Submitted:
12 August 2024
Posted:
14 August 2024
Read the latest preprint version here
Abstract
Keywords:
Introduction
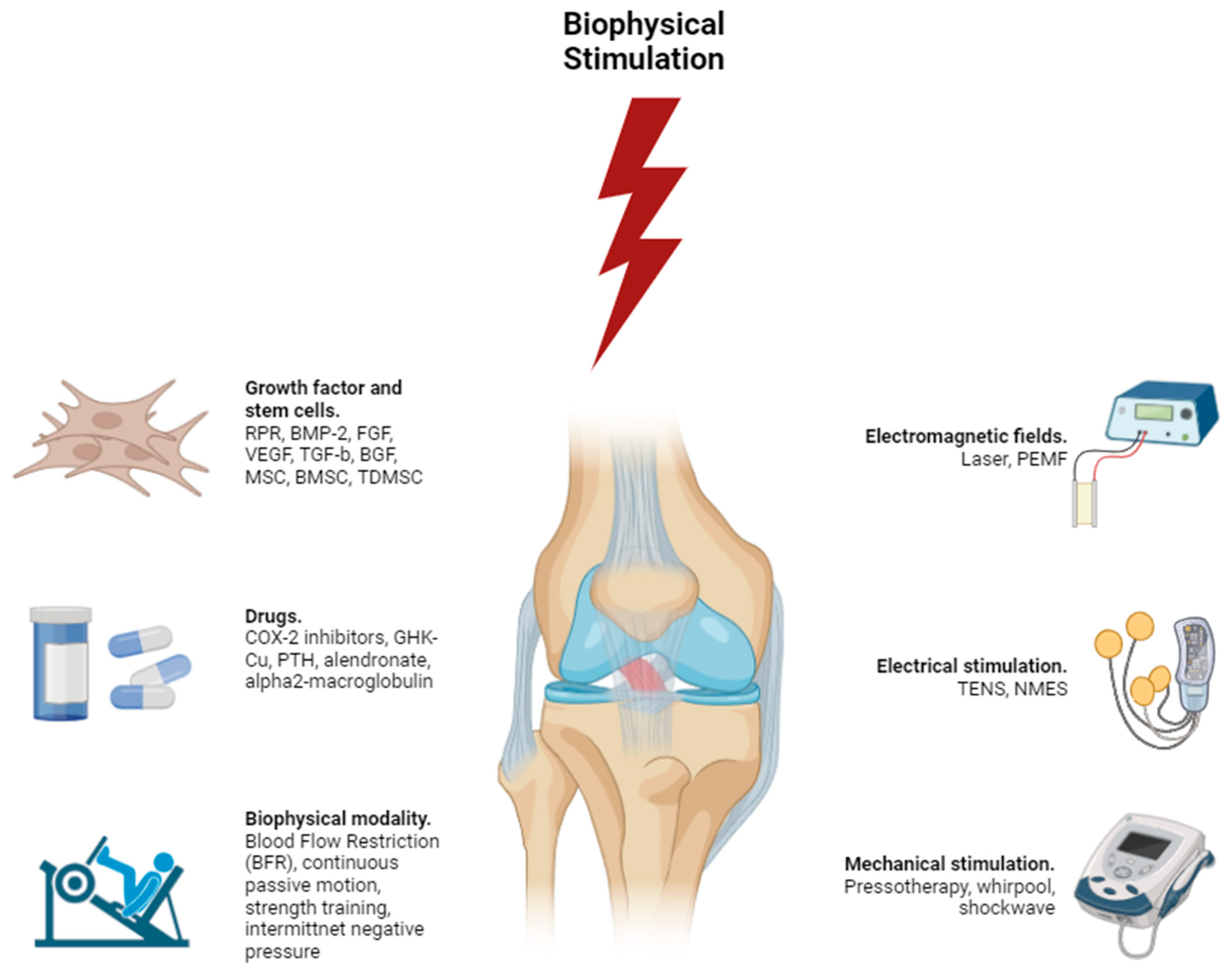
Biophysical Stimulation for ACL Injury Treatement
Biomechanical Factors
1. Kinematic and Kinetic Analysis
2. Impact of External Loads
3. Muscle Activation Patterns
Anatomical Factors
1. Femoral Notch Width
2. Tibial Slope
3. ACL Geometry
Physiological Factors
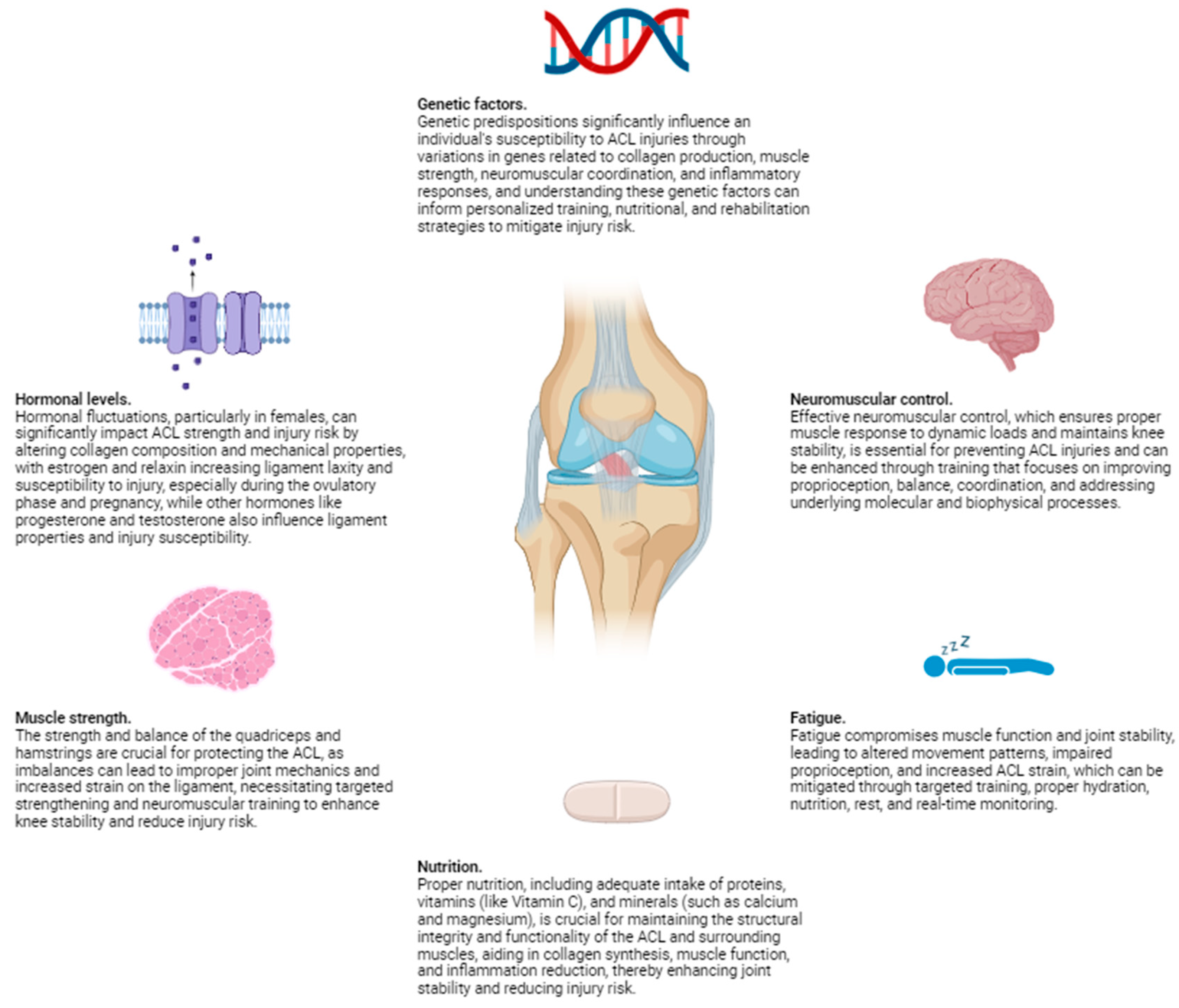
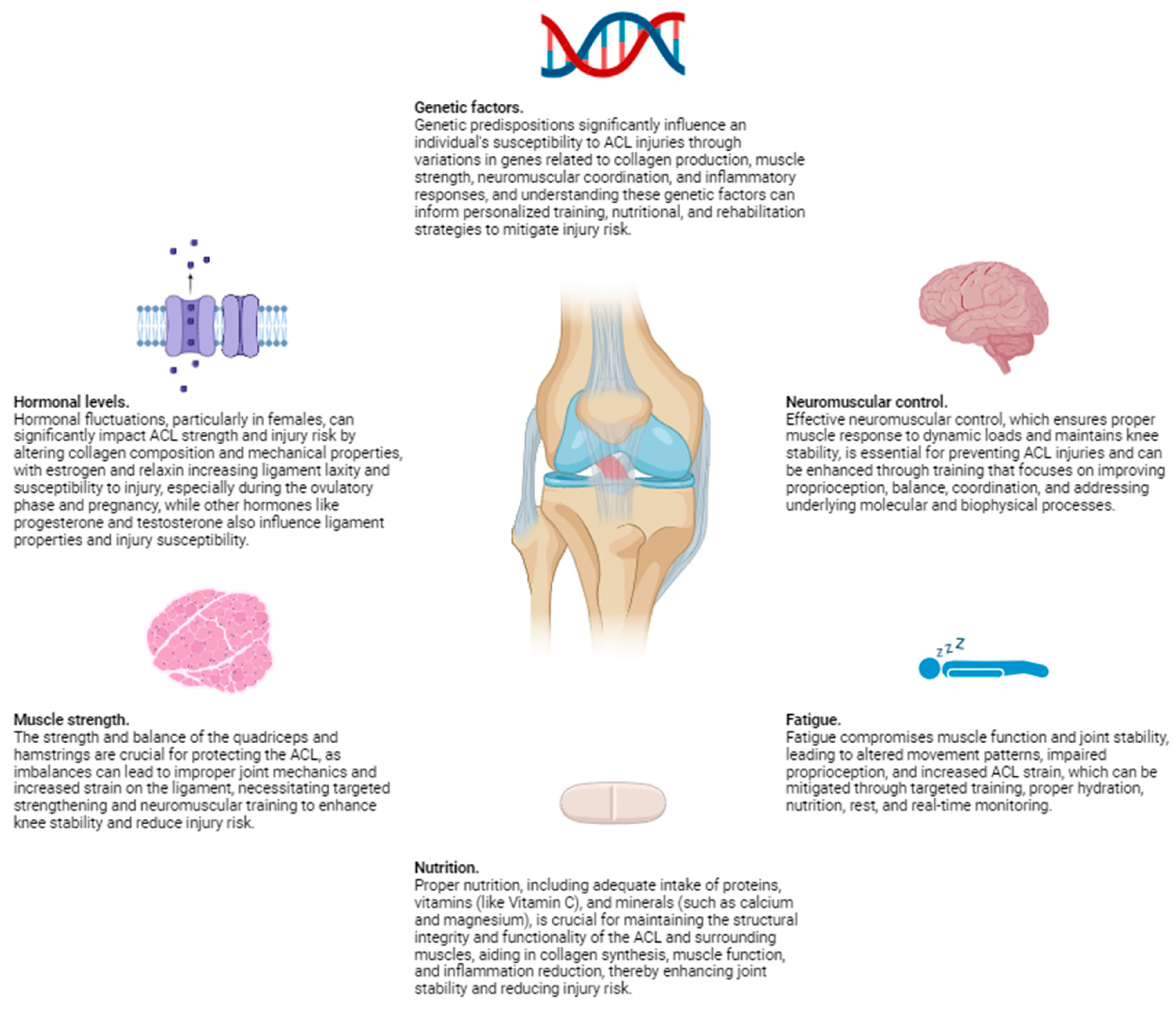
1. Hormonal Levels
2. Muscle Strength
3. Neuromuscular Control
4. Fatigue
Molecular Biophysics and Physiological Factors
1. Genetic Factors
2. Recovery and Rehabilitation
3. Nutritional Influences
Discussion
Integrated Approaches
1. Injury Prevention Programs
2. Screening and Risk Assessment
3. Rehabilitation Strategies
Conclusions
References
- Griffin, L. Y., Albohm, M. J., Arendt, E. A., Bahr, R., Beynnon, B. D., DeMaio, M.,... & Yu, B. (2006). Understanding and preventing noncontact anterior cruciate ligament injuries: a review of the Hunt Valley II meeting, January 2005. The American journal of sports medicine, 34(9), 1512-1532.
- Hewett, T. E., Myer, G. D., & Ford, K. R. (2006). Anterior cruciate ligament injuries in female athletes: Part 1, mechanisms and risk factors. The American journal of sports medicine, 34(2), 299-311.
- Quatman, C. E., & Hewett, T. E. (2009). The anterior cruciate ligament injury controversy: is “valgus collapse” a sex-specific mechanism? British journal of sports medicine, 43(5), 328-335.
- Sutton, K. M., & Bullock, J. M. (2013). Anterior cruciate ligament rupture: differences between males and females. Journal of the American Academy of Orthopaedic Surgeons, 21(1), 41-50.
- Yu, B., & Garrett, W. E. (2007). Mechanisms of non-contact ACL injuries. British journal of sports medicine, 41(Suppl 1), i47-i51.
- Boden, B. P., Griffin, L. Y., & Garrett, W. E. (2000). Etiology and prevention of noncontact ACL injury. The Physician and sportsmedicine, 28(4), 53-60.
- Renstrom, P., Ljungqvist, A., Arendt, E., Beynnon, B., Fukubayashi, T., Garrett, W.,... & Wojtys, E. (2008). Non-contact ACL injuries in female athletes: an International Olympic Committee current concepts statement. British journal of sports medicine, 42(6), 394-412.
- Boden, B. P., Griffin, L. Y., & Garrett, W. E. (2000). Etiology and prevention of noncontact ACL injury. Physician and Sportsmedicine, 28(4), 53-60.
- Hewett, T. E., Myer, G. D., & Ford, K. R. (2006). Anterior cruciate ligament injuries in female athletes: Part 1, mechanisms and risk factors. American Journal of Sports Medicine, 34(2), 299-311.
- Markolf, K. L., Burchfield, D. M., Shapiro, M. S., Shepard, M. F., Finerman, G. A., & Slauterbeck, J. L. (1995). Combined knee loading states that generate high anterior cruciate ligament forces. Journal of Orthopaedic Research, 13(6), 930-935.
- Myer, G. D., Ford, K. R., Palumbo, J. P., & Hewett, T. E. (2005). Neuromuscular training improves performance and lower-extremity biomechanics in female athletes. Journal of Strength and Conditioning Research, 19(1), 51-60.
- Renstrom, P., Ljungqvist, A., Arendt, E., Beynnon, B., Fukubayashi, T., Garrett, W.,... & Yu, B. (2008). Non-contact ACL injuries in female athletes: An International Olympic Committee current concepts statement. British Journal of Sports Medicine, 42(6), 394-412.
- Shultz, S. J., Schmitz, R. J., Benjaminse, A., Collins, M., Ford, K. R., Kulas, A. S.,... & Powers, C. M. (2012). ACL Research Retreat VII: An update on anterior cruciate ligament injury risk factor identification, screening, and prevention. Journal of Athletic Training, 47(5), 591-603.
- Yu, B., & Garrett, W. E. (2007). Mechanisms of non-contact ACL injuries. British Journal of Sports Medicine, 41(Suppl 1), i47-i51.
- Boden, B. P., Sheehan, F. T., Torg, J. S., & Hewett, T. E. (2010). Non-contact anterior cruciate ligament injuries: Mechanisms and risk factors. Journal of the American Academy of Orthopaedic Surgeons, 18(9), 520-527.
- Griffin, L. Y., Albohm, M. J., Arendt, E. A., Bahr, R., Beynnon, B. D., Demaio, M.,... & Yu, B. (2006). Understanding and preventing noncontact anterior cruciate ligament injuries: A review of the Hunt Valley II meeting, January 2005. American Journal of Sports Medicine, 34(9), 1512-1532.
- Mandelbaum, B. R., Silvers, H. J., Watanabe, D. S., Knarr, J. F., Thomas, S. D., Griffin, L. Y.,... & Garrett, W. (2005). Effectiveness of a neuromuscular and proprioceptive training program in preventing anterior cruciate ligament injuries in female athletes: 2-year follow-up. American Journal of Sports Medicine, 33(7), 1003-1010.
- Olsen, O. E., Myklebust, G., Engebretsen, L., & Bahr, R. (2004). Injury mechanisms for anterior cruciate ligament injuries in team handball: A systematic video analysis. American Journal of Sports Medicine, 32(4), 1002-1012.
- Paterno, M. V., Myer, G. D., Ford, K. R., & Hewett, T. E. (2004). Neuromuscular training improves single-limb stability in young female athletes. Journal of Orthopaedic & Sports Physical Therapy, 34(6), 305-316.
- Taylor, J. B., Waxman, J. P., Richter, S. J., & Shultz, S. J. (2015). Evaluation of the effectiveness of anterior cruciate ligament injury prevention programme training components: A systematic review and meta-analysis. British Journal of Sports Medicine, 49(2), 79-87.
- Dempsey, A. R., Lloyd, D. G., Elliott, B. C., Steele, J. R., & Munro, B. J. (2007). Changing sidestep cutting technique reduces knee valgus loading. American Journal of Sports Medicine, 35(11), 1891-1900.
- Benjaminse, A., Gokeler, A., Fleisig, G. S., Sell, T. C., & Otten, B. (2011). What is the true evidence for gender-related differences during plant and cut maneuvers? A systematic review. Knee Surgery, Sports Traumatology, Arthroscopy, 19(1), 42-54.
- Ford, K. R., Myer, G. D., Smith, R. L., Byrnes, R. N., Dopirak, S. E., & Hewett, T. E. (2005). Use of an overhead goal alters vertical jump performance and biomechanics. Journal of Strength and Conditioning Research, 19(2), 394-399.
- Krosshaug, T., Nakamae, A., Boden, B. P., Engebretsen, L., Smith, G., Slauterbeck, J. R.,... & Bahr, R. (2007). Mechanisms of anterior cruciate ligament injury in basketball: Video analysis of 39 cases. American Journal of Sports Medicine, 35(3), 359-367.
- Pappas, E., & Carpes, F. P. (2012). Lower extremity biomechanics: Prevention and management of injuries. Human Kinetics.
- Powers, C. M. (2010). The influence of abnormal hip mechanics on knee injury: A biomechanical perspective. Journal of Orthopaedic & Sports Physical Therapy, 40(2), 42-51.
- Quatman, C. E., & Hewett, T. E. (2009). The anterior cruciate ligament injury controversy: Is “valgus collapse” a sex-specific mechanism? British Journal of Sports Medicine, 43(5), 328-335.
- Shimokochi, Y., & Shultz, S. J. (2008). Mechanisms of noncontact anterior cruciate ligament injury. Journal of Athletic Training, 43(4), 396-408.
- Silvers, H. J., & Mandelbaum, B. R. (2007). Prevention of anterior cruciate ligament injury in the female athlete. British Journal of Sports Medicine, 41(Suppl 1), i52-i59.
- Waldén, M., Hägglund, M., & Ekstrand, J. (2011). High risk of new knee injury in elite footballers with previous anterior cruciate ligament injury. British Journal of Sports Medicine, 40(2), 158-162.
- Zazulak, B. T., Paterno, M., Myer, G. D., Romani, W. A., & Hewett, T. E. (2006). The effects of the menstrual cycle on anterior knee laxity: A systematic review. Sports Medicine, 36(10), 847-862.
| Factor | Description | Impact on ACL | Prevention and Intervention Strategies |
|---|---|---|---|
| Biomechanical Forces | Axial Loading, Anterior Tibial Translation, Rotational Forces | Causes ACL strain or rupture during activities like landing, cutting, pivoting, and sudden stops | Improve muscle strength and neuromuscular control, use proper footwear, consider playing surface conditions |
| Kinematic Analysis | Motion of knee joint, analyzing angles and velocities without considering forces | Identifies movement patterns that increase ACL injury risk, such as excessive knee valgus and improper landing mechanics | Focus on movement techniques, proper landing mechanics, and reducing knee valgus through training programs |
| Kinetic Analysis | Examines forces and torques acting on the knee | Provides insights into how different movements generate stress on the ACL, particularly during high-impact activities | Use strength and conditioning programs to enhance muscle balance and control, implement proper technique training |
| Muscle Strength and Coordination | Role of quadriceps and hamstrings in stabilizing the knee joint | Imbalances or improper timing of these muscles increase ACL strain, especially during high-impact activities | Strengthen quadriceps and hamstrings, balance training, neuromuscular control exercises |
| External Factors | Footwear, playing surface, and environmental conditions | Artificial turf and improper footwear can increase ACL injury risk due to greater traction and altered movement mechanics | Use appropriate footwear, choose safer playing surfaces, and adapt to environmental conditions |
| Molecular Biophysics of ACL | Collagen fibers, proteoglycans, molecular signaling pathways | Structural integrity and response to mechanical stress depend on collagen organization and biochemical interactions | Develop molecular therapies to enhance tissue repair, use novel biomaterials for ligament reconstruction |
| Kinematic and Kinetic Analyses | High-speed video analysis, motion capture studies, biomechanical modeling, and simulations | Identifies critical risk factors for ACL injuries, such as anterior tibial translation and internal tibial rotation | Implement targeted training programs to improve movement patterns and reduce risky maneuvers |
| Impact of External Loads | Valgus stress and axial loading | Increases ACL loading during dynamic activities like cutting maneuvers and sidestepping | Enhance knee stability through strength and conditioning, use braces or supports if necessary |
| Finite Element Modeling | Simulates interactions between bones, ligaments, and muscles under various loading conditions | Visualizes stress distribution across the ACL, highlighting critical points of failure | Inform design of training programs and interventions, develop more effective bracing techniques |
| Cadaveric Studies | Empirical data on ACL response to external loads | Validates computational models and identifies thresholds for ACL failure | Combine with modeling data to create comprehensive prevention strategies |
| Muscle Activation Patterns | Role of quadriceps, hamstrings, gastrocnemius, and gluteal muscles | Imbalanced or delayed activation increases ACL strain during dynamic movements | EMG studies to analyze activation patterns, neuromuscular training to optimize muscle function |
| Neuromuscular Control | Coordination of muscle activation patterns in response to sensory input | Proper activation and timing of muscles are crucial for stabilizing the knee and reducing ACL load | Plyometrics, agility drills, balance training to enhance neuromuscular control |
| Advanced EMG Techniques | Surface and intramuscular EMG | Provides detailed insights into muscle activation patterns | Integrate with motion capture technology and biomechanical modeling for comprehensive analysis |
| Molecular Mechanisms of Muscle Function | Actin and myosin interaction, role of calcium ions, mechanotransduction pathways, satellite cells in muscle repair and growth | Muscle fiber contraction, efficiency, and force generation impact knee stability | Research molecular cues for muscle adaptation, develop interventions to enhance muscle function and repair |
| Advanced Imaging Techniques | MRI, ultrasound elastography | Provides detailed views of ACL's internal structure and mechanical properties | Use imaging for early detection of stress and damage, monitor ligament condition |
| Computational Fluid Dynamics (CFD) | Fluid environment within the knee joint | Synovial fluid dynamics influence lubrication and nutrition of the ACL | Develop strategies to maintain optimal fluid dynamics for ligament health |
| Molecular Signaling Pathways | Mechanotransduction, interaction of proteins like integrins and focal adhesion kinase | Regulates cellular response to mechanical stress, affecting ACL integrity and healing | Target these pathways to promote healing and prevent injury at the molecular level |
| Role of ECM Proteins | Elastin and proteoglycans | Contribute to ligament's elasticity and resilience | Research interactions and responses to mechanical stress to develop better repair and reconstruction strategies |
| Factor | Description | Impact on ACL | Prevention and Intervention Strategies |
|---|---|---|---|
| Intercondylar Notch Width | Narrower notch width restricts ACL space, increasing likelihood of impingement during dynamic movements | Higher risk of ACL tears due to increased mechanical constraints | Advanced imaging (MRI), strength and conditioning programs, biomechanical training, notchplasty for recurrent injuries |
| Tibial Slope | Steeper posterior tibial slope increases anterior tibial translation during weight-bearing activities | Increased ACL strain and higher incidence of ACL injuries, especially during sudden deceleration | Biomechanical training, strength and conditioning, tibial slope modification surgery |
| Lower Limb Alignment (Q-Angle) | Larger Q-angle increases lateral forces on the knee, leading to greater valgus stress and internal tibial rotation | Creates biomechanical environment more susceptible to ACL strain during dynamic activities | Focus on reducing knee valgus through training programs, proper movement techniques, targeted strength exercises |
| ACL Size and Shape | Variations in cross-sectional area, length, curvature, and orientation affect mechanical properties | Smaller or thinner ACL less capable of handling high loads, irregular shapes may lead to uneven stress | Strengthen surrounding muscles, personalized training programs based on anatomical assessments |
| Gender Differences | Females typically have wider pelvis, greater Q-angle, more ligamentous laxity, and hormonal variations affecting ligament strength | Altered biomechanics, increased valgus alignment, higher incidence of ACL injuries | Gender-specific prevention programs, hormonal influence considerations, targeted neuromuscular training |
| Advanced Imaging Techniques | MRI and CT scans provide detailed views of knee anatomy and ACL structures | Identifies anatomical variations that predispose to ACL injuries | Use for risk assessment, personalized prevention strategies, and planning surgical interventions |
| Molecular Composition | ECM of ACL includes collagen, proteoglycans, elastin, and other molecules affecting mechanical properties | Variations affect tensile strength, elasticity, and ability to withstand loads | Research on collagen cross-linking, proteoglycan interactions, and development of biomaterials for ligament reconstruction |
| Genetic Factors | Genetic variations influence development and maintenance of knee structures | Affects expression of proteins involved in collagen synthesis, ECM organization, and bone morphology | Identify individuals at higher risk through genetic screening, personalized prevention strategies |
| Mechanotransduction Pathways | Cellular response to mechanical stress involves integrins, MAPK/ERK pathway, and other signaling molecules | Regulates ECM synthesis and degradation, affects ligament resilience and repair | Target these pathways for therapeutic interventions to enhance ACL resilience and repair |
| Oxidative Stress | Mechanical stress generates reactive oxygen species (ROS), causing oxidative damage to cellular components | Impairs fibroblast function and promotes ECM degradation | Antioxidant therapies to reduce oxidative stress and protect the ACL |
| Epigenetic Modifications | DNA methylation, histone modification, and non-coding RNA expression regulate gene expression in response to mechanical stress | Influences cellular adaptations and ligament health | Research on epigenetic mechanisms to develop strategies for promoting adaptive responses and preventing injury |
| Tissue Engineering | 3D bioprinting and scaffold-based approaches to create ligament constructs that mimic native ACL geometry and properties | Potentially improves outcomes for ACL reconstruction and repair | Design scaffolds and bioprinted tissues that promote proper cell alignment and mechanical strength |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




