Submitted:
19 October 2024
Posted:
21 October 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Surgical Procedure
2.3. Type of Excision and Cone Volume/Dimensions
2.4. Cytology
2.5. HR-HPV Determination
2.6. Colposcopy
2.7. Follow-up
2.8. Criteria for The Follow-Up Detection of CIN2+
2.9. Statistical Methods
3. Results
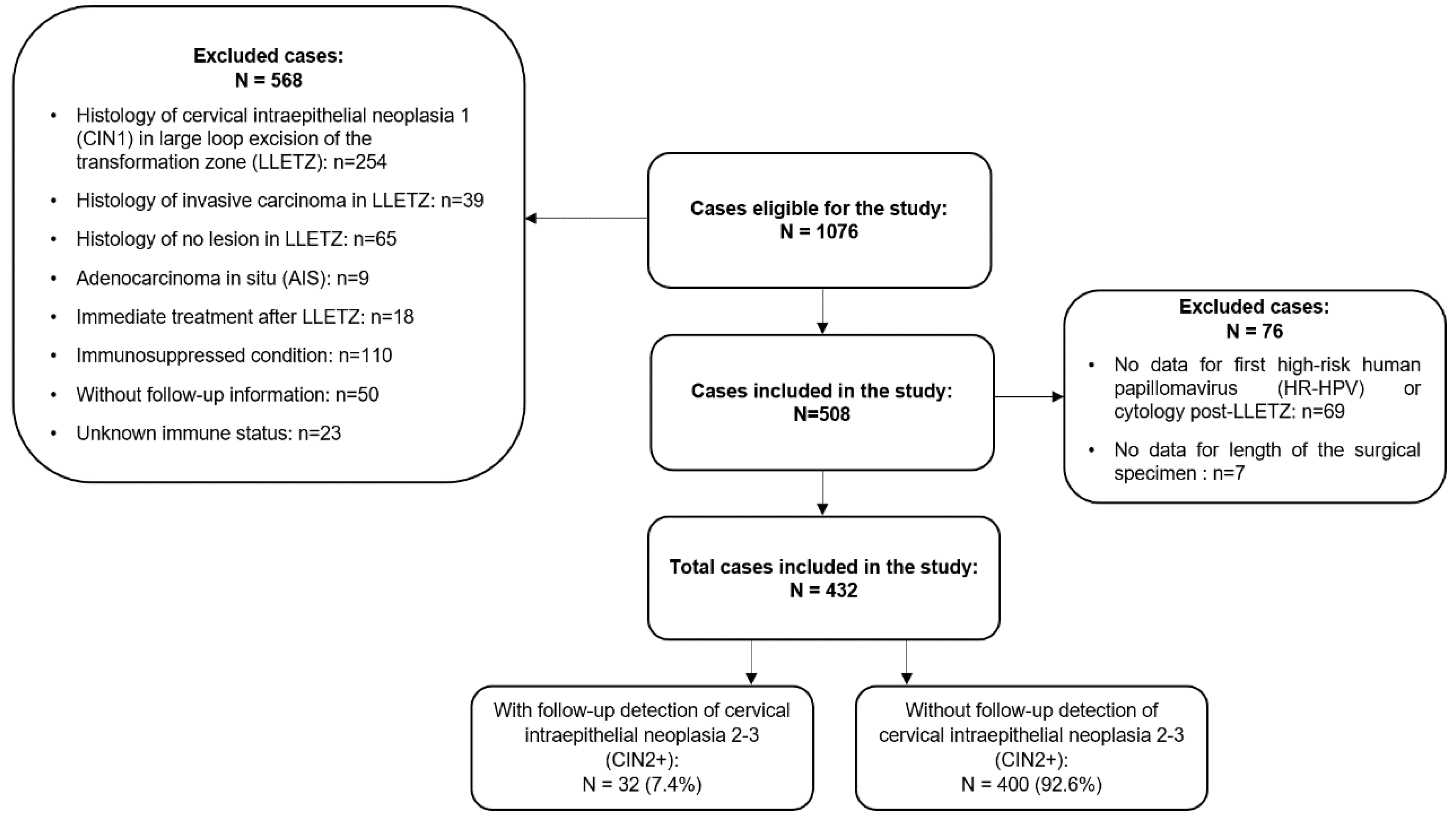
3.1. Study Population
3.2. Descriptive Characteristics Of The Study Cohort
3.3. Surgical margins, type of excision, and cone volume/dimensions
3.4. Predictors of a follow-up detection of CIN2+ by multivariate analysis
4. Discussion
4.1. Main Findings
4.2. Strengths and Limitations
4.3. Interpretation
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- CaCantor SB, Ph D, Atkinson EN, Ph D, Cardenas-turanzas M, et al. Natural History of Cervical Intraepithelial Neoplasia A Meta-analysis. Acta Cytol. 2005, 49, 405–415.
- McCredie MR, Sharples KJ, Paul C; et al. Natural history of cervical neoplasia and risk of invasive cancer in women with cervical intraepithelial neoplasia 3: a retrospective cohort study. Lancet Oncol. 2008, 9, 425–434. [Google Scholar] [CrossRef] [PubMed]
- D’Alessandro P, Arduino1 B, Borgo1 M, et al. Loop Electrosurgical Excision Procedure versus Cryotherapy in the Treatment of Cervical Intraepithelial Neoplasia: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Gynecol Minim Invasive Ther. 2018;7:145-151.
- Basu P, Taghavi K, Hu S, et al. Management of cervical premalignant lesions. Curr Probl Cancer. 2018;42:129–36.
- Bornstein J, Bentley J, Bösze P, et al. 2011 Colposcopic Terminology of the International Federation for Cervical Pathology and Colposcopy. Obstet Gynecol. 2012;120:166–72.
- NHS Cervical Screening Programme 2016. Available online: https://pathlabs.rlbuht.nhs.uk/colp_and_programme_mgment_2016.pdf (accessed on 5 June 2024).
- Arbyn M, Redman CWE, Verdoodt F, et al. Incomplete excision of cervical precancer as a predictor of treatment failure: a systematic review and meta-analysis. Lancet Oncol. 2017;18:1665–79.
- Kocken M, Helmerhorst TJM, Berkhof J, et al. Risk of recurrent high-grade cervical intraepithelial neoplasia after successful treatment: A long-term multi-cohort study. Lancet Oncol. 2011;12:441–50.
- Soutter WP, Sasieni P, Panoskaltsis T. Long-term risk of invasive cervical cancer after treatment of squamous cervical intraepithelial neoplasia. Int J Cancer. 2006;118:2048–55.
- Strander B, Andersson-Ellström A, Milsom I, et al. Long term risk of invasive cancer after treatment for cervical intraepithelial neoplasia grade 3: Population based cohort study. Br Med J. 2007;335:1077–80.
- Melnikow J, Mcgahan C, Sawaya GF, et al. Cervical Intraepithelial Neoplasia Outcomes After Treatment : Long-term Follow-up From the British Columbia Cohort Study. J Natl Cancer Inst. 2009;101:721–8.
- Fernández-Montolí ME, Tous S, Medina G, et al. Long-term predictors of residual or recurrent cervical intraepithelial neoplasia 2–3 after treatment with a large loop excision of the transformation zone: a retrospective study. BJOG An Int J Obstet Gynaecol. 2020;127:377–87.
- Papoutsis D, Rodolakis A, Mesogitis S, et al. Appropriate cone dimensions to achieve negative excision margins after large loop excision of transformation zone in the uterine cervix for cervical intraepithelial neoplasia. Gynecol Obstet Invest. 2013;75:163–8.
- Carcopino X, Mancini J, Prendiville W, et al. The Accuracy of Large Loop Excision of the Transformation Zone Specimen Dimensions in Determining Volume: A Multicentric Prospective Observational Study. J Low Genit Tract Dis. 2017;21:120–124.
- Phadnis S V, Atilade A, Young MPA, et al. The volume perspective : a comparison of two excisional treatments for cervical intraepithelial neoplasia ( laser versus LLETZ ). BJOG. 2010;117:615-9.
- Apgar BS, Zoschnick L, Wright TC. The 2001 Bethesda System Terminology. Am Fam Physician. 2003;68:1992–8.
- Schiffman MH, Kiviat NB, Burk RD, et al. Accuracy and Interlaboratory Reliability of Human Papillomavirus DNA Testing by Hybrid Capture. J Clin Microbiol. 1995;33:545–50.
- Martin IW, Steinmetz HB, Lefferts CL, et al. Evaluation of the Cobas 4800 HPV Test for Detecting High-Risk Human Papilloma-Virus in Cervical Cytology Specimens. Pathogens. 2012;1:30-6.
- Stasinou SM, Valasoulis G, Kyrgiou M, et al. Large Loop Excision of the Transformation Zone and Cervical Intraepithelial Neoplasia : A 22-Year Experience. Anticancer Res. 2012;32:4141–5.
- Foggiatto AI, De Carvalho NS, Fonseca FV, et al. Recurrence in Cervical High-Grade Squamous Intraepithelial Lesion: The Role of the Excised Endocervical Canal Length - Analysis of 2,427 Patients. J Low Genit Tract Dis. 2023;27:1–6.
- Cheung LC, Egemen D, Chen X, et al. 2019 ASCCP Risk-Based Management Consensus Guidelines: Methods for Risk Estimation, Recommended Management, and Validation. J Low Genit Tract Dis. 2020;24:90–101.
- Secondary Prevention of Cervical Cancer, 2022. Clinical Management of Abnormal Screening Results. Available online: https://www.aepcc.org/wp-content/uploads/2022/11/AEPCC-guidelines_Secondary-Prevention-2022.pdf (accessed on 21 March 2024).
- Papoutsis D, Rodolakis A, Antonakou A, et al. Cervical cone measurements and residual disease in LLETZ conisation for cervical intraepithelial neoplasia. In Vivo. 2011;25:691-5.
- Mirandez CC, Yoneda JY, Gertrudes LN, et al. The value of the endocervical margin status in LEEP: analysis of 610 cases. Arch Gynecol Obstet. 2022;306:851–6.
- Kawano K, Tsuda N, Nishio S; et al. Identification of appropriate cone length to avoid positive cone margin in high grade cervical intraepithelial neoplasia. J Gynecol Oncol. 2016, 27, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Kyrgiou M, Athanasiou A, Paraskevaidi M, et al. Adverse obstetric outcomes after local treatment for cervical preinvasive and early invasive disease according to cone depth: Systematic review and meta-analysis. BMJ. 2016;354:i3633.
- Baldauf JJ, Dreyfus M, Ritter J, et al. Risk of cervical stenosis after large loop excision or laser conization. J Obstet Gynecol. 1996; 88:933-8.
- Sparić R, Papoutsis D, Kadija S, et al. Psychosexual outcomes in women of reproductive age at more than two-years from excisional cervical treatment–a cross-sectional study. J Psychosom Obstet Gynecol. 2019;40:128–37.
- Serati M, Salvatore S, Cattoni E, et al. The impact of the loop electrosurgical excisional procedure for cervical intraepithelial lesions on female sexual function. J Sex Med. 2010;7:2267-2272.
- Desai KT, de Sanjosé S, Schiffman M. Treatment of Cervical Precancers is the Major Remaining Challenge in Cervical Screening Research. Cancer Prev Res. 2023;16:649–52.
- Reich O, Regauer S, Lara Gutierrez A; et al. Copy number profiling implicates thin high-grade squamous intraepithelial lesions as a true precursor of cervical human papillomavirus-induced squamous cell cancer. Lab Investig 2024, 104, 102108. [Google Scholar] [CrossRef] [PubMed]
- Kitson SJ, Greig E, Michael E; et al. European Journal of Obstetrics & Gynecology and Reproductive Biology Predictive value of volume of cervical tissue removed during LLETZ on subsequent preterm delivery : a cohort study. Eur J Obstet Gynecol Reprod Biol. 2014, 180, 51–55. [Google Scholar] [PubMed]
| Patient characteristics | Total n (%)* |
No CIN2+ detected (%)** | Follow-up detection of CIN2+ (%)** | P-value*** |
|---|---|---|---|---|
| Follow-up time (months) | 0.000**** | |||
| Median (IQR) | 70.9 (17.9-141) | 87.7 (23-143.5) | 11.5 (3.8-27.9) | |
| Age (years) | 0.100**** | |||
| Median (min-max) | 36.1 (18.3-77) | 36 (18.3-77) | 39 (24-62) | |
| Age at the time of LLETZ (years) | 0.022 | |||
| < 35 years old | 181 (41.9) | 174 (96.1) | 7 (3.9) | |
| ≥ 35 years old | 251 (58.1) | 226 (90.1) | 25 (9.9) | |
| Smoking habit | 0.788 | |||
| No | 195 (45.1) | 181 (92.8) | 14 (7.2) | |
| Yes | 209 (48.4) | 194 (92.8) | 15 (7.2) | |
| Unknown | 28 (6.5) | 25 (89.3) | 3 (10.7) | |
| Parity | 0.063 | |||
| Nulliparous | 118 (27.3) | 111 (94.1) | 7 (5.9) | |
| < 4 full-term births | 264 (61.1) | 246 (93.2) | 18 (6.8) | |
| ≥ 4 full-term births | 15 (3.5) | 11 (73.3) | 4 (26.7) | |
| Unknown | 35 (8.1) | 32 (91.4) | 3 (8.6) | |
| Contraceptive method | 0.824 | |||
| None | 77 (17.8) | 70 (90.9) | 7 (9.1) | |
| Hormonal | 113 (26.2) | 103 (91.2) | 10 (8.8) | |
| IUD | 47 (10.9) | 44 (93.6) | 3 (6.4) | |
| Condoms | 130 (30.1) | 123 (94.6) | 7 (5.4) | |
| Others | 19 (4.4) | 17 (89.5) | 2 (10.5) | |
| Unknown | 46 (106) | 43 (93.5) | 3 (6.5) | |
| HPV vaccine prior to or after LLETZ | 0.988 | |||
| No | 326 (75.5) | 302 (92.6) | 24 (7.4) | |
| Yes | 91 (21.1) | 84 (92.3) | 7 (7.7) | |
| Missing | 15 (3.5) | 14 (93.3) | 1 (6.7) | |
| HR-HPV result (HC2 and Cobas 4800) | ||||
| First HR-HPV post-LLETZ | 0.000 | |||
| Negative | 332 (76.9) | 320 (96.4) | 12 (3.6) | |
| Positive | 100 (23.1) | 80 (80.0) | 20 (20.0) | |
| First RLU HR-HPV post-LLETZ | 0.000**** | |||
| Median (IQR) | 0.2 (0.14-0.70) | 0.2 (0.14-0.5) | 2.25 (0.295-120.15) | |
| First RLU HR-HPV post-LLETZ category | 0.000 | |||
| Negative | 301 (69.7) | 289 (72.3) | 12 (37.5) | |
| 1-100 pg/ml | 60 (13.9) | 53 (88.3) | 7 (11.7) | |
| > 100 pg/ml | 27 (6.3) | 18 (66.7) | 9 (33.3) | |
| Unknown | 44 (10.2) | 40 (90.9) | 4 (9.1) | |
| Total | 432 (100.0) | 400 (92.6) | 32 (7.4) | |
| Surgical specimen characteristics | Total n (%)* |
No follow-up detection of CIN2+ (%)** | Follow-up detection of CIN2+ (%)** | P-value |
|---|---|---|---|---|
| Margin status | 0.001*** | |||
| Clear | 232 (53.7) | 224 (96.6) | 8 (3.4) | |
| Ecto+/endo- | 68 (15.7) | 65 (95.6) | 3 (4.4) | |
| Ecto-/endo+ | 70 (16.2) | 58 (82.9) | 12 (17.1) | |
| Ecto+/endo+ | 11 (2.5) | 9 (81.8) | 2 (18.2) | |
| Endo+/deep+ | 2 (0.45) | 2 (100.0) | 0 (0.00) | |
| All | 4 (0.9) | 4 (100.0) | 0 (0.00) | |
| Deep | 2 (0.45) | 2 (100.0) | 0 (0.00) | |
| Uncertain | 43 (10.0) | 36 (83.7) | 7 (16.3) | |
| Margin status category | 0.002*** | |||
| Clear | 232 (53.7) | 224 (96.6) | 8 (3.4) | |
| Involved | 157 (36.3) | 140 (89.2) | 17 (10.8) | |
| Uncertain | 43 (10.0) | 36 (83.7) | 7 (16.3) | |
| Type of excision | 0.678**** | |||
| Type 11 | 141 (32.6) | 129 (91.5) | 12 (8.5) | |
| Type 2 2 | 199 (46.1) | 184 (92.5) | 15 (7.5) | |
| Type 3 3 | 92 (21.3) | 87 (94.6) | 5 (5.4) | |
| Length (mm)4 | 0.356***** | |||
| Median (IQR) | 10.0 (7.0-10.5) | 10.0 (7.0-16.0) | 9.5 (7.0-13.0) | |
| Thickness (mm)5 | 0.172***** | |||
| Median (IQR) | 10.5 (9.5-12.5) | 11.0 (9.0-13.0) | 10.0 (9.0-13.0) | |
| Circumference (mm)6 | 0.461***** | |||
| Median (IQR) | 103.0 (90.6-120.0) | 101.0 (89.0-120.0) | 99.0 (85.5-119.0) | |
| Volume Carcopino (cm³)7 | 0.660***** | |||
| Median (IQR) | 3.94 (2.27-6.18) | 3.93 (2.27-6.17) | 3.66 (1.60-7.24) | |
| Volume Phadnis (cm³)8 | 0.329***** | |||
| Median (IQR) | 2.18 (1.31-3.50) | 2.26 (1.31-3.54) | 1.96 (1.19-2.93) | |
| Number of quadrants involved | 0.158*** | |||
| 1-2 | 203 (47.0) | 190 (93.6) | 13 (6.4) | |
| 3-4 | 158 (36.6) | 142 (89.9) | 16 (10.1) | |
| Not evaluable | 18 (4.2) | 16 (88.9) | 2 (11.1) | |
| Unknown | 53 (12.3) | 52 (98.1) | 1 (1.9) | |
| Total | 432 (100.0) | 400 (92.6) | 32 (7.4) | |
| Variables | n = 432 | Clear margins | Involved margins | Uncertain margins | P-value |
|---|---|---|---|---|---|
| Age (years) | < 0.001*** | ||||
| Median (min-max) | 35 (18-66) | 36 (20-77) | 42 (22-69) | ||
| Age (years) | < 0.001** | ||||
| < 35 years old, n (%)* | 181 | 112 (61.9) | 62 (34.3) | 7 (3.9) | |
| ≥ 35 years old, n (%)* | 251 | 120 (47.8) | 95 (37.8) | 36 (14.3) | |
| Type of excision | 0.035 | ||||
| Type 1, n (%)*1 | 141 | 65 (46.1) | 56 (39.7) | 20 (14.2) | |
| Type 2, n (%)*2 | 199 | 107 (53.8) | 76 (38.2) | 16 (8.0) | |
| Type 3, n (%)*3 | 92 | 60 (65.2) | 25 (27.2) | 7 (7.6) | |
| Length (mm)4 | 0.010*** | ||||
| Median (IQR) | 307 | 12.0 (8.0-16.0) | 10.0 (7.0-13.7) | 8.0 (5.0-13.0) | |
| Thickness (mm)5 | 0.742*** | ||||
| Median (IQR) | 432 | 10.5 (9.0-12.5) | 10.5 (9.5-12.5) | 11.0 (10.0-12.5) | |
| Circumference (mm)6 | 0.760*** | ||||
| Median (IQR) | 363 | 105 (88.9-120) | 100 (90.2-120) | 100 (94.1-120) | |
| Volume Carcopino (cm³)7 | 0.524*** | ||||
| Median (IQR) | 305 | 3.97 (2.42-6.13) | 3.85 (1.95-6.41) | 3.69 (1.53-7.09) | |
| Volume Phadnis (cm³)8 | 0.347*** | ||||
| Median (IQR) | 302 | 2.35 (1.42-3.49) | 2.09 (1.18-3.38) | 2.15 (0.92-3.68) | |
| Total | 432 | 232 | 157 | 43 | |
| Variables | HR (95% CI) | P-value* |
|---|---|---|
| HR-HPV test post-LLETZ (negative vs positive) | 7.36 (3.55-15.26) | < 0.001 |
| Involved vs clear margins | 3.94 (1.68-9.25) | 0.002 |
| Uncertain vs clear margins | 4.42 (1.55-12.55) | 0.005 |
| Age ≥ 35 years old vs < 35 years old | 2.92 (1.19-7.13) | 0.019 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




