Submitted:
18 February 2024
Posted:
19 February 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Results
Descriptive analysis
Disproportionality analyses
MedDRA® High Level Group Terms Analysis
3. Discussion
Descriptive analysis
Disproportional ADRs
Hangover manifestations
Dry mouth
Nightmares
Worsening of Depression
Strengths and Limitations
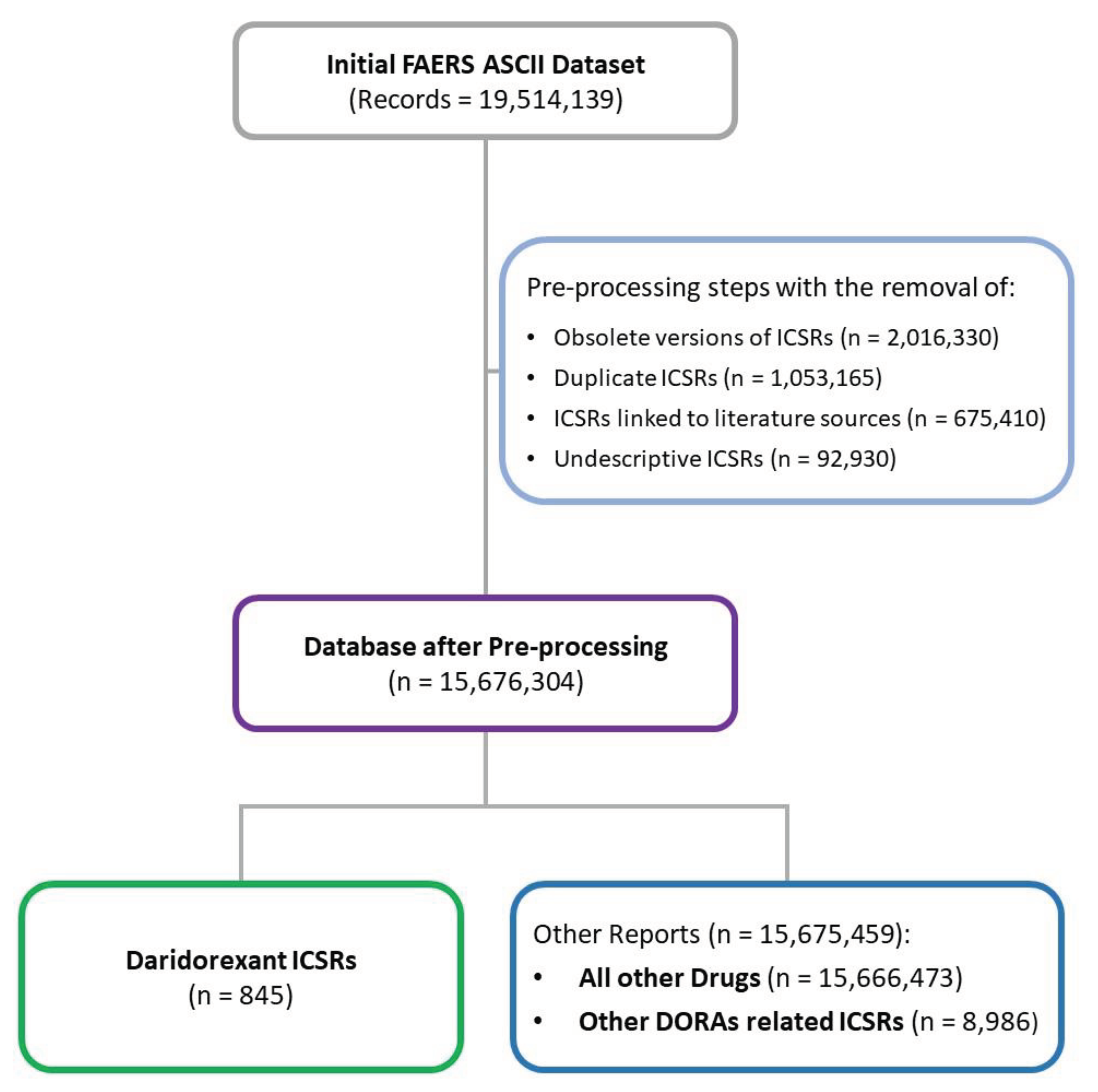
4. Materials and Methods
Data Source and extraction criteria
Data Analyses
Descriptive analysis
Disproportionality analysis
Case-by-case assessments, TTO calculation and ADRs expectedness evaluation
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Data Availability Statement
Conflicts of Interest
References
- American Psychiatric Association Diagnostic and Statistical Manual of Mental Disorders; American Psychiatric Association Publishing, 2022; ISBN 0-89042-575-2.
- Morin, C.M.; Jarrin, D.C. Epidemiology of Insomnia. Sleep. Med. Clin. 2022, 17, 173–191. [Google Scholar] [CrossRef] [PubMed]
- Brownlow, J.A.; Miller, K.E.; Gehrman, P.R. Insomnia and Cognitive Performance. Sleep. Med. Clin. 2020, 15, 71–76. [Google Scholar] [CrossRef]
- Hudgens, S.; Phillips-Beyer, A.; Newton, L.; Seboek Kinter, D.; Benes, H. Development and Validation of the Insomnia Daytime Symptoms and Impacts Questionnaire (IDSIQ). Patient-Patient-Centered Outcomes Res. 2021, 14, 249–268. [Google Scholar] [CrossRef] [PubMed]
- Wilson, S.; Anderson, K.; Baldwin, D.; Dijk, D.-J.; Espie, A.; Espie, C.; Gringras, P.; Krystal, A.; Nutt, D.; Selsick, H.; et al. British Association for Psychopharmacology Consensus Statement on Evidence-Based Treatment of Insomnia, Parasomnias and Circadian Rhythm Disorders: An Update. J. Psychopharmacol. 2019, 33, 923–947. [Google Scholar] [CrossRef]
- Riemann, D.; Baglioni, C.; Bassetti, C.; Bjorvatn, B.; Dolenc Groselj, L.; Ellis, J.G.; Espie, C.A.; Garcia-Borreguero, D.; Gjerstad, M.; Gonçalves, M.; et al. European Guideline for the Diagnosis and Treatment of Insomnia. J. Sleep. Res. 2017, 26, 675–700. [Google Scholar] [CrossRef] [PubMed]
- Qaseem, A.; Kansagara, D.; Forciea, M.A.; Cooke, M.; Denberg, T.D. Management of Chronic Insomnia Disorder in Adults: A Clinical Practice Guideline From the American College of Physicians. Ann. Intern. Med. 2016, 165, 125. [Google Scholar] [CrossRef] [PubMed]
- Agnew, S.; Vallières, A.; Hamilton, A.; McCrory, S.; Nikolic, M.; Kyle, S.D.; Fleming, L.; Crawford, M.R. Adherence to Cognitive Behavior Therapy for Insomnia. Sleep Med. Clin. 2021, 16, 155–202. [Google Scholar] [CrossRef]
- Madari, S.; Golebiowski, R.; Mansukhani, M.P.; Kolla, B.P. Pharmacological Management of Insomnia. Neurotherapeutics 2021, 18, 44–52. [Google Scholar] [CrossRef]
- Fluyau, D.; Revadigar, N.; Manobianco, B.E. Challenges of the Pharmacological Management of Benzodiazepine Withdrawal, Dependence, and Discontinuation. Ther. Adv. Psychopharmacol. 2018, 8, 147–168. [Google Scholar] [CrossRef]
- Schifano, F.; Chiappini, S.; Corkery, J.M.; Guirguis, A. An Insight into Z-Drug Abuse and Dependence: An Examination of Reports to the European Medicines Agency Database of Suspected Adverse Drug Reactions. Int. J. Neuropsychopharmacol. 2019, 22, 270–277. [Google Scholar] [CrossRef]
- Muehlan, C.; Roch, C.; Vaillant, C.; Dingemanse, J. The Orexin Story and Orexin Receptor Antagonists for the Treatment of Insomnia. J. Sleep. Res. 2023. [Google Scholar] [CrossRef]
- Saper, C.B.; Scammell, T.E.; Lu, J. Hypothalamic Regulation of Sleep and Circadian Rhythms. Nature 2005, 437, 1257–1263. [Google Scholar] [CrossRef]
- Stahl, S.M. Mechanism of Action of Suvorexant. CNS Spectr. 2016, 21, 215–218. [Google Scholar] [CrossRef]
- Xue, T.; Wu, X.; Chen, S.; Yang, Y.; Yan, Z.; Song, Z.; Zhang, W.; Zhang, J.; Chen, Z.; Wang, Z. The Efficacy and Safety of Dual Orexin Receptor Antagonists in Primary Insomnia: A Systematic Review and Network Meta-Analysis. Sleep Med. Rev. 2022, 61, 101573. [Google Scholar] [CrossRef]
- Kunz, D.; Dauvilliers, Y.; Benes, H.; García-Borreguero, D.; Plazzi, G.; Seboek Kinter, D.; Coloma, P.; Rausch, M.; Sassi-Sayadi, M.; Thein, S. Long-Term Safety and Tolerability of Daridorexant in Patients with Insomnia Disorder. CNS Drugs 2023, 37, 93–106. [Google Scholar] [CrossRef]
- European Medicines Agency Summary Of Product Characteristics - Qviviq. Human. medicine European public assessment reports Database 2022.
- Palagini, L.; Geoffroy, P.A.; Micoulaud-Franchi, J.A.; Gemignani, A.; Riemann, D. Potential Aggravation of Suicide Risk With Daridorexant. J. Clin. Psychiatry 2023, 84. [Google Scholar] [CrossRef] [PubMed]
- Nobile, B.; Olié, E.; Courtet, P. Possible Suicidal Risk With Daridorexant, a New Treatment for Insomnia. J. Clin. Psychiatry 2022, 84, 44433. [Google Scholar] [CrossRef]
- Salvo, F.; Micoulaud-Franchi, J.-A.; Palagini, L.; Geoffroy, P.A. Dual Orexin Receptor Antagonists and Suicide Risk. J. Clin. Psychiatry 2023, 84. [Google Scholar] [CrossRef]
- Montastruc, J.; Sommet, A.; Bagheri, H.; Lapeyre-Mestre, M. Benefits and Strengths of the Disproportionality Analysis for Identification of Adverse Drug Reactions in a Pharmacovigilance Database. Br. J. Clin. Pharmacol. 2011, 72, 905–908. [Google Scholar] [CrossRef]
- Cicala, G.; de Filippis, R.; Barbieri, M.A.; Cutroneo, P.M.; De Fazio, P.; Schoretsanitis, G.; Spina, E. Tolerability Profile of Paliperidone Palmitate Formulations: A Pharmacovigilance Analysis of the EUDRAVigilance Database. Front. Psychiatry 2023, 14. [Google Scholar] [CrossRef]
- Inácio, P.; Cavaco, A.; Airaksinen, M. The Value of Patient Reporting to the Pharmacovigilance System: A Systematic Review. Br. J. Clin. Pharmacol. 2017, 83, 227–246. [Google Scholar] [CrossRef]
- Weber, J.C.P. Epidemiology in the United Kingdom of Adverse Drug Reactions from Non-Steroidal Anti-Inflammatory Drugs. In; 1987; pp. 27–35.
- Kim, H.-J.; Jeong, H.E.; Bae, J.-H.; Baek, Y.-H.; Shin, J.-Y. Characteristics and Trends of Spontaneous Reporting of Therapeutic Ineffectiveness in South Korea from 2000 to 2016. PLoS ONE 2019, 14, e0212905. [Google Scholar] [CrossRef]
- Blenkinsopp, A.; Wilkie, P.; Wang, M.; Routledge, P.A. Patient Reporting of Suspected Adverse Drug Reactions: A Review of Published Literature and International Experience. Br. J. Clin. Pharmacol. 2007, 63, 148–156. [Google Scholar] [CrossRef]
- Markham, A. Daridorexant: First Approval. Drugs 2022, 82, 601–607. [Google Scholar] [CrossRef]
- Food and Drug Administration QUVIVIQ Full Prescribing Information. Available online: https://www.accessdata.fda.gov/drugsatfda_ docs/label/2022/214985s000lbl.pdf (accessed on 3 May 2023).
- Food and Drug Administration BELSOMRA Full Prescribing Information. Available online: https://www.accessdata.fda.gov/drugsatfda_ docs/label/2014/204569s000lbledt.pdf (accessed on 3 May 2023).
- Apessos, I.; Andreadis, D.; Steiropoulos, P.; Tortopidis, D.; Angelis, L. Investigation of the Relationship between Sleep Disorders and Xerostomia. Clin. Oral. Investig. 2020, 24, 1709–1716. [Google Scholar] [CrossRef]
- Lopez -Jornet, P.; Lucero Berdugo, M.; Fernandez-Pujante, A.; C, C.F.; Lavella C, Z.; A, P.-F.; J, S.R.; Silvestre, F.J. Sleep Quality in Patients with Xerostomia: A Prospective and Randomized Case-Control Study. Acta Odontol. Scand. 2016, 74, 224–228. [Google Scholar] [CrossRef]
- Roth, T.; Yardley, J.; Pinner, K.; Kumar, D.; Cheng, J.; Moline, M. P097 Incidence of Abnormal Dreams and Nightmares with Lemborexant in Adults with Insomnia: Results from Two Phase 3 Studies. Sleep Adv. 2021, 2, A52. [Google Scholar] [CrossRef]
- Rosenberg, R.; Murphy, P.; Zammit, G.; Mayleben, D.; Kumar, D.; Dhadda, S.; Filippov, G.; LoPresti, A.; Moline, M. Comparison of Lemborexant With Placebo and Zolpidem Tartrate Extended Release for the Treatment of Older Adults With Insomnia Disorder. JAMA Netw. Open 2019, 2, e1918254. [Google Scholar] [CrossRef]
- Kärppä, M.; Yardley, J.; Pinner, K.; Filippov, G.; Zammit, G.; Moline, M.; Perdomo, C.; Inoue, Y.; Ishikawa, K.; Kubota, N. Long-Term Efficacy and Tolerability of Lemborexant Compared with Placebo in Adults with Insomnia Disorder: Results from the Phase 3 Randomized Clinical Trial SUNRISE 2. Sleep 2020, 43. [Google Scholar] [CrossRef]
- Paul, F.; Schredl, M.; Alpers, G.W. Nightmares Affect the Experience of Sleep Quality but Not Sleep Architecture: An Ambulatory Polysomnographic Study. Borderline Pers. Disord. Emot. Dysregul 2015, 2, 3. [Google Scholar] [CrossRef]
- Clark, J.W.; Brian, M.L.; Drummond, S.P.A.; Hoyer, D.; Jacobson, L.H. Effects of Orexin Receptor Antagonism on Human Sleep Architecture: A Systematic Review. Sleep. Med. Rev. 2020, 53, 101332. [Google Scholar] [CrossRef]
- Dal Sacco, D. Dream Recall Frequency and Psychosomatics. Acta Biomed. 2022, 93, e2022046. [Google Scholar] [CrossRef]
- Stefani, A.; Högl, B. Nightmare Disorder and Isolated Sleep Paralysis. Neurotherapeutics 2021, 18, 100–106. [Google Scholar] [CrossRef]
- Petrous, J.; Furmaga, K. Adverse Reaction with Suvorexant for Insomnia: Acute Worsening of Depression with Emergence of Suicidal Thoughts. BMJ Case Rep. 2017, bcr-20. [Google Scholar] [CrossRef]
- Brundin, L.; Björkqvist, M.; Petersén, Å.; Träskman-Bendz, L. Reduced Orexin Levels in the Cerebrospinal Fluid of Suicidal Patients with Major Depressive Disorder. Eur. Neuropsychopharmacol. 2007, 17, 573–579. [Google Scholar] [CrossRef]
- Salvo, F.; Micoulaud-Franchi, J.-A.; Palagini, L.; Geoffroy, P.A. Dual Orexin Receptor Antagonists and Suicide Risk. J. Clin. Psychiatry 2023, 84. [Google Scholar] [CrossRef]
- Nutt, D.; Wilson, S.; Paterson, L. Sleep Disorders as Core Symptoms of Depression. Dialogues Clin. Neurosci. 2008, 10, 329–336. [Google Scholar] [CrossRef]
- Cutroneo, P.M.; Sartori, D.; Tuccori, M.; Crisafulli, S.; Battini, V.; Carnovale, C.; Rafaniello, C.; Capuano, A.; Poluzzi, E.; Moretti, U.; et al. Conducting and Interpreting Disproportionality Analyses Derived from Spontaneous Reporting Systems. Front. Drug Saf. Regul. 2024, 3. [Google Scholar] [CrossRef]
- Barbieri, M.A.; Sorbara, E.E.; Cicala, G.; Santoro, V.; Cutroneo, P.M.; Franchina, T.; Spina, E. Adverse Drug Reactions with HER2-Positive Breast Cancer Treatment: An Analysis from the Italian Pharmacovigilance Database. Drugs Real. World Outcomes 2022, 9, 91–107. [Google Scholar] [CrossRef]
- Khouri, C.; Salvo, F.; Raschi, E.; Fusaroli, M. Reporting of A Disproportionality Analysis for DrUg Safety - READUS. Available online: https://readus-statement.org/ (accessed on 15 January 2024).
| Characteristic | Daridorexant-related ICSRs (n = 845) |
Other DORAs related ICSRs (n = 8,986) |
|---|---|---|
| Sex, n° (%) | ||
| Women | 527 (62.4) | 4,914 (54.7) |
| Men | 275 (32.5) | 3,012 (33.5) |
| Not Available | 43 (5.9) | 1,060 (11.8) |
| Age Group, n° (%) | ||
| 0-17 | - | 25 (0.3) |
| 18-34 | 16 (1.9) | 288 (3.2) |
| 35-49 | 45 (5.3) | 591 (6.6) |
| 50-64 | 101 (12) | 1,065 (11.9) |
| 65-79 | 77 (9.1) | 1,254 (14.0) |
| 80+ | 22 (2.6) | 675 (7.5) |
| Not available | 584 (69.1) | 5,088 (56.6) |
| Reporter type, n° (%) | ||
| Consumer | 712 (84.3) | 3,426 (38.1) |
| Healthcare professional | 131 (15.5) | 5,549 (61.8) |
| Not specified | 2 (0.2) | 11 (0.1) |
| Seriousness, n° (%) | ||
| Not serious | 805 (95.3) | 7,427 (82.7) |
| Serious | 40 (4.7) | 1,559 (17.4) |
| Seriousness Criteria, n° (%) | ||
| Death | 9 (1.1) | 159 (1.8) |
| Disability | - | 73 (0.8) |
| Hospitalization | 3 (0.4) | 443 (4.9) |
| Life-Threatening | 1 (0.1) | 85 (0.9) |
| Other Serious Important Medical Event | 26 (3.1) | 797 (8.9) |
| Required Intervention | 1 (0.1) | 2 (0.0) |
| Not Available | 805 (95.3) | 7,427 (82.7) |
| MedDRA HLGTs | ICSRsa |
Daridorexant vs. RG1 ROR [95%CI] |
Daridorexant vs. RG2 ROR [95%CI] |
| Sleep disorders and disturbances | 326 | 26.42 [23.01, 30.35] | 1.84 [1.59, 2.13] |
| Sleep disturbances (incl subtypes) | 32 | 20.63 [14.49, 29.37] | 0.91 [0.63, 1.31] |
| Disturbances in thinking and perception | 44 | 7.15 [5.28, 9.68] | 1.13 [0.82, 1.55] |
| Therapeutic and nontherapeutic effects (excl toxicity) | 311 | 4.74 [4.12, 5.46] | 1.05 [0.91, 1.21] |
| Changes in physical activity | 10 | 4.36 [2.34, 8.14] | 1.88 [0.95, 3.69] |
| Product quality, supply, distribution, manufacturing and quality system issues | 69 | 3.98 [3.11, 5.08] | 4.12 [3.1, 5.47] |
| Salivary gland conditions | 14 | 3.38 [1.99, 5.73] | 2.21 [1.24, 3.94] |
| Headaches | 69 | 2.34 [1.83, 3] | 1.66 [1.27, 2.15] |
| Anxiety disorders and symptoms | 40 | 1.79 [1.31, 2.46] | 1.01 [0.73, 1.41] |
| Depressed mood disorders and disturbances | 25 | 1.73 [1.16, 2.57] | 1.98 [1.29, 3.06] |
| Suicidal and self-injurious behaviours NEC | 16 | 1.63 [0.99, 2.67] | 0.96 [0.57, 1.61] |
| Neurological disorders NEC | 114 | 1.61 [1.32, 1.96] | 1 [0.81, 1.23] |
| Movement disorders (incl parkinsonism) | 26 | 1.48 [0.96, 2.18] | 1.16 [0.77, 1.75] |
| Cardiac disorders, signs and symptoms NEC | 16 | 1.46 [0.89, 2.39] | 1.56 [0.92, 2.64] |
| Overdoses and underdoses NEC | 23 | 1.45 [0.96, 2.19] | 0.85 [0.55, 1.3] |
| Allergic conditions | 30 | 1.43 [0.94, 2.07] | 6.71 [4.24, 10.63] |
| General system disorders NEC | 194 | 1.31 [1.12, 1.54] | 2.11 [1.77, 2.5] |
| Lifestyle issues | 10 | 1.2 [0.64, 2.23] | 3.25 [1.6, 6.62] |
| Deliria (incl confusion) | 11 | 1.19 [0.66, 2.16] | 0.6 [0.33, 1.11] |
| Medication errors and other product use errors and issues | 102 | 1.18 [0.96, 1.45] | 1.21 [0.97, 1.51] |
| Skin appendage conditions | 21 | 0.94 [0.61, 1.44] | 2.49 [1.54, 4.03] |
| Mood disorders and disturbances NEC | 11 | 0.7 [0.39, 1.27] | 0.98 [0.53, 1.83] |
| Muscle disorders | 14 | 0.56 [0.33, 0.95] | 0.95 [0.55, 1.64] |
| Cardiac and vascular investigations (excl enzyme tests) | 11 | 0.54 [0.3, 0.98] | 1.23 [0.66, 2.31] |
| Gastrointestinal signs and symptoms | 41 | 0.54 [0.39, 0.73] | 1.25 [0.9, 1.74] |
| Gastrointestinal motility and defaecation conditions | 21 | 0.52 [0.34, 0.81] | 1.65 [1.03, 2.62] |
| Epidermal and dermal conditions | 34 | 0.49 [0.35, 0.69] | 2.03 [1.4, 2.95] |
| HRespiratory disorders NEC | 22 | 0.45 [0.29, 0.69] | 1.33 [0.85, 2.08] |
| MedDRA PTs | ICSRsa | Daridorexant vs. RG1 ROR [95%CI] |
Daridorexant vs. RG2 ROR [95%CI] |
Expb |
|---|---|---|---|---|
| Nightmare | 146 | 113.74 [95.13, 136] | 2.35 [1.93, 2.85] | Yes |
| Insomnia | 80 | 7.41 [5.88, 9.33] | 1.94 [1.51, 2.49] | No |
| Abnormal dreams | 64 | 52.79 [40.9, 68.13] | 1.16 [0.89, 1.52] | Yes |
| Somnambulism | 18 | 56.94 [35.67, 90.9] | 1.51 [0.91, 2.48] | Yes |
| Middle insomnia | 15 | 19.82 [11.89, 33.03] | 0.98 [0.58, 1.68] | No |
| Poor quality sleep | 10 | 11.51 [6.17, 21.48] | 0.55 [0.29, 1.04] | No |
| Sleep terror | 9 | 61.64 [31.93, 119.02] | 1.85 [0.91, 3.77] | No |
| Sleep-related eating disorder | 4 | 113.13 [42.23, 303.02] | 2.67 [0.89, 7.99] | Yes |
| Initial insomnia | 4 | 9.91 [3.71, 26.46] | 0.6 [0.22, 1.64] | No |
| Hypnagogic hallucination | 3 | 267.22 [85.32, 836.95] | 4 [1.06, 15.1] | Yes |
| MedDRA PTs | ICSRsa | Daridorexant vs. RG1 ROR [95%CI] |
Daridorexant vs. RG2 ROR [95%CI] |
Exp.b |
|---|---|---|---|---|
| Feeling abnormal | 64 | 6.19 [4.8, 7.99] | 1.75 [1.33, 2.29] | No |
| Fatigue | 45 | 1.41 [1.05, 1.91] | 2.28 [1.64, 3.17] | Yes |
| Hangover | 20 | 127.92 [81.98, 199.62] | 3.38 [2.04, 5.61] | Yes |
| Illness | 17 | 7.19 [4.44, 11.62] | 18.43 [8.41, 40.38] | No |
| Malaise | 12 | 0.61 [0.34, 1.07] | 1.07 [0.59, 1.95] | No |
| Feeling jittery | 6 | 6.89 [3.08, 15.37] | 1.25 [0.54, 2.93] | No |
| Asthenia | 6 | 0.37 [0.17, 0.83] | 1.16 [0.5, 2.71] | No |
| Energy increased | 5 | 18.7 [7.76, 45.06] | 6.68 [2.18, 20.47] | No |
| Crying | 5 | 2.95 [1.22, 7.1] | 2.67 [0.99, 7.13] | No |
| Concomitant disease aggravated | 4 | 15.43 [5.78, 41.23] | - | No |
| Sluggishness | 4 | 9.02 [3.38, 24.09] | 3.05 [0.99, 9.28] | Yes |
| Chest pain | 4 | 0.48 [0.18, 1.28] | 1.29 [0.46, 3.65] | No |
| Pain | 4 | 0.14 [0.05, 0.38] | 0.82 [0.29, 2.26] | No |
| Screaming | 3 | 10.74 [3.46, 33.39] | 2.66 [0.75, 9.46] | No |
| Discomfort | 3 | 1.16 [0.37, 3.6] | 2.91 [0.81, 10.44] | No |
| Swelling face | 3 | 1.06 [0.34, 3.3] | 2.91 [0.81, 10.44] | No |
| Condition aggravated | 3 | 0.27 [0.09, 0.83] | 1.88 [0.55, 6.43] | No |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).





