Submitted:
11 January 2024
Posted:
12 January 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study design
2.2. Study Population and Data Source
2.3. Clinical Data Collection
2.4. Oral Anticoagulant Eligibility
2.5. Assessment of INR Stability and Quality of Anticoagulation Control
2.6. Ethical Considerations
2.7. Data Analysis
3. Results
3.1. Patients’ characteristics
| Variable | Sub-Variable | N (%) |
|---|---|---|
| Age (Mean ± SD) | 67.43 ± 10.91 | |
| Sex | Male | 276 (42.8) |
| Female | 369 (57.2) | |
| Hypertension | 496 (76.9) | |
| Diabetes Mellitus | 299 (46.4) | |
| Dyslipidemia | 278 (43.1) | |
| Current Smoker | 71 (11.0) | |
| BMI, Mean ± SD | 29.65 ± 5.94 | |
| INR, Mean ± SD | 2.49 ± 1.15 | |
| CHA2DS2VASC score (Mean ± SD) | 3.70 ± 1.66 | |
| HAS BLED score (Mean ± SD) | 1.72 ± 1.16 | |
| First Time of AF Episode | Yes | 127 (19.7) |
| No | 518 (80.3) | |
| Type of AF | Paroxysmal | 135 (20.9) |
| Persistent | 94 (14.6) | |
| Long Standing | 166 (25.7) | |
| Permanent | 250 (38.8) | |
| Enrollment | Outpatient | 500 (77.5) |
| Inpatient | 145 (22.5) | |
| Reason of admission for inpatient | AF | 33 (5.1) |
| CVS | 73 (11.4) | |
| ACS Acute coronary syndrome | 23 (3.6) | |
| Heart failure | 29 (4.5) | |
| CVA | 10 (1.6) | |
| Systemic embolization | 3 (0.5) | |
| Bleeding | 8 (1.2) | |
| Non- Cardiovascular system | 41 (6.4) | |
| Echocardiogram findings | LVEF (Mean ± SD) | 50.95 ± 12.09 |
| Left atrial size (Mean ± SD) | 4.51 ± 0.81 | |
| Left ventricular hypertrophy | 247 (38.3) | |
| Pulmonary hypertension | 221 (34.4) | |
| Non rheumatic or metallic valve | 499 (77.4) | |
| History of CVA (n=645) | 105 (16.3) | |
| History of recurrent CVA (n=105) | 16 (15.2) | |
| Type of CVA (n=105) | Embolic | 34 (32.4) |
| Thrombotic | 17 (16.2) | |
| Hemorrhagic | 7 (6.7) | |
| Unknown | 47 (44.7) | |
| History of systemic embolization (n=645) | 16 (2.5) | |
| History of recurrent systemic embolization (n=16) | 1 (6.2) | |
| Site of systemic embolization (n=16) | Lower limbs | 9 (56.3) |
| Upper limbs | 2 (12.5) | |
| Mesenteric | 2 (12.5) | |
| Kidneys | 1 (6.25) | |
| Ophthalmic | 1 (6.25) | |
| Unknown site | 1 (6.25) |
| Variable | Sub-Variable | N (%) |
|---|---|---|
| Symptoms related to AF | Palpitation | 267 (41.4) |
| Shortness of breath | 252 (39.1) | |
| Fatigue | 169 (26.2) | |
| Dizziness | 81 (12.6) | |
| Chest pain | 11 (1.7) | |
| Syncope | 7 (1.1) | |
| Asymptomatic | 186 (28.8) | |
| AF related interventions | History of ablation | 5 (0.8) |
| History of occluder device | 3 (0.5) | |
| History of electric cardioversion | 38 (5.9) | |
| History of permanent pacemaker/ICD/CRT | 7 (1.1) | |
| Comorbidities | Congestive heart failure | 145 (22.5) |
| Valvular disease (rheumatic and non-rheumatic) | 107 (16.6) | |
| Cerebrovascular accident (old/new) | 105 (16.3) | |
| Coronary artery disease | 33 (5.1) | |
| Thyroid disease | 69 (10.7) | |
| Chronic kidney disease | 52 (8.1) | |
| Active cancer | 36 (6.6) | |
| Chronic Obstructive Pulmonary disease | 23 (3.6) | |
| Sleep apnea | 17 (2.6) |
| Variable | 1 month (n = 631) |
6 months (n = 607) |
12 months (n = 557) |
total in 12 months |
|---|---|---|---|---|
| Electric cardioversions | 2 | 2 | 3 | 7 |
| Ablations | 1 | 0 | 0 | 1 |
| Occluder device | 1 | 0 | 0 | 1 |
| Permanent pacemaker/ICD/CRT | 0 | 5 | 0 | 5 |
| Remained on warfarin therapy | 600 | 579 | 539 | - |
3.2. Response to warfarin treatment
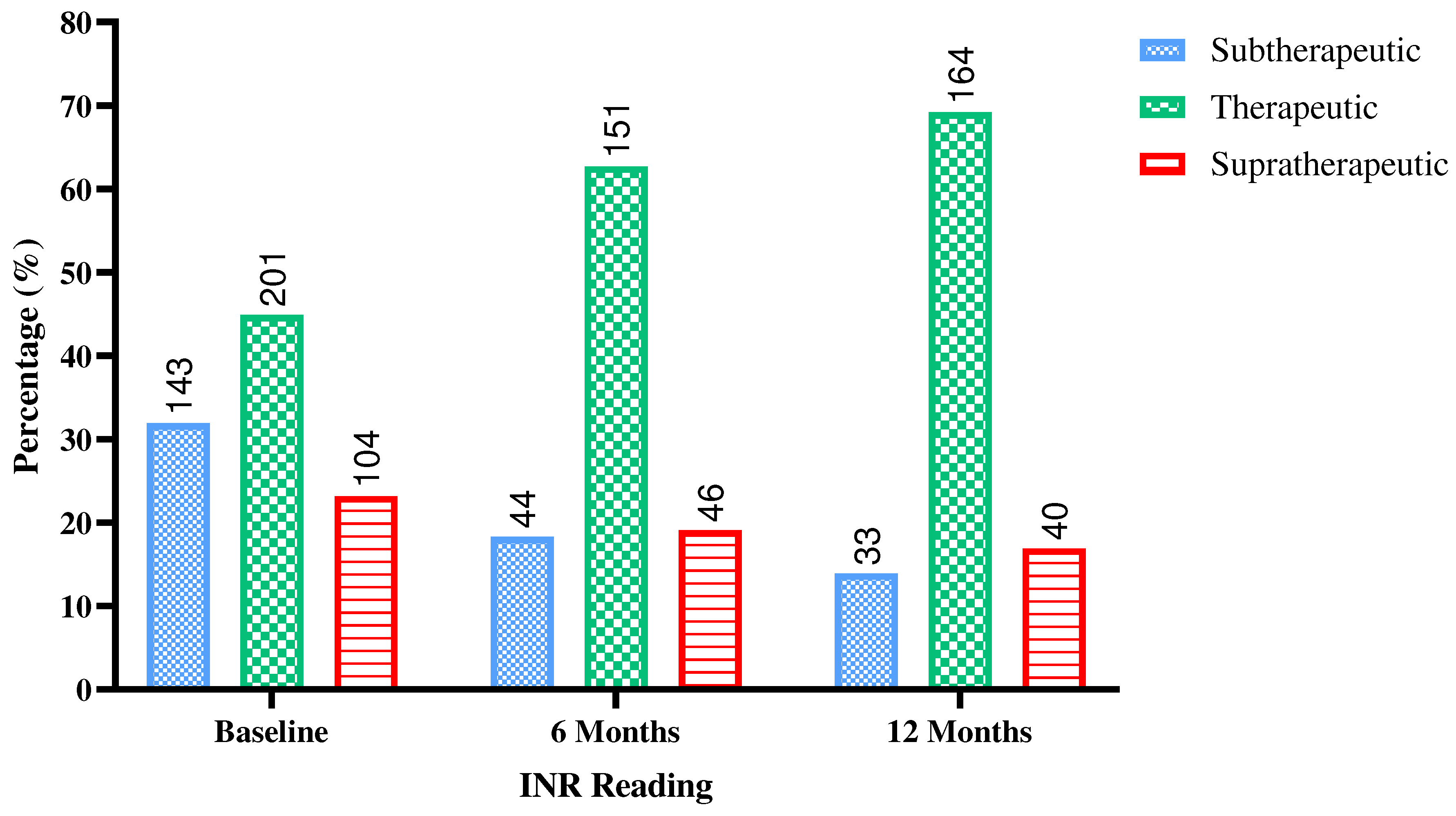
4. Discussion.
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Jonas, D.E.; Kahwati, L.C.; Yun, J.D.Y.; Middleton, J.C.; Coker-Schwimmer, M.; Asher, G.N. Screening for Atrial Fibrillation With Electrocardiography: Evidence Report and Systematic Review for the US Preventive Services Task Force. JAMA 2018, 320, 485–498. [Google Scholar] [CrossRef]
- Heo, R.; Cha, M.-J.; Kim, T.-H.; Lee, J.M.; Park, J.; Park, H.W.; Kang, K.-W.; Shim, J.; Uhm, J.-S.; Kim, J. Characteristics of symptom burden in atrial fibrillation with concomitant heart failure. International Journal of Arrhythmia 2020, 21, 1–8. [Google Scholar] [CrossRef]
- Jones, N.R.; Taylor, C.J.; Hobbs, F.D.R.; Bowman, L.; Casadei, B. Screening for atrial fibrillation: a call for evidence. Eur Heart J 2020, 41, 1075–1085. [Google Scholar] [CrossRef]
- Engdahl, J.; Rosenqvist, M. Large-scale screening studies for atrial fibrillation - is it worth the effort? J Intern Med 2021, 289, 474–492. [Google Scholar] [CrossRef]
- Fitzgerald, P.; Stancampiano, F.; Kurklinsky, A.; Nikpour, N.; McLeod, E.; Li, Z.; Oken, K.; Valery, J. Warfarin therapy in atrial fibrillation: assessment of patient knowledge of risks and benefits. J Community Hosp Intern Med Perspect 2020, 10, 179–187. [Google Scholar] [CrossRef] [PubMed]
- Coleman, C.I.; Costa, O.S.; Brescia, C.W.; Vardar, B.; Abdelgawwad, K.; Sood, N. Thromboembolism, bleeding and vascular death in nonvalvular atrial fibrillation patients with type 2 diabetes receiving rivaroxaban or warfarin. Cardiovasc Diabetol 2021, 20, 52. [Google Scholar] [CrossRef] [PubMed]
- Alshehri, A.M. Stroke in atrial fibrillation: Review of risk stratification and preventive therapy. J Family Community Med 2019, 26, 92–97. [Google Scholar] [CrossRef]
- Chen, A.; Stecker, E.; B, A.W. Direct Oral Anticoagulant Use: A Practical Guide to Common Clinical Challenges. J Am Heart Assoc 2020, 9, e017559. [Google Scholar] [CrossRef] [PubMed]
- Nielsen, P.B.; Larsen, T.B.; Skjoth, F.; Lip, G.Y. Outcomes Associated With Resuming Warfarin Treatment After Hemorrhagic Stroke or Traumatic Intracranial Hemorrhage in Patients With Atrial Fibrillation. JAMA Intern Med 2017, 177, 563–570. [Google Scholar] [CrossRef] [PubMed]
- Wańkowicz, P.; Nowacki, P.; Gołąb-Janowska, M. Atrial fibrillation risk factors in patients with ischemic stroke. Archives of Medical Science: AMS 2021, 17, 19. [Google Scholar] [CrossRef]
- Fohtung, R.B.; Rich, M.W. Identification of patients at risk of stroke from atrial fibrillation. Risk 2016, 5, 6. [Google Scholar] [CrossRef]
- Morotti, A.; Goldstein, J.N. Anticoagulant-associated intracerebral hemorrhage. Brain Hemorrhages 2020, 1, 89–94. [Google Scholar] [CrossRef]
- Gabet, A.; Olie, V.; Bejot, Y. Atrial Fibrillation in Spontaneous Intracerebral Hemorrhage, Dijon Stroke Registry (2006-2017). J Am Heart Assoc 2021, 10, e020040. [Google Scholar] [CrossRef] [PubMed]
- Ng, S.S.; Lai, N.M.; Nathisuwan, S.; Jahan, N.K.; Dilokthornsakul, P.; Kongpakwattana, K.; Hollingworth, W.; Chaiyakunapruk, N. Comparative efficacy and safety of warfarin care bundles and novel oral anticoagulants in patients with atrial fibrillation: a systematic review and network meta-analysis. Sci Rep 2020, 10, 662. [Google Scholar] [CrossRef] [PubMed]
- Hammoudeh, A.J.; Khader, Y.; Kadri, N.; Al-Mousa, E.; Badaineh, Y.; Habahbeh, L.; Tabbalat, R.; Janabi, H.; Alhaddad, I.A. Adherence to the 2019 AHA/ACC/HRS Focused Update of the 2014 AHA/ACC/HRS Guideline on the Use of Oral Anticoagulant Agents in Middle Eastern Patients with Atrial Fibrillation: The Jordan Atrial Fibrillation (JoFib) Study. Int J Vasc Med 2021, 2021, 5515089. [Google Scholar] [CrossRef] [PubMed]
- January, C.T.; Wann, L.S.; Calkins, H.; Chen, L.Y.; Cigarroa, J.E.; Cleveland, J.C.; Ellinor, P.T.; Ezekowitz, M.D.; Field, M.E.; Furie, K.L. 2019 AHA/ACC/HRS focused update of the 2014 AHA/ACC/HRS guideline for the management of patients with atrial fibrillation: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines and the Heart Rhythm Society. Journal of the American College of Cardiology 2019, 74, 104–132. [Google Scholar] [CrossRef] [PubMed]
- Pisters, R.; Lane, D.A.; Nieuwlaat, R.; de Vos, C.B.; Crijns, H.J.; Lip, G.Y. A novel user-friendly score (HAS-BLED) to assess 1-year risk of major bleeding in patients with atrial fibrillation: the Euro Heart Survey. Chest 2010, 138, 1093–1100. [Google Scholar] [CrossRef] [PubMed]
- Lip, G.Y.; Nieuwlaat, R.; Pisters, R.; Lane, D.A.; Crijns, H.J. Refining clinical risk stratification for predicting stroke and thromboembolism in atrial fibrillation using a novel risk factor-based approach: the euro heart survey on atrial fibrillation. Chest 2010, 137, 263–272. [Google Scholar] [CrossRef] [PubMed]
- Khatib, B.; Alsalamat, H.; Krishan, M.; Al-Zubiedi, S. Predictors of Anticoagulant Treatment Control in New Warfarin Patients in Jordan. Authorea Preprints 2023. [Google Scholar]
- Alhaddad, Z.; Hammoudeh, A.; Khader, Y.; Alhaddad, I.A. Demographics and Risk Profile of Elderly Middle Eastern Patients with Atrial Fibrillation: The Jordan Atrial Fibrillation (JoFib) Study. Vasc Health Risk Manag 2022, 18, 289–295. [Google Scholar] [CrossRef]
- Melgaard, L.; Gorst-Rasmussen, A.; Lane, D.A.; Rasmussen, L.H.; Larsen, T.B.; Lip, G.Y. Assessment of the CHA2DS2-VASc score in predicting ischemic stroke, thromboembolism, and death in patients with heart failure with and without atrial fibrillation. Jama 2015, 314, 1030–1038. [Google Scholar] [CrossRef]
- Singer, D.E.; Chang, Y.; Borowsky, L.H.; Fang, M.C.; Pomernacki, N.K.; Udaltsova, N.; Reynolds, K.; Go, A.S. A new risk scheme to predict ischemic stroke and other thromboembolism in atrial fibrillation: the ATRIA study stroke risk score. J Am Heart Assoc 2013, 2, e000250. [Google Scholar] [CrossRef] [PubMed]
- Wyse, D. Atrial Fibrillation Follow-up Investigation of Rhythm Management (AFFIRM) Investigators: A comparison of rate control and rhythm control in patients with atrial fibrillation. N Engl J Med 2002, 347, 1825–1833. [Google Scholar] [CrossRef] [PubMed]
- Jarrah, M.I.; Alrabadi, N.; Alzoubi, K.; Mhaidat, Q.N.; Hammoudeh, A. Is there a Concordance between CHA2DS2 VASc and HAS-BLED Scores in Middle Eastern Patients with Nonvalvular AF? Analysis of the Jordan Atrial Fibrillation (JoFib) Study. The Open Cardiovascular Medicine Journal 2022, 16. [Google Scholar] [CrossRef]
- Gomez-Doblas, J.J.; Muniz, J.; Martin, J.J.; Rodriguez-Roca, G.; Lobos, J.M.; Awamleh, P.; Permanyer-Miralda, G.; Chorro, F.J.; Anguita, M.; Roig, E.; et al. Prevalence of atrial fibrillation in Spain. OFRECE study results. Rev Esp Cardiol (Engl Ed) 2014, 67, 259–269. [Google Scholar] [CrossRef] [PubMed]
- Olesen, J.B.; Lip, G.Y.; Hansen, M.L.; Hansen, P.R.; Tolstrup, J.S.; Lindhardsen, J.; Selmer, C.; Ahlehoff, O.; Olsen, A.M.; Gislason, G.H.; et al. Validation of risk stratification schemes for predicting stroke and thromboembolism in patients with atrial fibrillation: nationwide cohort study. BMJ 2011, 342, d124. [Google Scholar] [CrossRef] [PubMed]
- January, C.T.; Wann, L.S.; Alpert, J.S.; Calkins, H.; Cigarroa, J.E.; Cleveland, J.C.; Conti, J.B.; Ellinor, P.T.; Ezekowitz, M.D.; Field, M.E. 2014 AHA/ACC/HRS guideline for the management of patients with atrial fibrillation: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and the Heart Rhythm Society. Journal of the American College of Cardiology 2014, 64, e1–e76. [Google Scholar] [CrossRef]
- Henriksson, K.M.; Farahmand, B.; Johansson, S.; Asberg, S.; Terent, A.; Edvardsson, N. Survival after stroke--the impact of CHADS2 score and atrial fibrillation. Int J Cardiol 2010, 141, 18–23. [Google Scholar] [CrossRef]
- Vemmos, K.; Ntaios, G.; Savvari, P.; Vemmou, A.M.; Koroboki, E.; Manios, E.; Kounali, A.; Lip, G.Y. Stroke aetiology and predictors of outcome in patients with heart failure and acute stroke: a 10-year follow-up study. Eur J Heart Fail 2012, 14, 211–218. [Google Scholar] [CrossRef]
- Kaplan, R.M.; Koehler, J.; Ziegler, P.D.; Sarkar, S.; Zweibel, S.; Passman, R.S. Stroke risk as a function of atrial fibrillation duration and CHA2DS2-VASc score. Circulation 2019, 140, 1639–1646. [Google Scholar] [CrossRef]
- Yao, X.; Gersh, B.J.; Sangaralingham, L.R.; Kent, D.M.; Shah, N.D.; Abraham, N.S.; Noseworthy, P.A. Comparison of the CHA2DS2-VASc, CHADS2, HAS-BLED, ORBIT, and ATRIA risk scores in predicting non–vitamin K antagonist oral anticoagulants-associated bleeding in patients with atrial fibrillation. The American Journal of Cardiology 2017, 120, 1549–1556. [Google Scholar] [CrossRef]
- Angiolillo, D.J.; Patti, G.; Chan, K.T.; Han, Y.; Huang, W.C.; Yakovlev, A.; Paek, D.; Del Aguila, M.; Girotra, S.; Sibbing, D. De-escalation from ticagrelor to clopidogrel in acute coronary syndrome patients: a systematic review and meta-analysis. J Thromb Thrombolysis 2019, 48, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Morrone, D.; Kroep, S.; Ricci, F.; Renda, G.; Patti, G.; Kirchhof, P.; Chuang, L.-H.; van Hout, B.; De Caterina, R. Mortality prediction of the CHA2DS2-VASc score, the HAS-BLED score, and their combination in anticoagulated patients with atrial fibrillation. Journal of clinical medicine 2020, 9, 3987. [Google Scholar] [CrossRef] [PubMed]
- Parsons, C.; Patel, S.I.; Cha, S.; Shen, W.K.; Desai, S.; Chamberlain, A.M.; Luis, S.A.; Aguilar, M.I.; Demaerschalk, B.M.; Mookadam, F.; et al. CHA(2)DS(2)-VASc Score: A Predictor of Thromboembolic Events and Mortality in Patients With an Implantable Monitoring Device Without Atrial Fibrillation. Mayo Clin Proc 2017, 92, 360–369. [Google Scholar] [CrossRef] [PubMed]
- Brambatti, M.; Connolly, S.J.; Gold, M.R.; Morillo, C.A.; Capucci, A.; Muto, C.; Lau, C.P.; Van Gelder, I.C.; Hohnloser, S.H.; Carlson, M. Temporal relationship between subclinical atrial fibrillation and embolic events. Circulation 2014, 129, 2094–2099. [Google Scholar] [CrossRef] [PubMed]
- Potpara, T.S.; Lip, G.Y.; Blomstrom-Lundqvist, C.; Boriani, G.; Van Gelder, I.C.; Heidbuchel, H.; Hindricks, G.; Camm, A.J. The 4S-AF scheme (stroke risk; symptoms; severity of burden; substrate): a novel approach to in-depth characterization (rather than classification) of atrial fibrillation. Thrombosis and haemostasis 2021, 121, 270–278. [Google Scholar] [CrossRef] [PubMed]
- Lip, G.; Freedman, B.; De Caterina, R.; Potpara, T.S. Stroke prevention in atrial fibrillation: Past, present and future. Comparing the guidelines and practical decision-making. Thromb Haemost 2017, 117, 1230–1239. [Google Scholar] [CrossRef]
- Cutugno, C.L. CE: Atrial Fibrillation: Updated Management Guidelines and Nursing Implications. Am J Nurs 2015, 115, 26–38, quiz 39, 49. [Google Scholar] [CrossRef]
- Nesheiwat, Z.; Goyal, A.; Jagtap, M.; Shammas, A. Atrial Fibrillation (Nursing). In StatPearls [Internet]; StatPearls Publishing, 2021. [Google Scholar]
| Variable | Sub-Variable | 1 month (n = 631) |
6 months (n = 607) |
12 months (n = 557) |
total in 12 months |
|---|---|---|---|---|---|
| Number of Death | 5 | 11 | 13 | 15 | |
| Number of CVA | 3 | 11 | 7 | 21 | |
| CVA recurrence | 0 | 1 | 2 | 3 | |
| Type of CVA | Embolic | 3 | 1 | 2 | 6 |
| Thrombotic | 0 | 4 | 2 | 6 | |
| Undefined | 0 | 6 | 3 | 9 | |
| Number of systemic embolization | 1 | 2 | 1 | 4 | |
| Systemic embolization recurrence | 0 | 0 | 0 | 0 | |
| Site of systemic embolization | Mesenteric | 1 | 0 | 0 | 1 |
| Lower limbs | 0 | 2 | 1 | 3 | |
| Number of major bleedings | 7 | 10 | 7 | 24 | |
| Number of bleeding episodes | 1 for all 7 cases | 1 for all 10 cases | 1 for 6 cases, and 3 for 1 case | 1 for 23 cases, and 3 for 1 case | |
| Type of bleeding | Bleeding leading to hospitalization | 2 | 4 | 4 | 10 |
| Intracranial | 0 | 4 | 2 | 6 | |
| Hemoglobin drop ≤ 2 g/dl | 2 | 2 | 1 | 5 | |
| Bleeding leading to transfusion | 3 | 0 | 0 | 3 | |
| Number of ACS | 2 | 0 | 0 | 2 | |
| Type of ACS | STEMI | 2 | 0 | 0 | 2 |
| NSTEACS | 2 | 2 | 2 | 6 | |
| Medical Interventions | PCI | 4 | 2 | 2 | 8 |
| INR value (Mean ± SD) Baseline 2.49 ± 1.15 |
2.6±1.16 | 2.53±0.77 | 2.55±1.05 | - |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




