Submitted:
02 January 2024
Posted:
03 January 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Statistical Analysis
3. Results
3.1. Seasonality
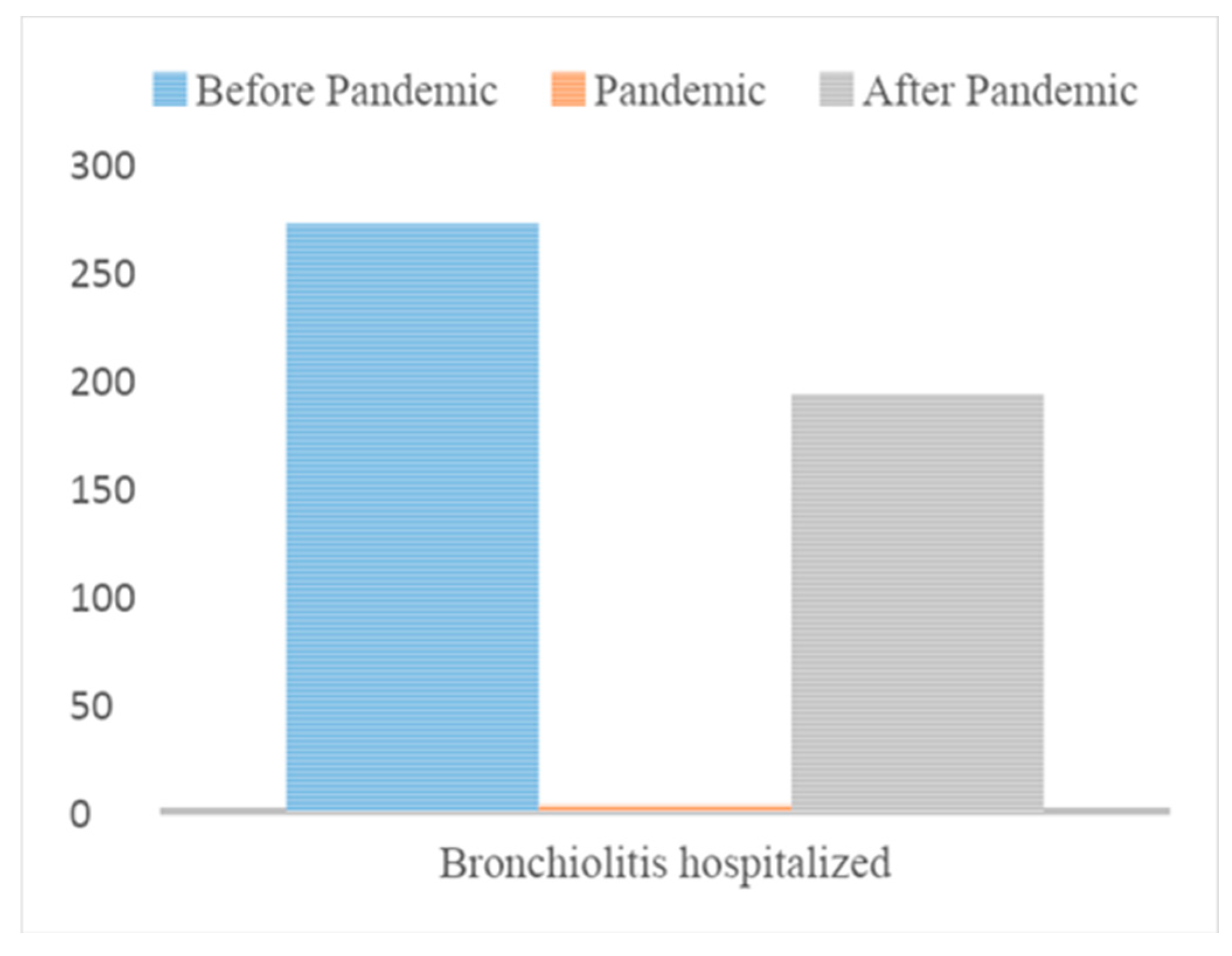
3.2. Clinical and Epidemiological Characteristics of Hospitalized Patients
| Complications | Yes | 12 (11%) | 12 (9%) | 0.82 |
| No | 97 (89%) | 116 (91%) | ||
| Hospitalization (days) | 6 (2-33) | 5 (1-13) | 0.051 | |
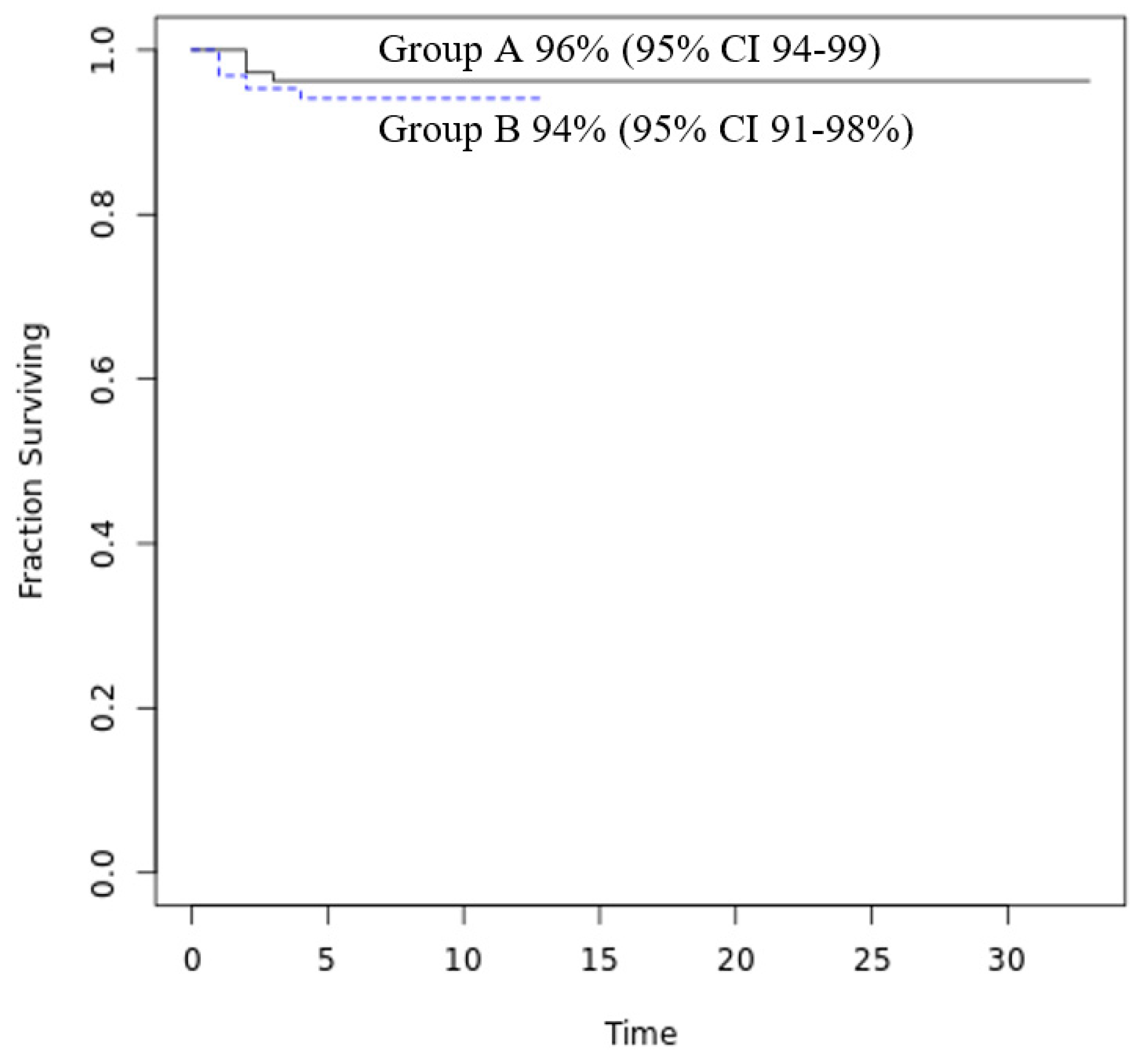
| Transfer to a Hub hospital | Yes | 4 (4%) | 7 (5%) | 0.55 |
| No | 105 (96%) | 121 (94%) |
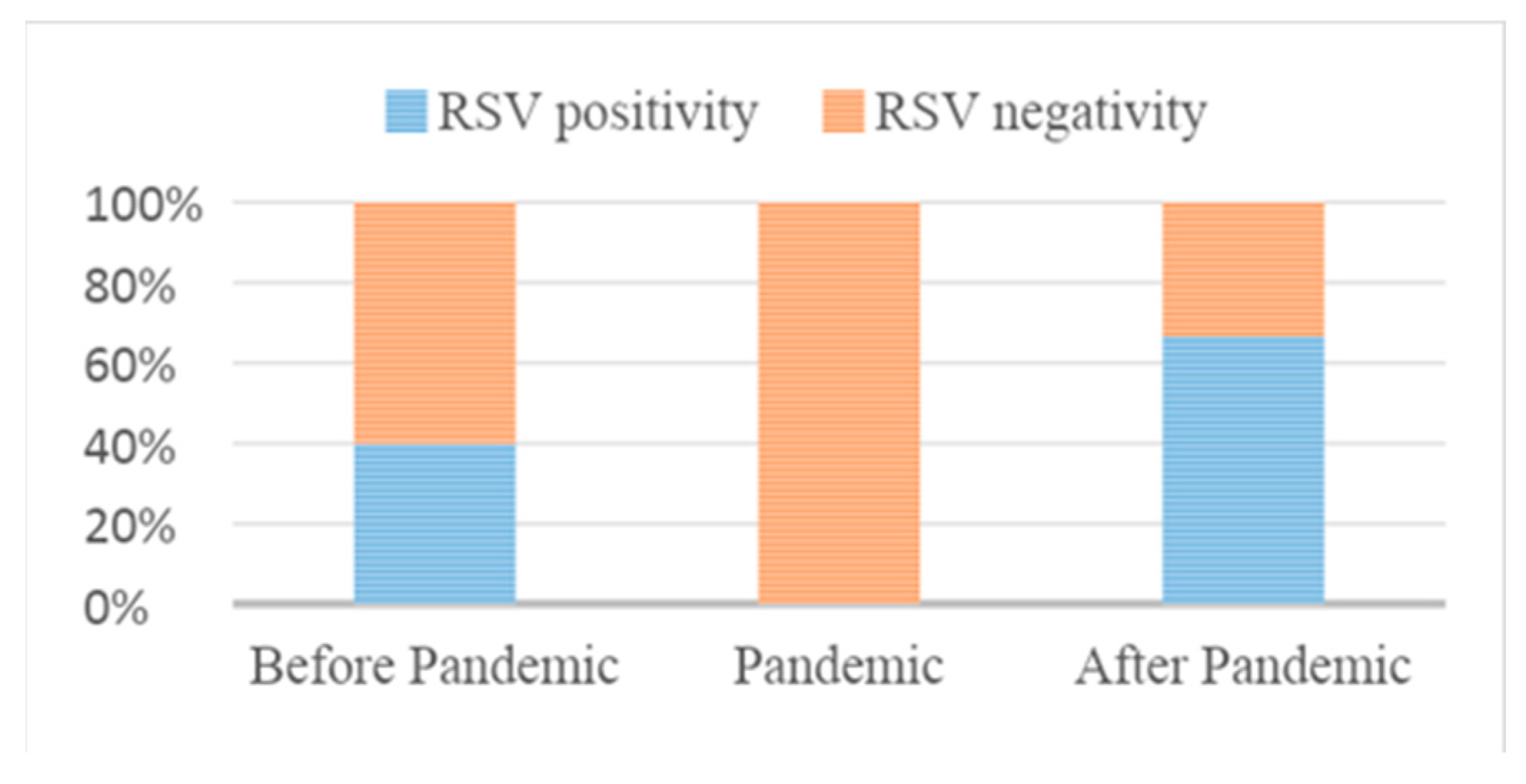
3.3. RSV Prevalence
| 2017-2020 | 2021-2023 | P value | |
| RSV positive | 109 (40%) | 128 (66%) | <0.0001 |
| RSV negative | 163 (60%) | 65 (34%) |
4. Discussion
5. Conclusions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Meissner HC. Viral Bronchiolitis in Children. Ingelfinger JR, ed. N Engl J Med. 2016;374(1):62-72. [CrossRef]
- Perez A, Lively JY, Curns A, et al. Respiratory Virus Surveillance Among Children with Acute Respiratory Illnesses — New Vaccine Surveillance Network, United States, 2016–2021. MMWR Morb Mortal Wkly Rep. 2022;71(40):1253-1259. [CrossRef]
- Manti S, Staiano A, Orfeo L, et al. UPDATE - 2022 Italian guidelines on the management of bronchiolitis in infants. Ital J Pediatr. 2023;49(1):19. [CrossRef]
- Cutrera R, Wolfler A, Picone S, et al. Impact of the 2014 American Academy of Pediatrics recommendation and of the resulting limited financial coverage by the Italian Medicines Agency for palivizumab prophylaxis on the RSV-associated hospitalizations in preterm infants during the 2016–2017 epidemic season: a systematic review of seven Italian reports. Ital J Pediatr. 2019;45(1):139. [CrossRef]
- Mazur NI, Martinón-Torres F, Baraldi E, et al. Lower respiratory tract infection caused by respiratory syncytial virus: current management and new therapeutics. Lancet Respir Med. 2015;3(11):888-900. [CrossRef]
- Viguria N, Navascués A, Juanbeltz R, Echeverría A, Ezpeleta C, Castilla J. Effectiveness of palivizumab in preventing respiratory syncytial virus infection in high-risk children. Hum Vaccines Immunother. 2021;17(6):1867-1872. [CrossRef]
- Azzari C, Baraldi E, Bonanni P, et al. Epidemiology and prevention of respiratory syncytial virus infections in children in Italy. Ital J Pediatr. 2021;47(1):198. [CrossRef]
- Li Y, Wang X, Msosa T, De Wit F, Murdock J, Nair H. The impact of the 2009 influenza pandemic on the seasonality of human respiratory syncytial virus: A systematic analysis. Influenza Other Respir Viruses. 2021;15(6):804-812. [CrossRef]
- Nascimento MS, Baggio DM, Fascina LP, Do Prado C. Impact of social isolation due to COVID-19 on the seasonality of pediatric respiratory diseases. Morrow BM, ed. PLOS ONE. 2020;15(12):e0243694. [CrossRef]
- Van Brusselen D, De Troeyer K, Ter Haar E, et al. Bronchiolitis in COVID-19 times: a nearly absent disease? Eur J Pediatr. 2021;180(6):1969-1973. [CrossRef]
- Foley DA, Yeoh DK, Minney-Smith CA, et al. The Interseasonal Resurgence of Respiratory Syncytial Virus in Australian Children Following the Reduction of Coronavirus Disease 2019–Related Public Health Measures. Clin Infect Dis. 2021;73(9):e2829-e2830. [CrossRef]
- Saravanos GL, Hu N, Homaira N, et al. RSV Epidemiology in Australia Before and During COVID-19. Pediatrics. 2022;149(2):e2021053537. [CrossRef]
- Public Health Surveillance Inforamtion for New Zealands Public Health Action. Laboratory-Based Virology Weekly Report, 2004–2019. 2021. Available online: https://surv.esr.cri.nz/virology/virology_weekly_report.php.
- Camporesi A, Morello R, Ferro V, et al. Epidemiology, Microbiology and Severity of Bronchiolitis in the First Post-Lockdown Cold Season in Three Different Geographical Areas in Italy: A Prospective, Observational Study. Children. 2022;9(4):491. [CrossRef]
- Tulyapronchote R, Selhorst JB, Malkoff MD, Gomez CR. Delayed sequelae of vertebral artery dissection and occult cervical fractures. Neurology. 1994;44(8):1397-1397. [CrossRef]
- Agha R, Avner JR. Delayed Seasonal RSV Surge Observed During the COVID-19 Pandemic. Pediatrics. 2021;148(3):e2021052089. [CrossRef]
- Guitart C, Bobillo-Perez S, Alejandre C, et al. Bronchiolitis, epidemiological changes during the SARS-CoV-2 pandemic. BMC Infect Dis. 2022;22(1):84. [CrossRef]
- Available online: http://www.ruparpiemonte.it/infostat/risultati.jsp.
- Kaplan EL, Meier P. Nonparametric Estimation from Incomplete Observations. J Am Stat Assoc. 1958;53(282):457-481. [CrossRef]
- Mantel N. Evaluation of survival data and two new rank order statistics arising in its consideration. Cancer Chemother Rep. 1966;50(3):163-170.
- Kruskal WH, Wallis WA. Use of Ranks in One-Criterion Variance Analysis. J Am Stat Assoc. 1952;47(260):583-621. [CrossRef]
- Curatola A, Graglia B, Ferretti S, et al. The acute bronchiolitis rebound in children after COVID-19 restrictions: a retrospective, observational analysis. Acta Biomed Atenei Parm. 2023;94(1):e2023031. [CrossRef]
- Pruccoli G, Castagno E, Raffaldi I, et al. The Importance of RSV Epidemiological Surveillance: A Multicenter Observational Study of RSV Infection during the COVID-19 Pandemic. Viruses. 2023;15(2):280. [CrossRef]
- Olsen SJ, Winn AK, Budd AP, et al. Changes in Influenza and Other Respiratory Virus Activity During the COVID-19 Pandemic — United States, 2020–2021. MMWR Morb Mortal Wkly Rep. 2021;70(29):1013-1019. [CrossRef]
- Weinberger Opek M, Yeshayahu Y, Glatman-Freedman A, Kaufman Z, Sorek N, Brosh-Nissimov T. Delayed respiratory syncytial virus epidemic in children after relaxation of COVID-19 physical distancing measures, Ashdod, Israel, 2021. Eurosurveillance. 2021;26(29). [CrossRef]
- Bermúdez Barrezueta L, Gutiérrez Zamorano M, López-Casillas P, Brezmes-Raposo M, Sanz Fernández I, Pino Vázquez MDLA. Influencia de la pandemia COVID-19 sobre la epidemiología de la bronquiolitis aguda. Enfermedades Infecc Microbiol Clínica. 2023;41(6):348-351. [CrossRef]
- Shanahan KH, Monuteaux MC, Bachur RG. Severity of Illness in Bronchiolitis Amid Unusual Seasonal Pattern During the COVID-19 Pandemic. Hosp Pediatr. 2022;12(4):e119-e123. [CrossRef]
- Correction to: Outbreak of Respiratory Syncytial Virus Bronchiolitis in Italy. Clin Infect Dis. 2023;76(4):777-779. [CrossRef]
- Nenna R, Matera L, Pierangeli A, et al. First COVID-19 lockdown resulted in most respiratory viruses disappearing among hospitalised children, with the exception of rhinoviruses. Acta Paediatr. 2022;111(7):1399-1403. [CrossRef]
- Ferrero F, Ossorio MF. Is there a place for bronchiolitis in the COVID-19 era? Lack of hospitalizations due to common respiratory viruses during the 2020 winter. Pediatr Pulmonol. 2021;56(7):2372-2373. [CrossRef]
- Wilder JL, Parsons CR, Growdon AS, Toomey SL, Mansbach JM. Pediatric Hospitalizations During the COVID-19 Pandemic. Pediatrics. 2020;146(6):e2020005983. [CrossRef]
- Lumley SF, Richens N, Lees E, et al. Changes in paediatric respiratory infections at a UK teaching hospital 2016–2021; impact of the SARS-CoV-2 pandemic. J Infect. 2022;84(1):40-47. [CrossRef]
- Koivisto K, Nieminen T, Mejias A, et al. Respiratory Syncytial Virus (RSV)–Specific Antibodies in Pregnant Women and Subsequent Risk of RSV Hospitalization in Young Infants. J Infect Dis. 2022;225(7):1189-1196. [CrossRef]
- Manti S, Leonardi S, Rezaee F, Harford TJ, Perez MK, Piedimonte G. Effects of Vertical Transmission of Respiratory Viruses to the Offspring. Front Immunol. 2022;13:853009. [CrossRef]
- Hatter L, Eathorne A, Hills T, Bruce P, Beasley R. Respiratory syncytial virus: paying the immunity debt with interest. Lancet Child Adolesc Health. 2021;5(12):e44-e45. [CrossRef]
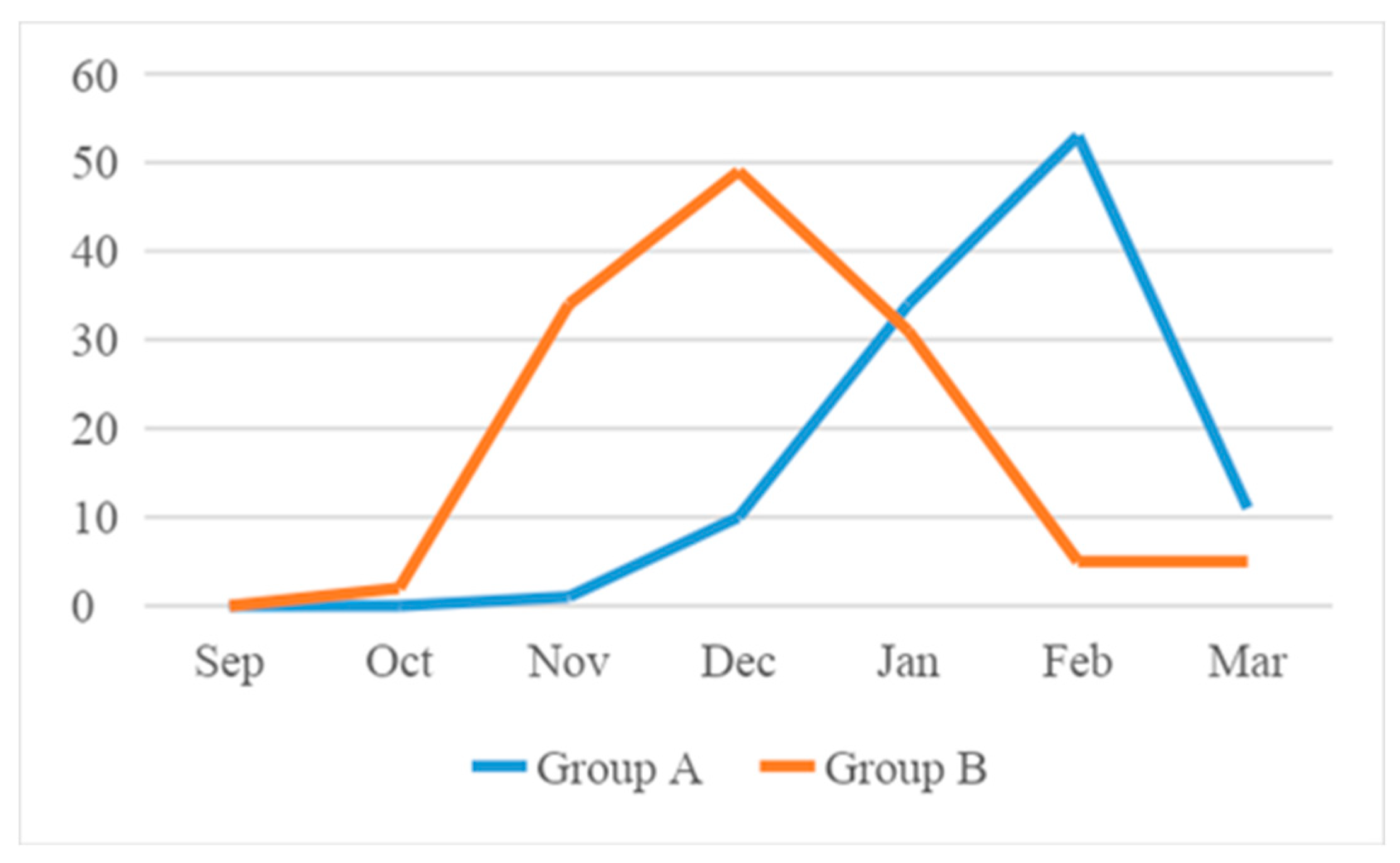
| Group A N=109 |
Group B N=128 |
P value | |
|---|---|---|---|
| September | 0 (0%) | 0 (0%) | <0.0001 |
| October | 0 (0%) | 2 (2%) | |
| November | 1 ( 1%) | 36 (28%) | |
| December | 10 (9%) | 49 (38%) | |
| January | 34 (31%) | 31 (24%) | |
| February | 53 (49%) | 5 (4%) | |
| March | 11 (10%) | 5 (4%) |
| Group A N=109 |
Group B N=128 |
P value | ||
|---|---|---|---|---|
| Gender | Male | 56 (51%) | 78 (61%) | 0.14 |
| Female | 53 (49%) | 50 (39%) | ||
| Prematurity | Yes | 12 (11%) | 15 (12%) | 0.36 |
| No | 95 (87%) | 106 (83%) | ||
| Unknown | 2 (2%) | 7 (5%) | ||
| Months at diagnosis | <1 | 37 (34%) | 62 (48%) | 0.0012 |
| 1-3 | 52 (48%) | 30 (23%) | ||
| 4-6 | 14 (13%) | 22 (17%) | ||
| 6-12 | 6 (5%) | 14 (11%) | ||
| Weight at diagnosis | < 4000 g | 21 (19%) | 22 (17%) | 0.21 |
| 31 (28%) | 34 (26%) | |||
| >5000 g | 57 (52%) | 69 54%) | ||
| Feeding | Breast-feed | 63 (58%) | 84 (66%) | 0.059 |
| Artificial | 37 (34%) | 26 (20%) | ||
| Weaned baby | 7 (6%) | 13 (10%) | ||
| Comorbidity | Yes | 6 (5%) | 10 (8%) | 0.6 |
| No | 102 (93% | 118 (92%) | ||
| Fever | Yes | 45 (41%) | 31 (24%) | 0.0054 |
| No | 64 (59%) | 97 (76%) | ||
| Profilaxed with Palivizumab | 0 (0%) | 1 (0,78%) | 1 | |
| Group A N=109 |
Group B N=128 |
P value | |||
|---|---|---|---|---|---|
| CRP high level (mg/dL) | 1.98 (0-63.5) | 1.19 (0-60.3) | 0.039 | ||
| Chest X-rays (number) | Yes | 23 (21%) | 19 (15%) | 0.23 | |
| No | 86 (79%) | 109 (85%) | |||
| Chest X-rays (pathologic results) | 13 (12%) | 10 (8%) | 0.27 | ||
| pCO2 higher level (mmHg) | 46 (28,2-64,1) | 48 (31,7-74) | 1 | ||
| Low-flow Oxygen | Yes | 64 (59%) | 79 (62%) | 0.69 | |
| No | 45 (41%) | 49 (38%) | |||
| Low-flow Oxygen days | 3 (0-8) | 3 (0-9) | 0.76 | ||
| High-flow Oxygen | Yes | 29 (27%) | 33 (26%) | 1 | |
| No | 80 (73%) | 94 (73%) | |||
| High-flow Oxygen days | 4 (1-8) | 5 (1-11) | 0.38 | ||
| Fraction of inspired Oxygen % | 35 (21-50) | 34 (25-65) | 0.56 | ||
| Areosolized drugs | Yes | 96 (88%) | 122 (95%) | 0.054 | |
| No | 13 (12%) | 6 (5%) | |||
| Antibiotics | Yes | 42 (38%) | 24 (19%) | 0.00082 | |
| No | 67 (61%) | 104 (81%) | |||
| Steroids | Yes | 13 (12%) | 17 (13%) | 0.84 | |
| No | 96 (88%) | 111 (87%) | |||
| Hydration IV | Yes | 32 (29%) | 23 (18%) | 0.045 | |
| No | 77 (71%) | 105 (82%) | |||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




