Submitted:
12 February 2024
Posted:
13 February 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction:
2. Methods:
2.1. Case Analysis:
- -
- Collection of clinical data from individuals with CL/P.
- -
- Examination of family histories, genetic profiles, and environmental exposures.
- -
- Identification of any associated syndromes or coexisting conditions.
2.2. Literature Review:
- -
- Systematic search of databases for relevant studies and articles.
- -
- Analysis of genetic, environmental, and teratogenic factors discussed in the literature.
- -
- Review of epidemiological studies on CL/P prevalence and risk factors.
3. Results:
3.1. Genetic Factors:
- -
- Identification of specific genetic mutations and polymorphisms associated with CL/P.
- -
- Analysis of familial clustering and heritability of CL/P.
- -
- Discussion of genetic syndromes such as Van der Woude syndrome and 22q11.2 Deletion Syndrome.
3.2. Environmental Factors:
- -
- Review of maternal factors, including nutrition, smoking, alcohol consumption, and drug exposure.
- -
- Examination of teratogenic agents and their potential impact on CL/P development.
- -
- Evaluation of the role of folic acid supplementation and maternal health during pregnancy.
3.3. Syndromic Associations:
- -
- Exploration of syndromes commonly linked to CL/P, such as Pierre Robin Syndrome.
- -
- Discussion of the genetic and phenotypic overlap with other congenital conditions.
4. Conclusion:
- -
- L: Left lip
- -
- A: Left alveolus (left tooth ridge)
- -
- H: Left hard palate
- -
- S: Soft palate midline
- -
- H: Right hard palate
- -
- A: Right alveolus (right tooth ridge)
- -
- L: Right lip
4.1. Aim of Study
4.2. Data and Data Preparation
4.3. Material
4.4. Statistical Methods
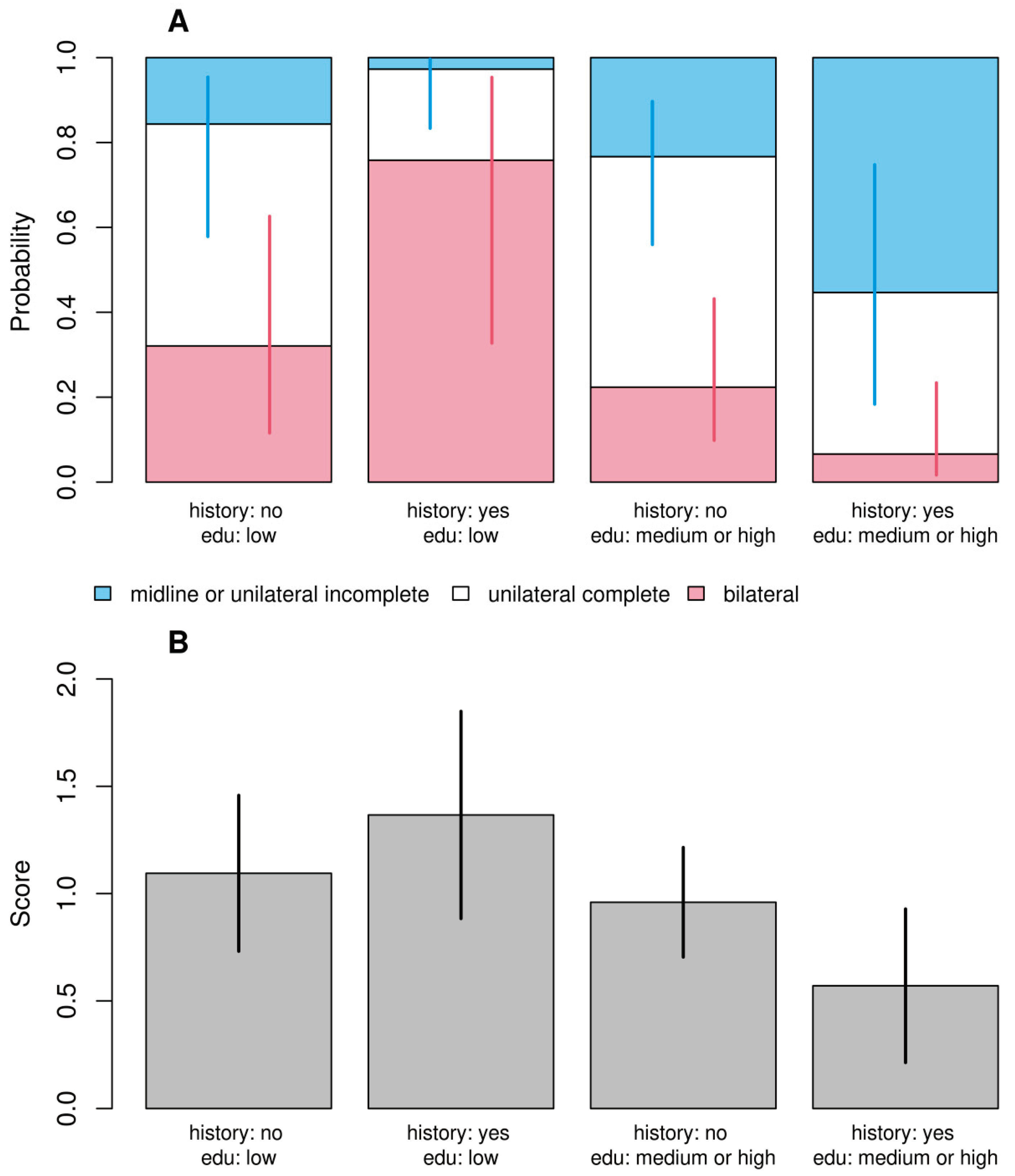
| Midline or unilateral incomplete | Unilateral complete | Bilateral | Score | |
|---|---|---|---|---|
| l | 1 | . | . | 0 |
| L | 3 | . | . | 0 |
| S | 6 | . | . | 0 |
| al | 1 | . | . | 0.333 |
| LA | 1 | . | . | 0.333 |
| sh | 1 | . | . | 0.333 |
| SL | 1 | . | . | 0.333 |
| SU | 1 | . | . | 0.333 |
| HSH | 4 | . | . | 0.333 |
| Lal | 1 | . | . | 0.333 |
| laHS | . | 2 | . | 1 |
| LAHS | . | 15 | . | 1 |
| Shal | . | 1 | . | 1 |
| SHAL | . | 24 | . | 1 |
| HSHAl | . | . | 1 | 1.333 |
| HSHAL | . | . | 2 | 1.333 |
| LAHSH | . | . | 2 | 1.333 |
| LAHSHL | . | . | 1 | 1.667 |
| lHSHAL | . | . | 1 | 1.667 |
| lahSHAL | . | . | 1 | 2 |
| LAHSHal | . | . | 1 | 2 |
| LAHSHAL | . | . | 11 | 2 |
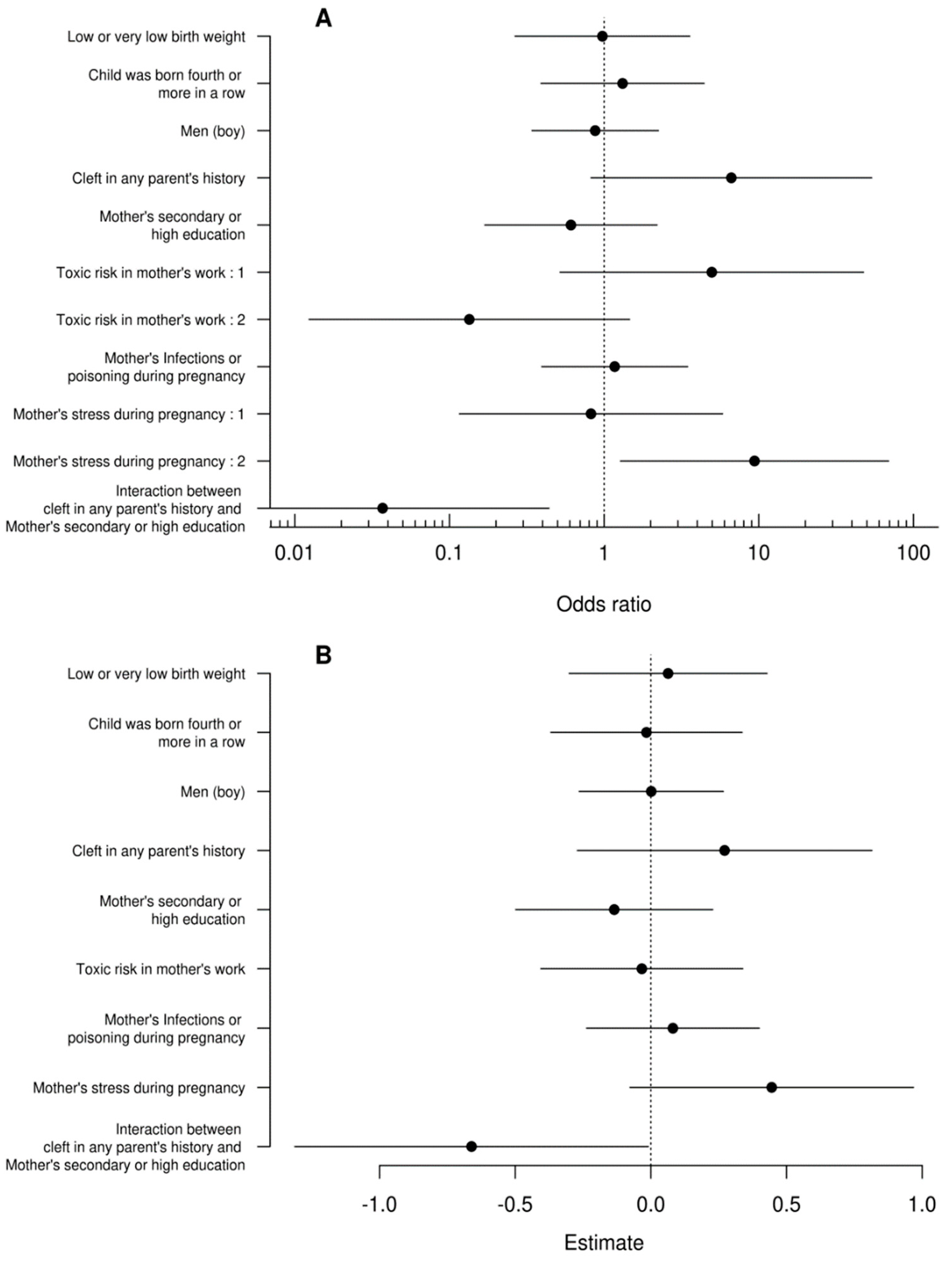
| Odds ratio | 97.5 % | 2.5 % | Estimate | Std. Error | z value | Pr(>|z|) | |
|---|---|---|---|---|---|---|---|
| (Intercept):1 | 5.3849 | 0.7187 | 0.0480 | -1.6836 | 0.6905 | -2.4383 | 0.0148 |
| (Intercept):2 | 0.4718 | 7.7150 | 0.5822 | 0.7511 | 0.6592 | 1.1395 | 0.2545 |
| Low or very low birth weight | 0.9747 | 3.7668 | 0.2794 | 0.0256 | 0.6636 | 0.0385 | 0.9693 |
| Child was born fourth or more in a row | 1.3162 | 2.5587 | 0.2256 | -0.2748 | 0.6195 | -0.4435 | 0.6574 |
| Men (boy) | 0.8755 | 2.9256 | 0.4459 | 0.1329 | 0.4799 | 0.2770 | 0.7818 |
| Cleft in any parent’s history | 6.6475 | 1.2151 | 0.0186 | -1.8942 | 1.0659 | -1.7772 | 0.0755 |
| Mother’s secondary or high education | 0.6102 | 5.9077 | 0.4546 | 0.4940 | 0.6542 | 0.7551 | 0.4502 |
| Toxic risk in mother’s work : 1 | 4.9688 | 1.9260 | 0.0210 | -1.6032 | 1.1524 | -1.3912 | 0.1642 |
| Toxic risk in mother’s work : 2 | 0.1344 | 80.8591 | 0.6845 | 2.0068 | 1.2173 | 1.6486 | 0.0992 |
| Mother’s Infections or drugs toxicity during pregnancy | 1.1702 | 2.5310 | 0.2885 | -0.1572 | 0.5540 | -0.2838 | 0.7766 |
| Mother’s stress during pregnancy : 1 | 0.8226 | 8.6182 | 0.1715 | 0.1953 | 0.9993 | 0.1955 | 0.8450 |
| Mother’s stress during pregnancy : 2 | 9.3879 | 0.7837 | 0.0145 | -2.2394 | 1.0182 | -2.1994 | 0.0278 |
| Interaction between cleft in any parent’s history and Mother’s secondary or high education | 0.0370 | 322.1006 | 2.2732 | 3.2980 | 1.2637 | 2.6098 | 0.0091 |
| Estimate | 2.5 % | 97.5 % | Std. Error | t value | Pr(>|t|) | |
|---|---|---|---|---|---|---|
| (Intercept) | 1.0946 | 0.7251 | 1.4641 | 0.1854 | 5.9050 | 0.0000 |
| Low or very low birth weight | 0.0635 | -0.3011 | 0.4280 | 0.1829 | 0.3470 | 0.7296 |
| Child was born fourth or more in a row | -0.0163 | -0.3688 | 0.3362 | 0.1768 | -0.0921 | 0.9269 |
| Men (boy) | 0.0013 | -0.2641 | 0.2668 | 0.1332 | 0.0100 | 0.9921 |
| Cleft in any parent’s history | 0.2718 | -0.2709 | 0.8146 | 0.2723 | 0.9984 | 0.3214 |
| Mother’s secondary or high education | -0.1350 | -0.4982 | 0.2281 | 0.1822 | -0.7413 | 0.4609 |
| Toxic risk in mother’s work | -0.0333 | -0.4055 | 0.3389 | 0.1867 | -0.1784 | 0.8589 |
| Mother’s Infections or poisoning during pregnancy | 0.0812 | -0.2370 | 0.3993 | 0.1596 | 0.5088 | 0.6125 |
| Mother’s stress during pregnancy | 0.4454 | -0.0770 | 0.9678 | 0.2620 | 1.6996 | 0.0935 |
| Interaction between cleft in any parent’s history and Mother’s secondary or high education | -0.6610 | -1.3124 | -0.0095 | 0.3268 | -2.0227 | 0.0468 |
5. Results
6. Discussion
References
- K. H. Wang et al., “Evaluation and integration of disparate classification systems for clefts of the lip,” Front. Physiol., vol. 5 MAY, no. May, pp. 1–11, 2014. [CrossRef]
- M. J. Dixon, M. L. Marazita, T. H. Beaty, and J. C. Murray, “Cleft lip and palate: Understanding genetic and environmental influences,” Nat. Rev. Genet., vol. 12, no. 3, pp. 167–178, 2011. [CrossRef]
- P. Hlongwa, J. Levin, and L. C. Rispel, “Epidemiology and clinical profile of individuals with cleft lip and palate utilising specialised academic treatment centres in South Africa,” PLoS One, vol. 14, no. 5, pp. 1–14, 2019. [CrossRef]
- C. Parada and Y. Chai, “Roles of BMP signaling pathway in lip and palate development,” Front. Oral Biol., vol. 16, pp. 60–70, 2012. [CrossRef]
- S. A. Tanaka, R. C. Mahabir, D. C. Jupiter, and J. M. Menezes, “Updating the epidemiology of cleft lip with or without cleft palate,” Plast. Reconstr. Surg., vol. 129, no. 3, pp. 511–518, 2012. [CrossRef]
- P. Pastuszak, I. Dunin-Wilczyńska, and A. Lasota, “Frequency of additional congenital dental anomalies in children with cleft lip, alveolar and palate,” J. Clin. Med., vol. 9, no. 12, pp. 1–10, 2020. [CrossRef]
- P. Stanier and G. E. Moore, “Genetics of cleft lip and palate: Syndromic genes contribute to the incidence of non-syndromic clefts,” Hum. Mol. Genet., vol. 13, no. REV. ISS. 1, pp. 73–81, 2004. [CrossRef]
- M. Vaivads, E. Balode, and M. Pilmane, “Factors affecting facial development and formation of cleft lip and palate: a literature review,” Pap. Anthropol., vol. 29, no. 2, pp. 22–35, 2020. [CrossRef]
- E. W. Harville, A. J. Wilcox, R. T. Lie, H. Vindenes, and F. Åbyholm, “Cleft lip and palate versus cleft lip only: Are they distinct defects?,” Am. J. Epidemiol., vol. 162, no. 5, pp. 448–453, 2005. [CrossRef]
- M. Kuriyama et al., “DNA methylation changes during cleft palate formation induced by retinoic acid in mice,” Cleft Palate-Craniofacial J., vol. 45, no. 5, pp. 545–551, 2008. [CrossRef]
- U. Radhakrishna, “Small players with a big role: MicroRNAs in pathophysiology of cleft lip and palate,” Indian J. Hum. Genet., vol. 18, no. 3, pp. 272–273, 2012. [CrossRef]
- M. Habibi and S. Vahdat, “Evaluation of the Correlation between Socioeconomic Factors and Pediatric Cleft Lip and Palate,” Mod. Med. Lab. J., vol. 4, no. 2, pp. 40–49, 2021. [CrossRef]
- J. C. Murray, “Gene/environment causes of cleft lip and/or palate,” Clin. Genet., vol. 61, no. 4, pp. 248–256, 2002. [CrossRef]
- D. Arguello and P. D. H. B. L. M. M. G. E.-L. M. , Kali S. Thomas, “ HHS Public Access,” Physiol. Behav., vol. 176, no. 1, pp. 139–148, 2017. [CrossRef]
- C. Cao, X. Xu, Q. Zheng, B. Shi, J. Li, and Y. Wang, “Growth and Development of Craniofacial Structures in Patients at Different Ages With Unrepaired Submucous Cleft Palate,” J. Oral Maxillofac. Surg., vol. 76, no. 11, pp. 2388–2397, 2018. [CrossRef]
- A. C. Allori, J. B. Mulliken, J. G. Meara, S. Shusterman, and J. R. Marcus, “Classification of cleft lip/palate: Then and now,” Cleft Palate-Craniofacial J., vol. 54, no. 2, pp. 175–188, 2017. [CrossRef]
- R. L. Strawderman, “Model selection and inference: A practical information-theoretic approach by Kenneth P. Burnham; David R. Anderson,” J. Am. Stat. Assoc., vol. 95, no. 449, p. 341, 2014.
- E. M. Baas, F. Bierenbroodspot, and J. De Lange, “Bilateral sagittal split osteotomy versus distraction osteogenesis of the mandible: A randomized clinical trial,” Int. J. Oral Maxillofac. Surg., vol. 44, no. 2, pp. 180–188, 2015. [CrossRef]
- M. L. Worley, K. G. Patel, and L. A. Kilpatrick, “Cleft Lip and Palate,” Clin. Perinatol., vol. 45, no. 4, pp. 661–678, 2018. [CrossRef]
- C. Ferrari-piloni, L. A. N. Barros, F. A. S. Jesuíno, and J. Valladares-neto, “Prevalence of cleft lip and palate and associated factors in Brazil’s Midwest: a single-center study,” Braz. Oral Res., vol. 35, pp. 1–9, 2021. [CrossRef]
- E. Berg, R. T. Lie, A. Sivertsen, and Ø. A. Haaland, “Parental age and the risk of isolated cleft lip: A registry-based study,” Ann. Epidemiol., vol. 25, no. 12, pp. 942-947.e1, 2015. [CrossRef]
- F. P. Kapos, L. A. White, K. A. Schmidt, S. E. Hawes, and J. R. Starr, “Risk of non-syndromic orofacial clefts by maternal rural-urban residence and race/ethnicity: A population-based case-control study in Washington State 1989-2014,” Paediatr. Perinat. Epidemiol., vol. 35, no. 3, pp. 292–301, 2021. [CrossRef]
- H. P. V. da Silva et al., “Risk factors and comorbidities in Brazilian patients with orofacial clefts,” Braz. Oral Res., vol. 32, pp. 1–12, 2018. [CrossRef]
- A. Kozma, “Gestational Diabetes Mellitus and the Development of Cleft Lip / Palate in Newborns,” Acta Endocrinol., vol. 15, no. 1, pp. 118–122, 2019. [CrossRef]
- C. M. McKinney, B. Chowchuen, W. Pitiphat, T. DeRouen, A. Pisek, and K. Godfrey, “Micronutrients and Oral Clefts: A Case-Control Study,” J. Dent. Res., vol. 92, no. 12, pp. 1089–1094, 2013. [CrossRef]
- W. Ni, T. Tian, L. Zhang, Z. Li, L. Wang, and A. Ren, “Maternal periconceptional consumption of sprouted potato and risks of neural tube defects and orofacial clefts,” Nutr. J., vol. 17, no. 1, pp. 19–23, 2018. [CrossRef]
- S. L. Carmichael, S. Tinker, S. A. Rasmussen, and G. M. Shaw, “Babies With Structural Birth Defects,” vol. 28, no. 4, pp. 338–344, 2015. [CrossRef]
- M. M. n, Eunsung Mouradian, “ NIH Public Access,” Bone, vol. 23, no. 1, pp. 1–7, 2008. [CrossRef]
- L. A. M. Welberg, K. V. Thrivikraman, and P. M. Plotsky, “Chronic maternal stress inhibits the capacity to up-regulate placental 11β-hydroxysteroid dehydrogenase type 2 activity,” J. Endocrinol., vol. 186, no. 3, pp. 7–12, 2005. [CrossRef]
- R. C. Andrews and B. R. Walker, “<Clin Sci 1999 Andrews-1.pdf>,” vol. 523, pp. 513–523, 1999.
- T. Yoneda and R. M. Pratt, “Vitamin B6 reduces cortisone-induced cleft palate in the mouse,” Teratology, vol. 26, no. 3, pp. 255–258, 1982. [CrossRef]
- J. Weingärtner, K. Lotz, J. Fanghänel, T. Gedrange, V. Bienengräber, and P. Proff, “Induktion und Prävention von Lippen-Kiefer-Gaumen-Segel-Spalten und Neuralrohrdefekten unter besonderer Berücksichtigung der B-Vitamine und des Methylierungszyklus,” J. Orofac. Orthop., vol. 68, no. 4, pp. 266–277, 2007. [CrossRef]
- A. Jahanbin, E. Shadkam, H. H. Miri, A. S. Shirazi, and M. Abtahi, “Maternal folic acid supplementation and the risk of oral clefts in offspring,” J. Craniofac. Surg., vol. 29, no. 6, pp. e534–e541, 2018. [CrossRef]
- M. C. Johnston and P. T. Bronsky, “Prenatal craniofacial development: New insights on normal and abnormal mechanisms,” Crit. Rev. Oral Biol. Med., vol. 6, no. 4, pp. 368–422, 1995. [CrossRef]
- Y. Sato et al., “Population attributable fractions of modifiable risk factors for nonsyndromic orofacial clefts: A prospective cohort study from the Japan environment and children’s study,” J. Epidemiol., vol. 31, no. 4, pp. 272–279, 2021. [CrossRef]
- A. J. Agopian et al., “Maternal occupational physical activity and risk for orofacial clefts,” Am. J. Ind. Med., vol. 60, no. 7, pp. 627–634, 2017. [CrossRef]
- R. Yadav, U. Verma, R. Tiwari, and O. Article, “Heterogeneous conceptualization of etiopathogenesis: Oral pyogenic granuloma,” Natl. J. Maxillofac. Surg., vol. 10, no. 1, pp. 3–7, 2019. [CrossRef]
- L. L. Moore, M. R. Singer, M. L. Bradlee, K. J. Rothman, and A. Milunsky, “A prospective study of the risk of congenital defects associated with maternal obesity and diabetes mellitus,” Epidemiology, vol. 11, no. 6, pp. 689–694, 2000. [CrossRef]
- S. V. Spilson, H. J. E. Kim, and K. C. Chung, “Association between maternal diabetes mellitus and newborn oral cleft,” Ann. Plast. Surg., vol. 47, no. 5, pp. 477–481, 2001. [CrossRef]
- A. Åberg, L. Westbom, and B. Källén, “Congenital malformations among infants whose mothers had gestational diabetes or preexisting diabetes,” Early Hum. Dev., vol. 61, no. 2, pp. 85–95, 2001. [CrossRef]
- T. Rosenthal and S. Oparil, “The effect of antihypertensive drugs on the fetus,” J. Hum. Hypertens., vol. 16, no. 5, pp. 293–298, 2002. [CrossRef]
- D. P. Xu, W. D. Qu, C. Sun, R. Y. Cao, D. W. Liu, and P. G. Du, “A Study on Environmental Factors for Nonsyndromic Cleft Lip and/or Palate,” J. Craniofac. Surg., vol. 29, no. 2, pp. 364–367, 2018. [CrossRef]
- A. Soim et al., “A population-based case–control study of the association between weather-related extreme heat events and orofacial clefts,” Birth Defects Res., vol. 110, no. 19, pp. 1468–1477, 2018. [CrossRef]
- B. Cheshmi, Z. Jafari, M. A. Naseri, and H. A. Davari, “Assessment of the correlation between various risk factors and orofacial cleft disorder spectrum: a retrospective case-control study,” Maxillofac. Plast. Reconstr. Surg., vol. 42, no. 1, 2020. [CrossRef]
- F. Bánhidy, E. H. Puhó, and A. E. Czeizel, “Efficacy of medical care of epileptic pregnant women based on the rate of congenital abnormalities in their offspring,” Congenit. Anom. (Kyoto)., vol. 51, no. 1, pp. 34–42, 2011. [CrossRef]
- R. J. Boyle, “Effects of certain prenatal drugs on the fetus and newborn.,” Pediatr. Rev., vol. 23, no. 1, pp. 17–24, 2002. [CrossRef]
- E. C. Ailes et al., “Association between antibiotic use among pregnant women with urinary tract infections in the first trimester and birth defects, National Birth Defects Prevention Study 1997 to 2011,” Birth Defects Res. Part A - Clin. Mol. Teratol., vol. 106, no. 11, pp. 940–949, 2016. [CrossRef]
- W. E. Benitz, “Antibacterial Medication Use During Pregnancy and Risk of Birth Defects: National Birth Defects Prevention Study,” Yearb. Neonatal Perinat. Med., vol. 2010, pp. 1–2, 2010. [CrossRef]
- K. J. Lin, A. A. Mitchell, W. P. Yau, C. Louik, and S. Hernández-Díaz, “Maternal exposure to amoxicillin and the risk of oral clefts,” Epidemiology, vol. 23, no. 5, pp. 699–705, 2012. [CrossRef]
- P. Pradat et al., “First Trimester Exposure to Corticosteroids and Oral Clefts,” Birth Defects Res. Part A - Clin. Mol. Teratol., vol. 67, no. 12, pp. 968–970, 2003. [CrossRef]
- R. Gitau, A. Cameron, N. M. Fisk, and V. Glover, “Fetal exposure to maternal cortisol,” Lancet, vol. 352, no. 9129, pp. 707–708, 1998. [CrossRef]
- C. C. Chi, S. H. Wang, G. Kirtschig, and F. Wojnarowska, “Systematic review of the safety of topical corticosteroids in pregnancy,” J. Am. Acad. Dermatol., vol. 62, no. 4, pp. 694–705, 2010. [CrossRef]
- A. V. Margulis et al., “Use of topiramate in pregnancy and risk of oral clefts,” Am. J. Obstet. Gynecol., vol. 207, no. 5, pp. 405.e1-405.e7, 2012. [CrossRef]
- K. L. Benninger et al., “Prenatal Exposures Are Associated With Worse Neurodevelopmental Outcomes in Infants With Neonatal Opioid Withdrawal Syndrome,” Front. Pediatr., vol. 8, no. August, pp. 1–10, 2020. [CrossRef]
- M. Fell, K. Dack, S. Chummun, J. Sandy, Y. Wren, and S. Lewis, “Maternal Cigarette Smoking and Cleft Lip and Palate: A Systematic Review and Meta-Analysis,” Cleft Palate-Craniofacial J., vol. 59, no. 9, pp. 1185–1200, 2022. [CrossRef]
- S. Lieff, A. F. Olshan, M. Werler, R. P. Strauss, J. Smith, and A. Mitchell, “Maternal cigarette smoking during pregnancy and risk of oral clefts in newborns,” Am. J. Epidemiol., vol. 150, no. 7, pp. 683–694, 1999. [CrossRef]
- J. C. Bell, C. Raynes-Greenow, R. M. Turner, C. Bower, N. Nassar, and C. M. O’Leary, “Maternal alcohol consumption during pregnancy and the risk of orofacial clefts in Infants: A Systematic Review and Meta-Analysis,” Paediatr. Perinat. Epidemiol., vol. 28, no. 4, pp. 322–332, 2014. [CrossRef]
- R. Molina-Solana, R. M. Yáñez-Vico, A. Iglesias-Linares, A. Mendoza-Mendoza, and E. Solano-Reina, “Current concepts on the effect of environmental factors on cleft lip and palate,” Int. J. Oral Maxillofac. Surg., vol. 42, no. 2, pp. 177–184, 2013. [CrossRef]
- D. O. Danis, K. Bachrach, J. Piraquive, A. P. Marston, and J. R. Levi, “Cleft Lip and Palate in Newborns Diagnosed With Neonatal Abstinence Syndrome,” Otolaryngol. - Head Neck Surg. (United States), vol. 164, no. 1, pp. 199–205, 2021. [CrossRef]
- A. M. Inchingolo et al., “Modifiable Risk Factors of Non-Syndromic Orofacial Clefts: A Systematic Review,” Children, vol. 9, no. 12, pp. 1–24, 2022. [CrossRef]
| Name of gene | Symbol |
|---|---|
| Transforming growth factor - alpha | TGFA |
| Transforming growth factor - 133 | TGF 133?? |
| Methylene tetrahydrofolate Reductase | MTHFR |
| - | - |
| Endothelin - 1 | ET1 |
| BCL3 Transcription Coactivator | BCL3 |
| Retinoic acid receptor alpha | RARA |
| MSX1-Msh Homeobox 1 | MSX-1 |
| Syndromes | Name of gene | Symbol |
|---|---|---|
| Waardenburg syndrome, type II A | Microphtalmia - Associated Transcription Factor | MITF |
| Di George syndrome | Di George syndrome chromosome region | CATCH 22 |
| Treacher Collins syndrome mandibulofacial dysostosis | Treacle Ribosome Biogenesis Factor 1 RNA Polymerase I and III Subunit C RNA Polymerase I and III Subunit D RNA Polymerase I Subunit B |
TCOF1, POLR1C, POLR1D, POLR1B |
| Van der Woude syndrome | Interferon Regulatory Factor – 6 | IRF 6 |
| CLP-Ectodermal dysplasia syndrome?? | Poliovirus receptor related-1 | PVRL1 |
| Ectrodactyly, ectodermal dysplasia orofacial cleft syndrome?? Pigment Anomaly-Ectrodactyly-Hypodontia Syndrome |
Tumor Protein P63 | TP63 |
| Zollinger syndrome-3 ?? Zellweger Syndrome | Peroxisomal Biogenesis Factor 2 | (PXMP3) PEX2 |
| Diastrophic dysplasia | Diastrophic dysplasia sulfate transporter | DTDST |
| Gorlin syndrome (Basal cell nevus syndrome 1) | Patched 1 | PTCH1 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




