Submitted:
30 October 2023
Posted:
31 October 2023
You are already at the latest version
Abstract
Keywords:
Introduction
Methods
Study design and population
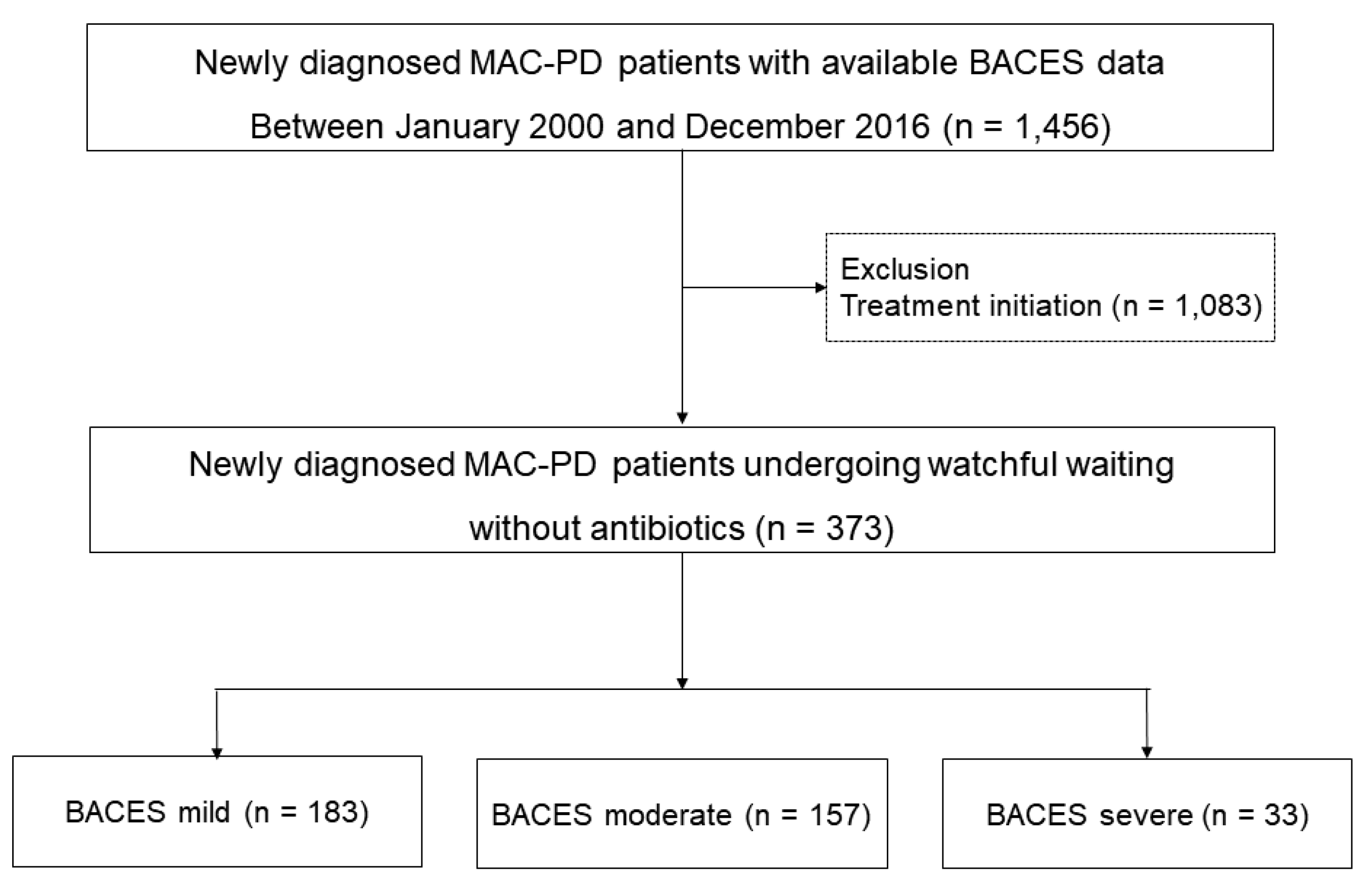
Evaluation of BACES severity
Sputum and radiological examinations
Evaluation of microbiological outcomes
Statistical analysis
Results
Baseline characteristics of study patients
| Variables | Total (n = 373) |
Spontaneous negative culture conversion (n = 153) |
No culture conversion (n = 220) |
p-value |
|---|---|---|---|---|
| BACES items | ||||
| BMI < 18.5kg/m2 | 73 (20) | 30 (20) | 43 (20) | 0.988 |
| Age ≥ 65 years | 153 (41) | 47 (31) | 106 (48) | 0.001 |
| Cavity | 36 (10) | 9 (6) | 27 (12) | 0.040 |
| Elevated ESR* | 234 (63) | 96 (63) | 138 (63) | 0.997 |
| Sex, male | 145 (39) | 56 (37) | 89 (41) | 0.453 |
| Ex- or current smoker | 98 (26) | 113 (74) | 161 (73) | 0.885 |
| Underlying condition | ||||
| Previous tuberculosis | 103 (28) | 43 (28) | 60 (27) | 0.860 |
| Chronic obstructive pulmonary disease | 24 (6) | 16 (11) | 8 (4) | 0.008 |
| Chronic pulmonary aspergillosis | 2 (1) | - | - | 0.515 |
| Lung cancer | 18 (5) | 6 (4) | 12 (6) | 0.497 |
| Symptoms† | ||||
| Cough | 230 (62) | 99 (65) | 131 (60) | 0.313 |
| Sputum | 227 (61) | 94 (61) | 133 (61) | 0.848 |
| Hemoptysis | 63 (17) | 28 (18) | 35 (16) | 0.544 |
| Weight loss | 17 (5) | 4 (3) | 13 (6) | |
| Positive sputum AFB smear | 122 (33) | 40 (26) | 82 (37) | 0.024 |
| Etiology | 0.081 | |||
| M. avium | 229 (61) | 102 (67) | 127 (58) | |
| M. intracellulare | 144 (39) | 51 (33) | 93 (42) | |
| Radiological phenotype | 0.096 | |||
| Nodular bronchiectatic form | 353 (94) | 147 (96) | 206 (94) | |
| Fibrocavitary form | 20 (5) | 6 (4) | 14 (6) |
Microbiological outcomes in patients without antibiotic treatment
| Watchful waiting | Total (n = 373) |
Mild (n = 183) |
Moderate (n = 157) |
Severe (n = 33) |
p-value | p-trend† |
|---|---|---|---|---|---|---|
| Spontaneous negative culture conversion | 153 (41) | 87/183 (48) | 58/157 (37) | 8/33 (24) | 0.017ac | 0.005 |
| Time to culture conversion, months | 6.2 (2.7 – 17.7) | 6.0 (2.2 – 16.1) | 5.4 (2.8 – 17.2) | 22.1 (14.2 – 88.5) | 0.008bc | 0.037 |
| Favorable outcome* | 157 (42) | 97/183 (53) | 54/157 (34) | 6/33 (18) | <0.001ac | <0.001 |
| Time to favorable outcome, months | 6.2 (2.5 – 15.8) | 6.2 (2.3 – 14.3) | 5.4 (2.5 – 14.0) | 40.3 (11.8 – 98.2) | 0.022 bc | 0.346 |
Factors associated with the microbiological outcome
| Variables | Univariable analysis | Multivariable analysis | ||
|---|---|---|---|---|
| Unadjusted HR (95% CI) |
p-value | Adjusted HR (95% CI) |
p-value | |
| Spontaneous negative culture conversion | ||||
| Ex- or current smoker | 0.85 (0.59 – 1.22) | 0.388 | 0.99 (0.66 – 1.49) | 0.971 |
| Underlying condition | ||||
| Previous pulmonary tuberculosis | 1.02 (0.72 – 1.46) | 0.901 | 1.12 (0.77 – 1.62) | 0.556 |
| Chronic obstructive pulmonary disease | 1.54 (0.91 – 2.58) | 0.106 | 1.76 (1.02 – 3.05) | 0.043 |
| Lung cancer | 0.92 (0.40 – 2.07) | 0.915 | 0.89 (0.38 – 2.08) | 0.792 |
| Etiology | ||||
| M. avium | Reference | Reference | ||
| M. intracellulare | 0.83 (0.60 – 1.17) | 0.287 | 0.83 (0.59 – 1.17) | 0.295 |
| BACES severity | ||||
| Mild | Reference | Reference | ||
| Moderate | 0.75 (0.54 – 1.05) | 0.093 | 0.74 (0.52 – 1.07) | 0.106 |
| Severe | 0.53 (0.26 – 1.10) | 0.089 | 0.49 (0.22 – 1.08) | 0.076 |
| Positive sputum AFB smear at diagnosis | 0.68 (0.47 – 0.97) | 0.034 | 0.70 (0.48 – 1.01) | 0.057 |
| Favorable outcome* | ||||
| Ex- or current smoker | 0.77 (0.53 – 1.12) | 0.167 | 1.04 (0.69 – 1.57) | 0.861 |
| Underlying condition | ||||
| Previous pulmonary tuberculosis | 0.83 (0.58 – 1.19) | 0.313 | 0.95 (0.65 – 1.38) | 0.767 |
| Chronic obstructive pulmonary disease | 1.11 (0.63 – 1.95) | 0.728 | 1.35 (0.75 – 2.44) | 0.317 |
| Lung cancer | 0.89 (0.40 – 2.02) | 0.785 | 1.01 (0.44 – 2.33) | 0.982 |
| Etiology | ||||
| M. avium | Reference | Reference | ||
| M. intracellulare | 0.67 (0.48-0.94) | 0.021 | 0.67 (0.47-0.94) | 0.020 |
| BACES severity | ||||
| Mild | Reference | Reference | ||
| Moderate | 0.63 (0.45 – 0.88) | 0.007 | 0.63 (0.44 – 0.91) | 0.013 |
| Severe | 0.37 (0.16 – 0.84) | 0.017 | 0.37 (0.16 – 0.90) | 0.028 |
| Positive sputum AFB smear | 0.79 (0.55 – 1.12) | 0.787 | 0.84 (0.59 – 1.20) | 0.333 |
Discussion
Author Contributions
Funding
Ethics Approval
Data Availability Statement
Acknowledgment
Competing Interests
Patient Consent For Publication
References
- Lee, H.; Myung, W.; Koh, W.J.; Moon, S.M.; Jhun, B.W. Epidemiology of nontuberculous mycobacterial infection, South Korea, 2007-2016. Emerg Infect Dis 2019, 25, 569–572. [Google Scholar] [CrossRef] [PubMed]
- Griffith, D.E.; Aksamit, T.; Brown-Elliott, B.A.; Catanzaro, A.; Daley, C.; Gordin, F.; Holland, S.M.; Horsburgh, R.; Huitt, G.; Iademarco, M.F.; et al. An official ATS/IDSA statement: diagnosis, treatment, and prevention of nontuberculous mycobacterial diseases. Am J Respir Crit Care Med 2007, 175, 367–416. [Google Scholar] [CrossRef]
- Daley, C.L.; Iaccarino, J.M.; Lange, C.; Cambau, E.; Wallace, R.J., Jr.; Andrejak, C.; Böttger, E.C.; Brozek, J.; Griffith, D.E.; Guglielmetti, L.; et al. Treatment of nontuberculous mycobacterial pulmonary disease: an official ATS/ERS/ESCMID/IDSA clinical practice guideline. Eur Respir J 2020, 56, 2000535. [Google Scholar] [CrossRef] [PubMed]
- Haworth, C.S.; Banks, J.; Capstick, T.; Fisher, A.J.; Gorsuch, T.; Laurenson, I.F.; Leitch, A.; Loebinger, M.R.; Milburn, H.J.; Nightingale, M.; et al. British Thoracic Society guidelines for the management of non-tuberculous mycobacterial pulmonary disease (NTM-PD). Thorax 2017, 72, ii1–ii64. [Google Scholar] [CrossRef] [PubMed]
- Pasipanodya, J.G.; Ogbonna, D.; Deshpande, D.; Srivastava, S.; Gumbo, T. Meta-analyses and the evidence base for microbial outcomes in the treatment of pulmonary Mycobacterium avium-intracellulare complex disease. J Antimicrob Chemother 2017, 72, i3–i19. [Google Scholar] [CrossRef]
- Hwang, J.A.; Kim, S.; Jo, K.W.; Shim, T.S. Natural history of Mycobacterium avium complex lung disease in untreated patients with stable course. Eur Respir J 2017, 49, 1600537. [Google Scholar] [CrossRef] [PubMed]
- Moon, S.M.; Jhun, B.W.; Baek, S.Y.; Kim, S.; Jeon, K.; Ko, R.E.; Shin, S.H.; Lee, H.; Kwon, O.J.; Huh, H.J.; et al. Long-term natural history of non-cavitary nodular bronchiectatic nontuberculous mycobacterial pulmonary disease. Respir Med 2019, 151, 1–7. [Google Scholar] [CrossRef]
- Kwon, B.S.; Lee, J.H.; Koh, Y.; Kim, W.S.; Song, J.W.; Oh, Y.M.; Lee, S.D.; Lee, S.W.; Lee, J.S.; Lim, C.M.; et al. The natural history of non-cavitary nodular bronchiectatic Mycobacterium avium complex lung disease. Respir Med 2019, 150, 45–50. [Google Scholar] [CrossRef]
- Kim, H.J.; Kwak, N.; Hong, H.; Kang, N.; Im, Y.; Jhun, B.W.; Yim, J.J. BACES score for predicting mortality in nontuberculous mycobacterial pulmonary disease. Am J Respir Crit Care Med 2021, 203, 230–236. [Google Scholar] [CrossRef]
- Kim, H.J.; Song, M.J.; Kwon, B.S.; Kim, Y.W.; Lim, S.Y.; Lee, Y.J.; Park, J.S.; Cho, Y.J.; Lee, C.T.; Lee, J.H. Usefulness of the BACES score in nontuberculous mycobacterial pulmonary disease for various clinical outcomes. Sci Rep 2023, 13, 7495. [Google Scholar] [CrossRef]
- Kim, B.G.; Jhun, B.W.; Kim, H.; Kwon, O.J. Treatment outcomes of Mycobacterium avium complex pulmonary disease according to disease severity. Sci Rep 2022, 12, 1970. [Google Scholar] [CrossRef] [PubMed]
- Jhun, B.W.; Moon, S.M.; Jeon, K.; Kwon, O.J.; Yoo, H.; Carriere, K.C.; Huh, H.J.; Lee, N.Y.; Shin, S.J.; Daley, C.L.; et al. Prognostic factors associated with long-term mortality in 1445 patients with nontuberculous mycobacterial pulmonary disease: a 15-year follow-up study. Eur Respir J 2020, 55, 1900798. [Google Scholar] [CrossRef]
- Jhun, B.W.; Kim, S.Y.; Moon, S.M.; Jeon, K.; Kwon, O.J.; Huh, H.J.; Ki, C.S.; Lee, N.Y.; Shin, S.J.; Daley, C.L.; et al. Development of macrolide resistance and reinfection in refractory Mycobacterium avium complex lung disease. Am J Respir Crit Care Med 2018, 198, 1322–1330. [Google Scholar] [CrossRef] [PubMed]
- Choi, Y.; Jhun, B.W.; Kim, J.; Huh, H.J.; Lee, N.Y. Clinical characteristics and outcomes of surgically resected solitary pulmonary nodules due to nontuberculous mycobacterial Infections. J Clin Med 2019, 8, 1898. [Google Scholar] [CrossRef]
- van Ingen, J.; Aksamit, T.; Andrejak, C.; Böttger, E.C.; Cambau, E.; Daley, C.L.; Griffith, D.E.; Guglielmetti, L.; Holland, S.M.; Huitt, G.A.; et al. Treatment outcome definitions in nontuberculous mycobacterial pulmonary disease: an NTM-NET consensus statement. Eur Respir J 2018, 51, 1800170. [Google Scholar] [CrossRef]
- Pan, S.W.; Shu, C.C.; Feng, J.Y.; Wang, J.Y.; Chan, Y.J.; Yu, C.J.; Su, W.J. Microbiological persistence in patients with Mycobacterium avium complex lung disease: The predictors and the impact on radiographic progression. Clin Infect Dis 2017, 65, 927–934. [Google Scholar] [CrossRef]
- Prieto, M.D.; Jang, J.; Franciosi, A.N.; Av-Gay, Y.; Bach, H.; Tebbutt, S.J.; Quon, B.S. Whole blood RNA-seq demonstrates an increased host immune response in individuals with cystic fibrosis who develop nontuberculous mycobacterial pulmonary disease. PLoS One 2022, 17, e0278296. [Google Scholar] [CrossRef]
- Hull, R.C.; Huang, J.T.J.; Barton, A.K.; Keir, H.R.; Ellis, H.; Cookson, W.O.C.; Moffatt, M.F.; Loebinger, M.R.; Chalmers, J.D. Sputum proteomics in nontuberculous mycobacterial lung disease. Chest 2022, 161, 1180–1191. [Google Scholar] [CrossRef]
- Pan, S.W.; Su, W.J.; Chan, Y.J.; Ho, M.L.; Feng, J.Y.; Shu, C.C.; Wang, J.Y.; Wang, H.C.; Yu, C.J.; Chen, Y.M. Disease progression in patients with nontuberculous mycobacterial lung disease of nodular bronchiectatic (NB) pattern: The roles of cavitary NB and soluble programmed death protein-1. Clin Infect Dis 2022, 75, 239–247. [Google Scholar] [CrossRef]
- Chalmers, J.D.; Goeminne, P.; Aliberti, S.; McDonnell, M.J.; Lonni, S.; Davidson, J.; Poppelwell, L.; Salih, W.; Pesci, A.; Dupont, L.J.; et al. The bronchiectasis severity index. An international derivation and validation study. Am J Respir Crit Care Med 2014, 189, 576–585. [Google Scholar] [CrossRef]
- Martínez-García, M.; de Gracia, J.; Vendrell Relat, M.; Girón, R.M.; Máiz Carro, L.; de la Rosa Carrillo, D.; Olveira, C. Multidimensional approach to non-cystic fibrosis bronchiectasis: the FACED score. Eur Respir J 2014, 43, 1357–1367. [Google Scholar] [CrossRef] [PubMed]
- Martinez-Garcia, M.A.; Athanazio, R.A.; Girón, R.; Máiz-Carro, L.; de la Rosa, D.; Olveira, C.; de Gracia, J.; Vendrell, M.; Prados-Sánchez, C.; Gramblicka, G.; et al. Predicting high risk of exacerbations in bronchiectasis: the E-FACED score. Int J Chron Obstruct Pulmon Dis 2017, 12, 275–284. [Google Scholar] [CrossRef] [PubMed]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




