Submitted:
05 December 2023
Posted:
07 December 2023
Read the latest preprint version here
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Protocol
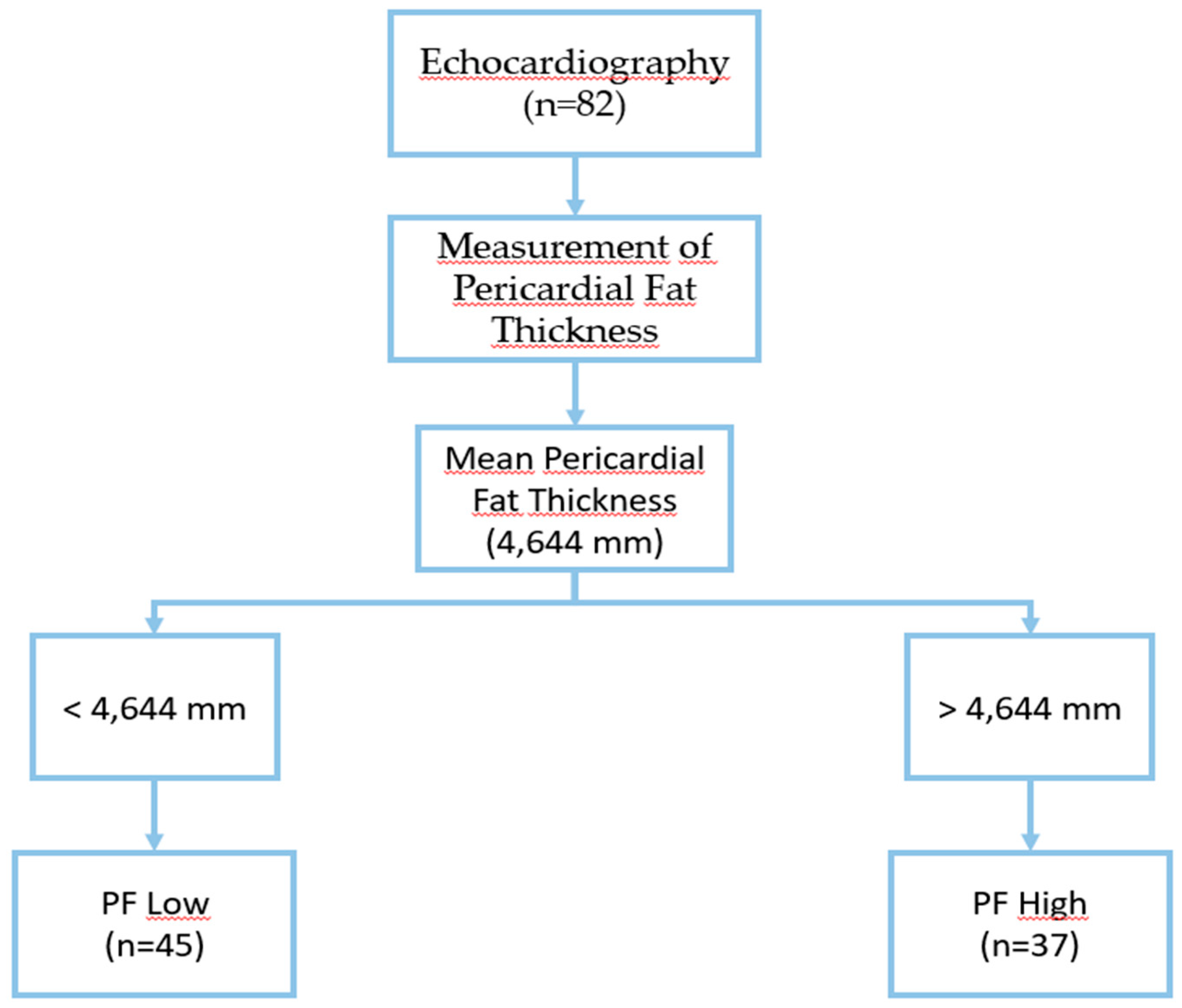
2.3. Study Variables
2.4. Statistical
2.5. Ethic
3. Results
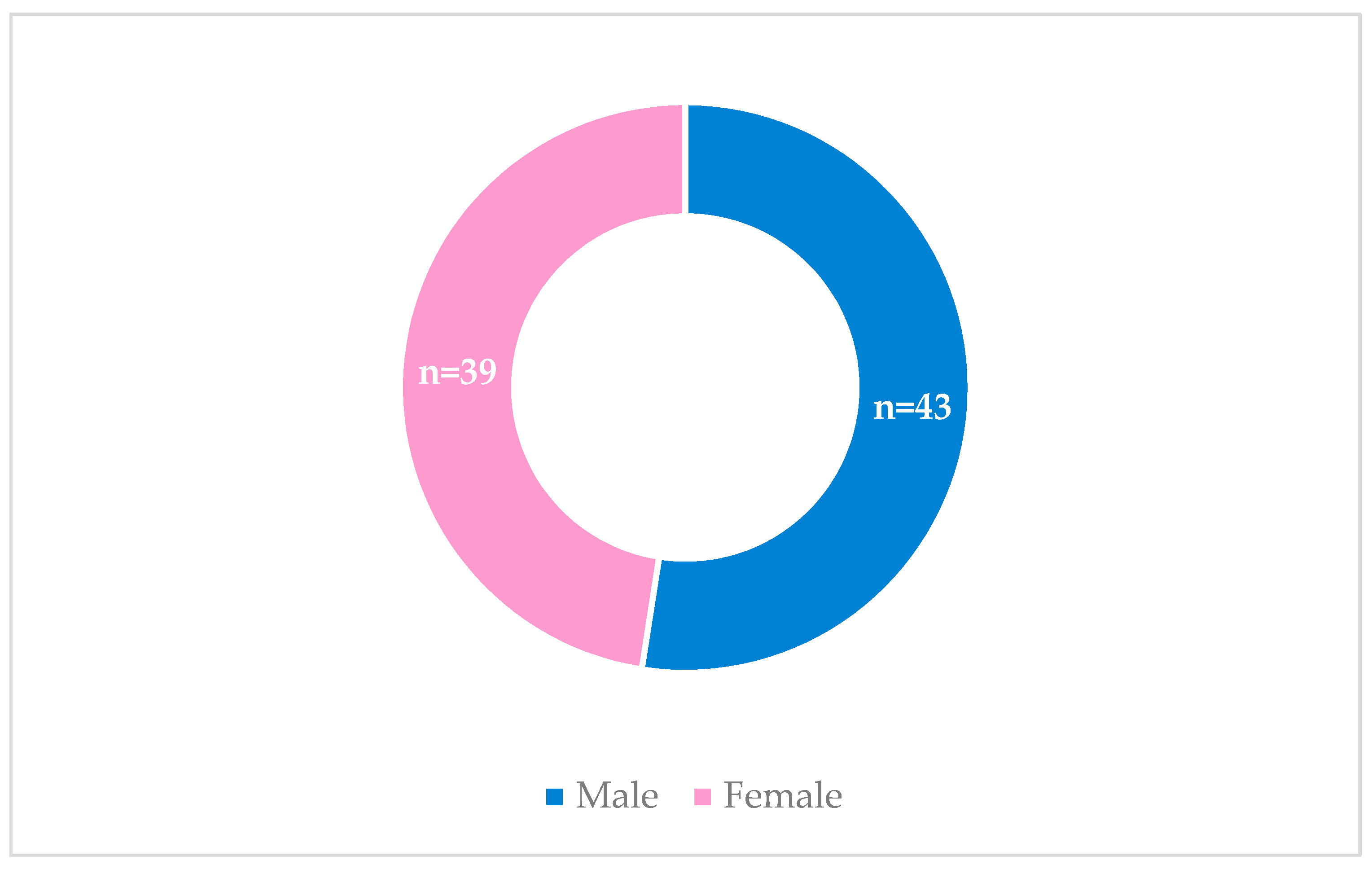
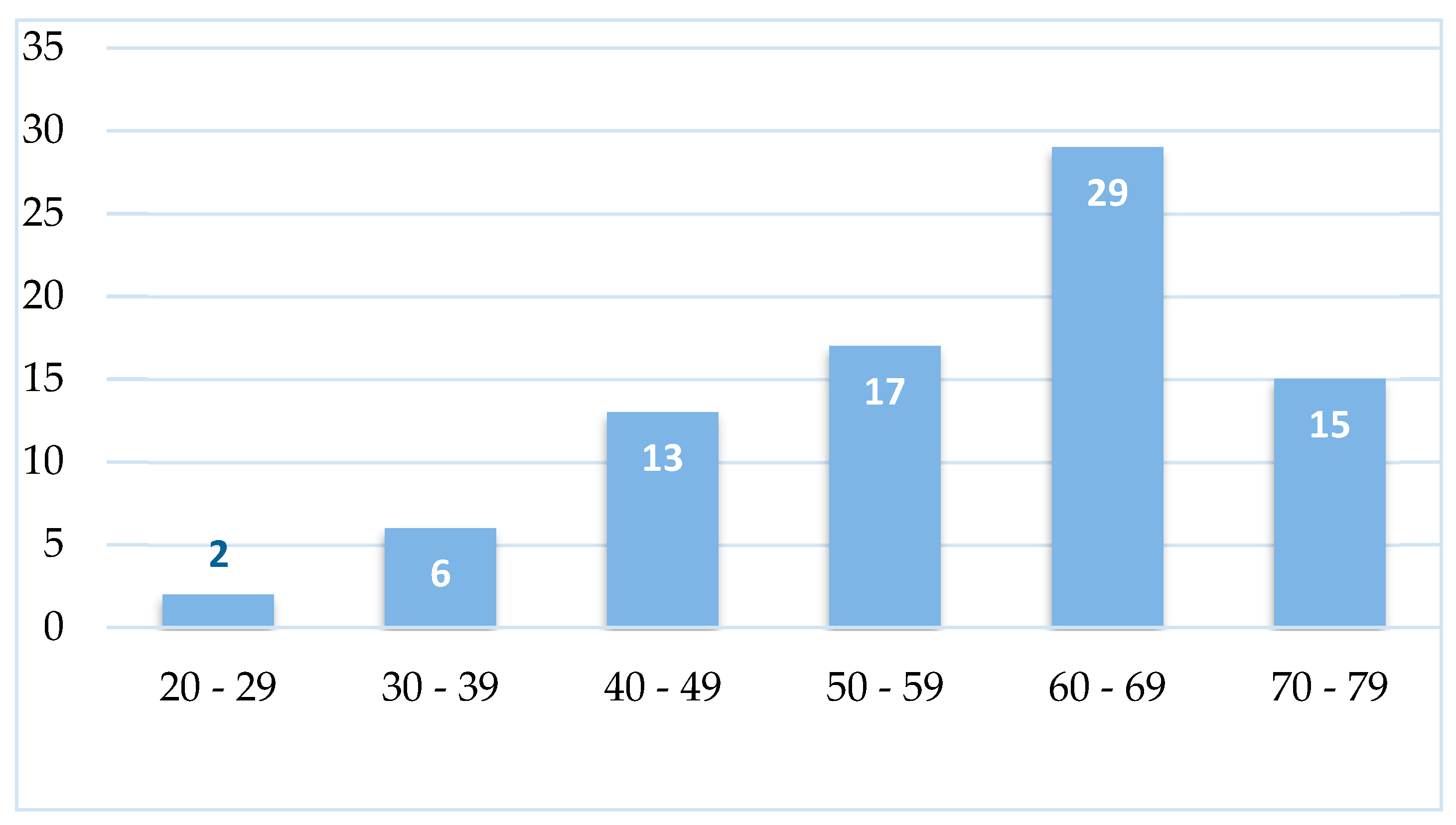
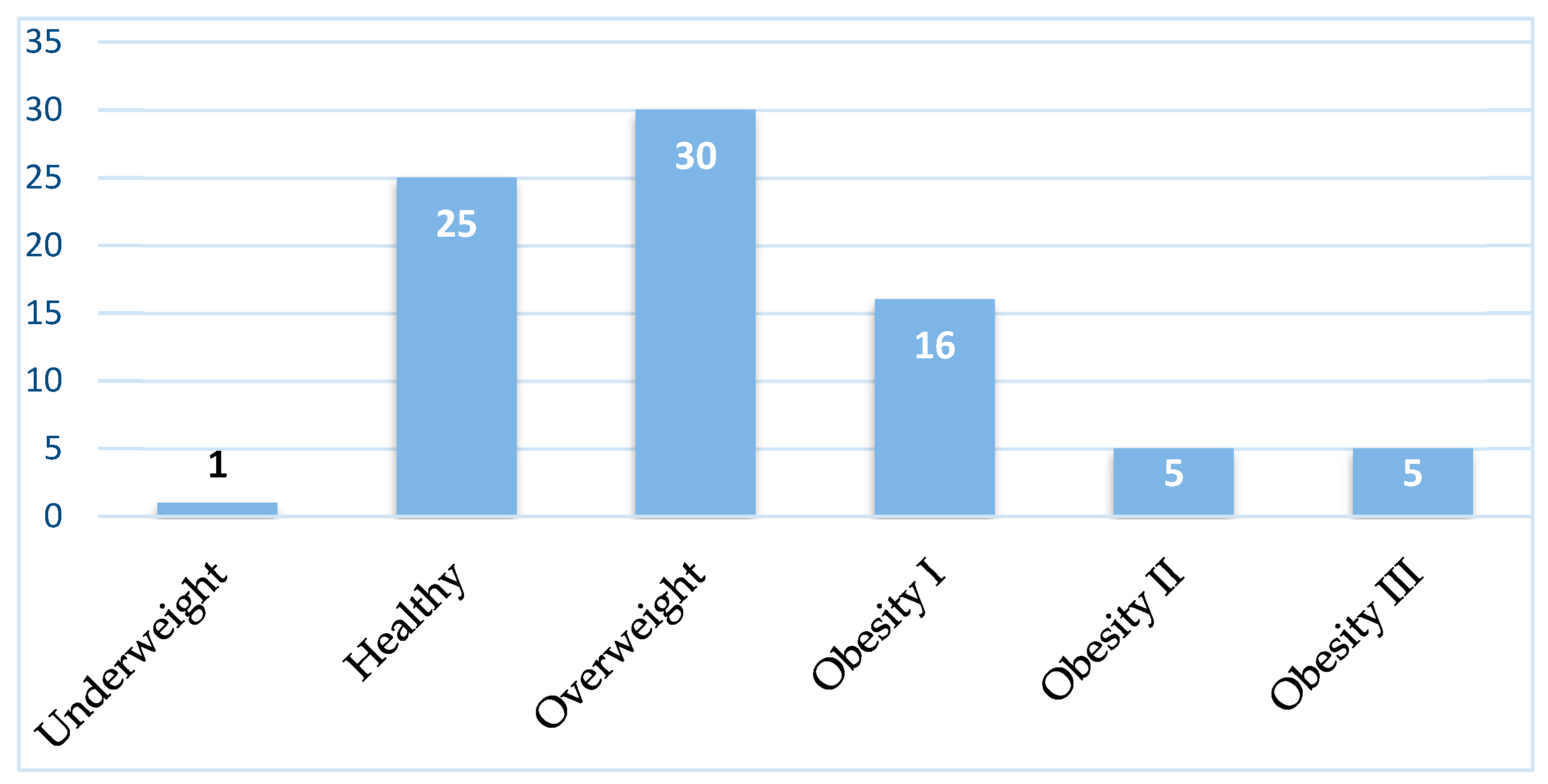
3.1. Abdominal Perimeter and Pericardial and Epicardial Fat
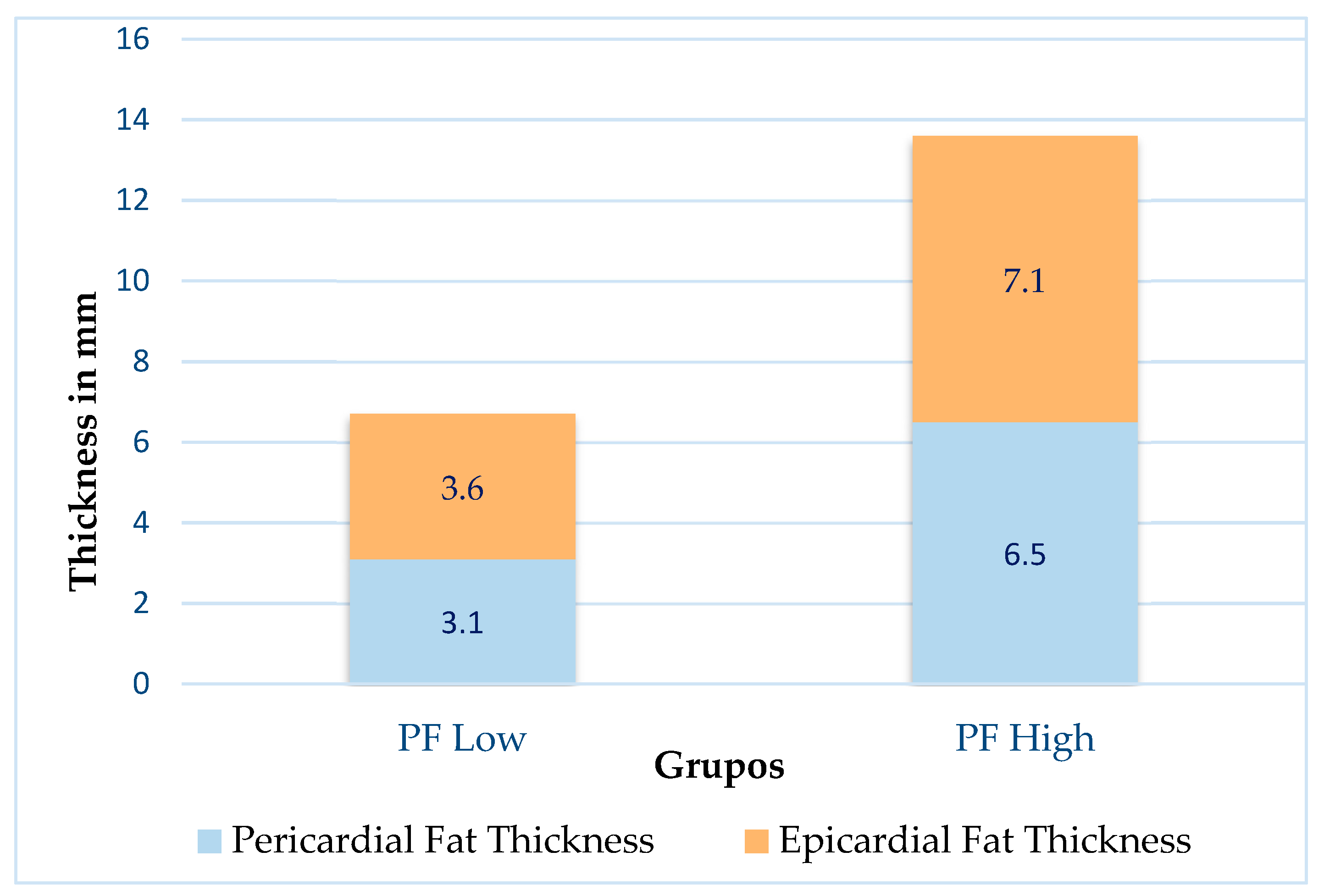
3.2. Association between Abdominal Circumference and Age Group
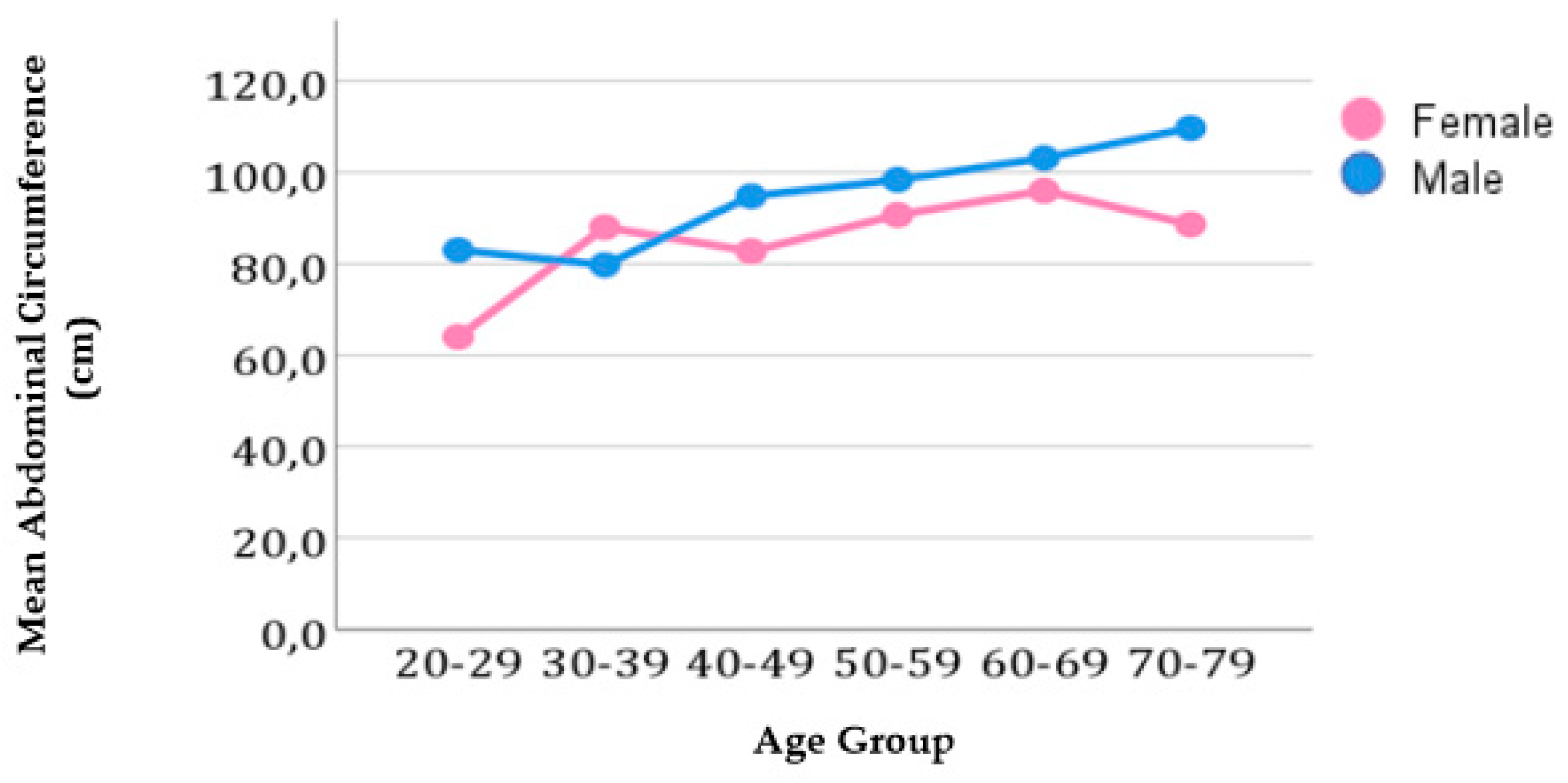
3.3. Relationship between Pericardial Fat and Abdominal Circumference
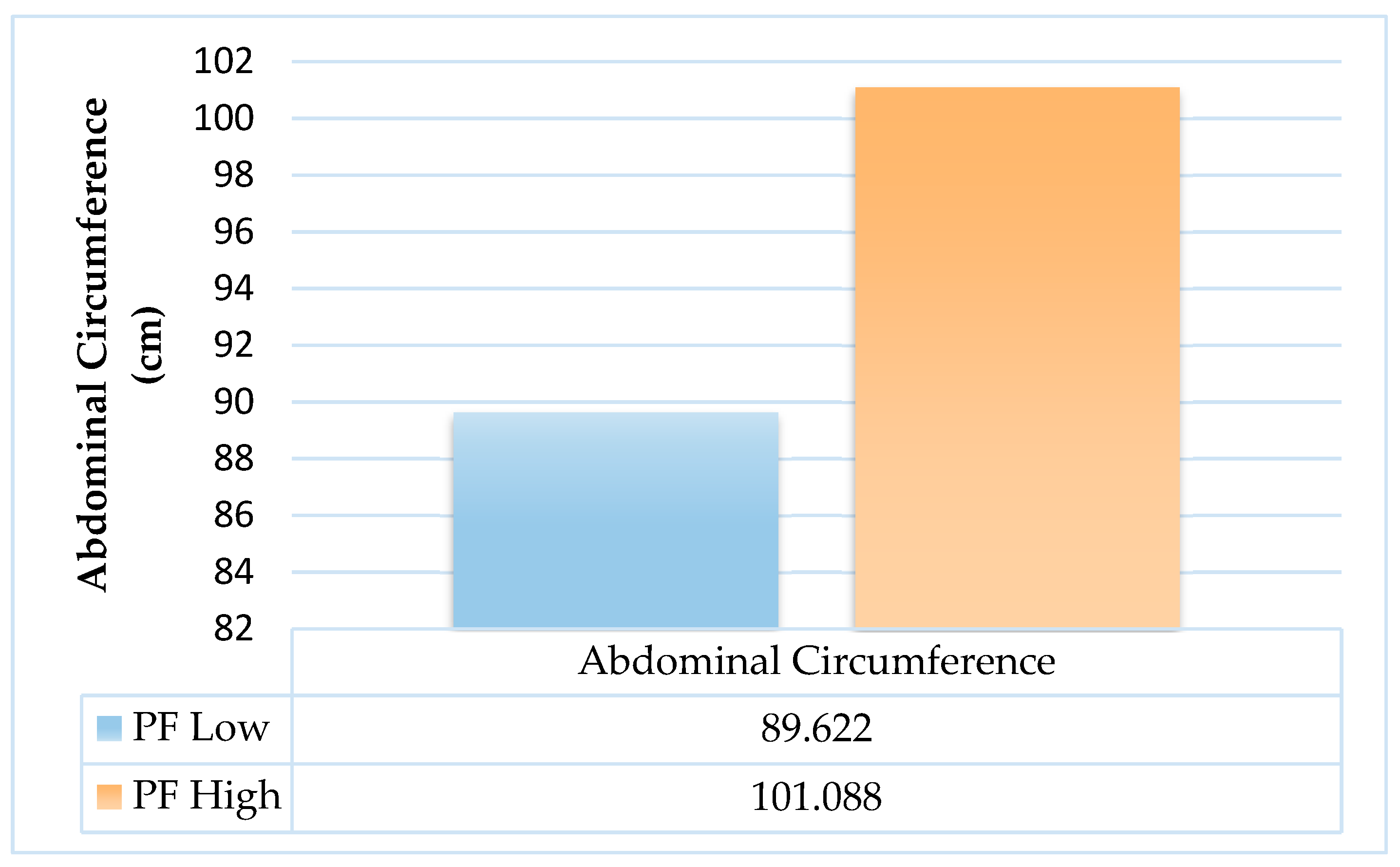
3.4. Assessment of echocardiographic variables and pericardial fat
3.5. Association between Abdominal Circumference and Pericardial and Epicardial Fat Thickness
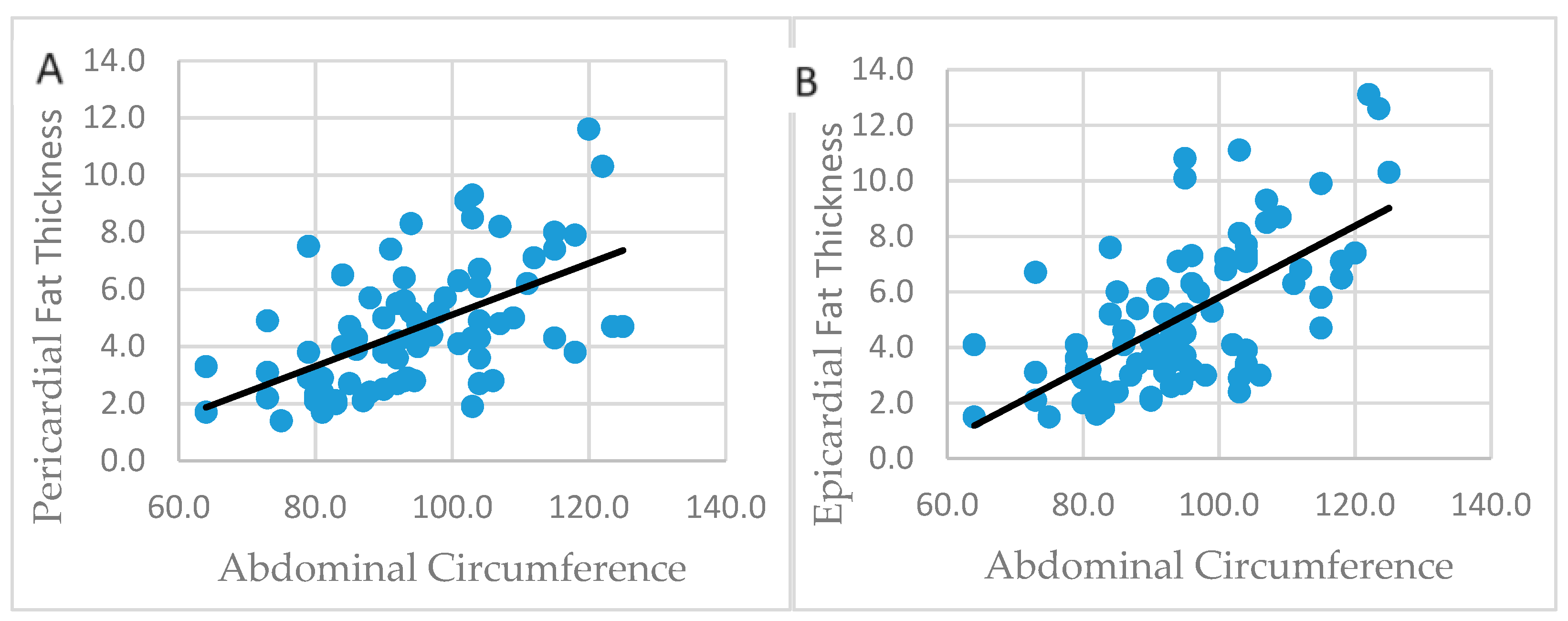
3.6. Association of echocardiographic variables with pericardial fat VS epicardial fat
3.7. Assessment between pericardial fat and the diagnosis of DD
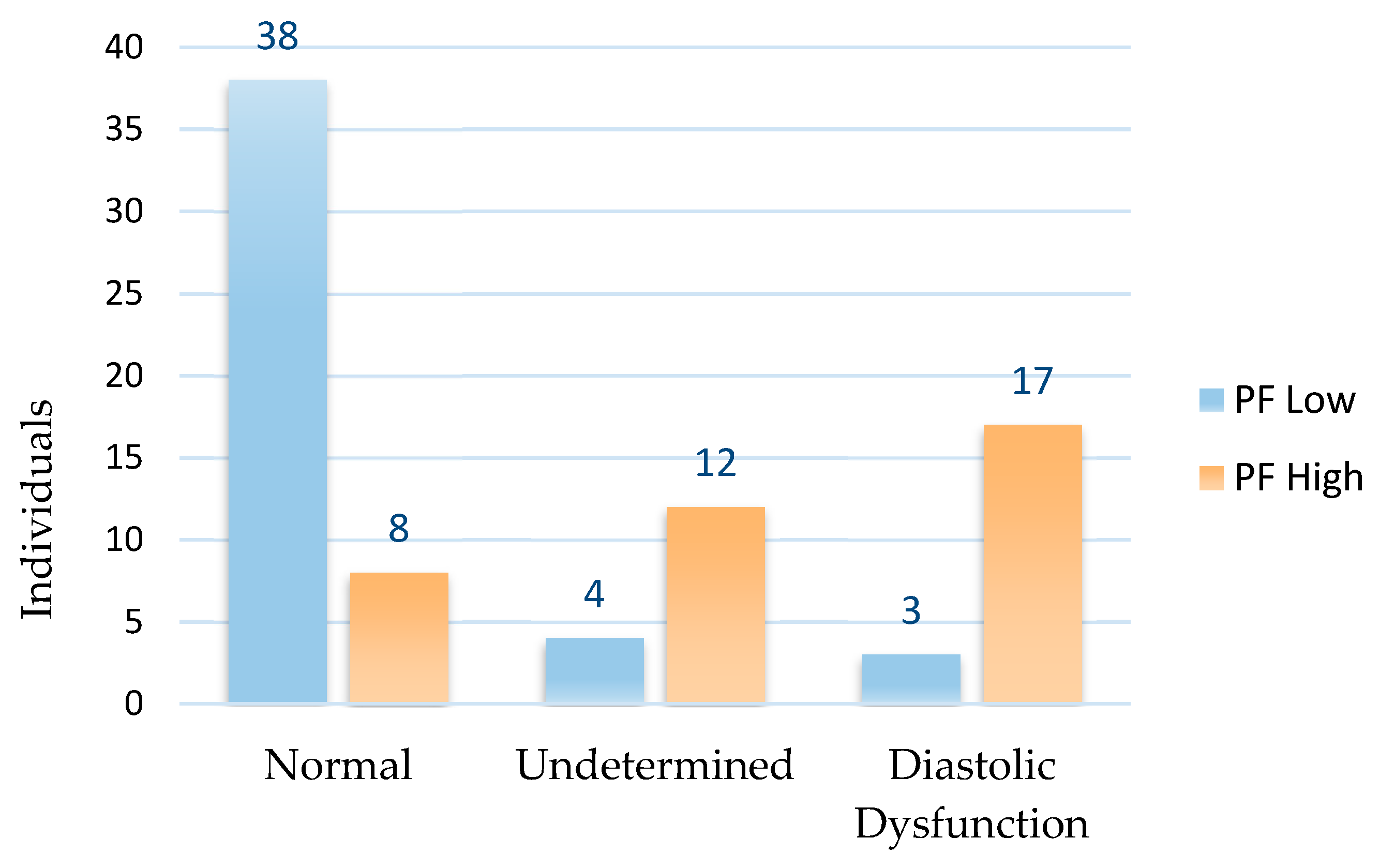
4. Discussion
4.1. Sample characterization
4.2. Association of abdominal circumference with age in male and female
4.3. Relationship between pericardial fat and abdominal Circumference
4.4. Assessment of echocardiographic variables and pericardial fat
4.5. Association of echocardiographic variables with pericardial fat VS epicardial fat
4.6. Assessment between pericardial fat and the diagnosis of DD
4.7. Limitations
5. Conclusions
References
- De Wit-Verheggen, V.H.W.; Altintas, S.; Spee, R.J.M.; Mihl, C.; Van Kuijk, S.M.J.; Wildberger, J.E.; et al. Pericardial fat and its influence on cardiac diastolic function. Cardiovasc Diabetol. 2020, 17, 19. [Google Scholar] [CrossRef] [PubMed]
- Ma, W.; Zhang, B.; Yang, Y.; Qi, L.; Zhou, J.; Li, M.; et al. Association of epicardial fat thickness with left ventricular diastolic function parameters in a community population. BMC Cardiovasc Disord. 2021, 1, 21. [Google Scholar] [CrossRef] [PubMed]
- Kitterer, D.; Latus, J.; Henes, J.; Birkmeier, S.; Backes, M.; Braun, N.; et al. Impact of long-term steroid therapy on epicardial and pericardial fat deposition: A cardiac MRI study. Cardiovasc Diabetol. 2015, 30, 14. [Google Scholar] [CrossRef] [PubMed]
- Tekin, I.; Edem, E. Association of epicardial fat tissue with coronary artery disease and left ventricle diastolic function indicators. Medical Science Monitor. 2018, 24, 6367–74. [Google Scholar] [CrossRef] [PubMed]
- Kenchaiah, S.; Ding, J.; Carr, J.J.; Allison, M.A.; Budoff, M.J.; Tracy, R.P.; et al. Pericardial Fat and the Risk of Heart Failure. J Am Coll Cardiol. 2021, 77, 2638–52. [Google Scholar] [CrossRef] [PubMed]
- Larsen, B.A.; Laughlin, G.A.; Saad, S.D.; Barrett-Connor, E.; Allison, M.A.; Wassel, C.L. Pericardial fat is associated with all-cause mortality but not incident CVD: The Rancho Bernardo Study. Atherosclerosis. 2015, 239, 470–5. [Google Scholar] [CrossRef] [PubMed]
- Lang, R.M.; Badano, L.P.; Mor-Avi, V.; Afilalo, J.; Armstrong, A.; Ernande, L.; et al. Recommendations for cardiac chamber quantification by echocardiography in adults: An update from the American society of echocardiography and the European association of cardiovascular imaging. Eur Heart J Cardiovasc Imaging. 2015, 16, 233–71. [Google Scholar] [CrossRef] [PubMed]
- Nagueh, S.F.; Smiseth, O.A.; Appleton, C.P.; Byrd, B.F.; Dokainish, H.; Edvardsen, T.; et al. Recommendations for the Evaluation of Left Ventricular Diastolic Function by Echocardiography: An Update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. Journal of the American Society of Echocardiography. 2016, 29, 277–314. [Google Scholar] [CrossRef]
- Okura, K.; Maeno, K.; Okura, S.; Takemori, H.; Toya, D.; Tanaka, N.; et al. Pericardial fat volume is an independent risk factor for the severity of coronary artery disease in patients with preserved ejection fraction. J Cardiol. 2015, 65, 37–41. [Google Scholar] [CrossRef]
- Hirata, Y.; Yamada, H.; Sata, M. Epicardial fat and pericardial fat surrounding the heart have different characteristics. Circulation Journal. Japanese Circulation Society; 2018, 82, 2475–6. [Google Scholar] [CrossRef]
- Son, J.W.; Sung, J.K.; Lee, J.W.; Youn, Y.J.; Ahn, M.S.; Ahn, S.G.; et al. Abdominal obesity and structure and function of the heart in healthy male Koreans the ARIRANG study. Medicine 2016, 95. [Google Scholar]
- Fontes-Carvalho, R.; Gonçalves, A.; Severo, M.; Lourenço, P.; Rocha Gonçalves, F.; Bettencourt, P.; et al. Direct, inflammation-mediated and blood-pressure-mediated effects of total and abdominal adiposity on diastolic function: EPIPorto study. Int J Cardiol. 2015, 191, 64–70. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Regional Office for Europe. WHO European Regional Obesity : Report 2022.
- Wharton, S.; Lau, D.C.W.; Vallis, M.; Sharma, A.M.; Biertho, L.; Campbell-Scherer, D.; et al. Obesity in adults: A clinical practice guideline. CMAJ. 2020, 192, E875–91. [Google Scholar] [CrossRef] [PubMed]
- Andrade, K.A.P.; Rojas, M.A.P. Abdominal circumference cut-off. Available online: http://doi.org/10.5281/zenodo.6981770. [CrossRef]
- Mitchell, C.; Rahko, P.S.; Blauwet, L.A.; Canaday, B.; Finstuen, J.A.; Foster, M.C.; et al. Guidelines for Performing a Comprehensive Transthoracic Echocardiographic Examination in Adults: Recommendations from the American Society of Echocardiography. Journal of the American Society of Echocardiography. 2019, 32, 1–64. [Google Scholar] [CrossRef] [PubMed]
- Eroğlu, S. How do we measure epicardial adipose tissue thickness by transthoracic echocardiography? Anadolu Kardiyoloji Dergisi. 2015, 15, 416–9. [Google Scholar]
- PERFIL REGIONAL DE SAÚDE REGIÃO CENTRO [Internet]. 2018. Available online: http://www.arscentro.min-saude.pt.
- Kuk, J.L.; Lee, S.; Heymsfield, S.B.; Ross, R. Waist circumference and abdominal adipose tissue distribution: influence of age and sex 1-3 [Internet]. 2005. Available online: https://academic.oup.com/ajcn/article/81/6/1330/4648767.
- Stevens, J.; Katz, E.G.; Huxley, R.R. Associations between gender, age and waist circumference. European Journal of Clinical Nutrition. 2010, 64, 6–15. [Google Scholar] [CrossRef] [PubMed]
- Mahabadi, A.A.; Massaro, J.M.; Rosito, G.A.; Levy, D.; Murabito, J.M.; Wolf, P.A.; et al. Association of pericardial fat, intrathoracic fat, and visceral abdominal fat with cardiovascular disease burden: The Framingham Heart Study. Eur Heart J. 2009, 30, 850–6. [Google Scholar] [CrossRef] [PubMed]
- Ni, X.; Jiao, L.; Zhang, Y.; Xu, J.; Zhang, Y.; Zhang, X.; et al. Correlation between the distribution of abdominal, pericardial and subcutaneous fat and muscle and age and gender in a middle-aged and elderly population. Diabetes, Metabolic Syndrome and Obesity 2021, 14, 2201–8. [Google Scholar] [CrossRef] [PubMed]
- Rabkin, S.W. The relationship between epicardial fat and indices of obesity and the metabolic syndrome: A systematic review and meta-analysis. Metabolic Syndrome and Related Disorders 2014, 12, 31–42. [Google Scholar] [CrossRef]
- Zhu, L.; Gu, S.; Wang, Q.; Zhou, X.; Wang, S.; Fu, C.; et al. Left ventricular myocardial deformation: A study on diastolic function in the Chinese male population and its relationship with fat distribution. Quant Imaging Med Surg. 2020, 10, 634–45. [Google Scholar] [CrossRef]
- Vaibhav Patel, B.B.; Mori, J.; McLean, B.A.; Basu, R.; Das, S.K.; Ramprasath, T.; et al. ACE2 deficiency worsens epicardial adipose tissue inflammation and cardiac dysfunction in response to diet-induced obesity. 2015. [Google Scholar]
- Iacobellis, G.; Leonetti, F.; Singh, N.; MSharma, A. Relationship of epicardial adipose tissue with atrial dimensions and diastolic function in morbidly obese subjects. Int J Cardiol. 2007, 115, 272–3. [Google Scholar] [CrossRef] [PubMed]
- Kim, J.S.; Kim, S.W.; Lee, J.S.; Lee, S.K.; Abbott, R.; Lee, K.Y.; et al. Association of pericardial adipose tissue with left ventricular structure and function: a region-specific effect? Cardiovasc Diabetol. 2021, 20. [Google Scholar] [CrossRef] [PubMed]
- Fox, C.S.; Gona, P.; Hoffmann, U.; Porter, S.A.; Salton, C.J.; Massaro, J.M.; et al. Pericardial fat, intrathoracic fat, and measures of left ventricular structure and function. Circulation. 2009, 119, 1586–91. [Google Scholar] [CrossRef] [PubMed]
- Mahajan, R.; Lau, D.H.; Brooks, A.G.; Shipp, N.J.; Manavis, J.; Wood, J.P.M.; et al. Electrophysiological, Electroanatomical, and Structural Remodeling of the Atria as Consequences of Sustained Obesity. J Am Coll Cardiol. 2015, 66, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Hahn, R.T.; Badano, L.P.; Bartko, P.E.; Muraru, D.; Maisano, F.; Zamorano, J.L.; et al. Tricuspid regurgitation: recent advances in understanding pathophysiology, severity grading and outcome. European Heart Journal Cardiovascular Imaging Oxford University Press. 2022, 23, 913–29. [Google Scholar] [CrossRef] [PubMed]
- Cai, A.; Liu, L.; Zhou, D.; Zhou, Y.; Tang, S.; Feng, Y. The patterns of left ventricular alteration by adipose tissue distribution: implication for heart failure prevention. ESC Heart Fail. 2021, 8, 3093–105. [Google Scholar] [CrossRef] [PubMed]
- Watanabe, K.; Kishino, T.; Sano, J.; Ariga, T.; Okuyama, S.; Mori, H.; et al. Relationship between epicardial adipose tissue thickness and early impairment of left ventricular systolic function in patients with preserved ejection fraction. Heart Vessels. 2016, 31, 1010–5. [Google Scholar] [CrossRef] [PubMed]
- van Woerden, G.; Gorter, T.M.; Westenbrink, B.D.; Willems, T.P.; van Veldhuisen, D.J.; Rienstra, M. Epicardial fat in heart failure patients with mid-range and preserved ejection fraction. Eur J Heart Fail. 2018, 20, 1559–66. [Google Scholar] [CrossRef]
- Obokata, M.; Reddy, Y.N.V.; Borlaug, B.A. Diastolic Dysfunction and Heart Failure With Preserved Ejection Fraction: Understanding Mechanisms by Using Noninvasive Methods. JACC: Cardiovascular Imaging Elsevier Inc.. 2020, 13, 245–57. [Google Scholar]
- Cherian, S.; Lopaschuk, G.D.; Carvalho, E. Cellular cross-talk between epicardial adipose tissue and myocardium in relation to the pathogenesis of cardiovascular disease. Am J Physiol Endocrinol Metab 2012, 303, 937–49. Available online: http://www.ajpendo.org. [CrossRef] [PubMed]
- Van De Weijer, T.; Schrauwen-Hinderling, V.B.; Schrauwen, P. Lipotoxicity in type 2 diabetic cardiomyopathy. Cardiovascular Research 2011, 92, 10–8. [Google Scholar] [CrossRef] [PubMed]
- Ng, A.C.T.; Goo, S.Y.; Roche, N.; van der Geest, R.J.; Wang, W.Y.S. Epicardial Adipose Tissue Volume and Left Ventricular Myocardial Function Using 3-Dimensional Speckle Tracking Echocardiography. Canadian Journal of Cardiology 2016, 32, 1485–92. [Google Scholar] [CrossRef] [PubMed]
- Arshi, B.; Aliahmad, H.A.; Ikram, M.A.; Bos, D.; Kavousi, M. Epicardial Fat Volume, Cardiac Function, and Incident Heart Failure: The Rotterdam Study. J Am Heart Assoc. 2023, 3, 12. [Google Scholar] [CrossRef]
| Total Population (n=82) | PF Low (n=45) | PF High (n=37) | (p-value) | |
| E (cm/s) * | 67,879 ± 16,57 | 69,41 ± 11,92 | 66,01 ± 20,92 | p=0,359 |
| DT (ms) * | 0,198 ± 0,0532 | 0,185 ± 0,039 | 0,213 ± 0,063 | p=0,0,13 |
| E/A ** | 1,030 ± 0,426 | 1,10 ± 0,34 | 0,94 ± 0,50 | p= 0,003 |
| septal e' (cm/s) * | 8,252 ± 2,449 | 9,57 ± 2,167 | 6,64 ± 1,70 | P<0,0001 |
| lateral e' (cm/s) * | 11,823 ± 3,201 | 13,23 ± 3,30 | 10,11 ± 2,06 | P<0,0001 |
| E/e' * | 7,339 ± 2,620 | 6,40 ± 2,01 | 8,48 ± 2,83 | P<0,0001 |
| LAV (ml/m2) * | 36,648 ± 8,332 | 32,80 ± 4,97 | 41,329 ± 9,22 | P<0,0001 |
| LVEF (%) * | 65,57 ± 5,624 | 66,52 ± 4,99 | 64,42 ± 6,18 | p=0,093 |
| LV Mass (g) * | 164,95 ± 52,338 | 149,64 ± 34,082 | 183,57 ± 63,99 | p=0,003 |
| TRJV (cm/s) ** | 2,466 ± 0,294 | 2,32 ± 0,22 | 2,65 ± 0,26 | P<0,0001 |
| LV Diameter (mm) * | 53,342 ± 5,197 | 52,07 ± 4,029 | 54,889 ± 6,037 | p=0,014 |
| Pericardial Fat | Epicardial Fat | |||||
| Correlação | Grau de Correlação | (p- value) | Correlação | Grau de Correlação | (p- value) | |
| E (cm/s) | -0,053 | Non-Significant | p=0,633 | 0,032 | Non-Significant | p=0,776 |
| DT (ms) | 0,222 | Low | p=0,045 | 0,208 | Non-Significant | p=0,061 |
| E/A | -0,363 | Moderate | p=0,001 | -0,403 | Moderate | p<0,0001 |
| septal e' (cm/s) | -0,686 | High | p<0,0001 | -0,731 | High | p<0,0001 |
| lateral e' (cm/s) | -0,630 | High | p<0,0001 | -0,662 | High | p<0,0001 |
| E/e' | 0,494 | Moderate | p<0,0001 | 0,592 | High | p<0,0001 |
| LAV (ml/m2) | 0,683 | High | p<0,0001 | 0,693 | High | p<0,0001 |
| LVEF (%) | -0,141 | Non-Significant | p=0,207 | -0,216 | Non-Significant | p=0,052 |
| LV Mass (g) | 0,359 | Moderate | p=0,001 | 0,397 | Moderate | p<0,0001 |
| TRJV (cm/s) | 0,629 | High | p<0,0001 | 0,610 | High | p<0,0001 |
| LV Diam (mm) | 0,227 | Low | p=0,041 | 0,282 | Low | p=0,010 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




