Submitted:
02 August 2024
Posted:
06 August 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Statistical Analysis
2.2. Statistical Significance Is Expressed as a p<0.05 Index
3. Results
4. Discussion
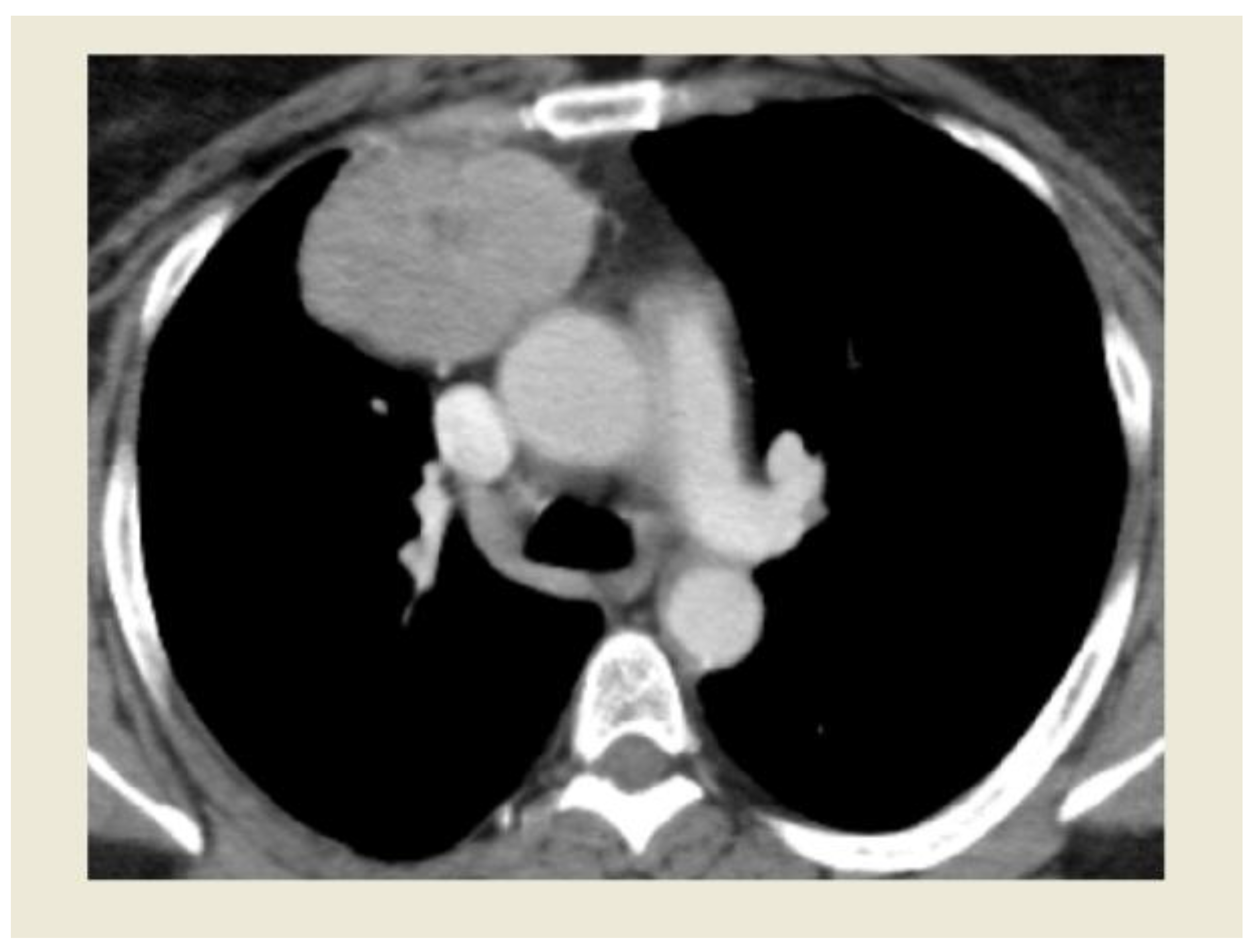
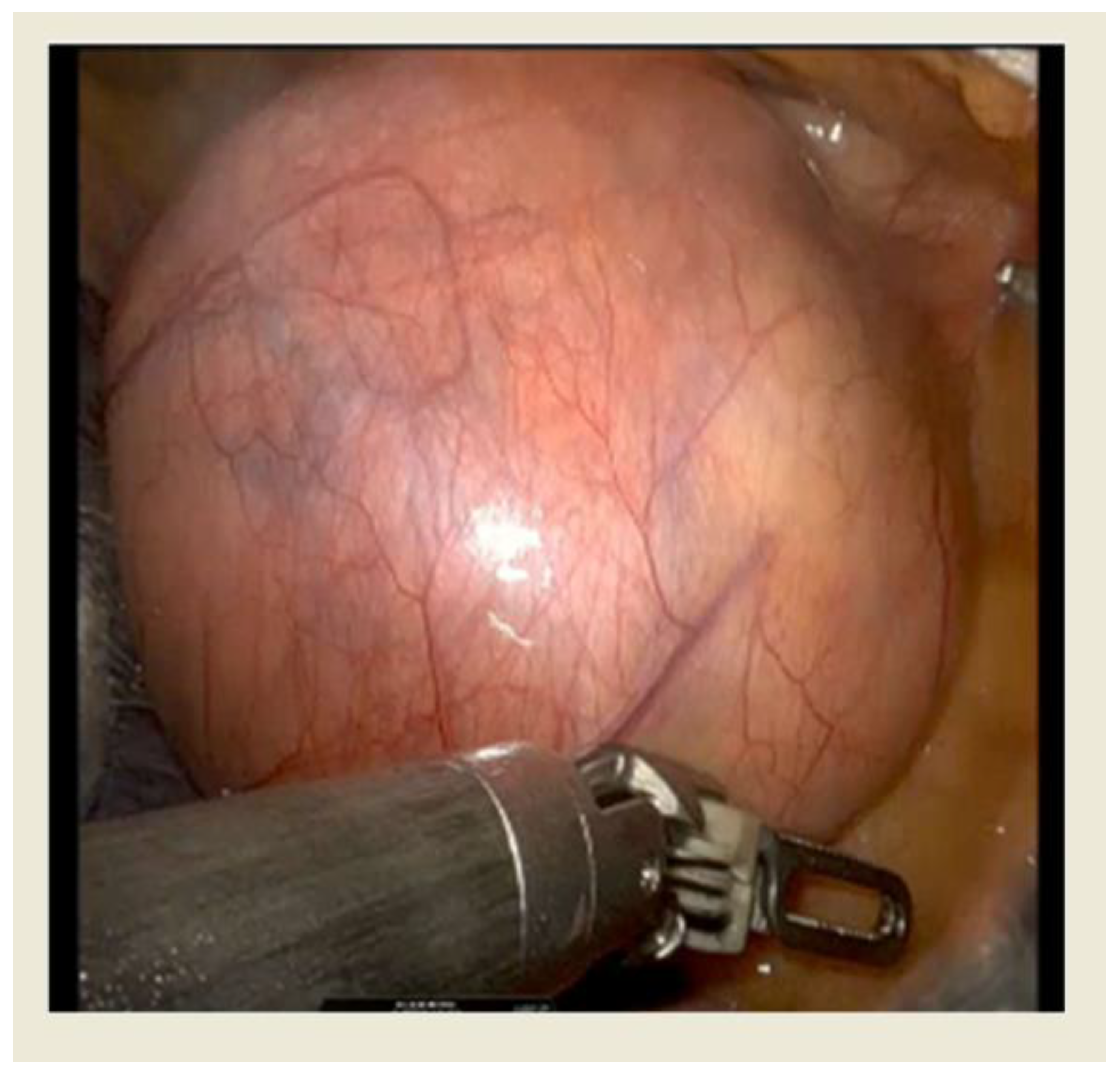
Funding
Institutional Review Board Statement
Conflicts of Interest
References
- Ruffini, E.; Filosso, P.L.; Guerrera, F.; et al. Optimal surgical approach to thymic malignancies: new trends challenging old dogmas. Lung Cancer. 2018, 118, 161–170. [Google Scholar] [CrossRef] [PubMed]
- Şehitogullari, A.; Nasır, A.; Anbar, R.; Erdem, K.; Bilgin, C. Comparison of perioperative outcomes of videothoracoscopy and robotic surgical techniques in thymoma. Asian J Surg. 2020, 43, 244–250. [Google Scholar] [CrossRef] [PubMed]
- Kaba, E.; Cosgun, T.; Ayalp, K.; Toker, A. Robotic thymectomy for myasthenia gravis. Ann Cardiothorac Surg 2019, 8, 288–291. [Google Scholar] [CrossRef]
- Melfi, F.; Fanucchi, O.; Davini, F.; et al. Ten-year experience of mediastinal robotic surgery in a single referral centre. Eur J Cardiothorac Surg. 2012, 41, 847e851. [Google Scholar] [CrossRef] [PubMed]
- Ye, B.; Tantai, J.C.; Ge, X.X.; et al. Surgical techniques for early- stage thymoma: video-assisted thoracoscopic thymectomy versus transsternal thymectomy. J Thorac Cardiovasc Surg. 2014, 147, 1599e1603. [Google Scholar] [CrossRef] [PubMed]
- Pennathur, A.; Qureshi, I.; Schuchert, M.J.; et al. Comparison of surgical techniques for early-stage thymoma: feasibility of minimally invasive thymectomy and comparison with open resection. J Thorac Cardiovasc Surg. 2011, 11, 694e701. [Google Scholar] [CrossRef] [PubMed]
- 5th ed. WHO Classification of Tumours. 5. International Agency for Research on Cancer, Lyon, France2021.
- Koga, K.; Matsuno, Y.; Noguchi, M.; et al. A review of 79 thymomas: modification of staging system and reappraisal of conventional division into invasive and non-invasive thymoma. Pathol Int. 1994, 44, 359–367. [Google Scholar] [CrossRef] [PubMed]
- Shields, T.W. Primary tumors and cysts of the mediastinum. In: Shields’ General Thoracic Surgery. 8th ed. Philadelphia: Lea & Febiger, 1972:908.
- D'Andrilli, A.; Venuta, F.; Rendina, E.A. Surgical approaches for invasive tumors of the anterior mediastinum. Thorac Surg Clin. 2010, 20, 265–284. [Google Scholar] [CrossRef] [PubMed]
- Marulli, G.; Comacchio, G.M.; Schiavon, M.; et al. Comparing robotic and trans-sternal thymectomy for early-stage thymoma: a propensity score-matching study. Eur J Cardiothorac Surg 2018, 54, 579–584. [Google Scholar] [CrossRef]
- Chiba, Y.; Miyajima, M.; Takase, Y.; Tsuruta, K.; Shindo, Y.; Nakamura, Y.; Ishii, D.; Sato, T.; Aoyagi, M.; Shiraishi, T.; Sonoda, T.; Watanabe, A. Robot-assisted and video-assisted thoracoscopic surgery for thymoma: comparison of the perioperative outcomes using inverse probability of treatment weighting method. Gland Surg 2022, 11, 1287–1300. [Google Scholar] [CrossRef]
- Friedant, A.J.; Handorf, E.A.; Su, S.; Scott, W.J. Minimally invasive versus open thymectomy for thymic malignancies: systematic review and meta-ana- lysis. J Thorac Oncol 2015, 11, 30–38. [Google Scholar] [CrossRef]
- Maurizi, G.; D'Andrilli, A.; Sommella, L.; Venuta, F.; Rendina, E.A. Transsternal thymectomy. Thorac Cardiovasc Surg. 2015, 63, 178–186. [Google Scholar] [CrossRef] [PubMed]
- Xie, A.; Tjahjono, R.; Phan, K.; Yan, T.D. Video-assisted thoracoscopic surgery versus open thymectomy for thymoma: a systematic review. Ann Cardiothorac Surg. 2015, 4, 495–508. [Google Scholar] [CrossRef] [PubMed]
- Qian, L.; Chen, X.; Huang, J.; et al. A comparison of three ap- proaches for the treatment of early-stage thymomas: robot- assisted thoracic surgery, video-assisted thoracic surgery, and median sternotomy. J Thorac Dis. 2017, 9, 1997e2005. [Google Scholar] [CrossRef]
- Shen, C.; Li, J.; Li, J.; Che, G. Robot-assisted thoracic surgery versus video- assisted thoracic surgery for treatment of patients with thymoma: a systematic review and meta-analysis. Thorac Cancer. 2022, 13, 151–161. [Google Scholar] [CrossRef] [PubMed]
- Wu, W.J.; Zhang, F.Y.; Xiao, Q.; Li, X.K. Does robotic-assisted thymectomy have advantages over video-assisted thymectomy in short-term outcomes? A systematic review and meta-analysis. Interact Cardiovasc Thorac Surg. 2021, 33, 385–394. [Google Scholar] [CrossRef]
- Wang, C.Q.; Wang, J.; Liu, F.Y.; Wang, W. Robot-assisted thoracoscopic surgery vs. sternotomy for thymectomy: A systematic review and meta-analysis. Front Surg. 2023, 9, 1048547. [Google Scholar] [CrossRef] [PubMed]
- Kang, C.H.; Hwang, Y.; Lee, H.J.; Park, I.K.; Kim, Y.T. Robotic thymectomy in anterior mediastinal mass: propensity score matching study with transsternal thymectomy. Ann Thorac Surg. 2016, 102, 895–901. [Google Scholar] [CrossRef]
- Marulli, G.; Rea, F.; Melfi, F.; et al. Robot-aided thoracoscopic thymectomy for early-stage thymoma: a multicenter European study. J Thorac Cardiovasc Surg. 2012, 144, 1125e1130. [Google Scholar] [CrossRef]
- Wilshire, C.L.; Vallieres, E.; Shultz, D.; Aye, R.W.; Farivar, A.S.; Louie, B.E. Robotic resection of 3 cm and larger thymomas is associated with low peri- operative morbidity and mortality. Innovations (Phila) 2016, 11, 321–326. [Google Scholar] [CrossRef]
- Kimura, T.; Inoue, M.; Kadota, Y.; et al. The oncological feasi- bility and limitations of video-assisted thoracoscopic thy- mectomy for early-stage thymomas. Eur J Cardiothorac Surg 2013, 44, e214–8. [Google Scholar] [CrossRef] [PubMed]
- Seong, Y.W.; Kang, C.H.; Choi, J.W.; Kim, H.S.; Jeon, J.H.; Park, I.K.; et al. Early clinic- al outcomes of robot-assisted surgery for anterior mediastinal mass: its superiority over a conventional sternotomy approach evaluated by pro- pensity score matching. Eur J Cardiothorac Surg 2014, 45, e68–e73; discussion e73. [Google Scholar] [CrossRef] [PubMed]
- Kneuertz, P.J.; Kamel, M.K.; Stiles, B.M.; Lee, B.E.; Rahouma, M.; Nasar, A.; et al. Robotic thymectomy is feasible for large thymomas: a propensity- matched comparison. Ann Thorac Surg 2017, 104, 1673–1678. [PubMed]
- Comacchio, G.M.; Schiavon, M.; Zirafa, C.C.; De Palma, A.; Scaramuzzi, R.; Meacci, E.; et al. Robotic thymectomy in thymic tumours: a multicentre, na- tion-wide study. Eur J Cardiothorac Surg 2024. [CrossRef]
- Pompili, C.; Koller, M.; Velikova, G.; et al. EORTC QLQ-C30 summary score reliably detects changes in QoL three months after anatomic lung resection for Non-Small Cell Lung Cancer (NSCLC). Lung Cancer 2018, 123, 149–154. [Google Scholar] [CrossRef] [PubMed]
- Mattioni, G.; Palleschi, A.; Mendogni, P.; Tosi, D. Approaches and outcomes of Robotic-Assisted Thoracic Surgery (RATS) for lung cancer: a narrative review. J Robot Surg. 2023, 17, 797–809. [Google Scholar] [CrossRef] [PubMed]
- Burt, B.M.; Yao, X.; Shrager, J.; et al. Determinants of complete resection of thymoma by minimally invasive and open thy- mectomy: analysis of an international registry. J Thorac Oncol 2017, 12, 129–136. [Google Scholar] [CrossRef]
- Park, J.H.; Na, K.J.; Kang, C.H.; Park, S.; Park, I.K.; Kim, Y.T. Robotic subxiphoid thymectomy versus lateral thymectomy: a propensity score-matched comparison. Eur J Cardiothorac Surg 2022, 62, ezac288. [Google Scholar] [CrossRef]
| RATS 40 | STERNOTOMY 40 | TORACOTOMY 40 | VATS 40 | ||||
| n (%) | n (%) | p | n (%) | p | n (%) | p | |
| Age, mean ± SD | 62.26 ± 8.57 | 54.14 ± 11.43 | 0.299 | 61.34 ± 9.8 | 0.892 | 61.28 ± 9.8 | 0.885 |
| Gender (M/F) | 14/26 | 16/24 | 0.817 | 10/30 | 0.465 | 15/25 | 1 |
| Miastenia | 8 (20%) | 16 (40%) | 0.087 | 6 (15%) | 0.769 | 7 (17.5%) | 1 |
| Surgery time, mean ± SD | 70.60 ± 8.13 | 116.41 ± 22.48 | 0.008 | 76.25 ± 13.15 | 0.598 | 90 ± 11.55 | 0.030 |
| Surgery time without docking, mean ± SD | 51.25 ± 16.52 | 116.41 ± 22.48 | 0.003 | 76.25 ± 13.15 | 0.005 | 90 ± 11.55 | 0.008 |
| Associated resections | 4 (10%) | 14 (35%) | 0.015 | 3 (7.5%) | 1 | 0 (0%) | 0.116 |
| Conversion rate | 0 (0%) | 0 (0%) | 1 | 0 (0%) | 1 | 6 (15%) | 0.026 |
| R0 | 39 (97.5%) | 40 (100%) | 1 | 36 (90%) | 0.036 | 39 (97.5%) | 1 |
| Lenght of stay in days, mean ± SD | 3.36 ± 1.73 | 7.44 ± 3.67 | < 0.001 | 4.12 ± 1.51 | 0.104 | 3.64 ± 1.38 | 0.530 |
| Morbidity | 3 (7.5%) | 5 (12.5%) | 0.712 | 5 (12.5%) | 0.712 | 5 (12.5%) | 0.712 |
| Histology A AB B1 B2 B3 |
5 (12.5%) 13 (32.5%) 5 (12.5%) 5 (12.5%) 12 (30%) |
5 (12.5%) 10 (25%) 10 (25%) 10 (25%) 5 (12.5%) |
1 0.622 0.252 0.252 0.099 |
11 (27.5%) 11 (27.5%) 10 (25%) 5 (12.5%) 3 (7.5%) |
0.161 0.161 0.252 1 0.019 |
8 (20%) 14 (35%) 7 (17.5%) 8 (20%) 3 (7.5%) |
0.546 1 0.755 0.546 0.019 |
| Masaoka I IIA IIB III |
10 (25%) 21 (52.5%) 8 (20%) 1 (2.5%) |
13 (32.5%) 13 (32.5%) 11 (27.5%) 3 (7.5%) |
0.622 0.113 0.600 0.615 |
10 (25%) 20 (50%) 10 (25%) 0 (0%) |
1 1 0.789 1 |
16 (40%) 11 (27.5%) 13 (32.5%) 0 (0%) |
0.232 0.039 0.309 1 |
| Dimensions, mean ± SD | 6.14 ± 1.86 | 7.72 ± 1.25 | 0.089 | 6.21 ± 1.49 | 0.877 | 4.71 ± 0.48 | 0.073 |
| Pain, mean ± SD 24 hours 48 hours |
2.2 ± 0.8 2.2 ± 0.7 |
5.2 ± 0.9 5.1 ± 0.6 |
0.003 0.004 |
5.8 ± 0.7 5.3 ± 0.7 |
0.001 0.001 |
4.3 ± 0.5 4.0 ± 0.9 |
0.004 0.014 |
| Cosmetic results, mean ±SD | 9.1 ± 0.5 | 4.1 ± 0.8 | 0.0001 | 6.1 ± 0.9 | 0.001 | 8 ± 0.8 | 0.052 |
| Approach | complications | N; % |
|---|---|---|
| RATS | 2 Atrial fibrillation 1 Moderate pleural effusion |
3; 7.5% |
| STERNOTOMY | 2 Phrenic nerve injury 1 Intraoperative ventricular fibrillation 1 Bleeding 1 Pneumonia |
5; 12.5% |
| THORACOTOMY | 1 Thoracotomy dehiscence 2 Emothorax requiring re-intervention 2 Pneumonia |
5; 12.5% |
| VATS | 1 Pulmonary embolism 1 Miastenic crisis 2 Bleeding 1 Pneumonia |
5; 12.5% |
| Approach | side | Type of associated resection | N; % |
|---|---|---|---|
| RATS | 2 left 2 right |
1 Anonymous vein 2 Atypical resection upper lobe 1 Pericardium |
4; 10% |
| Sternotomy | 2 left and 3 right 4 left and 2 right 2 lefts 1 right |
5 Pericardium 6 Atypical resection upper lobe 2 Phrenic nerves 1 Mediastinal pleura |
14; 35% |
| Thoracotomy | 1 left 1 left and 1 right |
1 Phrenic nerve 2 Atypical resection upper lobe |
3; 7.5% |
| VATS | 0 | 0 | 0; 0% |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




