Submitted:
12 January 2024
Posted:
12 January 2024
You are already at the latest version
Abstract
Keywords:
Introduction
Methods
Data Source
Study Population
Outcome and Predictor Variables
Statistical Analysis
| Standard parametric models | Flexible parametric scale |
|---|---|
| Weibull | Hazard |
| ln{− ln S(t; xi)} = ln{− ln S0(t)} + xiβ | ln{− ln S0(t; xi)} = s(ln t; γ) + xiβ |
| Loglogistic | Odds |
| logit{1 − S(t; xi)} = logit{1 − S0(t)} + xiβ | logit{1 − S(t; xi)} = s(ln t; γ) + xiβ |
| Lognormal | Probit |
| −Φ−1{S(ln t)} = −Φ−1{S0(ln t)} + xiβ | −Φ−1{S(ln t)} = s(ln t; γ) + xiβ |
Model Fit
Assessment of the Predictive Ability of Models
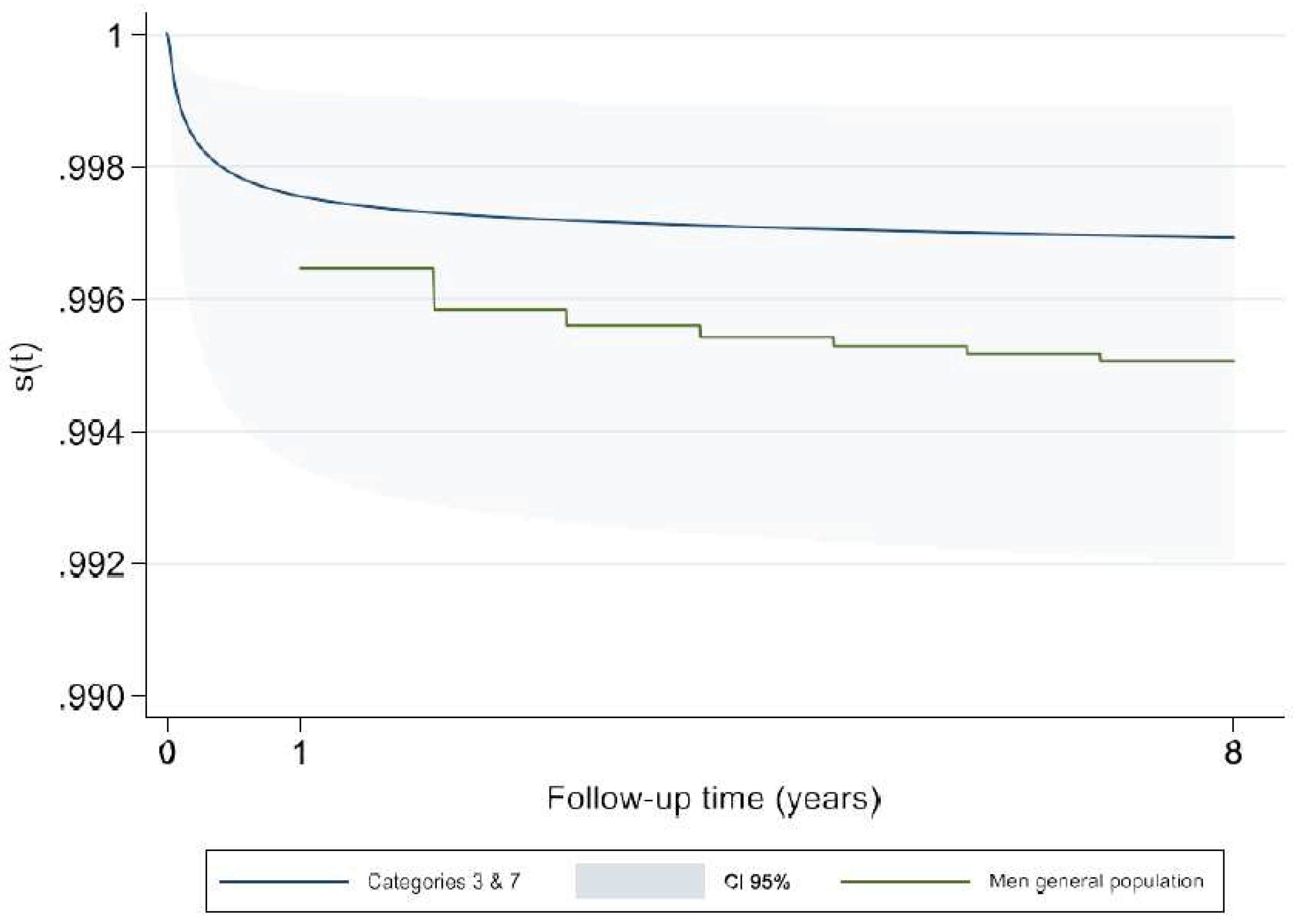
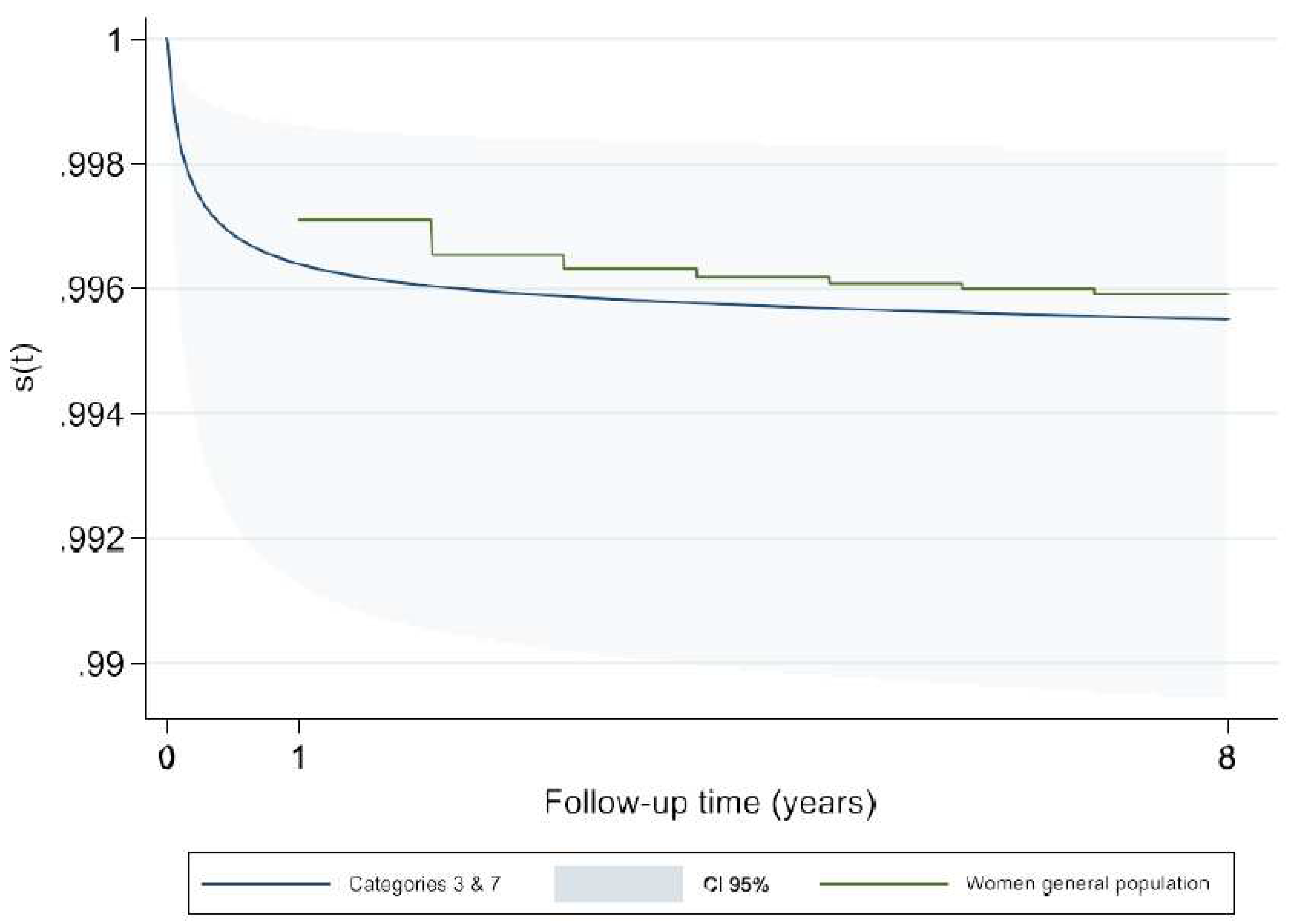
Comparison with the General Population
| N (%) or mean ± SD | 8-year survival rate (%) |
|
|---|---|---|
| Female | 1018 (54.1) | 96 |
| SGA† (< 10th percentile of Audipog’s curve) | 205 (10.9) | 93* |
| Surgery during 1st year of life | 382 (20.3) | 92* |
| Premature (< 37 weeks of gestation) | 240 (12.8) | 91* |
| * p < .05 Logrank test or ttest, as appropriate. † Small for Gestational Age |
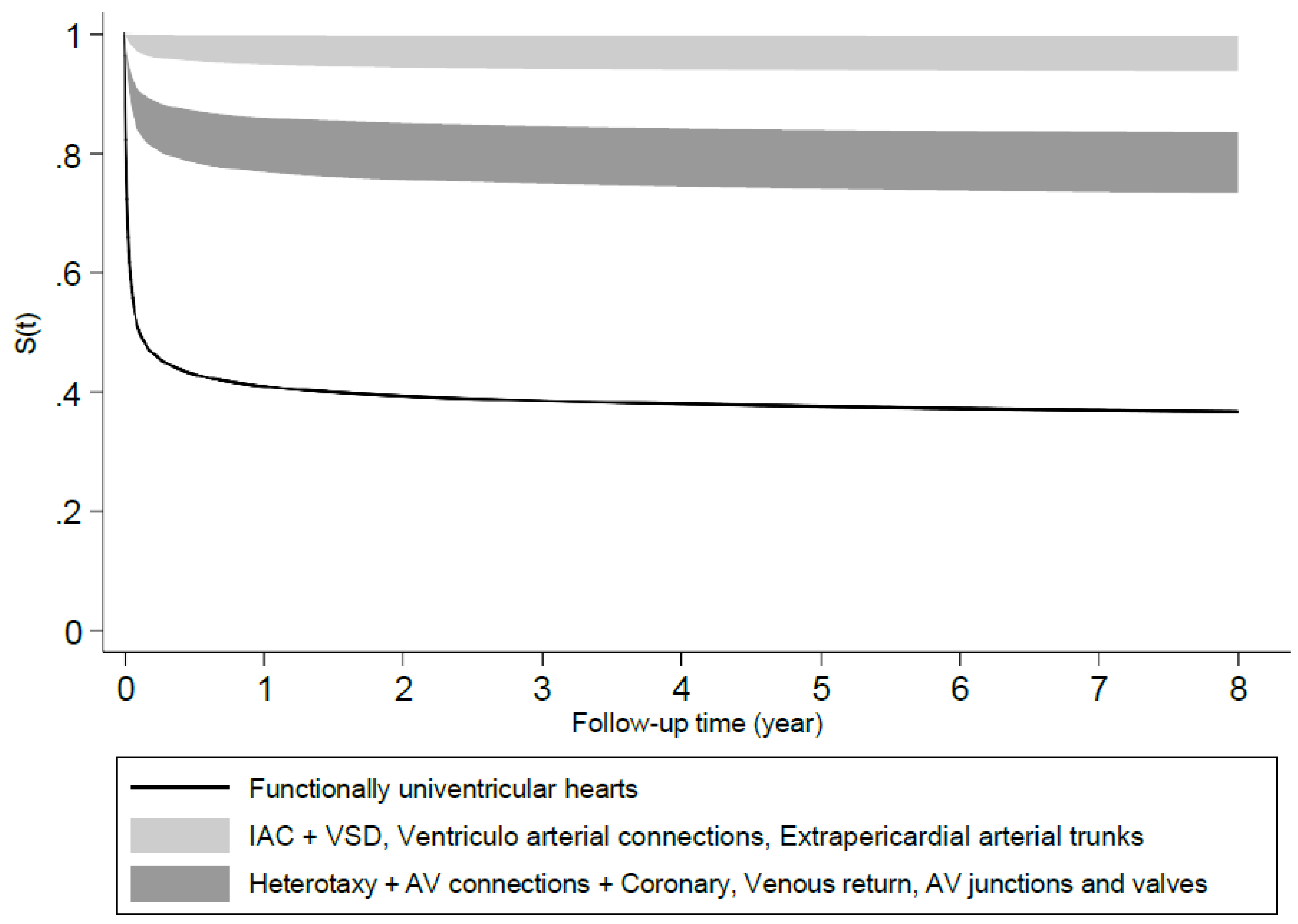
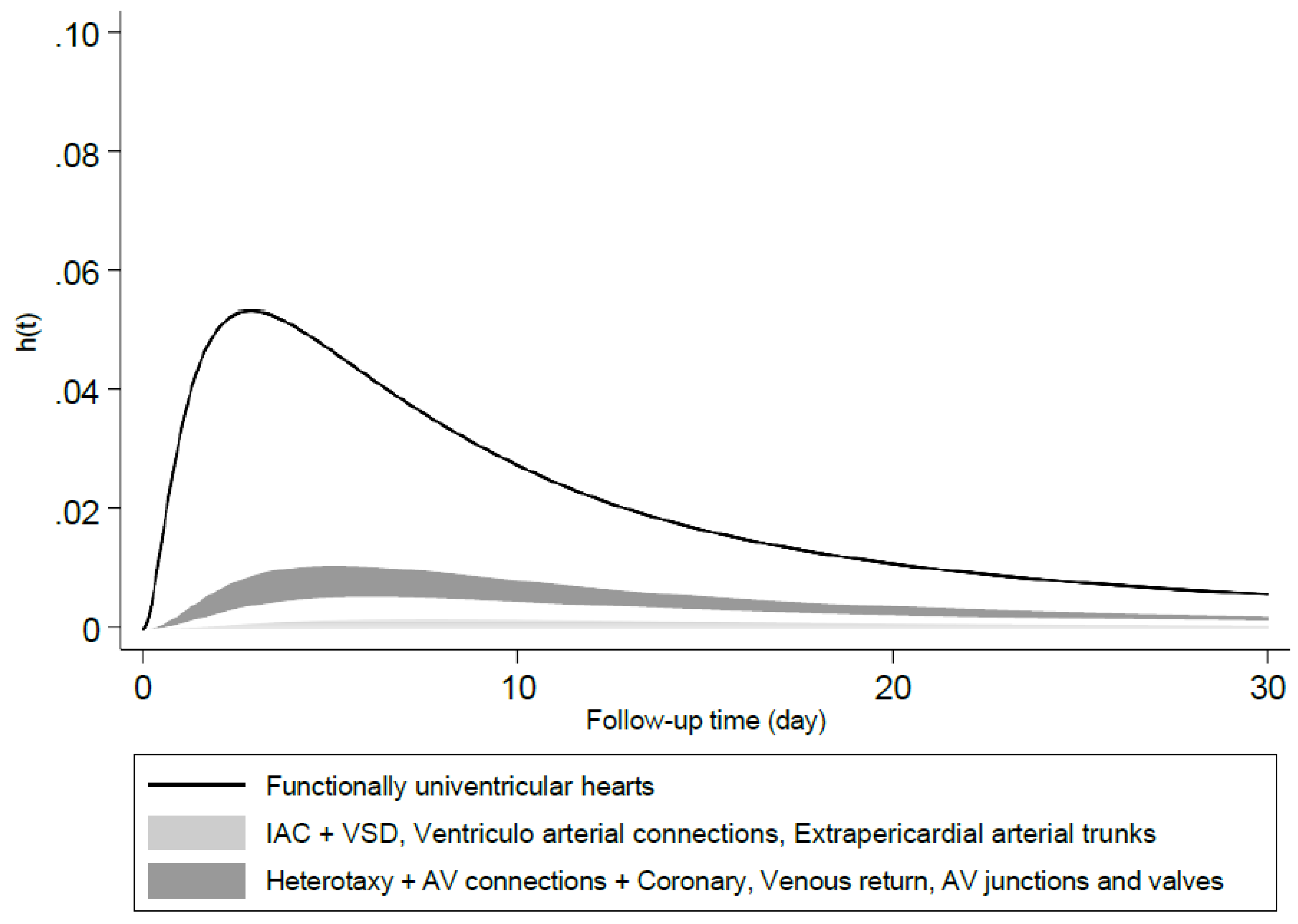
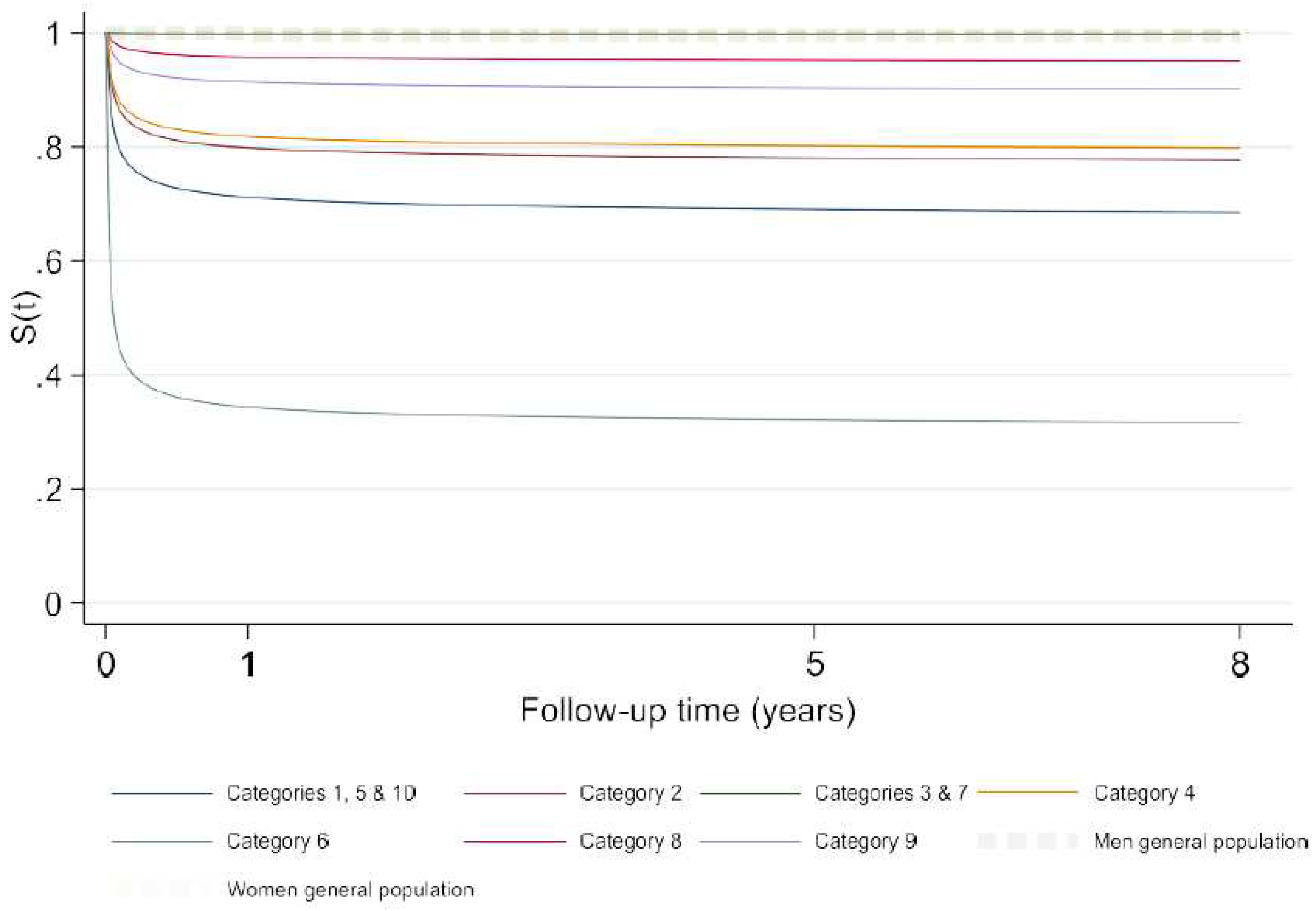
| ACC-CHD groups | N (%) | S(t)* |
|---|---|---|
| Heterotaxy, including isomerism and mirror-imagery + Complex anomalies of atrioventricular connections + Congenital anomalies of the coronary arteries (Heterotaxy + AV connections + Coronary anomalies) | 22 (1.2) | .68 [.45 - .83] |
| Anomalies of the venous return | 20 (1.1) | .80 [.55 - .92] |
| Anomalies of the atria and interatrial communications + Ventricular septal defects (IAC + VSD) | 1311 (69.7) | .99 [.988 - .997] |
| Anomalies of the atrioventricular junctions and valves | 48 (2.5) | .77 [.62 - .87] |
| Functionally univentricular hearts | 34 (1.8) | .44 [.27 - .60] |
| Anomalies of the ventricular outflow tracts (ventriculo-arterialconnections) | 360 (19.1) | .94 [.91 - .96] |
| Anomalies of the extrapericardial arterial trunks | 86 (4.6) | .92 [.84 - .96] |
| * 8-year survival rate and its 95% confidence interval in brackets |
| Model 1 | Model 2 | |
| Original dataset | ||
| Royston’s D | 1.43 | 1.60 |
| R2 | 0.45 [0.36 - 0.52] | 0.50 [0.41 - 0.58] |
| Bootstrap sampling | ||
| Royston’s D | 1.40 | 1.49 |
| R2 | 0.44 [0.35 - 0.51] | 0.47 [0.38 - 0.55] |
Discussion
Supplementary Materials
Appendix A
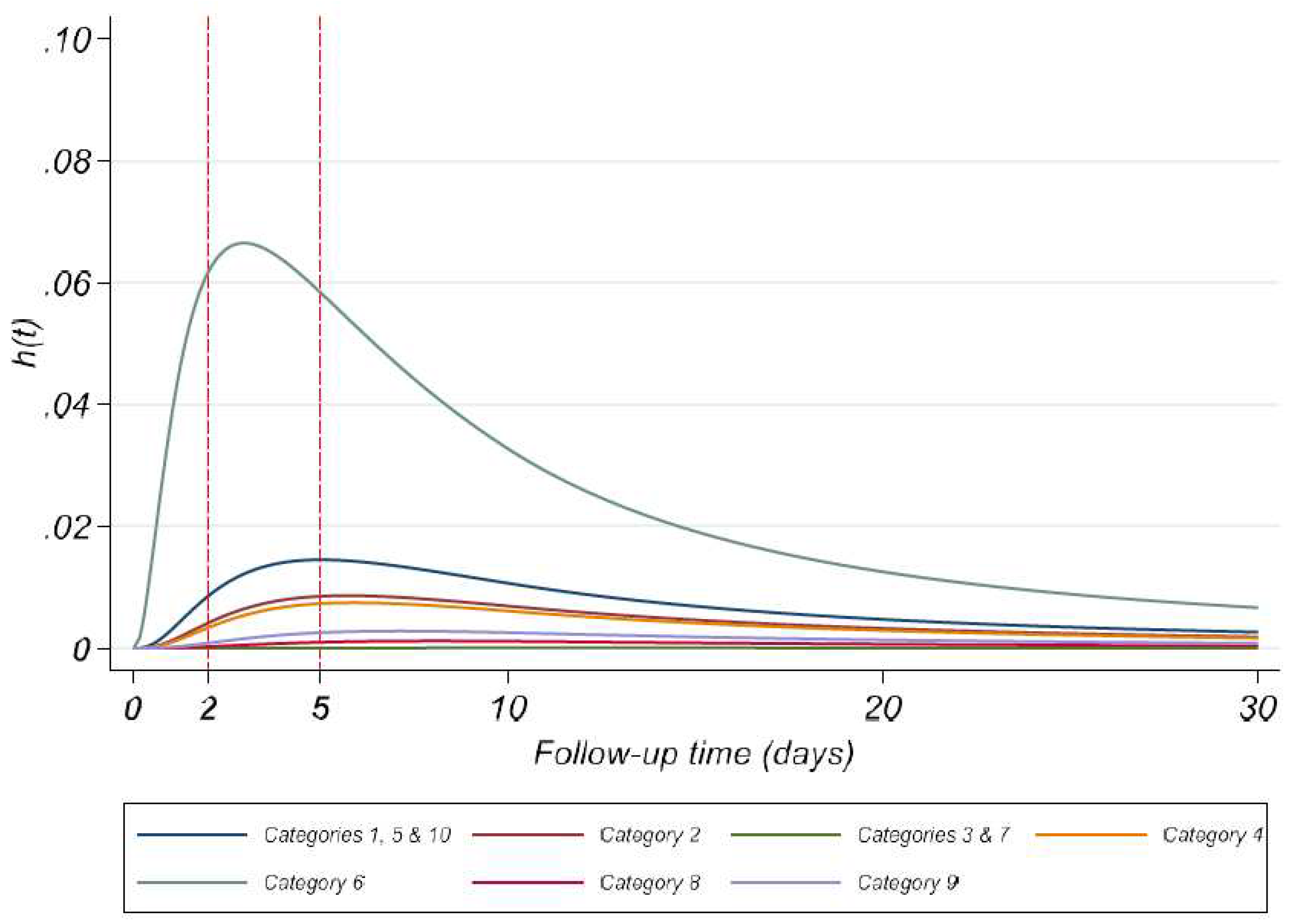

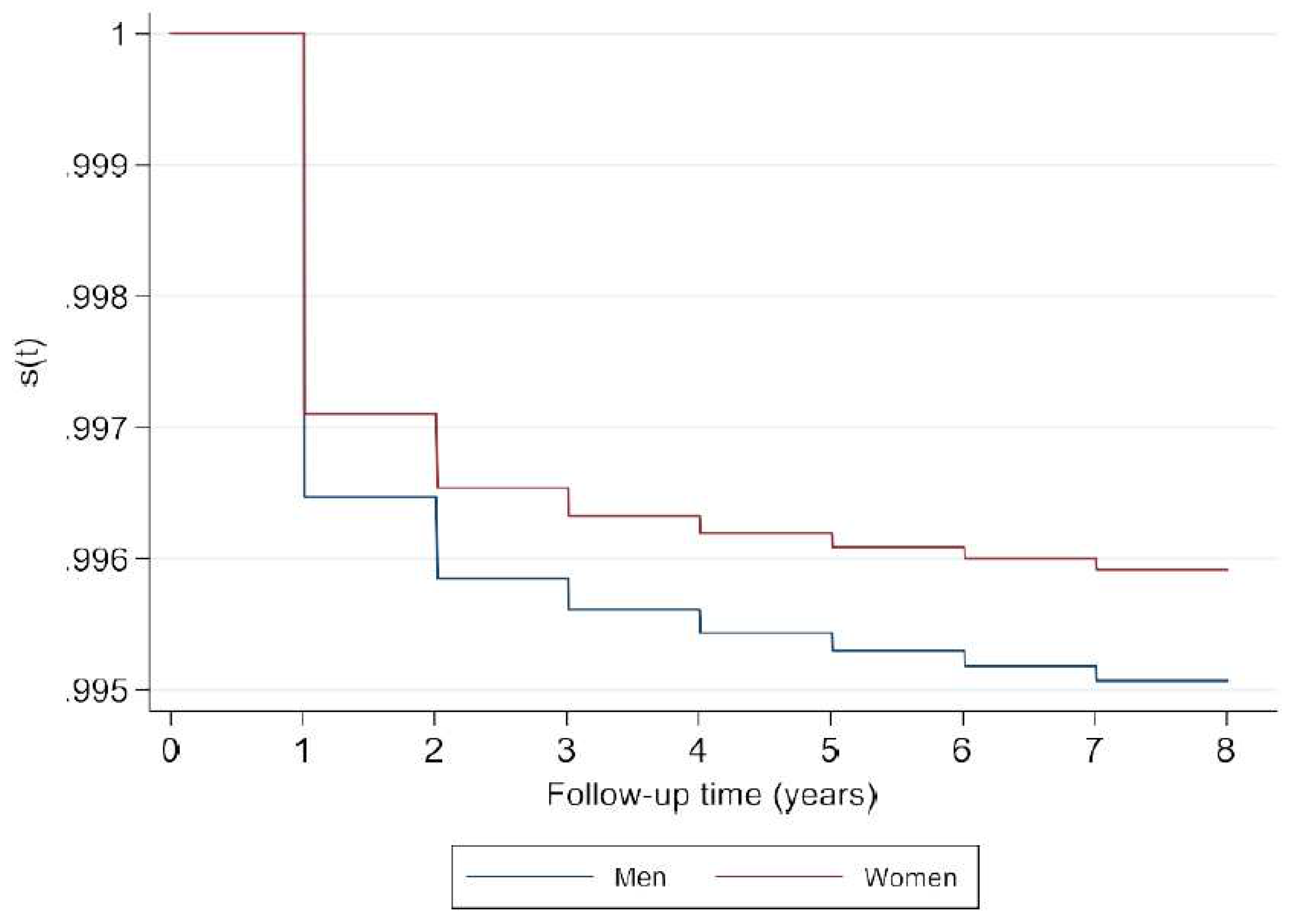
References
- Zipes DP, Libby P, Bonow RO, Mann DL, Tomaselli GF, Braunwald E, editors. Braunwald’s heart disease: a textbook of cardiovascular medicine. Eleventh edition, international edition. Philadelphia, PA: Elsevier; 2019. 1944 p.
- Khoshnood B, Lelong N, Houyel L, Thieulin A-C, Jouannic J-M, Magnier S, et al. Prevalence, timing of diagnosis and mortality of newborns with congenital heart defects: a population-based study. Heart. 2012, 98, 1667–73. [Google Scholar] [CrossRef] [PubMed]
- Khoshnood B, Lelong N, Houyel L, Thieulin A-C, Jouannic J-M, Magnier S, et al. Prevalence, timing of diagnosis and mortality of newborns with congenital heart defects: a population-based study. Heart. 2012, 98, 1667–73. [Google Scholar] [CrossRef] [PubMed]
- Congenital heart defects [Internet]. nhlbi.nih.gov. Available from: https://www.nhlbi.nih.gov/health-topics/congenital-heart-defects.
- van der Bom T, Zomer AC, Zwinderman AH, Meijboom FJ, Bouma BJ, Mulder BJM. The changing epidemiology of congenital heart disease. Nat Rev Cardiol. 2011, 8, 50–60. [Google Scholar] [CrossRef] [PubMed]
- Razzaghi H, Oster M, Reefhuis J. Long-Term Outcomes in Children with Congenital Heart Disease: National Health Interview Survey. J Pediatr. 2015, 166, 119–124. [Google Scholar] [CrossRef] [PubMed]
- Liu Y, Chen S, Zühlke L, Black GC, Choy M, Li N, et al. Global birth prevalence of congenital heart defects 1970–2017: updated systematic review and meta-analysis of 260 studies. Int J Epidemiol. 2019, 48, 455–63. [Google Scholar] [CrossRef] [PubMed]
- van der Linde D, Konings EEM, Slager MA, Witsenburg M, Helbing WA, Takkenberg JJM, et al. Birth Prevalence of Congenital Heart Disease Worldwide. J Am Coll Cardiol. 2011, 58, 2241–7.
- Tararbit K, Bui TTT, Lelong N, Thieulin A-C, Goffinet F, Khoshnood B. Clinical and socioeconomic predictors of pregnancy termination for fetuses with congenital heart defects: a population-based evaluation: Pregnancy termination for fetuses with CHD. Prenat Diagn. 2013, 33, 179–86. [Google Scholar] [CrossRef] [PubMed]
- Blue GM, Kirk EP, Sholler GF, Harvey RP, Winlaw DS. Congenital heart disease: current knowledge about causes and inheritance. Med J Aust. 2012, 197, 155–9. [Google Scholar] [CrossRef] [PubMed]
- Jenkins KJ, Correa A, Feinstein JA, Botto L, Britt AE, Daniels SR, et al. Noninherited Risk Factors and Congenital Cardiovascular Defects: Current Knowledge: A Scientific Statement From the American Heart Association Council on Cardiovascular Disease in the Young: Endorsed by the American Academy of Pediatrics. Circulation. 2007, 115, 2995–3014. [Google Scholar] [CrossRef] [PubMed]
- Houyel L, Khoshnood B, Anderson RH, Lelong N, Thieulin A-C, Goffinet F, et al. Population-based evaluation of a suggested anatomic and clinical classification of congenital heart defects based on the International Paediatric and Congenital Cardiac Code. Orphanet J Rare Dis. 2011, 6, 64. [Google Scholar] [CrossRef] [PubMed]
- Kattan MW, Gönen M. The prediction philosophy in statistics. Urol Oncol Semin Orig Investig. 2008, 26, 316–9. [Google Scholar]
- Moons KGM, Royston P, Vergouwe Y, Grobbee DE, Altman DG. Prognosis and prognostic research: what, why, and how? BMJ. 2009, 338, b375–b375. [Google Scholar] [CrossRef] [PubMed]
- Royston P, Lambert PC. Flexible parametric survival analysis using Stata: beyond the Cox model. College Station, TX: Stata Press; 2011. 347 p.
- Peduzzi P, Concato J, Feinstein AR, Holford TR. Importance of events per independent variable in proportional hazards regression analysis. II. Accuracy and precision of regression estimates. J Clin Epidemiol. 1995, 48, 1503–10.
- Vittinghoff E, McCulloch CE. Relaxing the rule of ten events per variable in logistic and Cox regression. Am J Epidemiol. 2007, 165, 710–8. [Google Scholar] [CrossRef] [PubMed]
- Royston P, Moons KGM, Altman DG, Vergouwe Y. Prognosis and prognostic research: Developing a prognostic model. BMJ. 2009, 338, b604–b604. [Google Scholar] [CrossRef] [PubMed]
- Choodari-Oskooei B, Royston P, Parmar MKB. A simulation study of predictive ability measures in a survival model I: Explained variation measures. Stat Med. 2012, 31, 2627–43. [Google Scholar] [CrossRef] [PubMed]
- Altman DG, Vergouwe Y, Royston P, Moons KGM. Prognosis and prognostic research: validating a prognostic model. BMJ. 2009, 338, b605–b605. [Google Scholar] [CrossRef] [PubMed]
- Harrell FE, Lee K, Mark DB. Multivariable prognostic models: Issues in developing models, evaluating assumptions and adequacy, and measuring and reducing errors. Stat Med. 1996, 15, 361–87. [Google Scholar] [CrossRef]
- Tables de mortalité par niveau de vie [Internet]. INSEE. Available from: https://www.insee.fr/fr/statistiques/3311422?sommaire=3311425.
| Number of interior knots |
d.f. | Centiles (uncensored log event-time) | |
|---|---|---|---|
| 1 | 2 | 50 | |
| 2 | 3 | 33, 67 | |
| 3 | 4 | 25, 50, 75 | |
| 4 | 5 | 20, 40, 60, 80 | |
| 5 | 6 | 17, 33, 50, 67, 83 | |
| 6 | 7 | 14, 29, 43, 57, 71, 86 | |
| 7 | 8 | 12.5, 25, 37.5, 50, 62.5, 75, 87.5 | |
| 8 | 9 | 11.1, 22.2, 33.3, 44.4, 55.6, 66.7, 77.8, 88.9 | |
| 9 | 10 | 10, 20, 30, 40, 50, 60, 70, 80, 90 | |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




