Submitted:
12 November 2024
Posted:
15 November 2024
You are already at the latest version
Abstract
Radiation has been used to treat meningiomas since the mid-1970s. Traditionally, radiation was reserved for patients unfit for major surgery or those with surgically inaccessible tumors. With an increased quantity and quality of imaging and an aging population, there has been a rise in incidentally diagnosed meningiomas in patients with smaller tumors at the time of diagnosis. Deciding if, how, and when to intervene must be determined on a case-by-case basis. Anatomical location and adjacent vital structures are crucial for decision-making. Prior review articles have detailed outcomes of radiosurgery in broad anatomical regions such as the skull base, but there has been a deluge of recent research on increasingly specific anatomical subregions. This review synthesizes information regarding specific anatomical subregions, including anatomical challenges, radiosurgical outcomes, and unique considerations. We utilized the highest levels of evidence available for each region, discuss details of published research, and explore future directions. Meningioma management remains individualized based on patient comorbidities, tumor location/characteristics, symptomatic burden, and patient age. In addition to SRS’s established role for surgically inaccessible, recurrent, and high-grade meningiomas, the use of SRS as upfront management for small asymptomatic meningiomas is increasingly investigated. For all sub-regions reported, radiosurgical intervention resulted in high tumor control rates and acceptably low adverse radiation events.
Keywords:
1. Introduction
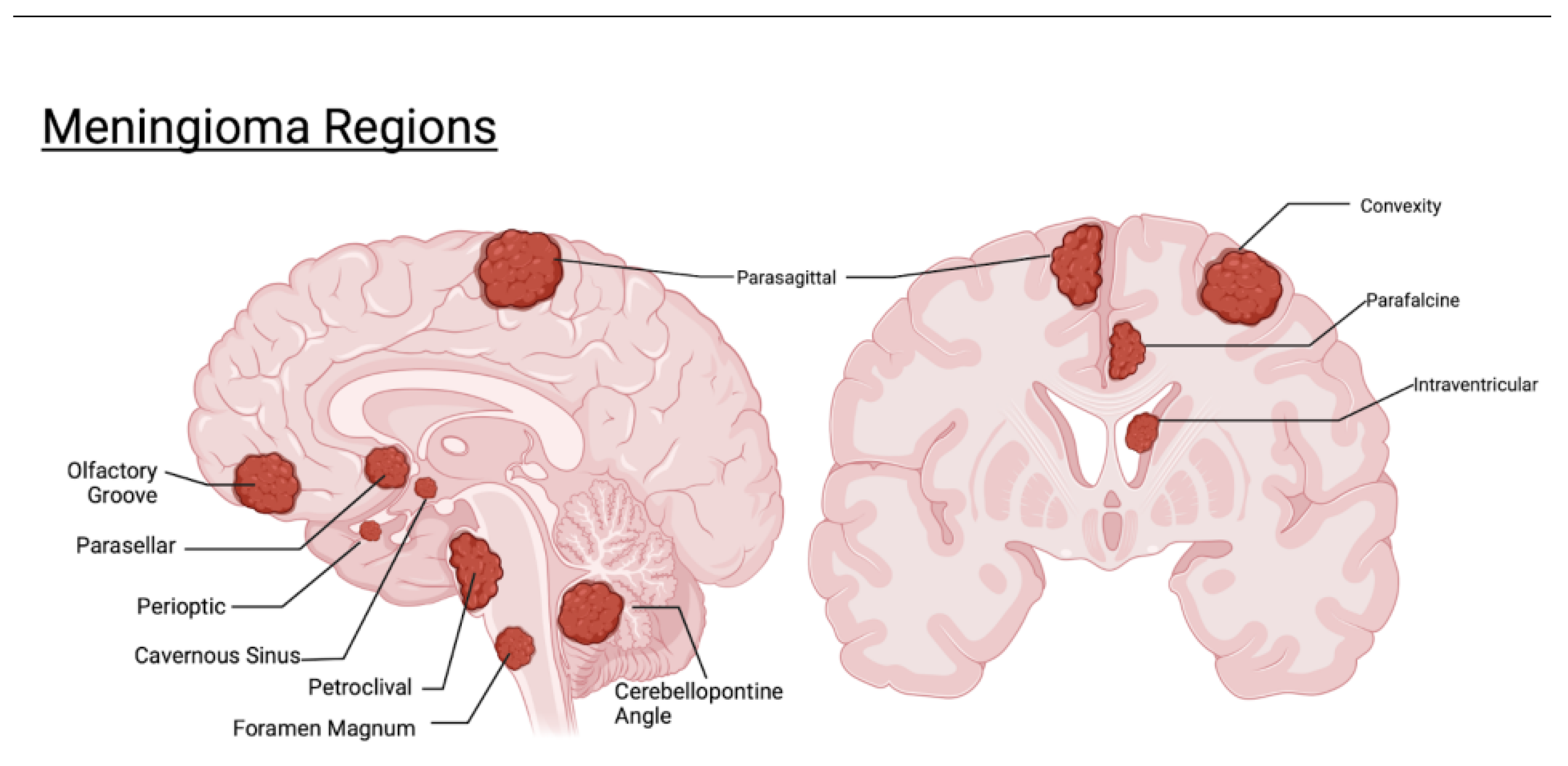
2. Classification by Location
3. Guidelines for Meningioma Treatment
4. Anatomical Locations and Updated Evidence
4.1. Parafalcine and Parasagittal
4.2. Convexity
4.3. Cavernous Sinus
4.4. Parasellar
4.5. Perioptic
4.6. Petroclival
4.7. Clinoidal
4.8. Intraventricular
4.9. Olfactory Groove
4.10. Cerebellopontine
4.11. Foramen Magnum
5. Discussion
5.1. Observation, Radiation, or Surgery
5.2. Radiation Dose and Technique
| Anatomical Location | Mean Marginal Dose (Single Session) | Mean Marginal Dose (Fractionated) |
|---|---|---|
| Parafalcine / Parasagittal | 14-18 Gy [45] | N/A |
| Convexity | 13.26 Gy [48] | 25 Gy (5 fractions) or 50.4 Gy (28 fractions) [104] |
| Cavernous Sinus | 12-14 Gy [55] | 51.2 Gy (15.5 sessions) [105] |
| Parasellar | 12-14 Gy [59,61] | 25-30 Gy (5-6 sessions) [33] |
| Perioptic | 10-12 Gy [63] | 25 Gy (5 sessions) [63] |
| Petroclival | 15 Gy [19] | N/A |
| Clinoidal | 12 Gy [76,78] | 25 Gy (5 sessions) [77] |
| Intraventricular | 12-16 Gy [79] | N/A |
| Olfactory Groove | 12 Gy [22] | 25 Gy (5 sessions) [86] |
| Cerebellopontine Angle | 12-15 Gy [36] | N/A |
| Foramen Magnum | 12-14 Gy [25] | 20 Gy (5 sessions) [25] |
5.3. Predicting Response to Radiation
5.4. Timing of Radiation Intervention
5.5. Future Treatment Horizons
6. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Buerki RA, Horbinski CM, Kruser T, Horowitz PM, James CD, Lukas RV. An overview of meningiomas. Future Oncol. 2018;14(21):2161-2177. [CrossRef]
- Bhat AR, Wani MA, Kirmani AR, Ramzan AU. Histological-subtypes and anatomical location correlated in meningeal brain tumors (meningiomas). J Neurosci Rural Pract. 2014;5(3):244-249. [CrossRef]
- Ostrom QT, Francis SS, Barnholtz-Sloan JS. Epidemiology of Brain and Other CNS Tumors. Curr Neurol Neurosci Rep. 2021;21(12):68. [CrossRef]
- Singh V, Bluestone A, Chen D, Shah A, Linden C, Bangiyev L. Meningiomas: Variations and Clinical Presentations.
- Wiemels J, Wrensch M, Claus EB. Epidemiology and etiology of meningioma. J Neurooncol. 2010;99(3):307-314. [CrossRef]
- Yarabarla V, Mylarapu A, Han TJ, McGovern SL, Raza SM, Beckham TH. Intracranial meningiomas: an update of the 2021 World Health Organization classifications and review of management with a focus on radiation therapy. Front Oncol. 2023;13:1137849. [CrossRef]
- Agarwal V, McCutcheon BA, Hughes JD, et al. Trends in Management of Intracranial Meningiomas: Analysis of 49,921 Cases from Modern Cohort. World Neurosurg. 2017;106:145-151. [CrossRef]
- Pinzi V, Biagioli E, Roberto A, et al. Radiosurgery for intracranial meningiomas: A systematic review and meta-analysis. Crit Rev Oncol Hematol. 2017;113:122-134. [CrossRef]
- McGregor JM, Sarkar A. Stereotactic Radiosurgery and Stereotactic Radiotherapy in the Treatment of Skull Base Meningiomas. Otolaryngol Clin North Am. 2009;42(4):677-688. [CrossRef]
- Ding D, Xu Z, McNeill IT, Yen CP, Sheehan JP. Radiosurgery for parasagittal and parafalcine meningiomas: Clinical article. J Neurosurg. 2013;119(4):871-877. [CrossRef]
- Goldsmith BJ, Wara WM, Wilson CB, Larson DA. Postoperative irradiation for subtotally resected meningiomas: A retrospective analysis of 140 patients treated from 1967 to 1990. J Neurosurg. 1994;80(2):195-201. [CrossRef]
- Wu A, Garcia MA, Magill ST, et al. Presenting Symptoms and Prognostic Factors for Symptomatic Outcomes Following Resection of Meningioma. World Neurosurg. 2018;111:e149-e159. [CrossRef]
- Sheehan JP, Williams BJ, Yen CP. Stereotactic radiosurgery for WHO grade I meningiomas. J Neurooncol. 2010;99(3):407-416. [CrossRef]
- Ruge MI, Tutunji J, Rueß D, et al. Stereotactic radiosurgery for treating meningiomas eligible for complete resection. Radiat Oncol. 2021;16(1):22. [CrossRef]
- Tuleasca C, Ruess D, Ruge M, Régis J. Stereotactic Therapies for Meningiomas. Adv Exp Med Biol. 2023;1416:107-119. [CrossRef]
- Goldbrunner R, Stavrinou P, Jenkinson MD, et al. EANO guideline on the diagnosis and management of meningiomas. Neuro-Oncol. 2021;23(11):1821-1834. [CrossRef]
- NAKASU S, NAKASU Y. Natural History of Meningiomas: Review with Meta-analyses. Neurol Med Chir (Tokyo). 2020;60(3):109-120. [CrossRef]
- Graillon T, Regis J, Barlier A, Brue T, Dufour H, Buchfelder M. Parasellar Meningiomas. Neuroendocrinology. 2020;110(9-10):780-796. [CrossRef]
- Wijaya JH, Arjuna YYE, July J. The role of stereotactic radiosurgery in the management of petroclival meningioma: a systematic review. J Neurooncol. 2022;159(1):33-42. [CrossRef]
- Mantziaris G, Pikis S, Bunevicius A, et al. Stereotactic radiosurgery for asymptomatic petroclival region meningiomas: a focused analysis from the IMPASSE study. Acta Neurochir (Wien). 2022;164(1):273-279. [CrossRef]
- Bin Alamer O, Palmisciano P, Mallela AN, et al. Stereotactic radiosurgery in the management of petroclival meningiomas: a systematic review and meta-analysis of treatment outcomes of primary and adjuvant radiosurgery. J Neurooncol. 2022;157(2):207-219. [CrossRef]
- Bunevicius A, Ahn J, Fribance S, et al. Stereotactic Radiosurgery for Olfactory Groove Meningiomas: An International, Multicenter Study. Neurosurgery. 2021;89(5):784-791. [CrossRef]
- Karaaslan B, Celtici E, Bulduk EB, et al. Stereotactic radiosurgery after subtotal resection of critically located grade i meningioma: a single-center experience and review of literature. Turk Neurosurg. Published online 2020. [CrossRef]
- Gande A, Kano H, Bowden G, et al. Gamma Knife radiosurgery of olfactory groove meningiomas provides a method to preserve subjective olfactory function. J Neurooncol. 2014;116(3):577-583. [CrossRef]
- Karras CL, Texakalidis P, Nie JZ, et al. Outcomes following stereotactic radiosurgery for foramen magnum meningiomas: a single-center experience and systematic review of the literature. Neurosurg Focus. 2022;53(5):E6. [CrossRef]
- Akyoldaş G, Samancı Y, Yılmaz M, Şengöz M, Peker S. Long-term results of gamma knife radiosurgery for foramen magnum meningiomas. Neurosurg Rev. 2021;44(5):2667-2673. [CrossRef]
- Malone J, Gaviolli E, Doody J, Sinclair J, Malone S. Unresectable Foramen Magnum Meningioma Treated with CyberKnife Robotic Stereotactic Radiosurgery. Cureus. Published online June 2, 2020. [CrossRef]
- Mehta GU, Zenonos G, Patibandla MR, et al. Outcomes of stereotactic radiosurgery for foramen magnum meningiomas: an international multicenter study. J Neurosurg. 2018;129(2):383-389. [CrossRef]
- Sun C, Dou Z, Wu J, et al. The Preferred Locations of Meningioma According to Different Biological Characteristics Based on Voxel-Wise Analysis. Front Oncol. 2020;10:1412. [CrossRef]
- Ogasawara C, Philbrick BD, Adamson DC. Meningioma: A Review of Epidemiology, Pathology, Diagnosis, Treatment, and Future Directions. Biomedicines. 2021;9(3):319. [CrossRef]
- Casali C, Del Bene M, DiMeco F. Falcine meningiomas. In: Handbook of Clinical Neurology. Vol 170. Elsevier; 2020:101-106. [CrossRef]
- Abdallah HM, Mallela AN, Wei Z, Abou-Al-Shaar H, Niranjan A, Lunsford LD. Gamma Knife radiosurgery for meningiomas of the confluence of the falx and tentorium. J Neurooncol. 2023;161(2):225-233. [CrossRef]
- Matoušek P, Cvek J, Čábalová L, et al. Does Endoscopic Transnasal Optic Nerve Decompression Followed by Radiosurgery Improve Outcomes in the Treatment of Parasellar Meningiomas? Medicina (Mex). 2022;58(8):1137. [CrossRef]
- Valencia-Ramos C, Arroyo Del Castillo JG, Aragon JF, et al. Prognostic Factors in the Surgery of Clinoidal Meningiomas. Cureus. Published online June 8, 2023. [CrossRef]
- Umekawa M, Shinya Y, Hasegawa H, Katano A, Saito N. Primary Stereotactic Radiosurgery Provides Favorable Tumor Control for Intraventricular Meningioma: A Retrospective Analysis. J Clin Med. 2023;12(3):1068. [CrossRef]
- Gendreau JL, Sheaffer K, Macdonald N, et al. Stereotactic radiosurgery for cerebellopontine meningiomas: a systematic review and meta-analysis. Br J Neurosurg. 2023;37(2):199-205. [CrossRef]
- Glenn CA, Tullos HJ, Sughrue ME. Natural history of intracranial meningiomas. In: Handbook of Clinical Neurology. Vol 169. Elsevier; 2020:205-227. [CrossRef]
- Hashimoto N, Rabo CS, Okita Y, et al. Slower growth of skull base meningiomas compared with non-skull base meningiomas based on volumetric and biological studies. J Neurosurg. 2012;116(3):574-580. [CrossRef]
- Lee EJ, Kim JH, Park ES, et al. A novel weighted scoring system for estimating the risk of rapid growth in untreated intracranial meningiomas. J Neurosurg. 2017;127(5):971-980. [CrossRef]
- Delgado-López PD, Montalvo-Afonso A, Martín-Alonso J, et al. Volumetric growth rate of incidental asymptomatic meningiomas: a single-center prospective cohort study. Acta Neurochir (Wien). 2021;163(6):1665-1675. [CrossRef]
- Sheehan J, Pikis S, Islim AI, et al. An international multicenter matched cohort analysis of incidental meningioma progression during active surveillance or after stereotactic radiosurgery: the IMPASSE study. Neuro-Oncol. 2022;24(1):116-124. [CrossRef]
- Bair MM, Munakomi S. Neuroanatomy, Falx Cerebri. In: StatPearls. StatPearls Publishing; 2024. Accessed February 6, 2024. http://www.ncbi.nlm.nih.gov/books/NBK545304/.
- Kong X, Gong S, Lee IT, Yang Y. Microsurgical treatment of parafalcine meningiomas: a retrospective study of 126 cases. OncoTargets Ther. 2018;11:5279-5285. [CrossRef]
- Mathiesen T. Chapter 9 - Parasagittal meningiomas. In: McDermott MW, ed. Handbook of Clinical Neurology. Vol 170. Meningiomas, Part II. Elsevier; 2020:93-100. [CrossRef]
- Pinzi V, Fariselli L, Marchetti M, Scorsetti M, Navarria P. Stereotactic Radiotherapy for Parasagittal and Parafalcine Meningiomas: Patient Selection and Special Considerations. Cancer Manag Res. 2019;Volume 11:10051-10060. [CrossRef]
- Sarris C, Sanai N. Convexity meningioma resection in the modern neurosurgical era. In: Handbook of Clinical Neurology. Vol 170. Elsevier; 2020:87-92. [CrossRef]
- Kondziolka D, Madhok R, Lunsford LD, et al. Stereotactic radiosurgery for convexity meningiomas: Clinical article. J Neurosurg. 2009;111(3):458-463. [CrossRef]
- Pikis S, Mantziaris G, Islim AI, et al. Stereotactic radiosurgery versus active surveillance for incidental, convexity meningiomas: a matched cohort analysis from the IMPASSE study. J Neurooncol. 2022;157(1):121-128. [CrossRef]
- Ruiz-Garcia H, Trifiletti DM, Mohammed N, et al. Convexity Meningiomas in Patients with Neurofibromatosis Type 2: Long-Term Outcomes After Gamma Knife Radiosurgery. World Neurosurg. 2021;146:e678-e684. [CrossRef]
- Ngnitewe Massa R, Minutello K, Mesfin FB. Neuroanatomy, Cavernous Sinus. In: StatPearls. StatPearls Publishing; 2024. Accessed February 6, 2024. http://www.ncbi.nlm.nih.gov/books/NBK459244/.
- Park KJ, Kano H, Iyer A, et al. Gamma Knife stereotactic radiosurgery for cavernous sinus meningioma: long-term follow-up in 200 patients. J Neurosurg. 2019;130(6):1799-1808. [CrossRef]
- Basak A, Ozbek M. Single-Fraction Gamma-Knife Radiosurgery with or without Previous Surgery for Cavernous Sinus Meningiomas: A Single-Center Experience and Systematic Literature Review. Niger J Clin Pract. 2023;26(5):545-551. [CrossRef]
- Zeiler FA, McDonald PJ, Kaufmann AM, et al. Gamma Knife Radiosurgery of Cavernous Sinus Meningiomas: An Institutional Review. Can J Neurol Sci J Can Sci Neurol. 2012;39(6):757-762. [CrossRef]
- Sughrue ME, Rutkowski MJ, Aranda D, Barani IJ, McDermott MW, Parsa AT. Treatment decision making based on the published natural history and growth rate of small meningiomas: A review and meta-analysis. J Neurosurg. 2010;113(5):1036-1042. [CrossRef]
- Fariselli L, Biroli A, Signorelli A, Broggi M, Marchetti M, Biroli F. The cavernous sinus meningiomas’ dilemma: Surgery or stereotactic radiosurgery? Rep Pract Oncol Radiother. 2016;21(4):379-385. [CrossRef]
- Sughrue ME, Rutkowski MJ, Aranda D, Barani IJ, McDermott MW, Parsa AT. Factors affecting outcome following treatment of patients with cavernous sinus meningiomas: Clinical article. J Neurosurg. 2010;113(5):1087-1092. [CrossRef]
- Spiegelmann R, Cohen ZR, Nissim O, Alezra D, Pfeffer R. Cavernous sinus meningiomas: a large LINAC radiosurgery series. J Neurooncol. 2010;98(2):195-202. [CrossRef]
- Kimball MM, Friedman WA, Foote KD, Bova FJ, Chi YY. Linear Accelerator Radiosurgery for Cavernous Sinus Meningiomas. Stereotact Funct Neurosurg. 2009;87(2):120-127. [CrossRef]
- Cohen-Inbar O, Tata A, Moosa S, Lee C chia, Sheehan JP. Stereotactic radiosurgery in the treatment of parasellar meningiomas: long-term volumetric evaluation. J Neurosurg. 2018;128(2):362-372. [CrossRef]
- Sheehan JP, Starke RM, Kano H, et al. Gamma Knife radiosurgery for sellar and parasellar meningiomas: a multicenter study: Clinical article. J Neurosurg. 2014;120(6):1268-1277. [CrossRef]
- Hu Y jia, Xie Y bing, Zhang L feng, Ding C, Chen J. Comparison of clinical outcomes in patients who underwent Gamma Knife radiosurgery for parasellar meningiomas with or without prior surgery. BMC Neurol. 2020;20(1):153. [CrossRef]
- Williams BJ, Yen CP, Starke RM, et al. Gamma Knife surgery for parasellar meningiomas: long-term results including complications, predictive factors, and progression-free survival: Clinical article. J Neurosurg. 2011;114(6):1571-1577. [CrossRef]
- Peters DR, Asher A, Conti A, et al. Single fraction and hypofractionated radiosurgery for perioptic meningiomas—tumor control and visual outcomes: a systematic review and meta-analysis. Neurosurg Rev. 2023;46(1):287. [CrossRef]
- Hénaux PL, Bretonnier M, Le Reste PJ, Morandi X. Modern Management of Meningiomas Compressing the Optic Nerve: A Systematic Review. World Neurosurg. 2018;118:e677-e686. [CrossRef]
- Bailo M, Gagliardi F, Boari N, Castellano A, Spina A, Mortini P. The Role of Surgery in Meningiomas. Curr Treat Options Neurol. 2019;21(10):51. [CrossRef]
- Bunevicius A, Anand RK, Suleiman M, et al. Stereotactic Radiosurgery for Perioptic Meningiomas: An International, Multicenter Study. Neurosurgery. 2021;88(4):828-837. [CrossRef]
- Asuzu DT, Bunevicius A, Kormath Anand R, et al. Clinical and radiologic outcomes after stereotactic radiosurgery for meningiomas in direct contact with the optic apparatus: an international multicenter study. J Neurosurg. 2022;136(4):1070-1076. [CrossRef]
- Chen HY, Chuang CC, Chen HC, et al. Clinical outcomes of fractionated stereotactic radiosurgery in treating perioptic meningiomas and schwannomas: A single-institutional experience. J Clin Neurosci. 2020;81:409-415. [CrossRef]
- Wei Z, Taori S, Song S, Deng H, Niranjan A, Lunsford LD. Does Adjuvant Gamma Knife Stereotactic Radiosurgery Have a Role in Treating Optic Nerve Sheath Meningiomas? J Neuro-Ophthalmol Off J North Am Neuro-Ophthalmol Soc. Published online July 5, 2023. [CrossRef]
- Su CF, Liu DW, Lee CC, Chiu TL. Volume-staged gamma knife surgery for the treatment of large skull base meningioma surrounding the optical apparatus: A snowman-shape design. J Chin Med Assoc. 2017;80(11):697-704. [CrossRef]
- El-Shehaby AMN, Reda WA, Abdel Karim KM, Nabeel AM, Emad Eldin RM, Tawadros SR. Single-session stereotactic radiosurgery for large perioptic meningiomas. J Neurosurg. 2023;139(3):780-789. [CrossRef]
- Hinojosa J, Hernandez JO, Teh BS, Paulino AC, Butler EB. Intensity Modulated Radiotherapy for Optic Nerve Sheath Meningioma. In: Jeremic B, Pitz S, eds. Primary Optic Nerve Sheath Meningioma. Medical Radiology. Springer Berlin Heidelberg; 2008:95-103. [CrossRef]
- Uy NW, Woo SY, Teh BS, et al. Intensity-modulated radiation therapy (IMRT) for meningioma. Int J Radiat Oncol Biol Phys. 2002;53(5):1265-1270. [CrossRef]
- Barber SM, Teh BS, Baskin DS. Fractionated Stereotactic Radiotherapy for Pituitary Adenomas: Single-Center Experience in 75 Consecutive Patients. Neurosurgery. 2016;79(3):406-417. [CrossRef]
- Nicosia L, Di Pietro S, Catapano M, et al. Petroclival meningiomas: radiological features essential for surgeons. ecancermedicalscience. 2019;13. [CrossRef]
- Bunevicius A, Pikis S, Anand RK, et al. Stereotactic radiosurgery for clinoid meningiomas: a multi-institutional study. Acta Neurochir (Wien). 2021;163(10):2861-2869. [CrossRef]
- Demiral S, Dincoglan F, Sager O, et al. Hypofractionated stereotactic radiotherapy (HFSRT) for who grade I anterior clinoid meningiomas (ACM). Jpn J Radiol. 2016;34(11):730-737. [CrossRef]
- Akyoldaş G, Hergünsel ÖB, Yılmaz M, Şengöz M, Peker S. Gamma Knife Radiosurgery for Anterior Clinoid Process Meningiomas: A Series of 61 Consecutive Patients. World Neurosurg. 2020;133:e529-e534. [CrossRef]
- Daza-Ovalle A, Bin-Alamer O, Flickinger J, Niranjan A, Lunsford LD. Outcomes after gamma knife radiosurgery for intraventricular meningiomas. J Neurooncol. 2022;160(1):23-31. [CrossRef]
- Samanci Y, Oktug D, Yilmaz M, Sengoz M, Peker S. Efficacy of gamma knife radiosurgery in the treatment of intraventricular meningiomas. J Clin Neurosci. 2020;80:38-42. [CrossRef]
- Kim IY, Kondziolka D, Niranjan A, Flickinger JC, Lunsford LD. Gamma knife radiosurgery for intraventricular meningiomas. Acta Neurochir (Wien). 2009;151(5):447-452. [CrossRef]
- Nundkumar N, Guthikonda M, Mittal S. Peritumoral edema following Gamma Knife radiosurgery as the primary treatment for intraventricular meningiomas. J Clin Neurosci. 2013;20(4):616-618. [CrossRef]
- Mindermann T, Heckl S, Mack A. High incidence of transient perifocal edema following upfront radiosurgery for intraventricular meningiomas. Acta Neurochir (Wien). 2020;162(9):2177-2182. [CrossRef]
- Christ SM, Farhadi DS, Junzhao S, et al. Efficacy and Safety of Primary Stereotactic Radiosurgery in Patients with Intraventricular Meningiomas. Adv Radiat Oncol. 2023;8(1):101098. [CrossRef]
- Candy NG, Hinder D, Jukes AK, Wormald PJ, Psaltis AJ. Olfaction preservation in olfactory groove meningiomas: a systematic review. Neurosurg Rev. 2023;46(1):186. [CrossRef]
- Liu J, Rojas R, Lam FC, Mirza FA, Mahadevan A, Kasper EM. Indications, feasibility, safety, and efficacy of CyberKnife radiotherapy for the treatment of olfactory groove meningiomas: a single institutional retrospective series. Radiat Oncol. 2020;15(1):63. [CrossRef]
- Zaorsky N, Shi W, Gunn V, Werner-Wasik M, Farrell C, Andrews DW. Fractionated Stereotactic Radiation Therapy and Stereotactic Radiosurgery for the Treatment of Olfactory Groove Meningiomas: Observations of 13 Patients with or Without Prior Surgery. Int J Radiat Oncol Biol Phys. 2012;84(3):S277. [CrossRef]
- Granick MS, Martuza RL, Parker SW, Ojemann RG, Montgomery WW. Cerebellopontine angle meningiomas: clinical manifestations and diagnosis. Ann Otol Rhinol Laryngol. 1985;94(1 Pt 1):34-38. [CrossRef]
- Ali MS, Magill ST, McDermott MW. Petrous face meningiomas. In: Handbook of Clinical Neurology. Vol 170. Elsevier; 2020:157-165. [CrossRef]
- Jahanbakhshi A, Azar M, Kazemi F, Jalessi M, Chanideh I, Amini E. Gamma Knife stereotactic radiosurgery for cerebellopontine angle meningioma. Clin Neurol Neurosurg. 2019;187:105557. [CrossRef]
- El-Shehaby AMN, Reda WA, Abdel Karim KM, Nabeel AM, Emad Eldin RM, Tawadros SR. Hearing preservation after Gamma Knife radiosurgery for cerebellopontine angle meningiomas. J Neurosurg. 2018;129(Suppl1):38-46. [CrossRef]
- Ortiz García IM, Jorques Infante AM, Cordero Tous N, Almansa López J, Expósito Hernández J, Olivares Granados G. Cerebellopontine angle meningiomas: LINAC stereotactic radiosurgery treatment. Neurocir Engl Ed. 2023;34(6):283-291. [CrossRef]
- Park SH, Kano H, Niranjan A, Flickinger JC, Lunsford LD. Stereotactic radiosurgery for cerebellopontine angle meningiomas: Clinical article. J Neurosurg. 2014;120(3):708-715. [CrossRef]
- Kienzler JC, Fandino J. Adaptive Hybrid Surgery Experiences in Benign Skull Base Tumors. Brain Sci. 2022;12(10):1326. [CrossRef]
- Marchetti M, Sahgal A, De Salles AAF, et al. Stereotactic Radiosurgery for Intracranial Noncavernous Sinus Benign Meningioma: International Stereotactic Radiosurgery Society Systematic Review, Meta-Analysis and Practice Guideline. Neurosurgery. 2020;87(5):879-890. [CrossRef]
- Islim AI, Mohan M, Moon RDC, et al. Incidental intracranial meningiomas: a systematic review and meta-analysis of prognostic factors and outcomes. J Neurooncol. 2019;142(2):211-221. [CrossRef]
- Pikis S, Mantziaris G, Samanci Y, et al. Stereotactic Radiosurgery for Incidentally Discovered Cavernous Sinus Meningiomas: A Multi-institutional Study. World Neurosurg. 2022;158:e675-e680. [CrossRef]
- Neromyliotis E, Kalamatianos T, Paschalis A, et al. Machine Learning in Meningioma MRI: Past to Present. A Narrative Review. J Magn Reson Imaging. 2022;55(1):48-60. [CrossRef]
- Momin AA, Shao J, Soni P, et al. Outcomes of salvage radiation for recurrent world health organization grade II meningiomas: a retrospective cohort study. J Neurooncol. 2021;152(2):373-382. [CrossRef]
- Walcott BP, Nahed BV, Brastianos PK, Loeffler JS. Radiation Treatment for WHO Grade II and III Meningiomas. Front Oncol. 2013;3:227. [CrossRef]
- Stafford SL, Pollock BE, Leavitt JA, et al. A study on the radiation tolerance of the optic nerves and chiasm after stereotactic radiosurgery. Int J Radiat Oncol Biol Phys. 2003;55(5):1177-1181. [CrossRef]
- Alfredo C, Carolin S, Güliz A, et al. Normofractionated stereotactic radiotherapy versus CyberKnife-based hypofractionation in skull base meningioma: a German and Italian pooled cohort analysis. Radiat Oncol Lond Engl. 2019;14:201. [CrossRef]
- Fatima N, Meola A, Pollom EL, Soltys SG, Chang SD. Stereotactic radiosurgery versus stereotactic radiotherapy in the management of intracranial meningiomas: a systematic review and meta-analysis. Neurosurg Focus. 2019;46(6):E2. [CrossRef]
- Girvigian MR, Chen JCT, Rahimian J, Miller MJ, Tome M. COMPARISON OF EARLY COMPLICATIONS FOR PATIENTS WITH CONVEXITY AND PARASAGITTAL MENINGIOMAS TREATED WITH EITHER STEREOTACTIC RADIOSURGERY OR FRACTIONATED STEREOTACTIC RADIOTHERAPY. Neurosurgery. 2008;62(5):A19. [CrossRef]
- Leroy HA, Tuleasca C, Reyns N, Levivier M. Radiosurgery and fractionated radiotherapy for cavernous sinus meningioma: a systematic review and meta-analysis. Acta Neurochir (Wien). 2018;160(12):2367-2378. [CrossRef]
- Mansouri A, Guha D, Klironomos G, Larjani S, Zadeh G, Kondziolka D. Stereotactic Radiosurgery for Intracranial Meningiomas: Current Concepts and Future Perspectives. Neurosurgery. 2015;76(4):362-371. [CrossRef]
- Rogers L, Zhang P, Vogelbaum MA, et al. Intermediate-risk meningioma: Initial outcomes from NRG Oncology RTOG 0539. J Neurosurg. 2018;129(1):35-47. [CrossRef]
- Rogers CL, Won M, Vogelbaum MA, et al. High-risk Meningioma: Initial Outcomes from NRG Oncology/RTOG 0539. Int J Radiat Oncol Biol Phys. 2020;106(4):790-799. [CrossRef]
- Knisely JPS, Haghdel A, Chang SJ, et al. Progression-Free Survival in Patients with WHO-2 Meningioma Undergoing Active Surveillance Based on DOTATATE PET Evidence of Gross Total Resection: Prospective Observational Study. Int J Radiat Oncol. 2023;117(2):e118-e119. [CrossRef]
- Rutland JW, Dullea JT, Shrivastava RK. Future directions for immunotherapy in meningioma treatment. Oncotarget. 2021;12(22):2300-2301. [CrossRef]
- Chao S, Rogers L. External beam radiation therapy for meningioma. In: Handbook of Clinical Neurology. Vol 170. Elsevier; 2020:259-278. [CrossRef]
- Kowalchuk RO, Shepard MJ, Sheehan K, et al. Treatment of WHO Grade 2 Meningiomas with Stereotactic Radiosurgery: Identification of an Optimal Group for SRS Using RPA. Int J Radiat Oncol. 2021;110(3):804-814. [CrossRef]
- Louis DN, Perry A, Reifenberger G, et al. The 2016 World Health Organization Classification of Tumors of the Central Nervous System: a summary. Acta Neuropathol (Berl). 2016;131(6):803-820. [CrossRef]
- Bowden G, Faramand A, Mallella A, et al. Does the Timing of Radiosurgery after Grade 1 Meningioma Resection Affect Long-Term Outcomes? Stereotact Funct Neurosurg. 2021;99(6):506-511. [CrossRef]
- Karimi S, Mansouri S, Nassiri F, et al. Clinical significance of checkpoint regulator “Programmed death ligand-1 (PD-L1)” expression in meningioma: review of the current status. J Neurooncol. 2021;151(3):443-449. [CrossRef]
- Mair MJ, Berghoff AS, Brastianos PK, Preusser M. Emerging systemic treatment options in meningioma. J Neurooncol. 2023;161(2):245-258. [CrossRef]
| Table 1. | Symptomatic Lesional Effects |
|---|---|
| Parasagittal / Falcine | Anterior: Personality change, confusion, and altered consciousness [1], reduced attention span, short-term memory deficits, emotional instability, and apathy [31] Middle: Motor symptoms, (commonly spastic weakness of contralateral foot and leg), sensory symptoms, partial seizures [31] Posterior: Visual alterations or headache [31] |
| Confluence of Falx and Tentorium | Headache, disequilibrium, visual dysfunction, impaired cognition or behavioral change, and upgaze paresis [32] |
| Convexity | Seizures and sensory changes [12] |
| Parasellar | Visual impairment [33] (Additional symptoms widely variable depending on subregional location) |
| Suprasellar | Asymmetric visual impairment [18] |
| Petroclival | CN V deficits [19], CN VI palsy, vertigo, dizziness, balance and walking disturbances, and weakness of the extremities[18] |
| Clinoidal | Visual disturbances [34] |
| Perioptic | Visual loss |
| Cavernous Sinus | Oculomotor nerve palsy [18] |
| Intraventricular | Visual field deficits, ataxia, paresis, seizure, and hydrocephalus [35] |
| Foramen Magnum | Dizziness/ataxia, cranial nerve deficits, numbness, weakness, and hydrocephalus [25] |
| Olfactory Groove | Mental status disturbances and headaches, partial or complete anosmia [24] |
| Cerebellopontine Angle | Tinnitus, hearing loss, dizziness, trigeminal dysfunction, neurocognitive impairment [36] |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).




