Submitted:
29 October 2023
Posted:
30 October 2023
You are already at the latest version
Abstract
Keywords:
1. Introduction:
2. Deforestation:
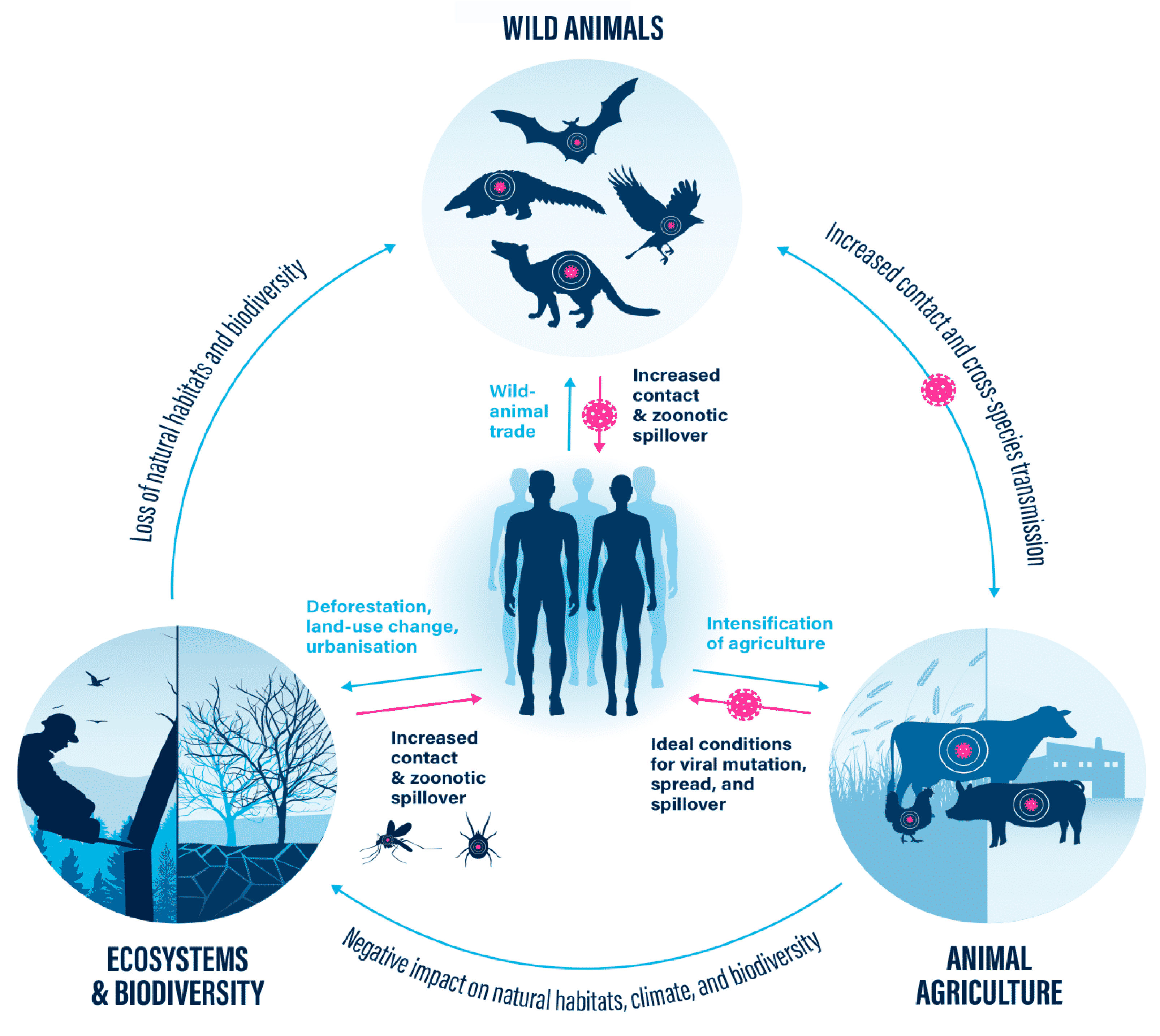
2.1. Consequences of deforestation:
2.1.1. Transmission bottlenecks:
2.1.2. Zoonotic spillover events:
3. Wild animals:
4. Animals agriculture:
5. Management of the disease’s prevention and control:
6.2. Uses of vaccines:
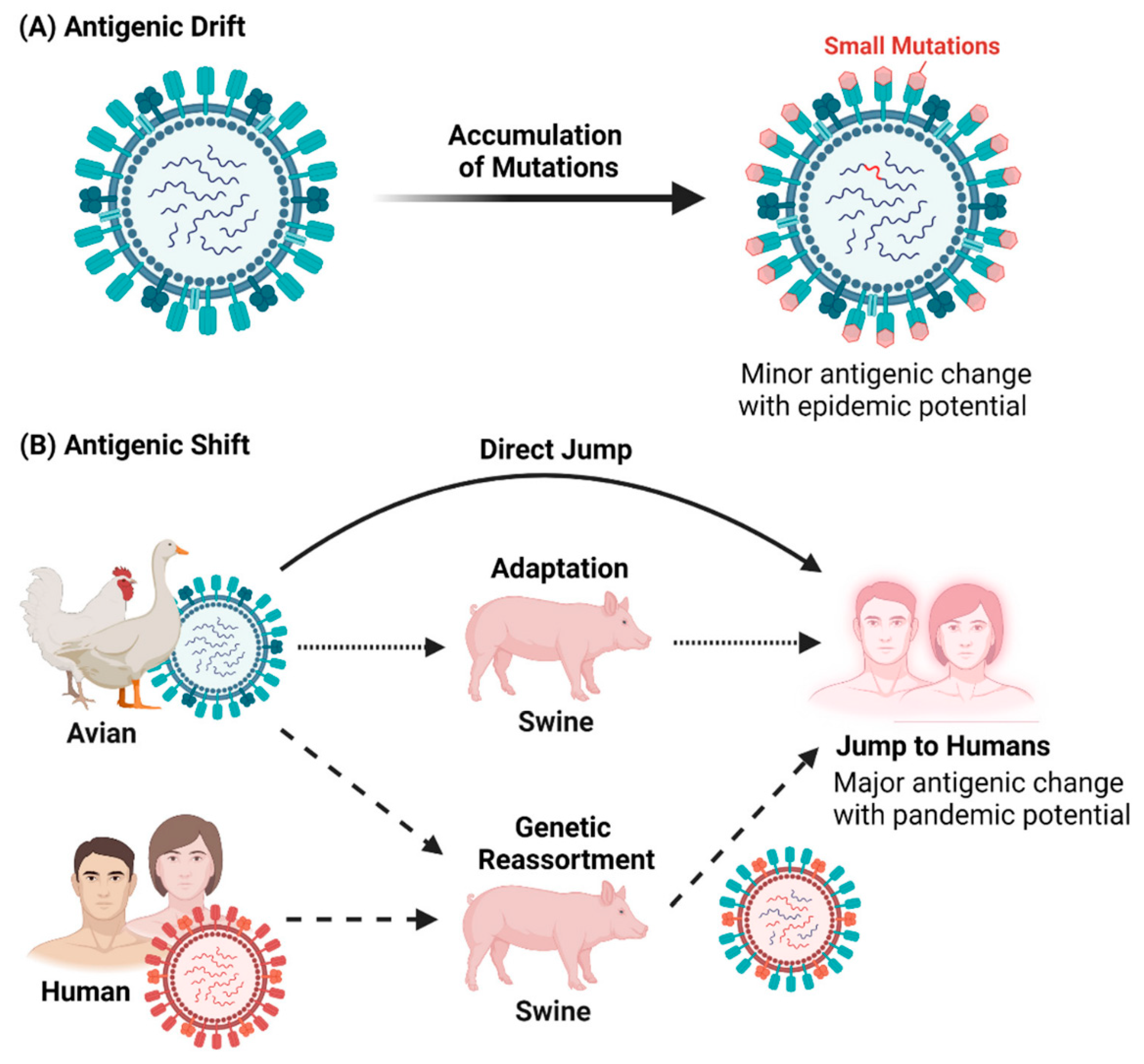
7. The effect of antigenic drift on vaccine effectiveness:
8. Climate change and Pollution:
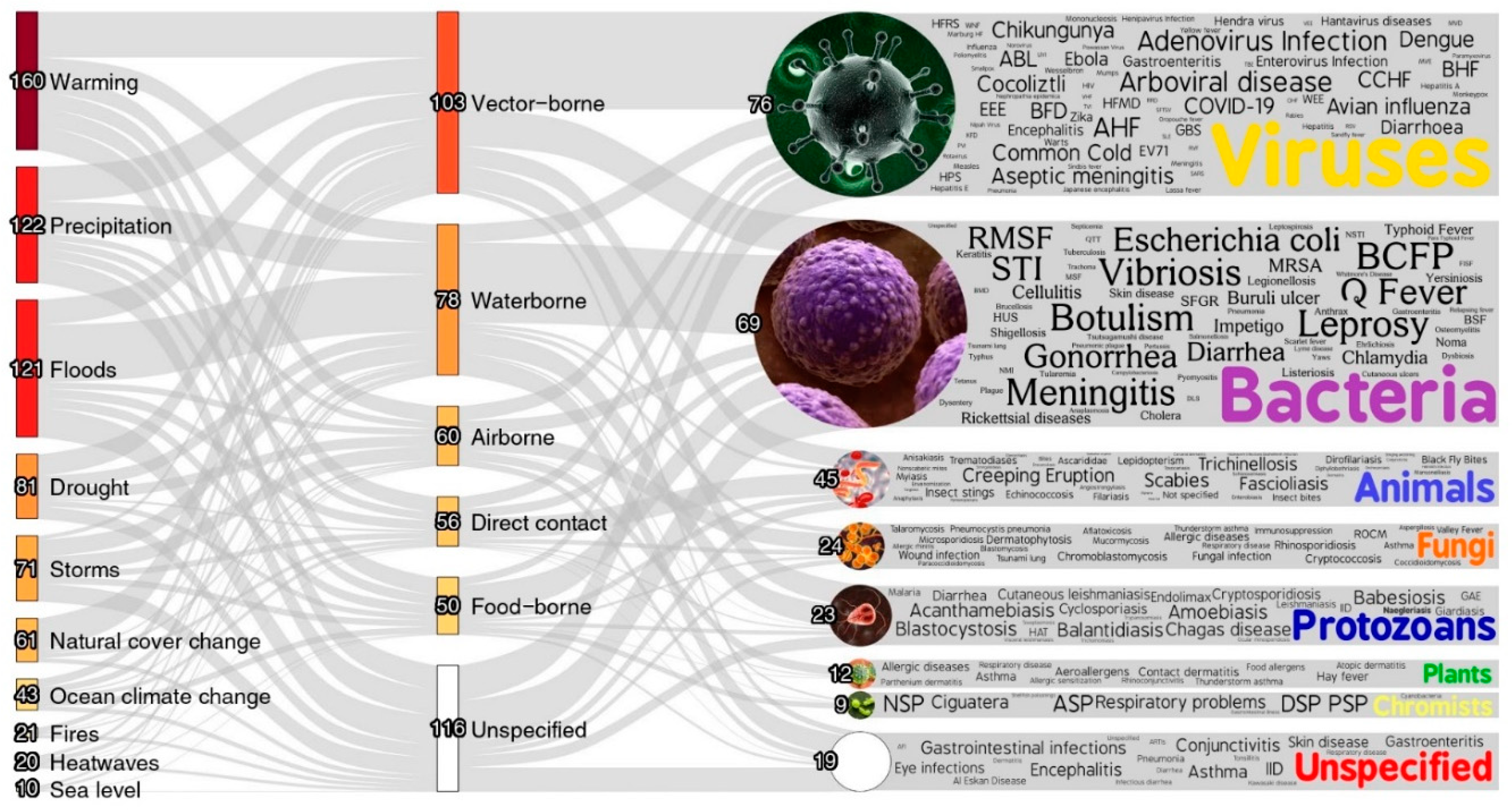
9. The Emerging Infectious Diseases burden:
10. Concluding remarks and future perspectives:
Authors’ Contributions
Ethical approval
Funding
Acknowledgment
Conflict of interest
References
- Woolhouse, M.E.J. Emerging diseases go global. Nature 2008, 451, 898–899. [Google Scholar] [CrossRef] [PubMed]
- Afelt, A.; Frutos, R.; Devaux, C. Bats, Coronaviruses, and Deforestation: Toward the Emergence of Novel Infectious Diseases? Front. Microbiol. 2018, 9, 702. [Google Scholar] [CrossRef]
- Daniels, P.W.; Halpin, K.; Hyatt, A.; Middleton, D. Infection and disease in reservoir and spillover hosts: determinants of pathogen emergence. Curr. Top. Microbiol. Immunol. 2007, 315, 113–131. [Google Scholar] [CrossRef] [PubMed]
- Wang, L.F.; Anderson, D.E. Viruses in bats and potential spillover to animals and humans. Curr. Opin. Virol. 2019, 34, 79–89. [Google Scholar] [CrossRef] [PubMed]
- Lin, X.D.; Wang, W.; Hao, Z.Y.; Wang, Z.X.; Guo, W.P.; Guan, X.Q.; Wang, M.R.; Wang, H.W.; Zhou, R.H.; Li, M.H.; et al. Extensive diversity of coronaviruses in bats from China. Virology 2017, 507, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Calisher, C.H.; Childs, J.E.; Field, H.E.; Holmes, K.V.; Schountz, T. Bats: important reservoir hosts of emerging viruses. Clin. Microbiol. Rev. 2006, 19, 531–545. [Google Scholar] [CrossRef]
- Chan, J.F.; To, K.K.; Tse, H.; Jin, D.Y.; Yuen, K.Y. Interspecies transmission and emergence of novel viruses: lessons from bats and birds. Trends Microbiol. 2013, 21, 544–555. [Google Scholar] [CrossRef]
- Peel, A.J.; Sargan, D.R.; Baker, K.S.; Hayman, D.T.S.; Barr, J.A.; Crameri, G.; Suu-Ire, R.; Broder, C.C.; Lembo, T.; Wang, L.F.; et al. Continent-wide panmixia of an African fruit bat facilitates transmission of potentially zoonotic viruses. Nat. Commun. 2013, 4, 2770. [Google Scholar] [CrossRef] [PubMed]
- Anthony, S.J.; Johnson, C.K.; Greig, D.J.; Kramer, S.; Che, X.; Wells, H.; Hicks, A.L.; Joly, D.O.; Wolfe, N.D.; Daszak, P.; et al. Global patterns in coronavirus diversity. Virus Evol. 2017, 3, vex012. [Google Scholar] [CrossRef]
- Brook, C.E.; Dobson, A.P. Bats as 'special' reservoirs for emerging zoonotic pathogens. Trends Microbiol. 2015, 23, 172–180. [Google Scholar] [CrossRef]
- Hansen, M.C.; Stehman, S.V.; Potapov, P.V.; Loveland, T.R.; Townshend, J.R.; DeFries, R.S.; Pittman, K.W.; Arunarwati, B.; Stolle, F.; Steininger, M.K.; et al. Humid tropical forest clearing from 2000 to 2005 quantified by using multitemporal and multiresolution remotely sensed data. Proc. Natl. Acad. Sci. United States Am. 2008, 105, 9439–9444. [Google Scholar] [CrossRef] [PubMed]
- Ellwanger, J.H.; Kulmann-Leal, B.; Kaminski, V.L.; Valverde-Villegas, J.M.; Veiga, A.; Spilki, F.R.; Fearnside, P.M.; Caesar, L.; Giatti, L.L.; Wallau, G.L.; et al. Beyond diversity loss and climate change: Impacts of Amazon deforestation on infectious diseases and public health. An. Da Acad. Bras. De Cienc. 2020, 92, e20191375. [Google Scholar] [CrossRef]
- Chapman, C.A.; Bicca-Marques, J.C.; Dunham, A.E.; Fan, P.; Fashing, P.J.; Gogarten, J.F.; Guo, S.; Huffman, M.A.; Kalbitzer, U.; Li, B.; et al. Primates Can Be a Rallying Symbol to Promote Tropical Forest Restoration. Folia Primatol. ; Int. J. Primatol. 2020, 91, 669–687. [Google Scholar] [CrossRef]
- Tuells, J.; Henao-Martínez, A.F.; Franco-Paredes, C. Yellow Fever: A Perennial Threat. Arch. Med. Res. 2022, 53, 649–657. [Google Scholar] [CrossRef]
- Weaver, S.C.; Reisen, W.K. Present and future arboviral threats. Antivir. Res. 2010, 85, 328–345. [Google Scholar] [CrossRef] [PubMed]
- de Thoisy, B.; Silva, N.I.O.; Sacchetto, L.; de Souza Trindade, G.; Drumond, B.P. Spatial epidemiology of yellow fever: Identification of determinants of the 2016-2018 epidemics and at-risk areas in Brazil. PLoS Neglected Trop. Dis. 2020, 14, e0008691. [Google Scholar] [CrossRef] [PubMed]
- Orkin, J.D.; Kuderna, L.F.K.; Marques-Bonet, T. The Diversity of Primates: From Biomedicine to Conservation Genomics. Annu. Rev. Anim. Biosci. 2021, 9, 103–124. [Google Scholar] [CrossRef]
- Rulli, M.C.; Santini, M.; Hayman, D.T.; D'Odorico, P. The nexus between forest fragmentation in Africa and Ebola virus disease outbreaks. Sci. Rep. 2017, 7, 41613. [Google Scholar] [CrossRef] [PubMed]
- Olivero, J.; Fa, J.E.; Real, R.; Márquez, A.L.; Farfán, M.A.; Vargas, J.M.; Gaveau, D.; Salim, M.A.; Park, D.; Suter, J.; et al. Recent loss of closed forests is associated with Ebola virus disease outbreaks. Sci. Rep. 2017, 7, 14291. [Google Scholar] [CrossRef]
- McCrone, J.T.; Lauring, A.S. Genetic bottlenecks in intraspecies virus transmission. Curr. Opin. Virol. 2018, 28, 20–25. [Google Scholar] [CrossRef]
- Wang, D.; Wang, Y.; Sun, W.; Zhang, L.; Ji, J.; Zhang, Z.; Cheng, X.; Li, Y.; Xiao, F.; Zhu, A.; et al. Population Bottlenecks and Intra-host Evolution During Human-to-Human Transmission of SARS-CoV-2. Front. Med. 2021, 8, 585358. [Google Scholar] [CrossRef] [PubMed]
- Plowright, R.K.; Parrish, C.R.; McCallum, H.; Hudson, P.J.; Ko, A.I.; Graham, A.L.; Lloyd-Smith, J.O. Pathways to zoonotic spillover. Nat. Rev.. Microbiol. 2017, 15, 502–510. [Google Scholar] [CrossRef] [PubMed]
- Ellwanger, J.H.; Chies, J.A.B. Zoonotic spillover: Understanding basic aspects for better prevention. Genet. Mol. Biol. 2021, 44, e20200355. [Google Scholar] [CrossRef] [PubMed]
- Sánchez, C.A.; Venkatachalam-Vaz, J.; Drake, J.M. Spillover of zoonotic pathogens: A review of reviews. Zoonoses Public Health 2021, 68, 563–577. [Google Scholar] [CrossRef] [PubMed]
- Cross, A.R.; Baldwin, V.M.; Roy, S.; Essex-Lopresti, A.E.; Prior, J.L.; Harmer, N.J. Zoonoses under our noses. Microbes Infect. 2019, 21, 10–19. [Google Scholar] [CrossRef] [PubMed]
- Daszak, P.; Cunningham, A.A.; Hyatt, A.D. Emerging infectious diseases of wildlife--threats to biodiversity and human health. Sci. (New York N.Y.) 2000, 287, 443–449. [Google Scholar] [CrossRef] [PubMed]
- Fan, Y.; Zhao, K.; Shi, Z.L.; Zhou, P. Bat Coronaviruses in China. Viruses 2019, 11. [Google Scholar] [CrossRef] [PubMed]
- Galindo-González, J. Live animal markets: Identifying the origins of emerging infectious diseases. Curr. Opin. Environ. Sci. Health 2022, 25, 100310. [Google Scholar] [CrossRef] [PubMed]
- Hollenbeck, J.E. Interaction of the role of Concentrated Animal Feeding Operations (CAFOs) in Emerging Infectious Diseases (EIDS). Infect. Genet. Evol. : J. Mol. Epidemiol. Evol. Genet. Infect. Dis. 2016, 38, 44–46. [Google Scholar] [CrossRef] [PubMed]
- Collin, É.; Périé, P.; Touboul, H. [Livestock-related zoonoses]. La Rev. Du Prat. 2019, 69, 328–332. [Google Scholar]
- Ashbolt, N.J. Microbial contamination of drinking water and disease outcomes in developing regions. Toxicology 2004, 198, 229–238. [Google Scholar] [CrossRef] [PubMed]
- Bondeson, L. Assessment of measures to prevent disease associated with animals in agricultural fairs--Maine, 2008. Am. J. Infect. Control 2009, 37, 665–667. [Google Scholar] [CrossRef]
- Tizard, I.R. Vaccination against coronaviruses in domestic animals. Vaccine 2020, 38, 5123–5130. [Google Scholar] [CrossRef] [PubMed]
- Hossain, A.D.; Jarolimova, J.; Elnaiem, A.; Huang, C.X.; Richterman, A.; Ivers, L.C. Effectiveness of contact tracing in the control of infectious diseases: a systematic review. Lancet Public Health 2022. [Google Scholar] [CrossRef] [PubMed]
- Destoumieux-Garzón, D.; Mavingui, P.; Boetsch, G.; Boissier, J.; Darriet, F.; Duboz, P.; Fritsch, C.; Giraudoux, P.; Le Roux, F.; Morand, S. The one health concept: 10 years old and a long road ahead. Front. Vet. Sci. 2018, 14. [Google Scholar] [CrossRef]
- Gow, N.A.; Johnson, C.; Berman, J.; Coste, A.T.; Cuomo, C.A.; Perlin, D.S.; Bicanic, T.; Harrison, T.S.; Wiederhold, N.; Bromley, M. The importance of antimicrobial resistance in medical mycology. Nat. Commun. 2022, 13, 5352. [Google Scholar] [CrossRef] [PubMed]
- Chebbac, K.; Ghneim, H.K.; El Moussaoui, A.; Bourhia, M.; El Barnossi, A.; Benziane Ouaritini, Z.; Salamatullah, A.M.; Alzahrani, A.; Aboul-Soud, M.A.; Giesy, J.P. Antioxidant and antimicrobial activities of chemically-characterized essential oil from Artemisia aragonensis Lam. against drug-resistant microbes. Molecules 2022, 27, 1136. [Google Scholar] [CrossRef] [PubMed]
- Mallah, N.; Orsini, N.; Figueiras, A.; Takkouche, B. Education level and misuse of antibiotics in the general population: a systematic review and dose–response meta-analysis. Antimicrob. Resist. Infect. Control 2022, 11, 1–22. [Google Scholar] [CrossRef]
- Shah, S.; Kasarla, R.R.; Yadav, N.S.; Shrestha, A.; Gautam, S.; Chaudhary, S.K. Antibiotic Resistance in Clinical Medicine. J. Univers. Coll. Med. Sci. 2022, 10, 66–71. [Google Scholar] [CrossRef]
- Sharma, J.; Sharma, D.; Singh, A.; Sunita, K. Colistin Resistance and Management of Drug Resistant Infections. Can. J. Infect. Dis. Med. Microbiol. 2022, 2022. [Google Scholar] [CrossRef]
- Jama, K. Socioeconomic Determinants of Antibiotic Resistance. 2022.
- Murugaiyan, J.; Kumar, P.A.; Rao, G.S.; Iskandar, K.; Hawser, S.; Hays, J.P.; Mohsen, Y.; Adukkadukkam, S.; Awuah, W.A.; Jose, R.A.M. Progress in alternative strategies to combat antimicrobial resistance: Focus on antibiotics. Antibiotics 2022, 11, 200. [Google Scholar] [CrossRef] [PubMed]
- Tiberi, S.; Utjesanovic, N.; Galvin, J.; Centis, R.; D'Ambrosio, L.; van den Boom, M.; Zumla, A.; Migliori, G.B. Drug resistant TB–latest developments in epidemiology, diagnostics and management. Int. J. Infect. Dis. 2022, 124, S20–S25. [Google Scholar] [CrossRef] [PubMed]
- Delany, I.; Rappuoli, R.; De Gregorio, E. Vaccines for the 21st century. EMBO Mol. Med. 2014, 6, 708–720. [Google Scholar] [CrossRef]
- Ophir, Y.; Walter, N.; Walter, D.; Velho, R.M.; Lokmanoglu, A.D.; Pruden, M.L.; Andrews, E.A. Vaccine hesitancy under the magnifying glass: A systematic review of the uses and misuses of an increasingly popular construct. Health Commun. 2022, 1–15. [Google Scholar] [CrossRef]
- Espindola, J.; Vaca, M. On the morality of vaccination tourism. Bioethics 2022, 36, 93–99. [Google Scholar] [CrossRef] [PubMed]
- Nan, Y.; Wu, C.; Zhao, Q.; Sun, Y.; Zhang, Y.J.; Zhou, E.M. Vaccine Development against Zoonotic Hepatitis E Virus: Open Questions and Remaining Challenges. Front. Microbiol. 2018, 9, 266. [Google Scholar] [CrossRef] [PubMed]
- Quan, L.; Al-Ansi, A.; Ariza-Montes, A.; Arraño-Muñoz, M.; Giorgi, G.; Han, H. Vaccine Passport and Traveler Behaviors in the New Market of the Domestic and International Tourism Industry Facing the With-Corona Era. Front. Psychol. 2022, 13, 900976. [Google Scholar] [CrossRef]
- Yuan, J.; Lam, W.T.W.; Xiao, J.; Ni, Y.M.; Cowling, B.J.; Liao, Q. Why do Chinese older adults in Hong Kong delay or refuse COVID-19 vaccination? A qualitative study based on Grounded Theory. J. Gerontol.. Ser. B Psychol. Sci. Soc. Sci. 1093. [Google Scholar] [CrossRef]
- Nurmi, J.; Harman, B. Why do parents refuse childhood vaccination? Reasons reported in Finland. Scand. J. Public Health 2022, 50, 490–496. [Google Scholar] [CrossRef]
- Wiysonge, C.S.; Ndwandwe, D.; Ryan, J.; Jaca, A.; Batouré, O.; Anya, B.M.; Cooper, S. Vaccine hesitancy in the era of COVID-19: could lessons from the past help in divining the future? Hum. Vaccines Immunother. 2022, 18, 1–3. [Google Scholar] [CrossRef]
- Kricorian, K.; Civen, R.; Equils, O. COVID-19 vaccine hesitancy: misinformation and perceptions of vaccine safety. Hum. Vaccines Immunother. 2022, 18, 1950504. [Google Scholar] [CrossRef]
- Patwary, M.M.; Alam, M.A.; Bardhan, M.; Disha, A.S.; Haque, M.Z.; Billah, S.M.; Kabir, M.P.; Browning, M.H.; Rahman, M.M.; Parsa, A.D. COVID-19 vaccine acceptance among low-and lower-middle-income countries: a rapid systematic review and meta-analysis. Vaccines 2022, 10, 427. [Google Scholar] [CrossRef] [PubMed]
- Bartoszko, J.; Loeb, M. The burden of influenza in older adults: meeting the challenge. Aging Clin. Exp. Res. 2021, 33, 711–717. [Google Scholar] [CrossRef] [PubMed]
- Yeo, J.Y.; Gan, S.K. Peering into Avian Influenza A(H5N8) for a Framework towards Pandemic Preparedness. Viruses 2021, 13. [Google Scholar] [CrossRef]
- Choi, M.J.; Yun, J.W.; Song, J.Y.; Ko, K.; Mould, J.F.; Cheong, H.J. A Comparative Analysis of Influenza-Associated Disease Burden with Different Influenza Vaccination Strategies for the Elderly Population in South Korea. Vaccines 2022, 10. [Google Scholar] [CrossRef] [PubMed]
- Zhang, R.; Hung, I.F. Approaches in broadening the neutralizing antibody response of the influenza vaccine. Expert Rev. Vaccines 2021, 20, 1539–1547. [Google Scholar] [CrossRef] [PubMed]
- Gottlieb, T.; Ben-Yedidia, T. Epitope-based approaches to a universal influenza vaccine. J. Autoimmun. 2014, 54, 15–20. [Google Scholar] [CrossRef]
- Semenza, J.C.; Rocklöv, J.; Ebi, K.L. Climate change and cascading risks from infectious disease. Infect. Dis. Ther. 2022, 11, 1371–1390. [Google Scholar] [CrossRef] [PubMed]
- Baker, R.E.; Mahmud, A.S.; Miller, I.F.; Rajeev, M.; Rasambainarivo, F.; Rice, B.L.; Takahashi, S.; Tatem, A.J.; Wagner, C.E.; Wang, L.-F. Infectious disease in an era of global change. Nat. Rev. Microbiol. 2022, 20, 193–205. [Google Scholar] [CrossRef] [PubMed]
- Mora, C.; McKenzie, T.; Gaw, I.M.; Dean, J.M.; von Hammerstein, H.; Knudson, T.A.; Setter, R.O.; Smith, C.Z.; Webster, K.M.; Patz, J.A. Over half of known human pathogenic diseases can be aggravated by climate change. Nat. Clim. Change 2022, 12, 869–875. [Google Scholar] [CrossRef]
- Rupasinghe, R.; Chomel, B.B.; Martínez-López, B. Climate change and zoonoses: A review of the current status, knowledge gaps, and future trends. Acta Trop. 2022, 226, 106225. [Google Scholar] [CrossRef]
- Wang, J.; Wah Yu, C.; Cao, S.-J. Urban development in the context of extreme flooding events. SAGE Publications Sage UK: London, England: 2022; Vol. 31, pp 3-6.
- Nazar, W.; Niedoszytko, M. Air pollution in Poland: A 2022 narrative review with focus on respiratory diseases. Int. J. Environ. Res. Public Health 2022, 19, 895. [Google Scholar] [CrossRef] [PubMed]
- Organization, W.H. Water for health: taking charge; World Health Organization (WHO): 2001.
- Holechek, J.L.; Geli, H.M.; Sawalhah, M.N.; Valdez, R. A global assessment: can renewable energy replace fossil fuels by 2050? Sustainability 2022, 14, 4792. [Google Scholar] [CrossRef]
- Yu, Z.; Khan, S.A.R.; Ponce, P.; Muhammad Zia-ul-haq, H.; Ponce, K. Exploring essential factors to improve waste-to-resource recovery: A roadmap towards sustainability. J. Clean. Prod. 2022, 350, 131305. [Google Scholar] [CrossRef]
- O. E. Olusegun, A. O. Anthony, O. E. O. R. CatherineTomilola, and C. U. Ogiesoba-Eguakun, "Public health concerns and water quality integrity of selected water sources in a peri-urban community," Sustainable Water Resources Management, vol. 8, no. 5, p. 150, 2022.
- Perera, F.; Nadeau, K. Climate change, fossil-fuel pollution, and children’s health. New Engl. J. Med. 2022, 386, 2303–2314. [Google Scholar] [CrossRef] [PubMed]
- Bloom, D.E.; Kuhn, M.; Prettner, K. Modern infectious diseases: macroeconomic impacts and policy responses. J. Econ. Lit. 2022, 60, 85–131. [Google Scholar] [CrossRef]
- Dhai, A. Are we preparing for the next pandemic? Health and Medical Publishing Group (HMPG): 2022; Vol. 15, pp 2-3.
- Kretzschmar, M.; Mangen, M.-J.J.; Pinheiro, P.; Jahn, B.; Fevre, E.M.; Longhi, S.; Lai, T.; Havelaar, A.H.; Stein, C.; Cassini, A. New methodology for estimating the burden of infectious diseases in Europe. PLoS Med. 2012, 9, e1001205. [Google Scholar] [CrossRef]
- Damaso, C.R. The 2022 monkeypox outbreak alert: Who is carrying the burden of emerging infectious disease outbreaks? Lancet Reg. Health–Am. 2022, 13. [Google Scholar] [CrossRef]
- Bhutta, Z.A.; Sommerfeld, J.; Lassi, Z.S.; Salam, R.A.; Das, J.K. Global burden, distribution, and interventions for infectious diseases of poverty. Infect. Dis. Poverty 2014, 3, 1–7. [Google Scholar] [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).



