Background
Total elbow arthroplasty (TEA) was originally developed as a specialized orthopedic intervention for the management of end-stage rheumatoid arthritis (RA). Over time, its clinical indications have expanded to encompass additional severe elbow joint pathologies, including osteoarthritis and complex distal humerus fractures, particularly in low-demand patients, typically over 65 years of age. Moreover, TEA is occasionally employed for less prevalent conditions such as hemophilic arthropathy, juvenile idiopathic arthritis, and primary or metastatic neoplasms.[
1,
2,
3] Nevertheless, contraindications such as neurological compromise affecting hand functionality, cognitive impairments (e.g., dementia), patient noncompliance, and open fractures must be carefully evaluated. Relative contraindications also exist for patients requiring weight-bearing functionality through the affected upper extremity.[
4]
Over the past two decades, the utilization of TEA has demonstrated variable trends. Earlier epidemiological studies reported an increasing incidence of the procedure, with an annual growth rate of approximately 6.4%.[
5] However, more contemporary analyses have highlighted a significant decline, with TEA volumes decreasing by 33% between 2010 and 2018.[
6] This trend may be attributed to advances in disease-modifying antirheumatic drugs, which have markedly enhanced the medical management of RA.[
7]
Hospitalization metrics indicate that the median length of stay for TEA procedures is approximately two days, [
8] with substantial variability in associated costs. Reported estimates range from
$16,300 ±
$4,000 to
$51,970, depending on variables such as geographical location, hospital system, type of charges reported, and insurance coverage. Additionally, the surgeon’s fees typically range between
$1,228 and
$1,842.[
5,
9]
Despite its therapeutic benefits, TEA is associated with a relatively high complication rate compared to other major joint arthroplasty procedures. These complication rates are influenced by patient-specific factors, surgical indications, and prosthetic design. TEA prostheses are available in constrained, unconstrained, and semiconstrained designs, each offering unique advantages and limitations. Historically, aseptic loosening has been the predominant cause of prosthesis failure. However, the advent of semi-constrained and unlinked prosthetic designs has mitigated its incidence. Conversely, prosthetic instability is more frequently observed with semiconstrained designs. Additional complications include infection, a major contributor to revision surgeries, and periprosthetic fractures, which account for approximately 12% of primary TEA failures. Less common complications include bushing wear, particularly with constrained designs, as well as ulnar nerve deficits and triceps dysfunction.[
10,
11,
12]
Postoperative care protocols remain heterogeneous, with significant variation in permitted ranges of motion, weight-bearing restrictions, and lifetime activity recommendations. Although consensus guidelines have not been established, general recommendations emphasize minimizing axial loading and weight-bearing, typically advising restrictions between 1 and 5 kilograms.[
13]
With the use if the National Inpatient Sample Database (NIS), the present study endeavors to further elucidate the clinical outcomes, complication rates, health care resource utilization, and postoperative management strategies associated with TEA, thereby contributing to a more comprehensive understanding of its evolving role in orthopedic practice.
Methods
Data Source and Study Population
This retrospective cohort study utilized data from the Nationwide Inpatient Sample (NIS), a comprehensive administrative database that captures inpatient hospitalizations across the United States. Patients who underwent total elbow arthroplasty (TEA) were identified using specific ICD-10 procedure codes, as detailed in the Appendix. The study period extended from January 1, 2016, to December 31, 2019, representing the most recent data available within the NIS framework at the time of analysis.
Inclusion and Exclusion Criteria
The study included patients who underwent elective TEA procedures during the designated study period, resulting in a final cohort of 4,110 cases. Non-elective admissions, including emergency or trauma-related procedures, were excluded to ensure homogeneity and minimize confounding factors.
Outcome Measures
Key outcomes analyzed in this study included temporal trends in TEA utilization, etiological distributions, patient demographic and clinical characteristics, prevalence of comorbidities, rates and types of postoperative complications, duration of hospital stay, and total hospitalization costs.
Statistical Analysis
All statistical analyses were performed using SPSS version 26. Chi-square tests and independent samples t-tests were employed to evaluate categorical and continuous variables, respectively. Crosstab analyses and risk ratio calculations were used to assess relationships between patient characteristics and postoperative outcomes. A significance threshold of p < 0.05 was applied across all statistical tests.
Risk ratios were specifically calculated to evaluate the relative likelihood of major postoperative complications, including heart failure, infection, acute kidney injury, blood transfusion, pneumonia, acute coronary artery disease, and blood loss anemia.
Ethical Considerations
The study was granted exempt status by the institutional review board, as the de-identified nature of the NIS dataset ensured compliance with ethical standards for human subject research.
Results
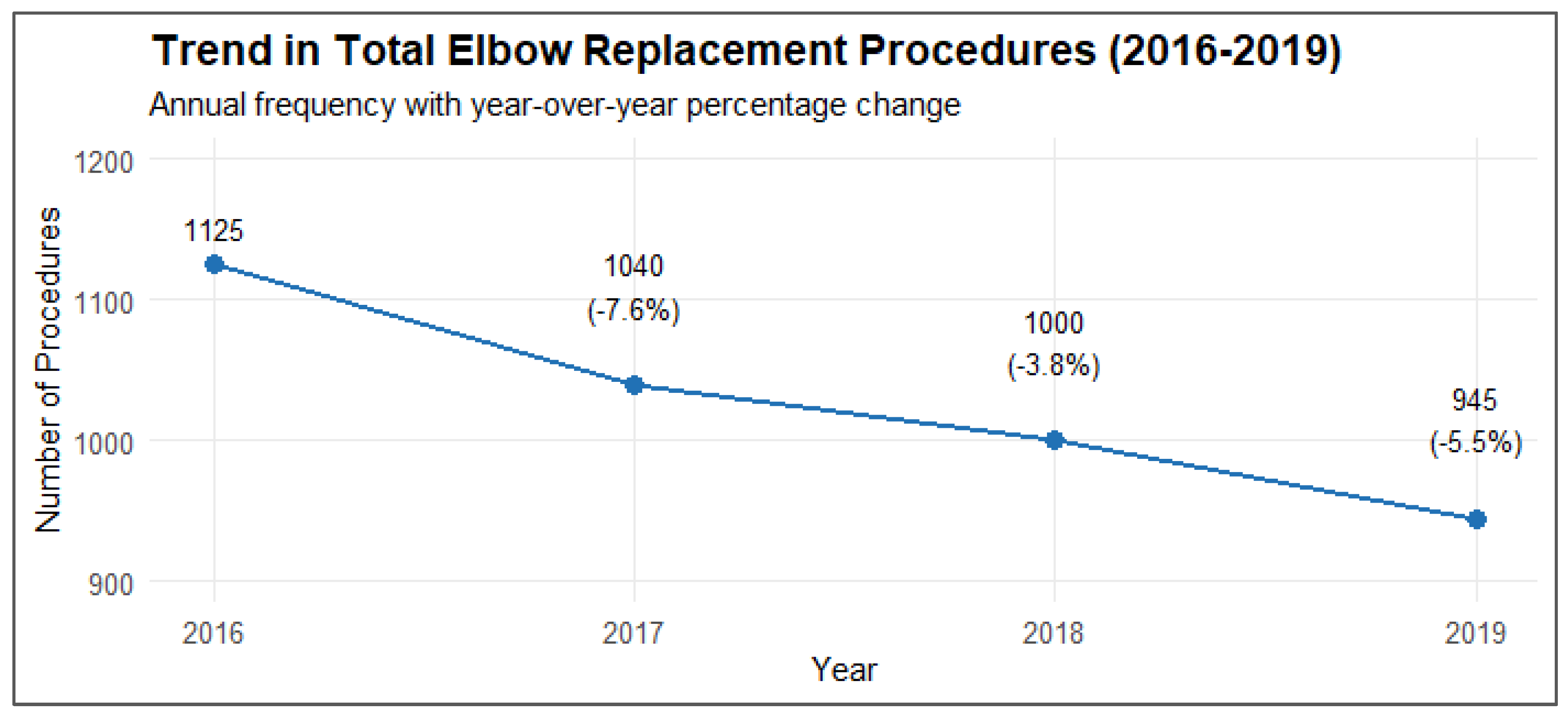
Between 2016 and 2019, there was a statistically significant downward trend in the number of total elbow replacement procedures (p=0.012). Starting from 1,125 procedures in 2016, the number decreased annually to 945 procedures in 2019, representing a total decline of 16% over the study period. The steepest year-over-year decline occurred in 2017 (-7.6%, -85 procedures), followed by more moderate decreases in 2019 (-5.5%, -55 procedures) and 2018 (-3.8%, -40 procedures). Linear regression analysis revealed a significant annual decrease of 58 procedures per year. Over the four-year period, the total number of procedures performed was 4,110, with the annual proportion of procedures showing a gradual decrease from 27.4% in 2016 to 23.0% in 2019.
Figure 1.
– Trends in Total Elbow Replacement Procedures (2016 – 2019).
Figure 1.
– Trends in Total Elbow Replacement Procedures (2016 – 2019).
Among 4,110 patients who underwent total elbow replacement, the mean age was 65.99 ± 13.47 years, with a predominance of female patients (75.3%). The majority of patients were White (72.6%), followed by Hispanic (10.3%), Black (6.7%), and Asian (1.8%) patients. Hypertension was the most prevalent comorbidity (51.3%), followed by mental disorders (38.1%), dyslipidemia (37.2%), and type 2 diabetes (19.5%). Less common comorbidities included sleep apnea (12.9%), COPD (11.6%), chronic kidney disease (8.2%), and anemia (6.6%), while alcohol abuse (1%) and current smoking (0.5%) were rare. Most procedures were performed in large hospitals (57.2%) and urban teaching facilities (82.4%). The geographic distribution showed a higher concentration in the South (36.5%) and Midwest (24.7%). Medicare was the primary payer for most cases (64.7%), followed by private insurance (23.2%). (
Table 1)
The median total hospital charges for total elbow arthroplasty (TEA) were
$78,473 (IQR:
$56,935–
$115,671
). The mean length of stay (LOS) was 2 days, reflecting a relatively short postoperative hospitalization period. (
Table 2)
In the multivariate analysis of complications following total elbow replacement (
Table 3), several significant associations were identified. Mechanical loosening was associated with younger age (OR 0.98 per year, 95% CI 0.97-1.00, p=0.045), hypertension (OR 2.49, 95% CI 1.48-4.21, p<0.001), and larger hospital size (OR 1.62, 95% CI 1.20-2.18, p=0.001). Medical complications showed distinct risk patterns: both urinary complications and heart complications were associated with increasing age (OR 1.07, p=0.001 and OR 1.08, p<0.001, respectively). Respiratory complications demonstrated strong associations with multiple factors, including sleep apnea (OR 7.44, 95% CI 2.91-19.05, p<0.001), chronic anemia (OR 10.68, 95% CI 3.24-35.17, p<0.001), and female sex (OR 5.85, 95% CI 1.22-28.21, p=0.027). Notably, chronic renal disease was a significant risk factor for both urinary tract infections (OR 4.37, 95% CI 1.22-15.70, p=0.024) and inflammatory complications (OR 4.93, 95% CI 1.30-18.67, p=0.019). Prosthetic pain showed a complex risk profile, with mental disorders (OR 2.67, 95% CI 1.19-6.01, p=0.017) and COPD (OR 2.93, 95% CI 1.09-7.84, p=0.032) increasing risk, while female sex was associated with lower risk (OR 0.32, 95% CI 0.14-0.77, p=0.010).
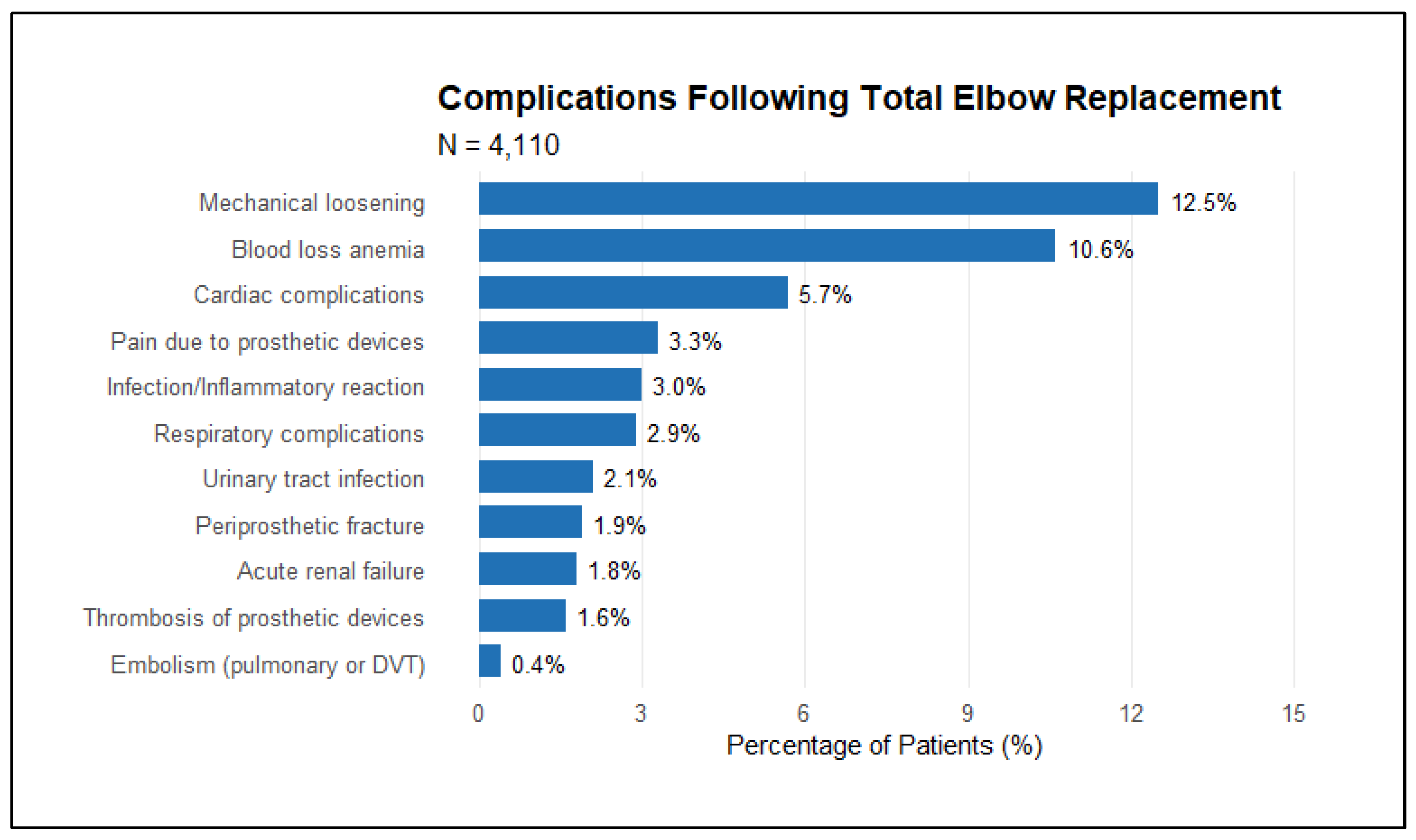
Figure 2.
– Postoperative Complications Total Elbow Replacement Patients.
Figure 2.
– Postoperative Complications Total Elbow Replacement Patients.
Discussion
This study provides a detailed analysis of total elbow arthroplasty (TEA) trends, demographics, and clinical outcomes using data from the Nationwide Inpatient Sample (2016–2019). It contextualizes TEA’s evolving role in orthopedic practice, with implications for patient management, surgical strategies, and healthcare resource allocation. Over the study period, a 16% reduction in annual TEA volume was observed, reflecting a significant shift in utilization patterns. This decline is largely attributed to the widespread use of disease-modifying antirheumatic drugs (DMARDs), which have mitigated joint destruction in rheumatoid arthritis. Historically, RA accounted for up to 80% of all TEA cases. However, global registry data indicate this proportion has dropped to under 15% (1,15,16). These findings affirm the success of biologics and combination DMARD therapies in reducing surgical interventions for inflammatory arthritis (7,17).
Simultaneously, trauma has become the leading indication for TEA, accounting for 40–50% of procedures globally (11,18,19). This shift represents a reorientation of surgical priorities, with TEA now preferred over open reduction-internal fixation (ORIF) for unreconstructable fractures in elderly osteoporotic patients. Evidence suggests TEA provides superior outcomes compared to ORIF in these populations, cementing its role as the definitive treatment for complex fractures (3,20). These trends demonstrate a broader redefinition of TEA’s utility within orthopedic surgery.
The demographic profile of TEA recipients reveals a predominance of older, White females, with a mean age of 65.99 years. This aligns with global trends, reflecting the higher prevalence of osteoporosis and fragility fractures among postmenopausal women (7,13). Such demographics highlight the need for tailored surgical and perioperative strategies to address challenges specific to this population. Mechanical loosening, a complication observed in 12.5% of cases in this study, remains a significant concern, particularly in elderly patients with fragile bone quality.
The COVID-19 pandemic disrupted TEA utilization dramatically, with procedural volumes halving in regions such as England and Australia in 2020 (16,19). Elective procedures were disproportionately affected, exacerbating delays in addressing both chronic arthropathies and acute fractures. These disruptions have highlighted existing disparities in healthcare access, particularly among socioeconomically disadvantaged populations. While procedural volumes are recovering, the long-term effects of these delays on patient outcomes require further investigation.
Institutional and surgical factors also significantly impact TEA outcomes. High-volume centers and experienced surgeons consistently report better results, underscoring the importance of procedural expertise and centralized care (7,15). However, a substantial proportion of surgeons perform fewer than five TEAs annually, raising concerns about variability in outcomes. Centralization initiatives in the U.K. and Australia aim to address this issue by consolidating TEA procedures within high-volume centers, improving consistency and outcomes (16,19).
Comorbidities emerged as critical determinants of TEA outcomes in this study. Hypertension, anemia, and respiratory conditions were identified as significant contributors to perioperative risks and postoperative complications, including mechanical loosening and infections. Poorly controlled RA and osteoporosis further exacerbated these risks, emphasizing the importance of preoperative optimization. Metabolic conditions, such as diabetes, were associated with systemic complications, including pneumonia and urinary tract infections, while cardiovascular diseases heightened risks of perioperative complications (21,22,23). These findings highlight the need for multidisciplinary care to optimize patient health prior to surgery.
Although our analysis included only primary total elbow arthroplasty (TEA), mechanical loosening emerged as the most frequently reported complication. However, this diagnosis cannot be accurately determined within the immediate postoperative period. This discrepancy may be attributed to miscoding during hospitalization, where the intended complication was likely prosthesis dislocation. Prosthesis dislocation is a recognized complication following TEA, though its reported incidence varies across studies. Ruth and Wilde documented a
6% dislocation rate in their study of capitellocondylar elbow replacements. Similarly, van der Lugt et al. reported a dislocation rate of
approximately 2% in Souter-Strathclyde total elbow prostheses, while Barco et al. observed a
4.5% dislocation rate in long-term follow-up of TEA for distal humeral fractures. Although prosthesis dislocation is not the most prevalent complication, these findings underscore its clinical significance in the postoperative management of TEA. [
24,
25,
26]
And since we mentioned mechanical loosening, it is still considered a common cause for revision surgeries particularly in younger, more active patients and those treated in high-volume centers (17, 19, 27). Blood loss anemia and cardiac complications also significantly impacted outcomes, underscoring the need for advanced perioperative management protocols. Trauma-related TEAs demonstrated higher complication rates than those performed for RA or osteoarthritis, reflecting the technical complexity and biological challenges of these cases (17,19). Future studies should explore surgical approaches, fixation techniques, and postoperative protocols to improve outcomes for trauma-related TEAs.
Infection, while less common than mechanical loosening, remains a significant cause of morbidity and revisions, accounting for 15–35% of revisions globally (25,26). Strategies such as antibiotic-laden cement and meticulous surgical techniques are critical to reducing infection rates. Nerve-related complications, though infrequent, are noteworthy, with the ulnar nerve particularly vulnerable during surgery (16,19).
Advances in prosthetic design have significantly influenced TEA outcomes. Linked prostheses, such as the Coonrad-Morrey and Nexel systems, remain the most widely used implants due to their superior stability and lower dislocation rates compared to unlinked designs. These systems achieve 10-year survivorship rates exceeding 80% (4,20,17). Unlinked prostheses, while offering greater range of motion, are associated with higher instability and revision rates, limiting their widespread adoption (17,19). Despite these advancements, persistent complications such as aseptic loosening and infection continue to challenge outcomes. Efforts to optimize implant design, cementation techniques, and surgical protocols are essential to mitigate these risks.
Our study has several notable strengths. First, it is the first analysis of total elbow arthroplasty (TEA) using the National Inpatient Sample (NIS) database, providing a nationally representative assessment of TEA utilization, complications, and outcomes. The inclusion of multiple years enhances the comprehensiveness of our dataset, ensuring a larger sample size than previous studies and improving the generalizability of findings. Second, we accounted for socioeconomic stratification and hospital characteristics, allowing for a more nuanced analysis of cost variations and healthcare resource utilization. By incorporating four years of data, we provide a broader overview of cost trends and length of stay, offering valuable insights into economic and institutional factors influencing TEA outcomes. Finally, this is the first study to analyze TEA outcomes using the ICD-10 coding system, ensuring relevance to contemporary clinical practice and healthcare reimbursement frameworks. This enhances the applicability of our findings and facilitates comparisons with future studies utilizing standardized coding methodologies.
This study has several limitations inherent to the use of the National Inpatient Sample (NIS) database in orthopedic surgery research. First, coding errors represent a significant challenge, as procedural and diagnostic codes rely on administrative data rather than direct clinical assessment. Misclassification, particularly between mechanical loosening and prosthesis dislocation, may lead to inaccuracies in complication rates. Second, the scope of hospitalization within NIS is limited to inpatient encounters, preventing analysis of outpatient or perioperative factors that may influence surgical outcomes. This restriction may underrepresent complications that do not manifest during the initial hospital stay or those managed in ambulatory settings. Third, the lack of long-term follow-up limits the ability to assess critical postoperative outcomes such as implant longevity, delayed infections, or late-onset mechanical failures. Without longitudinal patient data, conclusions regarding long-term TEA performance and survivorship remain incomplete.
In conclusion, this comprehensive analysis underscores the need for continued innovation and refinement in TEA practices. Standardizing cost evaluations, centralizing care for complex procedures, and addressing systemic disparities are critical to ensuring sustainable and effective utilization of TEA. Future research should focus on improving prosthetic design, optimizing perioperative care, and addressing demographic-specific needs to enhance outcomes and resource efficiency in this evolving field.
References
- Gay, D.M.; Lyman, S.; Do, H.; Hotchkiss, R.N.; Marx, R.G.; Daluiski, A. Indications and reoperation rates for total elbow arthroplasty: an analysis of trends in New York State. J Bone Joint Surg Am. 2012, 94, 110–117. [Google Scholar] [CrossRef] [PubMed]
- Shi, L.L.; Zurakowski, D.; Jones, D.G.; Koris, M.J.; Thornhill, T.S. Semiconstrained primary and revision total elbow arthroplasty with use of the Coonrad-Morrey prosthesis. J Bone Joint Surg Am. 2007, 89, 1467–1475. [Google Scholar] [CrossRef] [PubMed]
- Sørensen, B.W.; Brorson, S.; Olsen, B.S. Primary total elbow arthroplasty in complex fractures of the distal humerus. World J Orthop. 2014, 5, 368–372. [Google Scholar] [CrossRef] [PubMed]
- Day, J.S.; Lau, E.; Ong, K.L.; Williams, G.R.; Ramsey, M.L.; Kurtz, S.M. Prevalence and projections of total shoulder and elbow arthroplasty in the United States to 2015. J Shoulder Elbow Surg. 2010, 19, 1115–1120. [Google Scholar] [CrossRef]
- McKissack, H.; Karzon, A.R.; Hussain, Z.B.; Worden, J.A.; Heo, K.Y.; Cooke, H.L.; Ojimakinde, A.; Gottschalk, M.B.; Wagner, E.R. Is popularity of total elbow arthroplasty in the United States decreasing? An analysis of trends, demographics, and indications. JSES Rev Rep Tech. 2024, 4, 797–804. [Google Scholar]
- Korpela, M.; Laasonen, L.; Hannonen, P.; Kautiainen, H.; Leirisalo-Repo, M.; Hakala, M.; Paimela, L.; Blåfield, H.; Puolakka, K.; Möttönen, T.; FIN-RACo Trial Group. Retardation of joint damage in patients with early rheumatoid arthritis by initial aggressive treatment with disease-modifying antirheumatic drugs: five-year experience from the FIN-RACo study. Arthritis Rheum. 2004, 50, 2072–2081. [Google Scholar] [CrossRef] [PubMed]
- Zhou, H.; Orvets, N.D.; Merlin, G.; Shaw, J.; Dines, J.S.; Price, M.D.; Eichinger, J.K.; Li, X. Total Elbow Arthroplasty in the United States: Evaluation of Cost, Patient Demographics, and Complication Rates. Orthop Rev (Pavia). 2016, 8, 6113. [Google Scholar]
- Dafang Zhang, Brandon E. Earp, Philip Blazar, Factors associated with 30-day complication, reoperation, readmission, and length of stay after primary total elbow arthroplasty: a database study of 555 patients, Seminars in Arthroplasty: JSES, Volume 33, Issue 1, 2023, Pages 59-66. [CrossRef]
- Morrey, M.E.; Morrey, B.F.; Sanchez-Sotelo, J.; Barlow, J.D.; O'Driscoll, S. A review of the surgical management of distal humerus fractures and nonunions: From fixation to arthroplasty. J Clin Orthop Trauma. 2021, 20, 101477. [Google Scholar] [CrossRef] [PubMed]
- Polmear, M.M.; Scanaliato, J.P.; Rossettie, S.; Bader, J.; Nesti, L.J.; Dunn, J.C. Post-operative Immobilization in Total Elbow Arthroplasty for Rheumatoid Arthritis: A Systematic Review of Outcomes. J Surg Orthop Adv. 2022, 31, 209–217. [Google Scholar] [PubMed]
- Kim, J.M.; Mudgal, C.S.; Konopka, J.F.; Jupiter, J.B. Complications of total elbow arthroplasty. J Am Acad Orthop Surg. 2011, 19, 328–339. [Google Scholar] [CrossRef] [PubMed]
- Voloshin, I.; Schippert, D.W.; Kakar, S.; Kaye, E.K.; Morrey, B.F. Complications of total elbow replacement: a systematic review. J Shoulder Elbow Surg. 2011, 20, 158–168. [Google Scholar] [CrossRef]
- Dam, W.V.; Meijering, D.; Stevens, M.; Boerboom, A.L.; Eygendaal, D. Postoperative management of total elbow arthroplasty: Results of a European survey among orthopedic surgeons. PLoS One. 2022, 17, e0277662. [Google Scholar] [CrossRef] [PubMed]
- Prkic, A.; Welsink, C.; The, B.; van den Bekerom, M.P.J.; Eygendaal, D. Why does total elbow arthroplasty fail today? A systematic review of recent literature. Arch Orthop Trauma Surg. 2017, 137, 761–769. [Google Scholar] [CrossRef]
- Jenkins, P.J.; Watts, A.C.; Norwood, T.; Duckworth, A.D.; Rymaszewski, L.A.; McEachan, J.E. Total elbow replacement: outcome of 1,146 arthroplasties from the Scottish Arthroplasty Project. Acta Orthop. 2013, 84, 119–123. [Google Scholar] [CrossRef] [PubMed]
- Hamoodi, Z.; Sayers, A.; Whitehouse, M.R.; Rangan, A.; Kearsley-Fleet, L.; Sergeant, J.; Watts, A.C. Total elbow arthroplasty in England. Bone Joint J. 2024, 106-B, 1312–1320. [Google Scholar] [CrossRef] [PubMed]
- Tarallo, L.; Celli, A.; Delvecchio, M.; Costabile, L.; Ciacca, G.; Porcellini, G.; Catani, F. Long-term outcomes and trends in elbow arthroplasty with Coonrad-Morrey prosthesis: a retrospective study in large group of patients. Int Orthop. 2024, 48, 2689–2698. [Google Scholar] [CrossRef]
- Dehghan, N.; Furey, M.; Schemitsch, L.; Ristevski, B.; Goetz, T.; Schemitsch, E.H.; Canadian Orthopaedic Trauma Society (COTS); McKee, M. Long-term outcomes of total elbow arthroplasty for distal humeral fracture: results from a prior randomized clinical trial. J Shoulder Elbow Surg. 2019, 28, 2198–2204. [Google Scholar] [CrossRef]
- Viveen, J.; van den Bekerom, M.P.J.; Doornberg, J.N.; Hatton, A.; Page, R.; Koenraadt, K.L.M.; Wilson, C.; Bain, G.I.; Jaarsma, R.L.; Eygendaal, D. Use and outcome of 1,220 primary total elbow arthroplasties from the Australian Orthopaedic Association National Joint Arthroplasty Replacement Registry 2008-2018. Acta Orthop. 2019, 90, 511–516. [Google Scholar] [CrossRef]
- Zeltser, D.W.; Prentice, H.A.; Navarro, R.A.; Mirzayan, R.; Dillon, M.T.; Foroohar, A. Total Elbow Arthroplasty: A Descriptive Analysis of 170 Patients From a United States Integrated Health Care System. J Hand Surg Am. 2021, 46, 552–559. [Google Scholar] [CrossRef]
- Singh, J.A.; Ramachandran, R. Are there racial disparities in utilization and outcomes after total elbow arthroplasty? Rheumatol Int. 2015, 35, 1479–1487. [Google Scholar] [CrossRef]
- Toor, A.S.; Jiang, J.J.; Shi, L.L.; Koh, J.L. Comparison of perioperative complications after total elbow arthroplasty in patients with and without diabetes. J Shoulder Elbow Surg. 2014, 23, 1599–1606. [Google Scholar] [CrossRef] [PubMed]
- Lovy, A.J.; Keswani, A.; Dowdell, J.; Koehler, S.; Kim, J.; Hausman, M.R. Outcomes, complications, utilization trends, and risk factors for primary and revision total elbow replacement. J Shoulder Elbow Surg. 2016, 25, 1020–1026. [Google Scholar] [CrossRef] [PubMed]
- Ramirez, M.A.; Cheung, E.V.; Murthi, A.M. Revision Total Elbow Arthroplasty. J Am Acad Orthop Surg. 2017, 25, e166–e174. [Google Scholar] [CrossRef]
- Foster, B.K.; Ayalon, O.; Hoyer, R.; Hoyen, H.A.; Grandizio, L.C. Postoperative Elbow Instability: Options for Revision Stabilization. J Hand Surg Am. 2024, 49, 362–371. [Google Scholar] [CrossRef] [PubMed]
- Jupiter, J.B.; Ring, D. Treatment of unreduced elbow dislocations with hinged external fixation. J Bone Joint Surg Am. 2002, 84, 1630–1635. [Google Scholar] [CrossRef]
- Klug, A.; Gramlich, Y.; Buckup, J.; Schweigkofler, U.; Hoffmann, R.; Schmidt-Horlohé, K. Trends in total elbow arthroplasty: a nationwide analysis in Germany from 2005 to 2014. Int Orthop. 2018, 42, 883–889. [Google Scholar] [CrossRef] [PubMed]
Table 1.
– Patient Demographics and Characteristic of Total Elbow Replacement Patients.
Table 1.
– Patient Demographics and Characteristic of Total Elbow Replacement Patients.
| Characteristic |
N = 4,110 |
Age (years)
Mean (SD) |
65.99 (13.47) |
| Female |
619 (75.3%) |
| Race |
|
| White |
597 (72.6%) |
| Black |
55 (6.7%) |
| Hispanic |
85 (10.3%) |
| Asian |
15 (1.8%) |
| Others |
70 (8.5%) |
| Type 2 Diabetes |
160 (19.5%) |
| Hypertension |
422 (51.3%) |
| Dyslipidemia |
306 (37.2%) |
| Sleep Apnea |
106 (12.9%) |
| Chronic Anemia |
54 (6.6%) |
| Alcohol Abuse |
8 (1%) |
| Mental Disorders |
313 (38.1%) |
| Current Smoker |
4 (0.5%) |
| Chronic kidney Disease |
67 (8.2%) |
| COPD |
95 (11.6%) |
| Hospital Size |
|
| Small |
187 (22.7%) |
| Medium |
165 (20.1%) |
| Large |
470 (57.2%) |
| Geographic Region |
|
| Northeast |
134 (16.3%) |
| Midwest |
203 (24.7%) |
| South |
300 (36.5%) |
| West |
185 (22.5%) |
| Hospital Teaching Status |
|
| Rural |
105 (2.6) |
| Urban nonteaching |
620 (15.1)
|
| Urban teaching |
3385 (82.4)
|
| Primary Payer |
|
| Medicare |
532 (64.7%) |
| Medicaid |
46 (5.6%) |
| Private |
191 (23.2%) |
| other |
53 (6.4%) |
Table 2.
– Length of Stay and Total Charges of Total Elbow Replacement Patients.
Table 2.
– Length of Stay and Total Charges of Total Elbow Replacement Patients.
|
Length of Stay (days) Median [IQR] |
2 [1-3] |
Total Hospitalization Charges ($)
Median [IQR] |
78,473 [56,935-115,671] |
Table 3.
– Postoperative Complications Total Elbow Replacement Patients.
Table 3.
– Postoperative Complications Total Elbow Replacement Patients.
| Table 3. Postoperative Complications Following Total Elbow Replacement (N=4,110) |
|---|
| Complication |
% |
| Mechanical loosening |
12.5 |
| Blood loss anemia |
10.6 |
| Cardiac complications |
5.7 |
| Pain due to prosthetic devices |
3.3 |
| Infection/Inflammatory reaction |
3 |
| Respiratory complications |
2.9 |
| Urinary tract infection |
2.1 |
| Periprosthetic fracture |
1.9 |
| Acute renal failure |
1.8 |
| Thrombosis of prosthetic devices |
1.6 |
| Embolism (pulmonary or DVT) |
0.4 |
|
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).