Submitted:
18 March 2024
Posted:
19 March 2024
You are already at the latest version
Abstract
Keywords:
Introduction
Methods
Study Population
Air Quality and Meteorological Variables
Statistical Analysis
Results
Study Population
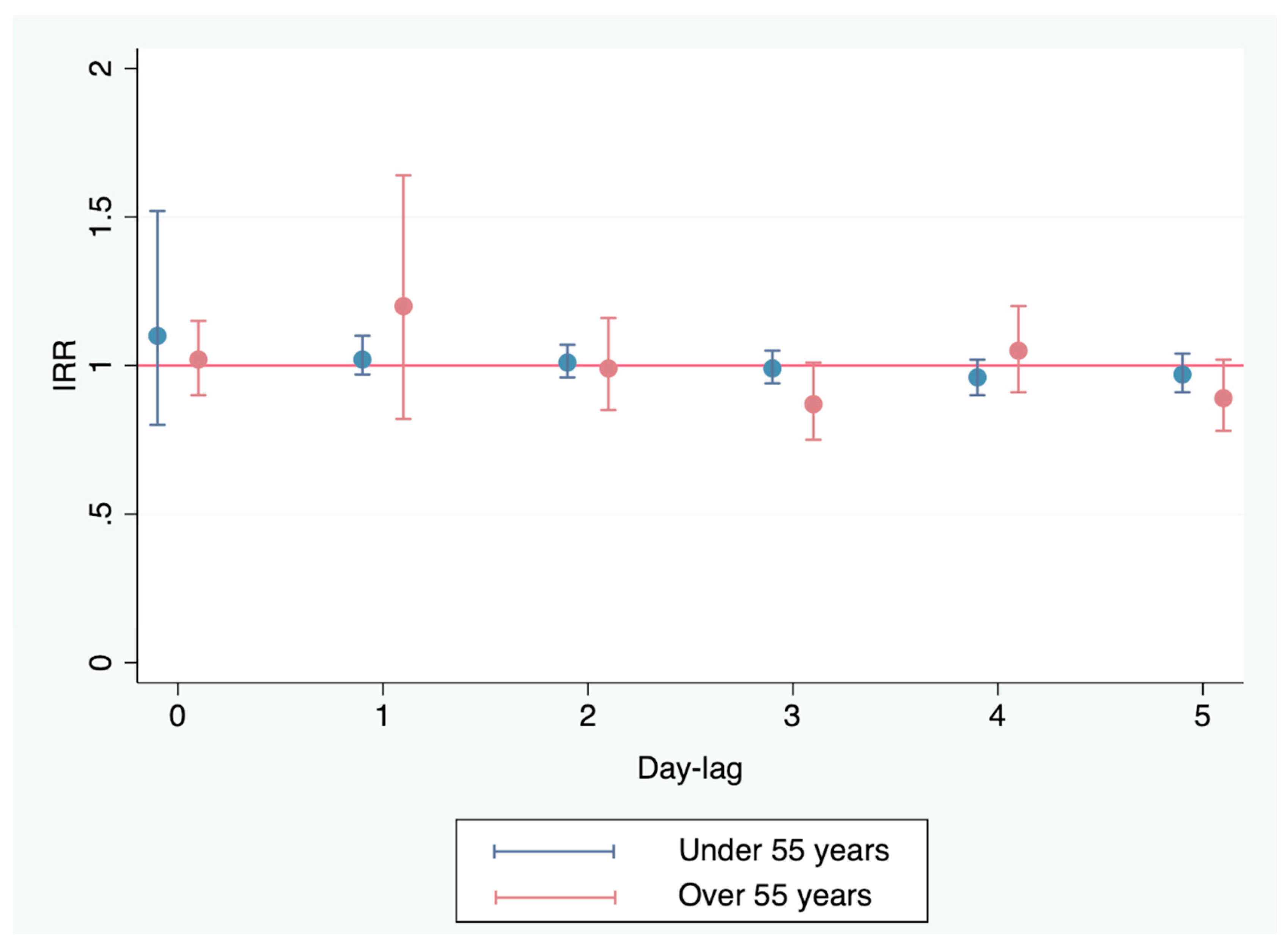
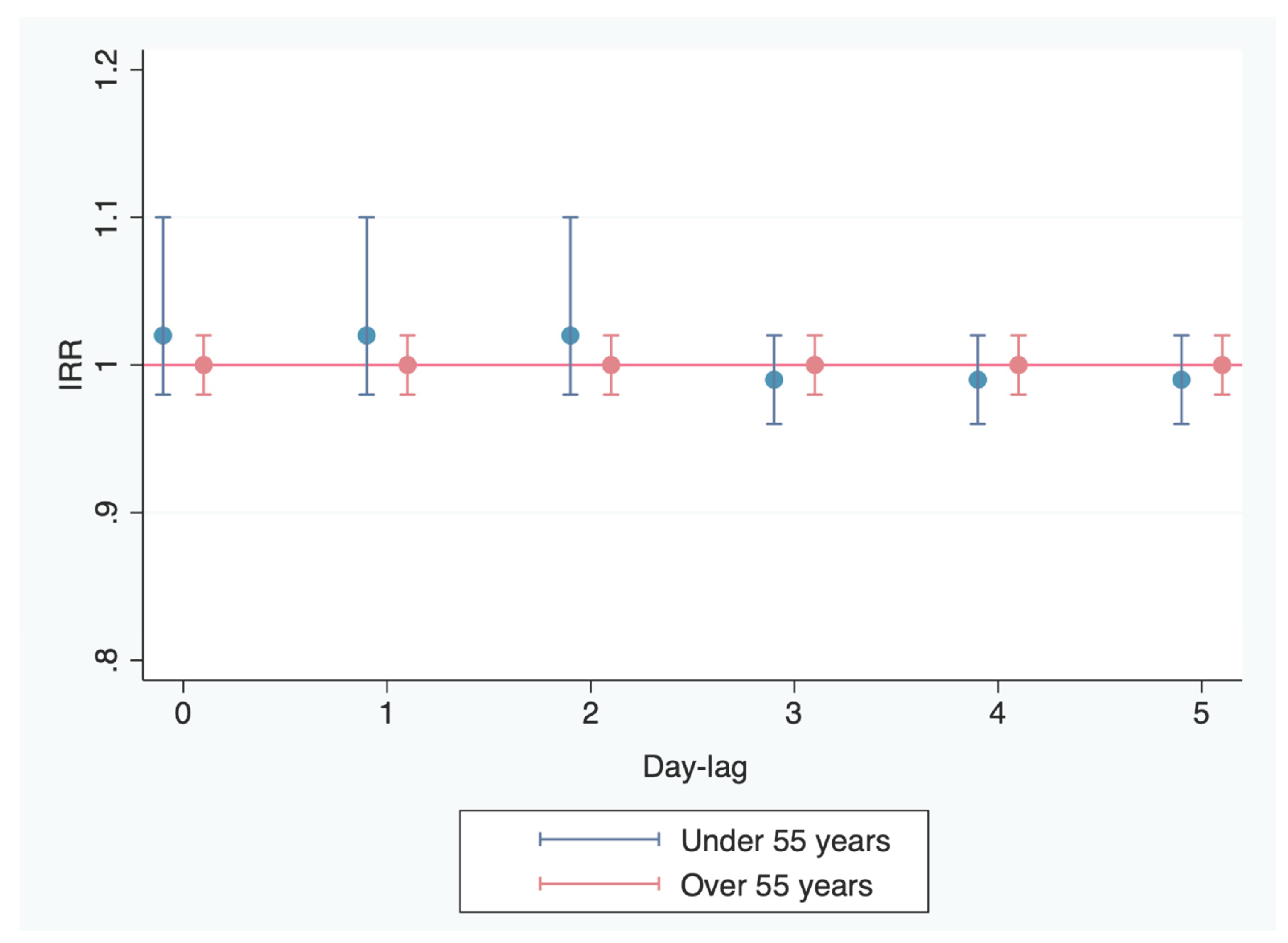
Patients with ACS under 55 years of age
Patients with ACS over 55 Years of Age
Discussion
Limitations
Conclusions
Supplementary Materials
Conflicts of Interests
Source of Funding
Acknowledgements
Author Contributions
Institutional Review Board Statement
Informed Consent Statement
Data Availability
References
- Benito Lozano, M.; Rodríguez, S. La imperiosa necesidad de programar la asistencia a urgencias, atendiendo al cambio climático y las crisis de calidad del aire. Rev Esp Urg Emerg. 2023, 2, 194–1977. [Google Scholar]
- Rodríguez, S.; Cuevas, E.; Prospero, J.M.; et al. Modulation of Saharan dust export by the North African dipole Atmos. Chem. Phys. 2015, 15, 7471–7486. [Google Scholar]
- Dominguez-Rodriguez, A.; Rodríguez, S.; Baez-Ferrer, N.; Abreu-Gonzalez, P.; Abreu-Gonzalez, J.; Avanzas, P.; Carnero, M.; Moris, C.; López-Darias, J.; Hernández-Vaquero, D. Impact of Saharan dust exposure on airway inflammation in patients with ischemic heart disease. Transl. Res. 2020, 224, 16–25. [Google Scholar] [CrossRef] [PubMed]
- Domínguez-Rodríguez, A.; Báez-Ferrer, N.; Abreu-González, P.; Rodríguez, S.; Díaz, R.; Avanzas, P.; Hernández-Vaquero, D. Impact of Desert Dust Events on the Cardiovascular Disease: A Systematic Review and Meta-Analysis. J. Clin. Med. 2021, 10, 727. [Google Scholar] [CrossRef] [PubMed]
- Pascual, I.; Avanzas, P.; Almendárez, M.; et al. STEMI, primary percutaneous coronary intervention and recovering of life expectancy: insights from the SurviSTEMI study. Rev Esp Cardiol (Engl Ed). 2021, 74, 829–837. [Google Scholar] [CrossRef] [PubMed]
- Smith, C.L.; Seigerman, M.; Adusumalli, S.; Giri, J.; Fiorilli, P.N.; Kolansky, D.M.; Kobayashi, T. Evolution and Outcomes of Premature Coronary Artery Disease. Curr. Cardiol. Rep. 2021, 23, 36. [Google Scholar] [CrossRef] [PubMed]
- Pérez, C.; Haustein, K.; Janjic, Z.; et al. Atmospheric dust modeling from meso to global scales with the online NMMB/BSC-Dust model – Part 1: Model description, annual simulations and evaluation, Atmos. Chem. Phys. 2011, 11, 13001–13027. [Google Scholar] [CrossRef]
- Lu, Y.; Zeger, S.L. On the equivalence of case-crossover and time series methods in environmental epidemiology. Biostatistics 2006, 8, 337–344. [Google Scholar] [CrossRef] [PubMed]
- Armstrong, B.G.; Gasparrini, A.; Tobias, A. Conditional Poisson models: a flexible alternative to conditional logistic case cross-over analysis. BMC Med Res. Methodol. 2014, 14, 122. [Google Scholar] [CrossRef] [PubMed]
- Bhaskaran, K.; Gasparrini, A.; Hajat, S.; Smeeth, L.; Armstrong, B. Time series regression studies in environmental epidemiology. Leuk. Res. 2013, 42, 1187–1195. [Google Scholar] [CrossRef] [PubMed]
- Bañeras, J.; Iglesies-Grau, J.; Téllez-Plaza, M.; Arrarte, V.; Báez-Ferrer, N.; Benito, B.; Ruiz, R.C.; Cecconi, A.; Domínguez-Rodríguez, A.; Rodríguez-Sinovas, A.; et al. Environment and cardiovascular health: causes, consequences and opportunities in prevention and treatment. 2022, 75, 1050–1058. [CrossRef]
- Münzel, T.; Hahad, O.; Sørensen, M.; Lelieveld, J.; Duerr, G.D.; Nieuwenhuijsen, M.; Daiber, A. Environmental risk factors and cardiovascular diseases: a comprehensive expert review. Cardiovasc. Res. 2022, 118, 2880–2902. [Google Scholar] [CrossRef] [PubMed]
- Kojima, S.; Michikawa, T.; Ueda, K.; Sakamoto, T.; Matsui, K.; Kojima, T.; Tsujita, K.; Ogawa, H.; Nitta, H.; Takami, A. Asian dust exposure triggers acute myocardial infarction. Eur. Hear. J. 2017, 38, 3202–3208. [Google Scholar] [CrossRef] [PubMed]
- Vodonos, A.; Friger, M.; Katra, I.; Krasnov, H.; Zahger, D.; Schwartz, J.; Novack, V. Individual Effect Modifiers of Dust Exposure Effect on Cardiovascular Morbidity. PLOS ONE 2015, 10, e0137714. [Google Scholar] [CrossRef] [PubMed]
- Domínguez-Rodríguez, A.; Rodríguez, S.; Baez-Ferrer, N.; et al. Impact of Saharan dust on the incidence of acute coronary syndrome. Rev Esp Cardiol (Engl Ed). 2021, 74, 321–328. [Google Scholar] [CrossRef] [PubMed]
- de Longueville, F.; Ozer, P.; Doumbia, S.; Henry, S. Desert dust impacts on human health: an alarming worldwide reality and a need for studies in West Africa. Int. J. Biometeorol. 2013, 57, 1–19. [Google Scholar] [CrossRef] [PubMed]
- Bañeras, J.; Ferreira-González, I.; Marsal, J.R.; Barrabés, J.A.; Ribera, A.; Lidón, R.M.; Domingo, E.; Martí, G.; García-Dorado, D. Short-term exposure to air pollutants increases the risk of ST elevation myocardial infarction and of infarct-related ventricular arrhythmias and mortality. Int. J. Cardiol. 2018, 250, 35–42. [Google Scholar] [CrossRef] [PubMed]
- Zeger, S.L.; Thomas, D.; Dominici, F.; Samet, J.M.; Schwartz, J.; Dockery, D.; Cohen, A. Exposure Measurement Error in Time-Series Studies of Air Pollution: Concepts and Consequences. Environ. Heal. Perspect. 2000, 108, 419. [Google Scholar] [CrossRef] [PubMed]
- Domínguez-Rodríguez, A.; Avanzas, P.; Báez-Ferrer, N.; Abreu-González, P.; Rodríguez, S.; Matos-Castro, S.; Hernández-Vaquero, D. Rationale and Design of the Impact of Air Pollution Due to DESERT Dust in Patients with HEART Failure (DESERT HEART). J. Clin. Med. 2023, 12, 4990. [Google Scholar] [CrossRef] [PubMed]
| Variable |
Under 55 years N = 686 |
Over 55 years N = 1730 |
P-value |
|---|---|---|---|
| Age (years) | 48.9 ± 5 | 69.9 ± 9 | < 0.001 |
| Women | 131 (19.1%) | 518 (29.9%) | < 0.001 |
| Arterial hypertension | 285 (41.6%) | 1257 (72.7%) | < 0.001 |
| Dyslipidemia | 333 (48.6%) | 1067 (61.7%) | < 0.001 |
| Diabetes | 129 (18.8%) | 754 (43.6%) | < 0.001 |
| Asthma | 24 (3.5%) | 58 (3.4%) | 0.9 |
| Chronic obstructive pulmonary disease | 10 (1.5%) | 122 (7.1%) | < 0.001 |
| Chronic kidney disease | 12 (1.8%) | 243 (14.1%) | < 0.001 |
| Previously known coronary disease | 108 (15.8%) | 566 (32.7%) | < 0.001 |
| Supraventricular arrhythmia | 3 (0.4%) | 146 (8.4%) | < 0.001 |
| Acute myocardial infarction | 438 (63.9%) | 912 (52.8%) | < 0.001 |
| Left ventricular dysfunction | 124 (18.1%) | 439 (25.4%) | < 0.001 |
| Killip class I II III IV |
648 (94.5%) 12 (1.8%) 2 (0.3%) 24 (3.5%) |
1423 (82.3%) 146 (8.5%) 46 (2.7%) 113 (6.5%) |
< 0.001 |
| Coronary artery lesions No lesions Single-vessel disease Two-vessel disease Three-vessel disease |
43 (6.4%) 409 (60.5%) 158 (23.4%) 66 (9.8%) |
135 (8.4%) 639 (39.7%) 442 (27.5%) 394 (24.5%) |
< 0.001 |
| Troponin I peak (ng/ml) | 26.6 ± 29.7 | 21.2 ± 27.7 | < 0.001 |
| Percutaneous transluminal coronary angioplasty treatment | 552 (80.5%) | 1090 (63.1%) | < 0.001 |
| Surgical treatment | 33 (4.8%) | 137 (7.9%) | 0.01 |
| In-hospital mortality | 9 (1.3%) | 120 (6.9%) | < 0.001 |
| One-year mortality among the survivors | 3 (0.4%) | 15 (0.9%) | 0.43 |
| Day | No ACS/day N = 1246 |
1 ACS/day N = 481 |
2 ACS/day N = 83 |
3 ACS/day N = 13 |
P-value |
|---|---|---|---|---|---|
| Day of admission PM10 (μg/m3) |
21.5 ± 23.4 | 21.5 ± 22.2 | 20.6 ± 18.7 | 14.3 ± 7.8 | 0.71 |
| 1 Day before PM10 (μg/m3) |
21.3 ± 21.2 | 21.4 ± 25.8 | 24 ± 28.1 | 16.2 ± 10.7 | 0.62 |
| 2 Days before PM10 (μg/m3) |
20.8 ± 19.2 | 22.6 ± 29.3 | 24.4 ± 29.2 | 16.6 ± 11.3 | 0.24 |
| 3 Days before PM10 (μg/m3) |
21.3 ± 21.6 | 21.7 ± 26.9 | 20.4 ± 13.2 | 17.2 ± 13.4 | 0.87 |
| 4 Days before PM10 (μg/m3) |
21.7 ± 24.2 | 20.6 ± 20.3 | 19.8 ± 12.9 | 20.8 ± 14.4 | 0.75 |
| 5 Days before PM10 (μg/m3) |
21.6 ± 23.8 | 20.8 ± 21.2 | 20.6 ± 16.1 | 19.2 ± 15 | 0.89 |
| Atmospheric variable | IRR (95% CI) |
|---|---|
| PM10 (μg/m3) | 1.1 (95% CI 0.8-1.52) |
| PM2.5-10 (μg/m3) | 0.84 (95% CI 0.55-1.29) |
| PM2.5 (μg/m3) | 1.01 (95% CI 0.82-1.24) |
| SO2 (μg/m3) | 1.01 (95% CI 0.91-1.1) |
| NO2 (μg/m3) | 1.03 (95% CI 0.98-1.1) |
| O3 (μg/m3) | 1 (95% CI 0.99-1.01) |
| Temperature (ºC) | 1 (95% CI 0.89-1.1) |
| Humidity (%) | 1 (95% CI 0.99-1) |
| Day | No ACS/day N = 723 |
1 ACS/day N = 646 |
2 ACS/day N = 321 |
3 or more ACS/day N = 134 |
P-value |
|---|---|---|---|---|---|
| Day of admission PM10 (μg/m3) |
22.1 ± 25.9 | 20.4 ± 19.3 | 22.2 ± 24.2 | 20.4 ± 15.5 | 0.84 |
| 1 Day before PM10 (μg/m3) |
22.5 ± 25.8 | 21.1 ± 22.7 | 20.9 ± 14.7 | 18.1 ± 21.12 | 0.64 |
| 2 Days before PM10 (μg/m3) |
22 ± 22.8 | 20.8 ± 22.4 | 21.4 ± 23.9 | 21.8 ± 23.4 | 0.89 |
| 3 Days before PM10 (μg/m3) |
21.9 ± 22.4 | 20.5 ± 21.6 | 22 ± 26.4 | 20.7 ± 23.1 | 0.85 |
| 4 Days before PM10 (μg/m3) |
21.1 ± 20.9 | 21.3 ± 22.4 | 22 ± 26.8 | 21.1 ± 25.7 | 0.99 |
| 5 Days before PM10 (μg/m3) |
21.4 ± 24.4 | 20.5 ± 19.5 | 22.2 ± 24.9 | 23.9 ± 25.9 | 0.75 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




