Submitted:
03 May 2026
Posted:
05 May 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Methods
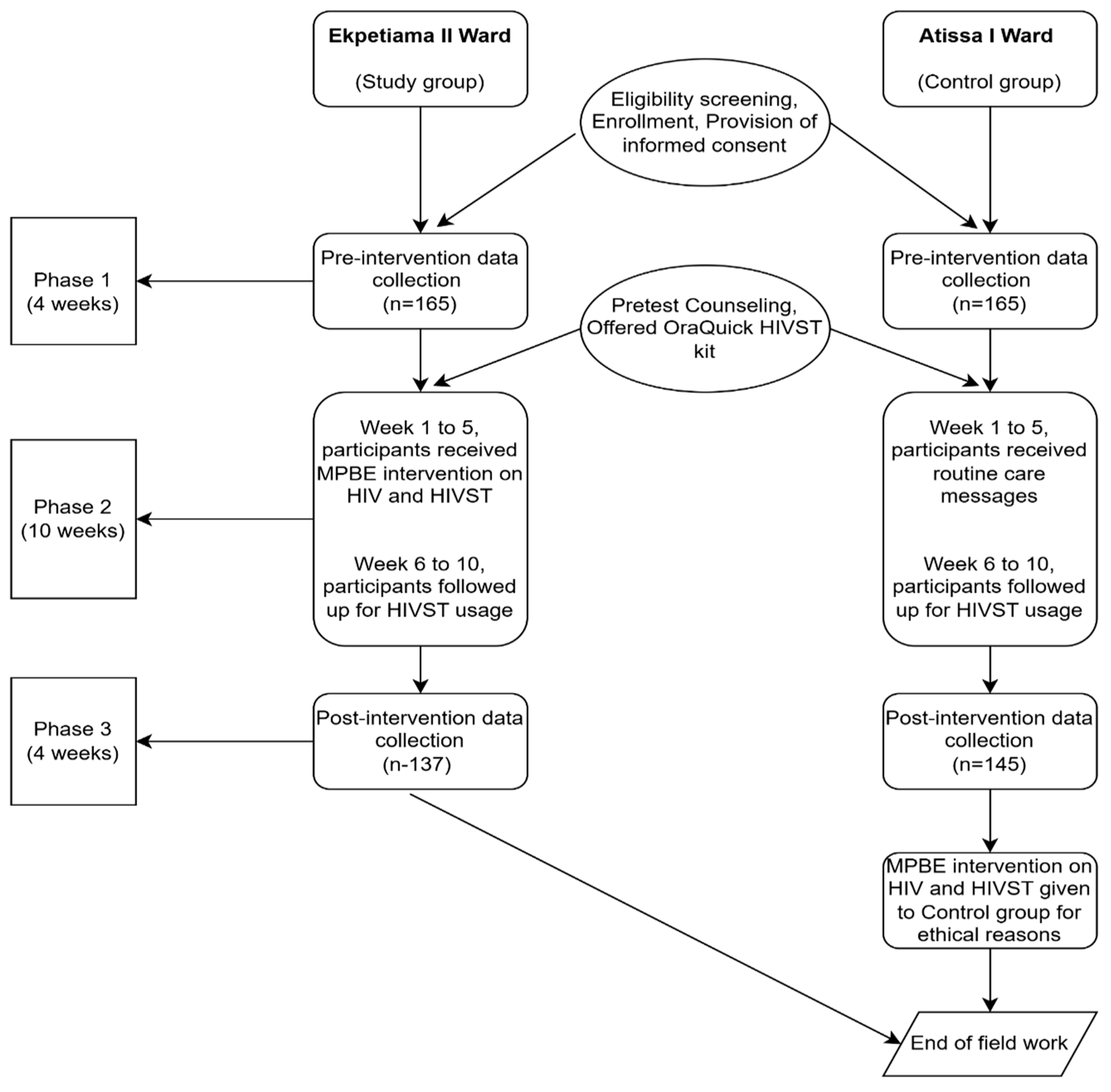
2.1. Study Design
2.2. Setting
2.3. Participants
2.4. Sample Size
2.5. Sampling Procedure
2.6. Participant Recruitment
2.7. Pre-Intervention Phase and Baseline Data Collection
2.8. Intervention
2.9. Outcome Measures
2.10. Post-Intervention Assessment
2.11. Statistical Analysis
2.12. Ethics Approval
3. Results
4. Discussion
5. Implications for Policy and Interventions
6. Summary of Findings
7. Study Limitations
8. Conclusions
9. Health Significance
10. Recommendations
- a.
-
Short-term recommendations:
- Scale up mobile phone-based educational programs targeting female sex workers to rapidly improve HIV and HIVST knowledge and testing uptake.
- Provide clear guidance and visual aids for oral-based HIVST kits to ensure correct usage and interpretation of results.
- Implement follow-up support via calls or messaging to verify testing and address user questions, leveraging the high engagement seen in the intervention group.
- b.
-
Mid-term recommendations:
- Integrate mobile education programs with local health services to ensure seamless linkage from self-testing to confirmatory testing and treatment.
- Tailor educational content to address socio-demographic variations, including literacy levels and secondary occupations, to maximize reach and engagement.
- Develop community-based campaigns to reduce stigma and normalize HIV self-testing among female sex workers and similar key populations.
- c.
-
Long-term recommendations:
- Expand digital health strategies to include multiple forms of HIVST kits and other preventive health tools to enhance overall health literacy and self-care capacity.
- Establish sustainable mobile health infrastructure, ensuring equitable access for marginalized populations without mobile phones.
- Conduct longitudinal studies to assess long-term behavioral change, HIV incidence reduction, and the cost-effectiveness of mobile phone-based interventions in broader populations.
Funding
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Abaya, S.T.; Ogoina, D.; Stow, J.; Abaye, B.B.; Emeka, C.; Raimi, M.O. Beyond the Epidemic: Effective Public Health Strategies in Response to Nigeria’s First Lassa Fever Outbreak in a Non-Endemic Region. JMIR Preprints 2024, 19/08/2024, 65539. Available online: https://preprints.jmir.org/preprint/65539. [CrossRef]
- Abdulraheem, A.F.; Ononokpono, D.N.; Raimi, M.O. Breaking Barriers: How Socio-Demographic, Cultural, and Geographic Factors Shape Skilled Birth Attendance in Nigeria – A Call for Equity and Empowerment. JMIR Preprints 2025a, 78050. Available online: https://preprints.jmir.org/preprint/78050.
- Abdulraheem, A.F.; Raimi, M.O.; Ononokpono, D.N. (2025b) Who Delivers Safely? The Hidden Role of Transport and Education in Nigeria’s Maternal Health Crisis. JMIR Preprints. 21/06/2025, 79460. Available online: https://preprints.jmir.org/preprint/79460. [CrossRef]
- Abdulraheem, A.F.; Ononokpono, D.N.; Raimi, M.O. Breaking barriers to safe motherhood: how social, cultural, and geographic inequalities shape skilled birth attendance in Nigeria. Sociol Int J. 2025c, 9(5), 188‒200. [Google Scholar] [CrossRef]
- Abiye, T.; Tano, D. A.; Morufu, O. R (2026) Extractive Economies, Invisible Burdens: Reframing Environmental Degradation in the Niger Delta as a Public Health Emergency. Preprints. [CrossRef]
- Adaka, O. A.; Owoaje, E. T.; Tella, A. O. Feasibility of mHealth interventions towards promoting HIV self-testing uptake in sub-Saharan Africa: A systematic review of literature. International Journal of Current Science Research and Review 2024, 7(1), 609–632. [Google Scholar] [CrossRef]
- Agusomu, T.D.; Ohwo, O.; Raimi, M.O. Living with the waters: perception, adaptation, and policy implications of flooding in Yenagoa metropolis, Nigeria. Open Access J Sci. 2025, 8(1), 117‒131. [Google Scholar] [CrossRef]
- Akankunda, S.; Nambi Najjuma, J.; Tayebwa, S.; Byamugisha, B.; Ariho, S.; Bahati, R. The role of mass media campaigns in improving adherence to antiretroviral therapy among adolescents living with HIV in southwestern Uganda. HIV/AIDS (Auckland, N.Z.) 2022, 14, 397–407. [Google Scholar] [CrossRef]
- Anthony, B.P.; Charles, O.; Raimi, M.O. 2025) Black Gold, Empty Plates: How Oil and Gas Are Destroying Food Security in the Niger Delta. JMIR Preprints. 13/05/2025, 77458. Available online: https://preprints.jmir.org/preprint/77458. [CrossRef]
- Atobauka, I.; Jacob, O. N. Poverty and women prostitution in Nigeria: A study of Wukari Local Government Area, Taraba State. International Journal of Integrative Education 2021, 4(9), 42–54. Available online: https://media.neliti.com/media/publications/352271-poverty-and-women-prostitution-in-nigeri-75ff2b39.pdf.
- Atuhaire, L.; Shumba, C. S.; Mapahla, L.; Maposa, I.; Nyasulu, P. S. Factors associated with adherence to HIV testing guidelines among HIV-negative female sex workers in Kampala, Uganda. IJID Regions 2022, 4, 25–32. [Google Scholar] [CrossRef] [PubMed]
- Ayele, M.; Alamrew, A.; Lake, E. S.; Yilak, G.; Tilahun, B. D.; Tenaw, L. A.; et al. Female sex workers’ perceptions, concerns and acceptability of OraQuick HIV self-test in Woldia town, North Wollo, Ethiopia: A qualitative study. BMJ Open 2025, 15(5), e096645. [Google Scholar] [CrossRef]
- Aziba-anyam, G.R.; Morufu, O.R. Leveraging Digital Platforms for Community-Driven Public Health Surveillance in the Niger Delta: A Feasibility Study from Bayelsa State, Nigeria. Oral Presentation Presented at the ACS-FUO Conference of the Faculty of Science, Federal University Otuoke, Bayelsa State on the theme: Harnessing Green Chemistry & Artificial Intelligence for Sustainable Development, which held Tuesday, 4th - Thursday 7th November; 2025; p. Pg. 124. [Google Scholar]
- Babatunde, A. O.; Agboola, P.; Babatunde, Y.; Ilesanmi, E. B.; Ayodele, H.; Ezechi, O. C. Assessment of knowledge and acceptability of HIV self-testing among students of selected universities in southwest Nigeria: An online cross-sectional study. Pan African Medical Journal 2022, 43, 94. [Google Scholar] [CrossRef]
- Balán, I. C.; Lopez-Ríos, J.; Nayak, S.; Lentz, C.; Arumugam, S.; Kutner, B. A.; et al. SMARTtest: A smartphone app to facilitate HIV and syphilis self- and partner-testing, interpretation of results, and linkage to care. AIDS and Behavior 2020, 24(5), 1560–1573. [Google Scholar] [CrossRef]
- Beecroft, A.; O, V.; N, P. P. Digital HIV self-testing as an exemplar: A perspective on benefits, challenges, and opportunities. Expert Review of Molecular Diagnostics 2024, 24(10). [Google Scholar] [CrossRef]
- Boisvert Moreau, M.; Kintin, F. D.; Atchekpe, S.; Batona, G.; Béhanzin, L.; Guédou, F. A.; et al. HIV self-testing implementation, distribution and use among female sex workers in Cotonou, Benin: A qualitative evaluation of acceptability and feasibility. BMC Public Health 2022, 22(1), 589. [Google Scholar] [CrossRef]
- Budhwani, H.; KR, H.; J, H.; J, W. HIV knowledge among cisgender female sex workers of Haitian descent working at the border of Haiti and Dominican Republic. Frontiers in Reproductive Health 2021, 3, 700861. [Google Scholar] [CrossRef]
- Christopher, O.E.; Teddy, C.A.; Uchenna, G.E.; Aziba-anyam, G.R.; Morufu, O.R. 2025) Digital Science Observatory (DSO) Web Application: Advancing Data Science for Sustainability. Oral Presentation Presented at the 1st International Conference of the Faculty of Science, Federal University Otuoke, Bayelsa State on the theme: Revolutionizing a Sustainable Tomorrow: Harnessing Science, Innovation and Community Power to Drive Circular Economy Solutions, Climate Resilience, and a Thriving Green Economy, which held Tuesday, 4th – Friday 7th March; 2025; p. Pp. 21. [Google Scholar]
- Christopher, O.E.; Muyi, A.; Teddy, C.A.; Rotifa, S.U.; Oyeyemi, A.S.; Uchenna, G.E.; Ansa, H.; Oyindiepreye, L.A.; Akinloye, B.O.; Morufu, O.R. Transforming Primary Healthcare in Nigeria: Enhancing Universal Health Coverage through Strong and Sustainable Primary Healthcare Laboratories; Qeios, 2024. [Google Scholar] [CrossRef]
- City Population. Bayelsa State, Nigeria - Population statistics, charts, map and location. 2022. Available online: https://citypopulation.de/en/nigeria/admin/NGA006__bayelsa/.
- Conserve, D. F.; Jennings, L.; Aguiar, C.; Shin, G.; Handler, L.; Maman, S. Systematic review of mobile-health behavioral interventions to improve uptake of HIV testing for vulnerable and key populations. Journal of Telemedicine and Telecare 2017, 23(2), 347–359. [Google Scholar] [CrossRef] [PubMed]
- Eduweb. Yenagoa wards - New and existing polling unit. 2020. Available online: https://www.eduweb.com.ng/yenagoa-wards-new-and-existing-polling-unit/.
- Ekholuenetale, M.; Nzoputam, C. I.; Okonji, O. C. Association between socio-economic factors and HIV self-testing knowledge amongst South African women. Southern African Journal of HIV Medicine 2022, 23(1), 1347. [Google Scholar] [CrossRef] [PubMed]
- Elemuwa, C.O.; Raimi, M.O.; Ainu, M.; Adias, T.C.; Ufuoma, R.S.; Elemuwa, U.G.; Oginifolunnia, O.C.; Rath, B.A.; Obermeier, P.E. Conquering Mpox: A Comprehensive Public Health Strategy for Addressing Mpox and Poxvirus Infections in Nigeria – Understanding Global Trends, Transmission Dynamics, and Effective Prevention and Control Measures in Nigeria. JMIR Preprints 2024, 14/10/2024, 67534. Available online: https://preprints.jmir.org/preprint/67534. [CrossRef]
- Emmanuel, F.; Ejeckam, C. C.; Green, K.; Adesina, A. A.; Aliyu, G.; Ashefor, G.; et al. HIV epidemic among key populations in Nigeria: Results of the integrated biological and behavioural surveillance survey (IBBSS), 2020–2021. Sexually Transmitted Infections 2025, 101(1). Available online: https://sti.bmj.com/content/101/1/10. [CrossRef]
- Eskezia, B. N.; Tafere, Y.; Aschale, A.; Moges, N. A. Uptake of HIV self-testing and associated factors among female sex workers at non-governmental HIV testing facilities in Debre Markos and Bahir Dar towns, Northwest Ethiopia, 2022. HIV/AIDS (Auckland, N.Z.) 2023, 15, 279–291. [Google Scholar] [CrossRef]
- Ezekiel, A.A.; Raimi, M.O. Pandemic Preparedness and the Infodemic: Communication Strategies to Mitigate Misinformation and Improve Public Compliance. JMIR Preprints 2026, 13/04/2026, 98088. Available online: https://preprints.jmir.org/preprint/98088. [CrossRef]
- Ezelote, C. J.; Nj, O.; Aj, M.; Ck, O.; Om, O.; Cj, O.; et al. Effect of peer health education intervention on HIV/AIDS knowledge amongst in-school adolescents in secondary schools in Imo State, Nigeria. BMC Public Health 2024, 24(1), 1029. [Google Scholar] [CrossRef]
- Figueroa, C.; Johnson, C.; Ford, N.; Sands, A.; Dalal, S.; Meurant, R.; et al. Reliability of HIV rapid diagnostic tests for self-testing compared with testing by health-care workers: A systematic review and meta-analysis. The Lancet HIV 2018, 5(6), e277–e290. [Google Scholar] [CrossRef]
- Fischer, A. E.; Phatsoane, M.; Majam, M.; Shankland, L.; Abrahams, M.; Rhagnath, N.; et al. Uptake of the Ithaka mobile application in Johannesburg, South Africa, for human immunodeficiency virus self-testing result reporting. Southern African Journal of HIV Medicine 2021, 22(1), 1197. [Google Scholar] [CrossRef]
- Folayan, M. O.; Odetoyinbo, M.; Harrison, A.; Brown, B. Rape in Nigeria: A silent epidemic among adolescents with implications for HIV infection. Global Health Action 2014, 7(1), 25583. [Google Scholar] [CrossRef]
- Garg, P. R.; Uppal, L.; Mehra, S.; Mehra, D. Mobile health app for self-learning on HIV prevention knowledge and services among a young Indonesian key population: Cohort study. JMIR mHealth and uHealth 2020, 8(9), e17646. [Google Scholar] [CrossRef] [PubMed]
- Ghana AIDS Commission (GAC). HIV and AIDS prevention program in Ghana: Training manual: Peer educator workshop. 2014. Available online: https://www.fhi360.org/wpcontent/uploads/drupal/documents/Manual%20FSW%20Peer%20Educators_reduced.pdf.
- Gous, N.; Fischer, A. E.; Rhagnath, N.; Phatsoane, M.; Majam, M.; Lalla-Edward, S. T. Evaluation of a mobile application to support HIV self-testing in Johannesburg, South Africa. Southern African Journal of HIV Medicine 2020, *21*(1), 1088. [Google Scholar] [CrossRef] [PubMed]
- Goyal, R. C. Research methodology for health professionals; Jaypee Brothers Medical Publishers, 2010. [Google Scholar]
- Grant, W.; Adan, M. A.; Samurkas, C. A.; Quigee, D.; Benitez, J.; Gray, B.; et al. Effect of participative web-based educational modules on HIV and sexually transmitted infection prevention competency among medical students: Single-arm interventional study. JMIR Medical Education 2023, 9, e42197. [Google Scholar] [CrossRef]
- Guillamet, L. J. V.; Babey, M. M.; Njah, M.; Blake, H.; Jasani, A.; Kyeng, R.; et al. Acceptability, feasibility and potential of an intervention using secret Facebook groups to complement existing HIV prevention strategies among female sex workers in Cameroon, a randomized pilot study. AIDS Care 2024, 36(4), 517–527. [Google Scholar] [CrossRef] [PubMed]
- Harichund, C.; Karim, Q. A.; Kunene, P.; Simelane, S.; Moshabela, M. HIV self-testing as part of a differentiated HIV testing approach: Exploring urban and rural adult experiences from KwaZulu-Natal, South Africa using a cross-over study design. BMC Public Health 2019, 19(1). [Google Scholar] [CrossRef]
- Harichund, C.; Kunene, P.; Simelane, S.; Karim, Q. A.; Moshabela, M. Repeat HIV testing practices in the era of HIV self-testing among adults in KwaZulu-Natal, South Africa. PLOS ONE 2019, 14(2), e0212343. [Google Scholar] [CrossRef]
- Henry, O.S.; Morufu, O.R. 2025) Surveillance in the Shadows: Reinventing Community-Based Disease Monitoring Systems in Rural Nigeria. Oral Presentation Presented at the 3rd Ku8+International Conference, Kwara State University, Malete with the theme “Innovation and Sustainability of Higher Education in a Changing World.”, which held on Wednesday, 6th – Friday 8th August; 2025. [Google Scholar]
- Janssen, R.; Engel, N.; Esmail, A.; Oelofse, S.; Krumeich, A.; Dheda, K.; et al. Alone but supported: A qualitative study of an HIV self-testing app in an observational cohort study in South Africa. AIDS and Behavior 2020, 24(2), 467–474. [Google Scholar] [CrossRef] [PubMed]
- Janssen, R.; Engel, N.; Pant Pai, N.; Esmail, A.; Dheda, K.; Thomas, R.; et al. ‘You’re only there on the phone’? A qualitative exploration of community, affect and agential capacity in HIV self-testing using a smartphone app. Sociology of Health & Illness 2021, *43*(3), 591–606. [Google Scholar] [CrossRef]
- Janssen, R.; Krumeich, A.; Esmail, A.; Thomas, R.; Dheda, K.; Pant Pai, N.; Engel, N. Moments of uncertainty: Exploring how an app-based oral HIV self-testing strategy fits in communities “living under” HIV risk. Medicine Anthropology Theory 2021, 8(2), 1–24. [Google Scholar] [CrossRef]
- Joint United Nations Programme on HIV/AIDS (UNAIDS). Country progress report - Nigeria. 2020. Available online: https://www.unaids.org/sites/default/files/country/documents/NGA_2020_countryreport.pdf.
- Joint United Nations Programme on HIV/AIDS (UNAIDS). Ending inequalities and getting on track to end AIDS by 2030. 2021. Available online: https://www.unaids.org/sites/default/files/media_asset/2021-political-declaration_summary-10-targets_en.pdf.
- Kakwi, J.D.; Yakasai, K.M.; Kakwi, J.D.; Raimi, M.O. Promotion over pixels: a mixed-methods analysis of vaccine communication strategies in Plateau State, Nigeria. BMJ Open 2025, e094029. [Google Scholar] [CrossRef]
- Kakwi, J.D.; Yakasai, K.M.; Raimi, M.O.; Kakwi, J.D. Understanding the Dynamics of COVID-19 Vaccine Uptake in Plateau State, Nigeria: Analyzing Socioeconomic, Cultural, and Communication Influences. JMIR Preprints 2024a, 30/12/2024, 70702. Available online: https://preprints.jmir.org/ojs/index.php/preprints/preprint/70702. [CrossRef]
- Kakwi, J.D.; Yakasai, K.M.; Kakwi, J.D.; Raimi, M.O. Campaigning Against Vaccine Hesitancy: Evaluating the Effectiveness of Health Communication on COVID-19 Vaccination Uptake in Plateau State, Nigeria. JMIR Preprints 2024b, 22/09/2024, 66755. Available online: https://preprints.jmir.org/preprint/66755. [CrossRef]
- Kelvin, E. A.; Akasreku, B. The evidence for HIV self-testing to increase HIV testing rates and the implementation challenges that remain. Current HIV/AIDS Reports 2020, 17(4), 281–289. [Google Scholar] [CrossRef]
- Kelvin, E. A.; George, G.; Mwai, E.; Kinyanjui, S.; Romo, M. L.; Odhiambo, J. O.; et al. A randomized controlled trial to increase HIV testing demand among female sex workers in Kenya through announcing the availability of HIV self-testing via text message. AIDS and Behavior 2019, 23(1), 116–125. [Google Scholar] [CrossRef] [PubMed]
- KoboToolbox KoboToolbox. n.d. Available online: https://www.kobotoolbox.org/.
- Merga, Kotu; Benti, T.; Edea, G.; Regea, F.; Zewdu, T.; Merga, H. Exploring HIV self-testing as an early detection strategy among female sex workers in Waliso town, Ethiopia: A community based cross sectional study. AIDS Research and Therapy 2025, 22(1), 36. [Google Scholar] [CrossRef] [PubMed]
- Kumwenda, M. K.; Mavhu, W.; Lora, W. S.; Chilongosi, R.; Sikwese, S.; Taegtmeyer, M.; et al. Feasibility and acceptability of a peer-led HIV self-testing model among female sex workers in Malawi: A qualitative study. BMJ Open 2021, 11(12), e049248. [Google Scholar] [CrossRef]
- Lora, W.; Desmond, N.; Obasi, A.; Kumwenda, M.; Taegtmeyer, M.; Tolhurst, R.; et al. “I wanted evidence that my status had changed, so that is why I tested”: Experiences with HIV self-testing among female sex workers in Malawi. AIDS Care 2020, 32(sup2), 206–213. [Google Scholar] [CrossRef]
- Ma, Z.; Guo, L.; Zhou, M.; Zuo, H. HIV/AIDS-related knowledge and attitudes towards HIV rapid testing among Chinese college students: Findings from a cross-sectional survey. Preventive Medicine Reports 2023, 9(36), 102409. [Google Scholar] [CrossRef]
- McGuire, M.; de Waal, A.; Karellis, A.; Janssen, R.; Engel, N.; Sampath, R.; et al. HIV self-testing with digital supports as the new paradigm: A systematic review of global evidence (2010–2021). EClinicalMedicine 2021, 39, 101059. [Google Scholar] [CrossRef]
- Mekonnen, H.; Manyazewal, T.; Kajogoo, V. D.; Getachew Assefa, D.; Gugsa Bekele, J.; Tolossa Debela, D. Advances in HIV self-testing: Systematic review of current developments and the road ahead in high-burden countries of Africa. SAGE Open Medicine 2023, 12, 20503121231220788. [Google Scholar] [CrossRef]
- Merga, K.; Benti, T.; Edea, G.; Regea, F.; Zewdu, T.; Merga, H. Exploring HIV self-testing as an early detection strategy among female sex workers in Waliso town, Ethiopia: A community based cross sectional study. AIDS Research and Therapy 2025, 22(1), 36. [Google Scholar] [CrossRef]
- Mhando, F.; M, N.; C, H.; K, O.; M, H.; S, J.; et al. Digital intervention services to promote HIV self-testing and linkage to care services: A bibliometric and content analysis-global trends and future directions. Frontiers in Public Health 2024, 16(45), 1606354. [Google Scholar] [CrossRef]
- Michael-Olomu, Oyintonyo; Gift, Raimi Aziba-anyam; Olalekan, Raimi Morufu. Strengthening Green Health System Sustainability through Enrollee-Centered Policy Reform: Insights from the National Health Insurance Scheme (NHIS) in Nigeria. Oral Presentation Presented at the ACS-FUO Conference of the Faculty of Science, Federal University Otuoke, Bayelsa State on the theme: Harnessing Green Chemistry & Artificial Intelligence for Sustainable Development, which held Tuesday, 4th - Thursday 7th November; 2025; p. Pg. 137. [Google Scholar]
- Mordecai, O.; Uchenna, G.E.; Emma, A.; Elemuwa, T.D.; Gabriel, J.O.; Egberipou, T.; Etim, E.O.; Christopher, O.E.; Morufu, O.R.; Anuoluwapo, B. Analyzing Nigeria’s Journey Towards Sustainable Development Goals: A Comprehensive Review From Inception to Present; Qeios, 2024. [Google Scholar] [CrossRef]
- Morufu, O.R.; Christopher, O.; Emeka, C.L.; Ebikapaye, O.; Alabo, A.F. Beyond Palliatives: Responding to the Current Flooding and Preventing the Next One from Kogi to Bayelsa State, 4th Edition ed; Bayelsa State Judiciary Magazine, 2022. [Google Scholar]
- Morufu, O.R.; Aziba-anyam, G.R.; Teddy, C.A. Evidence-based Environmental and Public Health Practices to Respond to the COVID-19 Crisis, 07 May 2021, PREPRINT (Version 1) available at Research Square; EMSID:EMS123969, 2021a. Available online: https://europepmc.org/article/PPRID/PPR335534. [CrossRef]
- Morufu, O.R.; Ebikapaye, O.; Tuebi, M.; Aziba-anyam, G.R.; Adedoyin, O.O.; Aishat, F.A.; Mariam, O.R.; Beatrice, O.J. Do Weak Institutions Prolong Crises? [#ENDSARs] in the Light of the Challenges and opportunities beyond COVID-19 Pandemic and the Next Normal in Nigeria. In Communication, Society and Media. ISSN 2576-5388 (Print) ISSN 2576-5396 (Online); 2021c; Vol. 4, No. 2, Available online: http://www.scholink.org/ojs/index.php/csm/article/view/3790. [CrossRef]
- Mshweshwe-Pakela, N.; Mabuto, T.; Shankland, L.; Fischer, A.; Hoffmann, C. J.; Tsukudu, D. Digitally supported HIV self-testing increases facility-based HIV testing capacity in Ekurhuleni, South Africa. Southern African Journal of HIV Medicine 2022, 23(1), 1352. [Google Scholar] [CrossRef] [PubMed]
- NACA. Report of the Key Population Programme Review in Nigeria; 2024. Available online: https://naca.gov.ng/wp-content/uploads/2024/09/Signed-KPPR-Draft-Final-Report-27082024DG-Director-RM-E.pdf.
- National Population Commission (NPC) [Nigeria]; ICF. Nigeria demographic and health survey 2018; NPC and ICF, 2019. [Google Scholar]
- Nimisingha, J.A.; Morufu, O.R.; Lawan, M.I.; Alina, P.; Anuoluwapo, A.B.; Sarah, S.J.; Funmilayo, A.A. 2024) Advancements in Disaster Response through Telemedicine and Emergency Medical Operating System (TELEMED-EMOS) Integration: A Narrative Review; Advance., 20 August 2024. [Google Scholar] [CrossRef]
- Nnko, S.; Nyato, D.; Kuringe, E.; Casalini, C.; Shao, A.; Komba, A.; et al. Female sex workers perspectives and concerns regarding HIV self-testing: An exploratory study in Tanzania. BMC Public Health 2020, 20(1), 959. [Google Scholar] [CrossRef]
- Ochalek, T. A.; Heil, S. H.; Higgins, S. T.; Badger, G. J.; Sigmon, S. C. A novel mHealth application for improving HIV and Hepatitis C knowledge in individuals with opioid use disorder: A pilot study. Drug and Alcohol Dependence 2018, 190, 224–228. [Google Scholar] [CrossRef]
- Ochonye, B.; Folayan, M. O.; Fatusi, A. O.; Bello, B. M.; Ajidagba, B.; Emmanuel, G.; et al. Sexual practices, sexual behavior and HIV risk profile of key populations in Nigeria. BMC Public Health 2019, 19(1), 1210. [Google Scholar] [CrossRef]
- Odubo, T.R.; Raimi, M.O. 2019) Resettlement and Readjustment Patterns of Rural Dwellers During and After Flood Disasters in Bayelsa State Nigeria. British Journal of Environmental Sciences 2019, Vol.7(No.3), Pp. 45–52. Available online: www.eajournals.org.
- Ogar, O. O.; Iruo, L. A.; Raimi, M. O. Evaluating public health education for the prevention of mother-to-child HIV transmission among pregnant women in Cross River State, Nigeria. Preprints 2026. [Google Scholar] [CrossRef]
- Ogunyemi, D.; Ogunmefun, O. T.; Oluwole, E.; Ekundayo, A. Knowledge, attitude, and utilization of HIV counseling and testing by female sex workers in Lagos State, Nigeria. Babcock University Medical Journal 2020, 3(2), 1–9. [Google Scholar] [CrossRef]
- Okechukwu, C.O.; Ainu, M.; Adias, T.C.; Elemuwa, C.O.; Rotifa, S.U.; Ogbointuwei, C.; Raimi, M.O.; Oweibia, M.; Alabo, A.F.; Okoyen, E.; Appah, W.W. Evaluating the Impact of Rotavirus Vaccination on Childhood Diarrhea Incidence in Bayelsa State, Nigeria: Achievements, Challenges, and Future Directions. JMIR Preprints 2024, 27/07/2024, 64822. Available online: https://preprints.jmir.org/preprint/64822. [CrossRef]
- Olaniyi, A.O.; Morufu, O.R. From Crisis to Catalyst: Leveraging Public Health Emergencies to Redesign Urban Health Policy in Nigerian Megacities. Oral Presentation Presented at the 3rd Ku8+International Conference, Kwara State University, Malete with the theme “Innovation and Sustainability of Higher Education in a Changing World.”, which held on Wednesday, 6th – Friday 8th August; 2025. [Google Scholar]
- Ortblad, K. F.; Kibuuka Musoke, D.; Ngabirano, T.; Nakitende, A.; Taasi, G.; Barresi, L. G.; et al. HIV self-test performance among female sex workers in Kampala, Uganda: A cross-sectional study. BMJ Open 2018, 8(11), e022652. [Google Scholar] [CrossRef] [PubMed]
- Oweibia, M.; Elemuwa, U.G.; Akpan, E.; et al. Analyzing Nigeria’s Journey Towards Sustainable Development Goals: A Comprehensive Review From Inception To Present [version 1; peer review: awaiting peer review]. F1000Research 2024, 13, 984. [Google Scholar] [CrossRef]
- Pai, N.; Esmail, A.; Chaudhuri, P. S.; Oelofse, S.; Pretorius, M.; Marathe, G.; et al. Impact of a personalised, digital, HIV self-testing app-based program on linkages and new infections in the township populations of South Africa. BMJ Global Health 2021, 6(9), e006032. [Google Scholar] [CrossRef]
- Patrício, A. C. F. A.; Bezerra, V. P.; Nogueira, J. A.; Moreira, M. A. S. P.; Camargo, B. V.; Santos, J. S. Knowledge of sex workers about HIV/AIDS and its influence on sexual practices. Revista Brasileira de Enfermagem 2019, 72(5), 1311–1317. [Google Scholar] [CrossRef]
- Perekibina, A.B.; Charles, O.; Morufu, O.R. Beyond Compliance: Evaluating Environmental Standards for oil Spills and their implications for Environmental Protection in the Niger Delta, Nigeria; Authorea., 2025. [Google Scholar] [CrossRef]
- Promise, V.I.; Alabere, I.; Abdulraheem, I.; Raimi, M.O. Improving Childhood Immunization Completion in Rural Bayelsa State, Nigeria: A Pragmatic Cluster Randomized Trial of Mobile Phone Reminders and Home Visits. Open Journal of Preventive Medicine 2026, 16, 1–20. [Google Scholar] [CrossRef]
- Promise, V.I.; Alabere, I.; Abdulraheem, I.; Raimi, M.O. The Effect of Mobile Phone and Home Visit on Childhood Vaccination Uptake in Rural Communities of Bayelsa State Nigeria. A Pragmatic Cluster Randomized Control Trial. JMIR Preprints 2025, 01/04/2025, 75332. Available online: https://preprints.jmir.org/preprint/75332. [CrossRef]
- Promise, V.I.; Macauley, T.; Alabere, I.; Abdulraheem, I.; Raimi, M.O. Closing the Gap: Assessment of Vaccination Coverage Among Under Two Children in Bayelsa State, Nigeria. JMIR Preprints. 2024, 29/12/2024, 70671. Available online: https://preprints.jmir.org/preprint/70671. [CrossRef]
- Raimi, M. O.; Ochayi, E. O. Assessment of the rate of sexually transmitted diseases in Kubwa F.C.T. Abuja, Nigeria. Science Journal of Public Health 2017, 5(5), 365–376. [Google Scholar] [CrossRef]
- Raimi, M.O.; Raimi, A.G. The Toughest Triage in Decision Impacts: Rethinking Scientific Evidence for Environmental and Human Health Action in the Times of Concomitant Global Crises. CPQ Medicine 2020, 11(1), 01–05. [Google Scholar]
- Raimi, M.O.; Moses, T.; Okoyen, E.; Sawyerr, H.O.; Joseph, B.O.; Oyinlola, B.O. A Beacon for Dark Times: Rethinking Scientific Evidence for Environmental and Public Health Action in the Coronavirus Diseases 2019 Era. In Medical and Research Microbiology; 2020; Vol. 1, p. 3. [Google Scholar]
- Raimi, M.O.; Mcfubara, K.G.; Abisoye, O.S.; Ifeanyichukwu, E.C.; Henry, S.O.; Raimi, G.A. Responding to the call through Translating Science into Impact: Building an Evidence-Based Approaches to Effectively Curb Public Health Emergencies [COVID-19 Crisis]. Global Journal of Epidemiology and Infectious Disease 2021, 1(1). Available online: https://www.scipublications.com/journal/index.php/gjeid/article/view/72. [CrossRef]
- Raimi, M.O.; Odubo, T.R.; Ogah, A. Women, Water and Development in the Global South. Oral Presentation Presented at the Multidisciplinary International Conference on Water in Africa (ICWA 2022) on the theme: Towards Successful Delivery of SDGs 3 & 6, which held February 09 – 11; 2022. [Google Scholar]
- Raimi, M.O.; Odubo, T.R.; Odubo, T.V.; Omidiji, A.O. (2022b) Gender and Sustainability in the Niger Delta. Oral Presentation Presented at the Multidisciplinary International Conference on Water in Africa (ICWA 2022) on the theme: Towards Successful Delivery of SDGs 3 & 6, which held February 09 – 11; 2022. [Google Scholar]
- Raimi, O.M.; Sunday, O.A.; Mcfubara, K.G.; Adias, T.C.; Raimi, G.A.; Daniel, A.A.; Izah, S.C.; Okoyen, E.; Ogbointuwei, C.; Clement, A.; Godspower, A.; Funmilayo, A.A. Raimi, M. O., Sunday, O. A., Sawyerr, H. O., Adias, T. C., Eds.; Perspective Chapter: Applying Innovative Research as a Tool to Advance Immunization Coverage in Bayelsa State, Nigeria. In Emerging Issues in Environmental Epidemiology and Its Reflection [Working Title]. IntechOpen.; 2022c. [Google Scholar] [CrossRef]
- Shava, E.; Manyake, K.; Mdluli, C.; Maribe, K.; Monnapula, N.; Nkomo, B.; et al. Acceptability of oral HIV self-testing among female sex workers in Gaborone, Botswana. PLOS ONE 2020, 15(7), e0236052. [Google Scholar] [CrossRef]
- Sibanda, E.; Taegtmeyer, M. Inequalities in uptake of HIV testing despite scale-up. The Lancet Global Health 2020, 8, e744–e745. [Google Scholar] [CrossRef]
- Tano, D.A.; Odafivwotu, O.; Morufu, O.R. Residents’ Perception and Adjustment to Floods in Yenagoa Metropolis, Nigeria; Advance., 12 September 2024. [Google Scholar] [CrossRef]
- Terefe, B.; Jembere, M. M.; Reda, G. B.; Asgedom, D. K.; Assefa, S. K.; Lakew, A. M. Knowledge and utilization of HIV self-testing, and its associated factors among women in sub–Saharan Africa: Evidence from 21 countries demographic and health survey. BMC Public Health 2024, 24(1), 1960. [Google Scholar] [CrossRef]
- Tokar, A.; Broerse, J. E. W.; Blanchard, J.; Roura, M. HIV testing and counseling among female sex workers: A systematic literature review. AIDS and Behavior 2018, 22(8), 2435–2457. [Google Scholar] [CrossRef] [PubMed]
- Tuebi, M.; Franco, A.; Raimi, M.O.; Chidubem, O.; Sampou, W.D. The Quality and Acceptance of Family Planning Services in Improving Bayelsa State: Lessons Learnt From a Review of Global Family Planning Programs. Greener Journal of Medical Sciences 2021, 11(2), 212–225. [Google Scholar]
- Tun, W.; Vu, L.; Dirisu, O.; Sekoni, A.; Shoyemi, E.; Njab, J.; et al. Uptake of HIV self-testing and linkage to treatment among men who have sex with men (MSM) in Nigeria: A pilot programme using key opinion leaders to reach MSM. Journal of the International AIDS Society 2018, 21 (Suppl 5), e25124. [Google Scholar] [CrossRef] [PubMed]
- Vara, P. A.; Buhulula, L. S.; Mohammed, F. A.; Njau, B. Level of knowledge, acceptability, and willingness to use oral fluid HIV self-testing among medical students in Kilimanjaro region, Tanzania: A descriptive cross-sectional study. AIDS Research and Therapy 2020, 17(1), 56. [Google Scholar] [CrossRef]
- Wang, C.; Wang, Y. J.; Tucker, J. D.; Xiong, M. Z.; Fu, H. Y.; Smith, M. K.; et al. Correlates of HIV self-testing among female sex workers in China: Implications for expanding HIV screening. Infectious Diseases of Poverty 2020, 9(1). Available online: https://pubmed.ncbi.nlm.nih.gov/33092641/. [CrossRef]
- Washington, T. A.; Applewhite, S.; Glenn, W. Using Facebook as a platform to direct young black men who have sex with men to a video-based HIV testing intervention: A feasibility study. Urban Social Work 2017, 1(1), 36–52. [Google Scholar] [CrossRef]
- Witzel, T. C.; Wright, T.; McCabe, L.; Gabriel, M. M.; Wolton, A.; Gafos, M.; et al. Impact and acceptability of HIV self-testing for trans men and trans women: A mixed-methods subgroup analysis of the SELPHI randomised controlled trial and process evaluation in England and Wales. EClinicalMedicine 2021, 32, 100700. [Google Scholar] [CrossRef]
- World Health Organization (WHO). HIV and AIDS. 2025. Available online: https://www.who.int/news-room/fact-sheets/detail/hiv-aids.
- Yusuf, B.A.; Morufu, O.R.; Agbebaku, H.U. Echoes of Outbreaks Past: Rethinking Public Health Preparedness in Sub-Saharan Africa in the Age of Emerging Pandemics. Oral Presentation Presented at the 3rd Ku8+International Conference, Kwara State University, Malete with the theme “Innovation and Sustainability of Higher Education in a Changing World.”, which held on Wednesday, 6th – Friday 8th August; 2025. [Google Scholar]
- Zhu, X.; Zhang, W.; Operario, D.; Zhao, Y.; Shi, A.; Zhang, Z.; et al. Effects of a mobile health intervention to promote HIV self-testing with MSM in China: A randomized controlled trial. AIDS and Behavior 2019, 23(11), 3129–3139. [Google Scholar] [CrossRef] [PubMed]
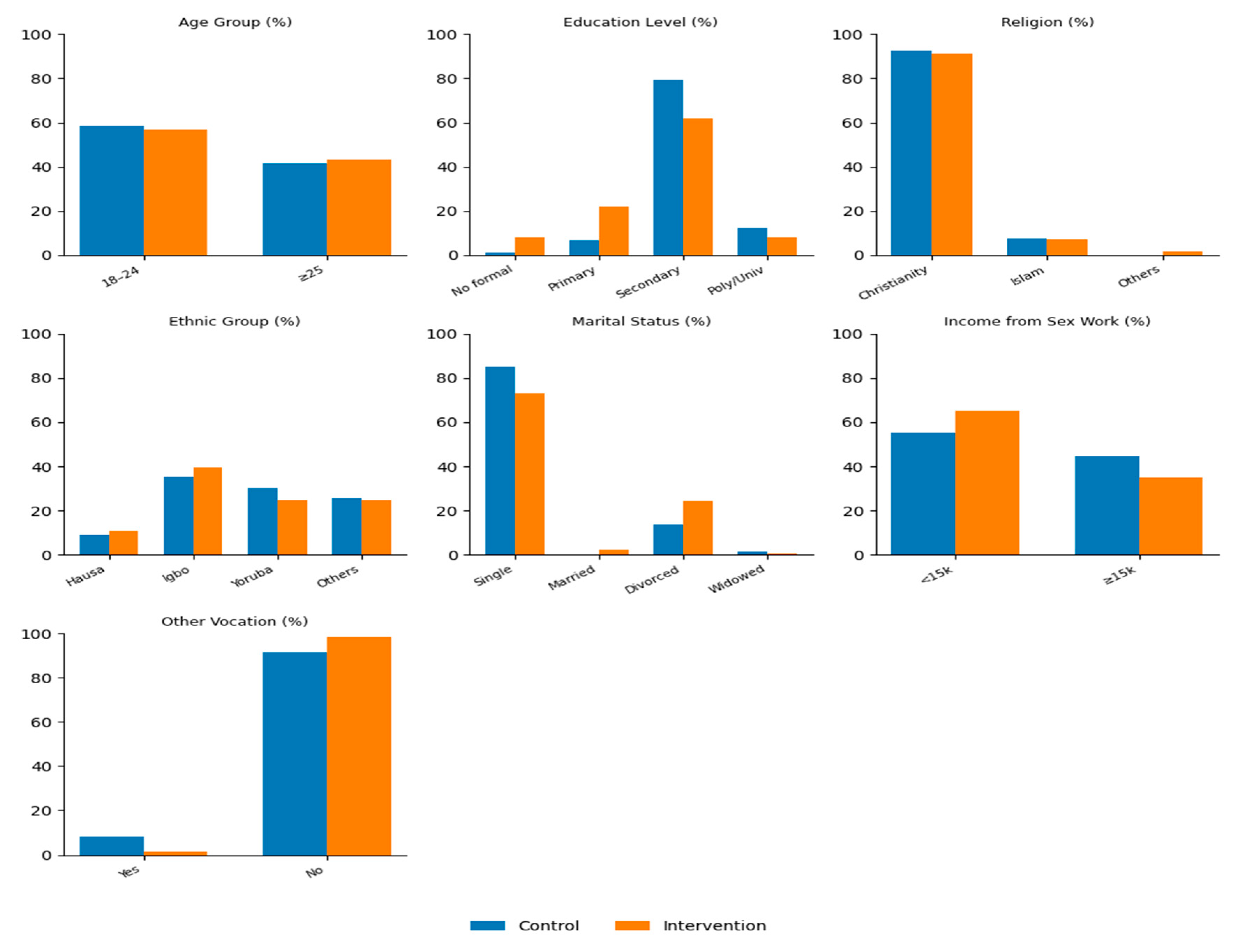
| Variables | Control group | Intervention group | Total | Test Statistic | P value |
|---|---|---|---|---|---|
| n = 145 (%) | n = 137 (%) | N=282 | |||
| Age in years | |||||
| Mean SD | 23.26 ± 3.177 | 24.32 ± 3.935 | 2.509 T | 0.013T | |
| Age group of respondents (Years) | |||||
| 18-24 | 85 (58.6) | 78 (56.9) | 163 (57.8) | 0.082 X | 0.810 X |
| ≥ 25 | 60 (41.4) | 59 (43.1) | 119 (42.2) | ||
| Educational level | |||||
| No formal education | 2 (1.4) | 11 (8.0) | 13 (4.6) | <0.001 F | |
| Primary | 10 (6.9) | 30 (21.9) | 40 (14.2) | ||
| Secondary | 115 (79.3) | 85 (62.0) | 200 (70.9) | ||
| Polytechnic/University | 18 (12.4) | 11 (8.0) | 29 (10.3) | ||
| Religion | |||||
| Christianity | 134 (92.4) | 125 (91.2) | 259 (91.8) | 0.536 F | |
| Islam | 11 (7.6) | 10 (7.3) | 21 (7.4) | ||
| Others a | 0 (0.0) | 2 (1.5) | 2 (0.7) | ||
| Ethnic group | |||||
| Hausa | 13 (9.0) | 15 (10.9) | 28 (9.9) | 1.412X | 0.703X |
| Igbo | 51 (35.2) | 54 (39.4) | 105 (37.2) | ||
| Yoruba | 44 (30.3) | 34 (24.8) | 78 (27.7) | ||
| Others b | 37 (25.5) | 34 (24.8) | 71 (25.2) | ||
| Marital Status | |||||
| Single | 123 (84.8) | 100 (73.0) | 223 (79.1) | 0.017 F | |
| Married | 0 (0.0) | 3 (2.2) | 3 (1.1) | ||
| Divorced | 20 (13.8) | 33 (24.1) | 53 (18.8) | ||
| Widowed | 2 (1.4) | 1 (0.7) | 3 (1.1) | ||
| Average weekly income from sex work (₦) | |||||
| Less than ₦15,000 | 80 (55.2) | 89 (65.0) | 169 (59.9) | 2.812 X | 0.060 X |
| ₦15,000 and above | 65 (44.8) | 48 (35.0) | 113 (40.1) | ||
| Other vocation apart from sex work | |||||
| Yesc | 12 (8.3) | 2 (1.5) | 14 (5.0) | 0.011 F | |
| No | 133 (91.7) | 135 (98.5) | 268 (95.5) | ||
| Average weekly income from other vocation (₦) | |||||
| Less than ₦15,000 | 12 (100.0) | 0 (0.0) | 12 (85.7) | 0.011 F | |
| ₦15,000 and above | 0 (0.0) | 2 (100.0) | 2 (14.3) | ||
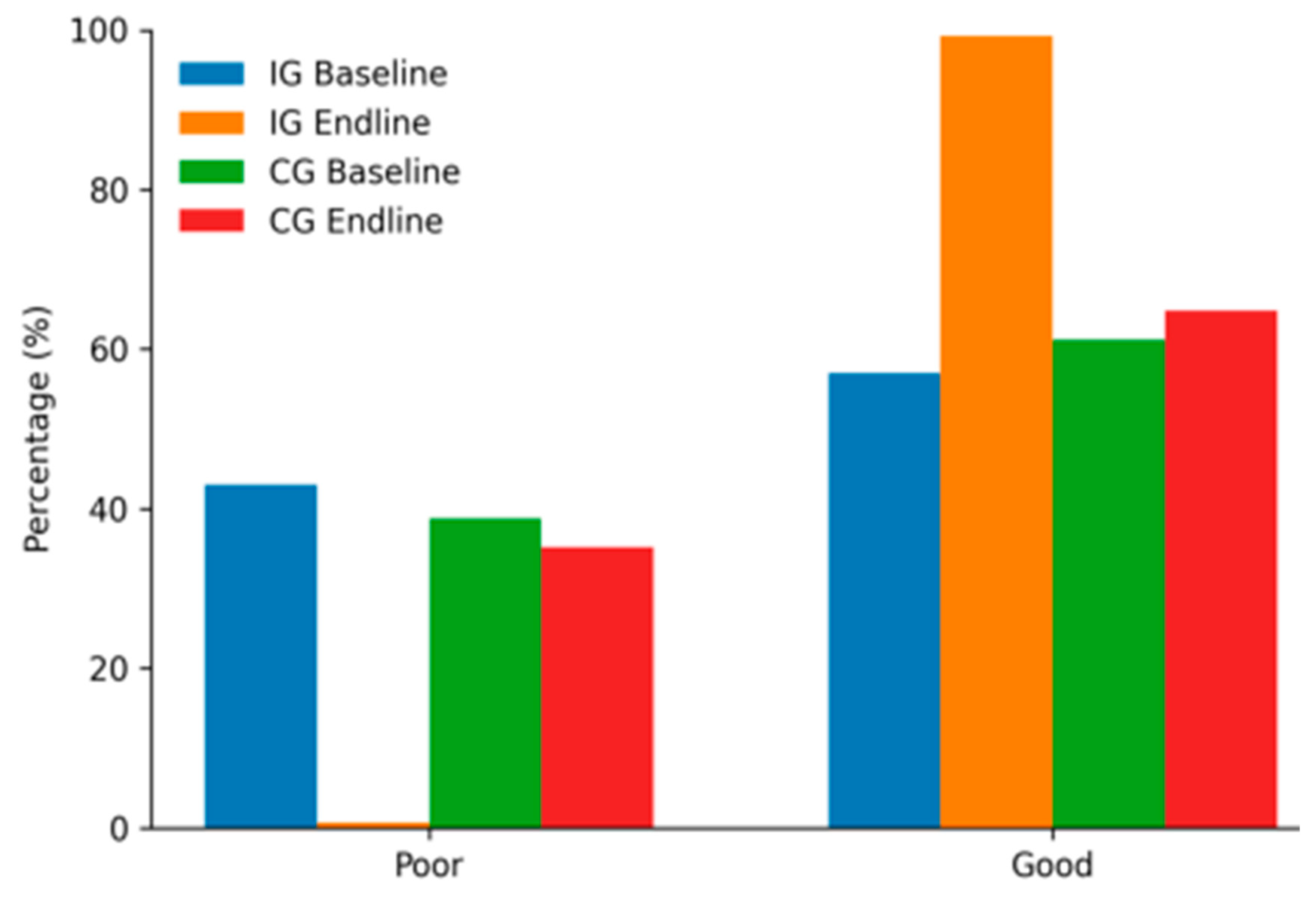
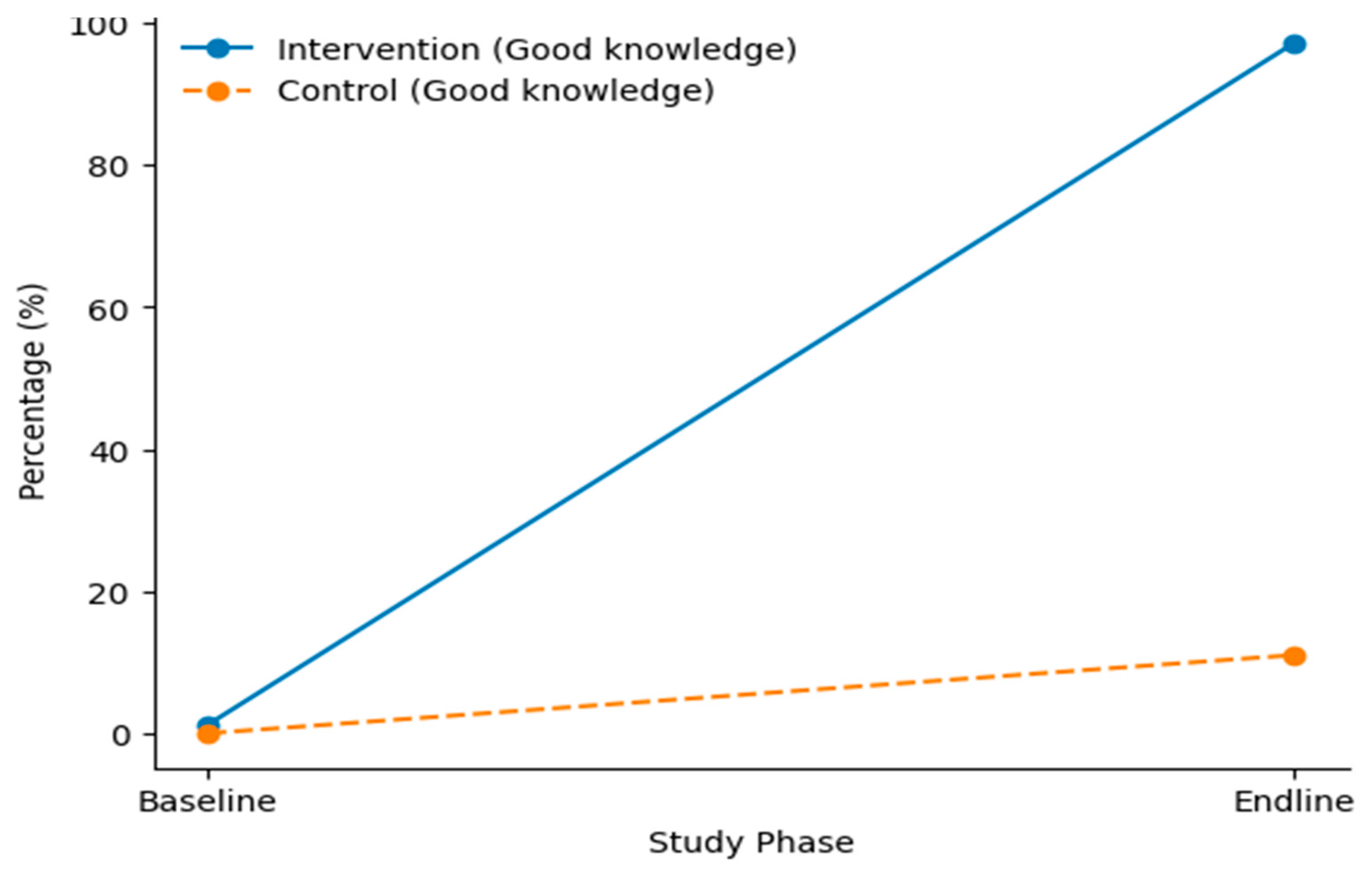
| HIV knowledge level | Baseline n (%) IG=165 CG= 165 |
Endline n (%) IG=137 CG= 145 |
% Change |
P-value |
DID estimate (95% CI, P-value) | |
|---|---|---|---|---|---|---|
| Intervention group | Poor knowledge | 71 (43.0) | 1 (0.7) | -42.3 | ||
| Good knowledge | 94 (57.0) | 136 (99.3) | 42.3 | <0.001 | ||
| 38.7(95% CI 0.25-0.53, p< 0.001) | ||||||
| Control group | Poor knowledge | 64 (38.8) | 51 (35.2) | -3.6 | ||
| Good knowledge | 101 (61.2) | 94 (64.8) | 3.6 | 0.296 | ||
| χ² (p-value) | 0.614 (0.433) X | (<0.001) F |
| HIVST knowledge level | Baseline n (%) IG=165 CG= 165 |
Endline n (%) IG=137 CG= 145 |
% Change |
P-value | DID estimate (95% CI, P-value) | |
|---|---|---|---|---|---|---|
| Intervention group | Poor knowledge | 163 (98.8) | 4 (2.9) | -95.9 | ||
| Good knowledge | 2 (1.2) | 133 (97.1) | 95.9 | <0.001 | ||
| 84.9(95% CI: 0.79-0.91, p< 0.001) | ||||||
| Control group | Poor knowledge | 165 (100.0) | 129 (89.0) | -11.0 | ||
| Good knowledge | 0 (0.0) | 16 (11.0) | 11.0 | <0.001 | ||
| χ² (p-value) | (0.498)F | (0.000)F |
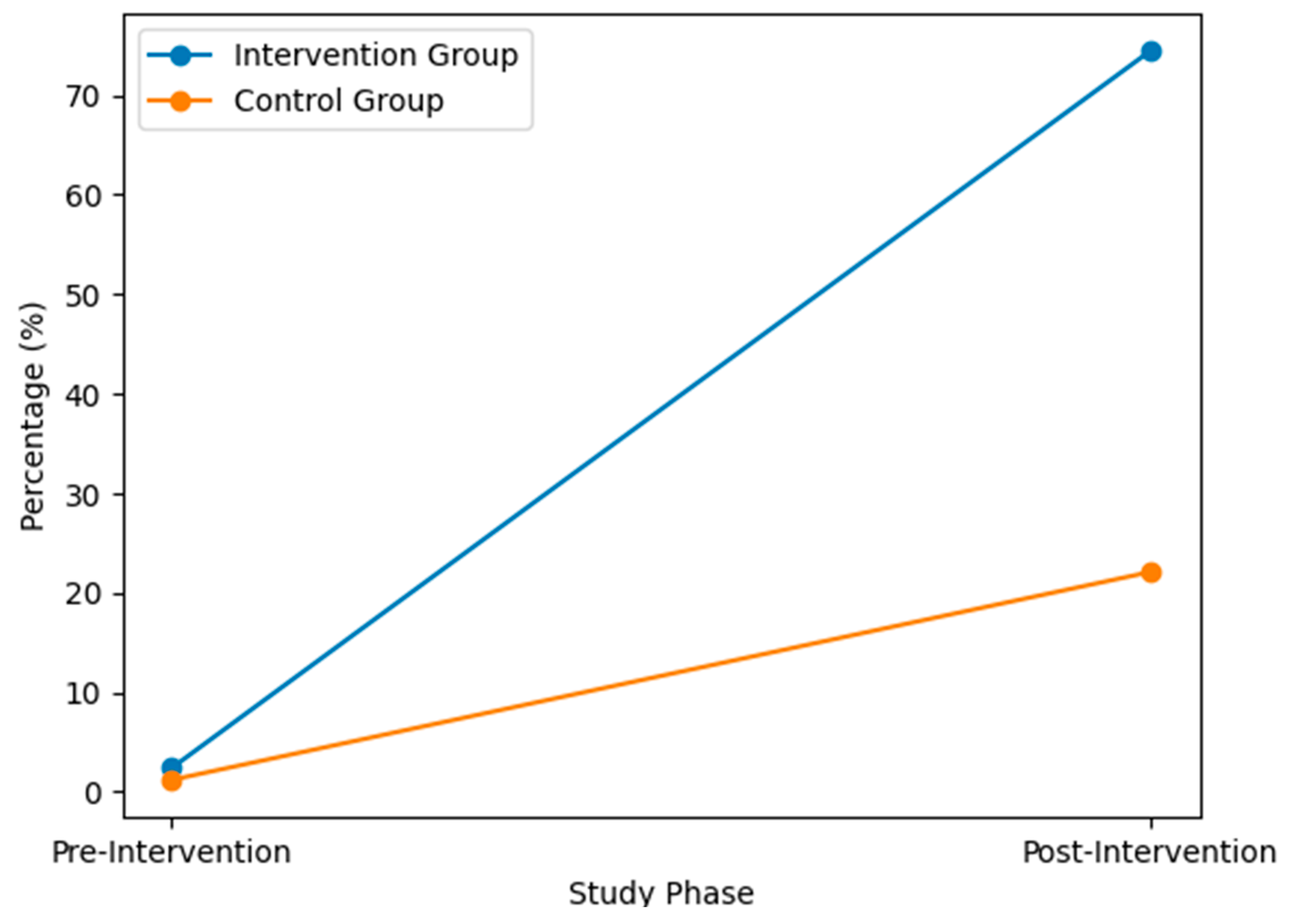
| Intervention Group |
Control Group |
|
|---|---|---|
| Pre-Intervention | 4 (2.4) | 2 (1.2) |
| Post -intervention | 102 (74.5) | 32 (22.1) |
| χ²(p-value) | < 0.001F | < 0.001F |
| D | 72.1 | 20.9 |
| DID estimate (95% CI, p-value) | 51.2 (95% CI 0.41-0.61, p< 0.001) | |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




