Background: COVID-19 manifested with a wide range of clinical symptoms, including asymptomatic or mild illness and life-threatening respiratory failure. We hypothesized that elevated predictors during intensive care unit (ICU) stays would independently predict mortality and the subsequent development of post-COVID-19 condition (PCC).
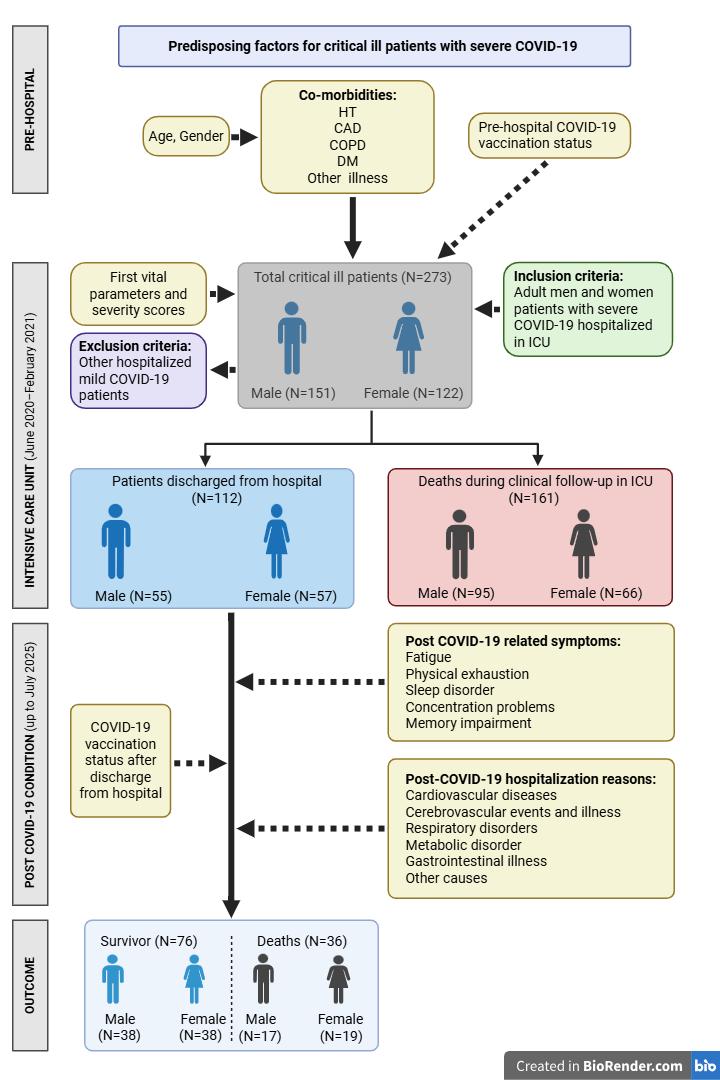
Methods: In this retrospective cohort study, we evaluated the clinical and laboratory determinants of mortality using hospital records in severe COVID-19 patients in conjunction with their PCC in survivors by self-reported survey. This research was conducted at XX University Hospital, and adult patients with laboratory-confirmed SARS-CoV-2 infection by RT-PCR assay who required ICU admission for respiratory failure or hemodynamic instability were included. Biomarkers were monitored throughout ICU stay to evaluate dynamic changes and their association with mortality. Survivors were followed from ICU discharge to assess readmissions, vaccination status, and post-COVID-19 condition, including fatigue, sleep disturbance, physical exhaustion, concentration problems, and memory impairment. Post-ICU mortality and hospitalization due to cardiovascular, respiratory, neurological, or other complications were recorded.
Results: A total of 273 critically ill patients were included, of whom 112 survived and 161 died during ICU stay. Non-survivors were older and had lower mean arterial pressure. Intubation was more frequent among non-survivors, and APACHE II scores were significantly higher in this group. Hospitalizations due to cardiovascular, respiratory, and neurological complications were particularly associated with increased hazard of death (HRs ≥2, p-values < 0.05). Patients who died after ICU discharge (31.5%) had higher rates of fatigue, physical exhaustion, and memory impairment, suggesting a strong correlation between biomarker derangements during ICU stay and PCC.
Conclusions: The present study was specifically designed to address this critical gap by evaluating whether biomarker trajectories during ICU follow-up not only predict in-hospital mortality but also serve as early determinants of Post-COVID status in survivors.