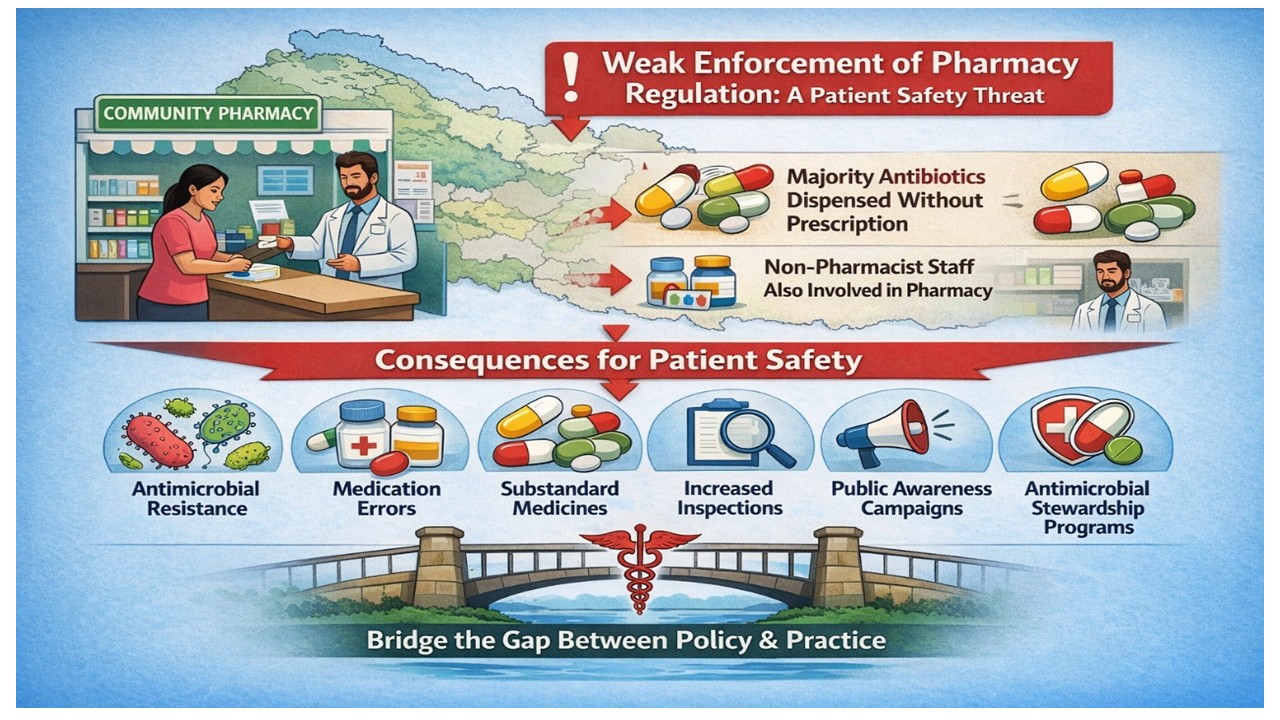
Background: Effective pharmacy regulation is a cornerstone of patient safety and rational medicine use. In Nepal, despite the existence of regulatory frameworks such as the Drug Act 2035 and policies restricting non-prescription sales of antibiotics, enforcement is weak and inconsistent, leading to widespread regulatory failure in community pharmacies. Problem: Multiple studies have documented widespread dispensing of antibiotics without valid prescriptions in community pharmacies across Nepal, with non-pharmacist staff frequently engaging in these practices. Analysis: Policy and practice gaps in Nepal’s pharmacy sector reflects systemic issues including insufficient regulatory capacity, workforce shortages of qualified pharmacists, market-driven dispensing behaviors, and low public awareness of rational medicine use. These structural barriers continue unsafe pharmaceutical care and weaken pharmacovigilance systems. Policy Implications: Strengthening enforcement must be reframed as a health systems and patient safety priority rather than a narrow regulatory task. A multi-pronged strategy including mandatory qualified pharmacist presence, enhanced inspection and compliance monitoring, integration of community pharmacies into national antimicrobial stewardship programs, and public awareness campaigns is urgently needed. Conclusion: Weak enforcement of pharmacy regulation in Nepal constitutes a significant but under-recognized threat to patient safety and antimicrobial stewardship. Translating existing policies into practice through systemic reforms can reduce medication-related harm and preserve antibiotic effectiveness.