4. Discussion
Previous studies(23) have shown that a complete blood count can identify early risk of developing sepsis and distinguish a poor prognosis. Among them, total white blood cells are composed of lymphocytes, monocytes, neutrophils, eosinophils, and basophils, and their increase is known to be caused by inflammation or infection, but it can also be caused by non-infectious diseases such as rheumatoid arthritis or cancer, so it is known to have low specificity in sepsis. Neutrophils are the most abundant in peripheral blood and quickly migrate to the site of infection to remove infectious agents in the event of infection, and are increased in sepsis, but can be caused by smoking or stress, and can also be increased in inflammatory bowel disease or rheumatic diseases, so they are not good for diagnosis and prognosis of sepsis, and eosinophils also migrate to the site of infection in infection and secrete cytokines, Eosinophil reduction has shown good sensitivity and specificity in the diagnosis of sepsis in some studies(24), but in a recent analysis (25) it was not found to be superior to CRP or procalcitonin. Furthermore, lymphocytes are an important component of the adaptive immune response, and although lymphopenia is associated with poor prognosis in sepsis, it can also be seen in nutritional deficiencies and autoimmune diseases (26). On the other hand, the ratio of neutrophils to lymphocytes reflects the diagnosis and prognosis of sepsis and is known to be superior to CRP and inferior to procalcitonin (27), but it is also increased in coronary artery disease and cancer, limiting its use (28).
Previous studies(29) have shown that platelet dysfunction in sepsis is present and associated with poor prognosis, and that dysfunction includes thrombocytopenia, mean platelet volume, and immature platelet fraction. Of these, thrombocytopenia was associated with a higher risk of death in the intensive care unit (30). However, thrombocytopenia is also associated with non-infectious diseases such as idiopathic thrombocytopenic purpura and systemic lupus erythematosus. Mean platelet volume is higher in sepsis than in localized infections, and increased mean platelet volume has been reported to be associated with more severe infections or antibiotic treatment failure, but it is also increased in heart disease and cerebral infarction, limiting its applicability to sepsis.
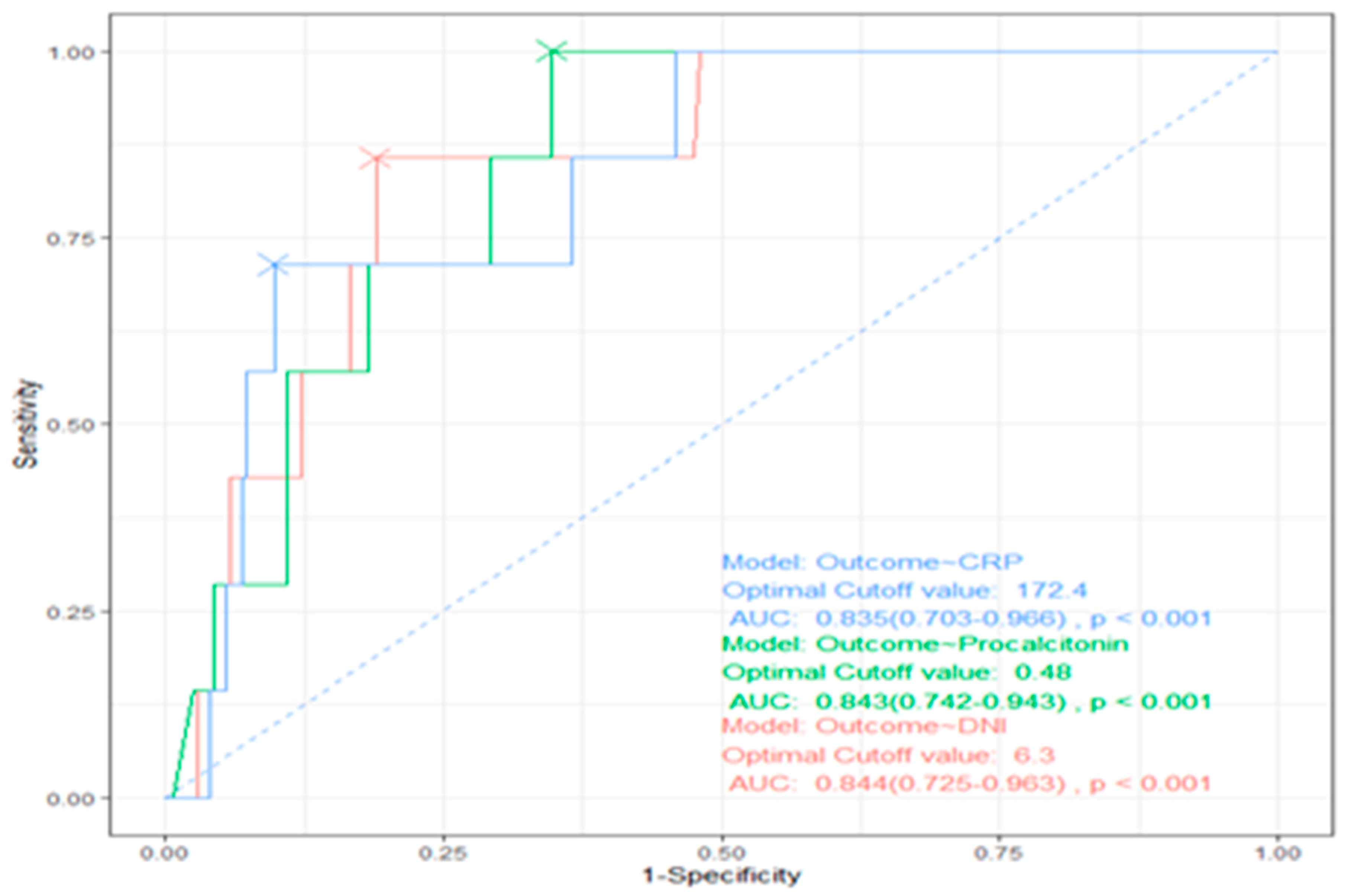
The present study aimed to assess the effectiveness of Delta Neutrophil Index (DNI) compared to other molecular biomarkers, such as procalcitonin (PCT) and C-reactive protein (CRP), in differentiating febrile septic patients from febrile non-septic patients in the emergency department and predicting prognosis. It is worth noting that previous studies (31) have established the utility of procalcitonin as a biomarker for diagnosing sepsis and predicting prognosis. However, our study demonstrates that DNI is a superior cytological marker for diagnosing and predicting sepsis when compared to procalcitonin.
Furthermore, our findings reveal a negative correlation between Mean Platelet Component (MPC) levels and DNI levels, indicating the potential of MPC in differentiating the causes of sepsis. These conclusions are drawn from the statistical analysis and comparative measurements of two molecular markers (PCT and CRP) and two cellular markers (DNI and MPC).
In our study, DNI levels increased above the baseline (1%) in both the febrile sepsis and non-sepsis groups. However, the increase was more pronounced in the febrile sepsis group compared to the febrile non-sepsis group (110 out of 123 (89.4%) vs. 61 out of 92 (66.3%), p=0.000). There was a significant difference in DNI levels between the febrile sepsis and non-sepsis groups (6.7±7.8% vs. 2.1±2.2%, p=0.000).
The elevated DNI levels observed in the febrile non-sepsis group may be attributed to non-infectious inflammation, such as trauma-related tissue damage, metabolic disorders, or autoimmune diseases. However, DNI levels were significantly higher in the febrile sepsis group compared to the febrile non-sepsis group, which supports previous reports highlighting the effectiveness of DNI in assessing sepsis (32). Accumulative studies have also suggested that DNI can be a diagnostic marker for sepsis ((14), (33), (15), (34)).
Consistent with prior research, our results demonstrate that DNI is effective in differentiating sepsis-related fever from non-sepsis-related fever. Furthermore, the cutoff value of 6.2% for DNI is more effective than CRP and PCT in predicting the prognosis of febrile sepsis, including outcomes such as mortality, organ failure, length of stay, and in-hospital surgery. Patients with a DNI value greater than 6.2% have a worse prognosis.
It is well-known that platelets are activated in various infectious and non-infectious pathological conditions, such as acute myocardial infarction (35), cerebrovascular disease (36), and diabetes mellitus (37). Similar to the aberrant neutrophil behaviour observed in sepsis, platelet activation plays a significant role in these conditions.
Patients with febrile sepsis and lower MPC levels are at an increased risk of death. This association can be attributed to the detrimental effects of platelet activation, including platelet depletion, thrombosis, and the development of disseminated intravascular coagulopathy (38). These complications can ultimately lead to multi-organ failure and even death (39).
These findings have significant clinical implications, suggesting that patients admitted to the emergency department with fever and suspected sepsis, particularly those with low MPC levels, should undergo prompt evaluation to identify the source of sepsis and initiate appropriate management strategies as early as possible.
Finally, inferential statistics revealed a significant negative correlation between DNI and MPC, and the strength of this inverse correlation varied depending on the origin of sepsis. Notably, this is the first report to demonstrate this relationship in the context of human sepsis. The strongest negative correlation between DNI and MPC was observed in cases of sepsis originating from the gastrointestinal tract and lungs (Pearson correlation coefficients: -0.611 for gastrointestinal tract origin, -0.492 for lung origin, and -0.312 for all sources of sepsis). This finding may provide valuable insights into the clinical application of identifying the focus of infection in sepsis. However, the consideration of using a panel of the best candidate markers may be superior to the use of each of crp, procalcitonin, and DNI alone in assessing the diagnosis and prognosis of sepsis, but there is not much room for consideration at this time because each biomarker alone is excellent for the diagnosis and prognosis of sepsis.
One possible explanation for the strong negative correlation between DNI and MPC in gastrointestinal and lung sepsis could be the dysbiosis of gut microbiota associated with the gut-lung axis (40). The human gut harbors a vast number of microbiomes, accounting for over 80% of the body’s lymphocytes, and plays a crucial role in the development and function of immune cells (41). In septic conditions, the gut microbiota undergoes dysbiosis (42) and increased permeability, leading to platelet activation, severe tissue damage, and ultimately multi-organ failure and death (43). Similarly, the gut-lung axis (GLA) can significantly impact the lungs during sepsis (44). Gut microbiota can modulate pulmonary immune responses and diseases through the mesenteric lymphatic system (41), (45). Therefore, we speculate that these intricate networks contribute to the more pronounced negative correlations observed in gastrointestinal and lung-origin sepsis compared to other causes of sepsis.
Our study demonstrated the predictive value of DNI and MPC in febrile sepsis and highlighted the potential benefit of utilizing both markers together to enhance the probability of predicting sepsis. Nevertheless, it is important to acknowledge the limitations of this study. Firstly, there were cases where initial cultures were not obtained in less than 5% of patients. Additionally, follow-up data was unavailable for less than 10% of eligible patients. Furthermore, patients with sepsis without fever were not evaluated. The one-year follow-up period in this study may not provide a comprehensive understanding of the long-term prognosis and outcome assessment of febrile patients with suspected sepsis. Therefore, future research with longer follow-up durations, ideally one year or more, is warranted. Lastly, it is important to note that this study utilized a retrospective design.
In summary: this study highlights the superiority of DNI over other molecular biomarkers, such as procalcitonin and CRP, in differentiating febrile septic patients from nonseptic febrile patients in the emergency department and predicting prognosis. MPC also contributes to the differentiation of causes in febrile sepsis. The clinical significance of DNI/MPC lies in their cost-effectiveness and applicability in various impending sepsis scenarios. Importantly, this study is the first to evaluate the diagnostic validity of simultaneously employing DNI and MPC in human cases of febrile sepsis.