Submitted:
09 January 2025
Posted:
09 January 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
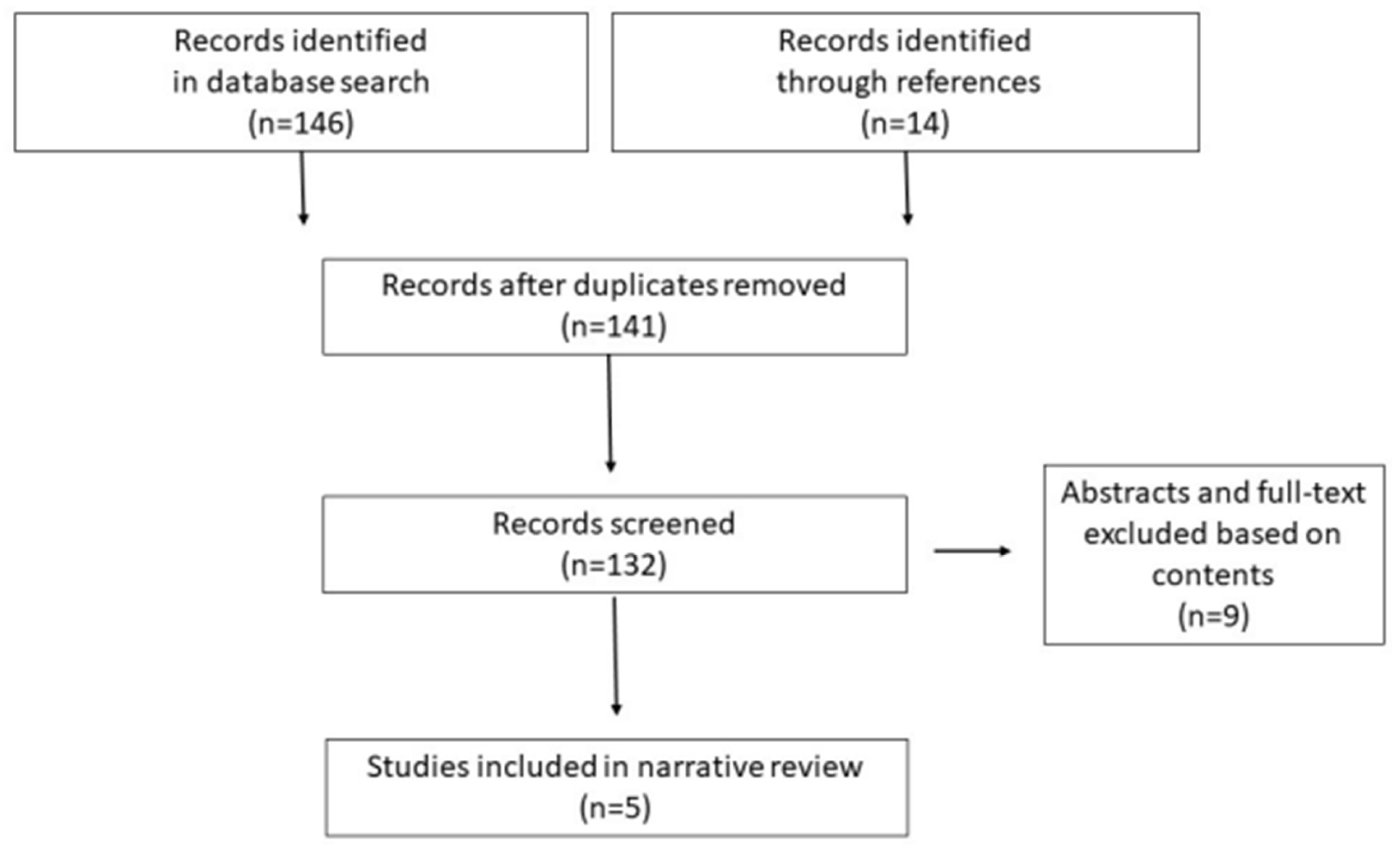
2. Study Design and Selection Criteria
3. Epidemiology and Etiology
4. Diagnosis and Imaging
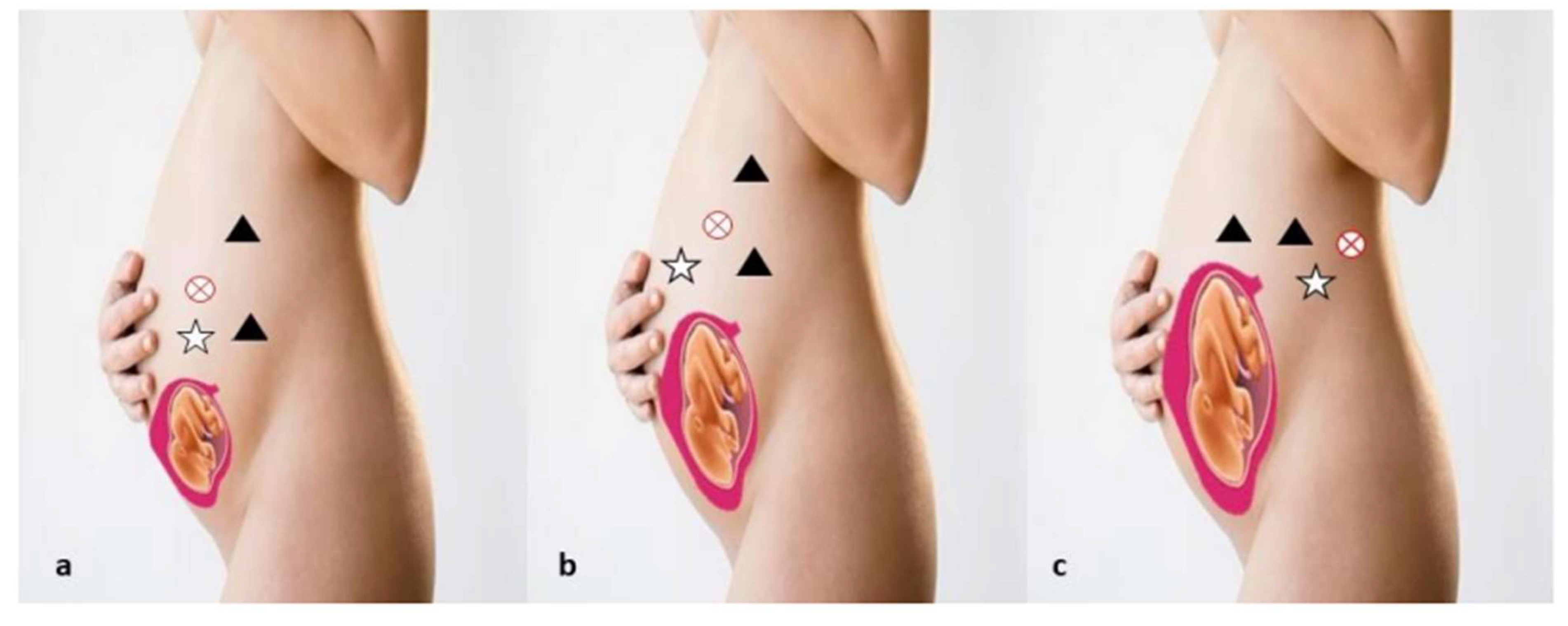
5. Robotic Management
6. Treatment Plan and Outcomes
Treatment of Metastatic Renal Tumors
7. Future Directions and Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Rajeev, S.; Brendan, B. Robot-assisted radical nephrectomy for renal-cell carcinoma during twin pregnancy. Urol Nephrol Open Access J. 2023, 11, 111–113. [Google Scholar]
- Xu, H.; Tan, S. Diagnosis and treatment of renal cell carcinoma during pregnancy. Cancer Manag Res. 2021, 13, 9423–9428. [Google Scholar] [CrossRef] [PubMed]
- Dell’Atti, L.; Borghi, C.; Galosi, AB. Laparoscopic approach in management of renal cell carcinoma during pregnancy: state of the art. Clin Genitourin Cancer 2019, 17, e822–830. [Google Scholar] [CrossRef]
- Palanivelu, C.; Rangarajan, M.; Senthilkumaran, S.; et al. Safety and efficacy of laparoscopic surgery in pregnancy: experience of a single institution. J Laparoendosc Adv Surg Tech A. 2017, 17, 186–190. [Google Scholar] [CrossRef] [PubMed]
- Ruiz Guerrero, E.; Claro, A.V.O.; Ledo Cepero, M.J.; Soto Delgado, M.; Álvarez-Ossorio Fernández, J.L. Robotic versus Laparoscopic Partial Nephrectomy in the New Era: Systematic Review. Cancers (Basel) 2023, 15, 1793. [Google Scholar] [CrossRef] [PubMed]
- Gettman, M.T.; Blute, M.L.; Chow, G.K.; Neururer, R.; Bartsch, G.; Peschel, R. Robotic-assisted laparoscopic partial nephrectomy: Technique and initial clinical ex-perience with daVinci robotic system. Urology 2004, 64, 914–918. [Google Scholar] [CrossRef] [PubMed]
- Haseebuddin, M.; Benway, B.M.; Cabello, J.M.; Bhayani, S.B. Robot- assisted partial nephrectomy: Evaluation of learning curve for an experienced renal surgeon. J. Endourol. 2010, 24, 57–61. [Google Scholar] [CrossRef]
- Wolters, V.; Heimovaara, J.; Maggen, C.; et al. Management of pregnancy in women with cancer. Int J. Gynecol Cancer 2021, 31, 314–322. [Google Scholar] [CrossRef]
- Kalampokas, E.; Vlahos, N.; Kalampokas, T.; Gurumurthy, M. Common Malignancies During Pregnancy: A Comprehensive Review. Cancer Diagn Progn. 2021, 1, 103–109. [Google Scholar] [CrossRef] [PubMed]
- Milosevic, B.; Likic Ladjevic, I.; Dotlic, J.; et al. Cancer during pregnancy: Twenty-two years of experience from a tertiary referral center. Acta Obstet Gynecol Scand. 2024, 103, 716–728. [Google Scholar] [CrossRef] [PubMed]
- Wang, C.; Li, X.; Peng, L.; Gou, X.; Fan, J. An update on recent developments in rupture of renal angiomyolipoma. Medicine (Baltimore). 2018, 97, e0497. [Google Scholar] [CrossRef]
- Chu, J.S.; Wang, Z.J. Protocol optimization for renal mass detection and characterization. Radiol Clin North Am. 2020, 58, 851–873. [Google Scholar] [CrossRef] [PubMed]
- Khazzaka, A.; Rassy, E. , Sleiman, Z. ; Boussios, S.; Pavlidis, N. Systematic review of fetal and placental metastases among pregnant patients with cancer. Cancer Treat Rev. 2022, 104, 102356. [Google Scholar]
- Caglayan, A.; Rabbani, RD.; Sanchez, E.; et al. Gestational Renal Cell Cancer- An Update. Anticancer Res. 2023, 43, 3871–3880. [Google Scholar] [CrossRef] [PubMed]
- Lambe, M.; Lindblad, P.; Wuu, J.; Remler, R.; Hsieh, C.C. Pregnancy and risk of renal cell cancer: a population-based study in Sweden. Br J Cancer, 2002, 86, 1425–1429. [Google Scholar] [CrossRef] [PubMed]
- Macleod, L.C.; Hotaling, J.M.; Wright, J.L.; et al. Risk factors for renal cell carcinoma in the VITAL study. J Urol. 2013, 190, 1657–1661. [Google Scholar] [CrossRef] [PubMed]
- Bergström, A.; Hsieh, C.C.; Lindblad, P.; Lu, C.M.; Cook, N.R.; Wolk, A. Obesity and renal cell cancer – a quantitative review. Br J Cancer 2001, 85, 984–990. [Google Scholar] [CrossRef] [PubMed]
- Schouten, L.J.; Van De Pol, J.; Kviatkovsky, M.J. , Van Den Brandt, P. A. Reproductive and external hormonal factors and the risk of renal cell cancer in the Netherlands Cohort Study. Cancer Epidemiol. 2022, 79, 102171. [Google Scholar] [PubMed]
- Aurilio, G.; Piva, F.; Santoni, M.; et al. The role of obesity in renal cell carcinoma patients: clinical pathological implications. Int J Mol Sci. 2019, 20, 5683. [Google Scholar] [CrossRef]
- Padala, S.A.; Barsouk, A.; Thandra, K.C.; et al. Epidemiology of renal cell carcinoma. World J Oncol. 2020, 11, 79–87. [Google Scholar] [CrossRef] [PubMed]
- Deckers, I.A.; Van Den Brandt, P.A.; Van Engeland, M.; et al. Polymorphisms in genes of the renin-angiotensin-aldosterone system and renal cell cancer risk: Interplay with hypertension and intakes of sodium, potassium and fluid. Int J Cancer 2015, 136, 1104–1116. [Google Scholar] [CrossRef]
- Yilmaz, E.; Oguz, F.; Tuncay, G.; et al. Renal cell carcinoma diagnosed during pregnancy: a case report and literature review. J Int Med Res. 2018, 46, 3422–3426. [Google Scholar] [CrossRef] [PubMed]
- Bettez, M.; Carmel, M. , Temmar, R. et al. Fatal fast-growing renal cell carcinoma during pregnancy. J Obstet Gynaecol Can. 2011, 33, 258–261. [Google Scholar]
- Casella, R.; Ferrier, C.; Giudici, G.; et al. Surgical management of renal cell carcinoma during the second trimester of pregnancy. Urol Int. 2006, 76, 180–181. [Google Scholar] [CrossRef] [PubMed]
- Bourgioti C, Konidari M, Gourtsoyianni S, Moulopoulos LA. Imaging during pregnancy: What the radiologist needs to know. Diagn Interv Imaging. 2021, 102, 593–603.
- Tremblay, E.; Thérasse, E.; Thomassin-Naggara, I.; Trop, I. Quality initiatives: guidelines for use of medical imaging during pregnancy and lactation. Radiographics 2012, 32, 897–911. [Google Scholar] [CrossRef] [PubMed]
- Gjelsteen, A.C.; Ching, B.H.; Meyermann, M.W.; et al. CT, MRI, PET, PET/CT, and ultrasound in the evaluation of obstetric and gynecologic patients. Surg Clin North Am. 2008, 88, 361–390. [Google Scholar] [CrossRef]
- Chen, J.; Lee, R.J.; Tsodikov, A.; Smith, L.; Gaffney, D.K. Does radiotherapy around the time of pregnancy for Hodgkin's disease modify the risk of breast cancer? Int J Radiat Oncol Biol Phys. 2004, 58, 1474–1479. [Google Scholar] [CrossRef]
- Goldberg-Stein, S.; Liu, B.; Hahn, P.F.; Lee, S.I. Body CT during pregnancy: utilization trends, examination indications, and fetal radiation doses. AJR Am J Roentgenol. 2011, 196, 146–151. [Google Scholar] [CrossRef] [PubMed]
- Kelaranta, A.; Mäkelä, T.; Kaasalainen, T.; Kortesniemi, M. Fetal radiation dose in three common CT examinations during pregnancy: Monte Carlo study. Phys Med. 2017, 43, 199–206. [Google Scholar] [CrossRef] [PubMed]
- Angel, E.; Wellnitz, C.V.; Goodsitt, M.M.; et al. Radiation dose to the fetus for pregnant patients undergoing multidetector CT imaging: Monte Carlo simulations estimating fetal dose for a range of gestational age and patient size. Radiology 2008, 249, 220–227. [Google Scholar] [CrossRef]
- Han, S.N.; Amant, F.; Michielsen, K.; et al. Feasibility of whole-body diffusion-weighted MRI for detection of primary tumour, nodal and distant metastases in women with cancer during pregnancy: a pilot study. Eur Radiol. 2018, 28, 1862–1874. [Google Scholar] [CrossRef]
- Khochikar, M.V. Management of urological cancers during pregnancy. Nat Rev Urol. 2010, 7, 195–205. [Google Scholar] [CrossRef]
- Moguel González, B.; Garcia Nava, M.; Orozco Guillén, O.A.; et al. Kidney biopsy during pregnancy: a difficult decision. A case series reporting on 20 patients from Mexico. J Nephrol. 2022, 35, 2293–2300. [Google Scholar]
- Ghorbani, H. ; Mottaghi,M.; Soltani, S. Renal Tumors in Pregnancy: A Case Report Focusing on the Timing of the Surgery and Patient Positioning. Case Rep Obstet Gynecol. 2022, 1143478. [Google Scholar]
- Guerre, M.; Boehnlein, C.; Sohaey, R.; Seideman, C.A. Imaging of Prenatal and Neonatal Intra-abdominal Genitourinary Tumors: a Review of the Literature. Curr Urol Rep. 2022, 23, 39–46. [Google Scholar] [CrossRef]
- Loughlin, K. The management of urological malignancies during pregnancy. Br J Urol. 1995, 76, 639–644. [Google Scholar] [CrossRef]
- Akpayak, I.; Shuiabu, S.; Ofoha, C.; Dakum, N.; Ramyil, V. Renal cell carcinoma in pregnancy: Still a management challenge. Afr J Urol. 2015, 21, 167–170. [Google Scholar] [CrossRef]
- Bettez, M.; Carmel, M.; Temmar, R.; et al. Fatal fast-growing renal cell carcinoma during pregnancy. J Obstet Gynaecol Can. 2011, 33, 258–261. [Google Scholar] [CrossRef]
- Wiles, R.; Hankinson, B.; Benbow, E.; Sharp, A. Making decisions about radiological imaging in pregnancy. BMJ. 2022, 377, e070486. [Google Scholar] [CrossRef]
- Capella, C.E.; Godovchik, J.; Chandrasekar, T.; Al-Kouatly, H.B. Nonobstetrical Robotic-Assisted Laparoscopic Surgery in Pregnancy: A Systematic Literature Review. Urology. 2021, 151, 58–66. [Google Scholar] [CrossRef]
- Park, S.Y.; Ham, WS.; Jung, H.J.; et al. Robot-assisted laparoscopic partial nephrectomy during pregnancy. J Robot Surg. 2008, 2, 193. [Google Scholar] [CrossRef]
- Ramirez, D.; Maurice, M.J.; Seager, C.; Haber, G.P. Robotic Partial Nephrectomy during Pregnancy: Case Report and Special Considerations. Urology 2016, 92, 1–5. [Google Scholar] [CrossRef]
- Völler, M.; Mahmud, W.; Vallo, S.; Grabbert, M.; John, P.; Khoder, W.Y. A 27-Year-Old Primigravida with a Right Renal Cell Carcinoma Removed at 30 Weeks of Gestation by Robot-Assisted Retroperitoneoscopic Partial Nephrectomy. Am J Case Rep. 2021, 22, e927164. [Google Scholar] [CrossRef]
- Tsutsui, K.; Miki, A.; Wakita, T.; et al. A case of robot-assisted laparoscopic partial nephrectomy during pregnancy. IJU Case Rep. 2023, 6, 458–460. [Google Scholar] [CrossRef]
- Dong, J.; Zhao, Y.; Xu, W. Case report: Retroperitoneal laparoscopic partial nephrectomy for T2 renal cell carcinoma during pregnancy. Front Oncol. 2020, 10, 552228. [Google Scholar] [CrossRef]
- Zhao, Y.; Yang, Z.; Xu, W.; Ji, Z.; Dong, J. Management of renal tumors during pregnancy: case reports. BMC Nephrol. 2021, 22, 127. [Google Scholar] [CrossRef]
- Kumar, S.S.; Collings, A.T.; Wunker, C.; et al. SAGES guidelines for the use of laparoscopy during pregnancy. Surg Endosc. 2024, 38, 2947–2963. [Google Scholar] [CrossRef]
- Ye, P.; Zhao, N.; Shu, J.; Shen, H.; et al. Laparoscopy versus open surgery for adnexal masses in pregnancy: a meta-analytic review. Arch Gynecol Obstet. 2019, 299, 625–634. [Google Scholar] [CrossRef]
- Lee, D.; Abraham, N. Laparoscopic radical nephrectomy during pregnancy: case report and review of the literature. J Endourol. 2008, 22, 517–518. [Google Scholar] [CrossRef]
- Berczi C, Flasko T. Renal Tumor in Pregnancy: A Case Report and Review of the Literature. Urol Int. 2017, 99, 367–369.
- Amant, F.; Berveiller, P.; Boere, I.A.; et al. Gynecologic cancers in pregnancy: guidelines based on a third international consensus meeting. Ann Oncol. 2019, 30, 1601–1612. [Google Scholar] [CrossRef]
- Wolters, V.; Heimovaara, J.; Maggen, C.; et al. Management of pregnancy in women with cancer. Int J Gynecol Cancer. 2021, 31, 314–322. [Google Scholar] [CrossRef]
- Ohyama, T.; Shimbo, M.; Endo, F.; et al. Renal cell carcinoma treatment during pregnancy: Histopathological findings suggestive of rapid tumor growth. IJU Case Rep. 2019, 2, 265–268. [Google Scholar] [CrossRef]
- Dey, S.; Pakrasi, R.; Saha, D.; Datta, S. Rapidly progressive growth of Renal Clear Cell Carcinoma and Gastrointestinal Stromal Tumor during the 3rd trimester of pregnancy: A clinical and diagnostic dilemma. Urol Case Rep. 2021, 40, 101891. [Google Scholar] [CrossRef]
- Zambrana, F.; Barbancho, C.; Huelves, M.; et al. Successful Pregnancy and Cancer Outcomes With Ipilimumab and Nivolumab for Metastatic Renal Cell Carcinoma: Case Report and Review of the Literature. J Immunother. 2023, 46, 27–28. [Google Scholar] [CrossRef]
- Campbell, S.C.; Uzzo, R.G.; Karam, J.A.; et al. Renal Mass and Localized Renal Cancer: Evaluation, Management, and Follow-up: AUA Guideline: Part II. J Urol. 2021, 206, 209–218. [Google Scholar] [CrossRef]
- Dai K, Jiang W, Chen S, Luo S, Ding S, Wang D. Case report: Going through pregnancy safely after twice partial nephrectomy for bilateral kidneys with HLRCC-associated RCC. Front Oncol. 2022, 12, 932996.
- Xu, H.; Tan, S. Diagnosis and Treatment of Renal Cell Carcinoma During Pregnancy. Cancer Manag Res. 2021, 13, 9423–9428. [Google Scholar] [CrossRef]
- Goebell, P.J.; Ivanyi, P.; Bedke, J.; et al. Consensus paper: current state of first- and second-line therapy in advanced clear-cell renal cell carcinoma. Future Oncol. 2020, 16, 2307–2328. [Google Scholar] [CrossRef]
- Yazigi, A.; Lecointe-Artzner, E.; Cesne, A.L.; et al. Pregnancy in Women with Metastatic Sarcomas. Oncologist. 2020, 25, e2010–e2012. [Google Scholar] [CrossRef]
- Khaled, H.; Lahloubi, N.A.; Rashad, N. Review on renal cell carcinoma and pregnancy: a challenging situation. J Adv Res. 2016, 7, 575–580. [Google Scholar] [CrossRef]
- Chys, B.; Dumont, S.; Van Calsteren, K.; et al. Renal neoplasm during pregnancy: a single center experience. Clin Genitourin Cancer. 2018, 16, e501–e507. [Google Scholar] [CrossRef] [PubMed]
- Boere, I.; Lok, C.; Vandenbroucke, T.; et al. Cancer in pregnancy: safety and efficacy of systemic therapies. Curr Opin Oncol. 2017, 29, 328–334. [Google Scholar] [CrossRef] [PubMed]
| Study |
Park SY et al.42 |
Ramirez D et al. 43 |
Völler M et al.44 |
Tsutsui K et al.48 |
Rajeev S =et al.1 |
| Patients, n. | 1 | 1 | 1 | 1 | 1 |
| Age, y | 36 | 35 | 27 | 36 | 23 |
| Age of gestation at diagnosis | 14 th w | 20 th w | 30 th w | 15 th w | 8 th w |
| Staging Imaging | MRI | MRI | MRI | CT | CT |
| Kidney Side | Left | Right | Right | Left | Left |
| Kidney Localization | Middle portion | Upper pole | Lower pole | Upper pole | Lower pole |
| Renal biopsy | No | No | No | No | Yes |
| Pathologic stage | T1a | T1b | T1b | T1a | T2a |
| Treatment | PN | PN | PN | PN | RN |
| Surgical approach | T | T | R | T | T |
| Histologic findings | RCC | RCC | CRCC | RCC | CRCC |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




