Submitted:
25 May 2023
Posted:
26 May 2023
You are already at the latest version
Abstract
Keywords:
1. Introduction
Objectives
2.1. Patients
- Early dementia stage.
- Insufficient data in the clinical file.
2.2. Safety
2.3. Clinical Outcome
2.4. Anthropometric Evaluation
2.4.1. Body mass index (BMI): BMI was obtained in most patients using the equation
2.4.2. Mid Upper Arm Circumference (MUAC) was evaluated using an inextensible measuring tape with a 1 mm resolution. MUAC results from evaluating several tissues representing fat and lean mass
2.4.3. Tricipital skinfold (TSF) was measured using a Lange Skinfold caliper with a 1 mm resolution. TSF evaluates the subcutaneous adipose tissue and estimates adipose reserves
2.4.4. The Mid-Arm Muscle Circumference (MAMC) was calculated according to the equation: MAMC = MUAC (cm) - 0.314 × TSF (mm). The MAMC allows us to estimate lean and muscle mass
2.5. Laboratory Evaluation
2.6. Ethical Considerations
2.7. Statistics
3. Results
3.1. Subjects
3.2. Anthropometry
3.2.1. Body mass index (BMI) at T0
3.2.2. Mid Upper Arm Circumference (MUAC) at T0
3.2.3. Tricipital Skinfold (TSF) at T0
3.2.4. Mid-Arm Muscle Circumference (MAMC) at T0
3.3. Laboratory Assessment
3.3.1. Serum Albumin at T0
3.3.2. Serum Transferrin at T0
3.3.3. Serum Total Cholesterol at T0
3.3.4. Hemoglobin at T0
| Total (n = 100) | Male (n=39) | Female (n=61) | Total Mean | |
|---|---|---|---|---|
| Anthropometry Results | ||||
| BMI | 39 Low | 13 Low | 26 Low | |
| 33 Normal | 16 Normal | 17 Normal | ||
| 28 High | 10 High | 18 High | ||
| MUAC | 77 Low | 31 Low | 46 Low | |
| 23 Normal | 8 Normal | 15 Normal | ||
| TSF | 84 Low | 29 Low | 55 Low | |
| 16 Normal | 10 Normal | 6 Normal | ||
| MAMC | 52 Low | 31 Low | 21 Low | |
| 48 Normal | 8 Normal | 40 Normal | ||
| Laboratory serum data | ||||
| Albumin | 64 Low | 31 Low | 33 Low | 3.25 g/dL |
| 36 Normal | 8 Normal | 28 Normal | ||
| Transferrin | 62 Low | 35 Low | 45 Low | 170.6 mg/dL |
| 34 Normal | 4 Normal | 16 Normal | ||
| Total Cholesterol | 51 Low | 28 Low | 23 Low | 164.4 mg/dL |
| 49 Normal | 11 Normal | 38 Normal | ||
| Hemoglobin* (n=65) | 43 low | 23 Low | 20 Low | 11.3 g/dl |
| 22 Normal | 2 Normal | 20 Normal | ||
3.4. Safety
3.5. Evolution Data According to Follow-Ups (T0 to T2)
3.6. Clinical Outcome
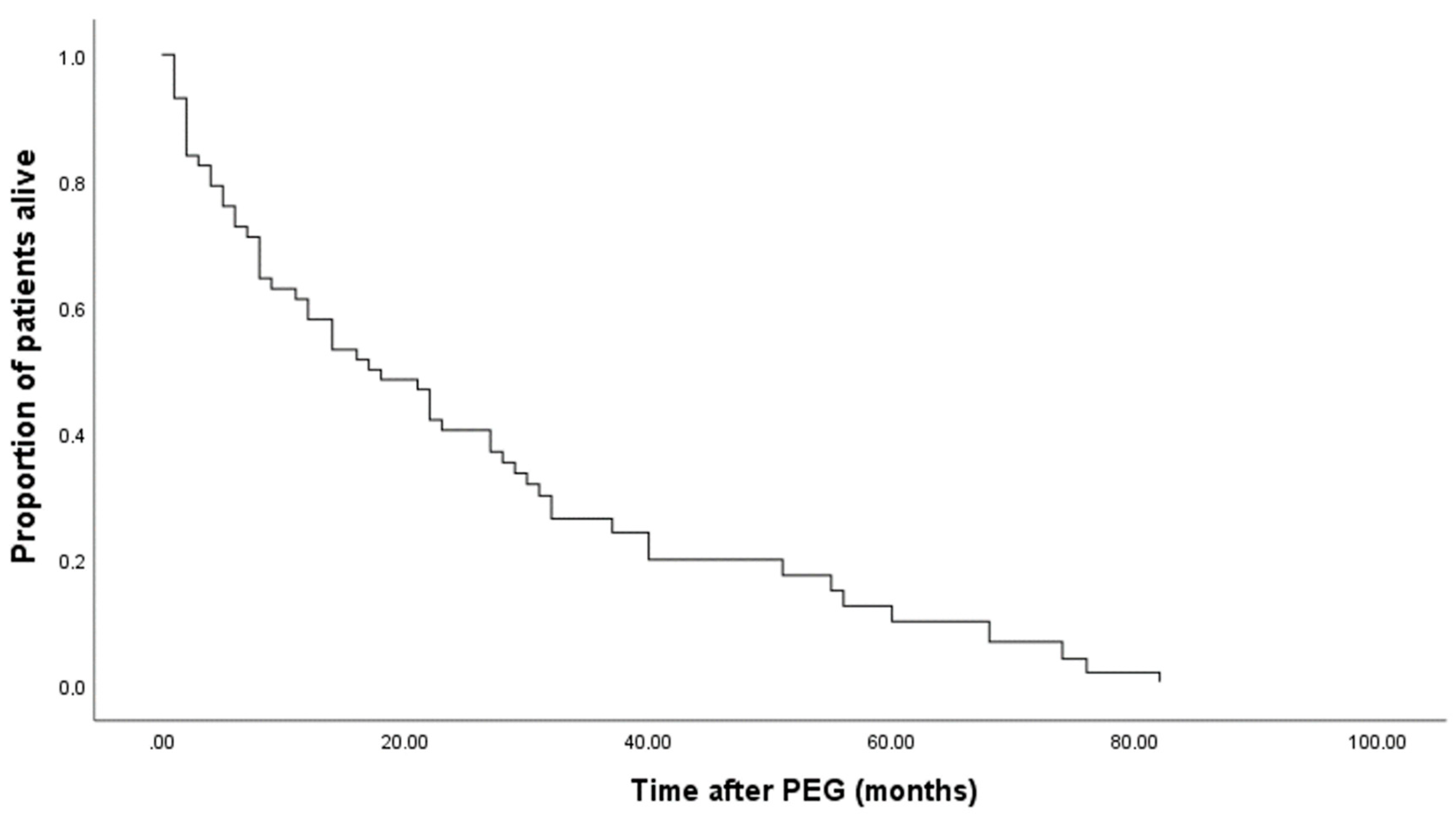
3.7. Kaplan-Meier Survival Analysis
3.8. Survival According to Data Follow-Ups (T0 to T2)
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Arvanitakis, Z.; Shah, R. C.; Bennett, D. A. Diagnosis and Management of Dementia: Review. JAMA 2019, 322 (16), 1589–1599. [CrossRef]
- Dementia: a public health priority. Who.int. https://www.who.int/publications/i/item/dementia-a-public-health-priority. (accessed on 6 January 2020).
- Prince, M.; Wimo, A.; Guerchet, M.; Ali, G.-C.; Wu, Y.-T.; Prina, M.; Kit, Y.; Xia, Z. Alzint.org. https://www.alzint.org/u/WorldAlzheimerReport2015.pdf (accessed 2020-01-06).
- Rikkert, M. G. M. O.; Tona, K. D.; Janssen, L.; Burns, A.; Lobo, A.; Robert, P.; Sartorius, N.; Stoppe, G.; Waldemar, G. Validity, Reliability, and Feasibility of Clinical Staging Scales in Dementia: A Systematic Review: A Systematic Review. Am. J. Alzheimers. Dis. Other Demen. 2011, 26 (5), 357–365. [CrossRef]
- Burke, W. J.; Houston, M. J.; Boust, S. J.; Roccaforte, W. H. Use of the Geriatric Depression Scale in Dementia of the Alzheimer Type. J. Am. Geriatr. Soc. 1989, 37 (9), 856–860. [CrossRef]
- Eisdorfer, C.; Cohen, D.; Tang, M. X. An Empirical Evaluation of the Global Deterioration Scale for Staging Alzheimer's Disease: Correction. Am J Psychiatry 1992, 149 (6). [CrossRef]
- Sclan, S. G.; Reisberg, B. Functional Assessment Staging (FAST) in Alzheimer's Disease: Reliability, Validity, and Ordinality. Int. Psychogeriatr. 1992, 4 Suppl 1, 55–69. [CrossRef]
- Volkert, D.; Chourdakis, M.; Faxen-Irving, G.; Frühwald, T.; Landi, F.; Suominen, M. H.; Vandewoude, M.; Wirth, R.; Schneider, S. M. ESPEN Guidelines on Nutrition in Dementia. Clin. Nutr. 2015, 34 (6), 1052–1073. [CrossRef]
- Sampson, E. L.; Candy, B.; Jones, L. Enteral Tube Feeding for Older People with Advanced Dementia. Cochrane Database Syst. Rev. 2009, No. 2, CD007209. [CrossRef]
- Goldberg, L. S.; Altman, K. W. The Role of Gastrostomy Tube Placement in Advanced Dementia with Dysphagia: A Critical Review. Clin. Interv. Aging 2014, 9, 1733–1739. [CrossRef]
- Salomon, R.; Garbi Novaes, C. Outcomes of Enteral Nutrition for Patients with Advanced Dementia: A Systematic Review. J Nutr Health Aging 2015, 19 (11), 169–177. [CrossRef]
- Brooke, J.; Ojo, O. Enteral Nutrition in Dementia: A Systematic Review. Nutrients 2015, 7 (4), 2456–2468. [CrossRef]
- Douglas, J. W.; Lawrence, J. C.; Turner, L. W. Social Ecological Perspectives of Tube-Feeding Older Adults with Advanced Dementia: A Systematic Literature Review. J. Nutr. Gerontol. Geriatr. 2017, 36 (1), 1–17. [CrossRef]
- American Geriatrics Society Ethics Committee and Clinical Practice and Models of Care Committee. American Geriatrics Society Feeding Tubes in Advanced Dementia Position Statement. J Am Geriatr Soc 2014, 62 (14), 1590–1593. [CrossRef]
- Orlandoni, P.; Jukic Peladic, N.; Cherubini, A. Enteral Nutrition in Advanced Dementia: An Unresolved Dilemma in Clinical Practice. Eur. Geriatr. Med. 2020, 11 (2), 191–194. [CrossRef]
- Goldberg, L.; Altman, K. The Role of Gastrostomy Tube Placement in Advanced Dementia with Dysphagia: A Critical Review. Clin. Interv. Aging 2014, 1733. [CrossRef]
- Sanders, D. S.; Anderson, A. J.; Bardhan, K. D. Percutaneous Endoscopic Gastrostomy: An Effective Strategy for Gastrostomy Feeding in Patients with Dementia. Clin. Med. 2004, 4 (3), 235–241. [CrossRef]
- Sanders, D. S.; Leeds, J. S.; Drew, K. The Role of Percutaneous Endoscopic Gastrostomy in Patients with Dementia. Br. J. Nurs. 2008, 17 (9), 588–594. [CrossRef]
- Nunes, G.; Santos, C. A.; Santos, C.; Fonseca, J. Percutaneous Endoscopic Gastrostomy for Nutritional Support in Dementia Patients. Aging Clin Exp Res 2016, 28 (5), 983–989. [CrossRef]
- Orlandoni, P.; Peladic, N. J.; Di Rosa, M.; Venturini, C.; Fagnani, D.; Sparvoli, D.; Giorgini, N.; Basile, R.; Cola, C. The Outcomes of Long Term Home Enteral Nutrition (HEN) in Older Patients with Severe Dementia. Clin. Nutr. 2019, 38 (4), 1871–1876. [CrossRef]
- Powell-Tuck J, Hennessy EM. A comparison of mid upper arm circumference, body mass index and weight loss as indices of undernutrition in acutely hospitalized patients. Clin. Nutr. 2003, 22(3):307-312. [CrossRef]
- Pereira, M.; Santos, C.; Fonseca, J. Body Mass Index Estimation on Gastrostomy Patients Using the Mid Upper Arm Circumference. The Journal of Aging Research & Clinical Practice 2010, 1, 252–255.
- Barosa, R.; Roque Ramos, L.; Santos, C. A.; Pereira, M.; Fonseca, J. Mid Upper Arm Circumference and Powell-Tuck and Hennessy's Equation Correlate with Body Mass Index and Can Be Used Sequentially in Gastrostomy Fed Patients. Clin. Nutr. 2018, 37 (5), 1584–1588. [CrossRef]
- World Health Organization—Europe. Nutrition—Body Mass Index—BMI. Available online: https://www.euro.who.int/en/health topics/disease-prevention/nutrition/a-healthylifestyle/body-mass-index-bmi~ (accessed on 6 January 2020 ).
- Frisancho, A. R. New Standards of Weight and Body Composition by Frame Size and Height for Assessment of Nutritional Status of Adults and the Elderly. Am. J. Clin. Nutr. 1984, 40 (4), 808–819. [CrossRef]
- Fonseca, J.; Santos, C. A. Clinical anatomy: anthropometry for nutritional assessment of 367 adults who underwent endoscopic gastrostomy. Acta Med. Port. 2013, 26 (3), 212–218.
- Sultan, S.; Nasir, K.; Qureshi, R.; Dhrolia, M.; Ahmad, A. Assessment of the Nutritional Status of the Hemodialysis Patients by Anthropometric Measurements. Cureus 2021, 13 (10), e18605. [CrossRef]
- Kuzuya, M.; Izawa, S.; Enoki, H.; Okada, K.; Iguchi, A. Is Serum Albumin a Good Marker for Malnutrition in the Physically Impaired Elderly? Clin. Nutr. 2007, 26 (1), 84–90. [CrossRef]
- Fonseca, J.; Adriana Santos, C.; Brito, J. Predicting Survival of Endoscopic Gastrostomy Candidates Using the Underlying Disease, Serum Cholesterol, Albumin and Transferrin Levels. Nutr. Hosp. 2013, 28 (4), 1280–1285. [CrossRef]
- Vyroubal, P.; Chiarla, C.; Giovannini, I.; Hyspler, R.; Ticha, A.; Hrnciarikova, D.; Zadak, Z. Hypocholesterolemia in Clinically Serious Conditions--Review. Biomed. Pap. Med. Fac. Univ. Palacky Olomouc Czech. Repub. 2008, 152 (2), 181–189. [CrossRef]
- Callahan, C. M.; Haag, K. M.; Weinberger, M.; Tierney, W. M.; Buchanan, N. N.; Stump, T. E.; Nisi, R. Outcomes of Percutaneous Endoscopic Gastrostomy among Older Adults in a Community Setting. J. Am. Geriatr. Soc. 2000, 48 (9), 1048–1054. [CrossRef]
- Volkert, D.; Berner, Y. N.; Berry, E.; Cederholm, T.; Coti Bertrand, P.; Milne, A.; Palmblad, J.; Schneider, S.; Sobotka, L.; Stanga, Z.; DGEM (German Society for Nutritional Medicine); Lenzen-Grossimlinghaus, R.; Krys, U.; Pirlich, M.; Herbst, B.; Schütz, T.; Schröer, W.; Weinrebe, W.; Ockenga, J.; Lochs, H.; ESPEN (European Society for Parenteral and Enteral Nutrition). ESPEN Guidelines on Enteral Nutrition: Geriatrics. Clin. Nutr. 2006, 25 (2), 330–360. [CrossRef]
- American Psychiatric Association (2000) Delirium, dementia, and amnestic and olther cognitive disorders. In: Diagnostic and statistical manual of mental disorders text revision, 4th edn. Washington, pp 135–180.

| LOW | NORMAL | HIGH | |
|---|---|---|---|
| < 65 YEARS | <18.5 kg/m2 | ≥18.5 - <25 kg/m2 | ≥25 kg/m2 |
| ≥ 65 YEARS | < 22 kg/m2 | ≥22 - <27 kg/m2 | ≥27 kg/m2 |
|
Comparisons Pairwise Recovery [Conf. Int.] |
Sig. | |||
|---|---|---|---|---|
| BMI | 1/2 | .328 [-1.468-.812] | .566 | |
| 2/3 | .073 [-.496-.642] | .798 | ||
| 1/3 | .255 [-1.494-.984] | .681 | ||
| MUAC | 1/2 | 2.172 [-5.473-9.817] | .571 | |
| 2/3 | .023 [-.498-.545] | .929 | ||
| 1/3 | 2.195 [-5.544-9.934] | .572 | ||
| MAMC | 1/2 | .666 [-8.317-6.984] | .862 | |
| 2/3 | .023 [-.498-.545] | .929 | ||
| 1/3 | .643 [-8.384-7.098] | .868 | ||
| TSF | 1/2 | .468 [-.226-1.162] | .182 | |
| 2/3 | .026 [-.751-.700] | .944 | ||
| 1/3 | .442 [-.438-1.323] | .318 | ||
| Albumin | 1/2 | .191 [.059-.324] | .006 | |
| 2/3 | .124 [-.001-.250] | .052 | ||
| 1/3 | .316 [.141-.490] | .001 | ||
| Transferrin | 1/2 | 14.356 [0.413-29.126] | .056 | |
| 2/3 | 18.375 [5.277-31.473] | .007 | ||
| 1/3 | 32.731[13.797-51.665] | .001 | ||
| Total Cholesterol | 1/2 | 4.707 [4.904-14.319] | .328 | |
| 2/3 | 2.976 [15.203-9.252] | .626 | ||
| 1/3 | 1.732 [14.075-17.538] | .826 | ||
| Hemoglobin | 1/2 | 4.454 [-8.045-16.953] | .467 | |
| 2/3 | 9.177 [-20.962-2.609] | .120 | ||
| 1/3 | 4.723 [-12.191-2.745] | .203 |
| Survival (month) | Meana | Mean CI 95% | Median |
|---|---|---|---|
| Female | 34.2 | 26.1-42.3 | 25.0 |
| Male | 17.2 | 10.1-24.3 | 7.0 |
| Total | 27.9 | 21.8-34 | 17.0 |
| Survival (month) | Meana | Mean CI 95% | Median |
|---|---|---|---|
| BMI at baseline (T0) | |||
| Low | 26.588 | 15.93-37.24 | 18.000 |
| Normal | 31.258 | 18.17-44.34 | 9.000 |
| High | 26.462 | 19.07-33.85 | 22.000 |
| Inferior | Superior | |||
|---|---|---|---|---|
| Sex (female) | .48 | .27 | .85 | .012 |
| hemoglobina_0 | .98 | .97 | .91 | .005 |
| BMI_02 | .89 | .81 | .98 | .023 |
| MUAC_02 | .90 | .79 | 1.0 | .172 |
| MAMC_02 | .88 | .76 | 1.0 | .094 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




