Submitted:
16 December 2023
Posted:
18 December 2023
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
3. Results
3.1. Results
3.2. Case Illustrations
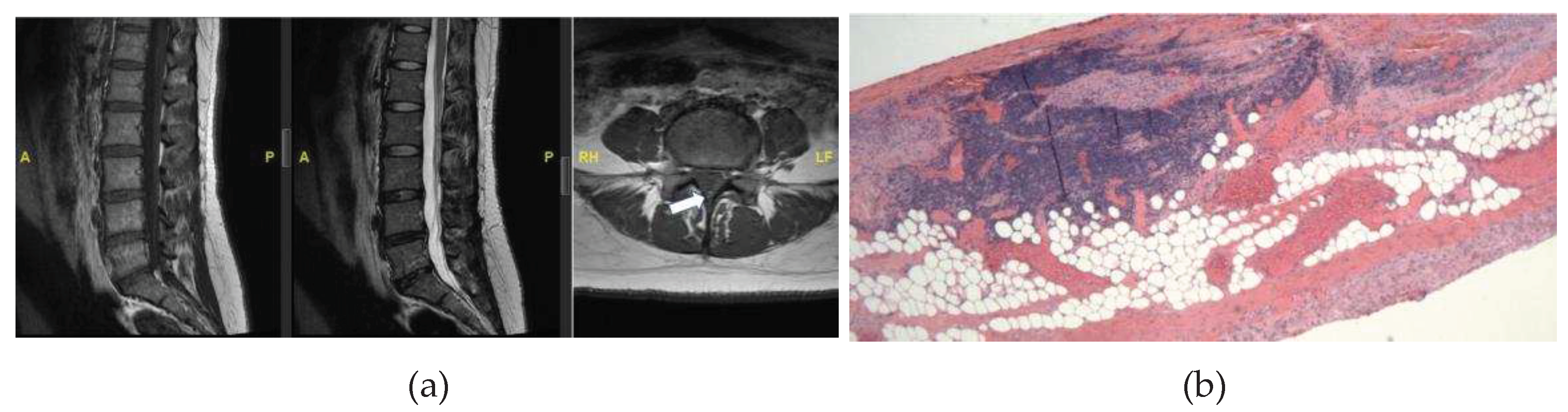
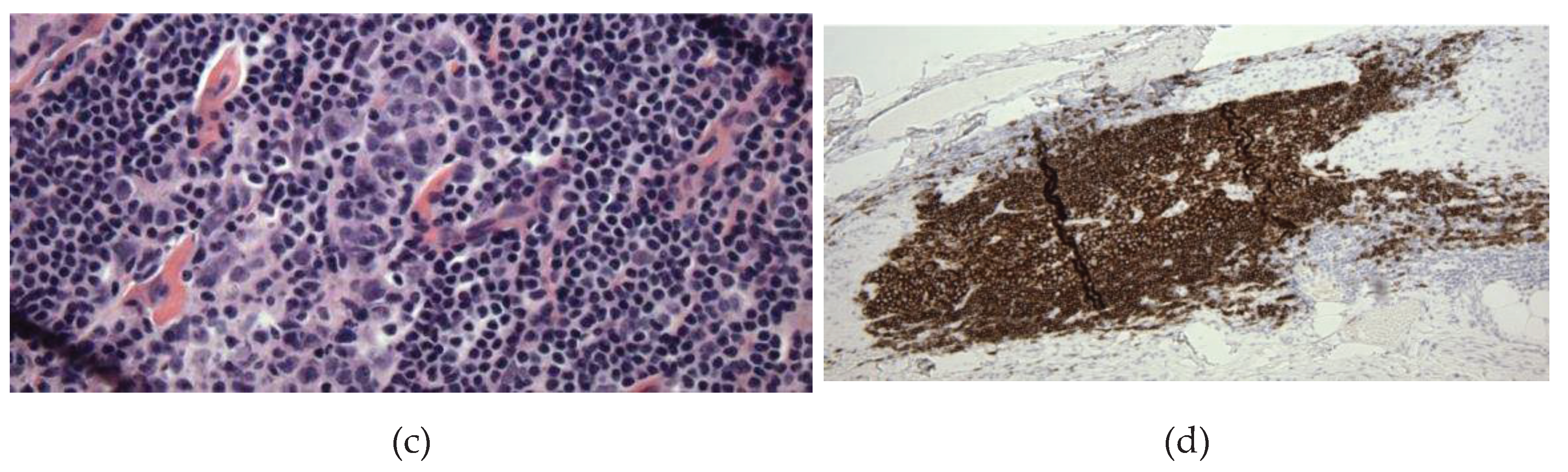
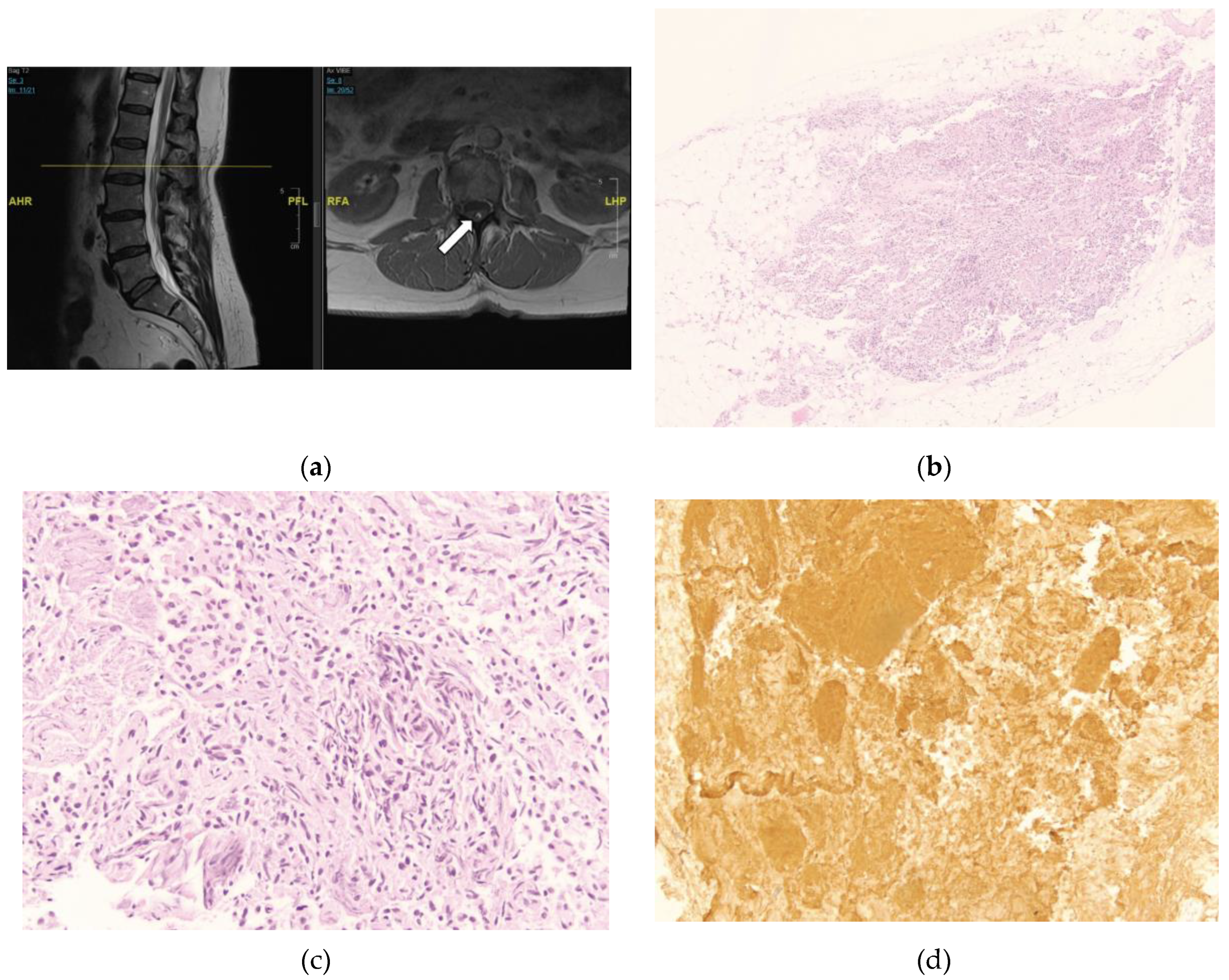
3.2.1. Case #1: Lymphoid Proliferation Suggestive of a Secondary Lymph Follicle
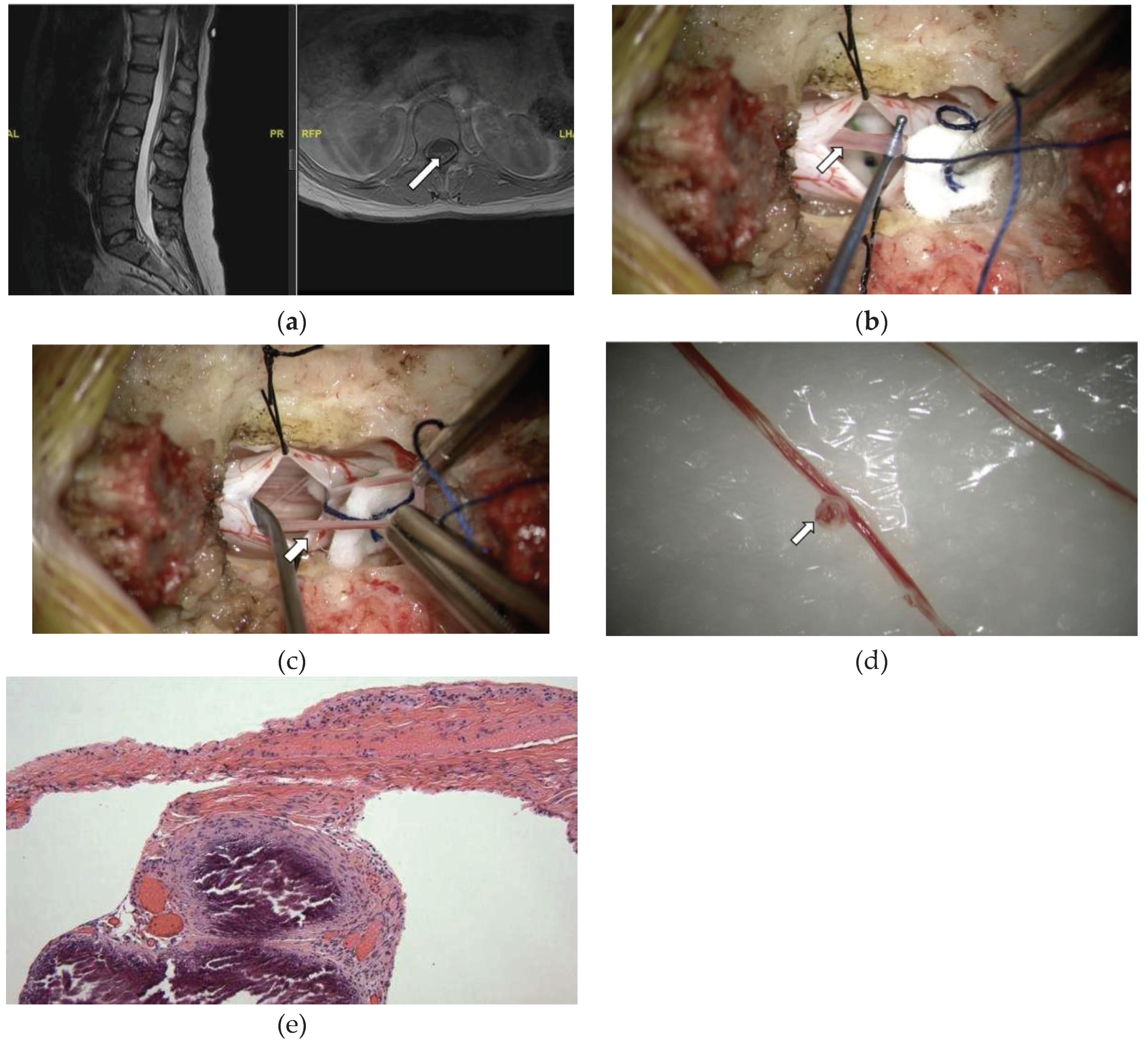
3.2.2. Case #2: Vascularity
3.2.3. Case #3: Ependymal Cell Proliferation
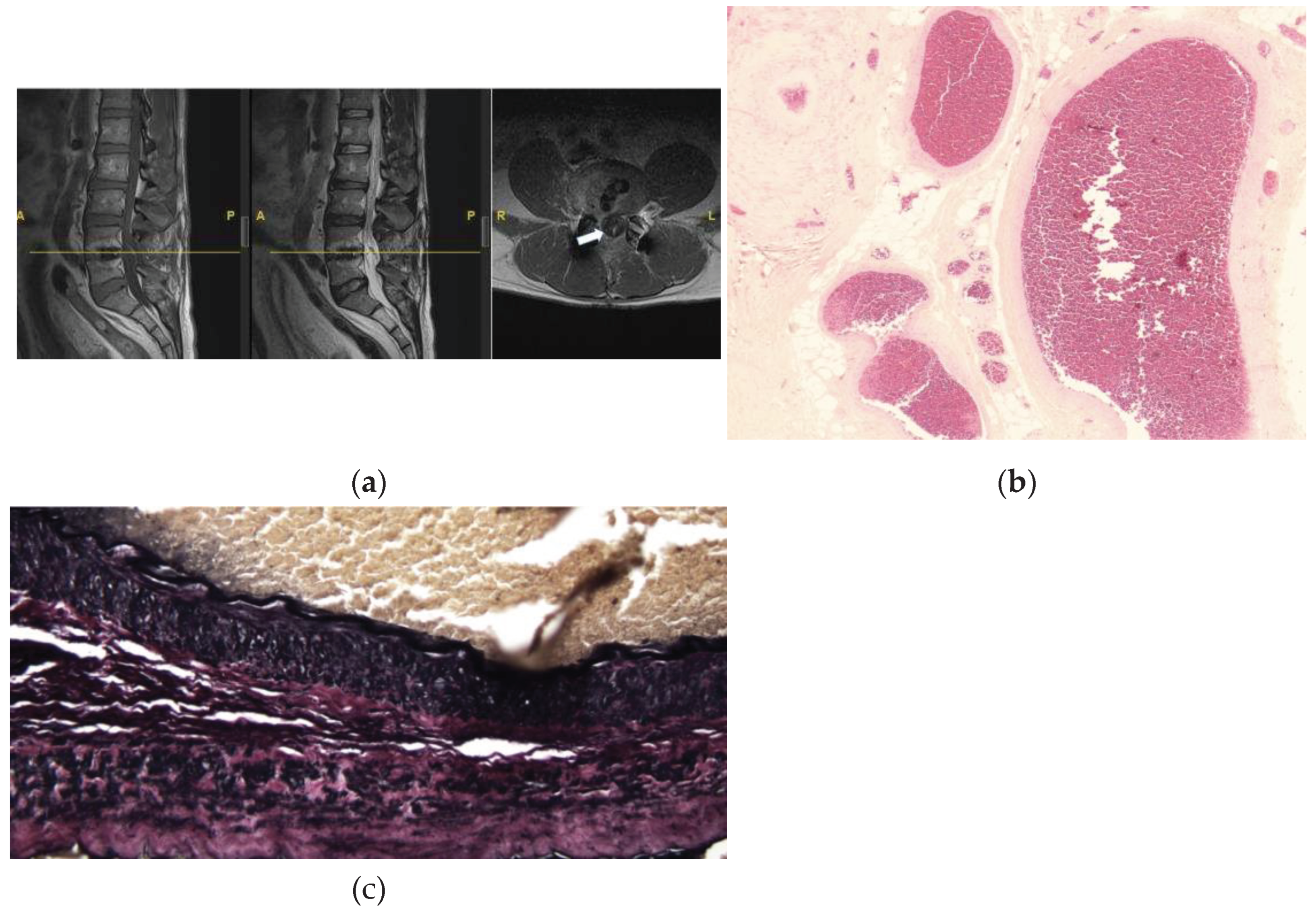
3.2.4. Case #4: Focal Calcifications
4. Discussion
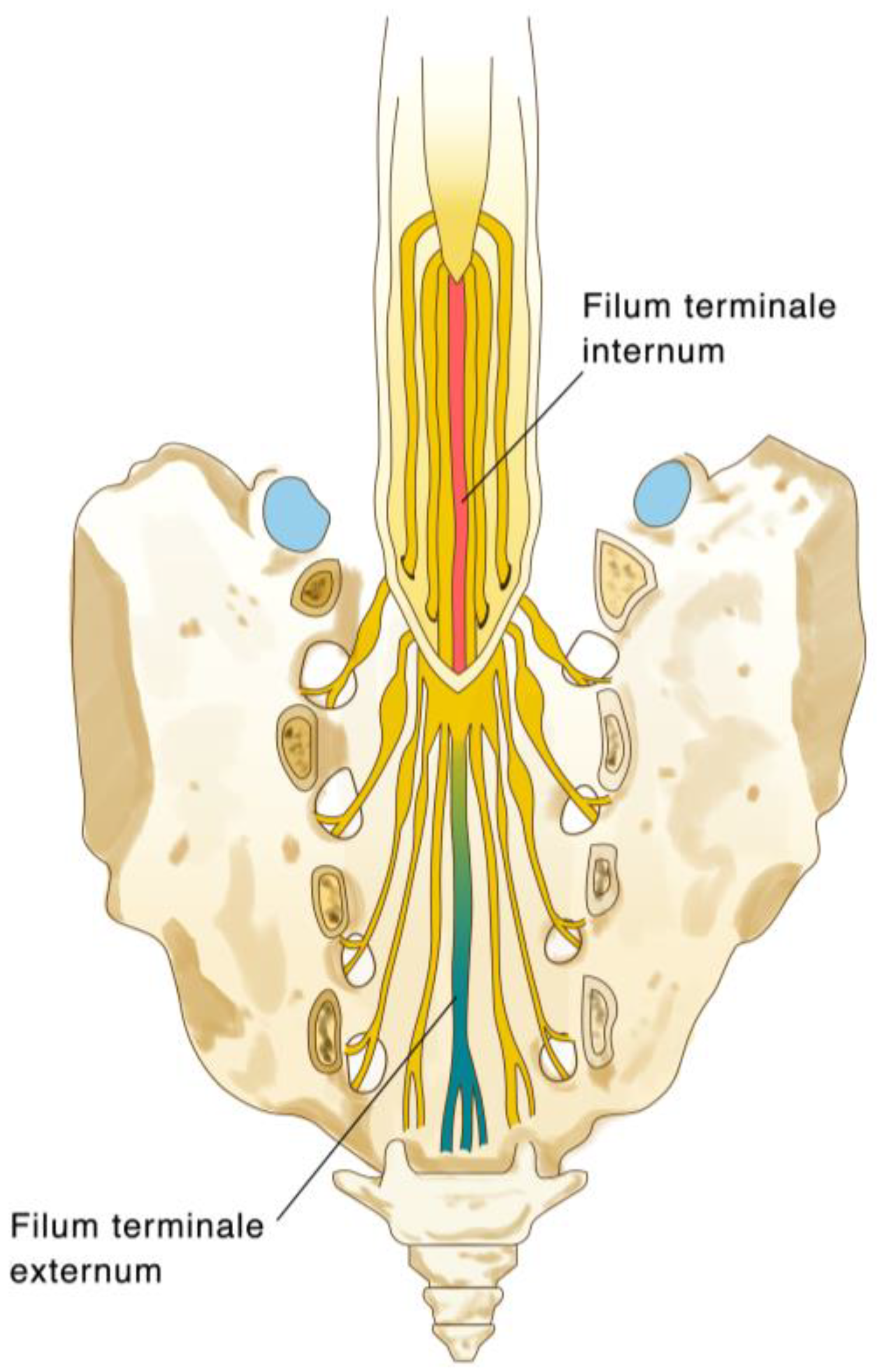
4.1. The Implication of Peripheral Nerves and Fat within the FT
4.2. Ependymal Proliferation and Vascularity within the FT
4.3. Inflammatory Cells and Calcifications
4.4. Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Acknowledgments
Conflicts of Interest
References
- Pinto, F.C.G.; Fontes, R.B. de V.; Leonhardt, M. de C.; Amodio, D.T.; Porro, F.F.; Machado, J. Anatomic Study of the Filum Terminale and Its Correlations with the Tethered Cord Syndrome. Neurosurgery 2002, 51, 725–729; discussion 729-30.
- De Vloo, P.; Monea, A.G.; Sciot, R.; van Loon, J.; Van Calenbergh, F. The Filum Terminale: A Cadaver Study of Anatomy, Histology, and Elastic Properties. World Neurosurg. 2016, 90, 565-573.e1. [CrossRef]
- Nasr, A.Y.; Hussein, A.M.; Zaghloul, S.A. Morphometric Parameters and Histological Study of the Filum Terminale of Adult Human Cadavers and Magnetic Resonance Images. Folia Morphol. 2018, 77, 609–619. [CrossRef]
- Klinge, P.M.; Srivastava, V.; McElroy, A.; Leary, O.P.; Ahmed, Z.; Donahue, J.E.; Brinker, T.; De Vloo, P.; Gokaslan, Z.L. Diseased Filum Terminale as a Cause of Tethered Cord Syndrome in Ehlers-Danlos Syndrome: Histopathology, Biomechanics, Clinical Presentation, and Outcome of Filum Excision. World Neurosurg. 2022, 162, e492–e502. [CrossRef]
- O’Connor, K.P.; Smitherman, A.D.; Milton, C.K.; Palejwala, A.H.; Lu, V.M.; Johnston, S.E.; Homburg, H.; Zhao, D.; Martin, M.D. Surgical Treatment of Tethered Cord Syndrome in Adults: A Systematic Review and Meta-Analysis. World Neurosurg. 2020, 137, e221–e241. [CrossRef]
- Leary, O.P.; Hagan, M.; Sullivan, P.L.Z.; McElroy, A.; Syed, S.; Liu, D.D.; Donahue, J.E.; Scarfo, K.-A.; Carayannopoulos, A.G.; Li, J.; et al. Adult-Onset Tethered Cord Syndrome: Case Series from a Comprehensive Interdisciplinary Spine Center. Interdiscip. Neurosurg. 2023, 33, 101773. [CrossRef]
- Liu, F.-Y.; Li, J.-F.; Guan, X.; Luo, X.-F.; Wang, Z.-L.; Dang, Q.-H. SEM Study on Filum Terminale with Tethered Cord Syndrome. Childs Nerv. Syst. ChNS Off. J. Int. Soc. Pediatr. Neurosurg. 2011, 27, 2141–2144. [CrossRef]
- Klinge, P.M.; McElroy, A.; Leary, O.P.; Donahue, J.E.; Mumford, A.; Brinker, T.; Gokaslan, Z.L. Not Just an Anchor: The Human Filum Terminale Contains Stretch Sensitive and Nociceptive Nerve Endings and Responds to Electrical Stimulation With Paraspinal Muscle Activation. Neurosurgery 2022, 91, 618–624. [CrossRef]
- Gupta, P.; Kumar, A.; Kumar, A.; Goel, S. Congenital Spinal Cord Anomalies: A Pictorial Review. Curr. Probl. Diagn. Radiol. 2013, 42, 57–66. [CrossRef]
- Selçuki, M.; Vatansever, S.; Inan, S.; Erdemli, E.; Bağdatoğlu, C.; Polat, A. Is a Filum Terminale with a Normal Appearance Really Normal? Childs Nerv. Syst. ChNS Off. J. Int. Soc. Pediatr. Neurosurg. 2003, 19, 3–10. [CrossRef]
- HARMEIER, J.W. THE NORMAL HISTOLOGY OF THE INTRADURAL FILUM TERMINALE. Arch. Neurol. Psychiatry 1933, 29, 308–316. [CrossRef]
- Pang, D.; Zovickian, J.; Moes, G.S. Retained Medullary Cord in Humans: Late Arrest of Secondary Neurulation. Neurosurgery 2011, 68, 1500–1519; discussion 1519. [CrossRef]
- Agarwalla, P.K.; Dunn, I.F.; Scott, R.M.; Smith, E.R. Tethered Cord Syndrome. Neurosurg. Clin. N. Am. 2007, 18, 531–547. [CrossRef]
- Jones, V.; Wykes, V.; Cohen, N.; Thompson, D.; Jacques, T.S. The Pathology of Lumbosacral Lipomas: Macroscopic and Microscopic Disparity Have Implications for Embryogenesis and Mode of Clinical Deterioration. Histopathology 2018, 72, 1136–1144. [CrossRef]
- Cools, M.J.; Al-Holou, W.N.; Stetler, W.R.J.; Wilson, T.J.; Muraszko, K.M.; Ibrahim, M.; La Marca, F.; Garton, H.J.L.; Maher, C.O. Filum Terminale Lipomas: Imaging Prevalence, Natural History, and Conus Position. J. Neurosurg. Pediatr. 2014, 13, 559–567. [CrossRef]
- Kural, C.; Guresci, S.; Simsek, G.G.; Arslan, E.; Tehli, O.; Solmaz, I.; Izci, Y. Histological Structure of Filum Terminale in Human Fetuses. J. Neurosurg. Pediatr. 2014, 13, 362–367. [CrossRef]
- Fontes, R.B.V.; Saad, F.; Soares, M.S.; de Oliveira, F.; Pinto, F.C.G.; Liberti, E.A. Ultrastructural Study of the Filum Terminale and Its Elastic Fibers. Neurosurgery 2006, 58, 978–984; discussion 978-984. [CrossRef]
- Yamada, S.; Knerium, D.S.; Mandybur, G.M.; Schultz, R.L.; Yamada, B.S. Pathophysiology of Tethered Cord Syndrome and Other Complex Factors. Neurol. Res. 2004, 26, 722–726. [CrossRef]
- Thompson, E.M.; Strong, M.J.; Warren, G.; Woltjer, R.L.; Selden, N.R. Clinical Significance of Imaging and Histological Characteristics of Filum Terminale in Tethered Cord Syndrome. J. Neurosurg. Pediatr. 2014, 13, 255–259. [CrossRef]
- McElroy, A.; Rashmir, A.; Manfredi, J.; Sledge, D.; Carr, E.; Stopa, E.; Klinge, P. Evaluation of the Structure of Myodural Bridges in an Equine Model of Ehlers-Danlos Syndromes. Sci. Rep. 2019, 9, 9978. [CrossRef]
- Abdulrazeq, H.; Shao, B.; Sastry, R.A.; Klinge, P.M. Microsurgical Approach for Resection of the Filum Terminale Internum in Tethered Cord Syndrome-a Case Demonstration of Technical Nuances and Vignettes. Acta Neurochir. (Wien) 2023. [CrossRef]
- Durdağ, E.; Börcek, P.B.; Öcal, Ö.; Börcek, A.Ö.; Emmez, H.; Baykaner, M.K. Pathological Evaluation of the Filum Terminale Tissue after Surgical Excision. Childs Nerv. Syst. ChNS Off. J. Int. Soc. Pediatr. Neurosurg. 2015, 31, 759–763. [CrossRef]
- Rafiee, F.; Mehan, W.A.; Rincon, S.; Rohatgi, S.; Rapalino, O.; Buch, K. Diagnostic Utility of 3D Gradient-Echo MR Imaging Sequences through the Filum Compared with Spin-Echo T1 in Children with Concern for Tethered Cord. AJNR Am. J. Neuroradiol. 2023, 44, 323–327. [CrossRef]
- Selden, N.R.; Nixon, R.R.; Skoog, S.R.; Lashley, D.B. Minimal Tethered Cord Syndrome Associated with Thickening of the Terminal Filum. J. Neurosurg. 2006, 105, 214–218. [CrossRef]
- Saker, E.; Henry, B.M.; Tomaszewski, K.A.; Loukas, M.; Iwanaga, J.; Oskouian, R.J.; Tubbs, R.S. The Filum Terminale Internum and Externum: A Comprehensive Review. J. Clin. Neurosci. Off. J. Neurosurg. Soc. Australas. 2017, 40, 6–13. [CrossRef]
- Picart, T.; Barritault, M.; Simon, E.; Robinson, P.; Barrey, C.; Meyronet, D.; Mertens, P. Anatomical and Histological Analysis of a Complex Structure Too Long Considered a Simple Ligament: The Filum Terminale. World Neurosurg. 2019, 129, e464–e471. [CrossRef]
- Koeller, K.K.; Rosenblum, R.S.; Morrison, A.L. Neoplasms of the Spinal Cord and Filum Terminale: Radiologic-Pathologic Correlation. Radiogr. Rev. Publ. Radiol. Soc. N. Am. Inc 2000, 20, 1721–1749. [CrossRef]
- Djindjian, M.; Ribeiro, A.; Ortega, E.; Gaston, A.; Poirier, J. The Normal Vascularization of the Intradural Filum Terminale in Man. Surg. Radiol. Anat. SRA 1988, 10, 201–209. [CrossRef]
- Selçuki, M.; Coşkun, K. Management of Tight Filum Terminale Syndrome with Special Emphasis on Normal Level Conus Medullaris (NLCM). Surg. Neurol. 1998, 50, 318–322; discussion 322. [CrossRef]
- Filippidis, A.S.; Kalani, M.Y.; Theodore, N.; Rekate, H.L. Spinal Cord Traction, Vascular Compromise, Hypoxia, and Metabolic Derangements in the Pathophysiology of Tethered Cord Syndrome. Neurosurg. Focus 2010, 29, E9. [CrossRef]
- Selden, N.R. Occult Tethered Cord Syndrome: The Case for Surgery. J. Neurosurg. 2006, 104, 302–304. [CrossRef]
- Takai, K.; Komori, T.; Taniguchi, M. Angioarchitecture of Filum Terminale Arteriovenous Fistulas: Relationship with a Tethered Spinal Cord. World Neurosurg. 2019, 122, e795–e804. [CrossRef]
- Giordan, E.; Brinjikji, W.; Ciceri, E.; Lanzino, G. Arteriovenous Fistulae of the Filum Terminale. J. Neurointerventional Surg. 2018, 10, 191–197. [CrossRef]
- Ding, D.; Law, A.J.; Scotter, J.; Brew, S. Lumbar Disc Herniation Exacerbating Venous Hypertension from a Spinal Perimedullary Arteriovenous Fistula of the Filum Terminale. J. Neurol. Sci. 2016, 369, 276–277. [CrossRef]
- Witiw, C.D.; Fallah, A.; Radovanovic, I.; Wallace, M.C. Sacral Intradural Arteriovenous Fistula Treated Indirectly by Transection of the Filum Terminale: Technical Case Report. Neurosurgery 2011, 69, E780-784; discussion E784. [CrossRef]
- Flores, B.C.; Klinger, D.R.; White, J.A.; Batjer, H.H. Spinal Vascular Malformations: Treatment Strategies and Outcome. Neurosurg. Rev. 2017, 40, 15–28. [CrossRef]
- Troude, L.J.; Melot, A.; Brunel, H.; Roche, P.-H. Arteriovenous Malformation of the Filum Terminale: An Exceptional Case. J. Neurosurg. 2016, 124, 1712–1715. [CrossRef]
- Baehring, J.M.; Damek, D.; Martin, E.C.; Betensky, R.A.; Hochberg, F.H. Neurolymphomatosis. Neuro-Oncol. 2003, 5, 104–115. [CrossRef]
- Alazawi, S.; Elomri, H.; Taha, R.; Bakr, M.; Abdelhamid, M.T.; Szabados, L.; Yassin, M.; Sabah, H.E.; Aboudi, K.; Ellahie, A.; et al. Neurolymphomatosis of the Median Nerve, Optic Nerve, L4 Spinal Nerve Root and Cauda Equina in Patients with B-Cell Malignancies: A Case Series. J. Med. Case Reports 2021, 15, 133. [CrossRef]
- Seneviratne, S.L.; Maitland, A.; Afrin, L. Mast Cell Disorders in Ehlers-Danlos Syndrome. Am. J. Med. Genet. C Semin. Med. Genet. 2017, 175, 226–236. [CrossRef]
- Henderson, F.C.S.; Austin, C.; Benzel, E.; Bolognese, P.; Ellenbogen, R.; Francomano, C.A.; Ireton, C.; Klinge, P.; Koby, M.; Long, D.; et al. Neurological and Spinal Manifestations of the Ehlers-Danlos Syndromes. Am. J. Med. Genet. C Semin. Med. Genet. 2017, 175, 195–211. [CrossRef]
- Uhthoff, H.K.; Loehr, J.W. Calcific Tendinopathy of the Rotator Cuff: Pathogenesis, Diagnosis, and Management. J. Am. Acad. Orthop. Surg. 1997, 5, 183–191. [CrossRef]
- Faure, A.; Khalfallah, M.; Perrouin-Verbe, B.; Caillon, F.; Deschamps, C.; Bord, E.; Mathe, J.-F.; Robert, R. Arachnoiditis Ossificans of the Cauda Equina. Case Report and Review of the Literature. J. Neurosurg. 2002, 97, 239–243. [CrossRef]
- Benyaich, Z.; Laghmari, M.; Ait Benali, S. Arachnoiditis Ossificans of the Lumbar Spine: A Rare Cause of Progressive Cauda Equina Syndrome. World Neurosurg. 2021, 148, 116–117. [CrossRef]
| Characteristic (Total N = 288) | N (%) or Mean (SD) |
|---|---|
| Age at Surgery (years) | 29.0 (± 21.3) |
| Adult Patients (>18 years) | 170 (59.0%) |
| Pediatric Patients (10–18 years) | 41 (14.2%) |
| Pediatric Patients (<10 years) | 77 (26.8%) |
| Gender (Female) | 202 (70.1%) |
| Diagnosis with Tethered Cord Syndrome | 288 (100%) |
| Mean # of TCS Triad Symptoms | 2.0 (± 1.2) |
| Back and/or Leg Pain | 203 (70.5%) |
| Neurological Signs & Symptoms Urological Symptoms Patients at 3-month follow-up Back and/or Leg Pain Neurological Signs & Symptoms Urological Symptoms Patients at 12-month follow-up Back and/or Leg Pain Neurological Signs & Symptoms Urological Symptoms |
212 (73.6%) 182 (63.2%) 185 (64.2%) 116 (62.7%) 68. (26.8%) 64 (34.6%) 163 (56.6%) 59 (63.2%) 84 (51.5%) 80 (49.1%) |
| Histopathologic Finding (Total N = 288) | N (%) | Age Distribution (# of Patients, Percentage Out of Entire Sample) | ||
|---|---|---|---|---|
| Pediatric (<10 years) | PEDIATRIC (10-18 years) | Adult Patients (>18 years) | ||
| Peripheral Nerves | 281 (97.6%) | 81 (28.12%) | 40 (13.89%) | 160 (55.56%) |
| Ependymal Cells | 204 (70.8%) | 49 (17.01%) | 30 (10.42%) | 125 (43.4%) |
| Fatty infiltration | 118 (41%) | 47 (16.32%) | 16 (5.56%) | 55 (19.1%) |
| Ganglion Cells | 111 (38.5%) | 29 (10.07%) | 17 (5.9%) | 65 (22.57%) |
| Neuropil | 44 (15.3%) | 17 (5.9%) | 2 (0.69%) | 25 (8.68%) |
| Vascular findings | 36 (12.5%) | 11 (3.82%) | 4 (1.39%) | 21 (7.29%) |
| Meningothelial Cells | 14 (4.9%) | 5 (1.74%) | 1 (0.35%) | 8 (2.78%) |
| Inflammatory cells | 11 (3.8%) | 2 (0.69%) | 1 (0.35%) | 8 (2.78%) |
| Elastin Fibers | 9 (3.1%) | 4 (1.39%) | 1 (0.35%) | 4 (1.39%) |
| Corpora Amylacea | 6 (2.1%) | 0 (0.0%) | 0 (0.0%) | 6 (2.08%) |
| Psammoma bodies | 3 (1.0%) | 0 (0.0%) | 0 (0.0%) | 3 (1.04%) |
| Rosenthal fibers | 2 (0.07%) | 0 (0.0%) | 0 (0.0%) | 2 (0.69%) |
| Melanocytes | 1 (0.03%) | 1 (0.35%) | 0 (0.0%) | 0 (0.0%) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




