Submitted:
02 December 2024
Posted:
03 December 2024
You are already at the latest version
Abstract
Background/Objectives: the SARS-CoV-2 (COVID-19) pandemic has significantly impacted a large portion of the global population. Numerous studies have investigated the potential outcomes of Coronavirus infection in pregnant women, aiming to identify variables that may be associated with either improved or worsened outcomes. In this context, nutritional factors have occasionally been hypothesized to play a potentially important role in preventing adverse obstetric outcomes in pregnant women affected by COVID-19. We conducted a comprehensive literature review to examine the relationship between COVID-19 and nutrition. Our objective was to provide an updated and state-of-the-art overview of the interactions between nutrition, COVID-19 infection during pregnancy, and perinatal, obstetric, and neonatal outcomes. Methods: we conducted a comprehensive literature search in electronic databases, namely PubMed, Medline, and Embase, focusing on the relationship between COVID-19 and the role of diet and micronutrients in pregnancy. Results: an adequate nutritional intake, coupled with a healthy lifestyle, along with the consumption of probiotics and prebiotics and the supplementation of specific micronutrients, appears to play a crucial role in preventing adverse outcomes and pregnancy complications associated with COVID-19. Conclusions: obstetric research must continue to advance preventive strategies against the SARS-CoV-2 virus, including those focused on nutrition.
Keywords:
1. Introduction
2. Materials and Methods
3. Results
3.1. COVID-19 and Pregnancy
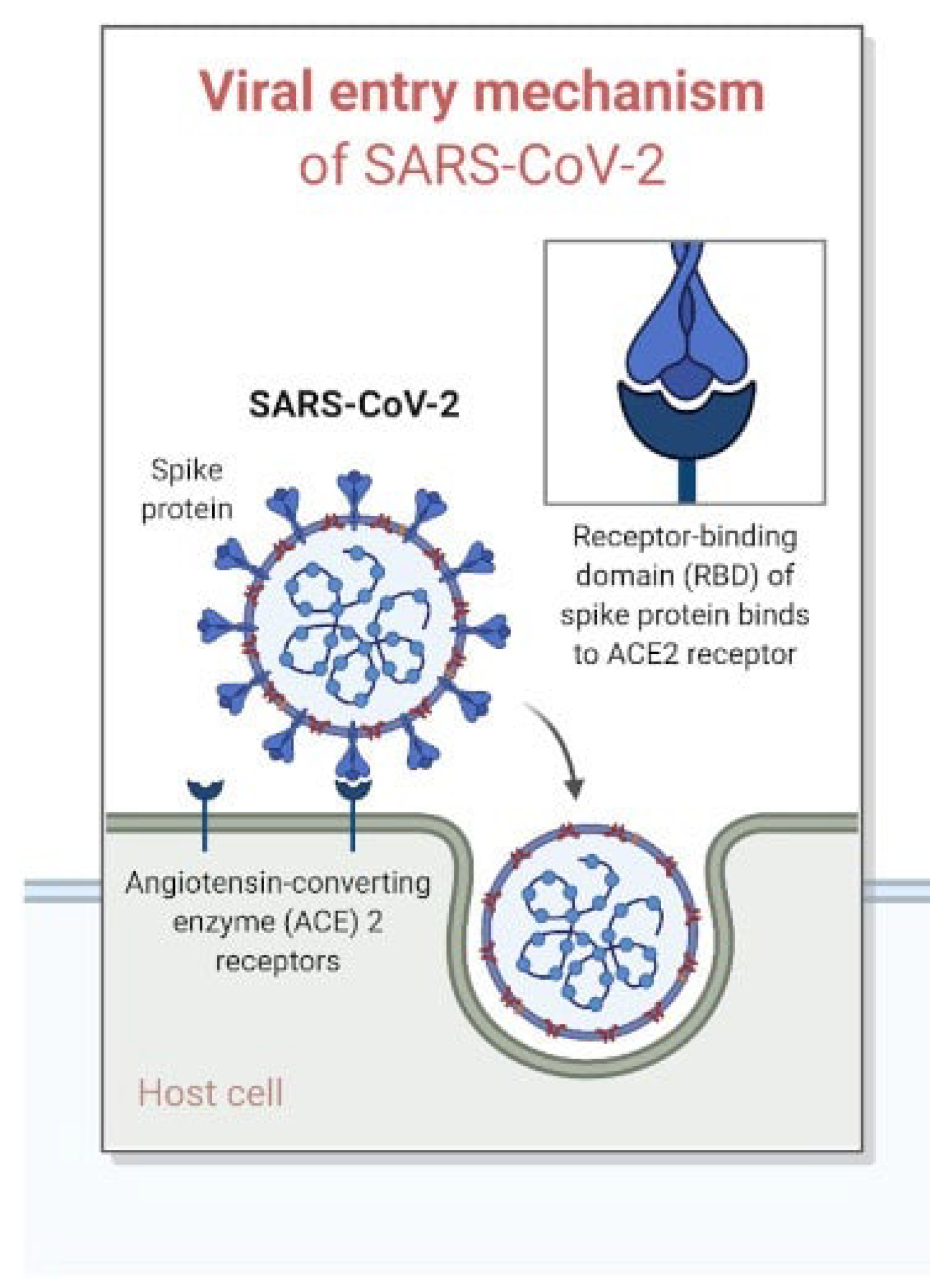
3.2. Role of ACE2 Receptor in the Pathogenesis of Placental Hypoxemia and Adverse Pregnancy Outcomes
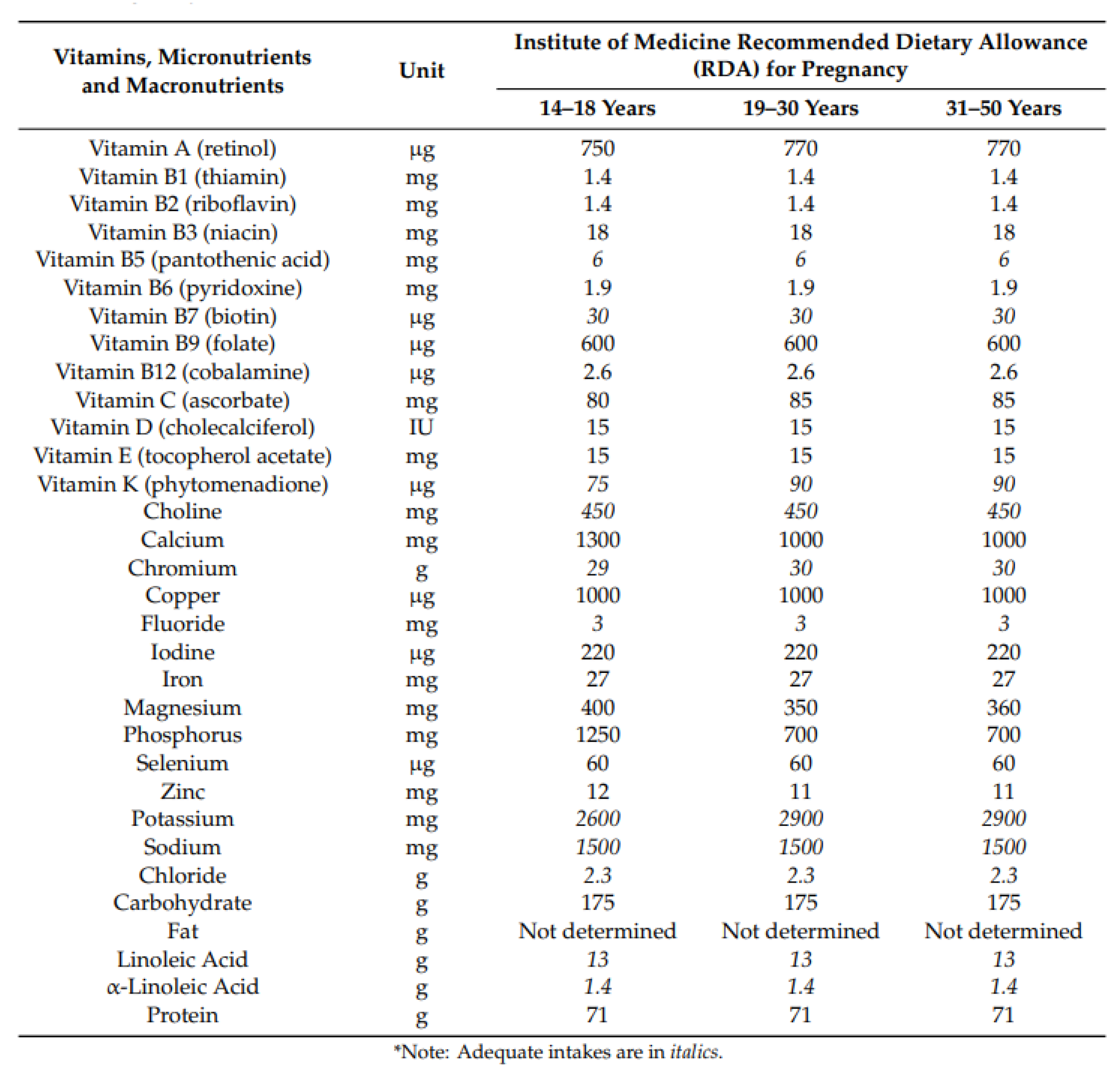
3.3. Recommended Dietary Allowances in Pregnancy
3.3.1. Role of Diet
3.4. Role of Vitamins
3.4.1. Vitamin D
3.4.2. Vitamin A, B, C and E
3.5. Role of Choline
3.6. Role of Iron
3.7. Role of Mineral
3.7.1. Zinc
3.7.2. Magnesium
3.7.3. Calcium
3.7.4. Selenium
3.8. Role of Omega Omega-3 polyunsaturated Fatty Acids
3.9. Role of Probiotic and Prebiotic
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- World Health Organization. WHO Coronavirus (COVID-19) dashboard. https://data.who.int/dashboards/covid19/cases?n=c. Accessed August 2024.
- Favre G, Pomar L, Musso D, Baud D. 2019-nCoV epidemic: what about pregnancies? Lancet 2020, 395, e40. [Google Scholar] [CrossRef] [PubMed]
- Schwartz DA, Graham AL. Potential Maternal and Infant Outcomes from Coronavirus 2019-nCoV (SARS-CoV-2) Infecting Pregnant Women: Lessons from SARS, MERS, and Other Human Coronavirus Infections. Viruses 2020, 12, 194. [Google Scholar] [CrossRef] [PubMed]
- Huang C, Wang Y, Li X, Ren L, Zhao J, Hu Y, et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet 2020, 395, 497–506. [Google Scholar] [CrossRef] [PubMed]
- Donati S, Corsi E, Maraschini A, Salvatore MA, ItOSS COVID-19 Working Group, ItOSS COVID-19 WORKING GROUP. The first SARS-CoV-2 wave among pregnant women in Italy: results from a prospective population-based study. Ann Ist Super Sanita 2021, 57, 272–285. [Google Scholar] [CrossRef]
- Lokken EM, Taylor GG, Huebner EM, Vanderhoeven J, Hendrickson S, Coler B, et al. Higher severe acute respiratory syndrome coronavirus 2 infection rate in pregnant patients. Am J Obstet Gynecol 2021, 225, 75.e1–75.e16. [Google Scholar] [CrossRef]
- Zaigham M, Andersson O. Maternal and perinatal outcomes with COVID-19: A systematic review of 108 pregnancies. Acta Obstet Gynecol Scand 2020, 99, 823–829. [Google Scholar] [CrossRef]
- Di Mascio D, Sen C, Saccone G, Galindo A, Grünebaum A, Yoshimatsu J, et al. Risk factors associated with adverse fetal outcomes in pregnancies affected by Coronavirus disease 2019 (COVID-19): a secondary analysis of the WAPM study on COVID-19. J Perinat Med 2020, 48, 950–958. [Google Scholar] [CrossRef]
- Chmielewska B, Barratt I, Townsend R, Kalafat E, van der Meulen J, Gurol-Urganci I, et al. Effects of the COVID-19 pandemic on maternal and perinatal outcomes: a systematic review and meta-analysis. Lancet Glob Heal 2021, 9, e759–72. [Google Scholar] [CrossRef]
- Edlow AG, Castro VM, Shook LL, Kaimal AJ, Perlis RH. Neurodevelopmental Outcomes at 1 Year in Infants of Mothers Who Tested Positive for SARS-CoV-2 During Pregnancy. JAMA Netw Open 2022, 5, e2215787. [Google Scholar] [CrossRef]
- Garcia-Flores V, Romero R, Xu Y, Theis KR, Arenas-Hernandez M, Miller D, et al. Maternal-fetal immune responses in pregnant women infected with SARS-CoV-2. Nat Commun 2022, 13, 320. [Google Scholar] [CrossRef]
- Dang D, Wang L, Zhang C, Li Z, Wu H. Potential effects of SARS-CoV-2 infection during pregnancy on fetuses and newborns are worthy of attention. J Obstet Gynaecol Res 2020, 46, 1951–1957. [Google Scholar] [CrossRef] [PubMed]
- Hoffmann M, Kleine-Weber H, Schroeder S, Krüger N, Herrler T, Erichsen S, et al. SARS-CoV-2 Cell Entry Depends on ACE2 and TMPRSS2 and Is Blocked by a Clinically Proven Protease Inhibitor. Cell 2020, 181, 271–280.e8. [Google Scholar] [CrossRef] [PubMed]
- Chen S, Huang B, Luo DJ, Li X, Yang F, Zhao Y, et al. Pregnancy with new coronavirus infection: clinical characteristics and placental pathological analysis of three cases. Chinese J Pathol 2020, 49, 418–423. [Google Scholar] [CrossRef]
- Ng WF, Wong SF, Lam A, Mak YF, Yao H, Lee KC, et al. The placentas of patients with severe acute respiratory syndrome: a pathophysiological evaluation. Pathology 2006, 38, 210–218. [Google Scholar] [CrossRef]
- Kosinska-Kaczynska K, Malicka E, Szymusik I, Dera N, Pruc M, Feduniw S, et al. The sFlt-1/PlGF Ratio in Pregnant Patients Affected by COVID-19. J Clin Med 2023, 12, 1059. [Google Scholar] [CrossRef]
- Di Mascio D, Khalil A, Saccone G, Rizzo G, Buca D, Liberati M, et al. Outcome of coronavirus spectrum infections (SARS, MERS, COVID-19) during pregnancy: a systematic review and meta-analysis. Am J Obstet Gynecol MFM 2020, 2, 100107. [Google Scholar] [CrossRef]
- Moltner S, de Vrijer B, Banner H. Placental infarction and intrauterine growth restriction following SARS-CoV-2 infection. Arch Gynecol Obstet 2021, 304, 1621–1622. [Google Scholar] [CrossRef]
- Sukhikh G, Petrova U, Prikhodko A, Starodubtseva N, Chingin K, Chen H, et al. Vertical Transmission of SARS-CoV-2 in Second Trimester Associated with Severe Neonatal Pathology. Viruses 2021, 13, 447. [Google Scholar] [CrossRef]
- National Academies of Sciences, Engineering and M. Dietary Reference Intakes tables and application. http://nationalacademies.org/hmd/Activities/Nutrition/SummaryDRIs/DRI-Tables.aspx.
- Chaari A, Bendriss G, Zakaria D, McVeigh C. Importance of Dietary Changes During the Coronavirus Pandemic: How to Upgrade Your Immune Response. Front Public Heal, 2020; 8. [CrossRef]
- Tsoupras A, Lordan R, Zabetakis I. Thrombosis and COVID-19: The Potential Role of Nutrition. Front Nutr 2020, 7. [CrossRef]
- Giannakou K, Evangelou E, Yiallouros P, Christophi CA, Middleton N, Papatheodorou E, et al. Risk factors for gestational diabetes: An umbrella review of meta-analyses of observational studies. PLoS One 2019, 14, e0215372. [Google Scholar] [CrossRef]
- Christian LM, Porter K. Longitudinal changes in serum proinflammatory markers across pregnancy and postpartum: Effects of maternal body mass index. Cytokine 2014, 70, 134–140. [Google Scholar] [CrossRef] [PubMed]
- Eskenazi B, Rauch S, Iurlaro E, Gunier RB, Rego A, Gravett MG, et al. Diabetes mellitus, maternal adiposity, and insulin-dependent gestational diabetes are associated with COVID-19 in pregnancy: the INTERCOVID study. Am J Obstet Gynecol 2022, 227, 74.e1–74.e16. [Google Scholar] [CrossRef]
- Liu P, Zheng J, Yang P, Wang X, Wei C, Zhang S, et al. The immunologic status of newborns born to SARS-CoV-2–infected mothers in Wuhan, China. J Allergy Clin Immunol 2020, 146, 101–109.e1. [Google Scholar] [CrossRef] [PubMed]
- Villar J, Ariff S, Gunier RB, Thiruvengadam R, Rauch S, Kholin A, et al. Maternal and Neonatal Morbidity and Mortality Among Pregnant Women With and Without COVID-19 Infection. JAMA Pediatr 2021, 175, 817. [Google Scholar] [CrossRef]
- Zhao P, Praissman JL, Grant OC, Cai Y, Xiao T, Rosenbalm KE, et al. Virus-Receptor Interactions of Glycosylated SARS-CoV-2 Spike and Human ACE2 Receptor. Cell Host Microbe 2020, 28, 586–601.e6. [Google Scholar] [CrossRef]
- Maiorino MI, Bellastella G, Longo M, Caruso P, Esposito K. Mediterranean Diet and COVID-19: Hypothesizing Potential Benefits in People With Diabetes. Front Endocrinol (Lausanne) 2020, 11. [CrossRef]
- Franquesa M, Pujol-Busquets G, García-Fernández E, Rico L, Shamirian-Pulido L, Aguilar-Martínez A, et al. Mediterranean Diet and Cardiodiabesity: A Systematic Review through Evidence-Based Answers to Key Clinical Questions. Nutrients 2019, 11, 655. [Google Scholar] [CrossRef]
- Ajala O, English P, Pinkney J. Systematic review and meta-analysis of different dietary approaches to the management of type 2 diabetes. Am J Clin Nutr 2013, 97, 505–516. [Google Scholar] [CrossRef]
- Peluso I, Romanelli L, Palmery M. Interactions between prebiotics, probiotics, polyunsaturated fatty acids and polyphenols: diet or supplementation for metabolic syndrome prevention? Int J Food Sci Nutr 2014, 65, 259–267. [Google Scholar] [CrossRef]
- Holick MF, Binkley NC, Bischoff-Ferrari HA, Gordon CM, Hanley DA, Heaney RP, et al. Evaluation, Treatment, and Prevention of Vitamin D Deficiency: an Endocrine Society Clinical Practice Guideline. J Clin Endocrinol Metab 2011, 96, 1911–1930. [Google Scholar] [CrossRef]
- Mercola J, Grant WB, Wagner CL. Evidence Regarding Vitamin D and Risk of COVID-19 and Its Severity. Nutrients 2020, 12, 3361. [Google Scholar] [CrossRef] [PubMed]
- Szarpak L, Filipiak KJ, Gasecka A, Gawel W, Koziel D, Jaguszewski MJ, et al. Vitamin D supplementation to treat SARS-CoV-2 positive patients. Evidence from meta-analysis. Cardiol J 2022, 29, 188–196. [Google Scholar] [CrossRef]
- Manca A, Cosma S, Palermiti A, Costanzo M, Antonucci M, De Vivo ED, et al. Pregnancy and COVID-19: The Possible Contribution of Vitamin D. Nutrients 2022, 14, 3275. [Google Scholar] [CrossRef] [PubMed]
- Sinaci S, Ocal DF, Yucel Yetiskin DF, Uyan Hendem D, Buyuk GN, Goncu Ayhan S, et al. Impact of vitamin D on the course of COVID-19 during pregnancy: A case control study. J Steroid Biochem Mol Biol 2021, 213, 105964. [Google Scholar] [CrossRef]
- Dahma G, Craina M, Dumitru C, Neamtu R, Popa ZL, Gluhovschi A, et al. A Prospective Analysis of Vitamin D Levels in Pregnant Women Diagnosed with Gestational Hypertension after SARS-CoV-2 Infection. J Pers Med 2023, 13, 1–13. [Google Scholar] [CrossRef]
- Lian R-H, Qi P-A, Yuan T, Yan P-J, Qiu W-W, Wei Y, et al. Systematic review and meta-analysis of vitamin D deficiency in different pregnancy on preterm birth. Medicine (Baltimore) 2021, 100, e26303. [Google Scholar] [CrossRef]
- Al-Kaleel A, Al-Gailani L, Demir M, Aygün H. Vitamin D may prevent COVID-19 induced pregnancy complication. Med Hypotheses 2022, 158, 2021–2023. [Google Scholar] [CrossRef]
- Szarpak L, Feduniw S, Pruc M, Ciebiera M, Cander B, Rahnama-Hezavah M, et al. The Vitamin D Serum Levels in Pregnant Women Affected by COVID-19: A Systematic Review and Meta-Analysis. Nutrients 2023, 15, 1–13. [CrossRef]
- Parisa G, Soliman M-S, Afsaneh V. Micronutrients Supplementation in Pregnant Women during COVID-19 Pandemy: Pros and Cons. Trends Pharm Sci 2021, 7, 153–160. [CrossRef]
- Bastos Maia S, Rolland Souza A, Costa Caminha M, Lins da Silva S, Callou Cruz R, Carvalho dos Santos C, et al. Vitamin A and Pregnancy: A Narrative Review. Nutrients 2019, 11, 681. [Google Scholar] [CrossRef]
- Nawsherwan N, Khan S, Zeb F, Shoain M, Nabi G, Ul HI et al. Selected Micronutrients: An Option to Boost Immunity against COVID-19 and Prevent Adverse Pregnancy Outcomes in Pregnant Women: A Narrative Review. Iran J Public Health 2020. [CrossRef]
- Rumbold A, Ota E, Nagata C, Shahrook S, Crowther CA. Vitamin C supplementation in pregnancy. Cochrane Database Syst Rev 2015, 2016. [CrossRef]
- Erol SA, Tanacan A, Anuk AT, Tokalioglu EO, Biriken D, Keskin HL, et al. Evaluation of maternal serum afamin and vitamin E levels in pregnant women with COVID-19 and its association with composite adverse perinatal outcomes. J Med Virol 2021, 93, 2350–2358. [Google Scholar] [CrossRef] [PubMed]
- Shim E, Park E. Choline intake and its dietary reference values in Korea and other countries: a review. Nutr Res Pract 2022, 16, S126. [Google Scholar] [CrossRef]
- Zeisel, SH. Choline: Critical Role During Fetal Development and Dietary Requirements in Adults. Annu Rev Nutr 2006, 26, 229–250. [Google Scholar] [CrossRef]
- Hoffman MC, Freedman R, Law AJ, Clark AM, Hunter SK. Maternal nutrients and effects of gestational COVID-19 infection on fetal brain development. Clin Nutr ESPEN 2021, 43, 1–8. [Google Scholar] [CrossRef]
- Germano C, Messina A, Tavella E, Vitale R, Avellis V, Barboni M, et al. Fetal Brain Damage during Maternal COVID-19: Emerging Hypothesis, Mechanism, and Possible Mitigation through Maternal-Targeted Nutritional Supplementation. Nutrients 2022, 14, 3303. [Google Scholar] [CrossRef]
- Chu D-M, Wahlqvist ML, Chang H-Y, Yeh N-H, Lee M-S. Choline and betaine food sources and intakes in Taiwanese. Asia Pac J Clin Nutr 2012, 21, 547–557. [Google Scholar]
- Brunst KJ, Wright RO, DiGioia K, Enlow MB, Fernandez H, Wright RJ, et al. Racial/ethnic and sociodemographic factors associated with micronutrient intakes and inadequacies among pregnant women in an urban US population. Public Health Nutr 2014, 17, 1960–1970. [Google Scholar] [CrossRef]
- Fischer LM, da Costa KA, Galanko J, Sha W, Stephenson B, Vick J, et al. Choline intake and genetic polymorphisms influence choline metabolite concentrations in human breast milk and plasma. Am J Clin Nutr 2010, 92, 336–346. [Google Scholar] [CrossRef]
- World Health Organization. Guideline: Daily Iron and Folic Acid Supplementation in Pregnant Women. Vol. 7. 153-160. 2012.
- VanderMeulen H, Strauss R, Lin Y, McLeod A, Barrett J, Sholzberg M, et al. The contribution of iron deficiency to the risk of peripartum transfusion: a retrospective case control study. BMC Pregnancy Childbirth 2020, 20, 196. [Google Scholar] [CrossRef]
- Uta M, Neamtu R, Bernad E, Mocanu AG, Gluhovschi A, Popescu A, et al. The Influence of Nutritional Supplementation for Iron Deficiency Anemia on Pregnancies Associated with SARS-CoV-2 Infection. Nutrients 2022, 14, 836. [Google Scholar] [CrossRef] [PubMed]
- Stoffel NU, Von Siebenthal HK, Moretti D, Zimmermann MB. Oral iron supplementation in iron-deficient women: How much and how often? Mol Aspects Med 2020, 75, 100865. [Google Scholar] [CrossRef] [PubMed]
- Wessels I, Maywald M, Rink L. Zinc as a Gatekeeper of Immune Function. Nutrients 2017, 9, 1286. [Google Scholar] [CrossRef]
- Chaffee BW, King JC. Effect of Zinc Supplementation on Pregnancy and Infant Outcomes: A Systematic Review. Paediatr Perinat Epidemiol 2012, 26, 118–137. [Google Scholar] [CrossRef]
- Fanni D, Gerosa C, Nurchi VM, Manchia M, Saba L, Coghe F, et al. The Role of Magnesium in Pregnancy and in Fetal Programming of Adult Diseases. Biol Trace Elem Res 2021, 199, 3647–3657. [Google Scholar] [CrossRef]
- World Health Organization. Geneva S. WHO Recommendations on Antenatal Care for a Positive Pregnancy Experience 2016.
- Citu IM, Citu C, Margan M-M, Craina M, Neamtu R, Gorun OM, et al. Calcium, Magnesium, and Zinc Supplementation during Pregnancy: The Additive Value of Micronutrients on Maternal Immune Response after SARS-CoV-2 Infection. Nutrients 2022, 14, 1445. [Google Scholar] [CrossRef]
- Taheri M, Bahrami A, Habibi P, Nouri F. A Review on the Serum Electrolytes and Trace Elements Role in the Pathophysiology of COVID-19. Biol Trace Elem Res 2021, 199, 2475–2481. [Google Scholar] [CrossRef]
- Martha JW, Wibowo A, Pranata R. Hypocalcemia is associated with severe COVID-19: A systematic review and meta-analysis. Diabetes Metab Syndr Clin Res Rev 2021, 15, 337–342. [Google Scholar] [CrossRef]
- Tanacan A, Erol SA, Anuk AT, Yetiskin FDY, Tokalioglu EO, Sahin S, et al. The Association of Serum Electrolytes with Disease Severity and Obstetric Complications in Pregnant Women with COVID-19: a Prospective Cohort Study from a Tertiary Reference Center. Geburtshilfe Frauenheilkd 2022, 82, 326–332. [Google Scholar] [CrossRef] [PubMed]
- Kiełczykowska M, Kocot J, Paździor M, Musik I. Selenium - a fascinating antioxidant of protective properties. Adv Clin Exp Med 2018, 27, 245–255. [Google Scholar] [CrossRef] [PubMed]
- Hasani M, Djalalinia S, Khazdooz M, Asayesh H, Zarei M, Gorabi AM, et al. Effect of selenium supplementation on antioxidant markers: a systematic review and meta-analysis of randomized controlled trials. Hormones 2019, 18, 451–462. [Google Scholar] [CrossRef] [PubMed]
- Moghaddam A, Heller R, Sun Q, Seelig J, Cherkezov A, Seibert L, et al. Selenium Deficiency Is Associated with Mortality Risk from COVID-19. Nutrients 2020, 12, 2098. [Google Scholar] [CrossRef]
- Zhang J, Taylor EW, Bennett K, Saad R, Rayman MP. Association between regional selenium status and reported outcome of COVID-19 cases in China. Am J Clin Nutr 2020, 111, 1297–1299. [Google Scholar] [CrossRef]
- Erol SA, Polat N, Akdas S, Aribal Ayral P, Anuk AT, Ozden Tokalioglu E, et al. Maternal selenium status plays a crucial role on clinical outcomes of pregnant women with COVID-19 infection. J Med Virol 2021, 93, 5438–5445. [Google Scholar] [CrossRef]
- Kipp AP, Strohm D, Brigelius-Flohé R, Schomburg L, Bechthold A, Leschik-Bonnet E, et al. Revised reference values for selenium intake. J Trace Elem Med Biol 2015, 32, 195–199. [Google Scholar] [CrossRef]
- Schomburg, L. Selenium Deficiency Due to Diet, Pregnancy, Severe Illness, or COVID-19—A Preventable Trigger for Autoimmune Disease. Int J Mol Sci 2021, 22, 8532. [Google Scholar] [CrossRef]
- Wong SF, Chow KM, Leung TN, Ng WF, Ng TK, Shek CC, et al. Pregnancy and perinatal outcomes of women with severe acute respiratory syndrome. Am J Obstet Gynecol 2004, 191, 292–297. [Google Scholar] [CrossRef]
- Yeoh YK, Zuo T, Lui GC-Y, Zhang F, Liu Q, Li AY, et al. Gut microbiota composition reflects disease severity and dysfunctional immune responses in patients with COVID-19. Gut 2021, 70, 698–706. [Google Scholar] [CrossRef]
- Dhar D, Mohanty A. Gut microbiota and Covid-19- possible link and implications. Virus Res 2020, 285, 198018. [Google Scholar] [CrossRef] [PubMed]
- Batista KS, de Albuquerque JG, Vasconcelos MHA de, Bezerra MLR, da Silva Barbalho MB, Pinheiro RO, et al. Probiotics and prebiotics: potential prevention and therapeutic target for nutritional management of COVID-19? Nutr Res Rev 2023, 36, 181–198. [Google Scholar] [CrossRef] [PubMed]
- Peters VBM, van de Steeg E, van Bilsen J, Meijerink M. Mechanisms and immunomodulatory properties of pre- and probiotics. Benef Microbes 2019, 10, 225–236. [CrossRef] [PubMed]
- Tang L, Gu S, Gong Y, Li B, Lu H, Li Q, et al. Clinical Significance of the Correlation between Changes in the Major Intestinal Bacteria Species and COVID-19 Severity. Engineering 2020, 6, 1178–1184. [Google Scholar] [CrossRef]
- Juárez-Castelán CJ, Vélez-Ixta JM, Corona-Cervantes K, Piña-Escobedo A, Cruz-Narváez Y, Hinojosa-Velasco A, et al. The Entero-Mammary Pathway and Perinatal Transmission of Gut Microbiota and SARS-CoV-2. Int J Mol Sci 2022, 23, 10306. [Google Scholar] [CrossRef]
- Leftwich HK, Vargas-Robles D, Rojas-Correa M, Yap YR, Bhattarai S, Ward D V. , et al. The microbiota of pregnant women with SARS-CoV-2 and their infants. Microbiome 2023, 11, 141. [Google Scholar] [CrossRef]
- Rodríguez, JM. The origin of human milk bacteria: is there a bacterial entero-mammary pathway during late pregnancy and lactation? Adv Nutr 2014, 5, 779–784. [Google Scholar] [CrossRef]
- Gernand AD, Schulze KJ, Stewart CP, West KP, Christian P. Micronutrient deficiencies in pregnancy worldwide: health effects and prevention. Nat Rev Endocrinol 2016, 12, 274–289. [Google Scholar] [CrossRef]
- Zhang P, He Z, Yu G, Peng D, Feng Y, Ling J, et al. The modified NUTRIC score can be used for nutritional risk assessment as well as prognosis prediction in critically ill COVID-19 patients. Clin Nutr 2021, 40, 534–541. [Google Scholar] [CrossRef]
- Fedullo AL, Schiattarella A, Morlando M, Raguzzini A, Toti E, De Franciscis P, et al. Mediterranean Diet for the Prevention of Gestational Diabetes in the Covid-19 Era: Implications of Il-6 In Diabesity. Int J Mol Sci 2021, 22, 1213. [Google Scholar] [CrossRef]
- Mate A, Reyes-Goya C, Santana-Garrido Á, Sobrevia L, Vázquez CM. Impact of maternal nutrition in viral infections during pregnancy. Biochim Biophys Acta - Mol Basis Dis 2021, 1867, 166231. [Google Scholar] [CrossRef]
- Ramirez Zegarra R, Dall’Asta A, Revelli A, Ghi T. COVID-19 and Gestational Diabetes: The Role of Nutrition and Pharmacological Intervention in Preventing Adverse Outcomes. Nutrients 2022, 14, 3562. [Google Scholar] [CrossRef] [PubMed]
- Walton GE, Gibson GR, Hunter KA. Mechanisms linking the human gut microbiome to prophylactic and treatment strategies for COVID-19. Br J Nutr 2021, 126, 219–227. [Google Scholar] [CrossRef]
- Vernocchi P, Del Chierico F, Putignani L. Gut Microbiota Metabolism and Interaction with Food Components. Int J Mol Sci 2020, 21, 3688. [Google Scholar] [CrossRef]
- Xavier-Santos D, Padilha M, Fabiano GA, Vinderola G, Gomes Cruz A, Sivieri K, et al. Evidences and perspectives of the use of probiotics, prebiotics, synbiotics, and postbiotics as adjuvants for prevention and treatment of COVID-19: A bibliometric analysis and systematic review. Trends Food Sci Technol 2022, 120, 174–192. [Google Scholar] [CrossRef]
- Alesci A, Pergolizzi S, Fumia A, Miller A, Cernigliaro C, Zaccone M, et al. Immune System and Psychological State of Pregnant Women during COVID-19 Pandemic: Are Micronutrients Able to Support Pregnancy? Nutrients 2022, 14, 2534. [Google Scholar] [CrossRef]
- Milani GP, Macchi M, Guz-Mark A. Vitamin C in the Treatment of COVID-19. Nutrients 2021, 13. [CrossRef]
- Skolmowska D, Głąbska D, Kołota A, Guzek D. Effectiveness of Dietary Interventions in Prevention and Treatment of Iron-Deficiency Anemia in Pregnant Women: A Systematic Review of Randomized Controlled Trials. Nutrients 2022, 14, 3023. [Google Scholar] [CrossRef]
- Salute ministero della Salute. Gravidanza fisiologica 2010.Accessed August 2024. ttps://www.salute.gov.it/imgs/C_17_pubblicazioni_1436_allegato.pdf.
- Pechlivanidou E, Vlachakis D, Tsarouhas K, Panidis D, Tsitsimpikou C, Darviri C, et al. The prognostic role of micronutrient status and supplements in COVID-19 outcomes: A systematic review. Food Chem Toxicol 2022, 162, 112901. [Google Scholar] [CrossRef]
- Alemzadeh E, Alemzadeh E, Ziaee M, Abedi A, Salehiniya H. The effect of low serum calcium level on the severity and mortality of Covid patients: A systematic review and meta-analysis. Immunity, Inflamm Dis 2021, 9, 1219–1228. [Google Scholar] [CrossRef]
- Tay MZ, Poh CM, Rénia L, MacAry PA, Ng LFP. The trinity of COVID-19: immunity, inflammation and intervention. Nat Rev Immunol 2020, 20, 363–374. [Google Scholar] [CrossRef] [PubMed]
- Freedman R, Hunter SK, Law AJ, Wagner BD, D’Alessandro A, Christians U, et al. Higher Gestational Choline Levels in Maternal Infection Are Protective for Infant Brain Development. J Pediatr 2019, 208, 198–206.e2. [Google Scholar] [CrossRef]

Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).



