Submitted:
05 February 2024
Posted:
06 February 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Animal Models
2.2. Tissue Dissociation into Single-Cell Suspension
2.3. Single-Cell RNA Sequencing Data Processing
2.4. Cluster Identification and Annotation
2.5. Pathway Enrichment Analysis
2.6. Trajectory Analysis
2.7. Cell–Cell Communication and Receptor–Ligand Interaction Analysis
2.8. TUNEL Staining
2.9. Flow Cytometric Analysis
2.10. Statistical Analysis
3. Results
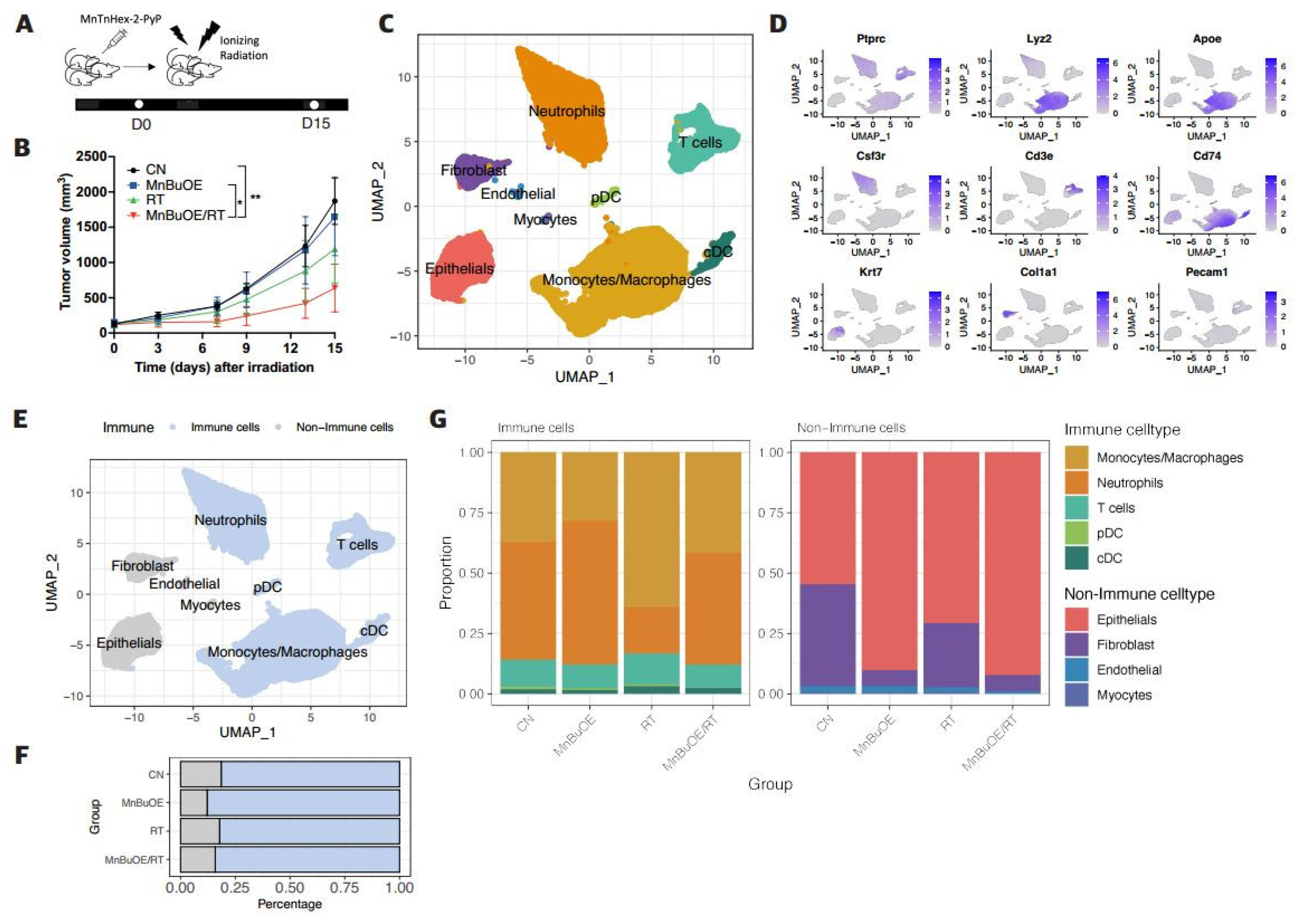
3.1. Effect of MnBuOE Coupled with Irradiation and Major Single-Cell Mapping in the 4T1 Tumor Mouse Model
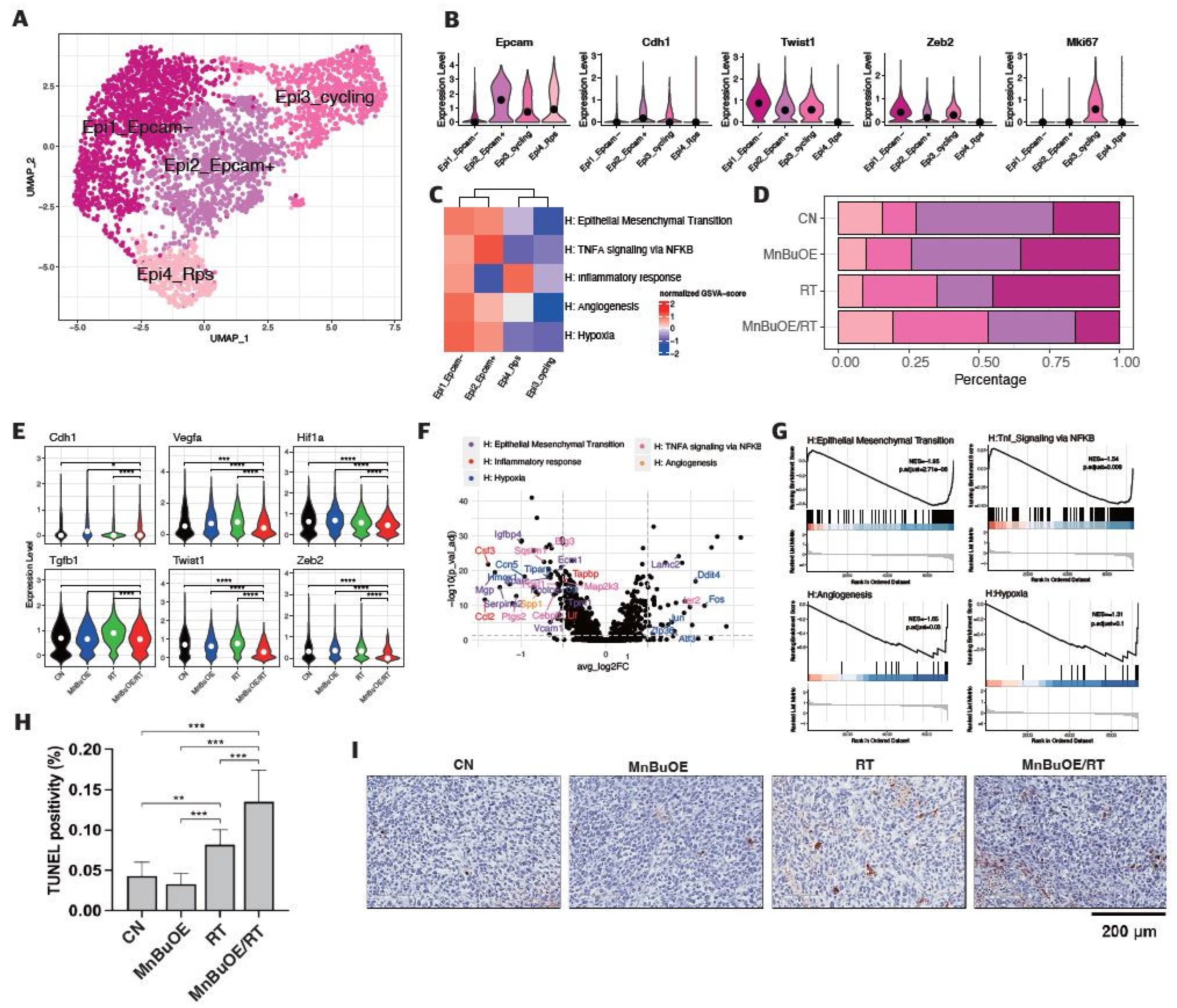
3.2. Epithelial Cell Clustering and Subtype Analysis of the 4T1 Tumor Treated with MnBuOE Coupled with Irradiation
3.3. Fibroblasts Clustering and Subtype Analysis of the 4T1 Tumor Treated with MnBuOE Coupled with Irradiation
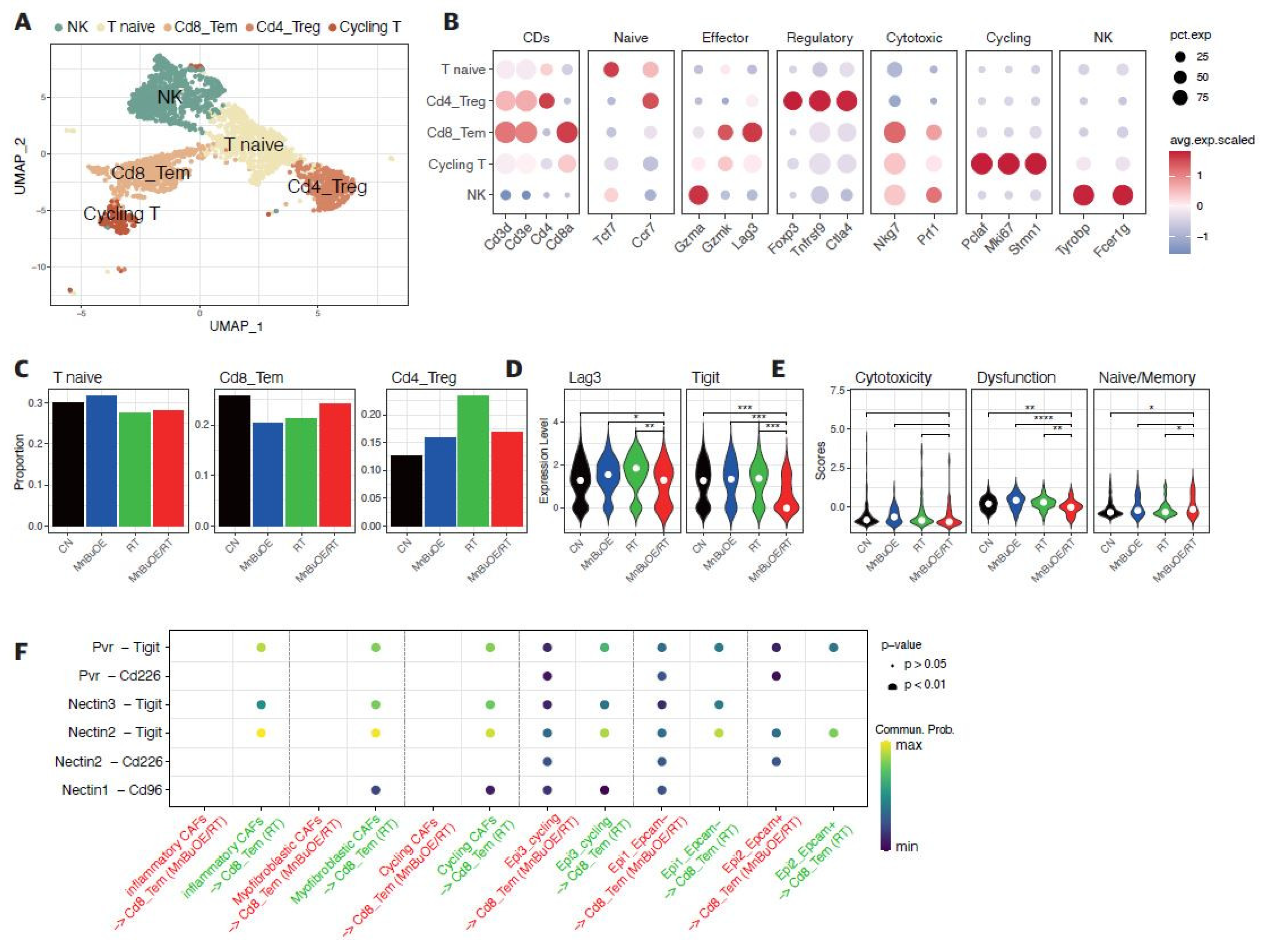
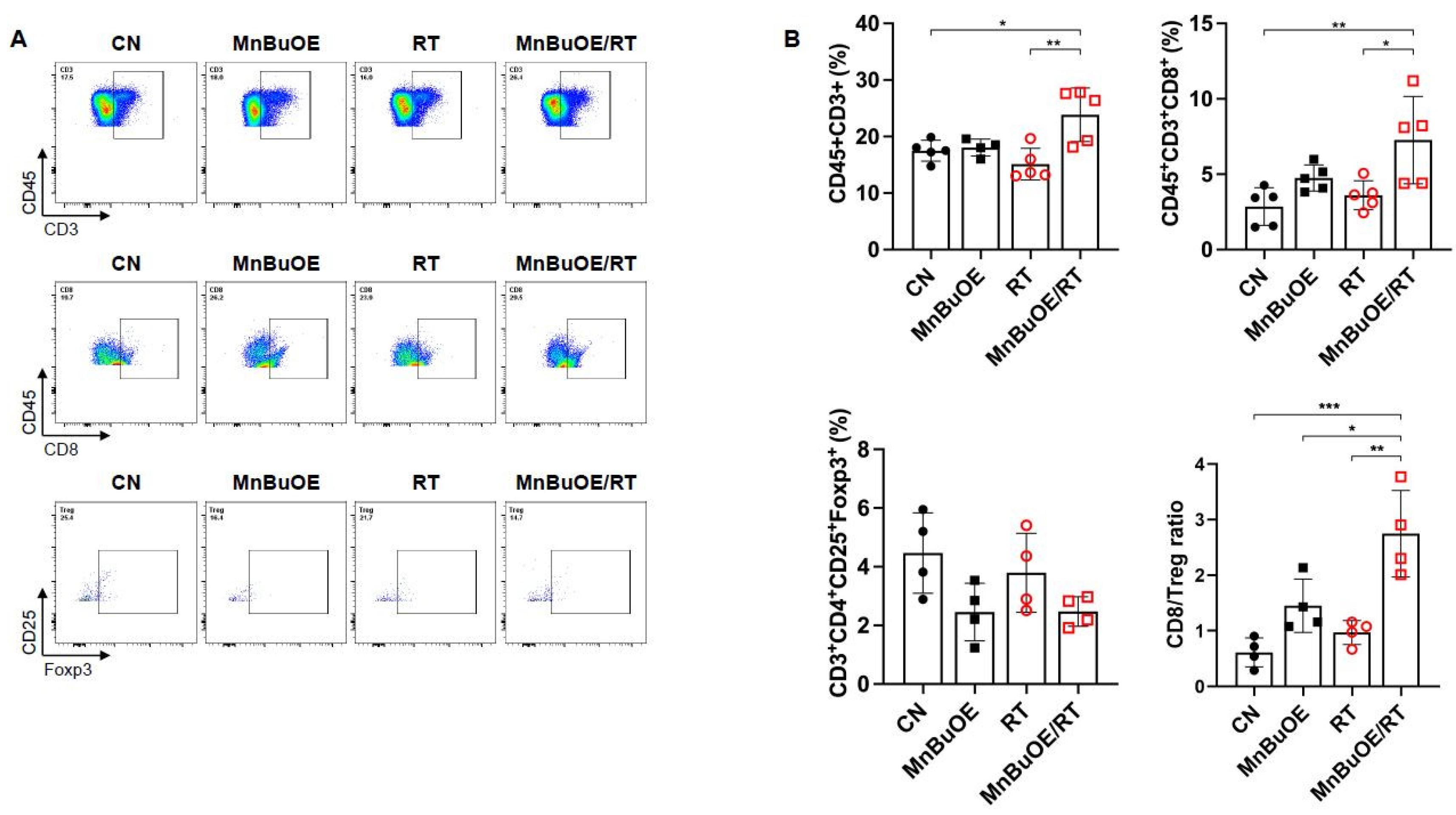
3.4. T Cells Clustering and Subtype Analysis of the 4T1 Tumor Treated with MnBuOE Coupled with Irradiation
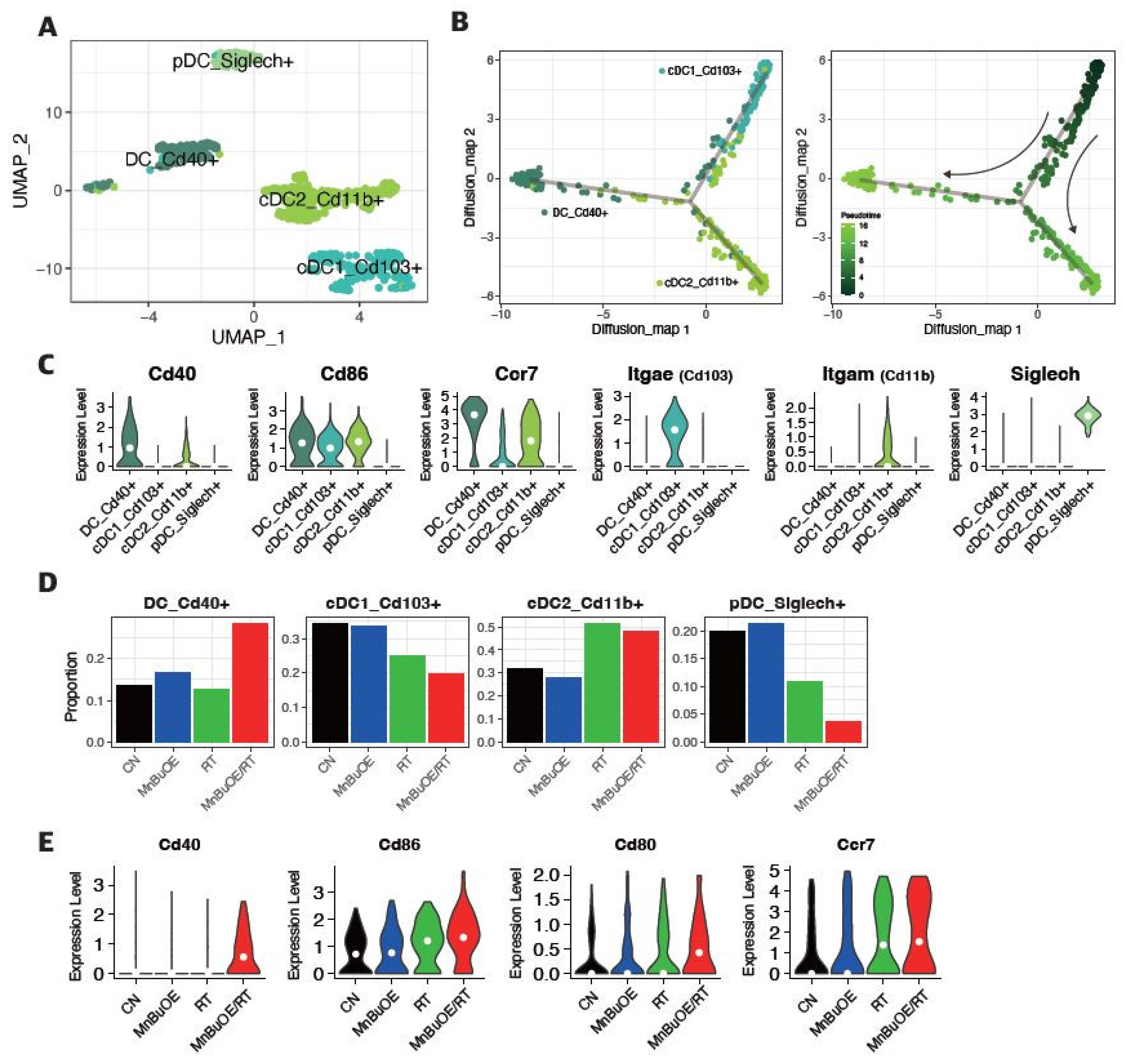
3.5. DC Clustering and Pseudotime Trajectory Analysis of the 4T1 Tumor Treated with MnBuOE Coupled with Irradiation
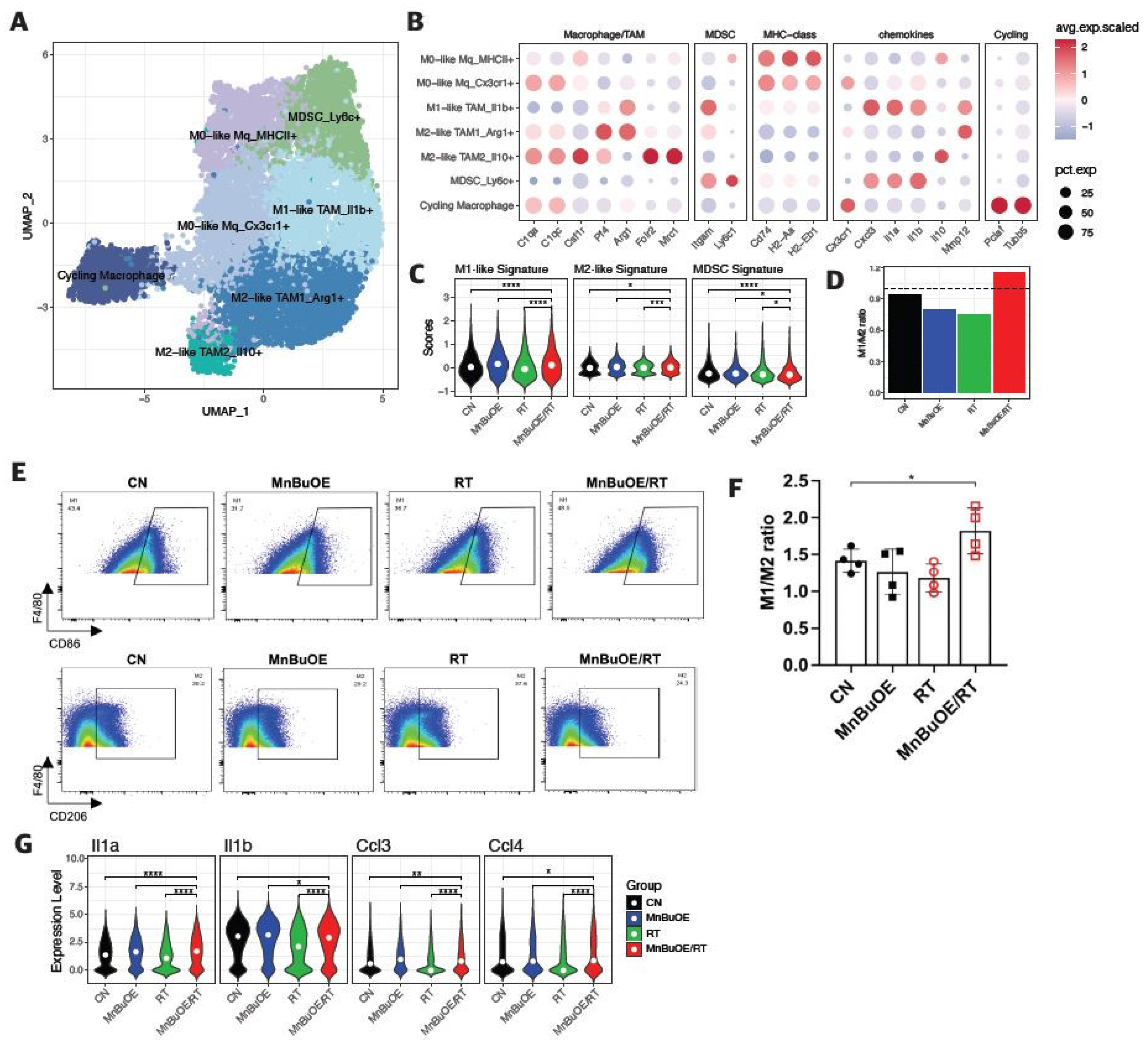
3.6. Macrophage Clustering and Phenotype Analysis of the 4T1 Tumor Treated with MnBuOE Coupled with Irradiation
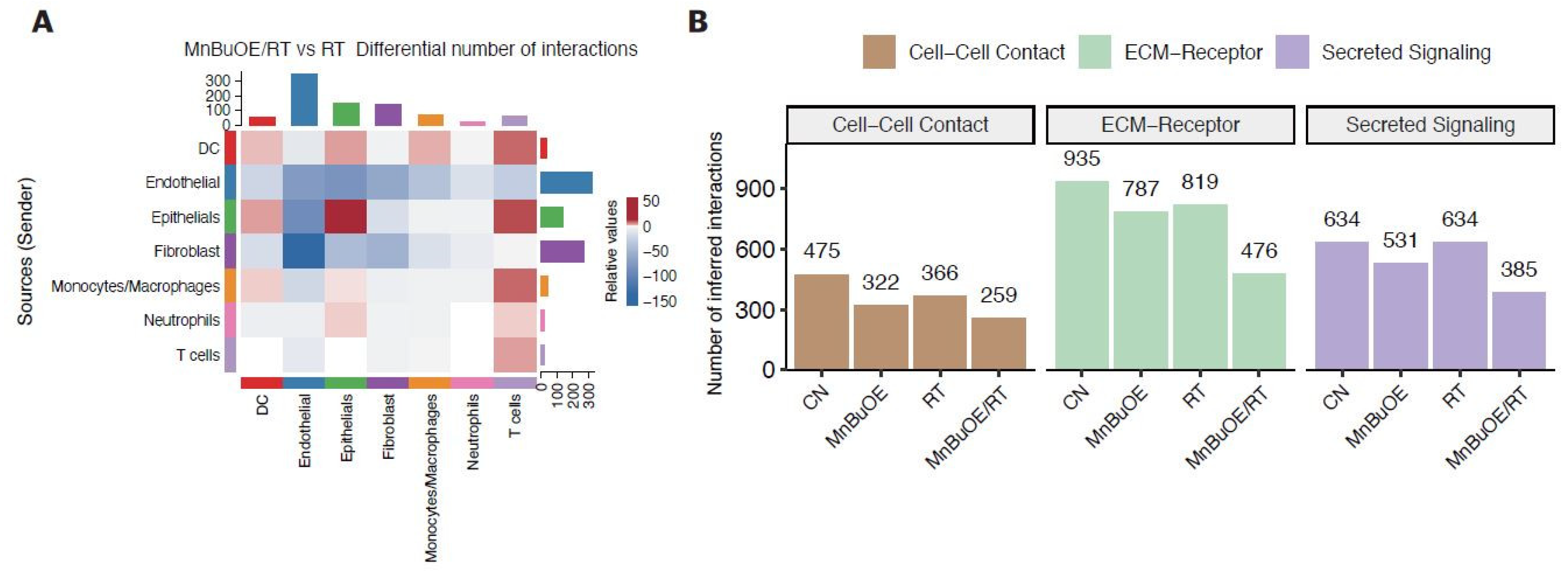
3.7. Intercellular Communications within TME Regulated by MnBuOE Coupled with Irradiation in the 4T1 Tumor Mice Model
4. Discussion
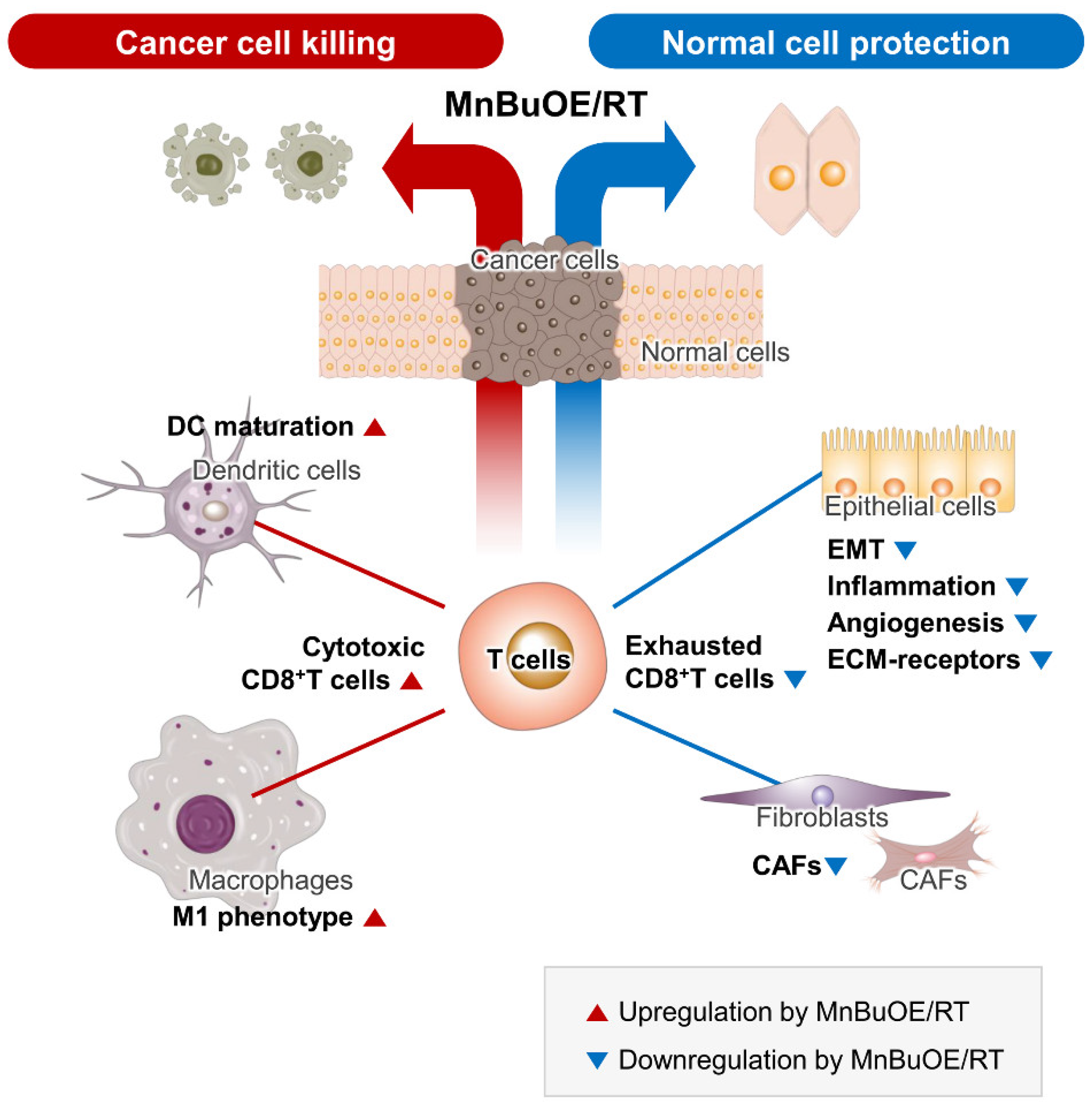
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- D.G. Franchina; C. Dostert; D. Brenner. Reactive Oxygen Species: Involvement in T Cell Signaling and Metabolism. Trends Immunol. 2018, 39, 489-502. [CrossRef]
- X. Chen; M. Song; B. Zhang; Y. Zhang. Reactive Oxygen Species Regulate T Cell Immune Response in the Tumor Microenvironment. Oxid Med Cell Longev. 2016, 2016, 1580967. [CrossRef]
- E.L. Yarosz; C.H. Chang. The Role of Reactive Oxygen Species in Regulating T Cell-mediated Immunity and Disease. Immune Netw. 2018, 18, e14. [CrossRef]
- S.Y. Lee; E.K. Jeong; M.K. Ju; H.M. Jeon; M.Y. Kim; C.H. Kim; H.G. Park; S.I. Han; H.S. Kang. Induction of metastasis, cancer stem cell phenotype, and oncogenic metabolism in cancer cells by ionizing radiation. Molecular Cancer 2017, 16, 10. [CrossRef]
- I. Batinic-Haberle; A. Tovmasyan; Z. Huang; W. Duan; L. Du; S. Siamakpour-Reihani; Z. Cao; H. Sheng; I. Spasojevic; A. Alvarez Secord. H(2)O(2)-Driven Anticancer Activity of Mn Porphyrins and the Underlying Molecular Pathways. Oxid Med Cell Longev. 2021, 2021, 6653790. [CrossRef]
- I. Batinic-Haberle; A. Tovmasyan; I. Spasojevic. Mn Porphyrin-Based Redox-Active Drugs: Differential Effects as Cancer Therapeutics and Protectors of Normal Tissue Against Oxidative Injury. Antioxid Redox Signal. 2018, 29, 1691-1724. [CrossRef]
- I. Batinic-Haberle; M.E. Tome. Thiol regulation by Mn porphyrins, commonly known as SOD mimics. Redox Biol. 2019, 25, 101139. [CrossRef]
- S.R. Birer; C.T. Lee; K.R. Choudhury; K.H. Young; I. Spasojevic; I. Batinic-Haberle; J.D. Crapo; M.W. Dewhirst; K.A. Ashcraft. Inhibition of the Continuum of Radiation-Induced Normal Tissue Injury by a Redox-Active Mn Porphyrin. Radiat Res. 2017, 188, 94-104. [CrossRef]
- Y. Yulyana; A. Tovmasyan; I.A. Ho; K.C. Sia; J.P. Newman; W.H. Ng; C.M. Guo; K.M. Hui; I. Batinic-Haberle; P.Y. Lam. Redox-Active Mn Porphyrin-based Potent SOD Mimic, MnTnBuOE-2-PyP(5+), Enhances Carbenoxolone-Mediated TRAIL-Induced Apoptosis in Glioblastoma Multiforme. Stem Cell Rev Rep. 2016, 12, 140-55. [CrossRef]
- K.A. Ashcraft; M.K. Boss; A. Tovmasyan; K. Roy Choudhury; A.N. Fontanella; K.H. Young; G.M. Palmer; S.R. Birer; C.D. Landon; W. Park; S.K. Das; T. Weitner; H. Sheng; D.S. Warner; D.M. Brizel; I. Spasojevic; I. Batinic-Haberle; M.W. Dewhirst. Novel Manganese-Porphyrin Superoxide Dismutase-Mimetic Widens the Therapeutic Margin in a Preclinical Head and Neck Cancer Model. Int J Radiat Oncol Biol Phys. 2015, 93, 892-900. [CrossRef]
- A. Flórido; N. Saraiva; S. Cerqueira; N. Almeida; M. Parsons; I. Batinic-Haberle; J.P. Miranda; J.G. Costa; G. Carrara; M. Castro; N.G. Oliveira; A.S. Fernandes. The manganese(III) porphyrin MnTnHex-2-PyP(5+) modulates intracellular ROS and breast cancer cell migration: Impact on doxorubicin-treated cells. Redox Biol. 2019, 20, 367-378. [CrossRef]
- M.K. Boss; R.E. Oberley-Deegan; I. Batinic-Haberle; G.A. Talmon; J.A. Somarelli; S. Xu; E.A. Kosmacek; B. Griess; S. Mir; S. Shrishrimal; M. Teoh-Fitzgerald; I. Spasojevic; M.W. Dewhirst. Manganese Porphyrin and Radiotherapy Improves Local Tumor Response and Overall Survival in Orthotopic Murine Mammary Carcinoma Models. Radiat Res. 2021, 195, 128-139. [CrossRef]
- A. Chatterjee; Y. Zhu; Q. Tong; E.A. Kosmacek; E.Z. Lichter; R.E. Oberley-Deegan. The Addition of Manganese Porphyrins during Radiation Inhibits Prostate Cancer Growth and Simultaneously Protects Normal Prostate Tissue from Radiation Damage. Antioxidants (Basel) 2018, 7, 21. [CrossRef]
- E.A. Kosmacek; A. Chatterjee; Q. Tong; C. Lin; R.E. Oberley-Deegan. MnTnBuOE-2-PyP protects normal colorectal fibroblasts from radiation damage and simultaneously enhances radio/chemotherapeutic killing of colorectal cancer cells. Oncotarget 2016, 7, 34532-45. [CrossRef]
- Z. Rajic; A. Tovmasyan; O.L. de Santana; I.N. Peixoto; I. Spasojevic; S.A. do Monte; E. Ventura; J.S. Rebouças; I. Batinic-Haberle. Challenges encountered during development of Mn porphyrin-based, potent redox-active drug and superoxide dismutase mimic, MnTnBuOE-2-PyP(5+), and its alkoxyalkyl analogues. J Inorg Biochem. 2017, 169, 50-60. [CrossRef]
- Katherine Peters; Adam Cohen; Nicholas Butowski; John Villano; Joe Mendez; Pierre Giglio; Tresa McGranahan; Chi Zhang; Jacob Smeltzer; Shahzad Raza; Burt Nabors; Mina Lobbous; James Herndon; Evan Buckley; David MacLeod; Sara Penchev; David Silberstein; Ines Batinic-Haberle; Ivan Spasojevic; Shayne Gad; David Radoff; Daniel Barboriak; James Crapo. LTBK-09. RESULTS OF BMX-HGG STUDY: A MULTI-INSTITUTIONAL, RANDOMIZED PHASE 2 CLINICAL TRIAL OF CONCURRENT CHEMORADIATION WITH OR WITHOUT BMX-001 IN PATIENTS WITH NEWLY DIAGNOSED HIGH GRADE GLIOMA. Neuro-oncology 2023. [CrossRef]
- S.W. Shin; C. Choi; G.H. Lee; A. Son; S.H. Kim; H.C. Park; I. Batinic-Haberle; W. Park. Mechanism of the Antitumor and Radiosensitizing Effects of a Manganese Porphyrin, MnHex-2-PyP. Antioxid Redox Signal. 2017, 27, 1067-1082. [CrossRef]
- S.W. Shin; C. Choi; H. Kim; Y. Kim; S. Park; S.Y. Kim; I. Batinic-Haberle; W. Park. MnTnHex-2-PyP(5+), Coupled to Radiation, Suppresses Metastasis of 4T1 and MDA-MB-231 Breast Cancer via AKT/Snail/EMT Pathways. Antioxidants (Basel) 2021, 10, 1769. [CrossRef]
- S. Shrishrimal; A. Chatterjee; E.A. Kosmacek; P.J. Davis; J.T. McDonald; R.E. Oberley-Deegan. Manganese porphyrin, MnTE-2-PyP, treatment protects the prostate from radiation-induced fibrosis (RIF) by activating the NRF2 signaling pathway and enhancing SOD2 and sirtuin activity. Free Radic Biol Med. 2020, 152, 255-270. [CrossRef]
- O.M. Ozpiskin; L. Zhang; J.J. Li. Immune targets in the tumor microenvironment treated by radiotherapy. Theranostics 2019, 9, 1215-1231. [CrossRef]
- E. Lo Presti; F. Dieli; S. Meraviglia. Tumor-Infiltrating γδ T Lymphocytes: Pathogenic Role, Clinical Significance, and Differential Programing in the Tumor Microenvironment. Front Immunol. 2014, 5, 607. [CrossRef]
- Y. Jiang; Y. Li; B. Zhu. T-cell exhaustion in the tumor microenvironment. Cell Death Dis. 2015, 6, e1792. [CrossRef]
- S. Brassart-Pasco; S. Brézillon; B. Brassart; L. Ramont; J.B. Oudart; J.C. Monboisse. Tumor Microenvironment: Extracellular Matrix Alterations Influence Tumor Progression. Front Oncol. 2020, 10, 397. [CrossRef]
- M.B. Giorello; F.R. Borzone; V. Labovsky; F.V. Piccioni; N.A. Chasseing. Cancer-Associated Fibroblasts in the Breast Tumor Microenvironment. J Mammary Gland Biol Neoplasia 2021, 26, 135-155. [CrossRef]
- M.L. Suvà; I. Tirosh. Single-Cell RNA Sequencing in Cancer: Lessons Learned and Emerging Challenges. Molecular Cell 2019, 75, 7-12. [CrossRef]
- J.J. Quinn; M.G. Jones; R.A. Okimoto; S. Nanjo; M.M. Chan; N. Yosef; T.G. Bivona; J.S. Weissman. Single-cell lineages reveal the rates, routes, and drivers of metastasis in cancer xenografts. Science 2021, 371, eabc1944. [CrossRef]
- Y. Hao; S. Hao; E. Andersen-Nissen; W.M. Mauck 3rd; S. Zheng; A. Butler; M.J. Lee; A.J. Wilk; C. Darby; M. Zager; P. Hoffman; M. Stoeckius; E. Papalexi; E.P. Mimitou; J. Jain; A. Srivastava; T. Stuart; L.M. Fleming; B. Yeung; A.J. Rogers; J.M. McElrath; C.A. Blish; R. Gottardo; P. Smibert; R. Satija. Integrated analysis of multimodal single-cell data. Cell 2021, 184, 3573-3587.e29.
- G. Finak; A. McDavid; M. Yajima; J. Deng; V. Gersuk; A.K. Shalek; C.K. Slichter; H.W. Miller; M.J. McElrath; M. Prlic; P.S. Linsley; R. Gottardo. MAST: a flexible statistical framework for assessing transcriptional changes and characterizing heterogeneity in single-cell RNA sequencing data. Genome Biol. 2015, 16, 278. [CrossRef]
- G. Korotkevich; V. Sukhov; N. Budin; B. Shpak; M.N. Artyomov; A. Sergushichev. Fast gene set enrichment analysis. bioRxiv. 2021. [CrossRef]
- X. Qiu; A. Hill; J. Packer; D. Lin; Y.A. Ma; C. Trapnell. Single-cell mRNA quantification and differential analysis with Census. Nat Methods 2017, 14, 309-315. [CrossRef]
- S. Jin; C.F. Guerrero-Juarez; L. Zhang; I. Chang; R. Ramos; C.H. Kuan; P. Myung; M.V. Plikus; Q. Nie. Inference and analysis of cell-cell communication using CellChat. Nat Commun. 2021, 12, 1088. [CrossRef]
- W. Chung; H.H. Eum; H.O. Lee; K.M. Lee; H.B. Lee; K.T. Kim; H.S. Ryu; S. Kim; J.E. Lee; Y.H. Park; Z. Kan; W. Han; W.Y. Park. Single-cell RNA-seq enables comprehensive tumour and immune cell profiling in primary breast cancer. Nat Commun. 2017, 8, 15081. [CrossRef]
- D. Lavie; A. Ben-Shmuel; N. Erez; R. Scherz-Shouval. Cancer-associated fibroblasts in the single-cell era. Nat Cancer 2022, 3, 793-807. [CrossRef]
- F. Wu; J. Yang; J. Liu; Y. Wang; J. Mu; Q. Zeng; S. Deng; H. Zhou. Signaling pathways in cancer-associated fibroblasts and targeted therapy for cancer. Signal Transduct Target Ther. 2021, 6, 218. [CrossRef]
- J. Winkler; A. Abisoye-Ogunniyan; K.J. Metcalf; Z. Werb. Concepts of extracellular matrix remodelling in tumour progression and metastasis. Nat Commun. 2020, 11, 5120. [CrossRef]
- A.T. Baker; M.H. Abuwarwar; L. Poly; S. Wilkins; A.L. Fletcher. Cancer-Associated Fibroblasts and T Cells: From Mechanisms to Outcomes. J Immunol. 2021, 206, 310-320. [CrossRef]
- A.M. van der Leun; D.S. Thommen; T.N. Schumacher. CD8(+) T cell states in human cancer: insights from single-cell analysis. Nat Rev Cancer 2020, 20, 218-232. [CrossRef]
- K.E. Pauken; E.J. Wherry. TIGIT and CD226: tipping the balance between costimulatory and coinhibitory molecules to augment the cancer immunotherapy toolkit. Cancer Cell 2014, 26, 785-787. [CrossRef]
- E.Y. Chiang; I. Mellman. TIGIT-CD226-PVR axis: advancing immune checkpoint blockade for cancer immunotherapy. J Immunother Cancer 2022, 10, e004711. [CrossRef]
- J. Yeo; M. Ko; D.H. Lee; Y. Park; H.S. Jin. TIGIT/CD226 Axis Regulates Anti-Tumor Immunity. Pharmaceuticals (Basel) 2021, 14, 200. [CrossRef]
- A. Gardner; B. Ruffell. Dendritic Cells and Cancer Immunity. Trends Immunol. 2016, 37, 855-865. [CrossRef]
- T. Hourani; J.A. Holden; W. Li; J.C. Lenzo; S. Hadjigol; N.M. O’Brien-Simpson. Tumor Associated Macrophages: Origin, Recruitment, Phenotypic Diversity, and Targeting. Front Oncol. 2021, 11, 788365. [CrossRef]
- T.D. Ricketts; N. Prieto-Dominguez; P.S. Gowda; E. Ubil. Mechanisms of Macrophage Plasticity in the Tumor Environment: Manipulating Activation State to Improve Outcomes. Front Immunol. 2021, 12, 642285. [CrossRef]
- D.I. Gabrilovich; S. Nagaraj. Myeloid-derived suppressor cells as regulators of the immune system. Nat Rev Immunol. 2009, 9, 162-74. [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).



