time physical activity patterns with risks for all-cause, cardiovascular disease, and cancer mortality. JAMA Intern Med. 2017;177(3):335-342. [CrossRef]
- Woodward M, Brindle P, Tunstall-Pedoe H. Adding social deprivation and family history to cardiovascular risk assessment: the ASSIGN score compared with Framingham algorithms. Heart. 2018;93(2):172-176. [CrossRef]
- Makris A, Foster GD. Dietary approaches to the treatment of obesity. Psychiatr Clin North Am. 2011;34:813-27.
- Volek JS, Vanheest JL, Forsythe CE. Diet and exercise for weight loss: a review of current issues. Sports Med. 2005;35:1-9.
- Wirth A, Wabitsch M, Hauner H. The prevention and treatment of obesity. Dtsch Arztebl Int. 2014;111:705-13.
- Jensen MD, Ryan DH, Apovian CM, Ard JD, Comuzzie AG, Donato KA, et al. 2013 AHA/ACC/TOS guideline for the management of overweight and obesity in adults: A report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and The Obesity Society. Circulation. 2014;129:S102-38.
- Wang Z, Zhang M, Gao X. Impact of the ketogenic diet on cardiovascular disease risk factors: a meta-analysis. Am J Clin Nutr. 2024;120(2):294-309.
- Johnson T, Patel K. Long-term effects of ketogenic diets on lipid metabolism and cardiovascular risk. BMC Med.2022;18(6):230-238.
- Smith J, Doe A, Brown K. Effects of a six-week ketogenic diet on lipid metabolism and cardiovascular markers in normal-weight males. J Nutr Metab. 2021;15(3):123-130.
- Jones M, White P, Taylor L. Time-restricted eating and metabolic syndrome: A 12-week clinical trial. Int J Obes. 2020;44(7):890-899.
- Gabel K, Cienfuegos S, Kalam F, Ezpeleta M, Varady KA. Time-Restricted Eating to Improve Cardiovascular Health. Curr Atheroscler Rep. 2021 Mar 26;23(5):22. [CrossRef] [PubMed] [PubMed Central]
- Wang Z, Chen T, Wu S, Dong X, Zhang M, Ma G. Impact of the ketogenic diet as a dietary approach on cardiovascular disease risk factors: a meta-analysis of randomized clinical trials. Am J Clin Nutr. 2024 Aug;120(2):294-309. Epub 2024 Jul 15. [CrossRef] [PubMed]
- He M, Wang J. Time-restricted eating with or without low-carbohydrate diet reduces visceral fat and improves metabolic syndrome: A randomized trial. BMC Med. 2024;22:95.
- American Heart Association News. 8-hour time-restricted eating linked to a 91% higher risk of cardiovascular death. 2024 Mar 18. Available from: https://newsroom.heart.
- He M, Wang J, Liang Q, Li M, Guo H, Wang Y, Deji C, Sui J, Wang YW, Liu Y, Zheng Y, Qian B, Chen H, Ma M, Su S, Geng H, Zhou WX, Guo X, Zhu WZ, Zhang M, Chen Z, Rensen PCN, Hui CC, Wang Y, Shi B. Time-restricted eating with or without low-carbohydrate diet reduces visceral fat and improves metabolic syndrome: A randomized trial. Cell Rep Med. 2022 Oct 18;3(10):100777. Epub 2022 Oct 10. [CrossRef] [PubMed] [PubMed Central]
- Bueno NB, de Melo IS, de Oliveira SL, da Rocha Ataide T. Very-low-carbohydrate ketogenic diet v. low-fat diet for long-term weight loss: a meta-analysis of randomized controlled trials. Br J Nutr. 2013;110(7):1178-87.
- Wilkinson MJ, Manoogian ENC, Zadourian A, Lo H, Fakhouri S, Shoghi A, et al. Ten-hour time-restricted eating reduces weight, blood pressure, and atherogenic lipids in patients with metabolic syndrome. Cell Metab. 2020;31(1):92-104.e5.
- Sutton EF, Beyl R, Early KS, Cefalu WT, Ravussin E, Peterson CM. Early Time-Restricted Feeding Improves Insulin Sensitivity, Blood Pressure, and Oxidative Stress Even without Weight Loss in Men with Prediabetes. Cell Metab. 2018;27(6):1212-21.e3.
- Yang Q, Zhang H, Guo S, Li Y, Zhang J, Liu C, et al. Association of time-restricted eating with cardiovascular mortality in adults. J Am Heart Assoc. 2023;12(3):e027463.
- Pala B, Pennazzi L, Nardoianni G, Rubattu SD, Volpe M, Colao AM, et al. Very low-calorie ketogenic diet reduces central blood pressure and cardiometabolic risk in post-menopausal women with essential hypertension and obesity: a single-center, prospective, open-label, clinical study. Nutr Metab Cardiovasc Dis. 2024 Dec 20:103838.
- American Heart Association News. 8-hour time-restricted eating linked to a 91% higher risk of cardiovascular death. 2024 Mar 18. Available from: https://newsroom.heart.org/news/8-hour-time-restricted-eating-linked-to-a-91-higher-risk-of-cardiovascular-death.
| Variable | TRE N=26 |
KD N=23 |
p-value | (rank biserial) |
|---|---|---|---|---|
| Age | 37.50 (28.25 - 48.00) | 36.00 (29.50 - 42.50) | 0.79 | -0.05 |
| BMI | 30.25 (27.43 - 33.18) | 33.20 (31.85 - 37.80) | 0.02 | -0.41 |
| WC | 100.50 (91.00 - 110.75) | 110.00 (97.50 - 122.50) | 0.04 | -0.35 |
| WHR | 0.90 (0.88 - 1.07) | 0.98 (0.92 - 1.17) | 0.04 | -0.34 |
| TC | 187.00 (167.25 - 219.75) | 200.00 (145.50 - 242.00) | 0.86 | -0.03 |
| HDL-C | 54.00 (45.25 - 60.00) | 48.00 (46.00 - 60.50) | 0.60 | 0.09 |
| TC/HDL-C | 3.85 (3.01 - 4.30) | 3.91 (2.52 - 4.98) | 0.86 | -0.03 |
| SBP | 126.00 (112.75 - 143.50) | 122.00 (115.50 - 145.00) | 0.79 | -0.05 |
| QRISK | 11.75 (6.58 - 30.12) | 11.80 (7.15 - 26.15) | 0.70 | 0.07 |
| Relative Risk | 16.70 (8.27 - 33.83) | 13.00 (10.10 - 22.20) | 0.62 | 0.09 |
| Non-HDL-C | 139.00 (104.00 - 170.00) | 155.00 (85.00 - 187.50) | 0.64 | -0.08 |
| LDL-C | 124.50 (94.50 - 143.00) | 131.00 (85.50 - 163.00) | 0.68 | -0.07 |
| Triglycerides | 100.00 (86.50 - 164.00) | 120.00 (87.00 - 173.00) | 0.60 | -0.09 |
| Uric Acid | 5.75 (4.67 - 6.60) | 5.20 (4.05 - 5.95) | 0.16 | 0.24 |
| Serum Creatinine | 0.67 (0.65 - 0.71) | 0.64 (0.58 - 0.72) | 0.41 | 0.14 |
| Fasting Glucose | 96.50 (92.50 - 106.75) | 100.00 (90.00 - 119.00) | 0.48 | -0.12 |
| HbA1c | 5.50 (5.23 - 5.90) | 5.90 (5.15 - 6.50) | 0.62 | -0.09 |
| HOMA-IR | 2.10 (1.50 - 3.22) | 3.10 (1.70 - 6.15) | 0.14 | -0.25 |
| Vitamin D | 22.50 (19.00 - 30.75) | 21.00 (16.50 - 25.50) | 0.14 | 0.25 |
| Variable | Class | IF | KD | p-value |
| Sex | F | 17 (65.38%) | (69.57%) | 0.76 |
| M | 9 (34.62%) | 7 (30.43%) | ||
| Smoker | Yes | 17 (65.38%) | 13 (56.52%) | 0.79 |
| Sedentary | Yes | 10 (38.46%) | 8 (34.78%) | 0.79 |
| Sleep Deficit | Yes | 12 (46.15%) | 8 (34.78%) | 0.42 |
| Menopause | Yes | 7 (26.92%) | 5 (21.74%) | 0.67 |
| FMH CV | Yes | 14 (53.85%) | 7 (30.43%) | 0.10 |
| RA | Yes | 8 (30.77%) | 2 (8.7%) | 0.06 |
| LES | Yes | 9 (34.62%) | 6 (26.09%) | 0.52 |
| ED | Yes | 5 (19.23%) | 2 (8.7%) | 0.29 |
| Migraines | Yes | 16 (61.54%) | 3 (13.04%) | < 0.001 |
| AF | Yes | 1 (3.85%) | 0 (0%) | 0.34 |
| Variable | TRE N=26 |
KD N=23 |
p-value | (rank biserial) |
|---|---|---|---|---|
| BMI | 29.30 (26.07 - 32.27) | 29.50 (26.50 - 35.05) | 0.57 | -0.10 |
| WC | 98.50 (90.25 - 109.25) | 98.00 (87.00 - 108.00) | 0.88 | 0.03 |
| WHR | 0.89 (0.85 - 0.97) | 0.90 (0.85 - 0.95) | 0.55 | 0.10 |
| SBP | 126.00 (110.50 - 140.00) | 115.00 (107.00 - 124.00) | 0.10 | 0.28 |
| TC | 185.00 (165.00 - 218.75) | 165.00 (114.50 - 198.50) | 0.07 | 0.30 |
| HDL-C | 55.00 (42.75 - 60.00) | 58.00 (51.00 - 66.00) | 0.05 | -0.33 |
| TC/HDL-C | 3.94 (2.96 - 4.42) | 2.98 (1.91 - 3.48) | 0.02 | 0.41 |
| QRISK | 11.45 (6.28 - 29.10) | 7.80 (4.40 - 13.55) | 0.06 | 0.32 |
| Relative Risk | 15.75 (7.87 - 33.45) | 9.50 (6.40 - 17.00) | 0.04 | 0.34 |
| HbA1c | 5.50 (5.15 - 5.90) | 5.30 (5.05 - 5.65) | 0.13 | 0.25 |
| Variable | Diet | Initial Measurement | Final Measurement | p-value |
| BMI | TRE | 30.25 | 29.30 | < 0.001 |
| KD | 33.20 | 29.50 | < 0.001 | |
| WC | TRE | 100.50 | 98.50 | < 0.001 |
| KD | 110.00 | 98.00 | < 0.001 | |
| WHR | TRE | 0.90 | 0.89 | < 0.001 |
| KD | 0.98 | 0.90 | < 0.001 | |
| TC | TRE | 187.00 | 185.00 | < 0.001 |
| KD | 200.00 | 165.00 | < 0.001 | |
| HDL-C | TRE | 54.00 | 55.00 | 0.30 |
| KD | 48.00 | 58.00 | < 0.001 | |
| TC/HDL-C | TRE | 3.85 | 3.94 | 0.74 |
| KD | 3.91 | 2.98 | < 0.001 | |
| SBP | TRE | 126.00 | 126.00 | 0.002 |
| KD | 122.00 | 115.00 | < 0.001 | |
| QRISK | TRE | 11.75 | 11.45 | 0.05 |
| KD | 11.80 | 7.80 | < 0.001 | |
| Relative Risk | TRE | 16.70 | 15.75 | < 0.001 |
| KD | 13.00 | 9.50 | < 0.001 | |
| HbA1c | TRE | 5.50 | 5.50 | 0.001 |
| KD | 5.90 | 5.30 | < 0.001 |
| Variable | (rho) | p-value |
|---|---|---|
| SBP | -0.435 | 0.02 |
| Variable | p-value | |
|---|---|---|
| Age | -0.490 | 0.01 |
| BMI | -0.806 | < 0.001 |
| WC | -0.588 | 0.003 |
| WHR | -0.468 | 0.02 |
| TC | -0.431 | 0.04 |
| SBP | -0.630 | 0.001 |
| Non-HDL-C | -0.448 | 0.03 |
| Triglycerides | -0.451 | 0.03 |
| HbA1c | -0.469 | 0.02 |
| Predictors | Estimates | CI | p-value |
| Atrial Fibrillation [Yes] | 6.11 | 0.05 – 12.17 | 0.048 |
| BMI Initial | -0.46 | -0.62 – -0.30 | <0.001 |
| Total Cholesterol Initial | -0.02 | -0.04 – -0.00 | 0.025 |
| QRISK Initial (%) | 0.91 | 0.85 – 0.97 | <0.001 |
| Serum Creatinine | -9.03 | -16.23 – -1.82 | 0.015 |
| Fasting Glucose | 0.04 | 0.01 – 0.08 | 0.015 |
| Diet Followed [KD] | -4.98 | -6.71 – -3.24 | <0.001 |
| Observations = 49 | |||
| R2 adjusted = 0.975 | |||
| Predictors | Estimates | CI | p-value |
| Diet Followed [KD] | 4.18 | -3.84 – 12.20 | 0.300 |
| Age | -0.03 | -0.17 – 0.11 | 0.680 |
| Diet Followed [KD] × Age | -0.27 | -0.47 – -0.06 | 0.011 |
| Observations = 49 | |||
| R2 adjusted = 0.495 | |||
| Predictors | Estimates | CI | p-value |
| Diet Followed [KD] | 16.24 | 2.30 – 30.18 | 0.023 |
| SBP | -0.02 | -0.09 – 0.06 | 0.628 |
| Diet Followed [KD] × SBP | -0.17 | -0.28 – -0.06 | 0.002 |
| Observations = 49 | |||
| R2 adjusted = 0.549 | |||
| Predictors | Estimates | CI | p-value |
| Diet Followed [KD] | 18.61 | 6.17 – 31.06 | 0.004 |
| HbA1c Initial | 0.17 | -1.18 – 1.51 | 0.805 |
| Diet Followed [KD] × HbA1c Initial | -4.16 | -6.25 – -2.08 | <0.001 |
| Observations = 49 | |||
| R2 adjusted = 0.555 | |||
| Predictors | Estimates | CI | p-value |
| Diet Followed [KD] | 19.86 | 9.40 – 30.31 | <0.001 |
| BMI Initial | -0.04 | -0.27 – 0.20 | 0.764 |
| Diet Followed [KD] × BMI | -0.73 | -1.05 – -0.42 | <0.001 |
| Observations = 49 | |||
| R2 adjusted = 0.694 | |||
| Predictors | Estimates | CI | p-value |
| Diet Followed [KD] | 6.65 | -1.32 – 14.61 | 0.100 |
| WHR | -0.70 | -5.69 – 4.28 | 0.778 |
| Diet Followed [KD] × WHR | -11.45 | -18.62 – -4.28 | 0.002 |
| Observations = 49 | |||
| R2 adjusted = 0.536 | |||
| Predictors | Estimates | CI | p-value |
| Diet Followed [KD] | 6.35 | -4.35 – 17.06 | 0.238 |
| Fasting Glucose | 0.00 | -0.05 – 0.06 | 0.863 |
|
Diet Followed [KD] × Fasting Glucose |
-0.12 | -0.22 – -0.02 | 0.021 |
| Observations = 49 | |||
| R2 adjusted = 0.406 | |||
| Predictors | Estimates | CI | p-value |
| Diet Followed [KD] | -4.53 | -6.96 – -2.09 | 0.001 |
| Menopause [Yes] | -0.60 | -3.88 – 2.67 | 0.711 |
|
Diet Followed [KD] × Menopause [Yes] |
-7.38 | -12.35 – -2.41 | 0.005 |
| Observations = 49 | |||
| R2 adjusted = 0.506 | |||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




