Submitted:
11 October 2023
Posted:
12 October 2023
You are already at the latest version
Abstract

Keywords:
1. Introduction
2. Materials and Methods
- Approval and Consent
- Study Design
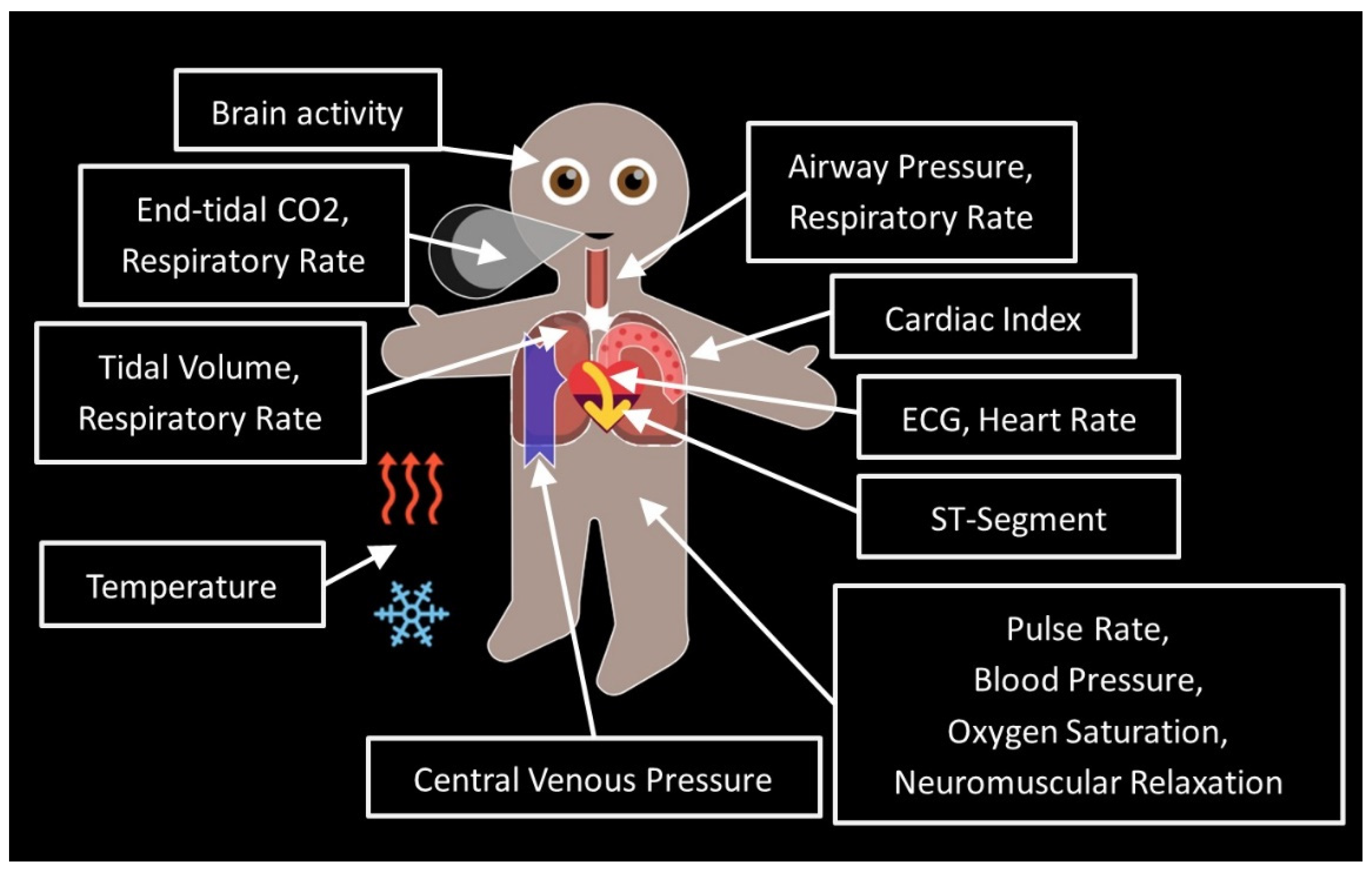
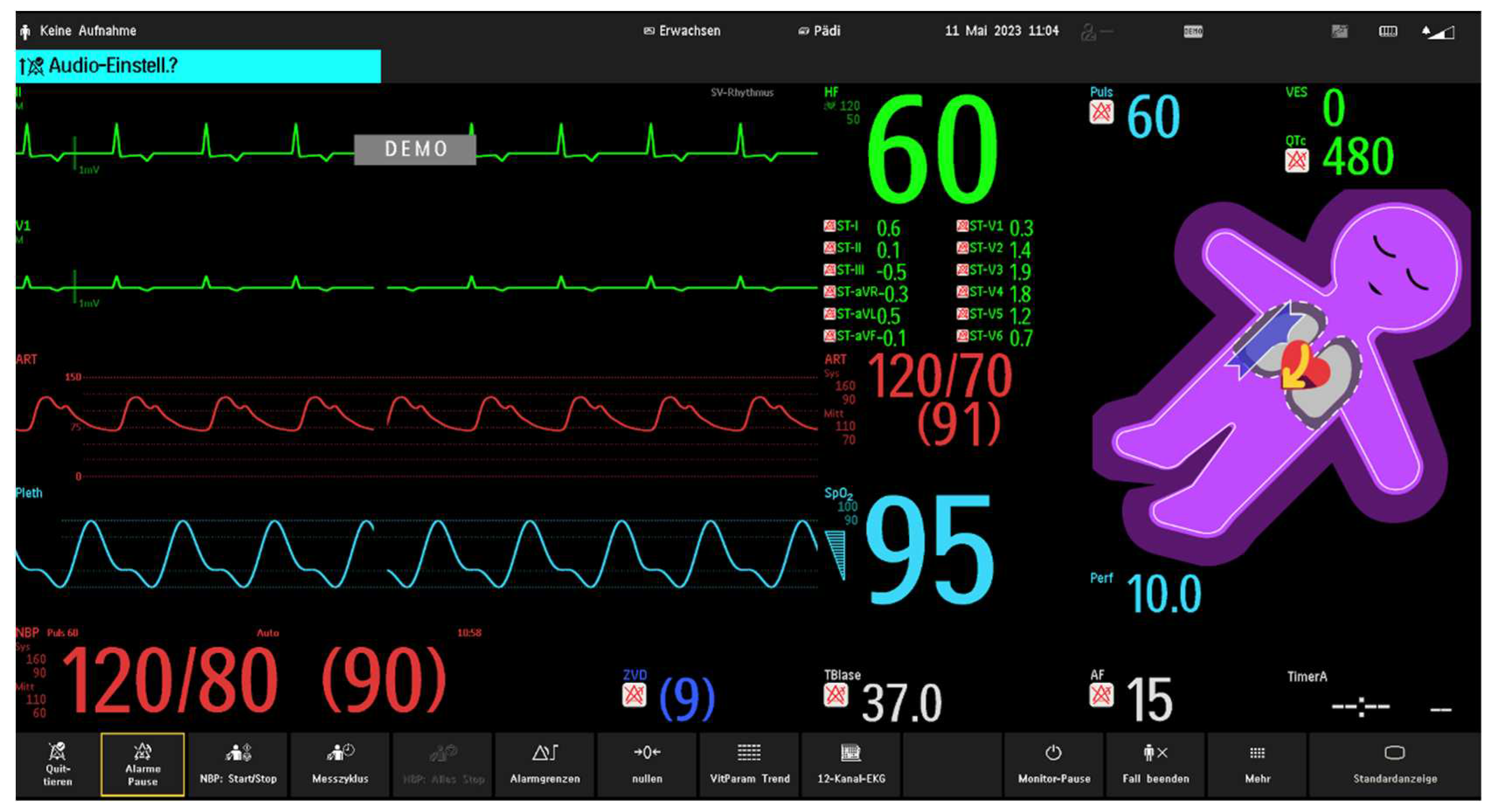
- Visual Patient Avatar in the Study Center
- Data Collection
- Data Analysis
- Open-ended Questions
- Demographic Data
3. Results
3.1. Participant Characteristics
| Participants (n = 14) | |
| Sex | |
| Female | 5 (35.7%) |
| Male | 9 (64.3%) |
| Participant age in years, median (IQR) | 42 (38–45) |
| Anesthesia experience in years, median (IQR) | 11 (6–14) |
| Role | |
| Certified nurse anesthetist | 4 (28.6%) |
| Resident 1–2 years of training | 1 (7.1%) |
| Resident 3–5 years of training | 1 (7.1%) |
| Resident with > 5 years of experience | 3 (21.4%) |
| Staff anesthesiologist | 5 (35.7%) |
| Educational material consulted | |
| Quick guide only | 4 (28.6%) |
| Tutorial video only | 0 |
| Both | 3 (21.4%) |
| None | 7 (50.0%) |
3.2. The Positive Impact of Visual Patient Avatar on Pediatric Anesthesia from Anesthesia Providers’ Perspective
3.2.1. Faster identification of problems through visual information, resulting in increased situation awareness
3.2.2. Usefulness of the tool for distracting children and reducing stress
3.3. Areas for Improvement of Visual Patient Avatar from Anesthesia Providers’ Perspective
3.3.1. Lack of Adaptability of the Visual Patient Avatar Thresholds for Children of Different Age Groups
3.3.2. Lack of quantitative information
3.4. Anesthesia Providers’ Comments on Children’s Reactions to Visual Patient Avatar
3.5. Anesthesia Providers’ Comments on Parents’ Reactions to Visual Patient Avatar
4. Discussion
Limitations and Strengths
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A
Appendix B
Appendix C
Appendix D
References
- Hashimoto, D.A.; et al. Artificial Intelligence in Anesthesiology: Current Techniques, Clinical Applications, and Limitations. Anesthesiology 2020, 132, 379–394. [Google Scholar] [CrossRef]
- Topol, E.J. High-performance medicine: the convergence of human and artificial intelligence. Nat Med 2019, 25, 44–56. [Google Scholar] [CrossRef] [PubMed]
- Drews, F.A. Patient monitors in critical care: Lessons for improvement. Advances in patient safety: new directions and alternative approaches (vol. 3: Performance and tools). 2008.
- Tscholl, D.W.; et al. Situation Awareness-Oriented Patient Monitoring with Visual Patient Technology: A Qualitative Review of the Primary Research. Sensors 2020, 20, 2112. [Google Scholar] [CrossRef] [PubMed]
- Endsley, M.R. Designing for Situation Awareness: An Approach to User-Centered Design, 2nd ed.CRC Press Inc.: Boca Raton, FL, USA, 2011. [Google Scholar]
- Oury, J.D.; Ritter, F.E.; Oury, J.D.; Ritter, F.E. How User-Centered Design Supports Situation Awareness for Complex Interfaces. In Building Better Interfaces for Remote Autonomous Systems: An Introduction for Systems Engineers; 2021. [Google Scholar]
- Katz, D. Gestalt psychology: its nature and significance. 1950.
- Wagemans, J.; et al. A century of Gestalt psychology in visual perception: I. Perceptual grouping and figure–ground organization. Psychological bulletin 2012, 138, 1172. [Google Scholar] [CrossRef]
- Croskerry, P. Clinical cognition and diagnostic error: applications of a dual process model of reasoning. Advances in health sciences education 2009, 14, 27–35. [Google Scholar] [CrossRef]
- Kahneman, D. Thinking, fast and slow. macmillan, 2011.
- Roche, T.R.; et al. Avatar-based patient monitoring in critical anaesthesia events: a randomised high-fidelity simulation study. Br J Anaesth 2021, 126, 1046–1054. [Google Scholar] [CrossRef]
- Reader, T.W.; et al. Team situation awareness and the anticipation of patient progress during ICU rounds. BMJ Qual Saf 2011, 20, 1035–1042. [Google Scholar] [CrossRef]
- Schulz, C.M.; et al. Situation awareness in anesthesia: concept and research. Anesthesiology 2013, 118, 729–742. [Google Scholar] [CrossRef]
- Schulz, C.M.; et al. Frequency and Type of Situational Awareness Errors Contributing to Death and Brain Damage: A Closed Claims Analysis. Anesthesiology 2017, 127, 326–337. [Google Scholar] [CrossRef] [PubMed]
- Schulz, C.M.; et al. Situation awareness errors in anesthesia and critical care in 200 cases of a critical incident reporting system. BMC Anesthesiol 2016, 16, 4. [Google Scholar] [CrossRef] [PubMed]
- Tscholl, D.W.; et al. Using an animated patient avatar to improve perception of vital sign information by anaesthesia professionals. Br J Anaesth 2018, 121, 662–671. [Google Scholar] [CrossRef]
- Tscholl, D.W.; et al. User perceptions of avatar-based patient monitoring: a mixed qualitative and quantitative study. BMC Anesthesiol 2018, 18, 188. [Google Scholar] [CrossRef]
- Bergauer, L.; Braun, J.; Roche, T.R.; Meybohm, P.; Hottenrott, S.; Zacharowski, K.; Raimann, F.J.; Rivas, E.; López-Baamonde, M.; Ganter, M.T.; Nöthiger, C.B. Avatar-based patient monitoring for intensive care units improves information transfer, diagnostic confidence and decreases perceived workload—A computer-based, multicentre comparison study. Sci Rep 2023, 13. [Google Scholar] [CrossRef] [PubMed]
- Garot, O.; et al. Avatar-based versus conventional vital sign display in a central monitor for monitoring multiple patients: a multicenter computer-based laboratory study. BMC Med Inform Decis Mak 2020, 20, 26. [Google Scholar] [CrossRef]
- Tscholl, D.W.; et al. The Mechanisms Responsible for Improved Information Transfer in Avatar-Based Patient Monitoring: Multicenter Comparative Eye-Tracking Study. J Med Internet Res 2020, 22, e15070. [Google Scholar] [CrossRef] [PubMed]
- Braun, V.; Clarke, V. Using Thematic Analysis in Psychology. Qualitative Research in Psychology 2006, 3, 77–101. [Google Scholar] [CrossRef]
- Fortier, M.A.; et al. Perioperative anxiety in children. Paediatr Anaesth 2010, 20, 318–322. [Google Scholar] [CrossRef] [PubMed]
- Kain, Z.N.; et al. Preoperative anxiety, postoperative pain, and behavioral recovery in young children undergoing surgery. Pediatrics 2006, 118, 651–658. [Google Scholar] [CrossRef] [PubMed]
- Wright, K.D.; et al. Prevention and intervention strategies to alleviate preoperative anxiety in children: a critical review. Behav Modif 2007, 31, 52–79. [Google Scholar] [CrossRef] [PubMed]
- Kain, Z.N.; et al. Preoperative anxiety in children. Predictors and outcomes. Arch Pediatr Adolesc Med 1996, 150, 1238. [Google Scholar] [CrossRef]
- Caldas, J.C.; Pais-Ribeiro, J.L.; Carneiro, S.R. General anesthesia, surgery and hospitalization in children and their effects upon cognitive, academic, emotional and sociobehavioral development—A review. Paediatr Anaesth 2004, 14, 910–915. [Google Scholar] [CrossRef] [PubMed]
- Kain, Z.N.; et al. Preoperative anxiety and emergence delirium and postoperative maladaptive behaviors. Anesth Analg 2004, 99, 1648–1654. [Google Scholar] [CrossRef] [PubMed]
- Vagnoli, L.; et al. Clown doctors as a treatment for preoperative anxiety in children: a randomized, prospective study. Pediatrics 2005, 116, e563-7. [Google Scholar] [CrossRef] [PubMed]
- Wennström, B.; Hallberg, L.R.; Bergh, I. Use of perioperative dialogues with children undergoing day surgery. J Adv Nurs 2008, 62, 96–106. [Google Scholar] [CrossRef]
- Tscholl, D.W.; et al. The Mechanisms Responsible for Improved Information Transfer in Avatar-Based Patient Monitoring: Multicenter Comparative Eye-Tracking Study. J Med Internet Res 2020, 22, e15070. [Google Scholar] [CrossRef]
- Atieno, O.P. An analysis of the strengths and limitation of qualitative and quantitative research paradigms. Problems of education in the 21stcentury 2009, 13. [Google Scholar]
| The Positive impact of Visual Patient Avatar on pediatric anesthesia | |
|
|
| Areas for improvement of Visual Patient Avatar in pediatric anesthesia | |
|
|
| Anesthesia Providers’ Comments on Children’s Reactions to Visual Patient Avatar | Anesthesia Providers’ Comments on Parents’ Reactions to Visual Patient Avatar |
|
|
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




