Submitted:
02 December 2024
Posted:
04 December 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
Statistical Analysis
3. Results
3.1. Patient Characteristics
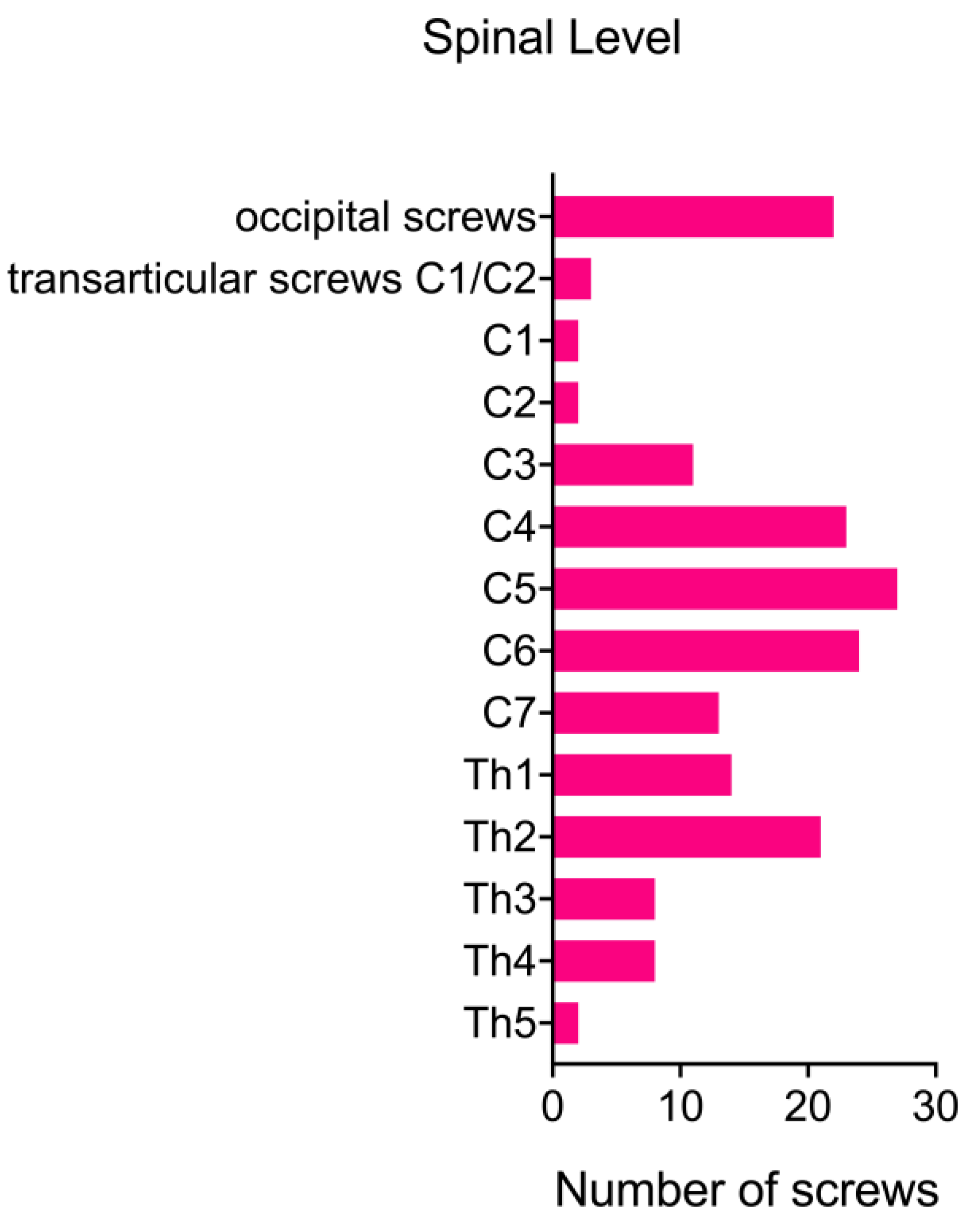
3.2. Extent of Surgical Spinal Fusion
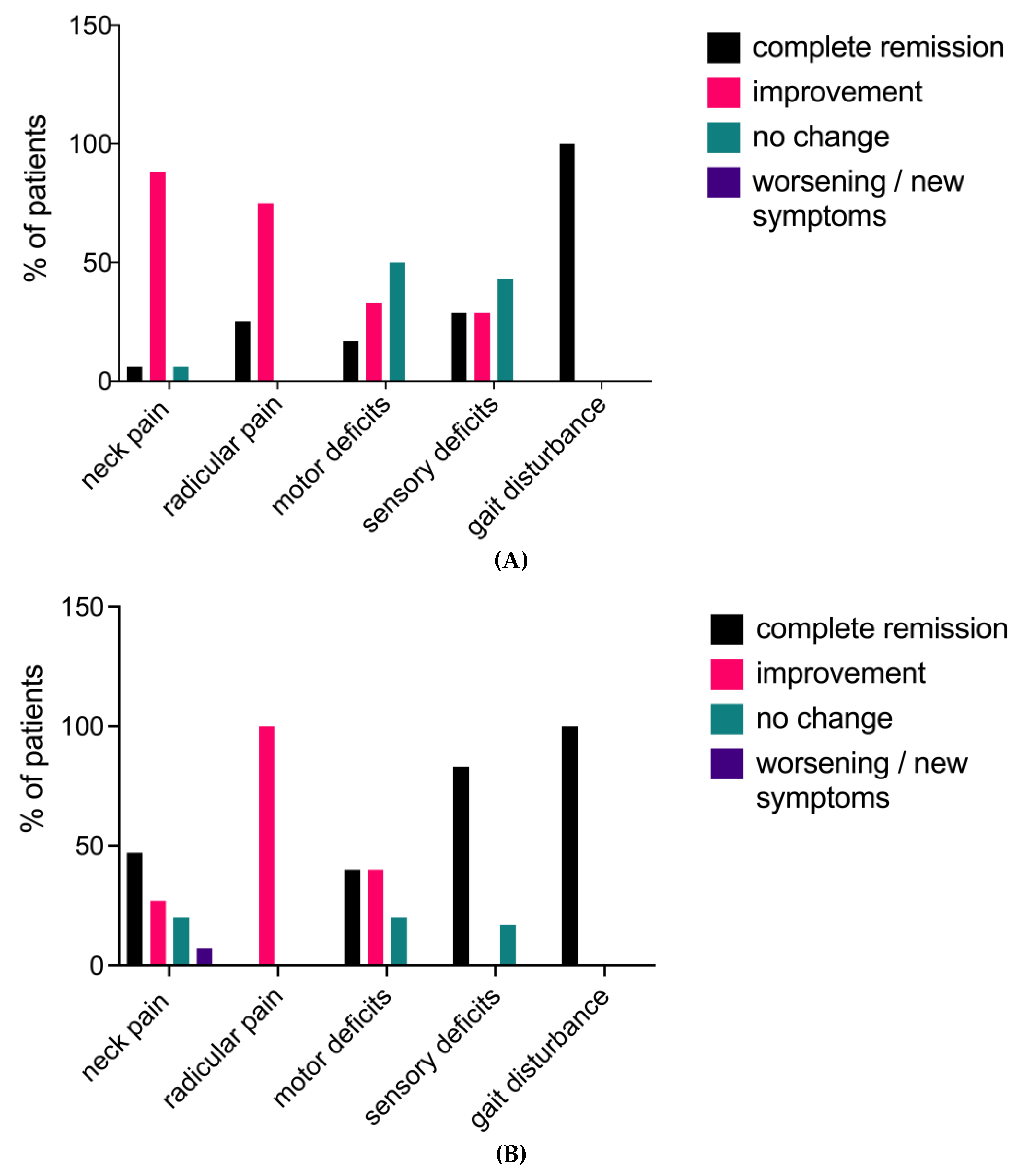
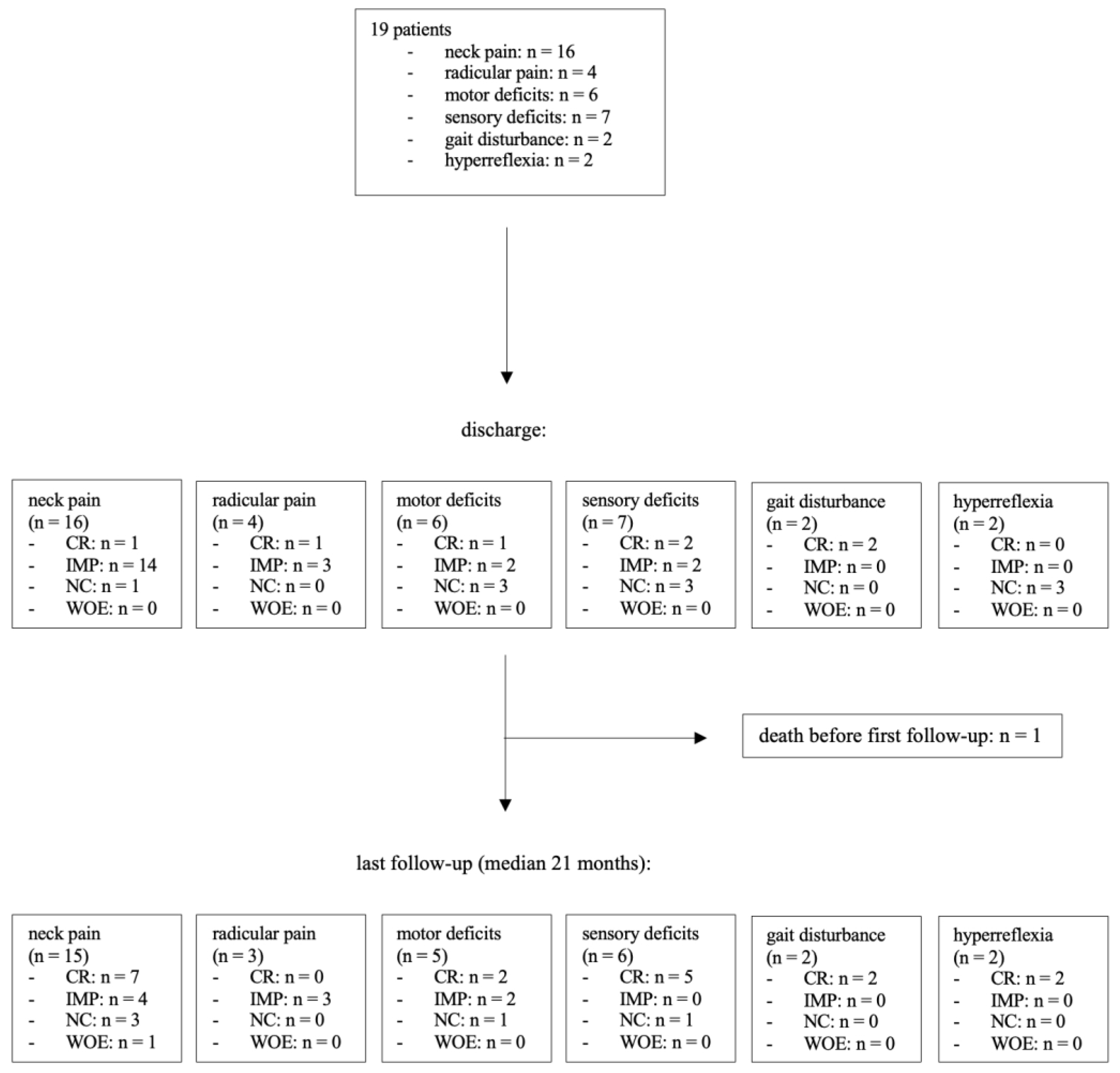
3.3. Symptoms at Discharge
3.4. Follow-Up and Clinical Long-Term Outcome
3.5. Radiological Findings
3.6. Complications and Adverse Events
3.7. Sensitivity, Specificity and Accuracy of iCT
4. Discussion
4.1. Clinical Outcome
4.2. Surgical Approach
4.3. Adverse Events & Revision Rate
4.4. Radiological Outcomes & Fusion Rates
4.5. Intraoperative CT Scan
4.6. Study Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Fehlings MG, Vaccaro A, Wilson JR, et al. Early versus delayed decompression for traumatic cervical spinal cord injury: results of the Surgical Timing in Acute Spinal Cord Injury Study (STASCIS). PLoS One. 2012;7(2):e32037. [CrossRef]
- Persson LC, Carlsson CA, Carlsson JY. Long-lasting cervical radicular pain managed with surgery, physiotherapy, or a cervical collar. A prospective, randomized study. Spine (Phila Pa 1976). Apr 1 1997;22(7):751-8. [CrossRef]
- Nikolaidis I, Fouyas IP, Sandercock PA, Statham PF. Surgery for cervical radiculopathy or myelopathy. Cochrane Database Syst Rev. Jan 20 2010;(1):CD001466. [CrossRef]
- Fehlings MG, Tetreault LA, Riew KD, et al. A Clinical Practice Guideline for the Management of Patients With Degenerative Cervical Myelopathy: Recommendations for Patients With Mild, Moderate, and Severe Disease and Nonmyelopathic Patients With Evidence of Cord Compression. Global Spine J. Sep 2017;7(3 Suppl):70S-83S. [CrossRef]
- Mummaneni PV, Kaiser MG, Matz PG, et al. Cervical surgical techniques for the treatment of cervical spondylotic myelopathy. J Neurosurg Spine. Aug 2009;11(2):130-41. [CrossRef]
- Emery SE, Bohlman HH, Bolesta MJ, Jones PK. Anterior cervical decompression and arthrodesis for the treatment of cervical spondylotic myelopathy. Two to seventeen-year follow-up. J Bone Joint Surg Am. Jul 1998;80(7):941-51. [CrossRef]
- Hilibrand AS, Fye MA, Emery SE, Palumbo MA, Bohlman HH. Impact of smoking on the outcome of anterior cervical arthrodesis with interbody or strut-grafting. J Bone Joint Surg Am. May 2001;83-A(5):668-73.
- Koller H, Reynolds J, Zenner J, et al. Mid- to long-term outcome of instrumented anterior cervical fusion for subaxial injuries. Eur Spine J. May 2009;18(5):630-53. [CrossRef]
- Kawakami M, Tamaki T, Iwasaki H, Yoshida M, Ando M, Yamada H. A comparative study of surgical approaches for cervical compressive myelopathy. Clin Orthop Relat Res. Dec 2000;(381):129-36. [CrossRef]
- Nevzati E, Fandino J, Schatlo B, et al. Validation and accuracy of intraoperative CT scan using the Philips AlluraXper FD20 angiography suite for assessment of spinal instrumentation. Br J Neurosurg. Dec 2017;31(6):741-746. [CrossRef]
- McCormack HM, Horne DJ, Sheather S. Clinical applications of visual analogue scales: a critical review. Psychol Med. Nov 1988;18(4):1007-19. [CrossRef]
- Vernon H, Mior S. The Neck Disability Index: a study of reliability and validity. J Manipulative Physiol Ther. Sep 1991;14(7):409-15.
- Nurick, S. Nurick S. The pathogenesis of the spinal cord disorder associated with cervical spondylosis. Brain. 1972;95(1):87-100. [CrossRef]
- Macnab I. Negative disc exploration. An analysis of the causes of nerve-root involvement in sixty-eight patients. J Bone Joint Surg Am. Jul 1971;53(5):891-903.
- Odom GL, Finney W, Woodhall B. Cervical disk lesions. J Am Med Assoc. Jan 4 1958;166(1):23-8. [CrossRef]
- Lenke LG, Betz RR, Harms J, et al. Adolescent idiopathic scoliosis: a new classification to determine extent of spinal arthrodesis. J Bone Joint Surg Am. Aug 2001;83-A(8):1169-81.
- Youssef JA, Heiner AD, Montgomery JR, et al. Outcomes of posterior cervical fusion and decompression: a systematic review and meta-analysis. Spine J. Oct 2019;19(10):1714-1729. [CrossRef]
- Anderson PA, Matz PG, Groff MW, et al. Laminectomy and fusion for the treatment of cervical degenerative myelopathy. J Neurosurg Spine. Aug 2009;11(2):150-6. [CrossRef]
- Lee MJ, Bazaz R, Furey CG, Yoo J. Risk factors for dysphagia after anterior cervical spine surgery: a two-year prospective cohort study. Spine J. Mar-Apr 2007;7(2):141-7. [CrossRef]
- Witwer BP, Trost GR. Cervical spondylosis: ventral or dorsal surgery. Neurosurgery. Jan 2007;60(1 Supp1 1):S130-6. [CrossRef]
- Woernle K, Marbacher S, Khamis A, Landolt H, Fandino J. Clinical Outcome after Laminectomy without Fusion for Cervical Spondylotic Myelopathy. Open Journal of Modern Neurosurgery. 2015;05(02):41-48. [CrossRef]
- Albert TJ, Vacarro A. Postlaminectomy kyphosis. Spine (Phila Pa 1976). Dec 15 1998;23(24):2738-45. [CrossRef]
- Lau D, Winkler EA, Than KD, Chou D, Mummaneni PV. Laminoplasty versus laminectomy with posterior spinal fusion for multilevel cervical spondylotic myelopathy: influence of cervical alignment on outcomes. J Neurosurg Spine. Nov 2017;27(5):508-517. [CrossRef]
- Asher AL, Devin CJ, Kerezoudis P, et al. Comparison of Outcomes Following Anterior vs Posterior Fusion Surgery for Patients With Degenerative Cervical Myelopathy: An Analysis From Quality Outcomes Database. Neurosurgery. Apr 1 2019;84(4):919-926. [CrossRef]
- Fehlings MG, Barry S, Kopjar B, et al. Anterior versus posterior surgical approaches to treat cervical spondylotic myelopathy: outcomes of the prospective multicenter AOSpine North America CSM study in 264 patients. Spine (Phila Pa 1976). Dec 15 2013;38(26):2247-52. [CrossRef]
- Audat ZA, Fawareh MD, Radydeh AM, et al. Anterior versus posterior approach to treat cervical spondylotic myelopathy, clinical and radiological results with long period of follow-up. SAGE Open Med. 2018;6:2050312118766199. [CrossRef]
- Muffoletto AJ, Hadjipavlou AG, Jensen RE, Nauta HJ, Necessary JT, Norcross-Nechay K. Techniques and pitfalls of cervical lateral mass plate fixation. Am J Orthop (Belle Mead NJ). Nov 2000;29(11):897-903.
- Kumar VG, Rea GL, Mervis LJ, McGregor JM. Cervical spondylotic myelopathy: functional and radiographic long-term outcome after laminectomy and posterior fusion. Neurosurgery. Apr 1999;44(4):771-7; discussion 777-8. [CrossRef]
- Katonis P, Papadakis SA, Galanakos S, et al. Lateral mass screw complications: analysis of 1662 screws. J Spinal Disord Tech. Oct 2011;24(7):415-20. [CrossRef]
- Scarone P, Vincenzo G, Distefano D, et al. Use of the Airo mobile intraoperative CT system versus the O-arm for transpedicular screw fixation in the thoracic and lumbar spine: a retrospective cohort study of 263 patients. J Neurosurg Spine. Oct 2018;29(4):397-406. [CrossRef]
- Farah K, Coudert P, Graillon T, et al. Prospective Comparative Study in Spine Surgery Between O-Arm and Airo Systems: Efficacy and Radiation Exposure. World Neurosurg. Oct 2018;118:e175-e184. [CrossRef]
- Mandelka E, Gierse J, Zimmermann F, Gruetzner PA, Franke J, Vetter SY. Implications of navigation in thoracolumbar pedicle screw placement on screw accuracy and screw diameter/pedicle width ratio. Brain Spine. 2023;3:101780. [CrossRef]
- Ille S, Baumgart L, Obermueller T, Meyer B, Krieg SM. Clinical efficiency of operating room-based sliding gantry CT as compared to mobile cone-beam CT-based navigated pedicle screw placement in 853 patients and 6733 screws. Eur Spine J. Dec 2021;30(12):3720-3730. [CrossRef]
- Jones AK, Odisio BC. Comparison of radiation dose and image quality between flat panel computed tomography and multidetector computed tomography in a hybrid CT-angiography suite. J Appl Clin Med Phys. Feb 2020;21(2):121-127. [CrossRef]
| Mean age | 59 (± 11) years |
| Sex | |
| male | 12 (63%) |
| female | 7 (37%) |
| Pathology | |
| neoplastic | 7 (37%) |
| metastasis | 4 (57%) |
| chordoma | 2 (29%) |
| plasmocytoma | 1 (14%) |
| degenerative | 6 (32%) |
| traumatic | 6 (32%) |
| fractures | |
| Proc. condylaris | 1 |
| Atlas (Jefferson fracture) | 1 |
| Dens (Anderson D’Alonzo Type 2) | 2 |
| Hangman’s fracture (Effendi Type 2) | 1 |
| incomplete burst (AO A3) | 1 |
| hyperextension fracture (AO B2) | 1 |
| Preoperative Symptoms | |
| neck pain | 16 (84%) |
| radicular pain | 4 (21%) |
| sensory deficit | 7 (37%) |
| motor deficit | 6 (32%) |
| gait disturbance | 2 (11%) |
| hyperreflexia | 2 (11%) |
| Preoperative radiological findings | |
| compression of brain stem | 1 (5%) |
| compression of cervical spinal cord | 7 (37%) |
| radiological signs of myelopathy | 5 (26%) |
| compression of nerve root | 5 (26%) |
| cervical spinal instability | 4 (21%) |
| atlanto-occipital subluxation | 1 (5%) |
| spondylolisthesis | 3 (16%) |
| kyphosis | 5 (26%) |
| Mean number of segments undergoing fusion | 4.74 |
| Extent of surgical fusion | |
| cervical spine only | 6 (32%) |
| inclusion of occipito-cervical junction | 5 (26%) |
| inclusion of upper thoracic spine | 11 (58%) |
| inclusion of occipito-cervical junction and upper thoracic spine | 1 (5%) |
| Patient | Extent of Fusion | Intraoperatively repositioned screws |
| 1 | Occipital – C5 | |
| 2 | Occipital – C5 | |
| 3 | Occipital – C5 | |
| 4 | Occipital – C6 | |
| 5 | Occipital – Th2 | C7, right side |
| 6 | C1 – C2 | |
| 7 | C3 – Th1 | C3, left side |
| 8 | C3 – Th3 | Th1, left side |
| 9 | C4 – C5 | |
| 10 | C4 – C7 | |
| 11 | C4 – C7 | |
| 12 | C4 – Th2 | Th1, bilaterally |
| 13 | C5 – Th1 | Th1, left side |
| 14 | C5 – Th2 | |
| 15 | C5 – Th3 | Th2, right side |
| 16 | C5 – Th4 | |
| 17 | C5 – Th4 | |
| 18 | C5 – Th4 | Th4, right side |
| 19 | C6 – Th4 |
| Neck Disability Index 0 points 1-5 points > 5 points Nurick Scale 0 points 1 point 2 points 3 points 4 points 5 points Modified Macnab Criteria excellent good fair poor |
3 (43%) 2 (29%) 2 (29%) 7 0 0 0 0 0 2 (29%) 3 (43%) 2 (29%) 0 |
Odom’s Critera excellent good fair poor Lenke and Bridwell Grade A Grade B Grade C Grade D |
4 (57%) 1 (14%) 2 (29%) 0 5 (38%) 4 (31%) 3 (23%) 1 (8%) |
| Intraoperative CT scan | |||||
| Postoperative CT scan | No violation | Minor violation | Moderate violation | Severe violation | Total |
| No violation | 102 | 8 | 0 | 0 | 110 |
| Minor violation | 6 | 17 | 1 | 0 | 24 |
| Moderate violation | 1 | 3 | 9 | 0 | 13 |
| Severe violation | 0 | 0 | 1 | 3 | 4 |
| Total | 109 | 28 | 11 | 3 | 151 |
| Extent of violation | Sensitivity (%) | Specificity (%) | Accuracy (%) |
| No violation | 92.7 | 82.9 | 90.0 |
| Minor violation (< 1/3 screw diameter) | 70.8 | 91.3 | 88.1 |
| Moderate violation (> 1/3 screw diameter, < 1 screw diameter) |
69.2 | 98.6 | 96.0 |
| Severe violation (> 1 screw diameter) | 75.0 | 100 | 99.3 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




