Submitted:
03 February 2023
Posted:
06 February 2023
You are already at the latest version
Abstract
Keywords:
1. Introduction
1.1. The present study
2. Materials and Methods
2.1. Participants
2.2. Questionnaires
2.3. Preprocessing
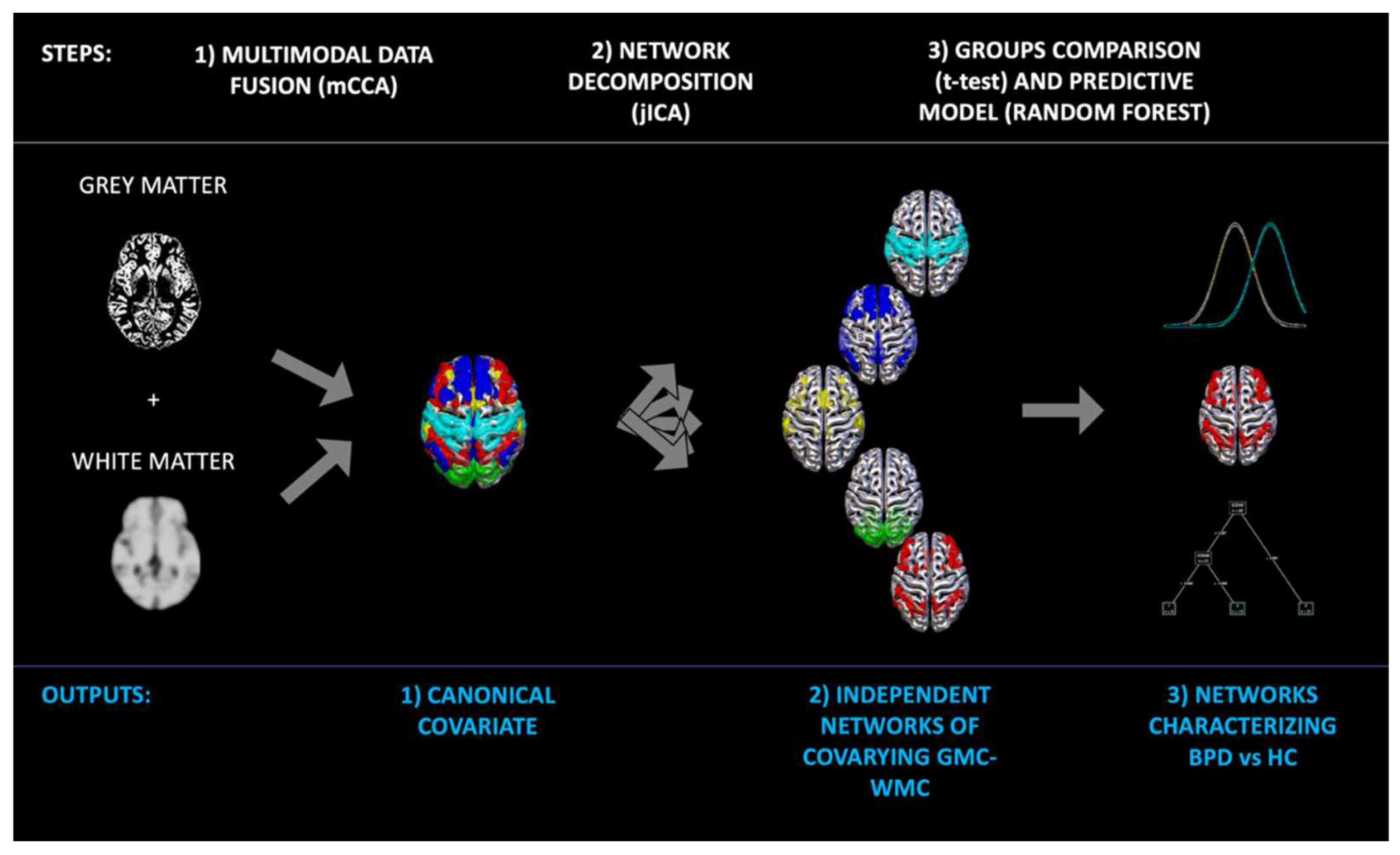
2.4. Data fusion unsupervised machine learning to decompose the brain into independent covarying GM-WM networks
2.5. Predictive model
3. Results
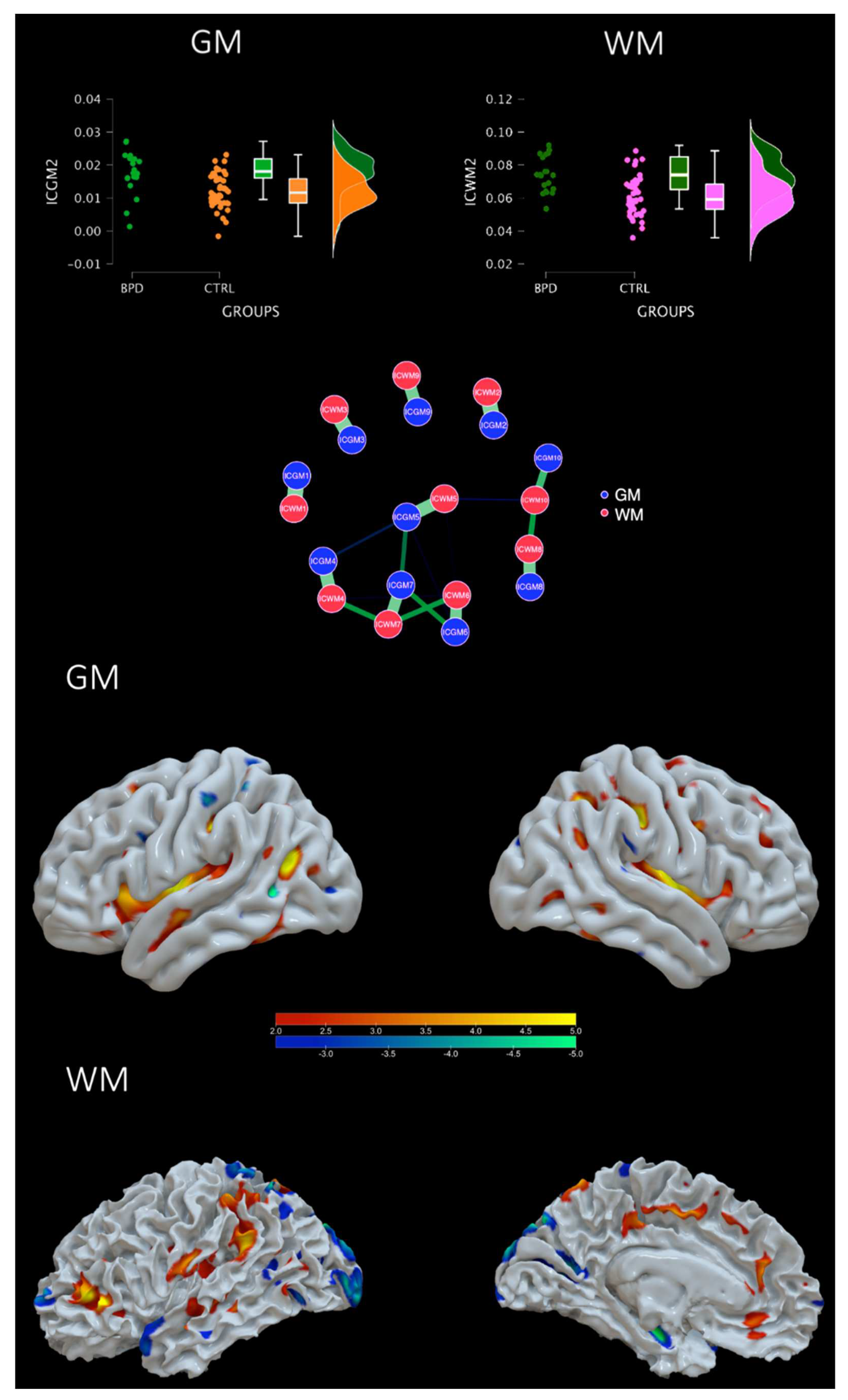
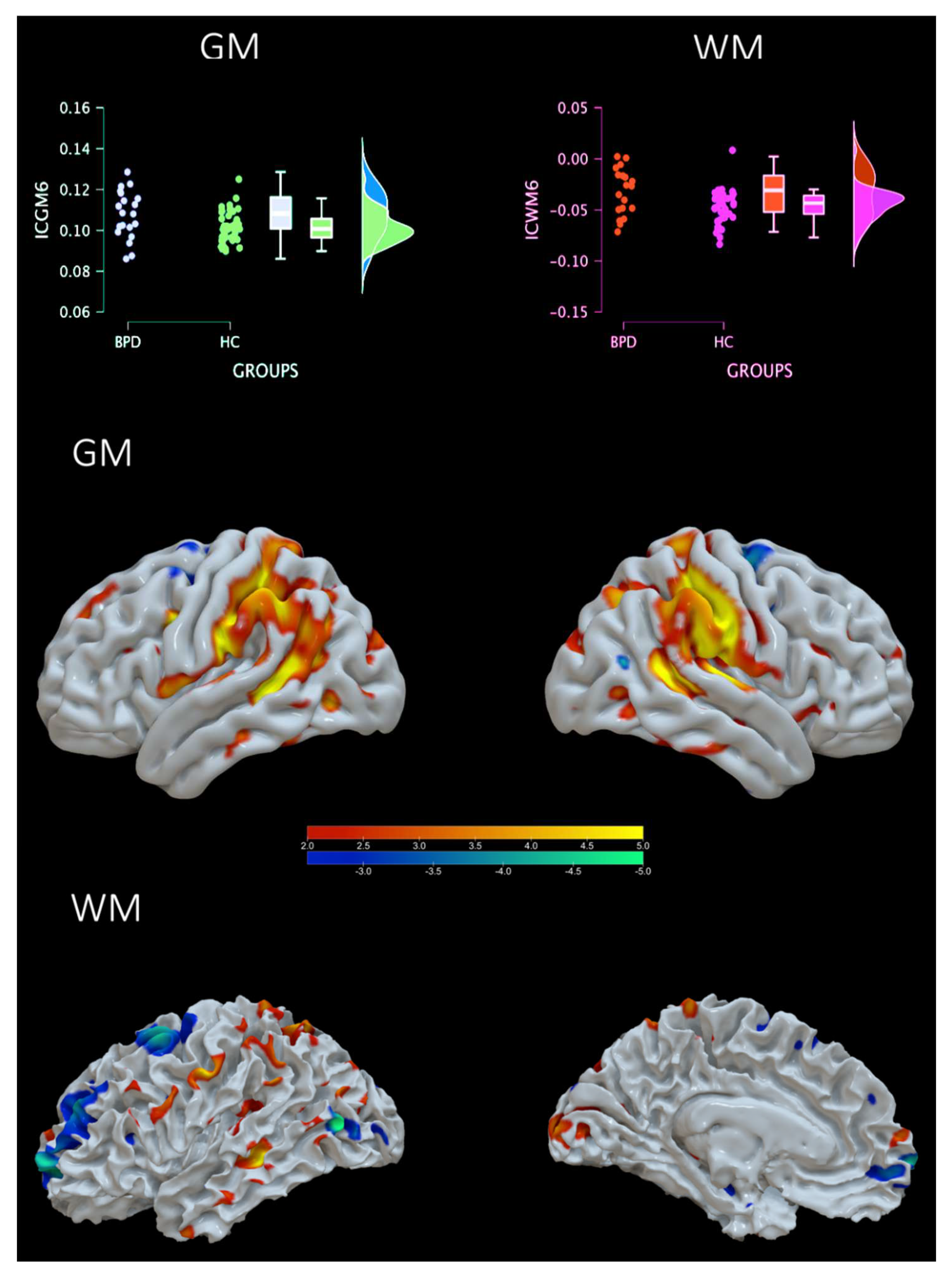
3.1. Groups comparison
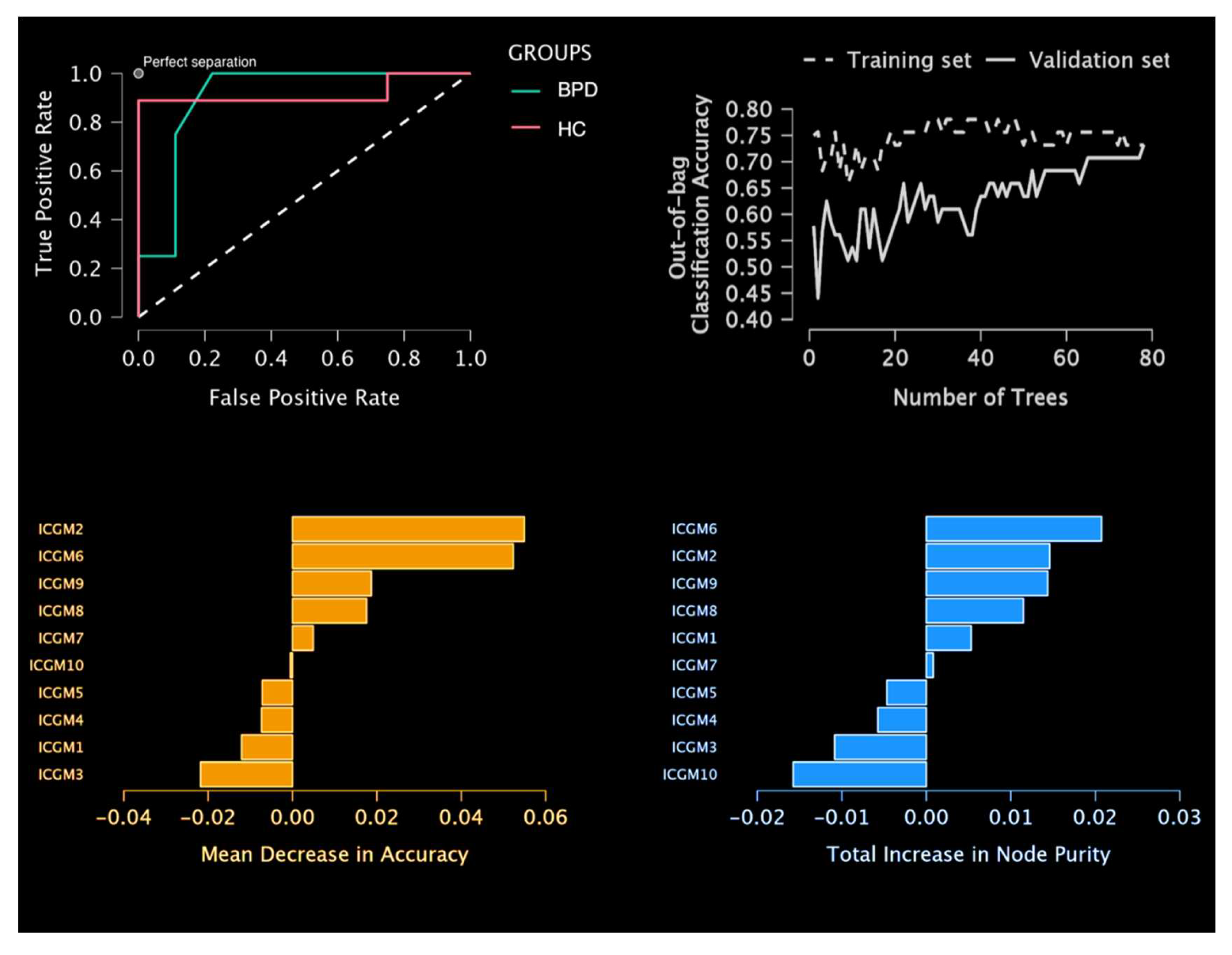
3.2. Predictive model results
3.3. Mediation Analysis
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Koenigsberg, H.W.; Harvey, P.D.; Mitropoulou, V.; Schmeidler, J.; New, A.S.; Goodman, M.; Silverman, J.M.; Serby, M.; Schopick, F.; Siever, L.J. Characterizing affective instability in borderline personality disorder. The American journal of psychiatry 2002, 159, 784–788. [Google Scholar] [CrossRef] [PubMed]
- Zanarini, MC. Psychotherapy of borderline personality disorder. Acta Psychiatr Scand. 2009, 120, 373–377. [Google Scholar] [CrossRef] [PubMed]
- Lenzenweger, M.F.; Lane, M.C.; Loranger, A.W.; Kessler, R.C. DSM-IV personality disorders in the National Comorbidity Survey Replication. Biological psychiatry 2007, 62, 553–564. [Google Scholar] [CrossRef] [PubMed]
- Trull, T.J.; Jahng, S.; Tomko, R.L.; Wood, P.K.; Sher, K.J. Revised NESARC personality disorder diagnoses: gender, prevalence, and comorbidity with substance dependence disorders. J. Personal. Disord. 2010, 24, 412–426. [Google Scholar] [CrossRef]
- Tomko, R.L.; Trull, T.J.; Wood, P.K.; Sher, K.J. Characteristics of borderline personality disorder in a community sample: comorbidity, treatment utilization, and general functioning. Journal of personality disorders 2014, 28, 734. [Google Scholar] [CrossRef]
- De Panfilis, C.; Schito, G.; Generali, I.; Gozzi, L.; Ossola, P.; Marchesi, C.; Grecucci, A. Emotions at the border: Increased punishment behavior during fair interpersonal exchanges in Borderline Personality Disorder. Journal of Abnormal Psychology 2019, 128, 162–172. [Google Scholar] [CrossRef] [PubMed]
- Hua, Y.; Meng, Y.J.; Li, X.J.; Zhang, C.; Liang, S.; Li, M.L.; ... Li, T. Common and distinct patterns of grey matter alterations in borderline personality disorder and bipolar disorder: voxel-based meta-analysis. The British Journal of Psychiatry 2019, 215, 395–403. [Google Scholar] [CrossRef] [PubMed]
- Wolf, R.C.; Thomann, P.A.; Sambataro, F.; Vasic, N.; Schmid, M.; Wolf, N.D. Orbitofrontal cortex and impulsivity in borderline personality disorder: an MRI study of baseline brain perfusion. European archives of psychiatry and clinical neuroscience 2012, 262, 677–685. [Google Scholar] [CrossRef]
- Ducasse, D.; Courtet, P.; Olie, E. Physical and social pains in borderline disorder and neuroanatomical correlates: a systematic review. Current Psychiatry Reports 2014, 16, 1–12. [Google Scholar] [CrossRef]
- Wrege, J.S.; Ruocco, A.C.; Euler, S.; Preller, K.H.; Busmann, M.; Meya, L. ; .. & Walter, M. Negative affect moderates the effect of social rejection on frontal and anterior cingulate cortex activation in borderline personality disorder. Cognitive, Affective, & Behavioral Neuroscience 2019, 19, 1273–1285. [Google Scholar] [CrossRef]
- Lou, J.; Sun, Y.; Cui, Z.; Gong, L. Common and distinct patterns of gray matter alterations in borderline personality disorder and posttraumatic stress disorder: a dual meta-analysis. Neuroscience Letters 2021, 741, 135–376. [Google Scholar] [CrossRef] [PubMed]
- Pan, N.; Wang, S.; Qin, K.; Li, L.; Chen, Y.; Zhang, X.; ... Gong, Q. Common and Distinct Neural Patterns of Attention-Deficit/Hyperactivity Disorder and Borderline Personality Disorder: A Multimodal Functional and Structural Meta-analysis. Biological Psychiatry: Cognitive Neuroscience and Neuroimaging 2022. [Google Scholar] [CrossRef] [PubMed]
- Irle, E.; Lange, C.; Sachsse, U. Reduced size and abnormal asymmetry of parietal cortex in women with borderline personality disorder. Biological psychiatry 2005, 57, 173–182. [Google Scholar] [CrossRef] [PubMed]
- Lyoo, I.K.; Han, M.H.; Cho, D.Y. A brain MRI study in subjects with borderline personality disorder. Journal of affective disorders 1998, 50, 235–243. [Google Scholar] [CrossRef]
- Hazlett, E.A.; New, A.S.; Newmark, R.; Haznedar, M.M.; Lo, J.N.; Speiser, L.J. ... & Buchsbaum, M.S. Reduced anterior and posterior cingulate gray matter in borderline personality disorder. Biological psychiatry 2005, 58, 614–623. [Google Scholar] [CrossRef] [PubMed]
- Ashburner, J.; Friston, K.J. Voxel-based morphometry—the methods. Neuroimage 2000, 11, 805–812. [Google Scholar] [CrossRef] [PubMed]
- Soloff, P.H.; Pruitt, P.; Sharma, M.; Radwan, J.; White, R.; Diwadkar, V.A. Structural brain abnormalities and suicidal behavior in borderline personality disorder. Journal of psychiatric research 2012, 46, 516–525. [Google Scholar] [CrossRef] [PubMed]
- Niedtfeld, I., I.; Schulze, L.; Krause-Utz, A.; Demirakca, T.; Bohus, M.; Schmahl, C. Voxel-based morphometry in women with borderline personality disorder with and without comorbid posttraumatic stress disorder. PloS one 2013, 8, e65824. [Google Scholar] [CrossRef]
- Schulze, L.; Schmahl, C.; Niedtfeld, I. Neural correlates of disturbed emotion processing in borderline personality disorder: a multimodal meta-analysis. Biological psychiatry 2016, 79, 97–106. [Google Scholar] [CrossRef]
- Aguilar-Ortiz S, Salgado-Pineda P, Marco-Pallarés J, Pascual JC, Vega D, Soler J, et al. Abnormalities in gray matter volume in patients with borderline personality disorder and their relation to lifetime depression: A VBM study. PLoS ONE 2018, 13, e0191946. [CrossRef]
- Dadomo, H.; Grecucci, A.; Giardini, I.; Ugolini, E.; Carmelita, A.; Panzeri, M. Schema Therapy for Emotional Dysregulation: Theoretical Implication and Clinical Applications. Frontiers in psychology 2016, 7, 1987. [Google Scholar] [CrossRef]
- Frederickson, J.J.; Messina, I.; Grecucci, A. Dysregulated Anxiety and Dysregulating Defenses: Toward an Emotion Regulation Informed Dynamic Psychotherapy. Frontiers in psychology 2018, 9, 2054. [Google Scholar] [CrossRef]
- Ruocco, A.C.; Amirthavasagam, S.; Zakzanis, K.K. Amygdala and hippocampal volume reductions as candidate endophenotypes for borderline personality disorder: a meta-analysis of magnetic resonance imaging studies. Psychiatry Research: Neuroimaging 2012, 201, 245–252. [Google Scholar] [CrossRef] [PubMed]
- Sorella, S.; Lapomarda, G.; Messina, I.; Frederickson, J.J.; Siugzdaite, R.; Job, R.; Grecucci, A. Testing the expanded continuum hypothesis of schizophrenia and bipolar disorder. Neural and psychological evidence for shared and distinct mechanisms. NeuroImage. Clinical 2019, 23, 101854. [Google Scholar] [CrossRef] [PubMed]
- Lapomarda, G.; Grecucci, A.; Messina, I.; Pappaianni, E.; Dadomo, H. Common and different gray and white matter alterations in Bipolar and Borderline Personality Disorder. Brain Research 2021. [Google Scholar] [CrossRef] [PubMed]
- Pappaianni, E.; De Pisapia, N.; Siugzdaite, R.; Crescentini, C.; Calcagnì, A.; Job, R.; Grecucci, A. Less is more: Psychological and morphometric differences between low vs high reappraisers. Cogn. Affect. Behav. Neurosci 2019, 20, 128–140. [Google Scholar] [CrossRef] [PubMed]
- Grecucci, A.; Lapomarda, G.; Messina, I.; Monachesi, B.; Sorella, S.; Siugzdaite, R. Structural features related to affective instability correctly classify patients with Borderline Personality Disorder. A Supervised Machine Learning approach. Frontiers in Psychiatry 2022, 13. [Google Scholar] [CrossRef]
- Sui, J.; Pearlson, G.; Caprihan, A.; Adali, T.; Kiehl, K.A.; Liu, J. ... & Calhoun, V.D. Discriminating schizophrenia and bipolar disorder by fusing fMRI and DTI in a multimodal CCA+ joint ICA model. Neuroimage 2011, 57, 839–855. [Google Scholar] [CrossRef] [PubMed]
- Mechelli, A.; Viera, S. (Eds.) Machine learning: methods and applications to brain disorders; Academic Press.
- Calhoun, V.D.; Adali, T.; Giuliani, N.R.; Pekar, J.J.; Kiehl, K.A.; Pearlson, G.D. Method for multimodal analysis of independent source differences in schizophrenia: combining gray matter structural and auditory oddball functional data. Hum Brain Mapp 2006, 27, 47–62. [Google Scholar] [CrossRef] [PubMed]
- Correa, N.M.; Li, Y.O.; Adali, T.; Calhoun, V.D. Canonical Correlation Analysis for Feature-Based Fusion of Biomedical Imaging Modalities and Its Application to Detection of Associative Networks in Schizophrenia. IEEE J Sel Top Sign Proces 2008, 2, 998–1007. [Google Scholar] [CrossRef]
- Plis, S.M.; Weisend, M.P.; Damaraju, E.; Eichele, T.; Mayer, A.; Clark, V.P. ... & Calhoun, V.D. Effective connectivity analysis of fMRI and MEG data collected under identical paradigms. Computers in biology and medicine 2011, 41, 1156–1165. [Google Scholar] [CrossRef]
- Sui, J.; He, H.; Yu, Q.; Chen, J.; Rogers, J.; Pearlson, G.D. ... & Calhoun, V.D. Combination of resting state fMRI, DTI, and sMRI data to discriminate schizophrenia by N-way MCCA+ jICA. Frontiers in human neuroscience 2013, 7, 235. [Google Scholar] [CrossRef] [PubMed]
- Grecucci, A.; Sorella, S.; Consolini, J. Decoding Individual Differences in Expressing and Suppressing Anger from Structural Brain Networks: a Supervised Machine Learning Approach. Behavioral Brain Research 2022, 439, 114245. [Google Scholar] [CrossRef] [PubMed]
- Ho, T.K. The Random Subspace Method for Constructing Decision Forests. IEEE Transactions on Pattern Analysis and Machine Intelligence 1998, 20, 832–844. [Google Scholar] [CrossRef]
- Ho, B.C.; Andreasen, N.C. (2002). Do structural brain deficits worsen following onset of first-episode schizophrenia? In SCHIZOPHRENIA RESEARCH (Vol. 53, No. 3, pp. 98–98). PO BOX 211, 1000 AE AMSTERDAM, NETHERLANDS: ELSEVIER SCIENCE BV.
- Breiman, L. Random Forests. Machine Learning 2001, 45, 5–32. [Google Scholar] [CrossRef]
- Fossati, A.; Madeddu, F.; Maffei, C. Borderline personality disorder and childhood sexual abuse: a meta-analytic study. Journal of personality disorders 1999, 13, 268–280. [Google Scholar] [CrossRef] [PubMed]
- Porter, C.; Palmier-Claus, J.; Branitsky, A.; Mansell, W.; Warwick, H.; Varese, F. Childhood adversity and borderline personality disorder: A meta-analysis. Acta Psychiatrica Scandinavica 2020, 141, 6–20. [Google Scholar] [CrossRef] [PubMed]
- Cicchetti, D.; Rogosch, F.A.; Hecht, K.F.; Crick, N.R.; Hetzel, S. Moderation of maltreatment effects on childhood borderline personality symptoms by gender and oxytocin receptor and FK506 binding protein 5 genes. Development and psychopathology 2014, 26, 831–849. [Google Scholar] [CrossRef]
- Hecht, K.F.; Cicchetti, D.; Rogosch, F.A.; Crick, N.R. Borderline personality features in childhood: The role of subtype, developmental timing, and chronicity of child maltreatment. Development and psychopathology 2014, 26, 805–815. [Google Scholar] [CrossRef]
- Belsky, D.W.; Caspi, A.; Arseneault, L.; Bleidorn, W.; Fonagy, P.; Goodman, M.; Houts, R.; Moffitt, T.E. Etiological features of borderline personality related characteristics in a birth cohort of 12-year-old children. Development and psychopathology 2012, 24, 251–265. [Google Scholar] [CrossRef]
- Gratz, K.L.; Latzman, R.D.; Tull, M.T.; Reynolds, E.K.; Lejuez, C.W. Exploring the association between emotional abuse and childhood borderline personality features: The moderating role of personality traits. Behavior therapy 2011, 42, 493–508. [Google Scholar] [CrossRef]
- Winsper, C.; Zanarini, M.; Wolke, D. Prospective study of family adversity and maladaptive parenting in childhood and borderline personality disorder symptoms in a non-clinical population at 11 years. Psychological medicine 2012, 42, 2405–2420. [Google Scholar] [CrossRef] [PubMed]
- Widom, C.S.; Czaja, S.J.; Paris, J. A prospective investigation of borderline personality disorder in abused and neglected children followed up into adulthood. Journal of personality disorders 2009, 23, 433–446. [Google Scholar] [CrossRef]
- Dadomo, H.; Salvato, G.; Lapomarda, G.; Ciftci, Z.; Messina, I.; Grecucci, A. Structural features predict sexual trauma and interpersonal problems in borderline personality disorder but not in controls: A multi-voxel pattern analysis. Frontiers in Human Neuroscience 2022. [Google Scholar] [CrossRef] [PubMed]
- Bernstein, D.P.; Fink, L.; Handelsman, L.; Foote, J. Childhood trauma questionnaire. Assessment of family violence: A handbook for researchers and practitioners; 1998. [Google Scholar]
- Zanarini, M.C. Zanarini Rating Scale for Borderline Personality Disorder (ZAN-BPD): a continuous measure of DSM-IV borderline psychopathology. Journal of personality disorders 2003, 17, 233. [Google Scholar] [CrossRef] [PubMed]
- Aron, A.R.; Robbins, T.W.; Poldrack, R.A. Inhibition and the right inferior frontal cortex. Trends in cognitive sciences 2004, 8, 170–177. [Google Scholar] [CrossRef]
- Penny, W.D.; Mattout, J.; Trujillo-Barreto, N. Bayesian model selection and averaging. In Statistical Parametric Mapping: The analysis of functional brain images. London: Elsevier; 2006. [Google Scholar]
- Gaser, C.; Dahnke, R.; Thompson, P.M.; Kurth, F.; Luders, E. CAT-a computational anatomy toolbox for the analysis of structural MRI data. BioRxiv. 2022. [CrossRef]
- Ashburner, J. A fast diffeomorphic image registration algorithm. Neuroimage 2007, 38, 95–113. [Google Scholar] [CrossRef]
- Acar, E.; Levin-Schwartz, Y.; Calhoun, V.D.; Adali, T. (2017, May). Tensor-based fusion of EEG and FMRI to understand neurological changes in schizophrenia. In 2017 IEEE International Symposium on Circuits and Systems (ISCAS) (pp. 1-4). IEEE. [CrossRef]
- Wax, M.; Kailath, T. Detection of signals by information theoretic criteria. IEEE Transactions on acoustics, speech, and signal processing 1985, 33, 387–392. [Google Scholar] [CrossRef]
- Himberg, J.; Hyvärinen, A.; Esposito, F. Validating the independent components of neuroimaging time series via clustering and visualization. Neuroimage 2004, 22, 1214–1222. [Google Scholar] [CrossRef]
- Himberg, J.; Hyvarinen, A. (2003, September). Icasso: software for investigating the reliability of ICA estimates by clustering and visualization. In 2003 IEEE XIII Workshop on Neural Networks for Signal Processing (IEEE Cat. No. 03TH8718) (pp. 259-268). IEEE. [CrossRef]
- Hastie, T.; Tibshirani, R.; Friedman, J. The elements of statistical learning; Springer series in statistics: New York, NY, USA, 2001. [Google Scholar]
- Kozak, M.J.; Cuthbert, B.N. The NIMH research domain criteria initiative: background, issues, and pragmatics. Psychophysiology 2016, 53, 286–297. [Google Scholar] [CrossRef]
- Baggio, T.; Grecucci, A.; Meconi, F.; Messina, I. Anxious brains: A combined data fusion machine learning approach to predict trait anxiety from morphometric features. Sensors 2023, 23. [Google Scholar] [CrossRef] [PubMed]
- Mitchell, M.R.; Potenza, M.N. Recent insights into the neurobiology of impulsivity. Current addiction reports 2014, 1, 309–319. [Google Scholar] [CrossRef] [PubMed]
- Bari, A.; Robbins, T.W. Inhibition and impulsivity: behavioral and neural basis of response control. Progress in neurobiology 2013, 108, 44–79. [Google Scholar]
- Lim, J.E.; Kim, S.; Seo, S.; Kang, W.; Kim, A.; Kang, Y. ... & Han, K.M. Association of prefrontal cortex thinning with high impulsivity in healthy adults. Psychiatry Investigation 2021, 18, 570. [Google Scholar]
- Lee, T.M.; Chan, C.C.; Han, S.H.; Leung, A.W.; Fox, P.T.; Gao, J.H. An event-related fMRI study on risk taking by healthy individuals of high or low impulsiveness. Neuroscience Letters 2008, 438, 138–141. [Google Scholar] [CrossRef] [PubMed]
- Pan, N.; Wang, S.; Zhao, Y.; Lai, H.; Qin, K.; Li, J. ... & Gong, Q. Brain gray matter structures associated with trait impulsivity: A systematic review and voxel-based meta-analysis. Human Brain Mapping 2021, 42, 2214–2235. [Google Scholar]
- Hirjak, D.; Thomann, A.K.; Kubera, K.M.; Wolf, R.C.; Jeung, H.; Maier-Hein, K.H.; Thomann, P.A. Cortical folding patterns are associated with impulsivity in healthy young adults. Brain imaging and behavior 2017, 11, 1592–1603. [Google Scholar] [CrossRef]
- Fineberg, N.A.; Chamberlain, S.R.; Goudriaan, A.E.; Stein, D.J.; Vanderschuren, L.J.; Gillan, C.M. ... & Potenza, M.N. New developments in human neurocognition: clinical, genetic, and brain imaging correlates of impulsivity and compulsivity. CNS spectrums 2014, 19, 69–89. [Google Scholar]
- Dalley, J.W.; Everitt, B.J.; Robbins, T.W. Impulsivity, compulsivity, and top-down cognitive control. Neuron 2011, 69, 680–694. [Google Scholar] [CrossRef]
- Carrington, S.J.; Bailey, A.J. Are there theory of mind regions in the brain? A review of the neuroimaging literature. Human brain mapping 2009, 30, 2313–2335. [Google Scholar] [CrossRef]
- Schurz, M.; Radua, J.; Tholen, M.G.; Maliske, L.; Margulies, D.S.; Mars, R.B. ... & Kanske, P. Toward a hierarchical model of social cognition: A neuroimaging meta-analysis and integrative review of empathy and theory of mind. Psychological Bulletin 2021, 147, 293. [Google Scholar] [PubMed]
- Messina, I.; Sambin, M.; Beschoner, P.; Viviani, R. Changing views of emotion regulation and neurobiological models of the mechanism of action of psychotherapy. Cognitive, Affective, & Behavioral Neuroscience 2016, 16, 571–587. [Google Scholar]
- Kernberg, O. Borderline personality organization. Journal of the American psychoanalytic Association 1967, 15, 641–685. [Google Scholar] [CrossRef] [PubMed]
- Roy, A. Childhood trauma and impulsivity. Possible relevance to suicidal behavior. Archives of suicide Research 2005, 9, 147–151. [Google Scholar] [CrossRef] [PubMed]
| BPD | HC | p-values | |
| Participants | 20 | 45 | |
| Age | 35.75 (±8.61) | 36.69 (±8.46) | p=0.401 |
| Gender | F=17, M=3 | F=34, M=11 | p=0.647 |
| Education | ≥ 8 years of formal education | ||
| Exclusion criteria | Neurological disease, psychoactive substance, pregnancy, MRI contraindications, previous head injury | Neurological disease, psychoactive substance, mental illness (SCID-II, SCID-IV), pregnancy, MRI contraindications, previous head injury | |
| Area | Brodmann Area | volume (cc) | Random effects: Max Value (x, y, z) |
|---|---|---|---|
| Postcentral Gyrus | 2, 3, 40 | 1.0/1.5 | 7.4 (-45, -26, 36)/10.0 (43, -24, 39) |
| Precentral Gyrus | 13 | 0.1/0.5 | 4.2 (-45, -21, 37)/8.7 (46, -21, 37) |
| Angular Gyrus | * | 0.0/0.8 | 0 (0, 0, 0)/8.7 (40, -58, 33) |
| Sub-Gyral | 37 | 1.3/2.0 | 6.4 (-22, 7, 47)/7.9 (40, -24, 36) |
| Middle Temporal Gyrus | 19, 21 | 1.9/0.1 | 7.9 (-39, -63, 22)/4.0 (58, -45, -2) |
| Insula | 13, 45 | 3.8/3.8 | 7.4 (-37, -4, 11)/6.3 (39, -11, 14) |
| Middle Frontal Gyrus | 6, 8, 11 | 0.4/1.8 | 5.4 (-24, 4, 44)/7.1 (25, 17, 41) |
| Precuneus | 7, 31, 39 | 0.5/2.4 | 5.9 (-16, -63, 21)/6.6 (13, -61, 38) |
| Cerebellar Tonsil | * | 1.2/1.2 | 6.4 (-27, -44, -42)/6.2 (33, -46, -39) |
| Superior Parietal Lobule | 7 | 0.3/0.4 | 5.9 (-25, -52, 43)/6.3 (30, -55, 43) |
| Superior Frontal Gyrus | 6 | 0.4/0.2 | 6.0 (-22, 11, 48)/4.1 (22, 15, 43) |
| Pyramis | * | 0.4/0.6 | 4.4 (-9, -80, -23)/5.7 (3, -80, -25) |
| Inferior Parietal Lobule | 40 | 0.2/0.7 | 4.4 (-28, -49, 43)/5.7 (40, -59, 38) |
| Fusiform Gyrus | 18, 36, 37 | 0.5/1.0 | 3.9 (-48, -42, -21)/5.7 (45, -43, -12) |
| Uncus (inc amygdala) | 20, 28, 36 | 0.4/0.0 | 5.6 (-30, -9, -29)/0 (0, 0, 0) |
| Extra-Nuclear | * | 0.9/0.1 | 5.6 (-34, 6, 5)/4.0 (37, -11, 7) |
| Medial Frontal Gyrus | * | 0.2/0.0 | 5.6 (-24, 36, 27)/0 (0, 0, 0) |
| Culmen | * | 0.9/0.2 | 5.4 (-1, -48, -1)/4.9 (3, -48, -1) |
| Claustrum | * | 0.4/0.4 | 4.8 (-34, -10, 9)/4.4 (36, -4, 6) |
| Declive | * | 0.2/0.5 | 3.9 (-4, -81, -21)/4.7 (6, -83, -20) |
| Superior Temporal Gyrus | 39, 41, 42 | 0.4/0.0 | 4.6 (-48, -24, 7)/0 (0, 0, 0) |
| Inferior Frontal Gyrus | 47 | 0.6/0.1 | 4.0 (-37, 25, 0)/4.6 (40, 6, 33) |
| Area | Brodmann Area | volume (cc) | random effects: Max Value (x, y, z) |
|---|---|---|---|
| Posterior Cingulate | 30, 31 | 2.3/1.8 | 13.4 (-22, -58, 8)/11.6 (22, -64, 10) |
| Cuneus | 17, 18, 19, 23, 30 | 4.0/5.1 | 11.7 (-16, -69, 10)/13.0 (21, -68, 10) |
| Extra-Nuclear | * | 0.6/0.8 | 11.7 (-21, -53, 8)/10.7 (25, -55, 8) |
| Thalamus | * | 3.8/2.0 | 9.3 (-10, -17, 9)/5.9 (9, -13, 8) |
| Lingual Gyrus | 18, 19 | 3.7/1.4 | 9.1 (-18, -52, 5)/6.8 (22, -54, 5) |
| Lateral Ventricle | * | 0.3/0.5 | 6.0 (-28, -58, 8)/8.3 (28, -58, 8) |
| Middle Temporal Gyrus | 39 | 0.8/0.3 | 8.1 (-50, -55, 7)/5.2 (34, -72, 19) |
| Sub-Gyral | * | 0.3/1.0 | 4.7 (-27, -89, 2)/6.8 (28, -54, 5) |
| Cerebellar Tonsil | * | 0.0/0.6 | 0(0, 0, 0)/6.4 (12, -56, -41) |
| Anterior Cingulate | 32 | 0.4/0.6 | 4.0 (-9, 26, 25)/5.8 (10, 41, 8) |
| Precuneus | 7 | 0.4/0.1 | 5.8 (-19, -62, 43)/4.2 (4, -73, 24) |
| Inferior Parietal Lobule | 40 | 0.3/0.5 | 5.7 (-40, -36, 57)/4.4 (53, -26, 28) |
| Middle Frontal Gyrus | 9 | 0.6/0.5 | 5.6 (-37, 15, 38)/5.2 (39, 18, 31) |
| Postcentral Gyrus | 1, 2, 3, 40 | 1.5/0.1 | 5.6 (-48, -19, 51)/4.1 (64, -28, 21) |
| Middle Occipital Gyrus | 18, 19 | 0.4/0.1 | 5.4 (-28, -86, 4)/3.8 (34, -75, 16) |
| Inferior Semi-Lunar Lobule | * | 0.0/0.6 | 0 (0, 0, 0)/4.8 (9, -59, -41) |
| Area | Brodmann Area | volume (cc) | random effects: Max Value (x, y, z) |
|---|---|---|---|
| Middle Temporal Gyrus | 37, 39 | 0.2/1.2 | 4.8 (-56, -56, 10)/9.9 (59, -51, -5) |
| Inferior Temporal Gyrus | 37 | 0.0/0.6 | 0 (0, 0, 0)/8.4 (62, -54, -5) |
| Middle Frontal Gyrus | 6, 8, 9, 10, 11, 46 | 2.2/3.6 | 5.5 (-45, 30, 39)/7.6 (49, 34, 33) |
| Inferior Frontal Gyrus | 10, 46, 47 | 1.4/0.0 | 7.1 (-48, 33, -13)/0 (0, 0, 0) |
| Superior Frontal Gyrus | 6, 8, 9, 10 | 1.2/1.8 | 6.5 (-19, 50, 38)/7.0 (22, 0, 65) |
| Superior Temporal Gyrus | 13, 22, 39 | 1.0/1.2 | 4.8 (-52, -16, 9)/6.9 (61, -49, 15) |
| Claustrum | * | 0.3/0.4 | 5.7 (-34, -6, 6)/6.8 (36, -5, 7) |
| Insula | 13 | 1.7/1.1 | 6.5 (-36, -2, 8)/5.8 (36, -5, 11) |
| Postcentral Gyrus | 1, 2, 3, 5 | 1.2/0.3 | 6.4 (-56, -27, 39)/5.2 (67, -14, 33) |
| Inferior Parietal Lobule | 40 | 2.2/1.5 | 6.0 (-46, -44, 48)/6.3 (52, -50, 43) |
| Extra-Nuclear | * | 0.6/0.8 | 4.6 (-34, -3, 3)/6.2 (36, -1, 7) |
| Precuneus | 7 | 0.6/0.3 | 5.7 (-9, -54, 48)/4.8 (22, -63, 46) |
| Superior Parietal Lobule | 7 | 0.0/0.4 | 0 (0, 0, 0)/5.1 (25, -60, 44) |
| Lentiform Nucleus | * | 0.6/0.3 | 4.5 (-15, 3, -5)/4.0 (15, 7, -4) |
| Cingulate Gyrus | 23, 24 | 0.4/0.4 | 4.3 (-1, 3, 27)/4.5 (3, 1, 28) |
| Anterior Cingulate | 24, 32 | 0.3/0.9 | 3.7 (-3, 35, 1)/4.3 (3, 35, 1) |
| Area | Brodmann Area | volume (cc) | random effects: Max Value (x, y, z) |
|---|---|---|---|
| Inferior Parietal Lobule | 7, 39, 40 | 0.8/2.7 | 8.1 (-28, -47, 56)/10.3 (34, -48, 56) |
| Sub-Gyral | 7, 20, 40 | 1.9/2.2 | 9.6 (-28, -50, 54)/8.0 (31, -44, 51) |
| Superior Parietal Lobule | 7 | 1.0/0.6 | 9.5 (-30, -51, 58)/9.1 (34, -49, 61) |
| Precuneus | 7, 31 | 1.4/0.7 | 9.0 (-28, -50, 49)/6.0 (30, -47, 48) |
| Fusiform Gyrus | 20, 36, 37 | 0.4/0.1 | 7.8 (-40, -17, -24)/4.1 (50, -42, -18) |
| Cuneus | 7, 17, 18, 19, 30 | 3.6/3.3 | 6.6 (-10, -76, 31)/6.7 (28, -83, 26) |
| Middle Temporal Gyrus | 19, 21, 39 | 0.1/1.3 | 3.7 (-62, -52, 0)/6.6 (55, -56, 8) |
| Lingual Gyrus | 18, 19 | 1.5/0.8 | 5.8 (-21, -64, 1)/4.6 (22, -63, 2) |
| Postcentral Gyrus | 1, 3, 5 | 0.8/0.0 | 5.6 (-43, -30, 62)/-999.0 (0, 0, 0) |
| Inferior Occipital Gyrus | 18 | 0.6/0.1 | 5.6 (-34, -89, -3)/4.2 (48, -80, -2) |
| Superior Frontal Gyrus | 9, 10, 11 | 1.2/1.0 | 5.5 (-15, 65, -10)/5.2 (16, 66, -13) |
| Inferior Temporal Gyrus | 20 | 0.5/0.1 | 5.5 (-43, -17, -27)/4.1 (50, -56, -12) |
| Middle Occipital Gyrus | 18, 19, 37 | 0.8/1.9 | 5.2 (-34, -89, 1)/5.2 (36, -79, 14) |
| Posterior Cingulate | 30 | 0.5/0.7 | 5.1 (-21, -64, 6)/4.8 (19, -58, 7) |
| Area | Brodmann Area | Volume (cc) | Random Effects: Max Value (x, y, z) |
|---|---|---|---|
| Postcentral Gyrus | 1, 2, 3, 4, 5, 7, 40, 43 | 6.1/7.4 | 9.3 (-52, -20, 30)/9.8 (53, -17, 31) |
| Middle Temporal Gyrus | 21, 22, 39 | 2.9/1.0 | 9.7 (-49, -41, 5)/6.2 (50, -43, 9) |
| Precuneus | 7, 19, 39 | 1.1/2.2 | 5.0 (-21, -62, 42)/9.0 (30, -61, 35) |
| Parahippocampal Gyrus | 19, 36, 37 | 3.3/2.0 | 8.7 (-28, -43, -7)/7.7 (30, -44, -5) |
| Inferior Parietal Lobule | 40 | 4.2/5.4 | 5.9 (-55, -23, 30)/8.7 (55, -28, 26) |
| Precentral Gyrus | 4, 6, 9, 13, 43 | 0.9/2.2 | 6.0 (-36, 4, 29)/8.4 (50, -17, 34) |
| Superior Temporal Gyrus | 22, 39, 41, 42 | 3.4/3.4 | 8.2 (-48, -49, 13)/8.1 (53, -45, 12) |
| Superior Parietal Lobule | 7 | 0.4/1.0 | 5.9 (-22, -59, 44)/8.2 (27, -58, 43) |
| Sub-Gyral | 43 | 1.6/3.1 | 7.0 (-46, -43, 5)/8.1 (30, -64, 32) |
| Inferior Frontal Gyrus | 9 | 0.5/0.0 | 7.8 (-39, 4, 32)/0 (0, 0, 0) |
| Fusiform Gyrus | 19, 20, 37 | 1.2/0.6 | 7.6 (-30, -36, -12)/5.6 (28, -47, -8) |
| Insula | 13, 41 | 0.1/1.9 | 3.8 (-46, -15, 12)/7.1 (46, -22, 16) |
| Angular Gyrus | 39 | 0.9/0.0 | 6.5 (-42, -58, 32)/0 (0, 0, 0) |
| Transverse Temporal Gyrus | 41, 42 | 0.1/0.7 | 3.9 (-53, -14, 12)/6.4 (48, -21, 12) |
| Supramarginal Gyrus | 40 | 1.3/0.2 | 6.4 (-39, -53, 27)/4.8 (52, -48, 22) |
| Anterior Cingulate | 24, 32 | 1.3/0.4 | 6.3 (-3, 32, -7)/4.9 (3, 29, -10) |
| Cuneus | 18, 19 | 0.2/1.3 | 4.0 (-7, -79, 14)/5.1 (10, -88, 14) |
| Culmen | * | 1.3/2.6 | 4.7 (-22, -41, -12)/4.9 (31, -39, -22) |
| Cingulate Gyrus | 31 | 0.9/0.3 | 4.7 (-1, -32, 36)/4.4 (1, -32, 39) |
| Lingual Gyrus | 18, 19 | 0.8/0.1 | 4.6 (-18, -55, -2)/3.6 (22, -53, -2) |
| Declive | * | 0.8/0.0 | 4.1 (-18, -59, -13)/0 (0, 0, 0) |
| Area | Brodmann Area | volume (cc) | random effects: Max Value (x, y, z) |
|---|---|---|---|
| Sub-Gyral | 6 | 0.8/0.8 | 6.4 (-21, 4, 51)/5.2 (25, -6, 56) |
| Middle Temporal Gyrus | * | 0.1/0.4 | 3.8 (-48, -63, 2)/5.8 (42, -66, 16) |
| Middle Frontal Gyrus | 6, 8 | 0.9/1.9 | 4.7 (-33, -2, 43)/5.6 (28, -6, 53) |
| Fusiform Gyrus | 20 | 0.1/0.5 | 4.0 (-42, -33, -16)/5.0 (43, -27, -18) |
| Medial Frontal Gyrus | 6 | 0.6/0.2 | 4.9 (-18, 7, 51)/4.5 (10, -10, 61) |
| Superior Frontal Gyrus | 6 | 0.5/0.3 | 4.4 (-13, -11, 63)/4.1 (18, -7, 63) |
| Area | Brodmann Area | volume (cc) | random effects: Max Value (x, y, z) |
|---|---|---|---|
| Middle Frontal Gyrus | 9, 46 | 1.4/0.1 | 10.2 (-46, 31, 33)/4.1 (48, 39, 26) |
| Precuneus | 7, 19 | 2.8/2.0 | 5.8 (-22, -74, 41)/9.9 (24, -70, 49) |
| Superior Parietal Lobule | 7 | 0.2/0.8 | 4.8 (-39, -57, 51)/8.8 (25, -69, 45) |
| Inferior Parietal Lobule | 39, 40 | 1.2/4.4 | 6.2 (-62, -40, 24)/8.4 (49, -42, 56) |
| Middle Occipital Gyrus | 19 | 0.9/0.0 | 7.3 (-39, -85, 17)/0 (0, 0, 0) |
| Precentral Gyrus | 4, 6, 44 | 0.8/4.1 | 5.8 (-61, -6, 21)/7.3 (55, -17, 35) |
| Supramarginal Gyrus | 40 | 0.7/0.2 | 7.1 (-62, -42, 27)/4.5 (49, -36, 34) |
| Postcentral Gyrus | 1, 2, 3, 7, 40, 43 | 2.0/3.9 | 5.6 (-43, -29, 53)/7.1 (53, -16, 31) |
| Superior Temporal Gyrus | 21, 22, 41, 42 | 0.4/2.2 | 5.0 (-65, -40, 21)/7.0 (67, -27, 15) |
| Cuneus | 17, 19 | 0.4/0.6 | 4.2 (-7, -92, 3)/6.1 (31, -82, 30) |
| Sub-Gyral | * | 0.7/0.3 | 6.1 (-46, -36, -13)/5.0 (18, -45, 62) |
| Transverse Temporal Gyrus | 41 | 0.0/0.4 | 0 (0, 0, 0)/5.9 (48, -29, 12) |
| Insula | 13 | 0.0/0.6 | 0 (0, 0, 0)/5.8 (52, -30, 18) |
| Middle Temporal Gyrus | 19, 21, 39 | 0.8/0.3 | 5.7 (-50, -75, 19)/5.3 (49, -63, 21) |
| Lingual Gyrus | 17, 19 | 0.8/0.0 | 5.1 (-22, -64, 1)/0 (0, 0, 0) |
| Superior Frontal Gyrus | 6, 8, 9, 10 | 0.4/0.1 | 4.6 (-22, 46, 39)/3.7 (12, 14, 50) |
| Area | Brodmann Area | volume (cc) | random effects: Max Value (x, y, z) |
|---|---|---|---|
| Precentral Gyrus | 6, 9 | 1.3/0.1 | 8.1 (-37, -6, 62)/3.7 (39, 16, 35) |
| Superior Frontal Gyrus | 6, 8, 9, 10, 11 | 5.1/3.0 | 7.3 (-10, -4, 67)/8.0 (25, -1, 66) |
| Middle Frontal Gyrus | 6, 8, 9, 10, 46 | 7.7/2.6 | 7.6 (-34, -3, 62)/7.0 (31, -3, 61) |
| Middle Occipital Gyrus | 19, 37 | 0.4/0.1 | 6.5 (-49, -67, 5)/3.8 (27, -70, 6) |
| Superior Parietal Lobule | 7 | 0.4/0.0 | 6.4 (-28, -54, 61)/0 (0, 0, 0) |
| Medial Frontal Gyrus | 6, 11 | 1.3/0.7 | 5.2 (-13, -4, 61)/6.4 (15, 1, 58) |
| Middle Temporal Gyrus | 21, 37, 39 | 0.2/0.6 | 5.5 (-46, -64, 6)/5.2 (68, -32, -7) |
| Sub-Gyral | 6 | 1.6/0.3 | 4.6 (-25, 15, 41)/5.3 (18, -2, 57) |
| Insula | 13 | 0.4/0.4 | 4.5 (-36, -5, 10)/4.6 (37, 0, 8) |
| Cingulate Gyrus | 32 | 0.3/0.5 | 3.8 (-18, 8, 44)/4.4 (15, 16, 36) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).




