Submitted:
08 September 2023
Posted:
18 September 2023
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Inclusion and Exclusion Criteria
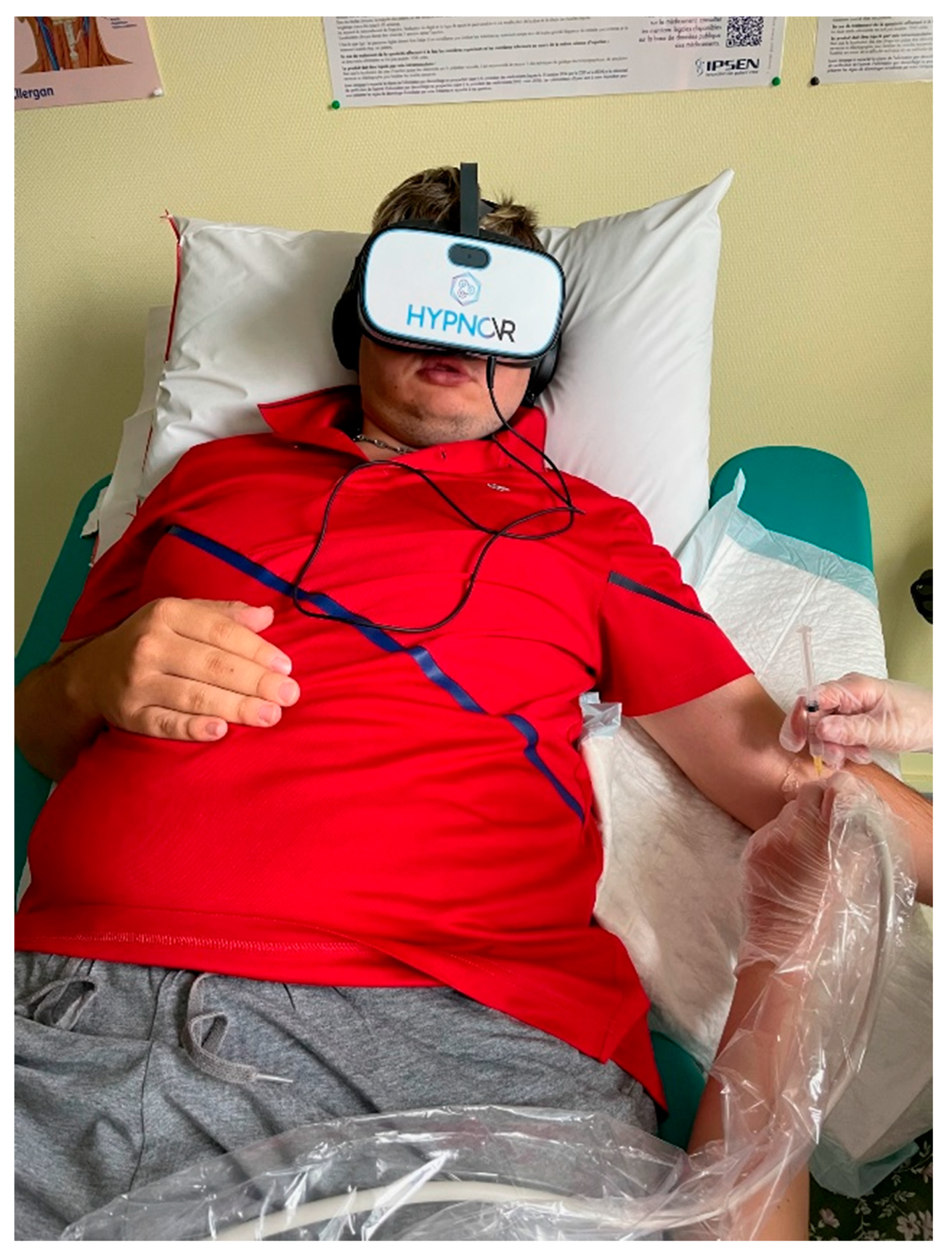
2.3. Procedure

2.4. Outcomes
2.5. Statistical Analysis
3. Results
3.1. Participants
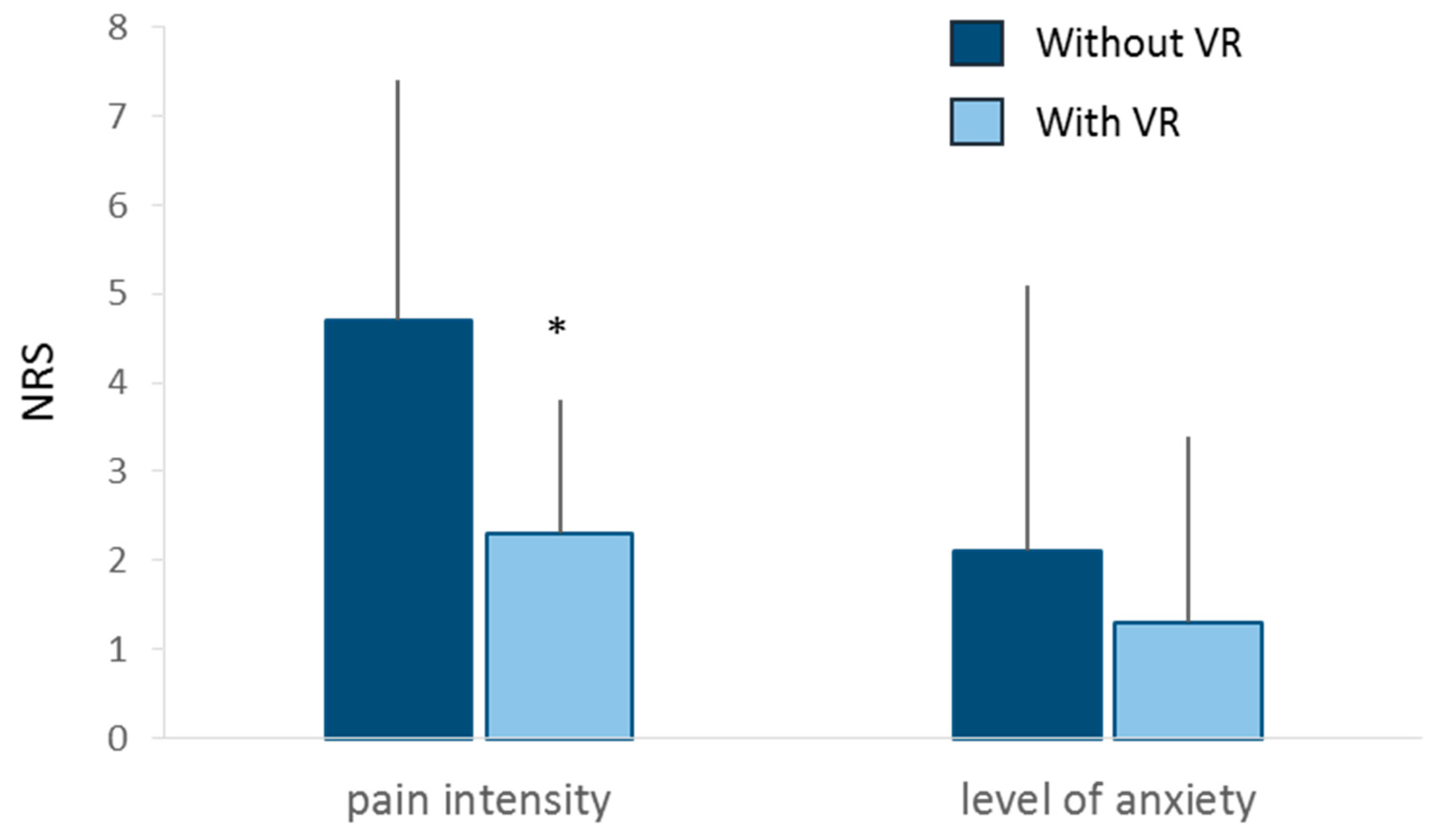
3.2. Primary and secondary outcomes
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Goudman L, Jansen J, De Smedt A, Billot M, Roulaud M, Rigoard P, et al. Virtual Reality during Intrathecal Pump Refills in Children: A Case Series. J Clin Med 2022;11:5877. [CrossRef]
- Chau JPC, Lo SHS, Choi KC, Butt L, Zhao J, Thompson DR. Participation self-efficacy plays a mediation role in the association between mobility and social participation among stroke survivors. Heart Lung J Crit Care 2021;50:857–62. [CrossRef]
- Afssaps. Recommandations de bonne pratique : Traitements médicamenteux de la spasticité. 2009.
- Cameron MH, Bethoux F, Davis N, Frederick M. Botulinum Toxin for Symptomatic Therapy in Multiple Sclerosis. Curr Neurol Neurosci Rep 2014;14:463. [CrossRef]
- Chaléat-Valayer E, Parratte B, Colin C, Denis A, Oudin S, Bérard C, et al. A French observational study of botulinum toxin use in the management of children with cerebral palsy: BOTULOSCOPE. Eur J Paediatr Neurol EJPN Off J Eur Paediatr Neurol Soc 2011;15:439–48. [CrossRef]
- Brochard S, Blajan V, Lempereur M, Garlantezec R, Houx L, Le Moine P, et al. Determining the technical and clinical factors associated with pain for children undergoing botulinum toxin injections under nitrous oxide and anesthetic cream. Eur J Paediatr Neurol EJPN Off J Eur Paediatr Neurol Soc 2011;15:310–5. [CrossRef]
- Mathevon L, Davoine P, Tardy M, Bouchet N, Gornushkina I, Pérennou D. Pain during botulinum toxin injections in spastic adults: Influence of patients’ clinical characteristics and of the procedure. Ann Phys Rehabil Med 2018;61:e359. [CrossRef]
- Fisher MT, Zigler CK, Houtrow AJ. Factors affecting procedural pain in children during and immediately after intramuscular botulinum toxin injections for spasticity. J Pediatr Rehabil Med 2018;11:193–7. [CrossRef]
- Bayon-Mottu M, Gambart G, Deries X, Tessiot C, Richard I, Dinomais M. Pain during injections of botulinum toxin in children: Influence of the localization technique. Ann Phys Rehabil Med 2014;57:578–86. [CrossRef]
- JOINDREAU-GAUDE V, NOËL N. Douleur et soins. In: Fondation Garches, Institut fédératif de recherche sur le handicap, editors. Handicap Douleur Actes 24es Entret. Fond. Garches Nanterre 24-25 Novembre 2011, Neuilly-Sur-Seine: Éd. GM Santé; 2011, p. 101–9.
- Francisco GE, Balbert A, Bavikatte G, Bensmail D, Carda S, Deltombe T, et al. A practical guide to optimizing the benefits of post-stroke spasticity interventions with botulinum toxin A: An international group consensus. J Rehabil Med 2021;53:jrm00134. [CrossRef]
- Nugud A, Alhoot S, Agabna M, Babiker MOE, El Bashir H. Analgesia and sedation modalities used with botulinum toxin injections in children with cerebral palsy: a literature review. Sudan J Paediatr 2021;21:6–12. [CrossRef]
- Fung S, Phadke CP, Kam A, Ismail F, Boulias C. Effect of topical anesthetics on needle insertion pain during botulinum toxin type A injections for limb spasticity. Arch Phys Med Rehabil 2012;93:1643–7. [CrossRef]
- Gubbay A, Langdon K. “Effectiveness of sedation using nitrous oxide compared with enteral midazolam for botulinum toxin A injections in children.” Dev Med Child Neurol 2009;51:491–2; author reply 492. [CrossRef]
- Nilsson S, Brunsson I, Askljung B, Påhlman M, Himmelmann K. A rectally administered combination of midazolam and ketamine was easy, effective and feasible for procedural pain in children with cerebral palsy. Acta Paediatr Oslo Nor 1992 2017;106:458–62. [CrossRef]
- Weiss RA, Lavin PT. Reduction of pain and anxiety prior to botulinum toxin injections with a new topical anesthetic method. Ophthal Plast Reconstr Surg 2009;25:173–7. [CrossRef]
- Gambart G, Mette F, Pellot A-S, Richard I. [Evaluation of analgesic protocol with nitrous oxide and EMLA cream during botulinum toxin injections in children]. Ann Readaptation Med Phys Rev Sci Soc Francaise Reeducation Fonct Readaptation Med Phys 2007;50:275–9. [CrossRef]
- Jones T, Moore T, Choo J. The Impact of Virtual Reality on Chronic Pain. PloS One 2016;11:e0167523. [CrossRef]
- Trost Z, France C, Anam M, Shum C. Virtual reality approaches to pain: toward a state of the science. Pain 2021;162:325–31. [CrossRef]
- Luque-Moreno C, Kiper P, Solís-Marcos I, Agostini M, Polli A, Turolla A, et al. Virtual Reality and Physiotherapy in Post-Stroke Functional Re-Education of the Lower Extremity: A Controlled Clinical Trial on a New Approach. J Pers Med 2021;11:1210. [CrossRef]
- Lambert V, Boylan P, Boran L, Hicks P, Kirubakaran R, Devane D, et al. Virtual reality distraction for acute pain in children. Cochrane Database Syst Rev 2020;10:CD010686. [CrossRef]
- Alemanno F, Houdayer E, Emedoli D, Locatelli M, Mortini P, Mandelli C, et al. Efficacy of virtual reality to reduce chronic low back pain: Proof-of-concept of a non-pharmacological approach on pain, quality of life, neuropsychological and functional outcome. PLOS ONE 2019;14:e0216858. [CrossRef]
- Smith V, Warty RR, Sursas JA, Payne O, Nair A, Krishnan S, et al. The Effectiveness of Virtual Reality in Managing Acute Pain and Anxiety for Medical Inpatients: Systematic Review. J Med Internet Res 2020;22:e17980. [CrossRef]
- Perrochon A, Borel B, Istrate D, Compagnat M, Daviet J-C. Exercise-based games interventions at home in individuals with a neurological disease: A systematic review and meta-analysis. Ann Phys Rehabil Med 2019;62:366–78. [CrossRef]
- Gold JI, Mahrer NE. Is Virtual Reality Ready for Prime Time in the Medical Space? A Randomized Control Trial of Pediatric Virtual Reality for Acute Procedural Pain Management. J Pediatr Psychol 2018;43:266–75. [CrossRef]
- Chau B, Chi B, Wilson T. Decreasing pediatric pain and agitation during botulinum toxin injections for spasticity with virtual reality: Lessons learned from clinical use. J Pediatr Rehabil Med 2018;11:199–204. [CrossRef]
- Sikka N, Shu L, Ritchie B, Amdur RL, Pourmand A. Virtual Reality-Assisted Pain, Anxiety, and Anger Management in the Emergency Department. Telemed J E-Health Off J Am Telemed Assoc 2019;25:1207–15. [CrossRef]
- Almugait M, AbuMostafa A. Author Correction: Comparison between the analgesic effectiveness and patients’ preference for virtual reality vs. topical anesthesia gel during the administration of local anesthesia in adult dental patients: a randomized clinical study. Sci Rep 2022;12:805. [CrossRef]
- Basak T, Demirtas A, Yorubulut SM. Virtual reality and distraction cards to reduce pain during intramuscular benzathine penicillin injection procedure in adults: A randomized controlled trial. J Adv Nurs 2021;77:2511–8. [CrossRef]
- Trompetto C, Marinelli L, Mori L, Puce L, Avanti C, Saretti E, et al. Effectiveness of Botulinum Toxin on Pain in Stroke Patients Suffering from Upper Limb Spastic Dystonia. Toxins 2022;14:39. [CrossRef]
- Baricich A, Battaglia M, Cuneo D, Cosenza L, Millevolte M, Cosma M, et al. Clinical efficacy of botulinum toxin type A in patients with traumatic brain injury, spinal cord injury, or multiple sclerosis: An observational longitudinal study. Front Neurol 2023;14:1133390. [CrossRef]
- Anwar K, Barnes MP. A pilot study of a comparison between a patient scored numeric rating scale and clinician scored measures of spasticity in multiple sclerosis. NeuroRehabilitation 2009;24:333–40. [CrossRef]
- Freitas L, de Araújo Val S, Magalhães F, Marinho V, Ayres C, Teixeira S, et al. Virtual reality exposure therapy for neuro-psychomotor recovery in adults: a systematic review. Disabil Rehabil Assist Technol 2021;16:646–52. [CrossRef]
- Mallari B, Spaeth EK, Goh H, Boyd BS. Virtual reality as an analgesic for acute and chronic pain in adults: a systematic review and meta-analysis. J Pain Res 2019;Volume 12:2053–85. [CrossRef]
- Eijlers R, Utens EMWJ, Staals LM, de Nijs PFA, Berghmans JM, Wijnen RMH, et al. Systematic Review and Meta-analysis of Virtual Reality in Pediatrics: Effects on Pain and Anxiety. Anesth Analg 2019;129:1344–53. [CrossRef]
- Johnson, MH. How does distraction work in the management of pain? Curr Pain Headache Rep 2005;9:90–5. [CrossRef]
- Indovina P, Barone D, Gallo L, Chirico A, De Pietro G, Giordano A. Virtual Reality as a Distraction Intervention to Relieve Pain and Distress During Medical Procedures: A Comprehensive Literature Review. Clin J Pain 2018;34:858–77. [CrossRef]
- Abiodun AO, Adesina MA. Virtual reality: a breakthrough in pain management? World News Nat Sci 2019:24–33.
- Wismeijer AAJ, Vingerhoets AJJM. The use of virtual reality and audiovisual eyeglass systems as adjunct analgesic techniques: a review of the literature. Ann Behav Med Publ Soc Behav Med 2005;30:268–78. [CrossRef]
- Rutter CE, Dahlquist LM, Weiss KE. Sustained efficacy of virtual reality distraction. J Pain 2009;10:391–7. [CrossRef]
- Birnie KA, Noel M, Parker JA, Chambers CT, Uman LS, Kisely SR, et al. Systematic review and meta-analysis of distraction and hypnosis for needle-related pain and distress in children and adolescents. J Pediatr Psychol 2014;39:783–808. [CrossRef]
- Koller D, Goldman RD. Distraction techniques for children undergoing procedures: a critical review of pediatric research. J Pediatr Nurs 2012;27:652–81. [CrossRef]
- Ventura S, Brivio E, Riva G, Baños RM. Immersive Versus Non-immersive Experience: Exploring the Feasibility of Memory Assessment Through 360° Technology. Front Psychol 2019;10:2509. [CrossRef]
- Goudman L, Jansen J, Billot M, Vets N, De Smedt A, Roulaud M, et al. Virtual Reality Applications in Chronic Pain Management: Systematic Review and Meta-analysis. JMIR Serious Games 2022;10:e34402. [CrossRef]
- Patterson DR, Hoffman HG, Chambers G, Bennetts D, Hunner HH, Wiechman SA, et al. Hypnotic Enhancement of Virtual Reality Distraction Analgesia during Thermal Pain: A Randomized Trial. Int J Clin Exp Hypn 2021;69:225–45. [CrossRef]
- Rousseaux F, Bicego A, Ledoux D, Massion P, Nyssen A-S, Faymonville M-E, et al. Hypnosis Associated with 3D Immersive Virtual Reality Technology in the Management of Pain: A Review of the Literature. J Pain Res 2020;13:1129–38. [CrossRef]
- Rousseaux F, Dardenne N, Massion PB, Ledoux D, Bicego A, Donneau A-F, et al. Virtual reality and hypnosis for anxiety and pain management in intensive care units: A prospective randomised trial among cardiac surgery patients. Eur J Anaesthesiol 2022;39:58–66. [CrossRef]
- Rousseaux F, Panda R, Toussaint C, Bicego A, Niimi M, Faymonville M-E, et al. Virtual reality hypnosis in the management of pain: Self-reported and neurophysiological measures in healthy subjects. Eur J Pain Lond Engl 2023;27:148–62. [CrossRef]
- Langlois P, Perrochon A, David R, Rainville P, Wood C, Vanhaudenhuyse A, et al. Hypnosis to manage musculoskeletal and neuropathic chronic pain: A systematic review and meta-analysis. Neurosci Biobehav Rev 2022;135:104591. [CrossRef]
- Bani Mohammad E, Ahmad M. Virtual reality as a distraction technique for pain and anxiety among patients with breast cancer: A randomized control trial. Palliat Support Care 2019;17:29–34. [CrossRef]
| Variables | mean ± SD / n (%) |
| Age (years) | 49.9 ± 10.6 |
| Sex Male Female |
8 (47.1%) |
| 9 (52.9%) | |
| Disease diagnosis Stroke Cerebral palsy Multiple sclerosis Cervical Myelopathy Hereditary spastic paraplegia Cerebrospinal meningitis |
9 (52.9%) |
| 3 (17.6%) | |
| 2 (11.8%) | |
| 1 (5.9%) | |
| 1 (5.9%) | |
| 1 (5.9%) | |
| Use of analgesic drugs No Yes |
14 (82,4%) |
| 3 (17,6%) | |
| Baseline pain intensity NRS (0-10) median (min-max) |
0 (0-4) |
| Trapezius | Levator scapulae | Pectoralis major | Pectoralis minor | Teres major | Deltoid | Biceps brachii | Brachialis | Brachioradialis | Triceps brachii | Pronator teres | Flexor carpi ulnaris | Flexor carpi radialis | Flexor digitorum superficialis | Flexor digitorum profundus | Flexor pollicis longus | Flexor pollicis brevis | Adductor pollicis | Abductor digiti minimi of hand | Interossei dorsales | |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Patient 1 | ||||||||||||||||||||
| Patient 2 | 1 | 1 | 1 | 1 | ||||||||||||||||
| Patient 3 | ||||||||||||||||||||
| Patient 4 | 1 | 1 | 1 | |||||||||||||||||
| Patient 5 | ||||||||||||||||||||
| Patient 6 | 1 | 1 | 1 | 1 | 1 | 1 | ||||||||||||||
| Patient 7 | ||||||||||||||||||||
| Patient 8 | ||||||||||||||||||||
| Patient 9 | 1 | 1 | 1 | 1 | 1 | 1 | ||||||||||||||
| Patient 10 | 1 | 1 | 1 | 1 | 1 | |||||||||||||||
| Patient 11 | 1 | 1 | ||||||||||||||||||
| Patient 12 | ||||||||||||||||||||
| Patient 13 | 1 | 1 | 1 | 1 | ||||||||||||||||
| Patient 14 | 1 | 1 | 1 | 1 | ||||||||||||||||
| Patient 15 | 1 | 1 | 1 | 1 | ||||||||||||||||
| Patient 16 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | ||||||||||||
| Patient 17 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | 1 | ||||||||||
| % | 1,1% | 1,1% | 3,4% | 1,1% | 1,1% | 1,1% | 4,5% | 10,1% | 3,4% | 1,1% | 1,1% | 3,4% | 3,4% | 7,9% | 6,7% | 2,2% | 1,1% | 3,4% | 2,2% | 3,4% |
| Rectus femoris | Adductor longus | Tibialis posterior | Gastrocnemius medial head | Gastrocnemius lateral head | Soleus | Flexor digitorum longus | Flexor hallucis longus | |
|---|---|---|---|---|---|---|---|---|
| Patient 1 | 1 | 1 | 1 | 1 | ||||
| Patient 2 | 1 | 1 | 1 | |||||
| Patient 3 | 1 | |||||||
| Patient 4 | ||||||||
| Patient 5 | 1 | 1 | 1 | 1 | ||||
| Patient 6 | ||||||||
| Patient 7 | 1 | 1 | 1 | |||||
| Patient 8 | 1 | 1 | 1 | 1 | 1 | 1 | ||
| Patient 9 | ||||||||
| Patient 10 | ||||||||
| Patient 11 | 1 | 1 | ||||||
| Patient 12 | 1 | 1 | ||||||
| Patient 13 | ||||||||
| Patient 14 | 1 | 1 | 1 | |||||
| Patient 15 | 1 | 1 | 1 | 1 | 1 | |||
| Patient 16 | ||||||||
| Patient 17 | ||||||||
| % | 3,4% | 2,2% | 5,6% | 7,9% | 7,9% | 7,9% | 1,1% | 1,1% |
| Variables | Without VR | With VR | p-value |
|---|---|---|---|
| Pain during procedure | 4.1 ± 2.7 | 2.3 ± 1.5 | 0.014 |
| Anxiety during procedure | 2.1 ± 3.0 | 1.3 ± 2.1 | 0.054 |
| Perceived percentage of improvement Pain intensity Level of Anxiety |
- |
39.7% ± 30.9% 21.5% ± 25.0% |
|
| Patient satisfaction (0-10) | - | 7.9 ± 1.6 | |
| Agreed to reuse VR for next injection Yes No |
- |
15 (88.2%) 2 (11.8%) |
|
| Does the patient recommend VR for other patients? Yes No |
- |
17 (100%) 0 (0%) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




