Submitted:
12 June 2023
Posted:
13 June 2023
Read the latest preprint version here
Abstract
Keywords:
1. Introduction
2. Methods
2.1. Search Strategy
2.2. Selection Criteria
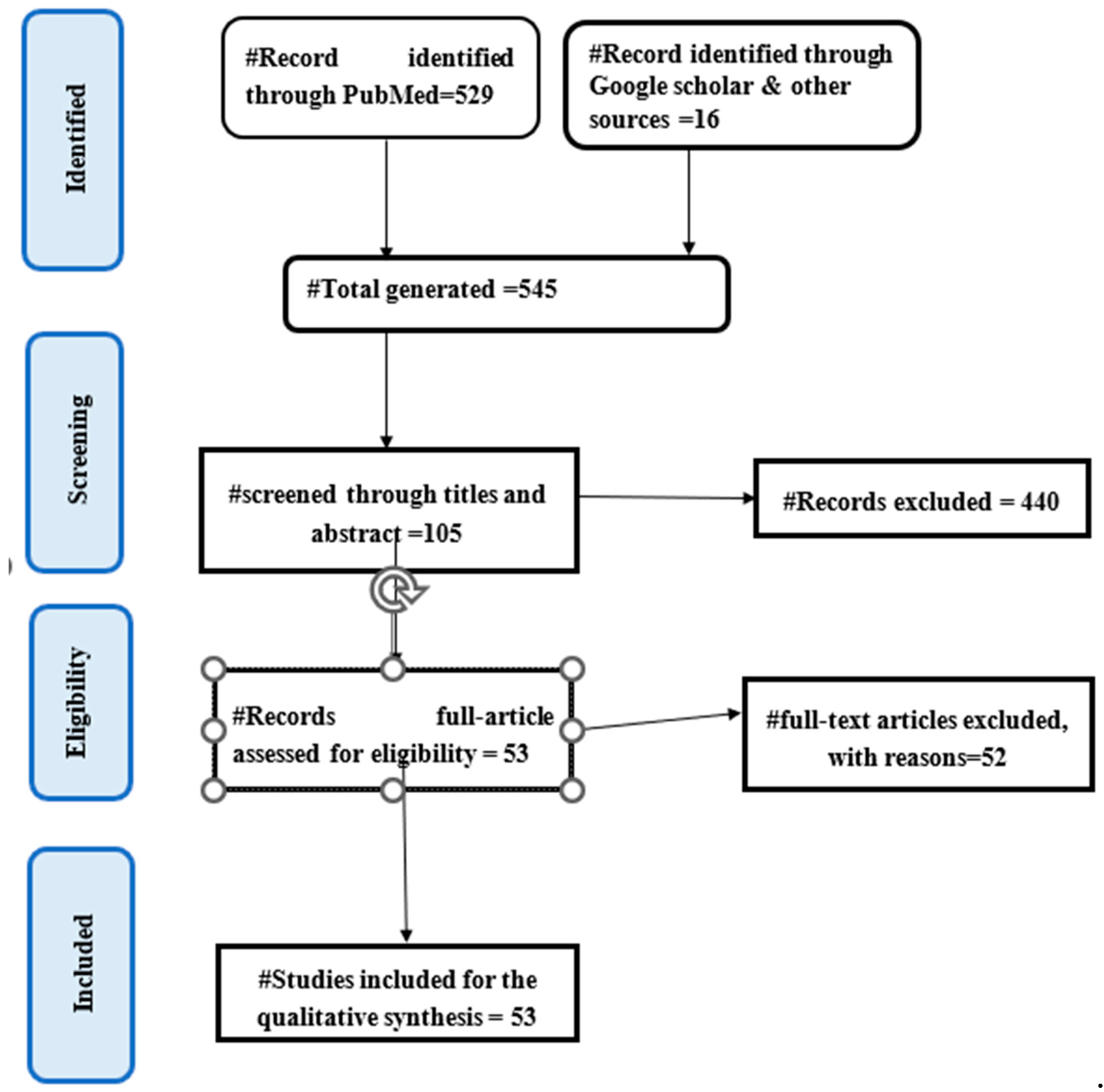
2.3. Study Selection Process
3. Global Epidemiology of Invasive H. Influenzae Disease
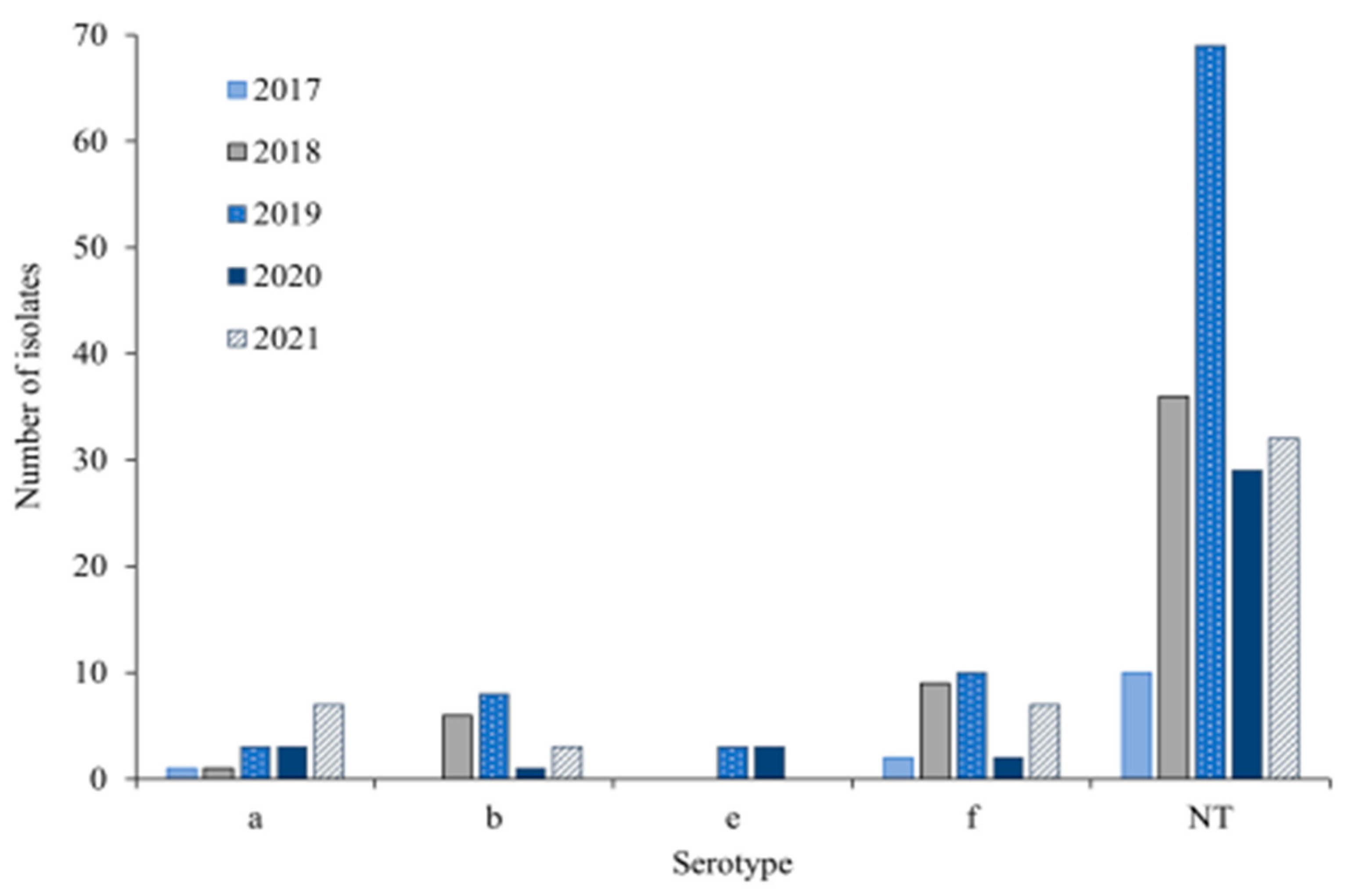
3.1. European Region (Euro)
3.2. African Region (AFR)
3.3. Region of the Americas (AMR)
3.4. South-East Asian Region (SEAR)
3.5. Eastern Mediterranean Region (EMR)
3.6. Western Pacific Region (WPR)
| Hi serotype | WHO Region | Country | Year | Specimen | Method used | Changes in incidence |
Incidence per 100,000*a | Vaccine | Ref | |||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Hia | AFRO | South Africa | 2017 | Blood | SA+PCR | Increased | 2.9 | No | [29] | |||
| Gambia | 2013 | Blood | SA+PCR | Not known | 10 | No | [30] | |||||
| AMR | USA | 2015 | Blood, CSF | SA or PCR | Increased | 8.3 | No | [11] | ||||
| Canada | 2021 | Blood, CSF | SA+PCR | Increased | 8.9 | No | [31] | |||||
| Brazil | 2000 | Blood | Not reported | Increased | 0.16 | No | [11] | |||||
| EURO | Portugal | 2018 | Blood, | PCR | Increased | 2.7 | No | [18] | ||||
| England | 2018 | Blood, | SA or PCR | Increased | 0.8 | No | [18] | |||||
| Germany | 2018 | Blood | Not reported | Decreased | 0.5 | No | [18] | |||||
| Hungary | 2017 | Blood | PCR | Not known | 5 | No | [18] | |||||
| Italy | Blood | SA or PCR | Increased | 0.02 | No | [11] | ||||||
| Ireland | 2009 | Blood | SA or PCR | Increased | 1 | No | [11] | |||||
| WPR | Australia | 2015 | Blood | SA+PCR | Increased | 6.4 | No | [17] | ||||
| Hib | AFR | South Africa | 2018 | Blood | PCR | Increased | 17 | Yes | [29] | |||
| Gambia | 2013 | Blood | PCR | Increased | 42 | Yes | [30] | |||||
| AMR | USA | 2018 | Blood | PCR+SA | Decreased | 0.02 | Yes | [11] | ||||
| Canada | 2018 | Blood, | SA+PCR | Decreased |
2.3 | Yes | [18] | |||||
| EURO | Portugal | 2018 | Blood, | PCR | Increased | 13.5 | Yes | [18] | ||||
| England | 2018 | Blood, | SA+PCR | Decreased | 1.2 | Yes | [18] | |||||
| Finland | 2018 | Blood,CSF | Not reported | Decreased | 3.5 | Yes | [18] | |||||
| Germany | 2018 | Blood | Not reported | Decreased | 2.4 | Yes | [11] | |||||
| Italy | 2018 | Blood | PCR | Increased | 11.5 | Yes | [11] | |||||
| Taiwan | 2002 | Blood | SA | Increased | 20 | Yes | [11] | |||||
| Hungary | 2017 | Blood | Not reported | Not known | 5 | Yes | [11] | |||||
| Ireland | 2018 | Blood | SA or PCR | Decreased | 2 | Yes | [32] | |||||
| EMR | Saudi Arabia | 2001 | Blood | PCR | Not reported | 40 | Yes | [24] | ||||
| UAE | 1999 | Blood | PCR | Not reported | 46 | Yes | [24] | |||||
| SEA | South Korea | 2001 | Blood | PCR | Not reported | 6.8 | Yes | [24] | ||||
| Philippine | 2000 | Blood | PCR | Increased | 95 | Yes | [24] | |||||
| Japan | 2007 | Blood | SA or PCR | Increased | 4.3 | Yes | [24] | |||||
| Singapore | 2007 | Blood | PCR | Decreased | 4.4 | Yes | [24] | |||||
| Taiwan | 2000 | Blood | PCR | Decreased | 3.2 | Yes | [24] | |||||
| Indonesia | 2005 | Blood | PCR | Increased | 67 | Yes | [24] | |||||
| WPR | Australia | 2013 | Blood, CSF | SA+PCR | Increased | 14.9 | Yes | [26] | ||||
| China | 2015 | Blood | SA or PCR | Increased | 74 | Yes | [11] | |||||
| Hong Kong | 2015 | Blood | SA+PCR | Increased | 2.7 | Yes | [11] | |||||
| Mongolia | 2008 | Blood | PCR or SA | Decreased | 2 | Yes | [11] | |||||
| Hic | AFR | South Africa | 2017 | Blood | PCR or SA | Not reported | 1.13 | No | [29] | |||
| Gambia | 2013 | Blood | PCR or SA | Not reported | 2 | No | [30] | |||||
| Hid | AFR | South Africa | 2017 | Blood | PCR or SA | Not reported | 0.31 | No | [29] | |||
| Gambia | 2017 | Blood | PCR or SA | Not reported | 2 | No | [30] | |||||
| AMR | Canada | 2018 | Blood,CSF | SA+PCR | Not reported | 0.1 | No | [18] | ||||
| Hif | AFR | South Africa | 2017 | Blood | SA+PCR | Not reported | 3.2 | No | [29] | |||
| Gambia | 2013 | Blood | SA+PCR | Not reported | 2 | No | [30] | |||||
| AMR | Canada | 2018 | Blood, | SA+PCR | Increased | 10.2 | No | [18] | ||||
| WPR | Australia | 2013 | Blood, CSF | SA+PCR | Increased | 10.6 | No | [18] | ||||
| EURO | England | 2018 | Blood | SA+PCR | Increased | 8.3 | No | [18] | ||||
| Germany | 2018 | Blood | Not reported | decreased | 9.8 | No | [11] | |||||
| Finland | 2018 | Blood | SA+PCR | Increased | 12.6 | No | [18] | |||||
| Portugal | 2018 | Blood, | PCR | Increased | 3.1 | No | [18] | |||||
| Italy | 2018 | Blood | SA+PCR | Increased | 4.6 | No | [11] | |||||
| Ireland | 2018 | Blood | SA+PCR | Increased | 7 | No | [32] | |||||
| Sweden | 2009 | Blood,CSF | PCR | Increased | 57 | No | [74] | |||||
| Hie | AFR | South Africa | 2017 | Blood | SA+PCR | Increase | 0.31 | No | [29] | |||
| Gambia | 2013 | Blood | Blood,CSF | Not known | 2 | No | [30] | |||||
| WPR | Australia | 2013 | Blood | SA+PCR | Increased | 14.9 | No | [18] | ||||
| EURO | Germany | 2018 | Blood | SA+PCR | Not reported | 2.4 | No | [11] | ||||
| Portugal | 2018 | Blood,CSF | PCR | Increased | 79.2 | No | [18] | |||||
| Portugal | 2018 | Blood,CSF | PCR | Increased | 1.5 | No | [18] | |||||
| Ireland | 2018 | Blood | SA+PCR | Increased | 6 | No | [32] | |||||
| NTHi | AFR | Gambia | 2013 | Blood | SA+PCR | Not known | 30 | No | [30] | |||
| South Africa | 2017 | Blood | Not reported | Increased | 64 | No | [29] | |||||
| AMR | Canada | 2018 | Blood, | SA+PCR | Increased | 74.2 | No | [18] | ||||
| USA | 2023 | Blood | SA+PCR | Increased | 92 | No | [33] | |||||
| SEA | Taiwan | 2002 | Blood | SA | Not Known | 80 | No | [27] | ||||
| EURO | Italy | 2018 | Blood | SA+PCR | Increased | 76.1 | No | [18] | ||||
| Germany | 2018 | Blood | Not reported | Increased | 84.5 | No | [18] | |||||
| Hungary | 2018 | Blood | SA+PCR | Increased | 79 | No | [11] | |||||
| Portugal | 2018 | Blood | PCR | Increased | 79.2 | No | [18] | |||||
| Finland | 2018 | Blood | SA+PCR | Increased | 79 | No | [18] | |||||
| Ireland | 2018 | Blood | SA+PCR | Increased | 83 | No | [32] | |||||
| Sweden | 2009 | Blood | PCR | Increased | 71 | No | [11] | |||||
| Spain |
2013 | Blood | SA | Increased | 85 | No | [27] | |||||
| Slovenia | 2008 | Blood | PCR | Increased | 85 | No |
[27] | |||||
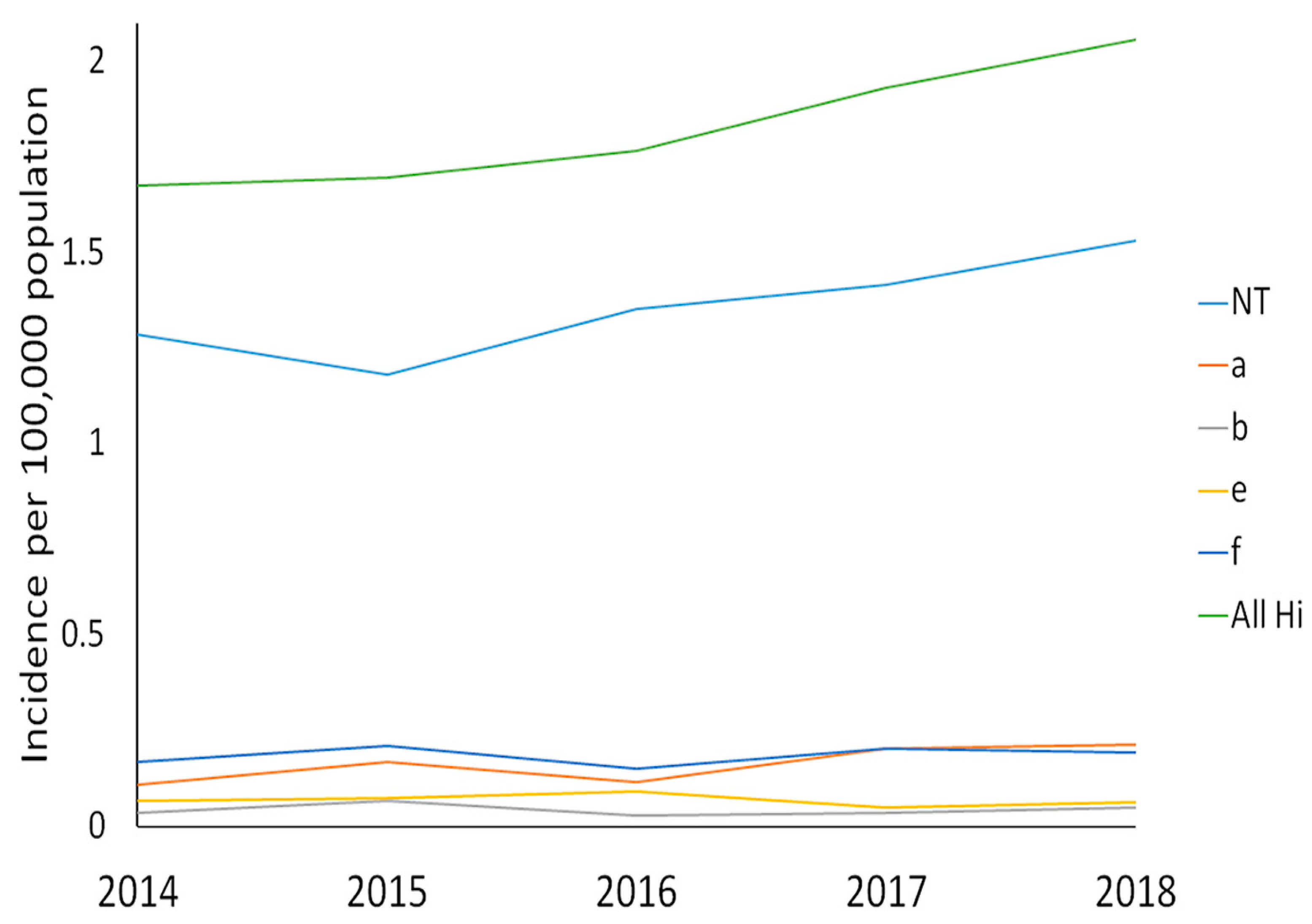
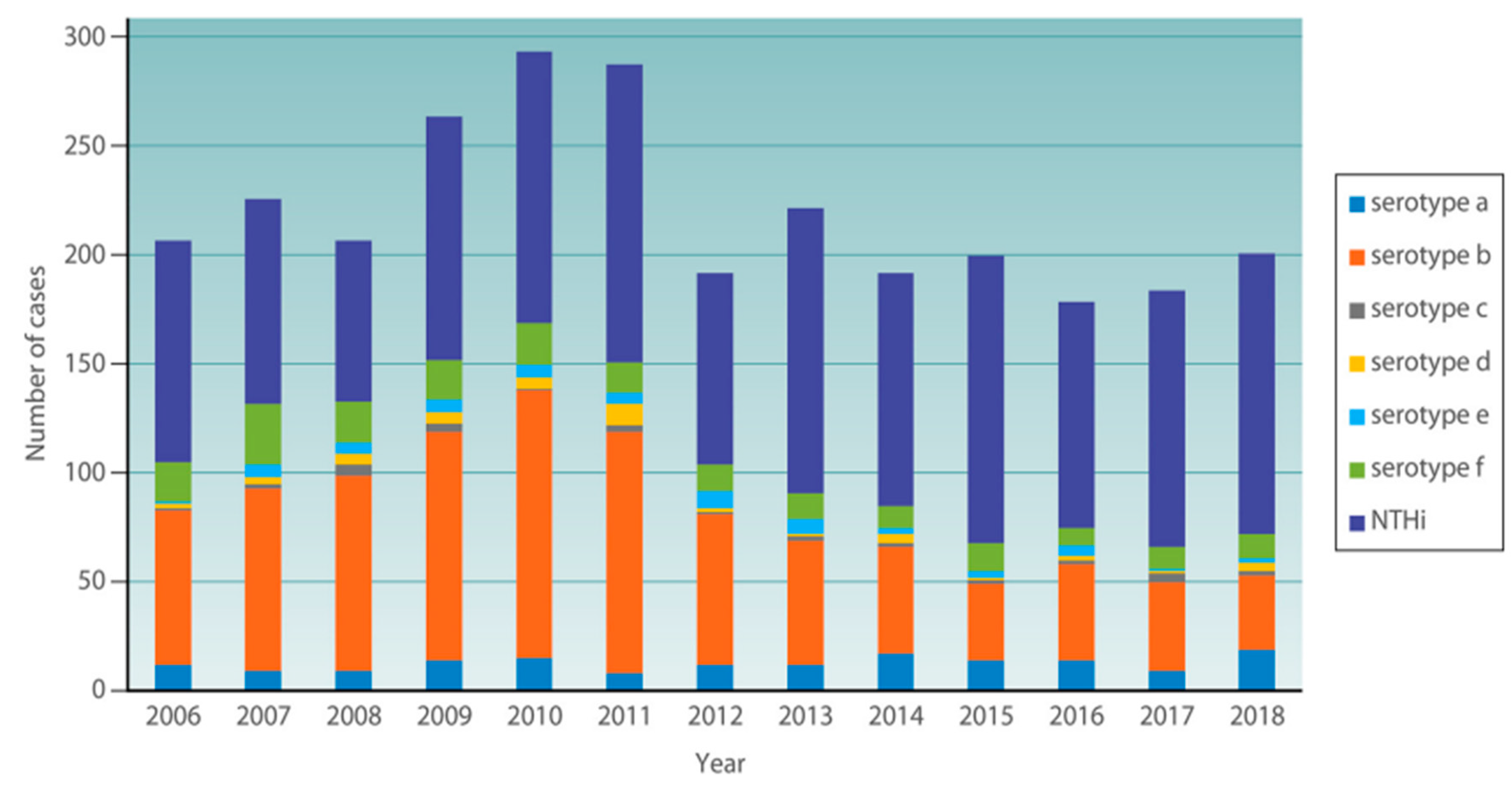
4. Pathogenesis
5. Genomic and molecular Characteristics
6. Emerging Invasive Haemophilus Influenzae Serotypes Disease
6.1. Invasiveness of Nontypeable Haemophilus influenzae (NTHi)
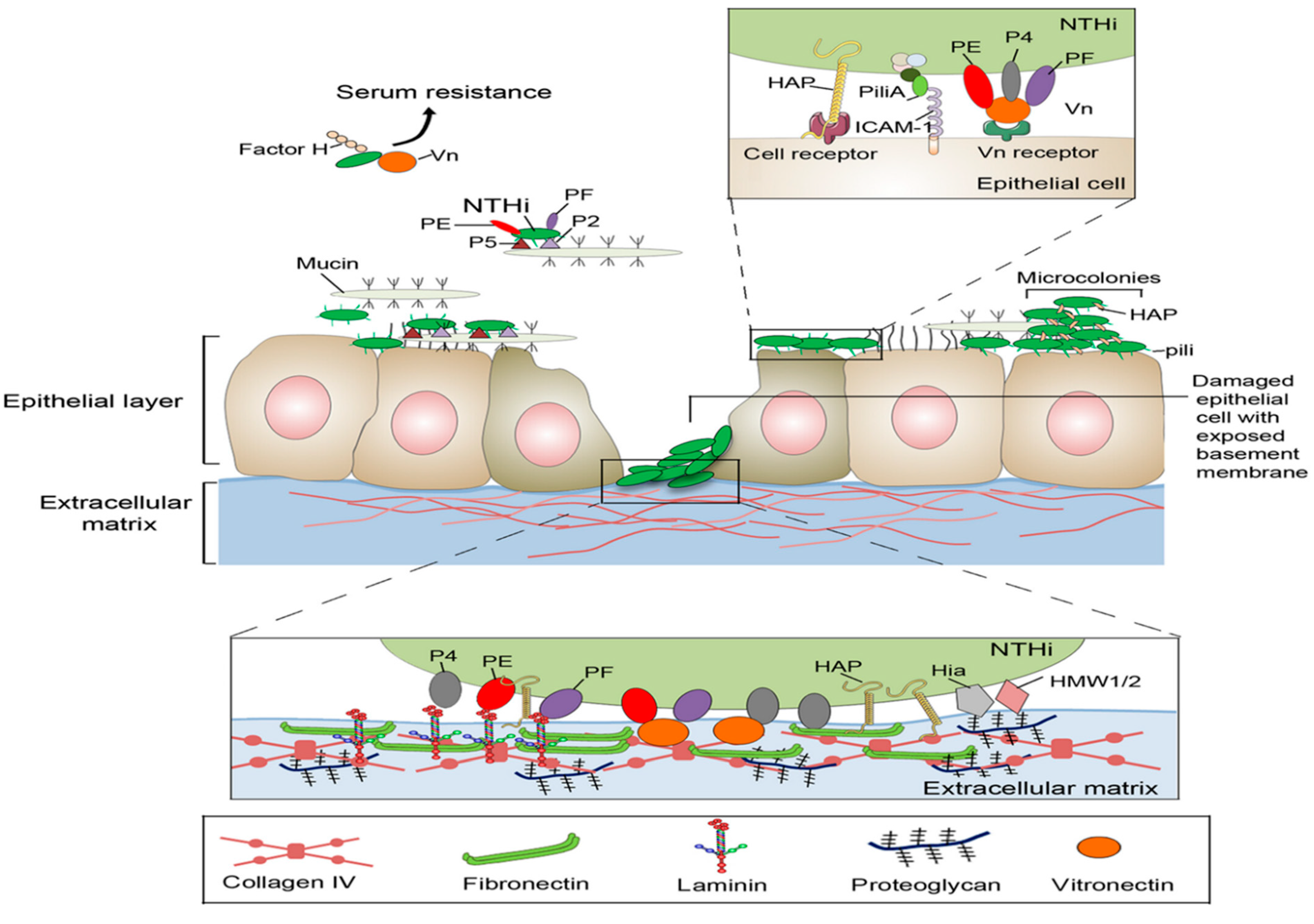
6.2. Invasiveness of typeable Haemophilus influenzae (a-f)
6.1.1. Haemophilus influenzae serotype b invasive diseases
6.1.2. Emergence of Capsulated Non–Serotype b (a, c, d, e, f)
7. Immune response to H. influenzae
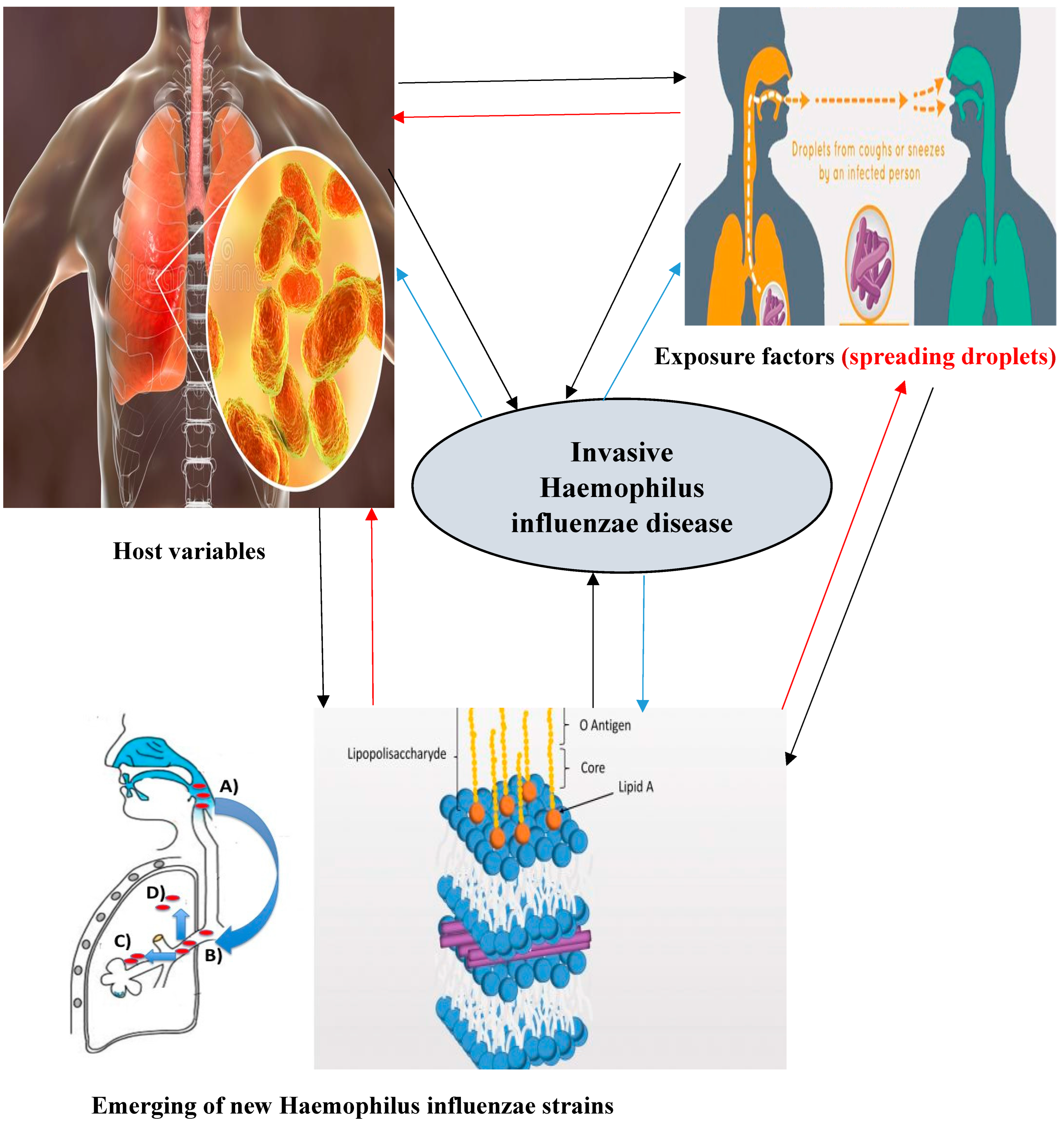
8. Prevention and control of invasive Haemophilus influenzae
9. Conclusion and future directions
- Globally, Haemophilus influenzae continues to be a common invasive Bacterial pathogen that dramatically raises morbidity and mortality. However, still little is known about the global presence of this pathogen and its emerging pathogenic strains.
- For some populations, ethnicity is a risk factor. The risk of invasive Hib infections is higher in American Indians, Inuits, black Africans, Melanesians, and African Americans. Whether this is due to truly biological differences or other factors is not clear and needs further studies on these populations.
- NTHi, Hia, Hif, and Hie cause an increasing number of invasive illnesses, especially in children and elderly people. However, the immune response to non-type b Hi infection is poorly studied.
- Even though there is still no vaccine available for strains other than type b (Hib).Immunization is necessary to guard against contracting invasive diseases brought on by nontypeable and other encapsulated strains of H. influenzae.
- H. influenzae can infect a person several times and a prior Hib infection could not protect you from a later infection. It is recommended to take the Hib vaccine even if one has already had Hib disease.
- The reasons for an increased susceptibility to NTHi, Hia, and Hif and Hie infection among some specific populations groups are still unknown and needs further research.
- Since Nontypeable Haemophilus influenzae's pathogenicity is significantly rising, international scientific organizations need to raise awareness of the emergence of invasive Hi pathogenicity and characterize the pathobiology of this microorganism.
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Conflicts of Interest
References
- Levinson, W.; Chin-Hong, P.; Joyce, E.; Nussbaum, J.; Schwartz, B. Host Defenses. Review of Medical Microbiology & Immunology: A Guide to Clinical Infectious Diseases (McGraw-Hill Education 2018.
- Ribeiro, G.S.; Reis, J.N.; Cordeiro, S.M.; Lima, J.B.; Gouveia, E.L.; Petersen, M.; Salgado, K.; Silva, H.R.; Zanella, R.C.; Almeida, S.C.G. Prevention of Haemophilus influenzae type b (Hib) meningitis and emergence of serotype replacement with type a strains after introduction of Hib immunization in Brazil. The Journal of infectious diseases 2003, 187, 109–116. [Google Scholar] [CrossRef] [PubMed]
- Resman, F.; Ristovski, M.; Ahl, J.; Forsgren, A.; Gilsdorf, J.R.; Jasir, A.; Kaijser, B.; Kronvall, G.; Riesbeck, K. Invasive disease caused by Haemophilus influenzae in Sweden 1997–2009; evidence of increasing incidence and clinical burden of non-type b strains. Clinical Microbiology and Infection 2011, 17, 1638–1645. [Google Scholar] [CrossRef] [PubMed]
- Ortiz-Romero, M.; Espejo-García, M.; Alfayate-Miguelez, S.; Ruiz-López, F.; Zapata-Hernandez, D.; Gonzalez-Pacanowska, A. Collaborators of Study Group of Infectious Diseases in the Child in Cartagena. Epidemiology of nasopharyngeal carriage by Haemophilus influenzae in healthy children: a study in the Mediterranean coast region. Pediatr Infect Dis J 2017, 36, 919–923. [Google Scholar] [CrossRef] [PubMed]
- O'Neill, J.M.; St. Geme III, J.W.; Cutter, D.; Adderson, E.E.; Anyanwu, J.; Jacobs, R.F.; Schutze, G.E. Invasive disease due to nontypeable Haemophilus influenzae among children in Arkansas. Journal of clinical microbiology 2003, 41, 3064–3069. [Google Scholar] [CrossRef]
- Chatziparasidis, G.; Kantar, A.; Grimwood, K. Pathogenesis of nontypeable Haemophilus influenzae infections in chronic suppurative lung disease. Pediatric Pulmonology 2023. [Google Scholar] [CrossRef]
- van Wessel, K.; Rodenburg, G.D.; Veenhoven, R.H.; Spanjaard, L.; van der Ende, A.; Sanders, E.A. Nontypeable Haemophilus influenzae invasive disease in The Netherlands: a retrospective surveillance study 2001–2008. Clinical Infectious Diseases 2011, 53, e1–e7. [Google Scholar] [CrossRef]
- Ulanova, M.; Tsang, R.S. Haemophilus influenzae serotype a as a cause of serious invasive infections. The Lancet infectious diseases 2014, 14, 70–82. [Google Scholar] [CrossRef]
- Tristram, S.; Jacobs, M.R.; Appelbaum, P.C. Antimicrobial resistance in Haemophilus influenzae. Clinical microbiology reviews 2007, 20, 368–389. [Google Scholar] [CrossRef]
- Slack, M.P. A review of the role of Haemophilus influenzae in community-acquired pneumonia. Pneumonia 2015, 6, 26–43. [Google Scholar] [CrossRef]
- Slack, M.; Cripps, A.; Grimwood, K.; Mackenzie, G.; Ulanova, M. Invasive Haemophilus influenzae infections after 3 decades of Hib protein conjugate vaccine use. Clinical microbiology reviews 2021, 34, e00028–e00021. [Google Scholar] [CrossRef]
- Ulanova, M. Global epidemiology of invasive Haemophilus influenzae type a disease: do we need a new vaccine? Journal of Vaccines 2013, 2013. [Google Scholar] [CrossRef]
- Peltola, H. Worldwide Haemophilus influenzae type b disease at the beginning of the 21st century: global analysis of the disease burden 25 years after the use of the polysaccharide vaccine and a decade after the advent of conjugates. Clinical microbiology reviews 2000, 13, 302–317. [Google Scholar] [CrossRef]
- Soeters, H.M.; Blain, A.; Pondo, T.; Doman, B.; Farley, M.M.; Harrison, L.H.; Lynfield, R.; Miller, L.; Petit, S.; Reingold, A. Current epidemiology and trends in invasive Haemophilus influenzae disease—United States, 2009–2015. Clinical Infectious Diseases 2018, 67, 881–889. [Google Scholar] [CrossRef]
- Tsang, R.; Bruce, M.; Lem, M.; Barreto, L.; Ulanova, M. A review of invasive Haemophilus influenzae disease in the Indigenous populations of North America. Epidemiology & Infection 2014, 142, 1344–1354. [Google Scholar]
- Giufrè, M.; Cardines, R.; Brigante, G.; Orecchioni, F.; Cerquetti, M. Emergence of invasive Haemophilus influenzae type a disease in Italy. Clinical Infectious Diseases 2017, 64, 1626–1628. [Google Scholar] [CrossRef]
- Organization, W.H. www. who. int/healthinfo/global_burden_disease/definition_regions/en.
- Duell, B.L.; Su, Y.C.; Riesbeck, K. Host–pathogen interactions of nontypeable Haemophilus influenzae: from commensal to pathogen. FEBS letters 2016, 590, 3840–3853. [Google Scholar] [CrossRef]
- Potts, C.C.; Topaz, N.; Rodriguez-Rivera, L.D.; Hu, F.; Chang, H.-Y.; Whaley, M.J.; Schmink, S.; Retchless, A.C.; Chen, A.; Ramos, E. Genomic characterization of Haemophilus influenzae: a focus on the capsule locus. BMC genomics 2019, 20, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Meiring, S.; Cohen, C.; de Gouveia, L.; du Plessis, M.; Kleynhans, J.; Quan, V.; Lengana, S.; Walaza, S.; von Gottberg, A. GERMS-SA annual surveillance report for laboratory-confirmed invasive meningococcal, Haemophilus influenzae and pneumococcal disease, South Africa, 2017. Public Health Surveillance 2019, 78. [Google Scholar]
- WHO, W. Definition of regional groupings. 2017.
- Organization, W.H. Health and well-being profile of the Eastern Mediterranean Region: an overview of the health situation in the Region and its countries in 2019. 2020.
- Pinto, M.; González-Díaz, A.; Machado, M.; Duarte, S.; Vieira, L.; Carriço, J.; Marti, S.; Bajanca-Lavado, M.; Gomes, J. Insights into the population structure and pan-genome of Haemophilus influenzae. Infection, Genetics and Evolution 2019, 67, 126–135. [Google Scholar] [CrossRef] [PubMed]
- Zulz, T.; Huang, G.; Rudolph, K.; DeByle, C.; Tsang, R.; Desai, S.; Massey, S.; Bruce, M.G. Epidemiology of invasive Haemophilus influenzae serotype a disease in the North American Arctic, 2006–2017. International Journal of Circumpolar Health 2022, 81, 2150382. [Google Scholar] [CrossRef]
- Trotter, C.L.; Lingani, C.; Fernandez, K.; Cooper, L.V.; Bita, A.; Tevi-Benissan, C.; Ronveaux, O.; Préziosi, M.-P.; Stuart, J.M. Impact of MenAfriVac in nine countries of the African meningitis belt, 2010–15: an analysis of surveillance data. The Lancet infectious diseases 2017, 17, 867–872. [Google Scholar] [CrossRef]
- Cheong, J.W.S.; Smith, H.; Heney, C.; Robson, J.; Schlebusch, S.; Fu, J.; Nourse, C. Trends in the epidemiology of invasive Haemophilus influenzae disease in Queensland, Australia from 2000 to 2013: what is the impact of an increase in invasive non-typable H. influenzae (NTHi)? Epidemiology & Infection 2015, 143, 2993–3000. [Google Scholar]
- Langereis, J.D.; de Jonge, M.I. Invasive disease caused by nontypeable Haemophilus influenzae. Emerging infectious diseases 2015, 21, 1711. [Google Scholar] [CrossRef]
- Belete, H.; Kidane, T.; Bisrat, F.; Molla, M.; Mounier-Jack, S.; Kitaw, Y. Routine immunization in Ethiopia. The Ethiopian Journal of Health Development 2015, 29. [Google Scholar]
- Diseases, N.I.f.C. GERMS South Africa: annual surveillance review 2018. 2018.
- Mackenzie, G.A.; Ikumapayi, U.N.; Scott, S.; Idoko, O.; Odutola, A.; Ndiaye, M.; Sahito, S.M.; Osuorah, C.D.; Manjang, A.; Jarju, S. Increased disease due to Haemophilus influenzae type b: population-based surveillance in eastern Gambia, 2008–2013. The Pediatric infectious disease journal 2015, 34, e107–e112. [Google Scholar] [CrossRef]
- McTaggart, L.R.; Cronin, K.; Seo, C.Y.; Wilson, S.; Patel, S.N.; Kus, J.V. Increased Incidence of Invasive Haemophilus influenzae Disease Driven by Non-Type B Isolates in Ontario, Canada, 2014 to 2018. Microbiology Spectrum 2021, 9, e00803–e00821. [Google Scholar] [CrossRef]
- McElligott, M.; Meyler, K.; Bennett, D.; Mulhall, R.; Drew, R.J.; Cunney, R. Epidemiology of Haemophilus influenzae in the Republic of Ireland, 2010–2018. European Journal of Clinical Microbiology & Infectious Diseases 2020, 39, 2335–2344. [Google Scholar]
- Oliver, S.E.; Rubis, A.B.; Soeters, H.M.; Reingold, A.; Barnes, M.; Petit, S.; Farley, M.M.; Harrison, L.H.; Como-Sabetti, K.; Khanlian, S.A. Epidemiology of Invasive Nontypeable Haemophilus influenzae Disease—United States, 2008–2019. Clinical Infectious Diseases 2023, ciad054. [Google Scholar] [CrossRef] [PubMed]
- Plotkin, S. A short history of vaccination. Vaccines. SA Plotkin and WA Orenstein. Philadelphia, Elsevier: 2004.
- Forsgren, A.; Riesbeck, K. Protein D of Haemophilus influenzae: a protective nontypeable H. influenzae antigen and a carrier for pneumococcal conjugate vaccines. Clinical Infectious Diseases 2008, 46, 726–731. [Google Scholar] [CrossRef] [PubMed]
- King, P.T.; Sharma, R. The lung immune response to nontypeable Haemophilus influenzae (lung immunity to NTHi). Journal of immunology research 2015, 2015. [Google Scholar] [CrossRef] [PubMed]
- Gilsdorf, J.R. What the pediatrician should know about non-typeable Haemophilus influenzae. Journal of Infection 2015, 71, S10–S14. [Google Scholar] [CrossRef]
- Su, Y.-C.; Resman, F.; Hörhold, F.; Riesbeck, K. Comparative genomic analysis reveals distinct genotypic features of the emerging pathogen Haemophilus influenzae type f. BMC genomics 2014, 15, 1–23. [Google Scholar] [CrossRef]
- Vikhe, P.P.; Purnell, T.; Brown, S.D.; Hood, D.W. Cellular immune response against nontypeable haemophilus influenzae infecting the preinflamed middle ear of the junbo mouse. Infection and Immunity 2019, 87, e00689–e00619. [Google Scholar] [CrossRef]
- Bakaletz, L.O.; Novotny, L.A. Nontypeable haemophilus influenzae (nthi). Trends in microbiology 2018, 26, 727–728. [Google Scholar] [CrossRef]
- Rate, A. Invasive Haemophilus influenzae disease.
- Kelly, D.F.; Moxon, E.R.; Pollard, A.J. Haemophilus influenzae type b conjugate vaccines. Immunology 2004, 113, 163–174. [Google Scholar] [CrossRef]
- Heliodoro, C.I.M.; Bettencourt, C.R.; Bajanca-Lavado, M.P.; Infection, P.G.f.t.S.o.H.i.I. Molecular epidemiology of invasive Haemophilus influenzae disease in Portugal: an update of the post-vaccine period, 2011–2018. European Journal of Clinical Microbiology & Infectious Diseases 2020, 39, 1471–1480. [Google Scholar]
- Gaultier, G. Humoral immunity in patients with chronic kidney disease and their response to pneumococcal immunization. 2020.
- Tønnessen, R.; García, I.; Debech, N.; Lindstrøm, J.C.; Wester, A.L.; Skaare, D. Molecular epidemiology and antibiotic resistance profiles of invasive Haemophilus influenzae from Norway 2017–2021. Frontiers in Microbiology 2022, 13. [Google Scholar] [CrossRef]
- Choi, J.; Cox, A.D.; Li, J.; McCready, W.; Ulanova, M. Activation of innate immune responses by Haemophilus influenzae lipooligosaccharide. Clinical and Vaccine Immunology 2014, 21, 769–776. [Google Scholar] [CrossRef] [PubMed]
- Jin, Z.; Romero-Steiner, S.; Carlone, G.M.; Robbins, J.B.; Schneerson, R. Haemophilus influenzae type a infection and its prevention. Infection and immunity 2007, 75, 2650–2654. [Google Scholar] [CrossRef] [PubMed]
- Dousha, L.; Sharma, R.; Lim, S.; Ngui, J.; Buckle, A.M.; King, P.T. Assessing Respiratory Immune Responses to Haemophilus Influenzae. JoVE (Journal of Visualized Experiments) 2021, e62572. [Google Scholar]
- Ladhani, S.; Slack, M.P.; Heath, P.T.; Von Gottberg, A.; Chandra, M.; Ramsay, M.E.; participants, E.U.I.B.I.S. Invasive Haemophilus influenzae disease, Europe, 1996–2006. Emerging infectious diseases 2010, 16, 455. [Google Scholar] [CrossRef] [PubMed]
- High, N.; Fan, F.; Schwartzman, J. Chapter 97—haemophilus influenzae. Molecular medical microbiology, vol. 3. Amsterdam: Academic Press: 2015.
- Hawdon, N.; Nix, E.B.; Tsang, R.S.; Ferroni, G.; McCready, W.G.; Ulanova, M. Immune response to Haemophilus influenzae type b vaccination in patients with chronic renal failure. Clinical and Vaccine Immunology 2012, 19, 967–969. [Google Scholar] [CrossRef] [PubMed]
- Heath, P.; Booy, R.; Griffiths, H.; Clutterbuck, E.; Azzopardi, H.; Slack, M.; Fogarty, J.; Moloney, A.; Moxon, E. Clinical and immunological risk factors associated with Haemophilus influenzae type b conjugate vaccine failure in childhood. Clinical infectious diseases 2000, 31, 973–980. [Google Scholar] [CrossRef] [PubMed]
- Soeters, H.M.; Oliver, S.E.; Plumb, I.D.; Blain, A.E.; Zulz, T.; Simons, B.C.; Barnes, M.; Farley, M.M.; Harrison, L.H.; Lynfield, R. Epidemiology of invasive Haemophilus influenzae serotype a disease—United States, 2008–2017. Clinical Infectious Diseases 2021, 73, e371–e379. [Google Scholar] [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).