Submitted:
06 December 2024
Posted:
09 December 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
Statistical Analysis
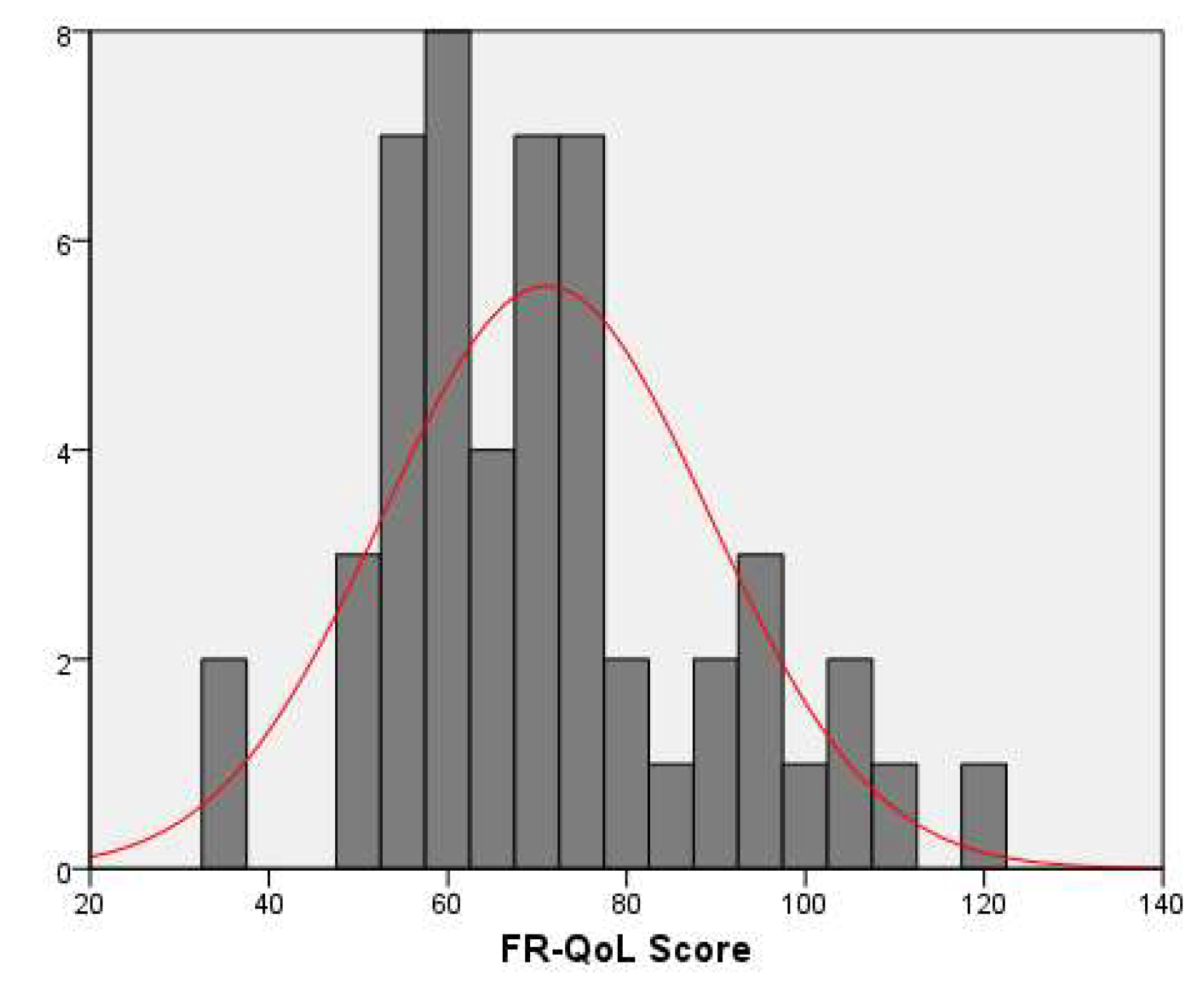
3. Results
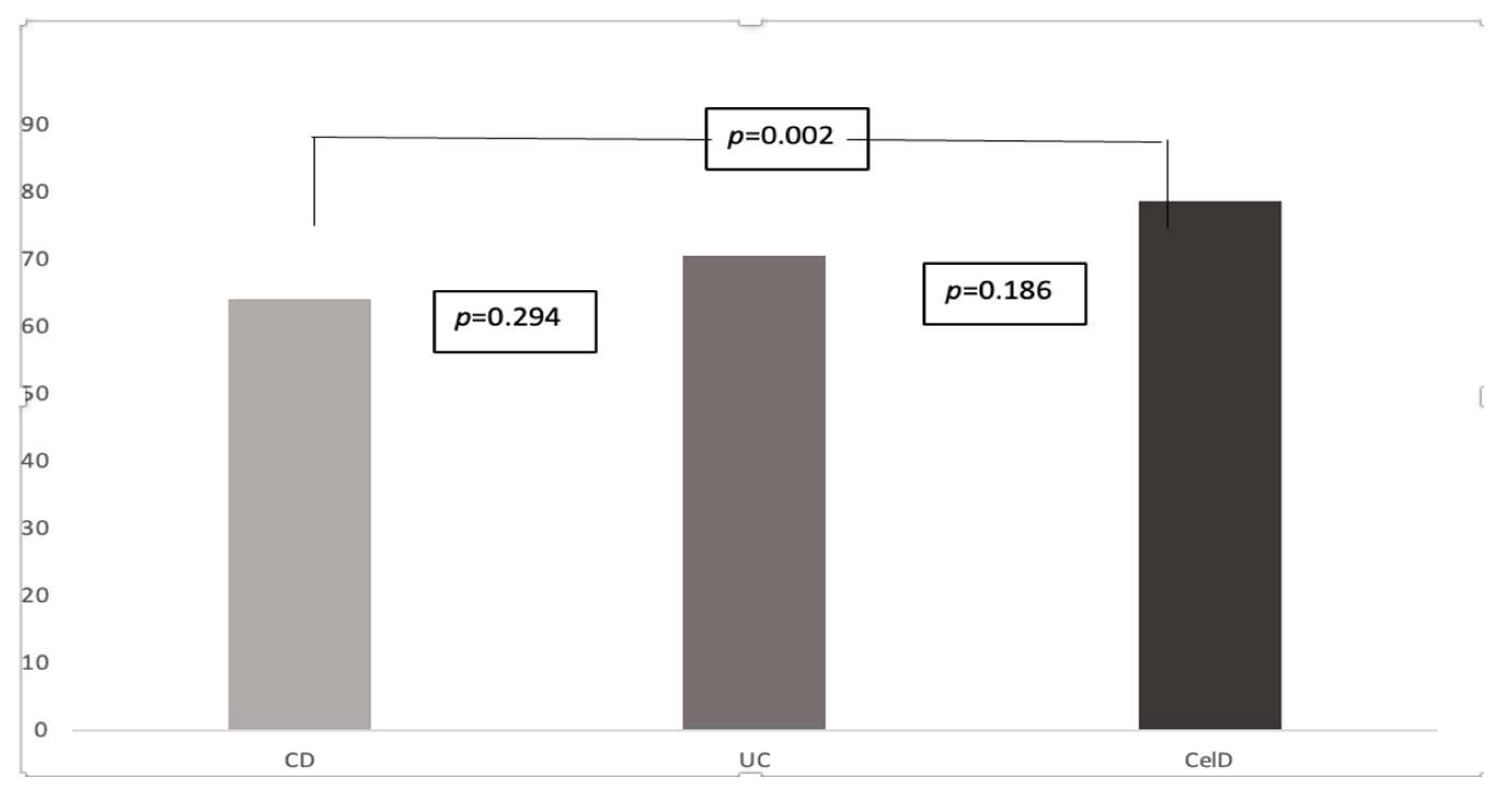
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Vuyyuru, S.K.; Kedia, S.; Sahu, P.; Ahuja, V. Immune-mediated inflammatory diseases of the gastrointestinal tract: Beyond Crohn’s disease and ulcerative colitis. JGH Open 2022, 6, 100–111. [Google Scholar] [CrossRef]
- Sahin, Y. Celiac disease in children: A review of the literature. World J Clin Pediatr 2021, 10, 53–71. [Google Scholar] [CrossRef]
- Caio, G.; Volta, U.; Sapone, A.; Leffler, D.A.; De Giorgio, R.; Catassi, C.; Fasano, A. Celiac disease: a comprehensive current review. BMC Med 2019, 17, 142. [Google Scholar] [CrossRef]
- Husby, S.; Koletzko, S.; Korponay-Szabó, I.; Kurppa, K.; Mearin, M.L.; Ribes-Koninckx, C.; Shamir, R.; Troncone, R.; Auricchio, R.; Castillejo, G.; Christensen, R.; Dolinsek, J.; Gillett, P.; Hróbjartsson, A.; Koltai, T.; Maki, M.; Nielsen, S.M.; Popp, A.; Størdal, K.; Werkstetter, K.; Wessels, M.; European Society Paediatric Gastroenterology, Hepatology and Nutrition. Guidelines for Diagnosing Coeliac Disease 2020. J Pediatr Gastroenterol Nutr 2020, 70, 141–156. [Google Scholar] [CrossRef]
- Almahmoud, E.; Alkazemi, D.U.Z.; Al-Qabandi, W. Growth Stunting and Nutritional Deficiencies among Children and Adolescents with Celiac Disease in Kuwait: A Case–Control Study. Children 2024, 11, 1042. [Google Scholar] [CrossRef] [PubMed]
- Mędza, A.; Szlagatys-Sidorkiewicz, A. Nutritional Status and Metabolism in Celiac Disease: Narrative Review. Journal of Clinical Medicine 2023, 12, 5107. [Google Scholar] [CrossRef] [PubMed]
- Russo, C.; Wolf, R.L.; Leichter, H.J.; Lee, A.R.; Reilly, N.R.; Zybert, P.; Green, P.H.R.; Lebwohl, B. Impact of a Child’s Celiac Disease Diagnosis and Management on the Family. Dig Dis Sci 2020, 65, 2959–2969. [Google Scholar] [CrossRef] [PubMed]
- Pinto-Sanchez, M.I.; Blom, J.J.; Gibson, P.R.; Armstrong, D. Nutrition Assessment and Management in Celiac Disease. Gastroenterology 2024, 167, 116–131. [Google Scholar] [CrossRef]
- Rosen, M.J.; Dhawan, A.; Saeed, S.A. Inflammatory Bowel Disease in Children and Adolescents. JAMA Pediatr 2015, 169, 1053–60. [Google Scholar] [CrossRef] [PubMed]
- Long, D.; Wang, C.; Huang, Y.; Mao, C.; Xu, Y.; Zhu, Y. Changing epidemiology of inflammatory bowel disease in children and adolescents. Int J Colorectal Dis 2024, 39, 73. [Google Scholar] [CrossRef]
- Levine, A.; Koletzko, S.; Turner, D.; Escher, J.C.; Cucchiara, S.; de Ridder, L.; Kolho, K.L.; Veres, G.; Russell, R.K.; Paerregaard, A.; Buderus, S.; Greer, M.L.; Dias, J.A.; Veereman-Wauters, G.; Lionetti, P.; Sladek, M.; Martin de Carpi, J.; Staiano, A.; Ruemmele, F.M.; Wilson, D.C.; European Society of Pediatric Gastroenterology, Hepatology, and Nutrition. ESPGHAN revised porto criteria for the diagnosis of inflammatory bowel disease in children and adolescents. J Pediatr Gastroenterol Nutr 2014, 58, 795–806. [Google Scholar] [CrossRef] [PubMed]
- Gerasimidis, K.; Godny, L.; Sigall-Boneh, R.; Svolos, V.; Wall, C.; Halmos, E. Current recommendations on the role of diet in the aetiology and management of IBD. Frontline Gastroenterol 2021, 13, 160–167. [Google Scholar] [CrossRef]
- Melton, S.L.; Day, A.S.; Bryant, R.V.; Halmos, E.P. Revolution in diet therapy for inflammatory bowel disease. JGH Open 2024, 8, 13097. [Google Scholar] [CrossRef] [PubMed]
- Ishige, T. Growth failure in pediatric onset inflammatory bowel disease: mechanisms, epidemiology, and management. Transl Pediatr 2019, 8, 16–22. [Google Scholar] [CrossRef] [PubMed]
- Hashash, J.G.; Elkins, J.; Lewis, J.D.; Binion, D.G. AGA Clinical Practice Update on Diet and Nutritional Therapies in Patients With Inflammatory Bowel Disease: Expert Review. Gastroenterology 2024, 166, 521–532. [Google Scholar] [CrossRef]
- Czuber-Dochan, W.; Morgan, M.; Hughes, L.D.; Lomer, M.C.; Lindsay, J.O.; Whelan, K. Perceptions and psychosocial impact of food, nutrition, eating and drinking in people with inflammatory bowel disease: A qualitative investigation of food-related quality of life. J. Hum. Nutr. Diet 2019, 33, 115–127. [Google Scholar] [CrossRef] [PubMed]
- Hughes, L.D.; King, L.; Morgan, M.; Ayis, S.; Direkze, N.; Lomer, M.C.; Lindsay, J.O.; Whelan, K. Food-related Quality of Life in Inflammatory Bowel Disease: Development and Validation of a Questionnaire. J. Crohn’s Colitis 2015, 10, 194–201. [Google Scholar] [CrossRef]
- Guadagnoli, L.; Mutlu, E.A.; Doerfler, B.; Ibrahim, A.; Brenner, D.; Taft, T.H. Food-related quality of life in patients with inflammatory bowel disease and irritable bowel syndrome. Qual Life Res 2019, 28, 2195–2205. [Google Scholar] [CrossRef]
- Van Doorn, R.K.; Winkler, L.M.; Zwinderman, K.H.; Mearin, M.L.; Koopman, H.M. CDDUX: a disease-specific health-related quality-of-life questionnaire for children with celiac disease. J Pediatr Gastroenterol Nutr 2008, 47, 147–52. [Google Scholar] [CrossRef]
- Levine, A.; Griffiths, A.; Markowitz, J.; Wilson, D.C.; Turner, D.; Russell, R.K.; Fell, J.; Ruemmele, F.M.; Walters, T.; Sherlock, M.; Dubinsky, M.; Hyams, J.S. Pediatric modification of the Montreal classification for inflammatory bowel disease: the Paris classification. Inflamm Bowel Dis 2011, 17, 1314–21. [Google Scholar] [CrossRef]
- Hughes, L.D.; King, L.; Morgan, M.; et al. Food-related quality of life in inflammatory bowel disease: development and validation of a questionnaire. J Crohn’s Colitis 2016, 10, 194–201. [Google Scholar] [CrossRef]
- https://www.uptodate.com/contents/measurement-of-growth-in-children?source=history_widget#H3606347, accessed on the 11th of November 2024.
- https://www.crohnscolitisfoundation.org/sites/default/files/2023-03/Pediatric%20Assessment%20Tools%20-%20Feb.%202023.pdf, accessed on the 11th of November 2024.
- Turner, D.; Griffiths, A.M.; Walters, T.D.; Seah, T.; Markowitz, J.; Pfefferkorn, M.; Keljo, D.; Waxman, J.; Otley, A.; LeLeiko, N.S.; Mack, D.; Hyams, J.; Levine, A. Mathematical weighting of the pediatric Crohn’s disease activity index (PCDAI) and comparison with its other short versions. Inflamm Bowel Dis 2012, 18, 55–62. [Google Scholar] [CrossRef] [PubMed]
- Turner, D.; Otley, A.R.; Mack, D.; Hyams, J.; de Bruijne, J.; Uusoue, K.; Walters, T.D.; Zachos, M.; Mamula, P.; Beaton, D.E.; Steinhart, A.H.; Griffiths, A.M. Development, validation, and evaluation of a pediatric ulcerative colitis activity index: a prospective multicenter study. Gastroenterology 2007, 133, 423–32. [Google Scholar] [CrossRef] [PubMed]
- Macedo, L.; Catarino, M.; Festas, C.; Alves, P. Vulnerability in Children with Celiac Disease: Findings from a Scoping Review. Children 2024, 11, 729. [Google Scholar] [CrossRef] [PubMed]
- C.D.; Berry, N.; Vaiphei, K.; Dhaka, N.; Sinha, S.K.; Kochhar, R. Quality of life in celiac disease and the effect of gluten-free diet. JGH Open 2018, 2, 124–128. [Google Scholar] [CrossRef]
- Falcomer, A.L.; de Lima, B.R.; Farage, P.; Fabris, S.; Ritter, R.; Raposo, A.; Teixeira-Lemos, E.; Chaves, C.; Zandonadi, R.P. Enhancing life with celiac disease: unveiling effective tools for assessing health-related quality of life. Front Immunol 2024, 15, 1396589. [Google Scholar] [CrossRef] [PubMed]
- Meyer, S. Promoting Effective Self-Management of the Gluten-Free Diet: Children’s and Adolescents’ Self-Generated Do’s and Don’ts. Int J Environ Res Public Health 2022, 19, 14051. [Google Scholar] [CrossRef] [PubMed]
- Fuller, M.K. Pediatric Inflammatory Bowel Disease: Special Considerations. Surg Clin North Am 2019, 99, 1177–1183. [Google Scholar] [CrossRef]
- Carroll, M.W.; Kuenzig, M.E.; Mack, D.R.; et al. The impact of inflammatory bowel disease in Canada 2018: children and adolescents with IBD. J Can Assoc Gastroenterol 2019, 2 (Suppl. 1), S49–S67. [Google Scholar] [CrossRef] [PubMed]
- Nowlin, S.; Manning, L.; Keefer, L.; Gorbenko, K. Perceptive eating as part of the journey in inflammatory bowel disease: Lessons learned from lived experience. Clin Nutr ESPEN 2021, 41, 299–304. [Google Scholar] [CrossRef] [PubMed]
- Bernstein, K.I.; Promislow, S.; Carr, R.; Rawsthorne, P.; Walker, J.R.; Bernstein, C.N. Information needs and preferences of recently diagnosed patients with in- flammatory bowel disease. Inflamm Bowel Dis 2011, 17, 590e8. [Google Scholar] [CrossRef] [PubMed]
- de Vries, J.H.M.; Dijkhuizen, M.; Tap, P.; Witteman, B.J.M. Patient’s Dietary Beliefs and Behaviours in Inflammatory Bowel Disease. Dig Dis 2019, 37, 131–139. [Google Scholar] [CrossRef] [PubMed]
- Sabino, J.; Lewis, J.D.; Colombel, J.F. Treating Inflammatory Bowel Disease With Diet: A Taste Test. Gastroenterology 2019, 157, 295–297. [Google Scholar] [CrossRef] [PubMed]
- Yin, T.; Tu, W.; Li, Y.; Yang, M.; Huang, L.; Zhang, S.; Xu, G. Risk of avoidant/restrictive food intake disorder in patients with inflammatory bowel disease: predictive value of disease phenotype, disease activity and food literacy. J Eat Disord 2023, 11, 211. [Google Scholar] [CrossRef] [PubMed]
- Limdi, J.K.; Aggarwal, D.; McLaughlin, J.T. Dietary Practices and Beliefs in Patients with Inflammatory Bowel Disease. Inflammatory Bowel Diseases 2016, 22, 164–170. [Google Scholar] [CrossRef] [PubMed]
- Khemiri, W.; Ayari, M.; Ghannouchi, A.; Mtir, M.; Abdelaali, Z.E.I.; Douggui, M.H.; Taieb, J. P980 Dietary perceptions and practices in patients with Inflammatory Bowel Disease. Journal of Crohn’s and Colitis 2024, 18, i1777. [Google Scholar] [CrossRef]
- Diederen, K.; Krom, H.; Koole, J.C.D.; Benninga, M.A.; Kindermann, A. Diet and Anthropometrics of Children With Inflammatory Bowel Disease: A Comparison With the General Population. Inflamm Bowel Dis 2018, 24, 1632–1640. [Google Scholar] [CrossRef] [PubMed]
- Subramanian, L.; Coo, H.; Jane, A.; Flemming, J.A.; Acker, A.; Hoggan, B.; Griffiths, R.; Sehgal, A.; Mulder, D. Celiac Disease and Inflammatory Bowel Disease Are Associated With Increased Risk of Eating Disorders: An Ontario Health Administrative Database Study. Clin Transl Gastroenterol 2024, 15, e00700. [Google Scholar] [CrossRef] [PubMed]
- Fisher, K.; Byham-Gray, L.; Rothpletz-Puglia, P. Characterizing the Parental Perspective of Food-Related Quality of Life in Families After Pediatric Inflammatory Bowel Disease Diagnosis. Gastroenterology Nursing 2021, 44, E69–E77. [Google Scholar] [CrossRef]
- Brown, S.C.; Whelan, K.; Frampton, C.; Wall, C.L.; Gearry, R.B.; Day, A.S. Food-Related Quality of Life in Children and Adolescents With Crohn’s Disease. Inflamm Bowel Dis 2022, 28, 1838–1843. [Google Scholar] [CrossRef] [PubMed]
- Zhu, W.; Zhang, Y.; Wang, L.D.; Li, J.; Hou, S. Factors influencing food-related quality of life in patients with inflammatory bowel disease: A systematic review. J Eval Clin Pract 2024. [Google Scholar] [CrossRef] [PubMed]
- Jiang, C.; Godoy-Brewer, G.; Rodriguez, A.; Graff, E.; Quintero, M.A.; Leavitt, J.; Lopez, J.; Goldberg, D.S.; Damas, O.M.; Whelan, K.; Abreu, M.T. Food-Related Quality of Life Is Impaired in Latinx and Non-Latinx Patients With Inflammatory Bowel Disease. Gastro Hep Adv 2024, 3, 773–782. [Google Scholar] [CrossRef] [PubMed]
- https://www.thebrainyinsights.com/report/gluten-free-products-market-13892, accessed on the 11th of November 2024.
- Iorfida, D.; Valitutti, F.; Vestri, A.; Di Rocco, A.; Cucchiara, S.; Lubrano, R.; Montuori, M. Dietary Compliance and Quality of Life in Celiac Disease: A Long-Term Follow-Up of Primary School Screening-Detected Patients. Front Pediatr 2021, 9, 787938. [Google Scholar] [CrossRef] [PubMed]
- Meyer, S.; Monachesi, C.; Barchetti, M.; Lionetti, E.; Catassi, C. Cross-Cultural Participation in Food-Related Activities and Quality of Life among Children with Celiac Disease. Children 2023, 10, 1300. [Google Scholar] [CrossRef]
- Berkhout, C.; Berbra, O.; Favre, J.; Collins, C.; Calafiore, M.; Peremans, L.; Van Royen, P. Defining and evaluating the Hawthorne effect in primary care, a systematic review and meta-analysis. Front Med 2022, 9, 1033486. [Google Scholar] [CrossRef] [PubMed]
| Crohn’s Disease (CD) n = 17 |
Ulcerative Colitis (UC) n = 17 |
Celiac Disease (CelD) n=17 |
p-value | |
|---|---|---|---|---|
| Sex [n (%)] | 0.379 | |||
| Male (n=21) | 9 (52.9%) | 5 (29.4) | 7 (41.2) | |
| Female (n=30) | 8 (47.1%) | 12 (70.6) | 10(58.8) | |
| Median age at diagnosis, years [IQR] | 13.2[10.85-15] | 12.3[9.15-14.4] | 4[2-7.9] | <0.001 |
| Median age at inclusion, years [IQR] | 16[12-16.75] | 16[14-17] | 13[10.8-16.4] | 0.383 |
| Median duration of evolution, years [IQR] | 17[9.5-45.5] | 22[9.5-60] | 102[75-132.6] | <0.001 |
| UC extension | - | <0.001 | ||
| E1 | - | 2 (11.8) | ||
| E2 | - | 2 (11.8) | ||
| E4 | - | 13 (76.4) | ||
| CD location [n (%)] | - | 0.824 | ||
| L1 | 6 (35.3) | - | ||
| L2 | 4(23.5) | - | ||
| L3 | 7 (41.2) | - | ||
| L4a | 1 (5.9) | - | ||
| CD behaviour [n (%)] | - | 0.029 | ||
| B1 | 13 (76.5) | - | ||
| B2 | 4 (23.5) | - | ||
| B3 | - | - | ||
| P | 2 (11.8) | - | ||
| PGA [n (%)] | - | 0.648 | ||
| 0 | 4 (23.5) | 7 (41.2) | ||
| 1 | 7 (41.2) | 4 (23.5) | ||
| 2 | 5 (29.4) | 4 (23.5) | ||
| 3 | 1 (5.9) | 2 (11.8) | ||
| Treatment regimen [n (%)] | ||||
| Diet (CDED±PEN) | 4 (23.5) | - | ||
| 5-ASA | 2 (11.8) | 8 (47.1) | ||
| IMM (AZA) | 6 (35.3) | 3 (17.6) | ||
| Biologics | 6 (35.3) | 6 (35.3) | - | 0.640* |
| IFX | 4 (23.5) | 6 (35.3) | ||
| ADA | 2 (11.8) | 0 (0) | ||
| Topic steroids/systemic steroids | 1 (5.9) | 1 (5.9) | ||
| Strict GFD | - | - | 16 (94.1) | |
| Nutritional status [n (%)] | 0.908 | |||
| Healthy weight | 12 (70.6) | 14 (82.3) | 12 (70.6) | |
| Underweight | 4 (23.5) | 2 (11.8) | 4(23.5) | |
| Overweight | 0 (0) | 1 (5.9) | 1(5.9) | |
| Class I obesity | 1 (5.9) | 0 (0) | ||
| History of surgery [n (%)] | 6 (35.3) | 0 (0) | - | 0.018 |
| CD* n = 17 |
UC** n = 17 |
p-value | |
|---|---|---|---|
| UC extension (n) | 0.504 | ||
| E1 | - | 60.5±2.1 | |
| E2 | - | 61±2.8 | |
| E4 | - | 73.5±20 | |
| CD location [n (%)] | - | 0.418 | |
| L1 | 61.3±3.4 | ||
| L2 +L2L4a | 59±4.8 | ||
| L3 | 69.3±18.4 | ||
| CD behaviour [n (%)] | - | 0.770 | |
| B1+B1p | 66±18.9 | ||
| B2 | 63±8.3 | ||
| History of surgery [n (%)] | - | 0.291 | |
| positive | 61.8±7 | ||
| negative | 70.3±19 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




