Submitted:
31 December 2024
Posted:
03 January 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
- Age <20 years or >70 years.
- Known diabetes or fasting glucose levels >126 mg/dL.
- Pregnancy.
- Systemic or ocular diseases (e.g., glaucoma, uveitis, high myopia, macular degeneration) or a history of ocular surgeries potentially causing retinal or choroidal damage.
- Nephroparenchymal, renovascular, malignant, or endocrine hypertension, or obstructive sleep apnea syndrome.
- Hereditary or non-hereditary kidney diseases, nephritic syndrome, or overt proteinuria/hematuria.
- Estimated glomerular filtration rate (eGFR) <15 mL/min/1.73 m² or renal replacement therapy (transplant or dialysis).
- Rapid decline in renal function, defined as a >25% reduction in eGFR or a >1.5-fold increase in serum creatinine levels from baseline[16].
- Poor-quality ultrasound imaging or abnormal renal morphology, as previously described[6].
- History or clinical evidence of heart failure (NYHA class II–IV), coronary artery disease, or cerebrovascular disease.
- Major non-cardiovascular conditions (e.g., liver cirrhosis, chronic obstructive pulmonary disease, or a history of malignancies).
- Conditions interfering with reliable blood pressure (BP) measurements using the oscillometric technique, such as atrial fibrillation, frequent ectopic beats, or second/third-degree atrioventricular blocks.
- Routine biochemical evaluations.
- 24-hour ambulatory brachial blood pressure monitoring (ABPM) using an oscillometric BP Lab Vasotens device.
- Optical Coherence Tomography Angiography (OCT-A).
- Renal Doppler ultrasound.
- 3D 7×7H Scan
- Macular Radial 6.0 Scan
- Angio-OCT 4.5 Scan
Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Conflicts of Interest
References
- «Structure and function of small arteries - PubMed». Consultato: 31 dicembre 2024. [Online]. Disponibile su: https://pubmed.ncbi.nlm.nih.gov/2217559/.
- C. W. Wong, T. Y. Wong, C.-Y. Cheng, e C. Sabanayagam, «Kidney and eye diseases: common risk factors, etiological mechanisms, and pathways», Kidney International, vol. 85, fasc. 6, pp. 1290–1302, giu. 2014. [CrossRef]
- A. S. Izzard, D. Rizzoni, E. Agabiti-Rosei, e A. M. Heagerty, «Small artery structure and hypertension: adaptive changes and target organ damage», J Hypertens, vol. 23, fasc. 2, pp. 247–250, feb. 2005. [CrossRef]
- U. Raff, T. K. Schwarz, B. M. W. Schmidt, M. P. Schneider, e R. E. Schmieder, «Renal resistive index--a valid tool to assess renal endothelial function in humans?», Nephrol Dial Transplant, vol. 25, fasc. 6, pp. 1869–1874, giu. 2010. [CrossRef]
- Y. Doi et al., «Association of renal resistive index with target organ damage in essential hypertension», Am J Hypertens, vol. 25, fasc. 12, pp. 1292–1298, dic. 2012. [CrossRef]
- «Geraci: Renal haemodynamics and severity of carotid... - Google Scholar». Consultato: 31 dicembre 2024. [Online]. Disponibile su: https://scholar.google.com/scholar_lookup?hl=en&volume=25&publication_year=2015&pages=160-166&journal=Nutr+Metab+Cardiovasc+Dis&issue=2&author=G+Geraci&author=G+Mul%C3%A8&author=M+Mogavero&title=Renal+haemodynamics+and+severity+of+carotid+atherosclerosis+in+hypertensive+patients+with+and+without+impaired+renal+function.
- M. M. Schwartz, E. J. Lewis, T. Leonard-Martin, J. B. Lewis, e D. Batlle, «Renal pathology patterns in type II diabetes mellitus: relationship with retinopathy. The Collaborative Study Group», Nephrol Dial Transplant, vol. 13, fasc. 10, pp. 2547–2552, ott. 1998. [CrossRef]
- «Mule: Retinal vascular imaging in cardiovascular... - Google Scholar». Consultato: 31 dicembre 2024. [Online]. Disponibile su: https://scholar.google.com/scholar_lookup?&title=Retinal%20vascular%20imaging%20in%20cardiovascular%20medicine%3A%20new%20tools%20for%20an%20old%20examination&journal=Atherosclerosis&doi=10.1016%2Fj.atherosclerosis.2017.11.001&volume=268&pages=188-90&publication_year=2018&author=Mul%C3%A8%2CG&author=Vadal%C3%A0%2CM&author=Geraci%2CG&author=Cottone%2CS.
- «Cheung: Retinal microvasculature as a model to study... - Google Scholar». Consultato: 31 dicembre 2024. [Online]. Disponibile su: https://scholar.google.com/scholar_lookup?&title=Retinal%20microvasculature%20as%20a%20model%20to%20study%20the%20manifestations%20of%20hypertension&journal=Hypertension&doi=10.1161%2FHYPERTENSIONAHA.111.189142&volume=60&pages=1094-103&publication_year=2012&author=Cheung%2CCYL&author=Ikram%2CMK&author=Sabanayagam%2CC&author=Wong%2CTY.
- S. K. Sharma et al., «Prognostic Role of Measurement of Renal Resistive Index in Systemic Sclerosis», Mediterr J Rheumatol, vol. 32, fasc. 4, pp. 345–349, dic. 2021. [CrossRef]
- A. Lubas, G. Kade, e S. Niemczyk, «Renal resistive index as a marker of vascular damage in cardiovascular diseases», Int Urol Nephrol, vol. 46, fasc. 2, pp. 395–402, 2014. [CrossRef]
- J. Radermacher, S. Ellis, e H. Haller, «Renal Resistance Index and Progression of Renal Disease», Hypertension, vol. 39, fasc. 2, pp. 699–703, feb. 2002. [CrossRef]
- J. A. Chirinos, P. Segers, T. Hughes, e R. Townsend, «Large Artery Stiffness in Health and Disease: JACC State-of-the-Art Review», J Am Coll Cardiol, vol. 74, fasc. 9, pp. 1237–1263, set. 2019. [CrossRef]
- S. Laurent e P. Boutouyrie, «Arterial stiffness: a new surrogate end point for cardiovascular disease», J Nephrol, vol. 20 Suppl 12, pp. S45-50, nov. 2007.
- P. I. Georgianos, P. A. Sarafidis, e A. N. Lasaridis, «Arterial Stiffness: A Novel Cardiovascular Risk Factor in Kidney Disease Patients», Current Vascular Pharmacology, vol. 13, fasc. 2, pp. 229–238, gen. 2015.
- R. Bellomo, C. Ronco, J. A. Kellum, R. L. Mehta, P. Palevsky, e Acute Dialysis Quality Initiative workgroup, «Acute renal failure - definition, outcome measures, animal models, fluid therapy and information technology needs: the Second International Consensus Conference of the Acute Dialysis Quality Initiative (ADQI) Group», Crit Care, vol. 8, fasc. 4, pp. R204-212, ago. 2004. [CrossRef]
- G. Mancia et al., «2023 ESH Guidelines for the management of arterial hypertension The Task Force for the management of arterial hypertension of the European Society of Hypertension: Endorsed by the International Society of Hypertension (ISH) and the European Renal Association (ERA)», Journal of Hypertension, vol. 41, fasc. 12, pp. 1874–2071, dic. 2023. [CrossRef]
- «Early Treatment Diabetic Retinopathy Study design and baseline patient characteristics. ETDRS report number 7», Ophthalmology, vol. 98, fasc. 5 Suppl, pp. 741–756, mag. 1991. [CrossRef]
- «N-Terminal Pro-Brain Natriuretic Peptide, C-Reactive Protein, and Urinary Albumin Levels as Predictors of Mortality and Cardiovascular Events in Older Adults | Acute Coronary Syndromes | JAMA | JAMA Network». Consultato: 31 dicembre 2024. [Online]. Disponibile su: https://jamanetwork.com/journals/jama/fullarticle/200640.
- «Increased renal resistive index in patients with essential hypertension: a marker of target organ damage. | Nephrology Dialysis Transplantation | Oxford Academic». Consultato: 31 dicembre 2024. [Online]. Disponibile su: https://academic.oup.com/ndt/article-abstract/14/2/360/1832953.
- S. Sezer, S. Karakan, T. Çolak, e M. Haberal, «Nocturnal Nondipping Hypertension Is Related to Dyslipidemia and Increased Renal Resistivity Index in Renal Transplant Patients», Transplantation Proceedings, vol. 43, fasc. 2, pp. 530–532, mar. 2011. [CrossRef]
- «Clinical Usefulness of Duplex Ultrasonography for the Assessment of Renal Arteriosclerosis in Essential Hypertensive Patients». Consultato: 31 dicembre 2024. [Online]. Disponibile su: https://www.jstage.jst.go.jp/article/hypres/24/1/24_1_13/_article/-char/ja/.
- «Central Pulse Pressure and Aortic Stiffness Determine Renal Hemodynamics | Hypertension». Consultato: 31 dicembre 2024. [Online]. Disponibile su: https://www.ahajournals.org/doi/full/10.1161/HYPERTENSIONAHA.111.177469.
- J. P. Campbell et al., «Detailed Vascular Anatomy of the Human Retina by Projection-Resolved Optical Coherence Tomography Angiography», Sci Rep, vol. 7, fasc. 1, p. 42201, feb. 2017. [CrossRef]
- G. Mule et al., «Association between early-stage chronic kidney disease and reduced choroidal thickness in essential hypertensive patients», Hypertension Research, vol. 42, gen. 2019. [CrossRef]
- «Impact of systemic vascular risk factors on the choriocapillaris using optical coherence tomography angiography in patients with systemic hypertension | Scientific Reports». Consultato: 31 dicembre 2024. [Online]. Disponibile su: https://www.nature.com/articles/s41598-019-41917-4.
- «Optical coherence tomography angiography changes in cardiovascular systemic diseases and risk factors: A Review - Monteiro-Henriques - 2022 - Acta Ophthalmologica - Wiley Online Library». Consultato: 31 dicembre 2024. [Online]. Disponibile su: https://onlinelibrary.wiley.com/doi/full/10.1111/aos.14851.
- C. Sun et al., «Systemic hypertension associated retinal microvascular changes can be detected with optical coherence tomography angiography», Sci Rep, vol. 10, fasc. 1, p. 9580, giu. 2020. [CrossRef]
- «Use of optical coherence tomography angiography for assessment of microvascular changes in the macula and optic nerve head in hypertensive patients without hypertensive retinopathy - ScienceDirect». Consultato: 31 dicembre 2024. [Online]. Disponibile su: https://www.sciencedirect.com/science/article/pii/S0026286219301943.
- «Tan: The application of optical coherence tomography... - Google Scholar». Consultato: 31 dicembre 2024. [Online]. Disponibile su: https://scholar.google.com/scholar_lookup?journal=Front.%20Med.&title=The%20Application%20of%20Optical%20Coherence%20Tomography%20Angiography%20in%20Systemic%20Hypertension:%20A%20Meta-Analysis&author=W.%20Tan&author=X.%20Yao&author=T.-T.%20Le&author=A.C.S.%20Tan&author=C.Y.%20Cheung&volume=8&publication_year=2021&pmid=34859021&doi=10.3389/fmed.2021.778330&.
- G. Mulè et al., «Relationship of choroidal thickness with pulsatile hemodynamics in essential hypertensive patients», J Clin Hypertens (Greenwich), vol. 23, fasc. 5, pp. 1030–1038, mag. 2021. [CrossRef]
- «Retinal capillary rarefaction is associated with arterial and kidney damage in hypertension | Scientific Reports». Consultato: 31 dicembre 2024. [Online]. Disponibile su: https://www.nature.com/articles/s41598-020-79594-3.
- «Relationship Between Carotid Atherosclerosis and Pulse Pressure with Renal Hemodynamics in Hypertensive Patients | American Journal of Hypertension | Oxford Academic». Consultato: 31 dicembre 2024. [Online]. Disponibile su: https://academic.oup.com/ajh/article-abstract/29/4/519/2622367.
| TOTAL | RRI<75 pct | RRI>75 pct | p | |
|---|---|---|---|---|
| Age, y | 48±13 | 48±12 | 52±14 | ns1 |
| Male sex (%) | 79 | 78 | 83 | ns |
| BMI (kg/m2) | 28±4.6 | 27.5±4.6 | 29.4±4.5 | ns |
| Waist circumference (cm) | 96±13 | 96±13 | 99±12 | ns |
| Smokers (%) | 22.2 | 17.4 | 38.9 | 0.054 |
| eGFR (mL/min/1.73 m²) | 87±20 | 90±19 | 76±24 | 0.018 |
| Urinary albumin excretion (mg/day) | 76 (31-252) | 36 (30-86) | 387(126-646) | 0.009 |
| Total Cholesterol (mg/dL) | 194±29 | 196±29 | 186±26 | ns |
| HDL-Cholesterol (mg/dL) | 48±12 | 49±12 | 45±9 | ns |
| Tryglicerides(mg/dL) | 118 (75-154) | 106 (89-131) | 122 (80-165) | 0.02 |
| Blood glucose (mg/dL) | 96±17 | 96±18 | 97±14 | ns |
| TOTAL | RRI<75 pct | RRI>75 pct | p | |
|---|---|---|---|---|
| Pharmacologically treated hypertensive subjects | 67.1 | 69.4 | 58.8 | ns1 |
| Antihypertensive drugs | ||||
| Angiotensin-converting enzyme (ACE) inhibitors,% | 29.1 | 27.4 | 35.3 | ns |
| Sartans, % | 37.9 | 40.3 | 29.4 | ns |
| Calcium channel blockers, % | 35.4 | 38.7 | 23.5 | ns |
| Alpha-2 Adrenergic Receptor Agonists, % | 7.6 | 3.2 | 23.5 | 0.005 |
| α – Blockers,% | 27.8 | 29 | 23.6 | ns |
| α β-blockers,% | 12.7 | 12.9 | 11.8 | ns |
| β-blockers,% | 12.7 | 14.5 | 5.8 | ns |
| Diuretics % | 35.4 | 33.9 | 41.2 | ns |
| Other cardiovascular agents | ||||
| Statins, % | 11.4 | 9.7 | 17.6 | ns |
| Antiplatelet agents, % | 25.3 | 29 | 11.8 | ns |
| Allopurinol, % | 6.3 | 4.8 | 11.8 | ns |
| TOTAL | RRI<75 pct | RRI>75 pct | p | |
|---|---|---|---|---|
| Clinic SBP (mmHg) | 137±12 | 137±13 | 136±11 | ns |
| Clinic DBP (mmHg) | 86±9 | 87±9 | 85±9 | ns |
| Clinic PP (mmHg) | 51±9 | 50±9 | 52±12 | ns |
| Heart Rate (bpm) | 73±11 | 74±12 | 72±11 | ns |
| Mean 24-h SBP (mmHg) | 130±13 | 133±13 | 138±13 | ns |
| Mean 24-h DBP (mmHg) | 82±9 | 83±9 | 82±9 | ns |
| 24-h PP (mmHg) | 47±10 | 45±10 | 52±9 | 0.013 |
| Daytime SBP (mmHg) | 134±13 | 129±13 | 134±13 | ns |
| Daytime DBP (mmHg) | 85±9 | 86±10 | 85±9 | ns |
| Daytime PP (mmHg) | 48±11 | 47±11 | 54±9 | 0.038 |
| Nighttime SBP (mmHg) | 119±14 | 117±13 | 126±15 | 0.03 |
| Nighttime DBP (mmHg) | 75±10 | 75±10 | 75±10 | ns |
| Nighttime PP (mmHg) | 44±10 | 43±9 | 51±10 | 0.001 |
| TOTAL | RRI<75 pct | RRI>75 pct | p | P* | |
|---|---|---|---|---|---|
| Parafoveal Vascular Plexus Density (%) – Superficial Layer | 37.3±0.87 | 37.4±0.84 | 36.9±0.89 | 0.053 | ns |
| Parafoveal Vascular Plexus Density (%) – Deep Layer | 38.3±1.08 | 38.3±1.06 | 38.3±1.19 | 0.956 | ns |
|
Foveal Vascular Density (%) –Superficial Layer |
34.5±1.88 | 34.7±1.69 | 33.7±2.34 | 0.147 | ns |
|
Foveal Vascular Density (%) –Deep Layer |
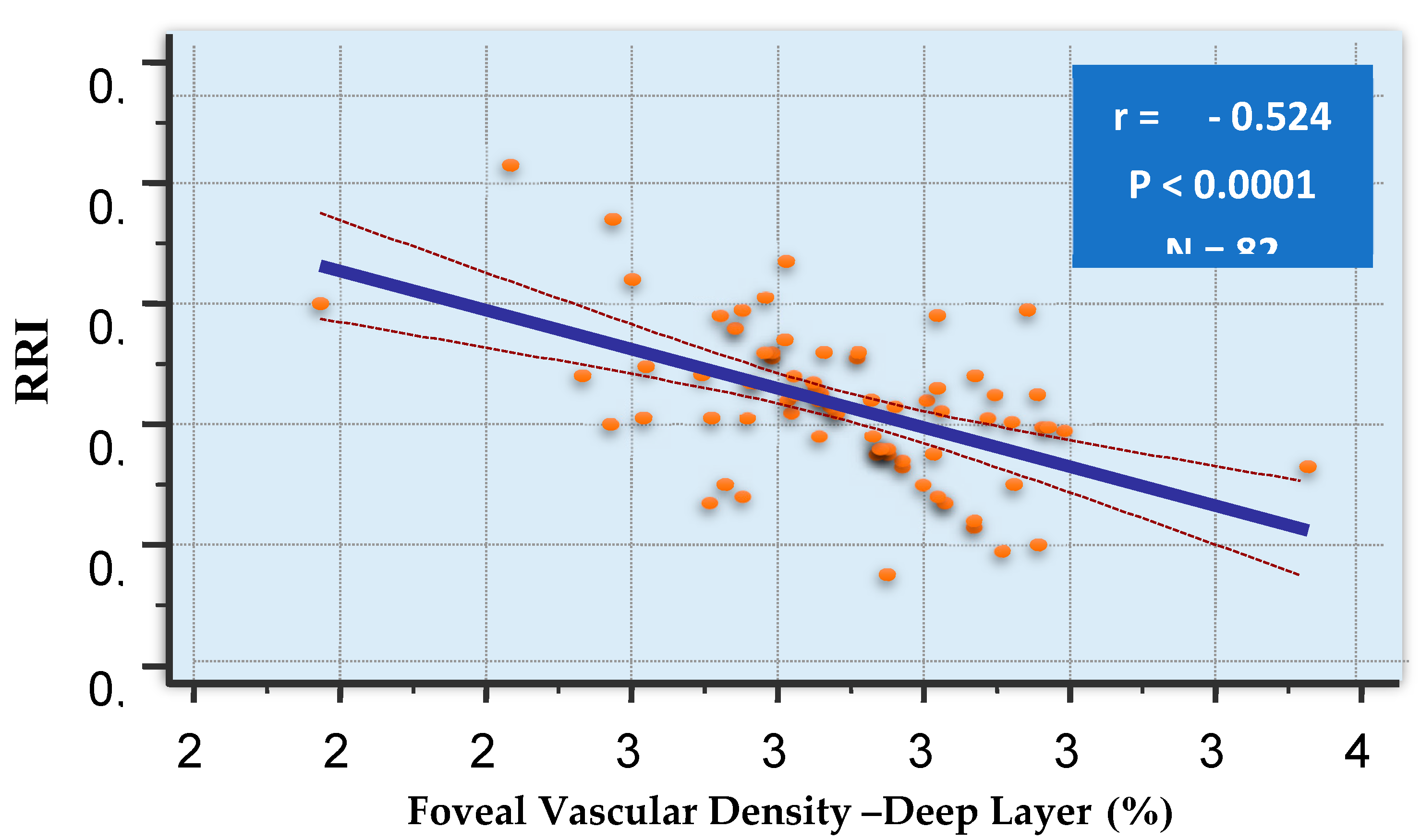
32.9±1.95 | 33.26±1.72 | 31.47±2.11 | 0.01 | 0.001 |
| Age | eGFR | Nighttime PP |
UAE | Deep foveal plexus vascular density |
|||
|---|---|---|---|---|---|---|---|
| (RRI) | r = | 0,235 | -0.288 | 0,3027 | 0,555* | -0,524 | |
| p= | 0,0336 | 0,0087 | 0,0057 | <0,001 | <0,001 |
|
Dependent variable: RRI |
B* | SE | R partial | P |
| Covariates | ||||
|
Foveal Vascular Density (%) –Deep Layer |
-0.0158 | 0.0029 | -0.549 | <0.0001 |
| Mean nighttime PP (mmHg) | 0.0020 | 0.0006 | 0.3063 | 0.0007 |
| Constant | 1.0468 |
|
Dependent variable: Foveal Vascular Density (%) –DeepLayer |
B* | SE | R partial | p |
| Covariates | ||||
| RRI | -18.98 | 3.43 | -0.549 | <0.0001 |
| Mean nighttime PP (mmHg) | 0.048 | 0.0027 | 0.2615 | 0.025 |
| Constant | 42.38 |
|
Dependent variable: RRI > o < 75 pct |
Odds ratio |
95%IC |
P |
| Covariates | |||
|
Foveal Vascular Density (%) –Deep Layer |
-0,5026 | 0,3129 - 0,8073 | 0.0044 |
| Mean nighttime PP (mmHg) | 1,1319 | 1,0493 - 1,2211 | 0.0014 |
| Constant | 15,3587 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




